Abstract
Study design: Case report and review of the literature.
Objectives: To describe two patients with angiolipoma in the ventral aspect of the lumbar epidural space, to discuss the clinical, radiologic, and surgical features of these lesions, and to review previously reported cases.
Setting: Rome, Italy.
Methods: Two cases, a 60-year-old man and a 54-year-old woman presented with lumbar–sciatic pain but with no abnormal neurological signs. Investigation (CT and MRI) demonstrated lumbar tumours.
Results: Laminectomy and excision of the tumors were performed, and symptoms improved immediately.
Conclusions: Magnetic resonance imaging with suppression fat sequences allows the recognition of these lesions. The prognosis after surgical removal of spinal angiolipoma is favorable.
Similar content being viewed by others
Introduction
Spinal angiolipomas are rare benign tumors. They contain mature lipomatous elements and proliferating vessels. These tumors have been suggested as an intermediate entity of a spectrum ranging from angiomas to lipomas. Angiolipomas account for only 0.14–1.2% of all tumors of the spinal axis and 3% of extradural spinal tumors1,2,3,4. A review of the international literature since 1892 to 2002 revealed 83 cases of spinal extradural angiolipomas including our two cases.4,5,6,7,8,9
Most spinal angiolipomas are found at thoracic level and arise in the posterior extradural space.4,5,6,7,8,9 Pure lumbar localization is extremely rare. Only six cases6,7,8,9,10,11,12 of lumbar angiolipomas are reported in the literature accessible to us (Table 1). Several excellent review articles4,5,6,7,8,9 are already available. The purpose of this report is to report two exceptionally rare cases of lumbar angiolipomas localized in the ventral aspect of the epidural space and to review the pertinent literature.
Case report 1
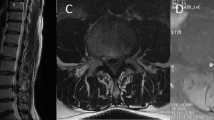
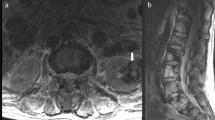
A 60-year-old man was admitted to our institution with a 2-year history of lumbosciatalgia. Neurological examination was negative. CT showed a hyperdense anterior epidural mass located at level L3–L4. The mass exhibited homogeneous contrast enhancement. MRI showed an area with signal intensity similar to that of the subcutaneous adipose tissue (Figure 1).
After performing a laminectomy, a brown, soft, well-vascularized tumor was found in the epidural space. The vertebral body presented an erosion of 1 × 0.5 cm. The lesion was dissected from the dura without difficulties and totally removed. Histology was that of angiolipoma (Figure 2). Postoperative period was uneventful and 2 years after operation the patient is asymptomatic.
Case report 2
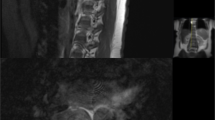
A 54-year-old woman presented with a 12-month history of lumbosciatalgia. On admission, neurological examination was negative. MRI showed an L3 anterior epidural lesion with both lipomatous and vascular components and homogeneous contrast enhancement (Figure 3). The lesion eroded into the posterior wall of the vertebral body and left pedicle. A bilateral laminectomy was performed and a mass of yellow–brown tissue was found. The lesion was located both into bone, with an erosion of 1 × 0.8 cm, and in the epidural space. The histopathological study revealed the tumor to be an angiolipoma (Figure 4). The postoperative course was uneventful. The patient is currently free of her previous symptoms.
Discussion
The first case of spinal angiolipoma was described by Berenbruch.13 Spinal angiolipomas were initially considered a hypervascular variant of spinal lipomas. In 1961, Howard and Helwig14 established angiolipoma as a clinico-pathological entity. These authors reported that the majority of these tumors are located in subcutaneous vessel, muscle, bone, and kidney.
Spinal epidural angiolipomas are quite rare and lumbar angiolipomas are extremely rare representing only 9.6% of all spinal extradural angiolipomas. These tumors occur in middle-aged women and preferentially affect the thoracic spine.9
The histopathogenesis of angiolipomas is unknown. They probably arise from abnormal primitive pluri-potential mesenchymal cells that can differentiate into lipomatous, angiomatous, or mixed tissue.15 Some authors suggested angiolipomas to be true hamartomas.15,16,17
The majority of reported spinal angiolipomas originate in the dorsal aspect of the thoracic segment and show no tendency to infiltrate the surrounding bone. According to Lin and Lin,18 angiolipomas are subdivided into two types: infiltrating and noninfiltrating. The infiltrating type is unencapsulated and contains areas in which the vascular constituent predominates. Rarely, spinal epidural angiolipomas show infiltrative behavior.7,8,10,16,19,20,21,22,23,24 Trabulo et al5 highlight that it is not clear if the infiltrative angiolipomas originate in the epidural space and infiltrate the bone, or if they originate in the bone and spread to the epidural space or if they arise in both compartments simultaneously. Infiltration of the vertebral body is often associated with anterior localization.5 In our cases of lumbar angiolipomas, the tumors were in the ventral epidural space but did not show any signs of bone infiltration. The only bone alteration observed in our cases was an erosion that contained the angiolipomas. In most cases, the time between onset of clinical symptoms and diagnosis is 1 year or less.25 Patients most commonly had long-standing pain and then developed progressive neurologic symptoms secondary to spinal cord compression. Similarly to other vascular lesions, onset or deterioration during pregnancy may occur.1,4,26 Rarely, angiolipomas may cause sudden deterioration by thrombosis, hemorrhage, or steal phenomena.4,6,16,27 The extremely unusual pure lumbar anterior localization of the lesions in our patients explains the atypical clinical presentation. In fact, both patients complained of lumbosciatalgic pain.
MRI is the imaging modality of choice in detecting angiolipomas. It must be emphasized that the true incidence of spinal angiolipomas could be greater than generally believed and MRI will likely increase the opportunities for detecting these lesions. However, neuroradiological diagnosis may be difficult, as the MRI findings of angiolipomas are easily missed. In our cases, preoperative diagnosis was suspected on the basis of simple MRI sequences and was confirmed by histologic examination. Angiolipomas appears as a hyperintense lesions on T1-weighted images.
Gadolinium enhancement is due to the vascularity of these tumors. This phenomenon allows differential diagnosis between extradural lipomatosis, which does not enhance, and spinal angiolipoma. We confirm that gadolinium infusion with fat saturation sequences are useful in the study of these lesions. This occurs because the gadolinium enhancement might be undetected being angiolipomas already hyperintense on T1 sequences. Moreover, fat suppression sequences may enhance areas of abnormal signal intensity within the fatty tumors.28
Spinal epidural angiolipomas are benign lesions and result in a good postoperative outcome, especially if affecting the lumbar level (Table 1). Surgery is the treatment of choice and in most cases of spinal angiolipomas, even if infiltrating, complete surgical removal is possible.6,9,10,11,12 Turgot,9 in an excellent review of the literature, concluded that even if infiltrating angiolipomas can be only partially resected, subtotal resection provides substantial symptomatic relief, because these lesions are slow growing and do not undergo malignant transformation. Radiotherapy has been given only in three cases reported in the literature,7,9,10,29 but there is no indication to give it for these benign lesions.
References
Haddad FS, Abla A, Allam CK . Extradural spinal angiolipoma. Surg Neurol 1986; 26: 473–486.
Miki T et al. Spinal angiolipoma: a case report. Acta Neurochir 1981; 58: 115–119.
Rubin G et al. Spinal extradural angiolipoma: case report and review of the literature. Spine 1992; 17: 719–723.
Boockvar JA et al. Subacute paraparesis induced by venous thrombosis of a spinal angiolipoma. Spine 1997; 22: 2304–2308.
Trabulo A et al. Spinal angiolipomas revisited: two case reports. Acta Neurochir (Wien) 1996; 138: 1311–1319.
Pagni CA, Canavero S . Spinal epidural angiolipoma: rare or unreported? Neurosurgery 1992; 31: 758–764.
Anson JA, Cybulski GR, Reyes M . Spinal extradural angiolipoma: a report of two cases and review of the literature. Surg Neurol 1990; 34: 173–178.
Sakaida H et al. Thoracic spinal angiomyolipoma with extracanal extension to the thoracic cavity. Spine 1997; 23: 391–394.
Turgot M . Spinal angiolipomas: report of a case and review of the cases published since the discovery of the tumor in 1890. Br J Neurosurg 1999; 13: 30–40.
Gonzalez-Crussi F, Enneking WF, Arean VM . Infiltrating angiolipoma. J Bone Joint Surg (Am) 1966; 48A: 1111–1124.
Lo Re F, Michelacci M . Considerazioni cliniche e chirurgiche su alcune malformazioni congenite vertebrali lombosacrali associate ad angiolipoma. Arch Putti Chir Organi Mov 1969; 24: 70–85.
Provenzale JM, McLendon RE . Spinal angiolipomas:main features. AJNR 1996; 17: 713–719.
Berenbruch K . Ein fall von multiplen angiolipomen kombiniert mit eniem angiom des ruckenmarks. Tubingen, 1890.
Howard WR, Helwig E . Angiolipoma. Arch Dermatol 1960; 82: 924–931.
Ehni G, Love JG . Intraspinal lipomas: report of cases; review of the literature, and clinical and pathologic study. Arch Neurol Psychiatry 1945; 53: 1–28.
von Hanwehr R, Apuzzo MLJ, Ahmadi J, Chandrasoma P . Thoracic spinal angiomyolipoma: case report and literature review. Neurosurgery 1985; 16: 406–411.
Giuffrè R . Spinal lipomas. In: Vinken PJ, Bruyn GW (eds) Handbook of Clinical Neurology, Vol 20: Part 2. Tumors of the Spine and Spinal Cord. North-Holland: Amsterdam 1976, pp 103–136.
Lin JJ, Lin F . Two entities in angiolipomas. A study of 459 cases of lipomas with review of literature on infiltrating angiolipoma. Cancer 1974; 34: 720–727.
Kuroda S, Abe H, Akino M, Yoshinobu I, Kazuo N . Infiltrating spinal angiolipoma causing myelopathy. Case report. Neurosurgery 1990; 27: 315–318.
Pearson J, Stellar S, Feigin I . Angiomyolipoma: long-term cure following a radical approach to malignant-appearing benign intraspinal tumor: report of three cases. J Neurosurg 1970; 33: 466–470.
Rivkind A, Margulies JY, Lebensart P, Sherman Y, Robin GC . Anterior approach for removal of spinal angiolipoma: a case report. Spine 1986; 11: 623–625.
Shiffer J, Giboa Y, Ariazoroff A . Epidural angiolipoma producing compression of the cauda equina. Neurochirurgia (Stuttg) 1980; 23: 117–120.
Taylor J, Harries BJ, Schurr PH . Extrathecal hemangiolipomas of the spinal canal. Br J Surg 1951; 39: 1–7.
Yamashita K, Fuji T, Nakai T, Hamada H, Kotoh K . Extradural spinal angiolipoma: report of a case studied with MRI. Surg Neurol 1993; 39: 49–52.
Preul MC, Leblanc R, Tampieri D, Robitaille Y, Pokrupa R . Spinal angiolipomas. Report of three cases. J Neurosurg 1993; 78: 280–286.
Cull DJ, Erdohazi M, Symon L . Extradural hemngiolipomas in the spinal canal: two cases presenting during pregnancy. Acta Naurochir 1978; 45: 187–193.
Padovani R, Tognetti F, Speranza S, Pozzati E . Spinal extrathecal hemangiolipomas: report of two cases and review of the literature. Neurosurgery 1982; 11: 674–677.
O'Donovan NA, Naik K, Maloney WJ, Liewellyn CG . Spinal angiolipoma mimicking extradural lipomatosis. Can Assoc Radiol J 1996; 47: 51–53.
Bucy PC, Ritchey H . Klippel–Feil's syndrome associated with compression of the spinal cord by an extradural hemangiolipoma. J Neurosurg 1947; 4: 476–481.
Author information
Authors and Affiliations
Rights and permissions
About this article
Cite this article
Rocchi, G., Caroli, E., Frati, A. et al. Lumbar spinal angiolipomas: report of two cases and review of the literature. Spinal Cord 42, 313–316 (2004). https://doi.org/10.1038/sj.sc.3101535
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.sc.3101535
Keywords
This article is cited by
-
Clinical features and surgical outcomes of spinal epidural angiolipomas
Acta Neurologica Belgica (2023)
-
Spinal extradural angiolipoma: report of two cases and review of the literature
European Spine Journal (2009)
-
Lumbar spinal angiolipoma: case report and review of the literature
European Spine Journal (2006)