Abstract
The present study was undertaken to compare the acute and long-term effects of escitalopram and citalopram on rat brain 5-HT neurotransmission, using electrophysiological techniques. In hippocampus, after 2 weeks of treatment with escitalopram (10 mg/kg/day, s.c.) or citalopram (20 mg/kg/day, s.c.), the administration of the selective 5-HT1A receptor antagonist WAY-100,635 (20–100 μg/kg, i.v.) dose-dependently induced a similar increase in the firing activity of dorsal hippocampus CA3 pyramidal neurons, thus revealing direct functional evidence of an enhanced tonic activation of postsynaptic 5-HT1A receptors. In dorsal raphe nucleus, escitalopram was four times more potent than citalopram in suppressing the firing activity of presumed 5-HT neurons (ED50=58 and 254 μg/kg, i.v., respectively). Interestingly, the suppressant effect of escitalopram (100 μg/kg, i.v.) was significantly prevented, but not reversed by R-citalopram (250 μg/kg, i.v.). Sustained administration of escitalopram and citalopram significantly decreased the spontaneous firing activity of presumed 5-HT neurons. This firing activity returned to control rate after 2 weeks in rats treated with escitalopram, but only after 3 weeks using citalopram, and was associated with a desensitization of somatodendritic 5-HT1A autoreceptors. These results suggest that the time course of the gradual return of presumed 5-HT neuronal firing activity, which was reported to account for the delayed effect of SSRI on 5-HT transmission, is congruent with the earlier onset of action of escitalopram vs citalopram in validated animal models of depression and anxiety.
Similar content being viewed by others
INTRODUCTION
Although the physiopathology of major depression is not fully defined, a growing body of evidence implicates the serotonin (5-HT) system as a possible therapeutic target of antidepressant treatments (Heninger and Charney, 1987; Price et al, 1990; Van Praag et al, 1990; Maes and Meltzer, 1995; Blier and de Montigny, 1998). Indeed, clinical evidence indicates that reduction of brain 5-HT levels, induced by a dietary depletion of L-tryptophan, can reverse the antidepressant action of selective 5-HT reuptake inhibitors (SSRI), monoamine oxidase inhibitors (MAOIs), and the α2-adrenoceptor antagonist mirtazapine (Bremner et al, 1997; Nishizawa et al, 1997; Moreno et al, 2000). Preclinical studies show that antidepressant treatments increase 5-HT neurotransmission with a time course that is consistent with their delayed therapeutic effect. This enhancement would, however, be mediated via different mechanisms. Long-term administration of either MAOIs or SSRIs results in a desensitization of the somatodendritic 5-HT1A autoreceptor of 5-HT neurons in the dorsal raphe nucleus (DRN), thereby allowing their firing rate to recover in the presence of the drugs (Blier et al, 1986; Chaput et al, 1986). In addition, long-term SSRI treatment also desensitizes terminal 5-HT1B/1D autoreceptors (Blier and Bouchard, 1994; Briley and Moret, 2000). Long-term treatment with the antidepressant mirtazapine increases 5-HT neurotransmission, as a result of a sustained increase in the firing activity of 5-HT neurons in the presence of decreased function of α2-adrenergic heteroreceptors located on 5-HT terminals (Haddjeri et al, 1997). Finally, long-term treatment with 5-HT1A receptor agonists, such as gepirone (Feiger et al, 2003), desensitizes the 5-HT1A autoreceptors on soma but not the postsynaptic 5-HT1A receptors located on CA3 pyramidal neurons (Blier and de Montigny, 1987; Schechter et al, 1990; Dong et al, 1998). Together, these indicate that adaptive changes in the 5-HT system may play a pivotal role in the therapeutic effect of antidepressant treatments.
Clinical and preclinical studies have shown that the citalopram effects on 5-HT reuptake inhibition and its antidepressant activity resides in the S-enantiomer (Hyttel et al, 1992; Montgomery et al, 2001; Burke et al, 2002; Wade et al, 2002; Lepola et al, 2004). In addition, using a variety of behavioral paradigms for depression/anxiety, it has been shown that escitalopram showed a more rapid and efficacious effect than citalopram, and that R-citalopram counteracted these effects in vivo and in vitro (Mørk et al, 2003; Sánchez et al, 2003a, 2003b; Sánchez and Kreilgaard, 2004).
The present study was undertaken to determine and compare whether acute and sustained administration of citalopram and its enantiomer escitalopram in rats, modified the firing activity of dorsal raphe presumed 5-HT neurons, the responsiveness of auto- (pre-) and postsynaptic 5-HT1A receptors, and overall 5-HT neurotransmission in the hippocampus. Parts of this work were previously published in abstract form (El Mansari et al, 2004).
MATERIALS AND METHODS
The experiments were carried out in male Sprague–Dawley rats (IFFA CREDO, L’Abresle, France) weighing 250–300 g at the day of the recording. They were kept under standard laboratory conditions (12:12 h light–dark cycle with free access to food and water). In the sustained administration experiments, groups of rats were treated with escitalopram (10 mg/kg/day) or citalopram (20 mg/kg/day) for 7, 14, and 21 days delivered subcutaneously (s.c.) with osmotic minipumps (Charles Rivers, France). Control rats received a minipump containing vehicle (NaCl 0.9%). The rats were tested with the minipumps in place. The animals were anesthetized with chloral hydrate (400 mg/kg, i.p.). Supplemental doses were given to maintain constant anesthesia and to prevent any nociceptive reaction to a tail pinch.
Experiments were performed in accordance with the European Communities Council Directives 86/609, OJ L 358,1, Dec 12, 1987, for the care and use of laboratory animals. All experiments were performed with the approval of the Regional Animal Care Committee (Faculty of Medicine, Claude Bernard University-Lyon 1), and complied with rules set forth in the National Institutes of Health Guide for the Care and Use of Laboratory Animals (publication 80-23).
Treatments
Two different lengths of treatment were used, one was short-term and the other was long-term treatment. On the one hand, in order to detect as early as possible changes in the sensitivity of 5-HT1A autoreceptors and a return to baseline activity of DRN neurons, recordings were made after 7, 14, and 21 days of treatments. On the other, as the 5-HT1A receptors in hippocampus adapt differently (see Blier and de Montigny, 1994 for a review), we aimed at recording the change in the sensitivity of these receptors following the putative return to normal discharge of DRN 5-HT neurons, that is, 14 days of treatment. In total, 10 mg/kg/day of escitalopram and 20 mg/kg/day of citalopram were used because they were shown to maximally increase extracellular 5-HT in the prefrontal cortex (see Ceglia et al, 2004).
Extracellular Unitary Recordings of Dorsal Raphe 5-HT Neurons
Extracellular recordings were performed with single-barreled glass micropipettes preloaded with fiberglass filaments in order to facilitate filling. The tip was broken back to 2–4 μm and filled with a 2 M NaCl solution saturated with Pontamine Sky Blue to stain the location of the last recording. The rats were placed in a stereotaxic frame and a burr hole was drilled on the midline, 1 mm anterior to lambda. Presumed DRN 5-HT neurons were encountered over a distance of 1 mm starting immediately below the ventral border of the Sylvius aqueduct. These neurons were identified using the criteria of Aghajanian (1978): a slow (0.5–2.5 Hz) and regular firing rate and long-duration (0.8–1.2 ms) positive action potentials; they were also verified to be located in DRN. For the acute studies, a dose–response curve of the suppressant effects on neuronal 5-HT firing of escitalopram and citalopram was constructed. To this end, in each rat only one neuron was studied with SSRIs and a dose of WAY 100635 (N-{2-[4(2-methoxyphenyl)-1-piperazinyl]ethyl}-N-(2-pyridinyl)cyclohexanecarboxamide trihydrochloride; 50–100 μg/kg, i.v.) was used to reverse the suppressant effect of both escitalopram and citalopram on the firing activity of DRN 5-HT neurons. To determine a putative interaction between the enantiomers of citalopram on the firing activity of 5-HT neurons, a dose of 250 μg/kg (i.v.) of R-citalopram was injected prior to escitalopram (100 μg/kg, i.v.=ED100). For the chronic studies, in order to determine the possible changes of the spontaneous firing activity of dorsal raphe 5-HT neurons, four to five electrode descents were carried out through this nucleus, in rats with minipumps in place. Finally, the sensitivity of 5-HT1A receptors was evaluated by using the 5-HT1A receptor agonist (±) 8-OH-DPAT (8-hydroxy-2-(di-n-propylamino)tetralin; ED100=5 μg/kg, i.v.).
Recordings from Dorsal Hippocampus CA3 Pyramidal Neurons
Recording and microiontophoresis were performed with five-barreled glass micropipettes broken back to 8–12 μm under microscopic control. The central barrel was filled with a 2 M NaCl solution and used for extracellular unitary recordings. The pyramidal neurons were identified by their large amplitude (0.5–1.2 mV) and long-duration (0.8–1.2 ms) simple spikes alternating with complex spike discharges (Kandel and Spencer, 1961). The side barrels contained the following solutions: 5-HT creatinine sulfate (2 mM in 200 mM NaCl, pH 4), quisqualate (1.5 mM in 200 mM NaCl, pH 8), and 2 M NaCl used for automatic current balancing. The rats were mounted in a stereotaxic apparatus and the microelectrodes were lowered at 4.2 mm lateral and 4.2 mm anterior to lambda into the CA3 region of the dorsal hippocampus. Since most hippocampus pyramidal neurons are not spontaneously active under chloral hydrate anesthesia, a leak or a small ejection current of quisqualate (+2 to −8 nA) was used to activate them within their physiological firing range (10–15 Hz; Ranck, 1975). A 10 or 20 nA ejection current of 5-HT was used, each ejection period lasting 50 s. To assess the effectiveness of the long-term treatment with citalopram and escitalopram, the recovery time 50 (RT50) method was used. The RT50 value has been shown to be a reliable index of the in vivo activity of the 5-HT reuptake process in the rat hippocampus. This value is obtained by calculating the time in seconds required for the neuron to recover 50% of its initial firing rate at the end of the microiontophoretic application of 5-HT onto CA3 pyramidal neuron. Thus, the blockade of the 5-HT transporter by an SSRI reveals a greater RT50 value than in controls (Piñeyro et al, 1994). The neuronal responsiveness to 5-HT was assessed using the IT50 method. It is the product of the current (in nA) used to eject 5-HT from the micropipette and the time (in seconds) required to obtain a 50% decrease from baseline of the firing rate of the recorded neuron. The more sensitive a neuron is to 5-HT, the smaller will be the IT50 value because the number of molecules ejected is proportional to the amount of coulombs (de Montigny and Aghajanian, 1978).
In order to assess the degree of activation of the postsynaptic 5-HT1A receptors exerting an inhibitory influence on the firing activity of CA3 pyramidal neurons, WAY 100,635 was administered intravenously to disinhibit the hippocampal neurons resulting in an increase of their firing activity. The disinhibition would be best determined if the neurons were not firing at a high rate; therefore, their firing rate was decreased to about 10–20 Hz by reducing the ejection current of quisqualate and the selective 5-HT1A receptor antagonist WAY 100,635 (20–100 μg/kg) was injected intravenously afterward (Haddjeri et al, 1998a; Besson et al, 2000). It is well established that the suppression of the firing activity of CA3 pyramidal neurons by microiontophoretic applied 5-HT is mediated through the activation of 5-HT1A receptors (de Montigny et al, 1984). If a tonic activation of postsynaptic 5-HT1A receptors exits, the firing activity of hippocampus CA3 pyramidal neurons will be lowered even though the responsiveness of these receptors to 5-HT is unchanged. Then the blockade of these receptors by WAY 100,635 will disinhibit the CA3 pyramidal neurons resulting in an increase of their firing activity (for more details see Haddjeri et al, 1998a). An intravenous injection of saline preceded the first injection of WAY 100,635 to eliminate any effect due to the injection by itself. The saline injection corresponds to the 0 mg/kg dose. WAY 100,635 was administered in incremental doses of 20 μg/kg at time intervals of 2 min. To avoid residual drug effects, only one cell was studied in each rat. The change of firing activity was assessed by calculating the mean firing rate of neurons from about 1–2 min prior to and after (until a ‘plateau’) the i.v. administration of the drugs and the percent of change was calculated.
Statistical Analyses
Statistical analysis was performed with SigmaStat for Window version 4.0 software (Jandel Corporation). Average are shown as the mean±SEM. Significance is considered for *P<0.05 and **P<0.01. A two-way analysis of variance (ANOVA) was performed on the firing rates on dorsal raphe 5-HT neurons in escitalopram and citalopram and control rats after 7-, 14-, or 21-days treatment. A Student's t-test or a one-way ANOVA was performed on the effects of 8-OH-DPAT, R-citalopram, and escitalopram on dorsal raphe 5-HT neuronal firing activity. One- and two-way repeated measures ANOVA were used to determine the effects of the different treatments on the firing rate of dorsal hippocampus CA3 pyramidal neurons when repeated doses of WAY 100,635 were given. Correlation coefficients (r-values) for the dose–response relationship observed in the dorsal raphe were calculated using simple linear/curvilinear regression analysis. Differences between the two regressions were assessed by comparing the ED50 values using the 95% confidence interval method.
RESULTS
Effects of Acute and Sustained Administration of Escitalopram and Citalopram on the Firing Activity of Dorsal Raphe 5-HT Neurons
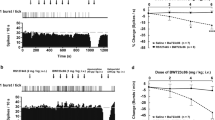
All dorsal raphe 5-HT neurons tested in the present study were inhibited, in a dose-dependent manner, by escitalopram and citalopram. As illustrated in Figure 1, escitalopram was more potent than citalopram in suppressing 5-HT neuronal firing activity in the DRN. In fact, the ED50 for citalopram and escitalopram was 254 and 58 μg/kg, respectively. This inhibitory effect was reversed by the intravenous administration of WAY 100,635, a selective 5-HT1A receptors antagonist.
Integrated firing rate histograms of dorsal raphe 5-HT neurons in naive rats showing their response to escitalopram and WAY-100,635 administrations (a) and to citalopram and WAY-100,635 administrations (b). (c) Dose–response curves of the suppressant effect of escitalopram and citalopram (25–500 μg/kg, i.v.) on the firing activity of 5-HT neurons in naive rats. P<0.05 using confident limits of ED50 values. Two to three rats were used for each dose (in each rat only one neuron was tested).
As illustrated in Figure 2, R-citalopram (250 μg/kg, i.v.) by itself did not modify the firing activity of dorsal raphe 5-HT neurons. In the absence of R-citalopram, the mean firing activity of 5-HT neurons was 1.6±0.2 Hz before the administration of 100 μg/kg of escitalopram and 0 Hz after escitalopram injection (n=6). Interestingly, after R-citalopram administration, the firing rate was 1.7±0.3 Hz before and 1.1+0.3 Hz after escitalopram injection (n=6). R-citalopram prevented significantly, but did not reverse (see Figure 2a, n=4), the suppressant effect of escitalopram on the firing activity of 5-HT neurons (P<0.01 using unpaired Student's t-test, Figure 2).
Integrated firing rate histograms of dorsal raphe 5-HT neurons in naive rats showing their response to escitalopram (a) and to R-citalopram, escitalopram and WAY-100,635 (b). (c) Mean results (±SEM) of the suppressant effect of escitalopram (100 μg/kg, i.v.) on the firing activity of 5-HT neurons in naive rats after saline or R-citalopram (250 μg/kg, i.v.) injections. The numbers at the bottom of the columns indicate the number of rats tested (in each rat only one neuron was tested). *P<0.05 vehicle vs R-citalopram using unpaired Student's t-test.
In rats treated with escitalopram and citalopram for 7 days, there was a decrease of the spontaneous firing activity of dorsal raphe 5-HT neurons (by 61 and 70%, respectively, Figure 3). After 14 days of treatment with escitalopram, a significant decrease of the firing activity of 5-HT neurons was no longer present when compared to controls (11%) while there was still a significant decrease of 58% in rats treated with citalopram (Figure 3). This mean firing activity was back to control value after 21 days of treatment with citalopram (Figure 3).
Mean (±SEM) of the firing rate of dorsal raphe 5-HT neurons in control rat and rats treated with escitalopram (10 mg/kg/day, s.c.) or citalopram (20 mg/kg/day, s.c.), for 7, 14, and 21 days. Note the recovery of firing of 5-HT neurons in rats treated with escitalopram for 14 days. *P<0.05, using two-way ANOVA. The numbers at the bottom indicate the total number of neurons recorded in each group of treated rats (six to seven rats were tested per group).
The 5-HT1A receptor agonist 8-OH-DPAT was used to assess the sensitivity of somatodendritic 5-HT1A autoreceptors in rats treated with escitalopram or citalopram for 14 or 21 days. The mean spontaneous firing activity of representative 5-HT neurons tested was 1.3±0.2 Hz in controls, 1.2±0.5 Hz in rats treated with escitalopram for 2 weeks, 0.6±0.1 Hz (n=6, t=3.43, df=10, P<0.01, using unpaired student's t-test) in rats treated with citalopram for 2 weeks, and 1.2±0.3 Hz in rats treated with citalopram for 3 weeks. For all neurons tested in control rats, the i.v. administration of 8-OH-DPAT (5 μg/kg) produced a complete suppression of the firing activity of dorsal raphe 5-HT neurons (Figure 4a). The suppressant effect of 8-OH-DPAT on the firing activity of 5-HT neurons was unchanged in rats treated with citalopram for 2 weeks (20 mg/kg/day, s.c., P>0.34 using one-way ANOVA followed by PLSD Fisher's test). Interestingly, this suppressant effect of 8-OH-DPAT on the firing activity of 5-HT neurons was significantly attenuated by 46%, in rats treated with escitalopram for 2 weeks (10 mg/kg/day, s.c., P<0.03 using one-way ANOVA followed by PLSD Fisher's test), and by 73% in rats treated with citalopram for 3 weeks (20 mg/kg/day, s.c., decrease in firing activity after 8-OH-DPAT injection=27±19%, n=5, P<0.01). One-way ANOVA showed no significant difference between these two groups of treated rats.
Integrated firing rate histograms of dorsal raphe 5-HT neurons showing their response to 8-OH-DPAT and WAY-100,635 injections in a control rat (a), in rat treated with escitalopram for 14 days (b) and in rat treated with citalopram for 14 days (c). Mean results±SEM is represented in (d). The numbers at the bottom of the columns indicate the number of rats tested (in each rat only one neuron was tested). *P<0.05 using one-way ANOVA followed by PLSD Fisher's test.
Effects of Sustained Treatment with Escitalopram and Citalopram on the Dorsal Hippocampus CA3 Pyramidal Neurons Responsiveness to WAY 100,635
For all CA3 pyramidal neurons tested, 5-HT (10 or 20 nA) induced an inhibition of their firing activity (Figure 5). This suppressant effect occurred in the absence of any alteration of the shape of the action potentials. Short- or long-term treatment with escitalopram or citalopram did not modify the suppressant effect of microiontophoretically applied 5-HT on the firing activity of CA3 pyramidal neurons. In fact, such treatments failed to modify the responsiveness of CA3 pyramidal neurons to microiontophoretically applied 5-HT: the mean IT50 value for 5-HT was not significantly different in rats treated with escitalopram or citalopram for 14 days when compared to controls: IT50 value for 5-HT was 13±2 (n=9) in control rats, 16±4.5 (n=6) in rats treated citalopram for 2 weeks, and 15±2 (n=8) in rats treated with escitalopram for 2 weeks (P>0.05, using one-way ANOVA). On the other hand, the mean RT50 value for 5-HT was significantly increased in rats treated with either escitalopram or citalopram. The mean RT50 value for 5-HT increased significantly following sustained administration of escitalopram and citalopram. The RT50 value for 5-HT was 13±2 s in control rats (n=9), 40.5±10 s in rats treated with escitalopram for 2 weeks (P<0.05, using one-way ANOVA followed by Dunnett test, n=8) and 40±9 s in rats treated with citalopram for 2 weeks (P<0.05, using one-way ANOVA followed by Dunnett test, n=6).
Integrated firing rate histograms of dorsal hippocampus CA3 pyramidal neurons showing their responsiveness to the microiontophoretic application of 5-HT and i.v. injection of WAY-100,635 in a control rat (a) and a rat treated for 2 weeks with escitalopram (10 mg/kg/day, s.c. (b)). These neurons were activated with quisqualate and horizontal bars indicate the duration of the applications for which the current is given in nanoamperes. Note the increase in firing activity of CA3 pyramidal neurons after the injection of WAY-100,635. (c) Degree (%±SEM) of increase of the firing activity of CA3 pyramidal neurons in control rats and treated rats with escitalopram and citalopram for 14 days (c) prior to and after the administration of WAY-100,635 (20–100 μg/kg, i.v.). n values indicate the number of neurons tested (in each rat only one neuron was tested). **P<0.01 using one-way ANOVA followed by PLSD test of Fisher.
The effect of WAY 100,635 on the quisqualate-activated firing activity of CA3 pyramidal neurons was assessed in controls and in rats treated with escitalopram and citalopram for 14 days (Figure 5). WAY 100,635 increased slightly the quisqualate-activated firing activity of CA3 pyramidal neurons within a dose range of 20–100 μg/kg (i.v.) in control rats (Figure 5). In rats treated with either escitalopram or citalopram for 14 days, WAY 100,635 induced a large and significant increase of the mean firing activity of CA3 pyramidal neurons, when compared to control (Figure 5). This significant increase was dose-dependent at 20 and 40 μg/kg and reaching a plateau starting at dose of 60–100 μg/kg, with an overall significantly greater increase after 14-day treatment of escitalopram and citalopram administration than control (P<0.001, using one-way ANOVA followed by PLSD test of Fisher). The increase firing activity of these neurons induced by WAY 100,635 was, however, similar in rats treated with escitalopram and citalopram for 14 days (increase of 400–600%, Figure 5).
DISCUSSION
In DRN, the marked decrease of the firing activity of 5-HT neurons followed by recovery after long-term administration of escitalopram and citalopram is in agreement with previous studies using citalopram and other SSRIs (Chaput et al, 1986; Blier and de Montigny, 1994). This decrease has been previously reported to result from a greater activation of somatodendritic 5-HT1A autoreceptors (Blier and de Montigny, 1983; Blier et al, 1984; Chaput et al, 1986; Le Poul et al, 1995) due to the increased levels of extracellular 5-HT in the DRN produced by SSRIs (Bel and Artigas, 1992; Hjorth et al, 1995; Romero et al, 1996). As with other SSRIs, the inhibitory effect 8-OH-DPAT on 5-HT neurons activity was attenuated in treated rats with escitalopram for 2 weeks and citalopram for 3 weeks in the present study, confirming the desensitization of 5-HT1A receptors in DRN (see Blier and de Montigny, 1994). With autoreceptor regulation decreased, there can be a return to normal firing activity and a greater release of 5-HT per impulse, thus leading to an increased serotonergic transmission at 5-HT1A receptors. In the present study, a complete recovery of 5-HT discharge was observed after 14-day treatment with escitalopram but not with citalopram (Figure 3). If the degree of 5-HT1A receptor desensitization is proportional to recovery of the activity of 5-HT neurons, one would expect levels of 5-HT1A receptor desensitization to translate into proportional change in firing activity of 5-HT neurons. Indeed, following 2 weeks of treatment with citalopram, while around 20% of neurons discharged at control rate and had attenuated response to 8-OH-DPAT (data not shown), the majority of 5-HT neurons fired at lower rate than control and presented no desensitized 5-HT1A autoreceptor, most likely explaining the lack of firing recovery of these neurons. In this regard, using in vitro recordings in DRN, a progressive increase in the proportion of 5-HT cells with desensitized 5-HT1A autoreceptors was observed with prolonged SSRI administration (Le Poul et al, 1995). The authors suggested that rather than the degree of 5-HT1A autoreceptor desensitization per se as being the critical parameter with regard to the mean recovery of 5-HT neuronal activity, it may be the number of 5-HT cells with desensitized 5-HT1A autoreceptors that is more important.
The reason for which there was a complete recovery of firing activity of 5-HT neurons following 2-week escitalopram treatment but not with citalopram is still unknown, but may involve additional effects of these SSRIs. It is conceivable that the difference in the time constant of 5-HT firing recovery with escitalopram vs citalopram may be due to the presence of R-citalopram attenuating the effect of escitalopram on the recovery of activity of 5-HT neurons. It was reported that escitalopram mediates citalopram's in vivo 5-HT uptake inhibitory activity (Hyttel et al, 1992; Owens et al, 2001). The present study shows that the inhibitory effect of escitalopram on DRN 5-HT neurons was prevented but not reversed by the administration of R-citalopram, suggesting that for racemate citalopram, the R-citalopram could counteract the effect of escitalopram. Indeed, microdialysis studies have shown that R-citalopram attenuated the augmenting effect of escitalopram on 5-HT release in frontal and prefrontal cortex (Mørk et al, 2003; Ceglia et al, 2004). In addition, it has been shown that R-citalopram attenuates antidepressant effect of escitalopram in rat chronic mild stress model (Sánchez et al, 2003a) and prevents anxiolytic effect of escitalopram in a rat ultrasonic vocalization model (Sánchez, 2003). The mechanism by which R-citalopram prevents the effect of escitalopram on 5-HT transmission is not yet fully elucidated. A putative competitive action between R-citalopram and escitalopram on the 5-HT transporter can be envisaged. Recently, a kinetic interaction of R-citalopram and escitalopram has been suggested to be a critical factor in the antagonistic effects of R-citalopram (Stórustovu et al, 2004; for a review see Sánchez et al, 2004). Furthermore, it was shown that S-and R-enantiomers stereoselectivity differs for the primary and allosteric sites and that allosteric ligands increase the binding affinity at the primary site by inducing conformational changes (Chen et al, 2004).
In hippocampus, the assertion that the inhibitory effect of 5-HT on the firing activity of CA3 pyramidal neurons is mediated by 5-HT1A receptor subtype, is supported by the observation that the selective 5-HT1A receptor antagonist WAY 100,635 produced marked reduction of the effect of microiontophoretically applied 5-HT (Haddjeri et al, 1998a; Besson et al, 2000). The sensitivity of postsynaptic 5-HT1A receptors was not changed after 14-day treatment with escitalopram and citalopram, as demonstrated by the ability of 5-HT, when applied microiontophoretically, to inhibit the CA3 pyramidal neurons to same extent as in control rats (see IT50 values). This result is in agreement with previous studies showing that 5-HT1A receptors in the hippocampus are normosensitive in rat treated with SSRIs (Piñeyro et al, 1994; Haddjeri et al, 1998a) or in 5-HT transporter knockout mice (Mannoury la Cour et al, 2001).
Should there be a greater tonic activation of these postsynaptic 5-HT1A receptors, one would expect their blockade by WAY 100,635 to result in a greater enhancement of the baseline firing activity of CA3 pyramidal neurons (Haddjeri et al, 1998a). In the present study, systemic injection of WAY 100,635 increased the firing activity of one-third of hippocampal cells in control rats. Although this disinhibition has not been reported in previous studies (Haddjeri et al, 1998a, 1998b; Rueter et al, 1998; Besson et al, 2000, Kasamo et al (2001) have shown that WAY 100,635 administration significantly increased the firing activity of CA1 pyramidal neurons of the dorsal hippocampus in quiet awake rats. This indicates that in nontreated rats endogenous 5-HT would tonically inhibit the spontaneous firing activity of CA1 pyramidal neurons through the activation of 5-HT1A receptors. As previously shown with several classes of antidepressants, the selective monoamine oxidase-A inhibitor befloxatone (Haddjeri et al, 1998b), the dual 5-HT/noradrenaline reuptake inhibitor, duloxetine (Rueter et al, 1998), or the α2-adrenoceptor antagonist mirtazapine and the SSRI paroxetine (Besson et al, 2000), the present study shows that sustained treatment with escitalopram and citalopram induced a strong but similar enhancement of the tonic activation of the postsynaptic 5-HT1A receptors in the dorsal hippocampus. One would expect a putatively greater tonic inhibitory activation of 5-HT1A receptors on hippocampal neurons in the presence of greater amount of 5-HT in the extracellular space. In frontal cortex, a greater increase in extracellular 5-HT was observed with escitalopram than citalopram, using microdialysis method (Mørk et al, 2003). More importantly, the increase of extracellular 5-HT in prefrontal cortex was greater following 13-day compared to 2-day treatment with escitalopram, but not after citalopram treatment (Ceglia et al, 2004). However, the increase of 5-HT level was similar in rats treated for 13 days with escitalopram (10 mg/kg/day) and citalopram (20 mg/kg/day) (Ceglia et al, 2004). Although no microdialysis studies were undertaken in hippocampus following long-term administration of these two SSRIs, several other studies have shown that the net impact of different SSRIs on extracellular 5-HT could vary with brain regions, such as between the frontal cortex and hippocampus (Malagié et al, 1996; Hervas and Artigas, 1998; see for a review Hjorth et al, 2000) depending on their innervation by DRN vs median raphe nucleus, respectively. The greater efficacy of escitalopram compared to citalopram in increasing extracellular 5-HT in hippocampus, if any, does not appear to result in differential increase in tonic activation of postsynaptic 5-HT1A receptors, as was shown with other antidepressant, thus suggesting that other mechanisms are involved. On the one hand, this discrepancy could stem from the fact that citalopram may be unique in that it exerts their antidepressant action differently from other SSRIs. In norepinephrine-deficient mice, unlike paroxetine, fluoxetine, and sertraline, citalopram has been shown to partially increase 5-HT levels in the hippocampus and reduce immobility, in tail suspension test in mice, independently of norepinephrine system integrity (Cryan et al, 2004). On the other, the regulation of postsynaptic 5-HT1A receptor function in hippocampus may occur at a level distal to the receptor, such as regulation of G protein expression. Indeed, although no change or increase in 5-HT1A receptor-stimulated [35S]GTPγS binding was observed in hippocampus following treatment with fluoxetine (see Hensler, 2003 for a review), changes in hippocampal 5-HT1A receptor-mediated inhibition of adenylyl cyclase activity have been reported following a such treatment (Newman et al, 1992).
The precise regulatory mechanism by which SSRIs increase 5-HT neurotransmission is still to be determined. Although complex, the combination of several adaptive changes such as desensitization of the 5-HT1A receptors in the raphe nucleus, amygdala and hypothalamus, normosensitive 5-HT1A receptors in hippocampus and cortex, and the interplay between 5-HT soma and nerve terminal might contribute, at least in part, to the antidepressant responses of SSRIs (for a review see Hjorth et al, 2000; Hensler, 2003). Nevertheless, the results obtained from raphe dorsalis suggest that the gradual recovery of normal firing activity of DRN neurons, which was reported to underlie the delayed effect of SSRI on 5-HT neurotransmission (Blier and de Montigny, 1994), is in accordance with the earlier onset of action of escitalopram vs citalopram in animal models of depression and anxiety (Sánchez et al, 2003a, 2003b; Fish et al, 2004).
References
Aghajanian GK (1978). Feedback regulation of central monoaminergic neurons: evidence from single cell recording studies. Essays Neurochem Neuropharmacol 3: 1–32.
Bel N, Artigas F (1992). Fluvoxamine preferentially increases extracellular 5-hydroxytryptamine in the raphe nuclei: an in vivo microdialysis study. Eur J Pharmacol 229: 101–103.
Besson A, Haddjeri N, Blier P, de Montigny C (2000). Effects of the co-administration of mirtazapine and paroxetine on serotonergic neurotransmission in the rat brain. Eur Neuropsychopharmacol 10: 177–188.
Blier P, Bouchard C (1994). Modulation of 5-HT release in the guinea-pig brain following long-term administration of antidepressant drugs. Br J Pharmacol 113: 485–495.
Blier P, de Montigny C (1987). Modification of 5-HT neuron properties by sustained administration of the 5-HT1A agonist gepirone: electrophysiological studies in the rat brain. Synapse 1: 470–480.
Blier P, de Montigny C (1983). Electrophysiological investigations on the effect of repeated zimelidine administration on serotonergic neurotransmission in the rat. J Neurosci 3: 1270–1278.
Blier P, de Montigny C (1994). Current advances and trends in the treatment of depression. Trends Pharmacol Sci 15: 220–226.
Blier P, de Montigny C (1998). Possible mechanisms underlying the antidepressant and anti-obsessional compulsive disorder responses. Biol Psychiatry 44: 313–323.
Blier P, de Montigny C, Azzaro AJ (1986). Modification of serotonergic and noradrenergic neurotransmissions by repeated administration of monoamine oxidase inhibitors: electrophysiological studies in the rat central nervous system. J Pharmacol Exp Ther 237: 987–994.
Blier P, de Montigny C, Tardiff D (1984). Effects of the two antidepressant drugs mianserin and indalpine on the serotonergic system: single-cell studies in the rat. Psychopharmacology 84: 242–249.
Bremner JD, Innis RB, Salomon RM, Staib LH, Ng CK, Miller HL et al (1997). Positron emission tomography measurement of cerebral metabolic correlates of tryptophan depletion-induced depressive relapse. Arch Gen Psychiatry 54: 364–374.
Briley M, Moret C (2000). The possible role of 5-HT(1B/D) receptors in psychiatric disorders and their potential as a target for therapy. Eur J Pharmacol 404: 1–12.
Burke WJ, Gergel I, Bose A (2002). Fixed-dose trial of the single isomer SSRI escitalopram in depressed outpatients. J Clin Psychiatry 63: 331–336.
Ceglia I, Acconcia S, Fracasso C, Colovic M, Caccia S, Invernizzi RW (2004). Effects of chronic treatment with escitalopram or citalopram on extracellular 5-HT in the prefrontal cortex of rats: role of 5-HT1A receptors. Br J Pharmacol 142: 469–478.
Chaput Y, Blier P, de Montigny C (1986). In vivo electrophysiological evidence for the regulatory role of autoreceptors on serotoninergic terminals. J Neurosci 6: 2796–2801.
Chen F, Larsen MB, Neubauer HA, Sinning S, Plenge P, Sánchez C et al (2004). Characterization of two overlapping S-citalopram binding sites on the serotonin transporter. European College of Neuropsychopharmacoly, 17th ECNP Congress, Stockholm, Sweden, October, 2004, P.6.068.
Cryan JF, O’Leary OF, Jin SH, Friedland JC, Ouyang M, Hirsch BR et al (2004). Norepinephrine-deficient mice lack responses to antidepressant drugs, including selective serotonin reuptake inhibitors. Proc Natl Acad Sci USA 101: 8186–8191.
de Montigny C, Aghajanian GK (1978). Tricyclic antidepressants: long-term treatment increases responsivity of rat forebrain neurons to serotonin. Science 22: 1303–1306.
de Montigny C, Blier P, Chaput Y (1984). Electrophysiologically-identified serotonin receptors in the rat CNS. Neuropharmacology 23: 1511–1520.
Dong J, de Montigny C, Blier P (1998). Full agonistic properties of Bay X 3702 on presynaptic and postsynaptic 5-HT1A receptors: electrophysiological studies in the rat hippocampus and dorsal raphe. J Pharmacol Exp Ther 286: 1239–1247.
El Mansari M, Sánchez C, Chouvet G, Haddjeri N (2004). In vivo electrophysiological study of the effects of escitalopram on the rat serotonergic neurotransmission. Coll Int Neuropsychopharmacol 24: 213.
Feiger AD, Heiser JF, Shrivastava RK, Weiss KJ, Smith WT, Sitsen JM et al (2003). Gepirone extended-release: new evidence for efficacy in the treatment of major depressive disorder. J Clin Psychiatry 64: 243–249.
Fish EW, Faccidomo S, Gupta S, Miczek KA (2004). Anxiolytic-like effects of escitalopram, citalopram, and R-citalopram in maternally separated mouse pups. J Pharmacol Exp Ther 308: 474–480.
Haddjeri N, Blier P, de Montigny C (1997). Effects of long-term treatment with the alpha 2-adrenoceptor antagonist mirtazapine on 5-HT neurotransmission. Naunyn Schmiedeberg's Arch Pharmacol 355: 20–29.
Haddjeri N, Blier P, de Montigny C (1998a). Antidepressant treatments tonically activate forebrain 5-HT1A receptors. J Neurosci 18: 10150–10156.
Haddjeri N, De Montigny C, Curet O, Blier P (1998b). Effect of the reversible monoamine oxidase-A inhibitor befloxatone on the rat 5-hydroxytryptamine neurotransmission. Eur J Pharmacol 343: 179–192.
Heninger GR, Charney DS (1987). Mechanisms of action of antidepressant treatments: implications for the ethiology and treatment of depression disorders. In: Meltzer HY (ed) Psychopharmacology: The Third Generation of Progress. Raven Press: New York. pp 535–544.
Hensler JG (2003). Regulation of 5-HT1A receptor function in brain following agonist or antidepressant administration. Life Sci 72: 1665–1682.
Hervas I, Artigas F (1998). Effect of fluoxetine on extracellular 5-hydroxytryptamine in rat brain. Role of 5-HT autoreceptors. Eur J Pharmacol 358: 9–18.
Hjorth S, Bengtsson HG, Milano S, Lundberg JF, Sharp T (1995). Studies on the role of 5-HT1A autoreceptors and alpha 1-adrenoceptors in the inhibition of 5-HT release-I. BMY7378 and prazosin. Neuropharmacology 34: 615–620.
Hjorth S, Bengtsson HJ, Kullberg A, Carlzon D, Peilot H, Auerbach SB (2000). Serotonin autoreceptor function and antidepressant drug action. J Psychopharmacol 14: 177–185.
Hyttel J, Bøgesø KP, Perregaard J, Sánchez C (1992). The pharmacological effect of citalopram residues in the (S)-(+)-enantiomer. J Neural Transm Gen Sect 88: 157–160.
Kandel ER, Spencer WA (1961). Electrophysiology of hippocampal neurons. II. After potentials and repetitive firing. J Neurophysiol 24: 243–259.
Kasamo K, Suzuki T, Tada K, Ueda N, Matsuda E, Ishikawa K (2001). Endogenous 5-HT tonically inhibits spontaneous firing activity of dorsal hippocampus CA1 pyramidal neurons through stimulation of 5-HT1A receptors in quiet awake rats: in vivo electrophysiological evidence. Neuropsychopharmacology 24: 141–151.
Lepola UM, Wade A, Andersen HF (2004). Do equivalent doses of escitalopram and citalopram have similar efficacy? A pooled analysis of two positive placebo-controlled studies in major depressive disorder. Int Clin Psychopharmacol 19: 149–155.
Le Poul E, Laaris N, Doucet E, Laporte AM, Hamon M, Lanfumey L (1995). Early desensitization of somato-dendritic 5-HT1A autoreceptors in rats treated with fluoxetine or paroxetine. Naunyn Schmiedeberg's Arch Pharmacol 352: 141–148.
Maes M, Meltzer HY (1995). The serotonin hypothesis of major depression. In: Bloom FE, Kupfer DJ (eds). Psychopharmacology: The Fourth Generation of Progress. Raven press: New York. pp 933–944.
Malagié I, Trillat AC, Douvier E, Anmella MC, Dessalies MC, Jacquet C et al (1996). Regional differences in the effect of the combined treatment of WAY 100635 and fluoxetine: an in vivo microdialysis study. Naunyn Schmiedebergs Arch Pharmacol 354: 785–790.
Mannoury la Cour C, Boni C, Hanoun N, Lesch KP, Hamon M, Lanfumey L (2001). Functional consequences of 5-HT transporter gene disruption on 5-HT1A receptor-mediated regulation of dorsal raphe and hippocampal cell activity. J Neurosci 21: 2178–2185.
Montgomery SA, Loft H, Sánchez C, Reines EH, Papp M (2001). Escitalopram (S-enantiomer of citalopram): clinical efficacy and onset of action predicted from a rat model. Pharmacol Toxicol 88: 282–286.
Moreno FA, Henninger GR, McGahuey CA, Delgado PL (2000). Tryptophan depletion and risk of depression relapse: a prospective study of tryptophan depletion as a potential predictor of depressive episodes. Biol Psychiatry 48: 327–329.
Mørk A, Kreilgaard M, Sánchez C (2003). The R-enantiomer of citalopram counteracts escitalopram-induced increase in extracellular 5-HT in the frontal cortex of freely moving rats. Neuropharmacology 45: 167–173.
Newman ME, Shapira B, Lerer B (1992). Regulation of 5-hydroxytryptamine1A receptor function in rat hippocampus by short- and long-term administration of 5-hydroxytryptamine1A agonist and antidepressants. J Pharmacol Exp Ther 260: 16–20.
Nishizawa S, Benkelfat C, Young SN, Leyton M, Mzengeza S, de Montigny C et al (1997). Differences between males and females in rates of serotonin synthesis in human brain. Proc Natl Acad Sci USA 94: 5308–5313.
Owens MJ, Knight DL, Nemeroff CB (2001). Second-generation SSRIs: human monoamine transporter binding profile of escitalopram and R-fluoxetine. Biol Psychiatry 50: 345–350.
Piñeyro G, Blier P, Dennis T, de Montigny C (1994). Desensitization of the neuronal 5-HT carrier following its long-term blockade. J Neurosci 14: 3036–3047.
Price LH, Charney DS, Delgado PL (1990). Clinical data on the role of serotonin in the mechanism(s) of action of antidepressant drug. J Clin Psychiatry 51: 44–50.
Ranck JB (1975). Behavioral correlates and firing repertoires of neurons in the dorsal hippocampal formation and septum of unrestrained rats. In: Isaacson RL, Pribram KH (eds). The Hippocampus. Plenum: New York. pp 207–244.
Romero L, Bel N, Artigas F, de Montigny C, Blier P (1996). Effect of pindolol on the function of pre- and postsynaptic 5-HT1A receptors: in vivo micrdialysis and electrophysiological studies in the rat brain. Neuropsychopharmacology 15: 349–360.
Rueter LE, de Montigny C, Blier P (1998). Electrophysiological characterization of the effect of long-term duloxetine administration on the rat serotonergic and noradrenergic systems. J Pharmacol Exp Ther 285: 404–412.
Sánchez C (2003). R-citalopram attenuates anxiolytic effects of escitalopram in a rat ultrasonic vocalisation model. Eur J Pharmacol 464: 155–158.
Sánchez C, Bergqvist PBF, Brennum LT, Gupta S, Hogg S, Larsen AK et al (2003b). Escitalopram, the S-(+)-enantiomer of citalopram, is selective serotonin reuptake inhibitor with potent effects in animal models predictive of antidepressant and anxiolytic activities. Psychopharmacology 167: 353–362.
Sánchez C, Bøgesø KP, Ebert B, Reines EH, Braestrup C (2004). Escitalopram versus citalopram: the surprising role of the R-enantiomer. Psychopharmacology 174: 163–176.
Sánchez C, Gruca P, Papp M (2003a). R-citalopram counteracts the antidepressant-like effect of escitalopram in a rat chronic mild stress model. Behav Pharmacol 14: 465–470.
Sánchez C, Kreilgaard M (2004). R-citalopram inhibits functional and 5-HTP-evoked behavioural responses to the SSRI, escitalopram. Pharmacol Biochem Behav 77: 391–398.
Schechter LE, Balanos FJ, Gozlan G, Lanfumey L, Haj-Dahmane S, Laporte AM et al (1990). Alterations of central serotonergic and dopaminergic neurotransmission in rats chronically treated with ipsapirone: biochemical and electrophysiological studies. J Pharmacol Exp Ther 255: 1335–1347.
Stórustovu S, Sánchez C, Porzgen P, Brennum LT, Larsen AK, Pulis M et al (2004). R-citalopram functionally antagonises escitalopram in vivo and in vitro: evidence for kinetic interaction at the serotonin transporter. Br J Pharmacol 142: 172–180.
Van Praag HM, Asnis GM, Khan RS (1990). Monoamines and abnormal behaviour: a multiaminergic perspective. Br J Psychiatry 157: 723–734.
Wade A, Michael Lemming O, Bang Hedegaard K (2002). Escitalopram 10 mg/day is effective and well tolerated in a placebo-controlled study in depression in primary care. Int Clin Psychopharmacol 17: 95–102.
Acknowledgements
We thank Dr P Blier (University of Ottawa Institute of Mental Health Research, Ottawa) for helpful comments to improve the manuscript. We thank also E Duboeuf for her technical assistance. This research was supported by INSERM, University of Claude Bernard Lyon1 and a grant from Lundbeck A/S.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
El Mansari, M., Sánchez, C., Chouvet, G. et al. Effects of Acute and Long-Term Administration of Escitalopram and Citalopram on Serotonin Neurotransmission: an In Vivo Electrophysiological Study in Rat Brain. Neuropsychopharmacol 30, 1269–1277 (2005). https://doi.org/10.1038/sj.npp.1300686
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.npp.1300686
Keywords
This article is cited by
-
Cingulate dynamics track depression recovery with deep brain stimulation
Nature (2023)
-
Information capacity and robustness of encoding in the medial prefrontal cortex are modulated by the bioavailability of serotonin and the time elapsed from the cue during a reward-driven task
Scientific Reports (2021)
-
Serotonin-2B receptor antagonism increases the activity of dopamine and glutamate neurons in the presence of selective serotonin reuptake inhibition
Neuropsychopharmacology (2020)
-
In vivo electrophysiological recordings of the effects of antidepressant drugs
Experimental Brain Research (2019)
-
Effects of combined escitalopram and aripiprazole in rats: role of the 5-HT1a receptor
Psychopharmacology (2019)