Abstract
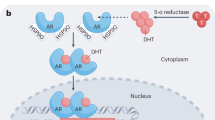
The normal prostate and early-stage prostate cancers depend on androgens for growth and survival, and androgen ablation therapy causes them to regress. Cancers that are not cured by surgery eventually become androgen independent, rendering anti-androgen therapy ineffective. But how does androgen independence arise? We predict that understanding the pathways that lead to the development of androgen-independent prostate cancer will pave the way to effective therapies for these, at present, untreatable cancers.
Key Points
-
Androgen-independent prostate cancer (AIPC) is an untreatable form of prostate cancer in which the normal dependence on androgens for growth and survival has been bypassed. AIPC is selected for by androgen ablation therapy.
-
The potential mechanisms by which AIPC develops can be divided into five categories.
-
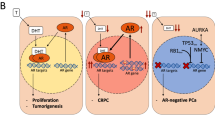
In the hypersensitive pathway, sensitivity to low circulating levels of androgen is increased by amplification of the androgen receptor (AR), mutations in the AR, increased levels of co-activators, or increased production of the potent androgen dihydrotestosterone. Tumours that use this mechanism continue to depend on both androgen and the AR.
-
By contrast, the promiscuous pathway bypasses the need for androgen (but not for AR) by broadening the specificity of the AR so that other steroid hormones — and even AR antagonists — can activate it.
-
Outlaw receptor pathways also bypass the need for androgen. In prostate cancer, outlaw receptors can be produced by crosstalk with growth factor signalling pathways, which lead to phosphorylation and activation of the AR in the absence of androgen.
-
Unlike the three pathways above, the bypass pathway is independent of AR. In this pathway, the pro-apoptotic mechanisms that are normally blocked by androgen are, instead, inhibited by a parallel mechanism such as upregulation of BCL2.
-
In the lurker cell pathway, it is proposed that malignant androgen- and AR-independent epithelial stem cells 'lurking' in the normal prostate become selected for by therapy.
-
By understanding which of these pathways is responsible for AIPC in individual patients, it might be possible to tailor therapies to each patient's needs, thereby outwitting the mechanisms that, so far, have made this disease intractable.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Greenlee, R. T., Taylor, M., Bolden, S. & Wingo, P. A. Cancer statistics: 2000. CA Cancer J. Clin. 50, 7–33 (2000).
Huggins, C. Endocrine-induced regression of cancers. Cancer Res. 27, 1925–1930 (1967).
Denmeade, S. R., Lin, X. S. & Isaacs, J. T. Role of programmed (apoptotic) cell death during the progression and therapy for prostate cancer. Prostate 28, 251–265 (1996).
Griffin, J. E. & Wilson, J. D. in Williams Testbook of Endocrinology 9th edn (eds Wilson, J. D., Foster, D. W., Kronenberg, H. M. & Larsen, P. R.) 819–876 (W. B. Saunders & Co., Philadelphia, 1998).
Quigley, C. A. et al. Androgen receptor defects: historical, clinical, and molecular perspectives. Endocr. Rev. 16, 271–321.
Brinkmann, A. O. et al. Mechanisms of androgen receptor activation and function. J. Steroid Biochem. Mol. Biol. 69, 307–313 (1999).
Nazareth, L. V. & Weigel, N. L. Activation of the human androgen receptor through a protein kinase A signaling pathway. J. Biol. Chem. 271, 19900–19907 (1996).
McKenna, N. J., Lanz, R. B. & O'Malley, B. W. Nuclear receptor coregulators: cellular and molecular biology. Endocr. Rev. 20, 321–344 (1999).
Howell, S. B. DNA microarrays for analysis of gene expression. Mol. Urol. 3, 295–300 (1999).
Ruijter, E. et al. Molecular genetics and epidemiology of prostate carcinoma. Endocr. Rev. 20, 22–45 (1999). An extensive review of the mutations found in prostate cancers.
Lee, W. H. et al. Cytidine methylation of regulatory sequences near the π-class glutathione S-transferase gene accompanies human prostatic carcinogenesis. Proc. Natl Acad. Sci. USA 91, 11733–11737 (1994).
Hyytinen, E. R. et al. Genetic changes associated with the acquisition of androgen-independent growth, tumorigenicity and metastatic potential in a prostate cancer model. Br. J. Cancer 75, 190–195 (1997).
Pilat, M. J., Kamradt, J. M. & Pienta, K. J. Hormone resistance in prostate cancer. Cancer Metastasis Rev. 17, 373–381 (1998).
Marcelli, M. et al. Androgen receptor mutations in prostate cancer. Cancer Res. 60, 944–949 (2000). Analysed a large number of prostate cancers confirming the high frequency of AR mutations in AIPC.
Koivisto, P. et al. Androgen receptor gene amplification: a possible molecular mechanism for androgen deprivation therapy failure in prostate cancer. Cancer Res. 57, 314–319.
Taplin, M. E. et al. Mutation of the androgen-receptor gene in metastatic androgen-independent prostate cancer. N. Engl. J. Med. 332, 1393–1398 (1995). Raised the possibility of frequent AR mutations in metastatic prostate cancer.
Tilley, W. D., Buchanan, G., Hickey, T. E. & Bentel, J. M. Mutations in the androgen receptor gene are associated with progression of human prostate cancer to androgen independence. Clin. Cancer Res. 2, 277–285 (1996).
Taplin, M. E. et al. Selection for androgen receptor mutations in prostate cancers treated with androgen antagonist. Cancer Res. 59, 2511–2515 (1999).
Culig, Z. et al. Expression, structure, and function of androgen receptor in advanced prostatic carcinoma. Prostate 35, 63–70 (1998).
Craft, N. et al. Evidence for clonal outgrowth of androgen-independent prostate cancer cells from androgen-dependent tumors through a two-step process. Cancer Res. 59, 5030–5036 (1999).
Buchanan, G. et al. Collocation of androgen receptor gene mutations in prostate cancer. Clin. Cancer Res. 7, 1273–1281 (2001). Description of precocious AR mutations in human and TRAMP models and analysis of the types of mutation that stimulate AR signalling.
Buchanan, G. et al. Mutations at the boundary of the hinge and ligand binding domain of the androgen receptor confer increased transactivation function. Mol. Endocrinol. 15, 46–56 (2001).
Cher, M. L. et al. Genetic alterations in untreated metastases and androgen-independent prostate cancer detected by comparative genomic hybridization and allelotyping. Cancer Res. 56, 3091–3102 (1996).
Bruchovsky, N. et al. Intermittent androgen suppression for prostate cancer: Canadian Prospective Trial and related observations. Mol. Urol. 4, 191–199; discussion 201 (2000).
Visakorpi, T. et al. In vivo amplification of the androgen receptor gene and progression of human prostate cancer. Nature Genet. 9, 401–406 (1995). This study defined the amplified AR as a mechanism for the hypersensitive pathway.
Palmberg, C. et al. Androgen receptor gene amplification at primary progression predicts response to combined androgen blockade as second line therapy for advanced prostate cancer. J. Urol. 164, 1992–1995 (2000).
Gregory, C. W., Johnson, R. T. Jr, Mohler, J. L., French, F. S. & Wilson, E. M. Androgen receptor stabilization in recurrent prostate cancer is associated with hypersensitivity to low androgen. Cancer Res. 61, 2892–2898.
Gregory, C. W. et al. A mechanism for androgen receptor-mediated prostate cancer recurrence after androgen deprivation therapy. Cancer Res. 61, 4315–4319 (2001).
Labrie, F. et al. Treatment of prostate cancer with gonadotropin-releasing hormone agonists. Endocr. Rev. 7, 67–74 (1986). An early review of the endocrinology and hormonal treatment of prostate cancer.
Makridakis, N. et al. A prevalent missense substitution that modulates activity of prostatic steroid 5α-reductase. Cancer Res. 57, 1020–1022 (1997).
Labrie, F. et al. Science behind total androgen blockade: from gene to combination therapy. Clin. Invest. Med. 16, 475–492 (1993).
Eisenberger, M. A. et al. Bilateral orchiectomy with or without flutamide for metastatic prostate cancer. N. Engl. J. Med. 339, 1036–1042 (1998).
Prostate Cancer Trialists' Collaborative Group. Maximum androgen blockade in advanced prostate cancer: an overview of the randomised trials. Lancet 355, 1491–1498 (2000).
Collette, L., Studer, U. E., Schroder, F. H., Denis, L. J. & Sylvester, R. J. Why phase III trials of maximal androgen blockade versus castration in M1 prostate cancer rarely show statistically significant differences. Prostate 48, 29–39 (2001).
Liotta, L. & Petricoin, E. Molecular profiling of human cancer. Nature Rev. Genet. 1, 48–56 (2000).
Veldscholte, J. et al. The androgen receptor in LNCaP cells contains a mutation in the ligand binding domain which affects steroid binding characteristics and response to antiandrogens. J. Steroid Biochem. Mol. Biol. 41, 665–669 (1992). Early definition of the LNCaP mutation that laid the foundations for understanding the promiscuous AR mechanism.
Gaddipati, J. P. et al. Frequent detection of codon 877 mutation in the androgen receptor gene in advanced prostate cancers. Cancer Res. 54, 2861–2864 (1994).
Culig, Z. et al. Mutant androgen receptor detected in an advanced-stage prostatic carcinoma is activated by adrenal androgens and progesterone. Mol. Endocrinol. 7, 1541–1550 (1993).
Small, E. J. & Srinivas, S. The antiandrogen withdrawal syndrome. Experience in a large cohort of unselected patients with advanced prostate cancer. Cancer 76, 1428–1434 (1995).
Gottlieb, B. et al. The Androgen Receptor Gene Mutations Database. Nucleic Acids Res. 26, 234–238 (1998).
Matias, P. M. et al. Structural evidence for ligand specificity in the binding domain of the human androgen receptor. J. Biol. Chem. 275, 26164–26171 (2000).
Sack, J. S. et al. Crystallographic structures of the ligand-binding domains of the androgen receptor and its T877A mutant complexed with the natural agonist dihydrotestosterone. Proc. Natl Acad. Sci. USA 98, 4904–4909 (2001).
McDonald, S., Brive, L., Agus, D. B., Scher, H. I. & Ely, K. R. Ligand responsiveness in human prostate cancer: structural analysis of mutant androgen receptors from LNCaP and CWR22 tumors. Cancer Res. 60, 2317–2322 (2000).
Navone, N. M. et al. Establishment of two human prostate cancer cell lines derived from a single bone metastasis. Clin. Cancer Res. 3, 2493–2500 (1997).
Zhao, X. Y. et al. Glucocorticoids can promote androgen-independent growth of prostate cancer cells through a mutated androgen receptor. Nature Med. 6, 703–706 (2000). Defined the double AR mutation creating a cortisol-responsive prostate cancer cell, expanding the promiscuous AR hypothesis to include circulating levels of corticosteroids.
Zhao, X. Y. et al. Two mutations identified in the androgen receptor of the new human prostate cancer cell line MDA PCa 2a. J. Urol. 162, 2192–2199 (1999).
Suzuki, H. et al. Androgen receptor gene mutations in human prostate cancer. J. Steroid Biochem. Mol. Biol. 46, 759–765 (1993).
Han, G. et al. Hormone status selects for spontaneous somatic androgen receptor variants that demonstrate specific ligand and cofactor dependent activities in autochthonous prostate cancer. J. Biol. Chem. 276, 11204–11213 (2001).
Thalmann, G. N. et al. LNCaP progression model of human prostate cancer: androgen-independence and osseous metastasis. Prostate 44, 91–103 (2000).
Culig, Z. et al. Switch from antagonist to agonist of the androgen receptor bicalutamide is associated with prostate tumour progression in a new model system. Br. J. Cancer 81, 242–251 (1999).
Adachi, M. et al. Androgen-insensitivity syndrome as a possible coactivator disease. N. Engl. J. Med. 343, 856–862 (2000).
Anzick, S. L. et al. AIB1, a steroid receptor coactivator amplified in breast and ovarian cancer. Science 277, 965–968 (1997).
Yeh, S. & Chang, C. Cloning and characterization of a specific coactivator, ARA70, for the androgen receptor in human prostate cells. Proc. Natl Acad. Sci. USA 93, 5517–5521 (1996).
Alen, P. et al. Interaction of the putative androgen receptor-specific coactivator ARA70/ELE1α with multiple steroid receptors and identification of an internally deleted ELE1β isoform. Mol. Endocrinol. 13, 117–128 (1999).
Gao, T., Brantley, K., Bolu, E. & McPhaul, M. J. RFG (ARA70, ELE1) interacts with the human androgen receptor in a ligand-dependent fashion, but functions only weakly as a coactivator in cotransfection assays. Mol. Endocrinol. 13, 1645–1656 (1999).
Miyamoto, H., Yeh, S., Wilding, G. & Chang, C. Promotion of agonist activity of antiandrogens by the androgen receptor coactivator, ARA70, in human prostate cancer DU145 cells. Proc. Natl Acad. Sci. USA 95, 7379–7384 (1998).
Lavinsky, R. M. et al. Diverse signaling pathways modulate nuclear receptor recruitment of N-CoR and SMRT complexes. Proc. Natl Acad. Sci. USA 95, 2920–2925 (1998).
McGuire, W. L., Chamness, G. C. & Fuqua, S. A. Estrogen receptor variants in clinical breast cancer. Mol. Endocrinol. 5, 1571–1577 (1991).
Culig, Z. et al. Androgen receptor activation in prostatic tumor cell lines by insulin-like growth factor-I, keratinocyte growth factor, and epidermal growth factor. Cancer Res. 54, 5474–5478 (1994). Early description of growth-factor activation of AR in the absence of ligand, developing the basis for the outlaw AR pathway.
Slamon, D. J. et al. Studies of the HER-2/neu proto-oncogene in human breast and ovarian cancer. Science 244, 707–712 (1989).
Borg, A. et al. ERBB2 amplification is associated with tamoxifen resistance in steroid-receptor positive breast cancer. Cancer Lett. 81, 137–144 (1994).
Pietras, R. J. et al. HER-2 tyrosine kinase pathway targets estrogen receptor and promotes hormone-independent growth in human breast cancer cells. Oncogene 10, 2435–2446 (1995).
Craft, N., Shostak, Y., Carey, M. & Sawyers, C. L. A mechanism for hormone-independent prostate cancer through modulation of androgen receptor signaling by the HER-2/neu tyrosine kinase. Nature Med. 5, 280–285 (1999). A leading example of the outlaw pathway with implications for the treatment of some cases of prostate cancer with Herceptin.
Yeh, S. et al. From HER2/Neu signal cascade to androgen receptor and its coactivators: a novel pathway by induction of androgen target genes through MAP kinase in prostate cancer cells. Proc. Natl Acad. Sci. USA 96, 5458–5463 (1999).
Slamon, D. J. et al. Use of chemotherapy plus a monoclonal antibody against HER2 for metastatic breast cancer that overexpresses HER2. N. Engl. J. Med. 344, 783–792 (2001).
Vogel, C. et al. First-line, single-agent Herceptin (trastuzumab) in metastatic breast cancer: a preliminary report. Eur. J. Cancer 37, S25–S29 (2001).
Agus, D. B. et al. Response of prostate cancer to anti-Her-2/neu antibody in androgen-dependent and -independent human xenograft models. Cancer Res. 59, 4761–4764 (1999).
Li, J. et al. PTEN, a putative protein tyrosine phosphatase gene mutated in human brain, breast, and prostate cancer. Science 275, 1943–1947 (1997).
Ittmann, M. M. Chromosome 10 alterations in prostate adenocarcinoma. Oncol. Rep. 5, 1329–1335 (1998).
Datta, S. R., Brunet, A. & Greenberg, M. E. Cellular survival: a play in three AKTs. Genes Dev. 13, 2905–2927 (1999).
Stambolic, V. et al. Negative regulation of PKB/AKT-dependent cell survival by the tumor suppressor PTEN. Cell 95, 29–39 (1998).
Wu, X., Senechal, K., Neshat, M. S., Whang, Y. E. & Sawyers, C. L. The PTEN/MMAC1 tumor suppressor phosphatase functions as a negative regulator of the phosphoinositide 3-kinase/AKT pathway. Proc. Natl Acad. Sci. USA 95,15587–15591 (1998).
Maehama, T. & Dixon, J. E. PTEN: a tumour suppressor that functions as a phospholipid phosphatase. Trends Cell Biol. 9, 125–128 (1999).
Zhou, H., Li, X. M., Meinkoth, J. & Pittman, R. N. AKT regulates cell survival and apoptosis at a postmitochondrial level. J. Cell Biol. 151, 483–494 (2000).
Medema, R. H., Kops, G. J., Bos, J. L. & Burgering, B. M. AFX-like Forkhead transcription factors mediate cell-cycle regulation by Ras and PKB through p27kip1. Nature 404, 782–787 (2000).
Graff, J. R. et al. Increased AKT activity contributes to prostate cancer progression by dramatically accelerating prostate tumor growth and diminishing p27Kip1 expression. J. Biol. Chem. 275, 24500–24505 (2000).
Wen, Y. et al. HER-2/neu promotes androgen-independent survival and growth of prostate cancer cells through the AKT pathway. Cancer Res. 60, 6841–6845 (2000).
Zhou, B. P. et al. HER-2/neu blocks tumor necrosis factor-induced apoptosis via the AKT/NF- κB pathway. J. Biol. Chem. 275, 8027–8031 (2000).
Signoretti, S. et al. HER-2-neu expression and progression toward androgen independence in human prostate cancer. J. Natl Cancer Inst. 92, 1918–1925 (2000).
Campbell, R. A. et al. Phosphatidylinositol 3-kinase/AKT-mediated activation of estrogen receptor α: a new model for anti-estrogen resistance. J. Biol. Chem. 276, 9817–9824 (2001).
McDonnell, T. J. et al. Expression of the protooncogene BCL-2 in the prostate and its association with emergence of androgen-independent prostate cancer. Cancer Res. 52, 6940–6944 (1992). Raised BCL2 overexpression as a potential example of the bypass pathway.
Colombel, M. et al. Detection of the apoptosis-suppressing oncoprotein Bcl2 in hormone-refractory human prostate cancers. Am. J. Pathol. 143, 390–400 (1993).
Liu, A. Y., Corey, E., Bladou, F., Lange, P. H. & Vessella, R. L. Prostatic cell lineage markers: emergence of Bcl2+ cells of human prostate cancer xenograft LuCaP 23 following castration. Int. J. Cancer 65, 85–89 (1996).
Gleave, M. et al. Progression to androgen independence is delayed by adjuvant treatment with antisense BCL-2 oligodeoxynucleotides after castration in the LNCaP prostate tumor model. Clin. Cancer Res. 5, 2891–2898 (1999).
Furuya, Y., Krajewski, S., Epstein, J. I., Reed, J. C. & Isaacs, J. T. Expression of BCL-2 and the progression of human and rodent prostatic cancers. Clin. Cancer Res. 2, 389–398.
Isaacs, J. T. The biology of hormone refractory prostate cancer. Why does it develop? Urol. Clin. North Am. 26, 263–273 (1999). Expounded the lurker cell hypothesis.
Bui, M. & Reiter, R. E. Stem cell genes in androgen-independent prostate cancer. Cancer Metastasis Rev. 17, 391–399 (1998).
Estrov, Z. et al. Persistence of self-renewing leukemia cell progenitors during remission in children with B-precursor acute lymphoblastic leukemia. Leukemia 8, 46–52 (1994).
Davi, F., Gocke, C., Smith, S. & Sklar, J. Lymphocytic progenitor cell origin and clonal evolution of human B-lineage acute lymphoblastic leukemia. Blood 88, 609–621 (1996).
Morris, M. J. & Scher, H. I. Novel strategies and therapeutics for the treatment of prostate carcinoma. Cancer 89, 1329–1348 (2000).
Mendelsohn, L. G. Prostate cancer and the androgen receptor: strategies for the development of novel therapeutics. Prog. Drug Res. 55, 213–233 (2000).
Gleave, M. E., Miayake, H., Goldie, J. Nelson, C. & Tolcher, A. Targeting BCL-2 gene to delay androgen-independent progression and enhance chemosensitivity in prostate cancer using antisense BCL-2 oligodeoxynucleotides. Urology 54, 36–46 (1999).
Kurita. T. et al. Paracrine regulation of apoptosis by steroid hormones in the male and female reproductive system. Cell Death Differ. 8, 192–200 (2001).
Chung, L. W. The role of stromal–epithelial interaction in normal and malignant growth. Cancer Surv. 23, 33–42 (1995).
Osborne, C. K. Tamoxifen in the treatment of breast cancer. N. Engl. J. Med. 339, 1609–1618 (1998).
Acknowledgements
We thank P. Malloy, A. Krishnan, D. Peehl and R. Roth for helpful discussions.
Author information
Authors and Affiliations
Corresponding author
Related links
Related links
DATABASE LINKS
FURTHER INFORMATION
Glossary
- ACTIVATING DOMAIN
-
Region of steroid hormone receptors that enhances target gene transcription.
- ZINC FINGER
-
Protein module in which conserved cysteine or histidine residues coordinate a zinc atom. Some zinc-finger regions bind specific DNA sequences; others are involved in protein–protein interactions.
- HEAT-SHOCK PROTEINS
-
(HSP). Molecular chaperones that are induced during cellular stress. They help regulate cellular homeostasis and promote survival.
- ANDROGEN RESPONSE ELEMENT
-
(ARE). Site composed of hexanucleotide repeats and a spacer, usually in the promoter regions of target genes, that contains the androgen receptor zinc-finger-binding region.
- GENERAL TRANSCRIPTION APPARATUS
-
(GTA). A complex of proteins with the potential to facilitate transcription of genes. In vivo specificity of gene transcription by the GTA is regulated by interacting transcription factors.
- LNCaP CELLS
-
A widely studied metastatic prostate cancer cell line that is androgen responsive.
- PROSTATE-SPECIFIC ANTIGEN
-
(PSA). A serine protease in the kallikrein gene family that is secreted into seminal fluid by prostatic epithelial cells and found in the serum. As it is almost exclusively a product of prostate cells, measurement in blood has proved to be exceptionally useful as a tumour marker for diagnosis of prostate cancer and monitoring the effectiveness of treatment.
- p160 CO-ACTIVATORS
-
p160 co-activators are a family of ∼ 160-kDa proteins that act as co-activators of nuclear receptors. SRC1 and TIF2 are members of this family.
- DOMINANT NEGATIVE
-
A protein with an inhibitory signal that overrides or blocks a positive signal for transcription.
- XENOGRAFT
-
A graft of tissue or cells transplanted between animals of different species.
- PROSTATIC INTRAEPITHELIAL NEOPLASIA
-
(PIN). Dysplastic cellular changes confined to the prostatic epithelium and considered to be a precursor to adenocarcinoma of the prostate.
Rights and permissions
About this article
Cite this article
Feldman, B., Feldman, D. The development of androgen-independent prostate cancer. Nat Rev Cancer 1, 34–45 (2001). https://doi.org/10.1038/35094009
Issue Date:
DOI: https://doi.org/10.1038/35094009
This article is cited by
-
USP54 is a potential therapeutic target in castration-resistant prostate cancer
BMC Urology (2024)
-
Arsenic-induced prostate cancer: an enigma
Medical Oncology (2024)
-
Canonical and truncated transglutaminase-2 regulate mucin-1 expression and androgen independency in prostate cancer cell lines
Cell Death & Disease (2023)
-
Post-transcriptional modification of m6A methylase METTL3 regulates ERK-induced androgen-deprived treatment resistance prostate cancer
Cell Death & Disease (2023)
-
Optimization Therapy by Coupling Intermittent Androgen Suppression with Impulsive Chemotherapy for a Prostate Cancer Model
Bulletin of Mathematical Biology (2023)