Abstract
Overexpression of the HMGA2 gene is a common feature of neoplastic cells both in experimental and human models. Intragenic and extragenic HMGA2 rearrangements responsible for HMGA2 gene overexpression have been frequently detected in human benign tumours of mesenchymal origin. To better understand the role of HMGA2 overexpression in human tumorigenesis, we have generated transgenic mice carrying the HMGA2 gene under the transcriptional control of the cytomegalovirus promoter. High expression of the transgene was demonstrated in all the mouse tissues analysed, whereas no expression of the endogenous HMGA2 gene was detected in the same tissues from wild-type mice. In this study, two indipendent lines of transgenic mice have been generated. By 6 months of age, 85% of female animals of both transgenic lines developed pituitary adenomas secreting prolactin and growth hormone. The transgenic males developed the same phenotype with a lower penetrance (40%) and a longer latency period (about 18 months). Therefore, these data demonstrate that the overexpression of HMGA2 leads to the onset of mixed growth hormone/prolactin cell pituitary adenomas. These transgenic mice may represent an important tool for the study of this kind of neoplasia.
Similar content being viewed by others
Introduction
The HMGA2 protein belongs to the High Mobility Group A (HMGA) family. Other members of this family include HMGA1a, HMGA1b and HMGA1c, three different isoforms of the HMGA1 gene (Johnson et al., 1989; Nagpal et al., 1999). They are small, non-histone, chromatin-associated proteins that bind DNA in AT-rich regions through three basic domains named ‘AT-hook’. The HMGA protein family members have no intrinsic transcriptional activity, but they can regulate transcription by altering the architecture of chromatin and facilitating the assembly of multiprotein complexes of transcriptional factors (Thanos and Maniatis, 1995).
HMGA gene expression is negligible in normal adult tissues, apart from a very low expression in CD34 positive stem cells (Rommel et al., 1997), and in mouse pre-adipocytic cells (Anand and Chada, 2000), and is essentially restricted to embryonic development (Chiappetta et al., 1996; Zhou et al., 1995). HMGA overexpression has been shown in several human and experimentally induced malignant tumours (Abe et al., 1999, 2000; Bandiera et al., 1998; Chiappetta et al., 1995, 1998, 2001; Fedele et al., 1996; Giancotti et al., 1987). HMGA proteins have a key role in malignant transformation since suppression of HMGA expression, by an antisense methodology, prevents malignant transformation of thyroid cells by acute retroviruses (Berlingieri et al., 1995).
Rearrangements of the HMGA2 gene have been frequently detected in human benign tumours of mesenchymal origin, including lipomas, pulmonary hamartomas, uterine leiomyomas, endometrial polyps and fibroadenomas of the breast (Ashar et al., 1995; Bol et al., 1996; Kazmierczak et al., 1995; Schoenmakers et al., 1995; Staats et al., 1996). 12q13–15 chromosomal translocations involving the HMGA2 gene locus, account for these rearrangements. The HMGA2 protein has three AT-hook domains and an acidic carboxy-terminal tail. The HMGA2 modifications consist in the loss of the acidic carboxy-terminal tail and fusion with ectopic sequences. Recent results show that the loss of the carboxy-terminal region, rather than the acquisition of new sequences, is sufficient to confer to HMGA2 the ability to transform NIH3T3 cells (Fedele et al., 1998). Moreover, transgenic mice carrying a truncated HMGA2 gene showed a giant phenotype together with abdominal/pelvic lipomatosis (Arlotta et al., 2000; Battista et al., 1999; Fedele et al., 2001). In several human benign tumours, overexpression of the wild type HMGA2 gene following chromosomal translocation has also been detected (Rogalla et al., 1996; Schoenberg Fejzo et al., 1996). However, the role of HMGA2 overexpression in tumorigenesis still needs to be defined.
Since transgenic mice provide a powerful experimental approach to define the role of oncogenes in neoplastic processes in vivo (Hogan, 1983), we generated transgenic mice carrying the HMGA2 wild type gene under transcriptional control of the cytomegalovirus (CMV) promoter to establish the role of HMGA2 overexpression in tumorigenesis. HMGA2 transgenic mice showed abundant HMGA2 expression in all normal tissues analysed, whereas no expression was observed in control mice. By 6 months of age the large majority (85%) of female HMGA2 mice developed pituitary adenomas secreting prolactin (PRL) and growth hormone (GH). The same phenotype appeared with lower penetrance (40%) and longer latency period (about 18 months) in HMGA2 males. Thus, in independently derived transgenic lines, we demonstrate a key role of HMGA2 overexpression in pituitary tumorigenesis. These mice have the potential to serve as a valuable experimental model for human pituitary adenomas.
Results
Generation of transgenic mice overexpressing the HMGA2 gene
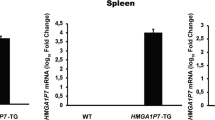
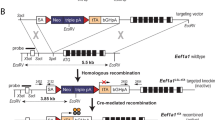
A wild type HMGA2 cDNA under the transcriptional control of the CMV promoter (Figure 1a) was microinjected into B6C3F2 fertilized eggs and subsequently transferred to pseudopregnant females. Analysis of the offspring, by Southern blot analysis of tail DNAs digested with BamHI and hybridized with a cDNA corresponding to the CMV promoter, led us to identify two potential founders (Figure 1b). They were bred with wild type C57BL/6J mice and two stable lines were obtained. Southern blot analysis confirmed the integration of the transgene (Figure 1b). Similar numbers of integrated copies were found in both transgenic lines (data not shown). All founders transmitted the transgene in a Mendelian fashion (data not shown). Those offspring that did not inherit the transgene were used in our studies as controls. Transgene expression was analysed by RT–PCR using total RNA extracted from brown adipose tissue (BAT), heart, pituitary gland, liver, spleen, and kidney (Figure 1c). The transgene expression was observed in all the analysed tissues. The highest expression was observed in spleen, kidney and pituitary gland, whereas the lowest expression was detected in liver tissue. No expression of endogenous HMGA2 was detected in tissues from transgenic (data not shown) or wild type control mice (Figure 1c, lanes 7 and 8), in accordance with previous published results (Battista et al., 1999).
(a) Schematic representation of the CMV/HMGA2 transgene. (b) Analysis of the integration of the CMV/HMGA2 construct by Southern Blot. DNA samples were as follows: lane 1: transgenic founder mouse (F0) #1; lane 2: transgenic F1 mouse from founder #1; lane 3: wild type F1 mouse from founder #1; lane 4: transgenic founder mouse (F0) #2; lane 5: wild type F1 mouse from founder #2; lane 6: transgenic F1 mouse from founder #2. (c) Analysis of the expression of the HMGA2 gene by RT–PCR. Lanes 1–6: RNAs extracted from different tissues of a HMGA2 transgenic mouse; lanes 7 and 8: RNA extracted from a pool of pituitary glands and a spleen of control mice
HMGA2 mice develop pituitary adenomas
At 12 months of age, most of the HMGA2 transgenic mice showed a deformed skull and several symptoms of head tilt (loss of equilibrium, excessive tear production and general behavioural changes suggestive of headache). Magnetic Resonance Imaging (MRI) analysis showed a large tumour mass in the skull base pushing the brain upward against the cranium and causing an alteration of the normal profile (Figure 2a). The mice with evident symptoms of head tilt were sacrificed and the tumour mass was analysed. In Figure 2b, dorsal and ventral views of a transgenic mouse brain with tumour is shown. A large haemorrhagic mass, spanning 2/3 of the extent of the brain, is located immediately caudal of the optic chiasm. The tumours were friable and easily detached from the surrounding brain tissue and there was no evidence of gross infiltration of the brain or sphenoid bone.
(a) MRI analysis of a female transgenic mouse 11 months old (right) compared to a wild type control mouse (left). The arrow indicates a large tumour mass in the skull base. (b) Dorsal (left) and ventral (right) views of a typical transgenic brain of a 12 months old female. Attached to the brain, but easily detachable, is a large haemorrhagic mass spanning 2/3 of the extend of the brain. (c) Histological analysis, by hematoxylin and eosin (H and E) stain, of a HMGA2 pituitary adenoma (original magnification 100×). Asterisk marks the neurohypophysis in the center of the intermediate lobe of the pituitary. All around the cleft is the tumoral tissue that completely obliterated the anterior pituitary. (d) Primary culture of cells from a HMGA2 pituitary adenoma. (e) Ultrastructure of a HMGA2 pituitary adenoma by electron microscopy. Magnification of main image 5200×. Inset in upper left corner shows structure of typical dense core granules
Sections from the tumour samples were paraffin embedded and stained with hematoxylin and eosin (Figure 2c). The tumours demonstrate a follicular type architecture with numerous blood lakes. The follicles were lined by cuboidal to polygonal cells with eosinophilic cytoplasm and hyperchromatic nuclei. There was no infiltration of surrounding brain tissue. Usually, at the edges of the tumour there were numerous hemosiderin laden macrophages indicative of remote haemorrhage. A portion of the intermediate lobe of the pituitary could be identified along with its adjacent neurohypophyseal tissue. The intermediate lobe was separated from the tumour cells by a fluid filled cleft. The tumour cells more closely resemble those of the anterior lobe (adenohypophysis). There was no evidence of any residual adenohypophysis in any of the mice with large tumours. It seems likely that the adenoma totally overgrew the normal gland or that the tumour cells were infiltrative and markedly expanded the gland. In support of the latter was the finding that very small, early tumours demonstrated infiltration of neoplastic cells into the normal adenohypophysis (data not shown). Accordingly, primary cultures of the tumours showed the typical epithelial phenotype of the adenohypophyseal cells (Bauer et al., 1990) (Figure 2d). Moreover, they were not able to grow indefinitely in culture or to induce tumorigenesis if injected into nude mice (data not shown). Ultrastructural analysis (Figure 2e) demonstrates a mixed population of polygonal tumour cells displaying varying numbers of neurosecretory type dense core granules compatible with neuroendocrine differentiation. These morphological findings are typical of a secreting pituitary adenoma. As shown in Table 1, pituitary adenomas were diagnosed in about 85% of the female transgenic HMGA2 mice by the age of 6 months. Conversely, in transgenic males the pathology appeared with a longer latency period (18 months of age) and a lower penetrance (about 40%).
HMGA2-induced pituitary adenomas secrete prolactin and growth hormone
Immunohistochemical studies using antisera immunoreactive to HMGA2 (Figure 3b) showed a strong nuclear staining, whereas no staining was observed without addition of the primary antibody (Figure 3a). Immunohistochemistry using antisera immunoreactive to murine pituitary hormones secreted from the anterior lobe was also carried out to define the subtype of the pituitary adenomas. As shown in Figure 3, a strong cytoplasmic immunoreactivity for PRL (Figure 3c and e) and GH (Figure 3d and f) was observed, whereas only very rare cells show immunoreactivity for Luteinizing Hormone (LH), Thyroid-Stimulating Hormone (TSH), Follicle-Stimulating Hormone (FSH), Melanocyte-Stimulating Hormone (MSH) or Adrenocorticotropic Hormone (ACTH) (data not shown). These rare immunoreactive cells most likely represent residual entrapped cells of the normal adenohypophysis that has been massively expanded by tumour cells. To determine whether or not PRL immunoreactive cells were also producing GH, serial sections were stained with antisera raised against PRL and GH. As it appears by the comparison of the images, the tumour consists of at least two cell populations: those secreting prolactin (Figure 3c and e) and those secreting growth hormone (Figure 3d and f). These results correlate well with the ultrastructural findings which indicate at least two populations of cells (Figure 2e): those with numerous dense core granules are fairly typical of growth hormone adenomas whereas cells with few dense core granules most likely represent prolactin producing cells. However, because we could not exclude the presence of a third population of mammosomatotroph cells secreting both hormones, cellular localization of GH and PRL was determined by in situ double immunofluorescent staining. As shown in Figure 4, the double red/green fluorescence of a pituitary adenoma from a HMGA2 mouse demonstrates the presence in the tumour of cells producing prolactin (green), growth hormone (red) and both hormones (yellow in the merging image). Thus, we conclude that the tumour consists of three different cell populations: one secreting GH, one secreting PRL and one secreting both hormones.
Immunohistochemical studies on HMGA2-induced pituitary adenomas using antisera immunoreactive to mouse pituitary hormones: (a) H and E staining. (b) Anti-HMGA2 antisera: strong, mainly nuclear staining was observed. (c) Anti-PRL antisera: strong cytoplasmic staining was observed in most of the cells. The inset shows the area reproduced in (e) at a higher magnification. (d) Anti-GH antisera: strong cytoplasmic staining was observed in many cells. The inset shows the area reproduced in (f) at a higher magnification; (c/e) and (d/f) are serial sections of the same adenoma area stained for PRL and GH, respectively. The cells producing GH and those producing prolactin are not the same
In situ double immunofluorescence of HMGA2-induced pituitary adenomas. Slices of pituitary adenomas from HMGA2 mice were processed for indirect immunofluorescence using Fluorescein (FITC: green stain), to reveal prolactin (Top Panel) and Texas red (TR: red stain), to reveal GH (Middle Panel). The bottom panel shows the merging image of the double red/green immunofluorescence labeling. Yellow spots are indicative of cells producing both PRL and GH hormones
The immunohistochemical results were confirmed at the mRNA level by a semiquantitative RT–PCR method. Figure 5a shows a drastic increase of GH and PRL gene expression in a representative pituitary adenoma compared to pituitary glands from control mice. Densitometric analysis was carried out to quantify this increase and the results, relative to the mean±s.e. of three different adenoma samples, are reported in Figure 5b. Equally, pit-1, a gene encoding a transcriptional factor that has been shown to be critical for pituitary-specific activation of the GH and PRL genes, was expressed at high levels in pituitary adenomas, whereas its expression was not detectable at all in normal pituitary gland (Figure 5a, right panel).
(a) RT–PCR showing the expression of PRL, GH and Pit-1 in HMGA2-induced pituitary adenomas and in pituitary from control mice. The cDNAs were co-amplified with β-actin as an internal control. (b) The differences of PRL and GH mRNA levels in pituitary adenomas compared to pituitary from control mice were analysed by densitometric analyses and the results were plotted as an histogram. (c) GH and PRL serum levels at different ages. TG/F=transgenic females; WT/F=wild type females; TG/M=transgenic males; WT/M=wild type males
PRL and GH circulating levels in HMGA2 and control mice at different ages were analysed by a radioimmunological assay. As shown in Figure 5c, both PRL and GH serum levels start to increase significantly, compared to control mice, at 6 months of age in transgenic females and at 18 months in transgenic males.
Other pathological findings in HMGA2 mice
The postmortem examination of 39 female and 28 male HMGA2 transgenic mice, sacrificed at 12 months of age, revealed pathological lesions other than the pituitary adenomas, with a generalized predisposition to tumour development. These results are summarized in Table 1. The majority of the HMGA2 mice showed large lactating mammary glands (Figure 6b) with the sporadic appearance of breast carcinomas (Figure 6d). The high secretion levels of PRL obviously account for this finding (Spady et al., 1999). In fact, it was not observed in transgenic mice with no pituitary adenomas. Another very frequent feature of these mice is the appearance of micropolycystic kidneys. As shown in Figure 6c, the kidney appears with multiple small cysts. This would suggest a certain role of the HMGA2 protein in kidney development. As described with the phenotype for mice carrying a truncated HMGA2 gene (Battista et al., 1999), HMGA2 mice also show abdominal/pelvic lipomatosis. However, this phenotype is less penetrant (20%) and the presence of fat tissue depots appears less abundant in these mice compared with the HMGA2/T mice (data not shown).
Other pathological findings in HMGA2 mice. (a) H and E staining of a mammary gland from a female control mouse: three normal alveolar ducts are shown among several adipocytic cells. (b) H and E staining of a mammary gland from a representative HMGA2 female mouse: an abnormally enlarged alveolar duct is shown with epithelial hyperproliferation and abundant lactating secretum in each cell. (c) H and E staining of kidney parenchyma from a representative HMGA2 mouse: multiple small cysts are shown. (d) MRI imagine of a HMGA2 female mouse: a mammary tumour (mt) is evident
Discussion
To define the role of HMGA2 overexpression in the process of tumorigenesis, we generated transgenic mice carrying the wild type HMGA2 gene under the transcriptional control of a strong promoter, such as that of cytomegalovirus, able to drive a significant and ubiquitous HMGA2 gene expression in adult tissues. Here we report the characterization of the most frequent pathological phenotype developed by these mice: a mixed growth hormone cell/prolactin cell pituitary adenoma. The pituitary adenomas show the presence of three cell types: one producing PRL hormone, one producing GH hormone and one producing both the above hormones, suggesting a polyclonal origin of this neoplasia. However, we cannot exclude completely the possibility of a hyperplastic growth of cells able to differentiate along these three histotypes. Interestingly, all the adenomas express high levels of Pit-1, which is a pituitary specific embryonic transcription factor constantly overexpressed in human pituitary adenomas secreting prolactin, growth hormone and/or TSH (Pellegrini-Bouiller et al., 1997). It can be speculated that HMGA2 leads to hyperplasia of cells expressing Pit-1 or alternatively that the abnormal growth of the embryonic cells secreting GH and PRL may induce Pit-1 expression.
The pituitary adenoma phenotype showed a high incidence in females, since it was present in 85% of the analysed mice. Conversely, only 40% of the males developed the same phenotype. The different hormonal background predisposing to this kind of tumour may account for these results (Spady et al., 1999). The high expression of PRL in females was responsible for mammary gland hyperplasia with lactating changes and the sporadic occurrence of breast adenocarcinomas. A high expression of PRL and GH was evidenced by the age of 6 months, although clinical symptoms appeared by the age of 12 months. These transgenic mice represent a valuable experimental model for PRL/GH secreting pituitary adenomas.
The high percentage of transgenic mice with pituitary adenomas, even though the transgene is expressed at high level in several mouse tissues other than pituitary gland, strongly indicates that the development of this neoplasia in mice overexpressing HMGA2 cannot be considered a non specific event. In fact, there is not a significant appearance of other kind of tumours, apart from large cell lymphomas in females (18%) and lung adenomas in males (25%). In addition, the development of pituitary adenomas occurs also in transgenic animals expressing either a truncated HMGA2 or a full length HMGA1 transgene (M Fedele, unpublished data). These data, taken together suggest a critical role of the HMGA genes in the regulation of PRL and GH secreting pituitary cell growth.
In a previous work from our laboratory, we have demonstrated that mice carrying a truncated HMGA2 gene, deprived of its carboxy-terminal tail (HMGA2/T mice), showed a drastic weight and size increase, with the presence of abdominal/pelvic lipomatosis (Battista et al., 1999). A similar phenotype was present also in the HMGA2 mice but with smaller fat pad depots and a relatively minor incidence (20%). Several hypotheses may be taken into consideration to explain this apparent discrepancy. First, the HMGA2/T mice have been generated following an ES mediated strategy that would allow a very high expression of the transgene, whereas the HMGA2 mice have been generated by the classical technique of microinjection of the transgene in fertilized eggs. Moreover, it is possible that the truncated HMGA2 form may show an increased activity in comparison with the wild type form. However, HMGA2 mice develop some pathology, such as micropolycystic kidney, not observed in HMGA2/T mice. These findings would suggest a role of the HMGA2 gene in the development of other organs. Further studies are required to assess the role of the HMGA2 gene in these processes.
Recent studies have shown that overexpression of the HMGA2 gene results in neoplastic transformation of rat fibroblast cells (Wood et al., 2000). However, the results presented here represent the first evidence of an oncogenic role of HMGA2 overexpression in vivo. Interestingly, according to the finding of HMGA2 modifications in benign tumours, and with the low oncogenicity shown by a truncated HMGA2 construct (Fedele et al., 1998), HMGA2 overexpression is associated also in this case with benign tumours, such as the pituitary adenomas described here.
A correlation between the phenotype induced by oncogenic activation in transgenic mice and the role of the same oncogenes in human pathology has been frequently demonstrated (Hogan, 1983). Therefore, we envisage a role of HMGA2 overexpression in human pituitary adenomas. Indeed, trisomy of chromosome 12, where the HMGA2 gene is located, represents the most frequent cytogenetic alteration in human PRL-secreting pituitary adenomas (Finelli et al., 2000). FISH analysis, using a HMGA2 PAC probe, shows amplification of the HMGA2 locus associated with the induction of HMGA2 protein expression in human prolactinomas but not in other pituitary adenoma histotypes, strongly suggesting a critical role of HMGA2 overexpression in this kind of human neoplasias (Finelli et al., 2002).
Material and methods
Generation of transgenic mice
A fragment NruI–PvuII (Figure 1a) containing the CMV promoter and the murine HMGA2 cDNA was microinjected into fertilized eggs of B6C3F2 mice that were then transferred to the oviducts of pseudopregnant females (Laboratory Animal Facility, Thomas Jefferson University, Philadelphia, PA, USA). Two transgenic founder mice were obtained and crossed to C57BL/6J wild type mice to establish transgenic lines. Germline transmission of the transgene was checked by Southern blot analysis of tail DNA from F1 offspring using a CMV fragment as probe. The expression of the HMGA2 transgene was evaluated in several tissues by a semi-quantitative RT–PCR-based assay, using a construct specific primer set, as already described (Battista et al., 1999).
RNA extraction and RT–PCR analyses
Tissues from transgenic animals were rapidly dissected, frozen on dry ice and stored at −80°C. Total RNA was extracted using TRI-reagent solution (Molecular Research Center) according to the manufacturers protocol and treated with DNAse I (GenHunter Corporation). One μg of RNA was reverse transcribed according to manufacturers instructions (Perkin Elmer). The PCR amplification was performed for 25 cycles (94°C for 30 s, 55°C for 30 s and 72°C for 30 s). Primers designed to specifically amplify the transcripts of the transfected construct and the endogenous HMGA2 gene have been already described (Battista et al., 1999). The other primers used to specifically amplify mouse pituitary genes were: PRL (forward: 5′ -CTCACTACATCCATACCCTG-3′, reverse: 5′-TCCTTTGGCTTCAGGATAGG-3′); GH (forward: 5′-AGATCACTGCTTGGCAATGG-3′, reverse: 5′-GAAAACAGACTGGACAAGGG-3′); Pit-1 (forward: 5′-CATTACTCTGTGCCTTCCTG-3′, reverse: 5′-CTCAGTTCTCGGATTTCTG-3′). In addition, a set of primers specific for mouse β-actin (forward: 5′-GTCAGAAGGACTCCTATGTG-3′, reverse: 5′-GCTCGTTGCCAATAGTGATG-3′) was added to each reaction to serve as internal control for the amount of cDNA tested. Amplification of RNA which was not reverse transcribed before PCR amplification was performed as well (data not shown). The PCR products were separated on 2% agarose gels, blotted and hybridized with specific probes.
MR imaging, histologic analysis, immunohistochemistry and electron microscopy
Magnetic Resonance Imaging was performed on a 1.5-T magnet system (GE medical System) using local receiver coils and an 8-cm field of view. Sagittal slices 3 mm thick were obtained with T1-weighting (TR/TE=400/11 ms). For light microscopy, tissues were fixed by immersion in 10% formalin and embedded in paraffin by standard procedures. Five μm sections were stained with hematoxylin and eosin (H and E) or processed for the Immunohistochemistry. The immunoperoxidase staining was performed using the avidinbiotin-peroxidase LSAB+kit (Dako) utilizing microwave antigen retrieval. The antisera used were directed to: HMGA2 (1 : 200); (Chiappetta et al., 1995), growth hormone (1 : 16 000) and prolactin (1 : 32 000). Growth hormone and prolactin antibodies were furnished by Dr AF Parlow, Scientific Director of the National Hormone and Pituitary Program. For Electron Microscopy, tissues were processed by standard procedures as previously described (Tsokos et al., 1987).
In situ double immunofluorescence
Five μm thick sections were placed on ProbeOn slides (Fisher Biotech) and stained with anti-prolactin antisera (rabbit anti-mouse, 1 : 50) and anti-growth hormone antisera (guinea pig anti-mouse, 1 : 10) utilizing microwave antigen retrieval. Secondary antibodies included FITC conjugated anti-rabbit (1 : 100), and Texas Red conjugated anti-guinea pig (1 : 50) antisera.
Serum hormone measurements
Serum PRL and GH concentration was measured using mouse PRL and GH RIAs consisting of reagents provided by Dr AF Parlow. In terms of Mouse PRL AFP6476C: IOD Ag=Mouse PRL AFP10777D, antiserum=Anti-mPRL AFP131078 (Rabbit), final dilution=1 : 500 000, BO/T=36.0% and 37.1%. In terms of Mouse GH AFP10783B: IOD Ag=mGH AFP10783B, antiserum=NIDDK-Anti-Rat GH-RIA-5 (AFP), final dilution=1 : 3 000 000, BO/T=45.9%. All hormone measurements are expressed as mean±s.e.m.
Primary cell cultures
Pituitary cell primary cultures were carried out as previously described (Weil et al., 1998). Briefly, pure tumour was placed in cold saline and washed twice in PBS (pH 7.4), which contained penicillin-streptomycin (Sigma). Tumour was minced and incubated in sterile 0.1% Trypsin (Sigma) and 0.01% Dnase (Sigma) in HBSS (Life Technologies, Inc.) at 37°C for 15 min. Cells were plated in poly-L-lysine (Sigma)-coated 16-mm plates in DMEM/F-12 (Biofluids), with 10% FCS (Life Technologies, Inc.) and pen-strep, at 37°C in 5% CO2.
Change history
09 December 2022
A Correction to this paper has been published: https://doi.org/10.1038/s41388-022-02535-z
References
Abe N, Watanabe T, Sugiyama M, Uchimura H, Chiappetta G, Fusco A, Atomi Y . 1999 Cancer Res. 59: 1169–1174
Abe N, Watanabe T, Masaki T, Mori T, Sugiyama M, Uchimura H, Fujioka Y, Chiappetta G, Fusco A, Atomi Y . 2000 Cancer Res. 60: 3117–3122
Anand A, Chada K . 2000 Nat. Genet 24: 377–380
Arlotta P, Tai AK, Manfioletti G, Clifford C, Jay G, Ono SJ . 2000 J. Biol. Chem. 275: 14394–14400
Ashar HR, Fejzo MS, Tkachenko A, Zhou X, Fletcher JA, Weremowicz S, Morton CC, Chada K . 1995 Cell 82: 57–65
Bandiera A, Bonifacio D, Manfioletti G, Mantovani F, Rustighi A, Zanconati F, Fusco A, Di Bonito L, Giancotti V . 1998 Cancer Res. 58: 426–431
Battista S, Fidanza V, Fedele M, Klein-Szanto AJP, Outwater E, Brunner H, Santoro M, Croce CM, Fusco A . 1999 Cancer Res. 59: 4793–4797
Bauer K, Carmeliet P, Schulz M, Baes M, Deuef C . 1990 Endocrinology 127: 1224–1233
Berlingieri MT, Manfioletti G, Santoro M, Bandiera A, Visconti R, Giancotti V, Fusco A . 1995 Mol. Cell. Biol. 15: 1545–1553
Bol S, Wanschura S, Thode B, Deichert U, Van de Ven WJ, Bartnitzke S, Bullerdiek J . 1996 Cancer Genet. Cytogenet. 90: 88–90
Chiappetta G, Bandiera A, Berlingieri MT, Visconti R, Manfioletti G, Battista S, Martinez-Tello FJ, Santoro M, Giancotti V, Fusco A . 1995 Oncogene 10: 1307–1314
Chiappetta G, Avantaggiato V, Visconti R, Fedele M, Battista S, Trapasso F, Merciai BM, Fidanza V, Giancotti V, Santoro M, Simeone A, Fusco A . 1996 Oncogene 13: 2439–2446
Chiappetta G, Tallini G, De Biasio MC, Manfioletti G, Martinez-Tello FJ, Pentimalli F, de Nigris F, Mastro A, Botti G, Fedele M, Berger N, Santoro M, Giancotti V, Fusco A . 1998 Cancer Res. 58: 4193–4198
Chiappetta G, Manfioletti G, Pentimalli F, Abe N, Di Bonito M, Vento MT, Giuliano A, Fedele M, Viglietto G, Santoro M, Watanabe T, Giancotti V, Fusco A . 2001 Int. J. Cancer 91: 147–151
Fedele M, Bandiera A, Chiappetta G, Battista S, Viglietto G, Manfioletti G, Casamassimi A, Santoro M, Giancotti V, Fusco A . 1996 Cancer Res. 56: 1896–1901
Fedele M, Berlingieri MT, Scala S, Chiariotti L, Viglietto G, Rippel V, Bullerdiek J, Santoro M, Fusco A . 1998 Oncogene 17: 413–418
Fedele M, Battista S, Manfioletti G, Croce CM, Giancotti V, Fusco A . 2001 Carcinogenesis 22: 1583–1591
Finelli P, Giardino D, Rizzi N, Buiatiotis S, Virduci T, Franzin A, Losa M, Larizza L . 2000 Int. J. Cancer 86: 344–350
Finelli P, Pierantoni GM, Giardino D, Losa M, Rodeschini O, Fedele M, Valtorta E, Mortini P, Croce CM, Larizza L, Fusco A . 2002 Cancer Res. in press
Giancotti V, Pani B, D'Andrea P, Berlingieri MT, Di Fiore PP, Fusco A, Vecchio G, Philp R, Crane-Robinson C, Nicolas RH, Wright CA, Goodwin GH . 1987 EMBO J. 6: 1981–1987
Hogan B . 1983 Nature 306: 313–314
Johnson KR, Lehn DA, Reeves R . 1989 Mol. Cell. Biol. 9: 2114–2123
Kazmierczak B, Wanschura S, Rosigkeit J, Mejer-Bolte K, Uschinsky K, Hanpt R, Schoenmakers EFPM, Barnitzke S, Van de Ven W, Bullerdiek J . 1995 Cancer Res. 55: 2497–2499
Nagpal S, Ghosn C, DiSepio D, Molina Y, Sutter M, Klein ES, Chandraratna RAS . 1999 J. Biol. Chem. 274: 22563–22568
Pellegrini-Bouiller I, Morange-Ramos I, Barlier A, Gunz G, Enjalbert A, Jaquet P . 1997 Horm. Res. 47: 251–258
Rogalla P, Drechsler K, Frey G, Hennig Y, Helmke B, Bonk U, Bullerdiek J . 1996 Am. J. Pathol. 149: 775–779
Rommel B, Rogalla P, Jox A, Kalle CV, Kazmierczak B, Wolf J, Bullerdiek J . 1997 26: 603–607
Schoenberg Fejzo M, Ashar HR, Krauter KS, Powell WL, Rein MS, Weremowicz S, Yoon SJ, Kucherlapati RS, Chada K, Morton CC . 1996 Genes Chrom. Cancer 17: 1–6
Schoenmakers EFPM, Wanschura S, Mols R, Bullerdiek J, Van den Berghe H, Van de Ven WJ . 1995 Nat. Genet. 10: 436–444
Spady TJ, McComb RD, Shull JD . 1999 Endocrine 11: 217–233
Staats B, Wanschura S, Hanisch P, Schoenmakers EF, Van de Ven WJ, Bartnitzke S, Bullerdiek J . 1996 Breast Cancer Res. Treat. 38: 299–303
Thanos D, Maniatis T . 1995 Cell 83: 1091–1100
Tsokos M, Scarpa S, Ross RA, Triche TJ . 1987 Am. J. Pathol. 128: 484–496
Weil RJ, Huang S, Pack S, Vortmeyer AO, Tsokos M, Lubensky IA, Oldfield EH, Zhuang Z . 1998 Cancer Res. 58: 4715–4720
Wood LJ, Maher JF, Bunton TE, Resar LM . 2000 Cancer Res. 60: 4256–4261
Zhou X, Benson KF, Ashar HR, Chada K . 1995 Nature 376: 771–774
Acknowledgements
We thank Andrea Vecchione for useful discussions about the autoptic analysis of mice, Chris Munnery for the technical expertise in performing the in situ double immunofluorescence staining and the Associazione Partenopea per le Ricerche Oncologiche (APRO) for its support. This work was supported by grants P01CA76259 and P30CA56036 from the National Cancer Institute to CM Croce and by grants from AIRC and MURST, projects ‘Terapie antineoplastiche innovative’ and ‘Piani di Potenziamento della Rete Scientifica e Tecnologica’. GM Pierantoni was supported by a fellowship from the FIRC.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Fedele, M., Battista, S., Kenyon, L. et al. Overexpression of the HMGA2 gene in transgenic mice leads to the onset of pituitary adenomas. Oncogene 21, 3190–3198 (2002). https://doi.org/10.1038/sj.onc.1205428
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.onc.1205428
Keywords
This article is cited by
-
Genomics and Epigenomics of Pituitary Tumors: What Do Pathologists Need to Know?
Endocrine Pathology (2021)
-
HMGA1-pseudogene7 transgenic mice develop B cell lymphomas
Scientific Reports (2020)
-
RPSAP52 lncRNA is overexpressed in pituitary tumors and promotes cell proliferation by acting as miRNA sponge for HMGA proteins
Journal of Molecular Medicine (2019)
-
mTOR promotes pituitary tumor development through activation of PTTG1
Oncogene (2017)
-
Oncofetal HMGA2 effectively curbs unconstrained (+) and (−) DNA supercoiling
Scientific Reports (2017)