Abstract
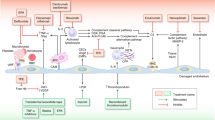
Transplantation-associated thrombotic microangiopathy (TA-TMA) is an infrequent but devastating syndrome that occurs in allogeneic hematopoietic stem cell transplant recipients, and is associated with a variety of transplantation-related factors, including conditioning regimens, immunosuppressive agents, GVHD and opportunistic infections. Progress in managing this condition has been hampered by lack of a consensus definition and poor understanding of the pathophysiology of the disorder. Two different groups recently have proposed consensus definitions, yet they fail to distinguish the primary syndrome from the secondary causes, such as a variety of infections, medication exposure or other conditions. Increasing evidence suggests that TA-TMA is a multifactorial disorder that is distinct from thrombotic thrombocytopenic purpura (TTP), and likely represents the final common pathway of a number of endothelial cell insults. TA-TMA responds poorly to conventional treatment for TTP, including plasma exchange, but newer agents, including daclizumab and defibrotide show promise. In addition, other agents known to modify endothelial responses to injury, including statins, prostacyclin analogues, endothelin-receptor antagonists and free radical scavengers, may lead to improved outcomes for patients affected by this disorder.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Powles RL, Clink HM, Spence D, Morgenstern G, Watson JG, Selby HJ et al. Cyclosporine A to prevent graft-versus-host disease in man after allogeneic bone marrow transplantation. Lancet 1980; 1: 327–329.
Laszik Z, Silva F . Hemolytic-uremic syndrome, thrombotic thrombocytopenic purpura, and systemic sclerosis (systemic scleroderma). In: Jennet JC, Olson JL, Schwartz MM, Silva FG (eds). Heptinstall's Pathology of the Kidney. Lippincott-Raven: Philadelphia, 1998, pp 1003–1057.
Sadler JE, Poncz M . Antibody-mediated thrombotic disorders: idiopathic thrombotic thrombocytopenic purpura and heparin-induced thrombocytopenia. In: Lichtman MA, Beutler E, Kipps TJ, Seligsohn U, Kaushansky K, Prchal J (eds). Williams Hematology. McGraw-Hill: New York, 2006, pp 2031–2054.
George JN, Li X, McMinn JR, Terrell DR, Vesely SK, Selby GB . Thrombotic thrombocytopenic purpura-hemolytic uremic syndrome following allogeneic hematopoietic stem cell transplantation: a diagnostic dilemma. Transfusion 2004; 44: 294–304.
Daly AS, Xenocostas A, Lipton JH . Transplantation-associated thrombotic microangiopathy: twenty-two years later. Bone Marrow Transplant 2002; 30: 709–715.
Ho VT, Cutler C, Carter S, Martin P, Adams R, Horowitz M et al. Blood and marrow transplant clinical trials network toxicity committee consensus summary: thrombotic microangiopathy after hematopoietic stem cell transplantation. Biol Blood Marrow Transplant 2005; 11: 571–575.
Ruutu T, Giovanni B, Benjamin RJ, Clark RE, George JN, Gratwohl A et al. Diagnostic criteria for hematopoietic stem cell transplant-associated microangiopathy: results of a consensus process by an international working group. Haematologica 2007; 92: 95–100.
Fuge R, Bird I, Fraser A, Hart D, Hunt L, Cornish JM et al. The clinical features, risk factors and outcome of thrombotic thrombocytopenic purpura occurring after bone marrow transplantation. Br J Haematol 2001; 113: 58–64.
Ruutu T, Hermans I, Niederwieser D, Gratwohl A, Kiehl M, Volin L et al. Thrombotic thrombocytopenic purpura after allogeneic stem cell transplantation: a survey of the European Group for Blood and Marrow Transplantation (EBMT). Br J Haematol 2002; 118: 1112–1119.
Roy V, Rizvi MA, Vesely SK, George JN . Thrombotic thrombocytopenic purpura-like syndromes following bone marrow transplantation: an analysis of associated conditions and clinical outcomes. Bone Marrow Transplant 2001; 27: 641–646.
Uderzo C, Bonanomi S, Busca A, Renoldi M, Ferrari P, Iacobelli M et al. Risk factors and severe outcome in thrombotic microangiopathy after allogeneic hematopoietic stem cell transplantation. Transplantation 2006; 82: 638–644.
Kondo M, Kojima S, Horibe K, Kato K, Matsuyama T . Hemolytic uremic syndrome after allogeneic or autologous hematopoietic stem cell transplantation for childhood malignancies. Bone Marrow Transplant 1998; 21: 281–286.
Paquette RL, Tran L, Landaw EM . Thrombotic microangiopathy following allogeneic bone marrow transplantation is associated with intensive graft-versus-host disease prophylaxis. Bone Marrow Transplant 1998; 22: 351–357.
Uderzo C, Fumagalli M, De Lorenzo P, Busca A, Vassallo E, Bonanomi S et al. Impact of thrombotic thrombocytopenic purpura on leukemic children undergoing bone marrow transplantation. Bone Marrow Transplant 2000; 26: 1005–1009.
Elliott MA, Nichols WL, Plumhoff EA, Ansell SM, Dispenzieri A, Gastineau DA et al. Posttransplantation thrombotic thrombocytopenic purpura: a single-center experience and a contemporary review. Mayo Clin Proc 2003; 78: 421–430.
Daly AS, Hasegawa WS, Lipton JH, Messner HA, Kiss TL . Transplantation-associated thrombotic microangiopathy is associated with transplantation from unrelated donors, acute graft-versus-host disease and venoocclusive disease of the liver. Transfus Apher Sci 2002; 27: 3–12.
Shimoni A, Yeshurun M, Hardan I, Avigdor A, Ben-Bassat I, Nagler A . Thrombotic microangiopathy after allogeneic stem cell transplantation in the era of reduced-intensity conditioning: the incidence is not reduced. Biol Blood Marrow Transplant 2004; 10: 484–493.
Nakamae H, Yamane T, Hasegawa T, Nakamae M, Terada Y, Hagihara K et al. Risk factor analysis for thrombotic microangiopathy after reduced-intensity or myeloablative allogeneic hematopoietic stem cell transplantation. Am J Hematol 2006; 81: 525–531.
Shulman H, Striker G, Deeg HJ, Kennedy M, Storb R, Thomas ED . Nephrotoxicity of cyclosporine A after allogeneic marrow transplantation-glomerular thromboses and tubular injury. New Engl J Med 1981; 305: 1392–1395.
Holler E, Kolb HJ, Hiller E, Mraz W, Lehmacher W, Gleixner B et al. Microangiopathy in patients on cyclosporine prophylaxis who developed acute graft versus-host disease after HLA-identical bone marrow transplantation. Blood 1989; 73: 2018–2024.
Sarkodee-Adoo C, Sotirescu D, Sensenbrenner L, Rapoport AP, Cottler-Fox M, Tricot G et al. Thrombotic microangiopathy in blood and marrow transplant patients receiving tacrolimus or cyclosporine A. Transfusion 2003; 43: 78–84.
Cutler C, Henry NL, Magee C, Li S, Kim HT, Alyea E et al. Sirolimus and thrombotic microangiopathy after allogeneic hematopoietic stem cell transplantation. Biol Blood Marrow Transplant 2005; 11: 551–557.
Couriel DR, Saliba R, Escalon MP, Hsu Y, Ghosh S, Ippoliti C et al. Sirolimus in combination with tacrolimus and corticosteroids for the treatment of resistant chronic graft-versus-host disease. Br J Haematol 2005; 130: 409–417.
Furlan M, Robles R, Solenthaler M, Wassmer M, Sandoz P, Lammle B . Deficient activity of von Willebrand factor-cleaving protease in chronic relapsing thrombotic thrombocytopenic purpura. Blood 1997; 89: 3097–3103.
Furlan M, Robles R, Galbusera M, Remuzzi G, Kyrle PA, Brenner B et al. Von Willebrand factor-cleaving protease in thrombotic thrombocytopenic purpura and the hemolytic-uremic syndrome. New Engl J Med 1998; 339: 1578–1584.
Gerritsen HE, Robles R, Lammle B, Furlan M . Partial amino acid sequence of purified von Willebrand factor-cleaving protease. Blood 2001; 98: 1654–1661.
Fujikawa K, Suzuki H, McMullen B, Chung D . Purification of human von Willebrand factor-cleaving protease and its identification as a new member of the metalloproteinase family. Blood 2001; 98: 1662–1666.
Levy GG, Nichols WC, Lian EC, Foroud T, McClintock JN, McGee BM et al. Mutations in a member of the ADAMTS gene family cause thrombotic thrombocytopenic purpura. Nature 2001; 413: 488–494.
Soejima K, Mimura N, Hirashima M, Maeda H, Hamamoto T, Nakagaki T et al. A novel human metalloprotease synthesized in the liver and secreted into the blood: possibly, the von Willebrand factor-cleaving protease? J Biochem (Tokyo) 2001; 130: 475–480.
Zheng X, Chung D, Takayama TK, Majerus EM, Sadler JE, Fujikawa K . Structure of von Willebrand factor-cleaving protease (ADAMTS13), a metalloprotease involved in thrombotic thrombocytopenic purpura. J Biol Chem 2001; 276: 41059–41063.
Tsai HM, Lian EC . Antibodies to von Willebrand factor-cleaving protease in acute thrombotic thrombocytopenic purpura. N Engl J Med 1998; 339: 1585–1594.
Sadler JE . Thrombotic thrombocytopenic purpura: a moving target. Hematology (Am Soc Hematol Educ Program) 2006, 415–420.
Sadler JE, Moake JL, Miyata T, George JN . Recent advances in thrombotic thrombocytopenic purpura. Hematology (Am Soc Hematol Educ Program) 2004, 407–423.
Bohm M, Betz C, Miesbach W, Krause M, von Auer C, Geiger H et al. The course of ADAMTS-13 activity and inhibitor titre in the treatment of thrombotic thrombocytopenic purpura with plasma exchange and vincristine. Br J Haematol 2005; 129: 644–652.
Tarr PI, Gordon CA, Chandler WL . Shiga-toxin-producing Escherichia coli and haemolytic uraemic syndrome. Lancet 2005; 365: 1073–1086.
Caprioli J, Noris M, Brioschi S, Pianetti G, Castelletti F, Bettinaglio P et al. Genetics of HUS: the impact of MCP, CFH, and IF on clinical presentation, response to treatment, and outcome. Blood 2006; 108: 1267–1279.
Vesely SK, George JN, Lammle B, Studt JD, Alberio L, El-Harake MA et al. ADAMTS13 activity in thrombotic thrombocytopenic purpura-hemolytic uremic syndrome: relation to presenting features and clinical outcomes in a prospective cohort of 142 patients. Blood 2003; 102: 60–68.
Van der Plas RM, Schiphorst M, Huizenga E . Von Willebrand factor proteolysis is deficient in classic, but not in bone marrow transplantation-associated thrombotic thrombocytopenic purpura. Blood 1999; 93: 3798–3802.
Arai S, Allan C, Streiff M, Hutchins GM, Vogelsang GB, Tsai HM . Von Willebrand-cleaving protease activity and proteolysis of von Willebrand factor in bone marrow transplant-associated thrombotic microangiopathy. Hematol J 2001; 2: 292–299.
Allford SL, Bird JM, Marks DI . Thrombotic thrombocytopenic purpura following stem cell transplantation. Leuk Lymphoma 2002; 43: 1921–1926.
Kentouche K, Zintl F, Angerhaus D, Fuchs D, Hermann J, Schneppenheim R et al. von Willebrand factor-cleaving protease (ADAMTS13) in the course of stem cell transplantation. Semin Thromb Hemost 2006; 32: 98–104.
Peyvandi F, Siboni SM, Lambertenghi Deliliers D, Lavoretano S, De Fazio N, Mornoi B et al. Prospective study on the behaviour of the metalloprotease ADAMTS13 and of von Willebrand factor after bone marrow transplantation. Br J Haematol 2006; 134: 187–195.
Laurence J, Mitra D, Steiner M, Staiano-Coico L, Jaffe E . Plasma from patients with idiopathic and human immunodeficiency virus-associated thrombotic thrombocytopenic purpura induces apoptosis in microvascular endothelial. Blood 1996; 87: 3245–3254.
Mitra D, Jaffe E, Weksler B, Hajjar KA, Soderland C, Laurence J . Thrombotic thrombocytopenic purpura and sporadic hemolytic-uremic syndrome plasmas induced apoptosis in restricted lineages of human microvascular endothelial cells. Blood 1997; 89: 1224–1234.
Dang CT, Magid M, Weksler B, Chadburn A, Laurence J . Enhanced endothelial apoptosis in splenic tissue of patients with thrombotic thrombocytopenic purpura. Blood 1999; 93: 1264–1270.
Cohen H, Bull HA, Seddon A, Enayat MS, Hill FG, Woolf N et al. Vascular endothelial cell function and ultrastructure in thrombotic microangiopathy following allogeneic bone marrow transplantation. Eur J Haematol 1989; 43: 207–214.
Testa S, Manna A, Porcellini A, Maffi F, Morstabilini G, Denti N et al. Increased plasma level of vascular endothelial glycoprotein thrombomodulin as an early indicator of endothelial damage in bone marrow transplantation. Bone Marrow Transplant 1996; 18: 383–388.
Richard S, Seigneur M, Blann A, Adams R, Renard M, Puntous M et al. Vascular endothelial lesion in patients undergoing bone marrow transplantation. Bone Marrow Transplant 1996; 18: 955–959.
Salat C, Holler E, Kolb HJ, Pihusch R, Reinhardt B, Hiller E . Endothelial cell markers in bone marrow transplant recipients with and without acute graft versus host disease. Bone Marrow Transplant 1997; 19: 909–914.
Nurnberger W, Michelmann I, Burdach S, Gobel U . Endothelial dysfunction after bone marrow transplantation: increase of soluble thrombomodulin and PAI-1 in patients with multiple transplant-related complications. Ann Hematol 1998; 76: 61–65.
Kanamori H, Maruta A, Sasaki S, Yamazaki E, Ueda S, Katoh K et al. Diagnostic value of hemostatic parameters in bone marrow transplant-associated thrombotic microangiopathy. Bone Marrow Transplant 1998; 21: 705–709.
Takatsuka H, Wakae T, Mori A, Okada M, Fujimori Y, Takemoto Y et al. Endothelial damage caused by cytomegalovirus and human herpesvirus-6. Bone Marrow Transplant 2003; 31: 475–479.
Takatsuka H, Wakae T, Mori A, Okada M, Suehiro A, Okamoto T et al. Thrombotic thrombocytopenic purpura and hemolytic uremic syndrome following allogeneic bone marrow transplantation. Bone Marrow Transplant 2002; 29: 907–911.
Qu L, Kiss JE . Thrombotic microangiopathy in transplantation and malignancy. Semin Thromb Hemost 2005; 31: 691–699.
Richardson PG, Murakami C, Jin Z, Warren D, Momtaz P, Hoppensteadt D et al. Multi-institutional use of defibrotide in 88 patients after stem cell transplantation with severe veno-occlusive disease and multisystem organ failure: response without significant toxicity in a high-risk population and factors predictive of outcome. Blood 2002; 100: 4337–4343.
Corbacioglu S, Greil J, Peters C, Wulffraat N, Laes HJ, Dilloo D et al. Defibrotide in the treatment of children with veno-occlusive disease (VOD): a retrospective multicentre study demonstrates therapeutic efficacy upon early intervention. Bone Marrow Transplant 2004; 33: 189–195.
Goon PK, Lip GY, Boos CJ, Stonelake PS, Blann AD . Circulating endothelial cells, endothelial progenitor cells, and endothelial microparticles in cancer. Neoplasia 2006; 8: 79–88.
Jimenez JJ, Jy W, Mauro LM, Horstman LL, Ahn YS . Elevated endothelial microparticles in thrombotic thrombocytopenic purpura: findings from brain and renal microvascular cell culture and patients with active disease. Br J Haematol 2001; 112: 81–90.
Morel O, Toti F, Hugel B, Bakouboula B, Camoin-Jau L, Dignat-George F et al. Procoagulant microparticles: disrupting the vascular homeostasis equation? Arterioscl Thromb Vasc Biol 2006; 26: 2594–2604.
Mallat Z, Benamer H, Hugel B, Benessiamo J, Steg PG, Freyssinet JM et al. Elevated levels of shed membrane microparticles with procoagulant potential in the peripheral circulating blood of patients with acute coronary syndromes. Circulation 2000; 101: 841–843.
Jimenez JJ, Jy W, Mauro LM, Horstman LL, Soderland C, Ahn YS . Endothelial microparticles released in thrombotic thrombocytopaenic purpura express von Willebrand factor and markers of endothelial activation. Br J Haematol 2003; 123: 896–902.
Jy W, Jimenz J, Mauro LM, Horstmann LL, Cheng P, Ahn ER et al. Endothelial microparticles induce formation of platelet aggregates via a von Willebrand factor/ristocetin dependent pathway, rendering them resistant to dissociation. J Thromb Haemost 2005; 3: 1301–1308.
Pihusch V, Rank A, Steber R, Pihusch M, Pihusch R, Toth B et al. Endothelial cell-derived microparticles in allogeneic hematopoietic stem cell recipients. Transplantation 2006; 81: 1405–1409.
Nomura S, Ishii K, Kanazawa S, Uoshima N, Ishida H, Yoshihara T et al. Significance of elevation in cell-derived microparticles after allogeneic stem cell transplantation: transient elevation of platelet-derived microparticles in TMA/TTP. Bone Marrow Transplant 2005; 36: 921–922 (letter).
Gardner G, Mesler D, Gitelman HJ . Hemolytic uremic syndrome following cisplatin, bleomycin, and vincristine chemotherapy: a report of a case and a review of the literature. Ren Fail 1989; 11: 133–137.
Hoorn CM, Wagner JG, Petry TW, Roth RA . Toxicity of mitomycin C toward cultured pulmonary artery endothelium. Toxicol Appl Pharmacol 1995; 130: 87–94.
Kohn S, Fradis M, Podoshin L, Ben-David J, Zidan J, Robinson E . Endothelial injury of capillaries in the stria vascularis of guinea pigs treated with cisplatin and gentamicin. Ultrastruct Pathol 1997; 21: 289–299.
Nagaya S, Wada H, Oka K, Tanigawa M, Tamaki S, Tsuzi K et al. Hemostatic abnormalities and increased vascular endothelial cell markers in patients with red cell fragmentation syndrome induced by mitomycin C. Am J Hematol 1995; 50: 237–243.
Oner AF, Gurgey A, Kirazli S, Okur H, Tunc B . Changes of hemostatic factors in children with acute lymphoblastic leukemia receiving combined chemotherapy including high dose methylprednisolone and L-asparaginase. Leuk Lymphoma 1999; 33: 361–364.
Chow AY, Chin C, Dahl G, Rosenthal DN . Anthracyclines cause endothelial injury in pediatric cancer patients: a pilot study. J Clin Oncol 2006; 24: 925–928.
Fajardo LF . The pathology of ionizing radiation as defined by morphologic patterns. Acta Oncol 2005; 44: 13–22.
Matsuda Y, Hara J, Miyoshi H, Osugi Y, Fujisaki H, Takai K et al. Thrombotic microangiopathy associated with reactivation of human herpesvirus-6 following high-dose chemotherapy with autologous bone marrow transplantation in young children. Bone Marrow Transplant 1999; 24: 919–923.
Grigg A, Clouston D . Disseminated fungal infection and early onset microangiopathy after allogeneic bone marrow transplantation. Bone Marrow Transplant 1995; 15: 795–797.
Biedermann BC, Sahner S, Gregor M, Tsakiris DA, Jeanneret C, Pober JS et al. Endothelial injury mediated by cytotoxic T lymphocytes and loss of microvessels in chronic graft versus host disease. Lancet 2002; 359: 2078–2083.
Martinez MT, Bucher CH, Stussi G, Heim D, Buser A, Tsakiris DA et al. Transplant-associated microangiopathy (TAM) in recipients of allogeneic hematopoietic stem cell transplants. Bone Marrow Transplant 2005; 36: 993–1000.
Rosenthal RA, Chukwuogo NA, Ocasio VH, Kahng KU . Cyclosporine inhibits endothelial cell prostacyclin production. J Surg Res 1989; 46: 593–596.
Voss BL, Hamilton KK, Samara EN, McKee PA . Cyclosporine suppression of endothelial prostacyclin generation: a possible mechanism for nephrotoxicity. Transplantation 1988; 45: 793–796.
Lau DC, Wong KL, Hwang WS . Cyclosporine toxicity on cultured rat microvascular endothelial cells. Kidney Int 1989; 35: 604–613.
Benigni A, Morigi M, Perico N, Zoja C, Amuchastegui CS, Piccinelli A et al. The acute effect of FK506 and cyclosporine on endothelial cell function and renal vascular resistance. Transplantation 1992; 54: 775–780.
Nitta K, Uchida K, Tsutsui T, Horita S, Hayashi T, Ozu H et al. Cyclosporin A induces glomerular endothelial cell injury in vitro. Acta Pathol Jpn 1993; 43: 367–371.
Azizian M, Ramenaden ER, Shah G, Wilasrusmee C, Bruch D, Kittur DS . Augmentation of ischemia/reperfusion injury to endothelial cells by cyclosporine A. Am Surg 2004; 70: 438–442.
Nacar A, Kiyici H, Ogus E, Zagyapan R, Demirhan B, Ozdemir H et al. Ultrastructural examination of glomerular and tubular changes in renal allografts with cyclosporine toxicity. Ren Fail 2006; 28: 543–547.
Burke GW, Ciancio G, Cirocco R, Markou M, Olson L, Contreras N et al. Microangiopathy in kidney and simultaneous pancreas/kidney recipients treated with tacrolimus: evidence of endothelin and cytokine involvement. Transplantation 1999; 68: 1336–1342.
Fortin MC, Raymond MA, Madore F, Fugere JA, Paquet M, St-Louis G et al. Increased risk of thrombotic microangiopathy in patients receiving a cyclosporine-sirolimus combination. Am J Transplant 2004; 4: 946–952.
Togitani K, Takeyama K, Yokozawa T, Andoh M, Narabayashi M, Kobayashi Y et al. Thrombotic microangiopathy of hyperacute onset after autologous peripheral blood stem cell transplantation in malignant lymphoma. Bone Marrow Transplant 1998; 21: 1263–1266.
Iacopino P, Pucci G, Arcese W, Bosi A, Falda M, Locatelli F et al. Severe thrombotic microangiopathy: an infrequent complication of bone marrow transplantation. Gruppo Italiano Trapianto Midollo Osseo (GITMO). Bone Marrow Transplant 1999; 24: 47–51.
Furlong T, Storb R, Anasetti C, Appelbaum FR, Deeg HJ, Doney K et al. Clinical outcome after conversion to FK 506 (tacrolimus) therapy for acute graft-versus-host disease resistant to cyclosporine or for cyclosporine-associated toxicities. Bone Marrow Transplant 2000; 26: 985–991.
Rock G, Shumak KH, Sutton DM, Busdkard NA, Nair RC . Cryosupernatant as replacement fluid for plasma exchange in thrombotic thrombocytopenic purpura. Members of the Canadian Apheresis Group. Br J Haematol 1996; 94: 383–386.
Rizvi MA, Vesely SK, George JN, Chandler L, Duvall D, Smith JW et al. Complications of plasma exchange in 71 consecutive patients treated for clinically suspected thrombotic thrombocytopenic purpura-hemolytic-uremic syndrome. Transfusion 2000; 40: 896–901.
McMinn JR, Thomas IA, Terrell DR, Duvall D, Vesely SK, George JN . Complications of plasma exchange in thrombotic thrombocytopenic purpura-hemolytic uremic syndrome: a study of 78 additional patients. Transfusion 2003; 43: 415–416 (letter).
Howard MA, Williams LA, Terrell DR, Duvall D, Vesely SK, Georgre JN . Complications of plasma exchange in patients treated for clinically suspected thrombotic thrombocytopenic purpura-hemolytic uremic syndrome. Transfusion 2006; 46: 154–156 (letter).
Zeigler ZR, Shadduck RK, Nath R, Andrews III DF . Pilot study of combined cryosupernatant and protein A immunoadsorption exchange in the treatment of grade 3-4 bone marrow transplant-associated thrombotic microangiopathy. Bone Marrow Transplant 1996; 17: 81–86.
Dua A, Zeigler ZR, Shadduck RK, Nath R, Andrews III DF, Agha M . Apheresis in grade 4 bone marrow transplant associated thrombotic microangiopathy: a case series. J Clin Apheresis 1996; 11: 176–184.
George JN, Selby GB . Thrombotic microangiopathy after allogeneic bone marrow transplantation: a pathologic abnormality associated with diverse clinical syndromes. Bone Marrow Transplant 2004; 33: 1073–1074.
Wolff D, Wilhelm S, Hahn J, Gentilini C, Hilgendorf I, Steiner B et al. Replacement of calcineurin inhibitors with daclizumab in patients with transplantation-associated microangiopathy or renal insufficiency associated with graft-versus-host disease. Bone Marrow Transplant 2006; 38: 445–451.
Corti P, Uderzo C, Tagliabue A, Della Volpe A, Annaloro C, Tagliaferri E et al. Defibrotide as a promising treatment for thrombotic thrombocytopenic purpura in patients undergoing bone marrow transplantation. Bone Marrow Transplant 2002; 29: 542–543 (letter).
Au WY, Ma ES, Lee TL, Ha SY, Fung AT, Lie AKW et al. Successful treatment of thrombotic microangiopathy after haematopoietic stem cell transplantation with rituximab. Br J Haematol 2007; 137: 475–478.
Takatsuka H, Takemoto Y, Iwata N, Suehiro A, Hamano T, Okamoto T et al. Oral eicosapentaenoic acid for complications of bone marrow transplantation. Bone Marrow Transplant 2001; 28: 769–774.
Kajiume T, Nagita A, Yoshimi S, Kobayashi K, Kataoka N . A case of hemolytic-uremic syndrome improved with nitric oxide. Bone Marrow Transplant 2000; 25: 109–110.
Schroder H . Defibrotide protects endothelial cells, but not L929 tumour cells, from tumour necrosis factor-α-mediated cytotoxicity. J Pharm Pharmocol 1995; 47: 250–252.
Kobbe G, Schneider P, Rohr U, Fenk R, Neumann F, Aivado M et al. Treatment of severe steroid refractory acute graft-versus-host disease with infliximab, a chimeric human/mouse anti-TNFalpha antibody. Bone Marrow Transplant 2001; 28: 47–49.
Couriel D, Saliba R, Hicks K, Ippoliti C, de Lima M, Hosing C et al. Tumor necrosis factor-α blockade for the treatment of acute GVHD. Blood 2004; 104: 649–654.
Patriarca F, Sperotto A, Damiani D, Morreale G, Bonifazi F, Olivieri A et al. Infliximab treatment for steroid refractory acute graft versus host disease. Haematologica 2004; 89: 1352–1359.
Uberti JP, Ayash L, Ratanatharathorn V, Silver S, Reynolds C, Becker M et al. Pilot trial on the use of etanercept and methylprednisolone as primary treatment for acute graft-versus-host disease. Biol Blood Marrow Transplant 2005; 11: 680–687.
Kennedy GA, Butler J, Western R . Combination antithymocyte globulin and soluble TNFalpha inhibitor (etanercept) +/− mycophenolate mofetil for treatment of steroid refractory acute graft-versus-host disease. Bone Marrow Transplant 2006; 37: 1143–1147.
Busca A, Locatelli F, Marmont F, Ceretto C, Falda M . Recombinant human soluble tumor necrosis factor receptor fusion protein as treatment for steroid refractory graft-versus-host disease following allogeneic hematopoietic stem cell transplantation. Am J Hematol 2007; 82: 45–52.
Ambrosi P, Aillaud MF, Habib G, Kreitmann B, Metras D, Luccioni R et al. Fluvastatin decreases soluble thrombomodulin in cardiac transplant recipients. Thromb Haemost 2000; 84: 46–48.
Chello M, Carassiti M, Agro F, Mastroroberto P, Pugliese G, Colonna D et al. Simvastatin blunts the increase of circulating adhesion molecules after coronary artery bypass surgery with cardiopulmonary bypass. J Cardiothorac Vasc Anesth 2004; 18: 605–609.
Chello M, Goffredo C, Patti G, Candura D, Melfi R, Mastrobuoni S et al. Effects of atorvastatin on arterial endothelial function in coronary bypass surgery. Eur J Cardiothorac Surg 2005; 28: 805–810.
Patti G, Chello M, Pasceri V, Colonna D, Nusca A, Miglionico M et al. Protection from procedural myocardial injury by atorvastatin is associated with lower levels of adhesion molecules after percutaneous coronary intervention: results from the ARMYDA-CAMs (Atorvastatin for Reduction of Myocardial Damage during Angioplasty-Cell Adhesion Molecules) substudy. J Am Coll Cardiol 2006; 48: 1560–1566.
Boehme MW, Gao IK, Norden C, Lemmel EM . Decrease in circulating endothelial cell adhesion molecule and thrombomodulin levels during oral iloprost treatment in rheumatoid arthritis patients: preliminary results. Rheumatol Int 2006; 26: 340–347.
Wilasrusmee C, Ondocin P, Bruch D, Shah G, Kittur S, Wilarusmee S et al. Amelioration of cyclosporine A effect on microvasculature by endothelin inhibitor. Surgery 2003; 134: 384–389.
Bohm F, Settergren M, Gonon AT, Pernow J . The endothelin-1 receptor antagonist bosentan protects against ischaemia/reperfusion-induced endothelial dysfunction in humans. Clin Sci (Lond) 2005; 108: 357–363.
Yamshita T, Shoge M, Oda E, Yamamoto Y, Giddings JC, Kashiwagi S et al. The free-radical scavenger, edaravone, augments NO release from vascular cells and platelets after laser-induced, acute endothelial injury in vivo. Platelets 2006; 17: 201–206.
Sueishi K, Mishima K, Makino K, Itoh Y, Tsuruya K, Hirakata H et al. Protection by a radical scavenger edaravone against cisplatin-induced nephrotoxicity in rats. Eur J Pharmacol 2002; 451: 203–208.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Batts, E., Lazarus, H. Diagnosis and treatment of transplantation-associated thrombotic microangiopathy: real progress or are we still waiting?. Bone Marrow Transplant 40, 709–719 (2007). https://doi.org/10.1038/sj.bmt.1705758
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1705758
Keywords
This article is cited by
-
Early vascular toxicity after pediatric allogeneic hematopoietic stem cell transplantation
Bone Marrow Transplantation (2022)
-
Treatment outcome and efficacy of therapeutic plasma exchange for transplant-associated thrombotic microangiopathy in a large real-world cohort study
Bone Marrow Transplantation (2022)
-
Transplant-associated thrombotic microangiopathy: theoretical considerations and a practical approach to an unrefined diagnosis
Bone Marrow Transplantation (2021)
-
Secondary failure of platelet recovery in patients treated with high-dose thiotepa and busulfan followed by autologous stem cell transplantation
International Journal of Hematology (2020)
-
High mortality in hematopoietic stem cell transplant-associated thrombotic microangiopathy with and without concomitant acute graft-versus-host disease
Bone Marrow Transplantation (2019)