Abstract
Aims To systematically review the literature on the prevalence and incidence of diabetic retinopathy (DR) and macular oedema (MO).
Methods A search of the bibliographic databases (Medline, Embase, CINAHL) was conducted up to October 2001. Selected relevant studies were scrutinized and included in the review.
Results A total of 359 studies were included. The studies were reported in nearly 100 different journals and in over 50 countries. The majority of the studies were US-based, with large studies such as the Wisconsin Epidemiologic Study of Diabetic Retinopathy dominating the literature. The studies were quite dated and highly heterogeneous in nature in terms of patient selection with variable inclusion criteria (age range, gender, diabetes duration and type, ethnicity, comorbidity, and DR status, assessment, and classification).
Conclusions There are inconsistencies between epidemiological studies, and differences in study methods may contribute to conflicting reports of prevalence and incidence of DR and MO in diabetic populations. As new therapies for DR and its associated complications emerge, the need to capture and monitor new epidemiological data becomes increasingly important to be able to assess the impact and effectiveness of these therapies. Robust, longitudinal capture of patient data is, therefore, essential to evaluate the impact of current practice on the epidemiology of diabetic eye complications.
Similar content being viewed by others
Introduction
Diabetes mellitus results in considerable morbidity and mortality, affecting about 180 million people worldwide.1 The disease is classified according to two distinct groups of patients: type I diabetes (previously known as ‘insulin dependent’ or ‘juvenile onset’) is characterized by destruction of the insulin secretory pancreatic β-cells of the islets of Langerhans caused by an autoimmune process, usually leading to absolute insulin deficiency; type II diabetes (noninsulin dependent, adult-onset) is characterized by insulin resistance in peripheral tissues and an insulin secretory defect of the β-cell.2 Between 70 and 90% of diabetic patients have type II diabetes.3 However, current statistics suggest that an estimated 50% of diabetes sufferers remain undiagnosed.4, 5, 6
The total number of people with diabetes is expected to rise to an estimated 300 million cases by the year 2025, with the most significant increases in developing countries, thought to be the result of population growth, ageing, obesity, and sedentary lifestyles.7 Proportionally, the global population is predicted to increase by 64% between the years 1995 and 2025, compared with the prevalence of diabetes mellitus among adults, which is expected to rise by over 120%.7 Indeed, by 2010, the number of people suffering from type II diabetes, which constitutes 90–95% of diabetic patients,8 is set to double.9
The development of diabetes immediately increases a patient's propensity for developing a broad spectrum of irreversible complications.10 Complications of diabetes can be largely divided into macrovascular and microvascular complications. The macrovascular complications include cerebrovascular disease, coronary heart disease, and peripheral vascular disease. The microvascular complications include diabetic retinopathy (DR), diabetic neuropathy, and diabetic nephropathy. The prevalence of these complications is strongly related to the prevalence, type, and duration of diabetes; therefore, the increasing global population, changing age demographics, and predicted rise in the proportion of adults suffering from diabetes will inevitably be accompanied by an increase in the frequency of diabetic complications.
Diabetes has many manifestations in the eye, of which cataracts and DR are the most significant cause of visual impairment and blindness, and people with diabetes are 25 times more likely than the general population to become blind.11 In developed countries, diabetic eye disease represents the leading cause of blindness in adults under 75 years.12 DR is the most common complication in type I diabetes and nearly all patients will have some degree of retinopathy 15–20 years after diagnosis.13, 14, 15, 16 Similarly, more than 60% of type II diabetes sufferers will have evidence of DR during this period.14, 17 Visual impairment as a result of DR has a significant impact on patients' quality of life,18 and can compromise their ability to manage successfully their disease, which can in turn have a negative impact on the incidence of other diabetic complications and overall life expectancy.
DR is a progressive disease predominantly affecting the integrity of the microscopic vessels found in the retina. DR can be broadly divided into two clinical stages: nonproliferative and proliferative diabetic retinopathy (PDR). During nonproliferative DR, the earliest visible sign of retinal damage results from abnormal permeability and/or nonperfusion of capillaries, leading to the formation of microaneurysms.19, 20 Abnormal capillary permeability results in the leaking of fluid and solutes into the surrounding retinal tissue, which collects around the macula; this is referred to as macular oedema (MO) and it threatens visual acuity. PDR develops following the occlusion of retinal capillaries leading to retinal ischaemia, which promotes the development of neovascularization, a process by which new blood vessels proliferate on the surface of the retina. However, these vessels are fragile and haemorrhage easily. The resulting accumulation of blood in the vitreous cavity from these haemorrhaging vessels seriously impairs vision. This may be permanent due to further complications such as traction retinal detachment leading to registered blindness. It has been estimated that without treatment for PDR, 50% of all patients will become blind within 5 years following diagnosis.21
The aim of this systematic review is to provide a comprehensive overview of the published literature pertaining to the epidemiology of DR and MO.
Methods
Literature search
Three electronic bibliographic databases of medical literature (Medline, Embase, and CINAHL) were interrogated using customized searches developed by one of the authors (MA) in conjunction with a Cochrane Collaboration trained Trials Co-ordinator. The searches were limited to reported studies on humans published in English language papers. The Publication Type filter was applied to exclude comments, letters, and editorial citations. Medline was searched, initially, from January 1966 to July 2001, Embase from January 1980 to July 2001, and CINAHL from January 1982 to July 2001. In addition, the 38 most productive journals in terms of articles identified from pilot electronic searches were hand-searched from January 2001 to identify articles incorrectly indexed and those awaiting indexing. A rerun of the electronic searches up to and including October 2001 provided the final reference list for data abstraction.
Indexing terms differ between databases; therefore, a different search strategy was developed for each database searched (Table 1). The three search strategies were constructed in two sections:
-
MeSH subject headings and free-text terms relating to DR and ME. Free-text terms used to describe the staging of diabetic retinopathy were also included.
-
Epidemiological studies and relevant study designs. This section consisted of MeSH subject headings covering the scope of incidence and prevalence of disease in a population and the associated issue of risk factors and staging and screening for the disease.
Results
The original Medline search generated 4720 citations. After a review of the publication abstracts by the Cochrane Trials Co-ordinator, 361 publications were considered relevant. Relevant articles were original reports of studies designed to describe specifically incidence and/or prevalence or DR or MO. Editorials, letters, and reviews, as well as original papers describing biochemical and pathogenic mechanisms and treatment trials identified by the electronic search were excluded. The Embase search generated 1570 citations, and these were merged with the results of the Medline search, and duplicate publications discarded. This search identified an additional 35 articles on Embase that had not been identified on Medline. The CINAHL search generated 88 citations, which were merged with the results from the Medline and Embase searches. This did not generate any additional, relevant citations. Altogether, a total of 396 citations were identified as potentially relevant at this stage. The hand search identified a further 16 citations for consideration, and the rerun search up to October 2001, unfiltered by the trials coordinator, added a further 309 potential articles. All the resulting abstracts were then independently assessed by three of the authors (MA, HB, RW), and following review of full articles, a total of 359 articles were included in the literature review.
Citations—overall commentary
The 359 articles were reported in nearly 100 different journals and included studies carried out in over 50 countries. The majority of the reports were relatively recent, with only 70 studies pre-1990. Studies were principally US-based, with the Wisconsin Epidemiologic Study of Diabetic Retinopathy (WESDR) accounting for a significant number of articles. Some of the US-based studies included Native American populations, and several studies examined differences in DR incidence, prevalence, and associated risk factors in those of Hispanic and black American origin. Studies from the UK, Sweden, Japan, Australia, Denmark, Finland, Germany, and India accounted for 129 reports. A number of UK studies report on DR rates among British South Asian populations.
DR incidence and prevalence
Approximately one-third of studies were reports of people with type I diabetes, one-third reported type II diabetes and the remaining third reported mixed populations including both type I and type II. Just under one-half of the reports involved studies of population-based (as opposed to clinic-based) cohorts; however, this figure is partly a reflection of the large output from a few large longitudinal population studies such as the WESDR.
The publications pertaining to prevalence and incidence of DR were found to be highly heterogeneous in terms of subject selection with variable inclusion criteria, such as age range, gender, diabetes duration and type, ethnicity, comorbidity and DR status, assessment and classification. A large number of studies were of clinical attendees. Published data cover a wide range of countries (European, American, African, Asian, Australasian) and population groups (controls, type I diabetes, type II diabetes treated by diet, type II diabetes treated with oral hypoglycaemic agents, type II diabetes treated with insulin); however, studies are limited in scope and the literature is dominated by a few large studies (eg WESDR).
Prevalence studies
Point prevalence can be defined as the proportion of cases of a disorder or disease in a particular population at a particular point in time, whereas lifetime prevalence is the proportion of the population who have a history of a given condition at a particular point in time.
A total of 153 references provided prevalence data for DR (including PDR) or MO (including clinically significantly MO; CSMO) in type I, type II, or mixed populations. The range of prevalence data was wide, and a summary of the data is given in Table 2.9, 13, 15, 16, 17, 22, 23, 24, 25, 26, 27, 28, 29, 30, 31, 32, 33, 34, 35, 36, 37, 38, 39, 40, 41, 42, 43, 44, 45, 46, 47, 48, 49, 50, 51, 52, 53, 54, 55, 56, 57, 58, 59, 60, 61, 62, 63, 64, 65, 66, 67, 68, 69, 70, 71, 72, 73, 74, 75, 76, 77, 78, 79, 80, 81, 82, 83, 84, 85, 86, 87, 88, 89, 90, 91, 92, 93, 94, 95, 96, 97, 98, 99, 100, 101, 102, 103, 104, 105, 106, 107, 108, 109, 110, 111, 112, 113, 114, 115, 116, 117, 118, 119, 120, 121, 122, 123, 124, 125, 126, 127, 128, 129, 130, 131, 132, 133, 134, 135, 136, 137, 138, 139, 140, 141, 142, 143, 144, 145, 146, 147, 148, 149, 150, 151, 152, 153, 154, 155, 156, 157, 158, 159, 160, 161, 162, 163, 164, 165, 166, 167, 168, 169 Those studies that specifically report the prevalence of retinopathy at diagnosis (rather than pooled prevalence data from patients who may have had varied exposure to the disease) suggest that the prevalence of DR of any severity in people with newly diagnosed diabetes is dependent upon the type of diabetes (type I or type II). Generally, the prevalence of retinopathy at diagnosis of type I diabetes is reportedly low, between 0 and 3%,45, 59, 101, 160 while a higher proportion of those with newly diagnosed type II diabetes have evidence of DR (6.7–30.2%).14, 32, 39, 79, 98, 104, 160, 166, 170
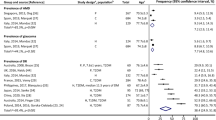
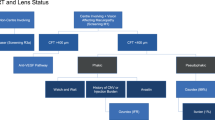
Studies not confined to newly diagnosed diabetes show that the prevalence of DR in type I and type II diabetes is strongly correlated with duration of disease. Type I and type II patients enrolled into the WESDR, which began in 1979 and included 2990 patients across 11 counties in southern Wisconsin, USA, were more likely to have evidence of DR or PDR the longer the duration of their disease (Table 3).171 The WESDR also identified an association between insulin treatment and the prevalence of DR or PDR in type II patients (Figure 1). Of the type II patients who had evidence of DR, 62% were treated with insulin and 36% were treated without insulin.95 Similarly, 25 and 5% of patients showed evidence of PDR with and without insulin treatment, respectively. This effect is also evident in a Swedish study where noninsulin-treated type II patients were categorized into those treated with oral hypoglycaemic agents or by diet alone and compared with type I patients. DR was identified in a similar proportion of type I and type II patients treated with insulin (68.3 vs 65.9%) compared with 30 and 6.7% of type II patients treated with oral hypoglycaemic agents or diet, respectively.144
Frequency of MO by duration of diabetes in insulin-treated patients with young-onset diabetes (a) and patients with insulin- and noninsulin-treated older-onset diabetes (b). Reprinted from Klein R, Klein BE, Moss SE, Davis MD, DeMets DL. The Wisconsin Epidemiologic Study of Diabetic Retinopathy IV. Diabetic macular edema. Ophthalmology 1984; 91: 1464–1474, copyright (1984), with permission from Elsevier Science.96
In contrast to the results in newly diagnosed type I diabetes cited above, the Diabetes Control and Complications Trial (DCCT) was a clinical study conducted from 1983 to 1993 by the National Institute of Diabetes and Digestive and Kidney Diseases involving volunteers with type I diabetes from 29 medical centres in Canada and the USA. The trial reports fundal photographic evidence of DR in 44.4% of patients with diabetes of less than 5 years duration and retinopathic changes on fluorescein angiography in 22% of patients, which were not evident from fundal photography.172 Thus, 54.2% of patients had DR at baseline and 67.1% had DR within 5 years of diabetes duration.
The United Kingdom Prospective Diabetes Study (UKPDS) was a 20-year study involving 23 centres in the UK with more than 5000 patients with type II diabetes. This study also found a higher prevalence of DR in newly diagnosed type II diabetes than have other studies. In a subset of 2964 white, newly referred patients, DR (defined as microaneurysms or worse in one eye) was present in 39 and 35% of men and women, respectively; ‘cotton wool’ spots and neovascularization were also present in 8% of men and 4% of women.104 Other findings from the UK are summarized in Table 4.
The prevalence of MO has also been found to be related to the duration of the disease. In 919 type I and 1121 type II patients enrolled into the WESDR, 0% of type I patients with less than 5 years' disease duration showed evidence of MO, compared with 29% after 20 years duration. Similarly, within 5 years of diagnosis, only 3% of type II patients had MO, compared with 28% after 20 years' duration.96 Similar prevalence data have been reported in other studies in type II patients (8,77 5.4,42 3.7,136 8.2,149 4.7–8.2,64 2%98). The effect of insulin treatment on MO prevalence has also been investigated in type II patients; in 902 type I patients, 674 insulin-treated type II patients, and 696 noninsulin-treated patients from the WESDR, MO was present in 18, 20, and 12% of patients, respectively, after 15 years' disease duration95, 96 In a study in Sweden, MO prevalence rates of patients undergoing three-field stereo fundal photography were 16, 26.1, 8.6, and 0.6% in type I patients and type II patients treated with insulin, oral hypoglycaemic agents, or diet alone, respectively.144 The prevalence of clinically significant MO (ie MO that threatens central visual function; CSMO) is reportedly low in patients with type I diabetes (5%)96, 173 and type II diabetes (2%)118 in the first years following diagnosis. However, this increases to more than 20% in people who have had type I diabetes for 25 years.96 While these studies are valuable, it is important to recognize that the definition of CSMO is based on subjective criteria, and the degree of interstudy differences based on application of methodology is unknown at this time. Clearly, the most reliable data are derived from longitudinal studies from within the same patient population such as the WESDR and the UKPDS, where rigid clinical criteria were applied; however, even between these two studies, methodological differences apply. There is undoubtedly a need for a more objective method for determination of CSMO that can be universally applied.
A number of other studies have been conducted in Australia, Denmark, Finland, Sweden, Germany, India, Italy, Japan, and other European, Asian, and African countries (see Table 2). A few of these studies looked at large numbers of patients (between 2631 and 10 709 patients);61, 88, 91, 104, 112, 114, 116, 118, 121, 139, 143, 158, 164 however, the majority of the remaining studies recruited smaller numbers of patients.
In Australia, 29% of 4744 older patients (>40 years old) enrolled in the Visual Impairment Project had DR, 2.8% of whom had untreated sight-threatening retinopathy.116 Another large Australian study yielded similar prevalence rates (32.4%) in 3654 people aged 49 years or older undergoing eye examinations.118 Of the patients studied, 21% had evidence of DR within 1 year of diagnosis, while DR was present in 68% of patients after 20 years of disease.
The European Diabetes Study (EURODIAB) investigated patients from 31 centres in 16 European countries. The overall mean prevalence of DR in type I patients (n=3250) for all the participating centres was found to be 35.9% (range 18.9–68.8%), while the mean prevalence rate for PDR was 10.8% (range 3–19.8%).158 In the UK, in a population-based study of 10 709 diabetes patients identified through health district audit and data linkage, 16.5% had DR.121 DR prevalence was found to be slightly higher in Sweden following a population-based study; of 4127 patients identified in a health district, 27% were identified from their medical records as having DR.114
Two large studies in India screened type II patients. In 6792 patients, the prevalence of any DR was 34.1%, with 3.4% having PDR and 6.4% MO.143 In the second slightly smaller study (n=3010), DR was present in fewer patients (20%), although the prevalence of PDR was virtually identical (3.7%).139 A large population-based study in Libya (n=8922) found that just under one-third (30.5%) of type II patients had DR.88 In Barbados, DR was present in 28.5% of black/mixed race (almost entirely type II) patients.112 Of these patients, under 1% were found to have PDR, and CSMO was found in 8.6% of patients.
Ethnic variation
Several studies in the USA investigate the prevalence of DR in the Hispanic, Mexican, African American, and Native Americans (Pima, Sioux, Hopi, and Navajo).25, 45, 52, 60, 61, 65, 66, 67, 69, 70, 124, 126, 141, 146, 164 Of these, only five were comparative studies between ethnic groups.52, 65, 67, 69, 70 One study reported a similar prevalence in Hispanics and non-Hispanic whites,52 whereas the remaining four reported differences between blacks, whites, Mexicans, and Hispanics. In the third National Health and Nutrition Examination Survey in the USA, the prevalence of DR was 46% higher in blacks and 84% higher in Mexican Americans than whites with diabetes (Table 5).70
Outside of the US, the prevalence of DR in Fiji has been reported to be 52.6% (47% in Fijians and 53% in Indians) vs 13.3% in Australians (21% in Indians and 13% in Europeans).29 In the Fijian population, significantly more people had evidence of moderate-to-severe DR or PDR compared with Australians. Three other studies have examined ethnic differences in DR prevalence. The studies in South Africa and the UK report a similar prevalence between people of African, European, and Indian origin with type II diabetes,92 Asian and Europeans,38 and black West Indians, Jamaicans, and Caucasians.35
Incidence studies
Disease incidence can be defined as the number of new cases of a particular disease occurring over a defined time period. Incidence data can also be presented on the percentage of cases progressing to the next stage of a disease over a defined time period.
A total of 70 references provided incidence data for DR, PDR, or MO in type I, type II, or mixed cohorts. The range of incidence data for these studies is given in Table 6.101, 174, 175, 176, 177, 178, 179, 180, 181, 182, 183, 184, 185, 186, 187, 188, 189, 190, 191, 192, 193, 194, 195, 196, 197, 198, 199, 200, 201, 202, 203, 204, 205, 206, 207, 208, 209, 210, 211, 212, 213, 214, 215, 216, 217, 218, 219, 220, 221, 222, 223, 224, 225, 226, 227, 228, 229, 230, 231, 232, 233, 234, 235, 236, 237, 238, 239, 240, 241 The spread of countries and populations covered in the studies pertaining to DR incidence was more limited than those for prevalence, and dominated by the WESDR.
The 4-year incidence of any DR in 891 people with type I diabetes enrolled in the WESDR was estimated to be 59%.213 In the same study, 987 type II patients were split into two groups: those treated with insulin and those not treated with insulin. The 4-year incidence of any DR in these two groups of type II patients was 47.4 and 34.4%, respectively. Progression of DR and progression to PDR was observed in 41.2 and 10.5% of type I patients during the 4-year study. DR progression was seen in just over one-third (34%) of insulin-treated type II patients and 24.9% of noninsulin-treated type II patients. Progression to PDR was seen in 7.4 and 2.3% of these patients, respectively. In the three patient groups (type I, insulin-treated type II, and non-insulin-treated type II), the 4-year incidence of CSMO was 4.3, 5.1, and 1.3%, respectively, whereas the incidence of legal blindness was found to be 1.5, 3.2, and 2.7%, respectively.213 In another group of 1075 patients in the WESDR, 4.7% developed PDR and 2.8% developed CSMO after 4 years.209 In these patients, those experiencing one or more steps of progression (on the Early Treatment of Diabetic Retinopathy Study (ETDRS) scale) after 4 years were calculated to be 5.85 times more likely to develop PDR in the next 6 years compared with those with no progression.
The 10-year incidence of any DR, MO, or visual loss in patients enrolled in the WESDR was 89.3, 20.1, and 9.2% in type I diabetes (n=996), 79.2, 25.4, and 32.8% in insulin-treated type II diabetes (n=674), and 66.9, 13.9, and 21.4% in noninsulin-treated type II diabetes (n=696), respectively.211 The 10-year incidence of visual loss was also investigated as part of the WESDR in 891 type I, 485 insulin-treated type II, and 502 noninsulin-treated type II patients.226 At 10 years, blindness (visual acuity of 20/200 or less) was 1.8, 4.0, and 4.8% in type I, insulin-treated type II, and noninsulin-treated type II patients, respectively.226 In these three groups of patients, the 10-year incidence of doubling of the visual angle (visual acuity of 20/40 or less) was 9.2, 32.8, and 21.4%, respectively, while visual impairment (measured as a loss of 15 letters on a scale of 0–70 letters) was 9.4, 37.2, and 23.9%, respectively.226 Subjects have since been followed up for 14 years, and the 14-year rate of progression of DR was 86% in 634 type I diabetes patients, as measured by stereo fundal photography (grade Airlie House).173 Regression occurred in 17% of these patients and 37% had progression to PDR, whereas the incidence of MO was 26%. In 880 type I patients, the cumulative 14-year incidence rate of blindness, doubling of the visual angle, and visual impairment (classified as above) were 2.4, 14.2, and 12.7%, respectively.227
The ETDRS enrolled 3711 patients with mild-to-severe non-PDR or early PDR in both eyes. One eye of each patient was assigned randomly to early photocoagulation and the other to deferral photocoagulation. Follow-up examinations were scheduled at least every 4 months. The study showed that focal photocoagulation of CSMO, but not scatter photocoagulation, is effective in reducing the risk of moderate visual loss.242 The chance of developing high-risk PDR in 1 year ranged from 1% with mild DR at baseline to 3–8% for moderate, 15% for severe, and 45% for very severe DR. The incidence rose to 16, 27–39, 56, and 71% after 5 years in the respective groups.14
In 1919 patients with newly diagnosed type II diabetes in the UKPDS, 22% of those with no sign of DR at baseline developed DR at 6 years, and in 29% of patients with baseline DR, DR progressed two or more steps on the ETDRS scale after 6 years' disease duration.237 The risk of photocoagulation in relation to baseline DR severity was also examined in the UKPDS. Over 60% of newly diagnosed type II patients (n=3709) were free of DR at baseline: 0.2% required photocoagulation at 3 years, 1.1% at 6 years, and 2.6% at 9 years.217 This compares with those patients with more severe retinopathy features at entry (14% of patients enrolled), of which 15.3% received photocoagulation at 3 years and 31.9% after 9 years. In those patients with microaneurysms in one eye at baseline, 0, 1.8, and 4.7% needed treatment at 3, 6, and 9 years, respectively (Table 7).
There are also a number of studies from Europe, Africa, Australia, and Asia in both type I and type II diabetes. In Japan, the incidence rate of DR in 394 type II patients was 48.1/1000 person-years (PY) and progression to PDR in those patients with baseline DR was 57.7/1000 PY.232 In type I diabetes, the cumulative incidence of PDR has been estimated to be 20% at 15 years, 40% at 19 years, and rising to 70% at 29 years of diabetes duration.241
Discussion
This systematic review of the literature has described studies examining the prevalence and incidence for the development of DR and its associated retinal complications. The methodological approach used to identify articles for inclusion in the literature review is based upon the ideals of the Cochrane Collaboration. The search strategies are systematic, sensitive, and transparent. The Cochrane Collaboration is principally concerned with the comparison of treatments using randomized controlled trials, and therefore the key terms or MESH headings from those studies are becoming increasingly effective as authors become aware of the importance of accurately key wording their publications. However, the epidemiological studies described here are of varying designs, thereby necessitating the complex searching strategies employed to identify them. In addition, the key diabetes, ophthalmological, and general medicine journals were searched manually for the final 6-month period covered by the electronic searches to reduce the likelihood of nonidentification of studies due to a time delay in cataloguing the electronic bibliographic databases used. While no methodological strategy can guarantee complete incorporation of all relevant citations, the approach taken in this review is considered robust.
The literature is dominated by a few large studies such as the WESDR, UKPDS, DCCT, and ETDRS trials. These trials are regarded by many as the ‘gold standard’, and patients have since been followed up for a number of years, providing excellent information on the incidence of disease progression. However, the large studies—important as they are—are now dated, and in some cases may reflect treatment from a previous era. The smaller studies are often limited in scope and may uncover confounding or conflicting results due to their small sample size. In addition, a number of studies are also clinic-based as opposed to population-based. While these studies are valuable, the data they produce may not be generalized and the frequency and severity of a disease may be overestimated. For example, people with long-standing diabetes who have difficulty managing their disease may be referred more frequently for eye examination to specialists, rather than being treated in the community. For this reason, population-based studies may more accurately reflect the true situation. The heterogeneous nature of studies (eg patient selection criteria, diabetes type) and the disparity between study methods (eg eight-field colour fundal photography vs two-field retinal imagery vs ophthalmoscopy vs slit-lamp examination) may contribute to conflicting reports of prevalence and incidence—sometimes even within the same country—making direct comparison of studies difficult. This highlights the need for consistent data capture within and between countries.
Recently, computerized diagnostic testing screening has been evaluated and compared with other established means of testing, that is, ophthalmologist vs physician vs optometrist.243 The automated computer-based method was shown to be as effective as the ‘gold standard’ screening by an ophthalmologist for the detection of any retinopathy. This screening process is instantly translatable across studies and does not ‘fatigue’, making it an attractive possibility for the detection of retinopathy in diabetic patients. Automated detection may provide a useful role by identifying retinal images worthy of closer inspection or by eliminating up to 50% or more of the screening population who have no retinopathy.243
Diabetic retinopathy: the problem
Studies that are of sufficient size to stratify for age and duration of eye disease clearly show an increase in the prevalence of DR in older age groups with long-standing disease. As many as 100% of type I diabetic patients have been observed to develop some degree of retinopathy after 20–30 years,16, 84, 85 peaking at about 10–15 years after diagnosis. Although some studies document a decline in retinopathy prevalence after this time, it is likely linked to differential survival during the later stages of the disease. Nevertheless, the prevalence of blindness and visual impairment is declining over time, despite no evidence of a reduction in the incidence of DR. This is likely due to better glycaemic, blood pressure, and lipid control. It is further helped by improved screening practices, recent advances in laser treatment, and increased disease awareness. The timely and appropriate care for diabetic patients can significantly reduce visual loss over time, not only improving patients' quality of life, but reducing the financial burden associated with the complications of visual impairment. However, as DR can progress irreversibly with relatively few visual symptoms,187 the importance of early and adequate ophthalmological screening and subsequent treatment for all patients with diabetes is imperative.218, 244 It is also known that, despite adequate glycaemic and blood pressure control, DR can progress and once the disease process reaches a certain stage, its effects become irreversible. This phenomenon of ‘retinopathic momentum’ was defined in the DCCT and suggests that once DR progresses far enough down the line, then the momentum carries it forward, and that any form of intervention would not affect its relentless progress.245 Nevertheless, screening and treatment have been predicted to prevent approximately three-quarters of expected cases of blindness in areas of the UK.246 Despite this, studies suggest that over one-third of diabetic patients do not adhere to screening guidelines,247, 248, 249 endangering their visual acuity and long-term health. In addition, the provision of treatment guidelines for DR was found to have little impact on the healthcare management of the community, suggesting that mere dissemination of these guidelines is not adequate to change referral or treatment behaviours of physicians.250
Future directions
The phenomenon of retinopathic momentum needs to be further investigated with large studies looking at the different stages of DR and their progression rates, and it is postulated that different therapies may have different ‘windows’ of therapeutic effect in the overall DR disease process. Despite evidence suggesting that intensive glycaemic therapy is effective in controlling diabetic complications, maintaining strict blood glucose levels (and blood pressure) has proven difficult for many patients with diabetes, and the risk of hypoglycaemia is increased under this treatment regimen.187, 245 Consequently, this therapy is not suited to all individuals, and even strict blood glucose regimens do not completely eliminate the threat of retinopathy.251 Unfortunately, some patients will also become visually impaired or blind and will require photocoagulation or surgical vitrectomy as a result of their underlying disease.252, 253 Thus, microvascular complications may be regarded as a partially preventable but inevitable outcome of diabetes,254 suggesting that biochemical mechanisms other than hyperglycaemia alone are involved in the pathogenesis of DR.74, 255 This inevitability of the development of DR in many patients—in some cases leading to visual impairment and even blindness—despite intensive glycaemic control signals the need to capitalize on current screening programmes and treatment options while developing novel, improved treatments for the underlying condition. Evaluation of current screening programmes largely supports the view that they are effective in the identification of early DR and MO.175 However, they must be widely, reliably, and economically applied, and they clearly have to be supported by effective treatment programmes consisting, at present, of laser photocoagulation for the treatment of advanced retinopathy including PDR and sight-threatening MO. Present literature is limited in terms of the acceptability of different approaches to screening, methods of maximizing uptake, and the effects of less than optimal uptake on the sensitivity of programmes (as opposed to the sensitivity of screening methods). This is an avenue that should be further explored.
Development of new compounds for the treatment of neovascularization represents a significant advance in the ability to treat diabetic patients, with the hope of preventing visual impairment and blindness in significant proportions of patients. These compounds are being developed to target the underlying cellular mechanisms of retinal complications. Vascular endothelial growth factor (VEGF) is a well-described mediator of ocular angiogenesis and permeability—indeed, it was first identified as a permeability factor—as is protein kinase-C-beta (PKC-β), a regulatory enzyme involved downstream of the VEGF receptor.256 PKC-β is present in high levels in the retina, and increased activation of this enzyme leads to increased production of VEGF.256 Therefore, targeting PKC-β with inhibitors or antagonists may arrest the development and/or progression of DR.256 Indeed, clinical trials with an orally administered PKC-β inhibitor have demonstrated a significant beneficial effect on abnormal retinal haemodynamics.257 Two Phase III randomized controlled trials are currently underway with such an inhibitor and hold much promise for the future.256 In addition, other potential treatments such as the use of statins and anti-adhesion molecules are clinical concepts and currently under experimental development, bringing hope for the future treatment and prevention of diabetic retinal complications.
As new therapies become available, the need to capture and monitor new epidemiological data becomes ever more important to help determine the size of the economic burden and also how progression of DR relates to novel treatments. Additionally, a general consensus is developing among ophthalmologists, which suggests there is a ‘low-risk’ category of DR patients, where intervention can have a significant impact, and a ‘high-risk’ group of DR patients where intervention is not so effective. Further research is needed in order to establish whether such a distinction exists. With these points in mind, epidemiological studies in the future need to make use of standard criteria and apply consistent terminology for the definition and identification of stages of DR and MO. The studies should, whenever possible, include samples that are representative of the communities from which they are drawn.
Robust longitudinal collection of patient data will be essential to be able to identify the true extent of diagnosed retinal complications of diabetes, in turn providing healthcare planners with essential information to aid future decision-making.
References
World Health Organisation. The World Health Report 2002. Available at: http://www.who.int/whr/en/ Accessed November 2002.
Report of the Expert Committee on the Diagnosis and Classification of Diabetes Mellitus. Diabetes Care 1997; 20: 1183–1197.
Bennett N, Dodd T, Flatley J, Freeth S, Bolling K . Health Survey for England 1993. Social Survey Division of the Office of Population Censuses and Surveys, HMSO, London, 1995.
Nabarro JDN . Diabetes in the United Kingdom: some facts and figures. Diabetic Med 1988; 5: 816–822.
Simmons D, Williams DR, Powell MJ . The Coventry Diabetes Study: prevalence of diabetes and impaired glucose tolerance in Europids and Asians. Q J Med 1991; 81: 1021–1030.
British Diabetic Association Report. Diabetes in the United Kingdom. 1996.
King H, Aubert RE, Herman WH . Global burden of diabetes, 1995–2025: prevalence, numerical estimates, and projections. Diabetes Care 1998; 21: 1414–1431.
Florence JA, Yeager BF . Treatment of type 2 diabetes mellitus. Am Fam Physician 1999; 59: 2835–2844, 2849–2850.
Zimmet P . Diabetes and obesity worldwide — epidemics in full flight. Presented at the 60th Scientific Sessions of the American Diabetes Association, 10 June 2000, San Antonio, TX.
Donnelly R, Emslie-Smith AM, Gardner ID, Morris AD . ABC of arterial and venous disease: vascular complications of diabetes. BMJ 2000; 320: 1062–1066.
National Society to Prevent Blindness. Visual Problems in the US Data Analysis Definitions. Data Sources, Detailed Data Tables, Analysis, Interpretation. National Society to Prevent Blindness: New York, 1980, pp 1–46.
National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Diseases. Diabetes in America, 2nd ed. National Institutes of Health, National Institute of Diabetes and Digestive and Kidney Diseases: Bethesda, MD, 1995.
Klein R, Klein BE, Moss SE, Davis MD, DeMets DL . The Wisconsin Epidemiologic Study of Diabetic Retinopathy. II. Prevalence and risk of diabetic retinopathy when age at diagnosis is less than 30 years. Arch Ophthalmol 1984; 102: 520–526.
Aiello LP, Gardner TW, King GL, Blankenship G, Cavallerano JD, Ferris III FL et al. Diabetic retinopathy. Diabetes Care 1998; 21: 143–156.
Johansen J, Sjolie AK, Elbol P, Eshoj O . The relation between retinopathy and albumin excretion rate in insulin-dependent diabetes mellitus. From the Funen County Epidemiology of Type I Diabetes Complications Survey. Acta Ophthalmol 1994; 72: 347–351.
Orchard TJ, Dorman JS, Maser RE, Becker DJ, Drash AL, Ellis D et al. Prevalence of complications in IDDM by sex and duration. Pittsburgh Epidemiology of Diabetes Complications Study II. Diabetes 1990; 39: 1116–1124.
Klein R, Klein BE, Moss SE, Davis MD, DeMets DL . The Wisconsin Epidemiologic Study of Diabetic Retinopathy III. Prevalence and risk of diabetic retinopathy when age at diagnosis is 30 or more years. Arch Ophthalmol 1984; 102: 527–532.
Brown MM, Brown GC, Sharma S, Shah G . Utility values and diabetic retinopathy. Am J Ophthalmol 1999; 128: 324–330.
Cogan DG, Toussaint D, Kuwabar T . Retinal vascular patterns. IV. Diabetic retinopathy. Arch Ophthalmol 1961; 66: 366–378.
Engerman RL . Pathogenesis of diabetic retinopathy. Diabetes 1989; 38: 1203–1206.
Hamilton AMP, Ulbig MW, Polkinghorne P . Management of Diabetic Retinopathy. BMJ Publishing Group: London, 1996.
Abood AlSamarrai AR, Mughni AA, Thabit A . Diabetic proliferative retinopathy in Yemen. Afro-Asian J Ophthalmol 1995; 13: 106–108.
Agardh E, Torffvit O, Agardh CD . The prevalence of retinopathy and associated medical risk factors in type I (insulin-dependent) diabetes mellitus. J Intern Med 1989; 226: 47–52.
Benson WH, Farber ME . Diabetic retinopathy in a rural diabetic population. Prevalence and risk. West Virginia Med J 1989; 85: 141–143.
Berinstein DM, Stahn RM, Welty TK, Leonardson GR, Herlihy JJ . The prevalence of diabetic retinopathy and associated risk factors among Sioux Indians. Diabetes Care 1997; 20: 757–759.
Bo S, Cavallo-Perin P, Gentile L, Repetti E, Pagano G . Influence of a familial history of diabetes on the clinical characteristics of patients with type 2 diabetes mellitus. Diabetic Med 2000; 17: 538–542.
Bognetti E, Calori G, Meschi F, Macellaro P, Bonfanti R, Chiumello G . Prevalence and correlations of early microvascular complications in young type I diabetic patients: role of puberty. J Pediatr Endocrinol Metab 1997; 10: 587–592.
Broadbent DM, Scott JA, Vora JP, Harding SP . Prevalence of diabetic eye disease in an inner city population: the Liverpool Diabetic Eye Study. Eye 1999; 13: 160–165.
Brooks B, Chong R, Ho I, Capstick F, Molyneaux L, Oo TT et al. Diabetic retinopathy and nephropathy in Fiji: comparison with data from an Australian diabetes centre. Aust N Z J Ophthalmol 1999; 27: 9–13.
Cahill M, Halley A, Codd M, O'Meara N, Firth R, Mooney D et al. Prevalence of diabetic retinopathy in patients with diabetes mellitus diagnosed after the age of 70 years. Br J Ophthalmol 1997; 81: 218–222.
Chang C, Lu F, Yang YC, Wu JS, Wu TJ, Chen MS et al. Epidemiologic study of type 2 diabetes in Taiwan. Diabetes Res Clin Pract 2000; 50 (Suppl 2): S49–S59.
Chang CJ, Fu CC, Chen MS, Yang CL, Chen YJ, Chuang LM et al. A comparison of newly and previously diagnosed diabetics in Taiwan. J Form Med Assoc 1990; 89: 264–269.
Chen MS, Kao CS, Chang CJ, Wu TJ, Fu CC, Chen CJ et al. Prevalence and risk factors of diabetic retinopathy among non insulin-dependent diabetic subjects. Am J Ophthalmol 1992; 114: 723–730.
Collins VR, Dowse GK, Plehwe WE, Imo TT, Toelupe PM, Taylor HR . High prevalence of diabetic retinopathy and nephropathy in Polynesians of Western Samoa. Diabetes Care 1995; 18: 1140–1149.
Cruickshank JK, Alleyne SA . Black West Indian and matched White diabetics in Britain compared with diabetics in Jamaica: body mass, blood pressure, and vascular disease. Diabetes Care 1987; 10: 170–179.
Dandona L, Dandona R, Naduvilath TJ, McCarty CA, Rao GN . Population based assessment of diabetic retinopathy in an urban population in southern India. Br J Ophthalmol 1999; 83: 937–940.
Danielsen R, Jonasson F, Helgason T . Prevalence of retinopathy and proteinuria in type I diabetics in Iceland. Acta Med Scand 1982; 212: 277–280.
Das BN, Thompson JR, Patel R, Rosenthal AR . The prevalence of eye disease in Leicester: a comparison of adults of Asian and European descent. J Roy Soc Med 1994; 87: 219–222.
Davis TM, Stratton IM, Fox CJ, Holman RR, Turner RC . UK Prospective Diabetes Study 22. Effect of age at diagnosis on diabetic tissue damage during the first 6 years of NIDDM. Diabetes Care 1997; 20: 1435–1441.
De Pablos PL, Martinez J, Martinez MP, Doreste JA . Prevalence of micro- and macroalbuminuria in a Canadian population of type 2 diabetic patients. Relationship with blood pressure, lipid profile, obesity and metabolic control. Diabetes Metab 1998; 24: 337–343.
Delcourt C, Vauzelle-Kervroedan F, Cathelineau G, Papoz L . Low prevalence of long-term complications in non-insulin-dependent diabetes mellitus in France: a multicenter study. CODIAB-INSERM-ZENECA Pharma Study Group. J Diabetes Complicat 1998; 12: 88–95.
Delcourt C, Villatte-Cathelineau B, Vauzelle-Kervroedan F, Cathelineau G, Papoz L . Visual impairment in type 2 diabetic patients. A multicentre study in France. CODIAB-INSERM-ZENECA Pharma Study Group. Acta Ophthalmol Scand 1995; 73: 293–298.
Diabetes Control Complications Trial Research Group. Clustering of long-term complications in families with diabetes in the diabetes control and complications trial. Diabetes 1997; 46: 1829–1839.
Donovan RJ . Prevalence of retinopathy in a diabetic clinic. BMJ 1978; 1: 1441–1442.
Dorf A, Ballintine EJ, Bennett PH, Miller M . Retinopathy in Pima Indians. Relationships to glucose level, duration of diabetes, age at diagnosis of diabetes, and age at examination in a population with a high prevalence of diabetes mellitus. Diabetes 1976; 25: 554–560.
Dowse GK, Humphrey AR, Collins VR, Plehwe W, Gareeboo H, Fareed D et al. Prevalence and risk factors for diabetic retinopathy in the multiethnic population of Mauritius. Am J Epidemiol 1998; 147: 448–457.
Dyck PJ, Kratz KM, Karnes JL, Litchy WJ, Klein R, Pach JM et al. The prevalence by staged severity of various types of diabetic neuropathy, retinopathy, and nephropathy in a population-based cohort: the Rochester Diabetic Neuropathy Study. Neurology 1993; 43: 817–824.
Ebeling P, Koivisto VA . Occurrence and interrelationships of complications in insulin-dependent diabetes in Finland. Acta Diabetol 1997; 34: 33–38.
el Haddad OA, Saad MK . Prevalence and risk factors for diabetic retinopathy among Omani diabetics. Br J Ophthalmol 1998; 82: 901–906.
Elbagir MN, Eltom MA, Mahadi EO, Berne C . Pattern of long-term complications in Sudanese insulin-treated diabetic patients. Diabetes Res Clin Pract 1995; 30: 59–67.
Erasmus RT, Alanamu RA, Bojuwoye B, Oluboyo P, Arije A . Diabetic retinopathy in Nigerians: relation to duration of diabetes, type of treatment and degree of control. East Afr Med J 1989; 66: 248–254.
Estacio RO, McFarling E, Biggerstaff S, Jeffers BW, Johnson D, Schrier RW et al. Overt albuminuria predicts diabetic retinopathy in Hispanics with NIDDM. Am J Kidney Dis 1998; 31: 947–953.
Fairchild JM, Hing SJ, Donaghue KC, Bonney MA, Fung AT, Stephens MM et al. Prevalence and risk factors for retinopathy in adolescents with type I diabetes. Med J Aust 1994; 160: 757–762.
Falck AA, Kaar ML, Laatikainen LT . Prevalence and risk factors of retinopathy in children with diabetes. A population-based study on Finnish children. Acta Ophthalmol 1993; 71: 801–809.
Falkenberg M, Finnstrom K . Associations with retinopathy in type 2 diabetes: a population-based study in a Swedish rural area. Diabetic Med 1994; 11: 843–849.
Fernandez-Vigo J, Sanchez MJ, Diaz RA, Barros J, Tome M, Bueno J . The prevalence of diabetic retinopathy in northwest Spain. An epidemiological study of diabetic retinopathy in Galicia. I. Acta Ophthalmol 1993; 71: 22–26.
Fernando DJ, Siribaddana S, De S, Subasinge Z . Prevalence of retinopathy in a Sri Lankan diabetes clinic. Ceylon Med J 1993; 38: 120–123.
Florkowski CM, Scott RS, Moir CL, Graham PJ . Clinical and biochemical outcomes of type 2 diabetes mellitus in Canterbury, New Zealand: a 6-year cohort study. Diabetes Res Clin Pract 1998; 40: 167–173.
Frank RN, Hoffman WH, Podgor MJ, Joondeph HC, Lewis RA, Margherio RR et al. Retinopathy in juvenile-onset diabetes of short duration. Ophthalmology 1980; 87: 1–9.
Freeman WL, Hosey GM . Diabetic complications among American Indians of Washington, Oregon, and Idaho. Prevalence of retinopathy, end-stage renal disease, and amputations. Diabetes Care 1993; 16: 357–360.
Gabir MM, Hanson RL, Dabelea D, Imperatore G, Roumain J, Bennett PH et al. Plasma glucose and prediction of microvascular disease and mortality: evaluation of 1997 American Diabetes Association and 1999 World Health Organization criteria for diagnosis of diabetes. Diabetes Care 2000; 23: 1113–1118.
Garancini P, Micossi P, Valsania P, Radaelli G, Bandello F, Scialdone A et al. Prevalence of retinopathy in diabetic subjects from out-patient clinics in Lombardy (Italy), and associated risk factors. A multicentre epidemiologic study. Diabetes Res Clin Pract 1989; 6: 129–138.
Gonzalez Villalpando ME, Gonzalez VC, Arredondo PB, Martinez Diaz SV, Mitchell B, Rivera MD et al. Moderate-to-severe diabetic retinopathy is more prevalent in Mexico City than in San Antonio, Texas. Diabetes Care 1997; 20: 773–777.
Gonzalez Villalpando ME, Gonzalez VC, Arredondo PB, Stern MP . Diabetic retinopathy in Mexico. Prevalence and clinical characteristics. Arch Med Res 1994; 25: 355–360.
Haffner SM, Fong D, Stern MP, Pugh JA, Hazuda HP, Patterson JK et al. Diabetic retinopathy in Mexican Americans and non-Hispanic whites. Diabetes 1988; 37: 878–884.
Haffner SM, Hazuda HP, Stern MP, Patterson JK, van Heuven WA, Fong D . Effects of socioeconomic status on hyperglycemia and retinopathy levels in Mexican Americans with NIDDM. Diabetes Care 1989; 12: 128–134.
Hamman RF, Mayer EJ, Moo-Young GA, Hildebrandt W, Marshall JA, Baxter J . Prevalence and risk factors of diabetic retinopathy in non-Hispanic whites and Hispanics with NIDDM. San Luis Valley Diabetes Study. Diabetes 1989; 38: 1231–1237.
Hapnes R, Bergrem H . Diabetic eye complications in a medium sized municipality in southwest Norway. Acta Ophthalmol Scand 1996; 74: 497–500.
Harris EL, Feldman S, Robinson CR, Sherman S, Georgopoulos A . Racial differences in the relationship between blood pressure and risk of retinopathy among individuals with NIDDM. Diabetes Care 1993; 16: 748–754.
Harris MI, Klein R, Cowie CC, Rowland M, Byrd-Holt DD . Is the risk of diabetic retinopathy greater in non-Hispanic blacks and Mexican Americans than in non-Hispanic whites with type 2 diabetes. A US population study. Diabetes Care 1998; 21: 1230–1235.
Hashim R, Khan FA, Khan DA, Shaukat A . Prevalence of microvascular complications in diabetic patients. J Coll Physicians Surgeons Pakistan 1999; 9: 120–122.
Haupt E, Benecke A, Haupt A, Herrmann R, Vogel H, Walter C . The KID Study VI: diabetic complications and associated diseases in younger type 2 diabetics still performing a profession. Prevalence and correlation with duration of diabetic state, BMI and C-peptide. Exp Clin Endocrinol Diabetes 1999; 107: 435–441.
Henricsson M, Gottsater A, Jeppsson JO, Fernlund P, Sundkvist G . The frequency and severity of retinopathy are related to HbA1c values after, but not at, the diagnosis of NIDDM. J Intern Med 1998; 244: 149–154.
Henricsson M, Nilsson A, Groop L, Heijl A, Janzon L . Prevalence of diabetic retinopathy in relation to age at onset of the diabetes, treatment, duration and glycemic control. Acta Ophthalmol Scand 1996; 74: 523–527.
Heriot WJ, Borger JP, Zimmet P, King H, Taylor R, Raper LR . Diabetic retinopathy in a natural population. Aust J Ophthalmol 1983; 11: 175–179.
Herman WH, Aubert RE, Engelgau MM, Thompson TJ, Ali MA, Sous ES et al. Diabetes mellitus in Egypt: glycaemic control and microvascular and neuropathic complications. Diabetic Med 1998; 15: 1045–1051.
Hirvela H, Laatikainen L . Diabetic retinopathy in people aged 70 years or older. The Oulu Eye Study. Br J Ophthalmol 1997; 81: 214–217.
Holl RW, Lang GE, Grabert M, Heinze E, Lang GK, Debatin KM . Diabetic retinopathy in pediatric patients with type-1 diabetes: effect of diabetes duration, prepubertal and pubertal onset of diabetes, and metabolic control. J Pediatr 1998; 132: 790–794.
Hu YH, Pan XR, Liu PA, Li GW, Howard BV, Bennett PH . Coronary heart disease and diabetic retinopathy in newly diagnosed diabetes in Da Qing, China: the Da Qing IGT and Diabetes Study. Acta Diabetol 1991; 28: 169–173.
Incorvaia C, Parmeggiani F, Mingrone G, Sebastiani A, De S . Prevalence of retinopathy in diabetic thalassaemic patients. J Pediatr Endocrinol Metab 1998; 11 (Suppl 3): 879–883.
Ishihara M, Yukimura Y, Yamada T . Diabetic complications and their relationships to risk factors in a Japanese population. Diabetes Care 1984; 7: 533–538.
Isomaa B, Henricsson M, Lehto M, Forsblom C, Karanko S, Sarelin L et al. Chronic diabetic complications in patients with MODY3 diabetes. Diabetologia 1998; 41: 467–473.
Jerneld B, Algvere P . Prevalence of retinopathy in diabetes treated with oral antihyperglycaemic agents. Acta Ophthalmol 1985; 63: 535–540.
Jerneld B, Algvere P . Relationship of duration and onset of diabetes to prevalence of diabetic retinopathy. Am J Ophthalmol 1986; 102: 431–437.
Jerneld B . Prevalence of diabetic retinopathy. A population study from the Swedish island of Gotland. Acta Ophthalmol 1988; 188: 3–32.
Johansen J, Sjolie AK, Eshoj O . Refraction and retinopathy in diabetic children below 16 years of age. Acta Ophthalmol 1994; 72: 674–677.
Joner G, Brinchmann-Hansen O, Torres CG, Hanssen KF . A nationwide cross-sectional study of retinopathy and microalbuminuria in young Norwegian type I (insulin-dependent) diabetic patients. Diabetologia 1992; 35: 1049–1054.
Kadiki OA, Roaed RB . Epidemiological and clinical patterns of diabetes mellitus in Benghazi, Libyan Arab Jamahiriya. Eastern Med Health J 1999; 5: 6–13.
Kahn HA, Bradley RF . Prevalence of diabetic retinopathy. Age, sex, and duration of diabetes. Br J Ophthalmol 1975; 59: 345–349.
Kahn HA, Leibowitz HM, Ganley JP, Kini MM, Colton TC, Nickerson RS et al. The Framingham Eye Study I. Outline and major prevalence findings. Am J Epidemiol 1977; 106: 17–32.
Kahn HA, Milton RC . Revised Framingham Eye Study — prevalence of glaucoma and diabetic retinopathy. Am J Epidemiol 1980; 111: 769–776.
Kalk WJ, Joannou J, Ntsepo S, Mahomed I, Mahanlal P, Becker PJ et al. Ethnic differences in the clinical and laboratory associations with retinopathy in adult onset diabetes: studies in patients of African, European and Indian origins. J Intern Med 1997; 241: 31–37.
Kernell A, Dedorsson I, Johansson B, Wickstrom CP, Ludvigsson J, Tuvemo T . Prevalence of diabetic retinopathy in children and adolescents with IDDM. A population-based multicentre study. Diabetologia 1997; 40: 307–310.
Khoo DH, Tan KT, Yeo KT, Chew W, Yong V, Tan YT . Diabetic retinopathy — results of a two year screening programme in two medical units in Singapore. Ann Acad Med Singapore 1990; 19: 484–488.
Klein R, Davis MD, Moss SE, Klein BE, DeMets DL . The Wisconsin Epidemiologic Study of Diabetic Retinopathy. A comparison of retinopathy in younger and older onset diabetic persons. Adv Exp Med Biol 1985; 189: 321–335.
Klein R, Klein BE, Moss SE, Davis MD, DeMets DL . The Wisconsin Epidemiologic Study of Diabetic Retinopathy IV. Diabetic macular edema. Ophthalmology 1984; 91: 1464–1474.
Klein R, Klein BE, Moss SE, Davis MD, DeMets DL . Retinopathy in young-onset diabetic patients. Diabetes Care 1985; 8: 311–315.
Klein R, Klein BE, Moss SE, Linton KL . The Beaver Dam Eye Study. Retinopathy in adults with newly discovered and previously diagnosed diabetes mellitus. Ophthalmology 1992; 99: 58–62.
Klein R, Klein BE, Moss SE . A population-based study of diabetic retinopathy in insulin-using patients diagnosed before 30 years of age. Diabetes Care 1985; 8 (Suppl 1): 71–76.
Klein R, Klein BE, Moss SE . Epidemiology of proliferative diabetic retinopathy. Diabetes Care 1992; 15: 1875–1891.
Klein R, Palta M, Allen C, Shen G, Han DP, D'Alessio DJ . Incidence of retinopathy and associated risk factors from time of diagnosis of insulin-dependent diabetes. Arch Ophthalmol 1997; 115: 351–356.
Klein R . Retinopathy in a population-based study. Trans Am Ophthalmol Soc 1992; 90: 561–594.
Knuiman MW, Welborn TA, McCann VJ, Stanton KG, Constable IJ . Prevalence of diabetic complications in relation to risk factors. Diabetes 1986; 35: 1332–1339.
Kohner EM, Aldington SJ, Stratton IM, Manley SE, Holman RR, Matthews DR et al. United Kingdom Prospective Diabetes Study 30: diabetic retinopathy at diagnosis of non-insulin-dependent diabetes mellitus and associated risk factors. Arch Ophthalmol 1998; 116: 297–303.
Kokkonen J, Laatikainen L, van Dickhoff K, Miettinen R, Tuominen M, Lautala P . Ocular complications in young adults with insulin-dependent diabetes mellitus since childhood. Acta Paediatr 1994; 83: 273–278.
Kostraba JN, Klein R, Dorman JS, Becker DJ, Drash AL, Maser Re et al. The epidemiology of diabetes complications study. IV. Correlates of diabetic background and proliferative retinopathy. Am J Epidemiol 1991; 133: 381–391.
Kravchenko VI, Tronko ND, Pankiv VI, Venzilovich YM, Prudius FG . Prevalence of diabetes mellitus and its complications in the Ukraine. Diabetes Res Clin Pract 1996; 34 (Suppl): S73–S78.
Kuiv R, Tein P, Algvere PV, Backlund LB, Holm O . Photographic detection of retinopathy in insulin-treated diabetes. A population study in the city of Tartu, Estonia. Acta Ophthalmol Scand 1997; 75: 447–456.
Kuzuya T, Akanuma Y, Akazawa Y, Uehata T . Prevalence of chronic complications in Japanese diabetic patients. Diabetes Res Clin Pract 1994; 24 (Suppl): S159–S164.
Larsson LI, Alm A, Bergenheim T, Lithner F, Bergstrom R . Retinopathy in diabetic patients aged 15–50 years in the county of Umea, Sweden. Acta Ophthalmol Scand 1999; 77: 430–436.
Leese GP, Ahmed S, Newton RW, Jung RT, Ellingford A, Baines P et al. Use of mobile screening unit for diabetic retinopathy in rural and urban areas. BMJ 1993; 306: 187–189.
Leske MC, Wu SY, Hyman L, Li X, Hennis A, Connell AM et al. Diabetic retinopathy in a black population: the Barbados Eye Study. Ophthalmology 1999; 106: 1893–1899.
Levitt NS, Adams G, Salmon J, Marks IN, Musson G, Swanepoel C et al. The prevalence and severity of microvascular complications in pancreatic diabetes and IDDM. Diabetes Care 1995; 18: 971–974.
Lundman B, Engstrom L . Diabetes and it's complications in a Swedish county. Diabetes Res Clin Pract 1998; 39: 157–164.
Malone JI, Morrison AD, Pavan PR, Cuthbertson DD . Prevalence and significance of retinopathy in subjects with type I diabetes of less than 5 years' duration screened for the Diabetes Control and Complications Trial. Diabetes Care 2001; 24: 522–526.
McKay R, McCarty CA, Taylor HR . Diabetic retinopathy in Victoria, Australia: the Visual Impairment Project. Br J Ophthalmol 2000; 84: 865–870.
McLeod BK, Thompson JR, Rosenthal AR . The prevalence of retinopathy in the insulin-requiring diabetic patients of an English country town. Eye 1988; 2: 424–430.
Mitchell P, Smith W, Wang JJ, Attebo K . Prevalence of diabetic retinopathy in an older community. The Blue Mountains Eye Study. Ophthalmology 1998; 105: 406–411.
Mitchell P . The prevalence of diabetic retinopathy: a study of 1300 diabetics from Newcastle and the Hunter Valley. Aust J Ophthalmol 1980; 8: 241–246.
Mohan V, Vijayaprabha R, Rema M . Vascular complications in long-term south Indian NIDDM of over 25 years' duration. Diabetes Res Clin Pract 1996; 31: 133–140.
Morgan CL, Currie CJ, Stott NCH, Smithers M, Butler CC, Peters JR . The prevalence of multiple diabetes-related complications. Diabetic Med 2000; 17: 146–151.
Moriarty BJ, Dunn DT, Moriarty AP . Diabetic maculopathy in a Jamaican population. Int Ophthalmol 1989; 13: 301–303.
Moss SE, Klein R, Klein BE . Alcohol consumption and the prevalence of diabetic retinopathy. Ophthalmology 1992; 99: 926–932.
Nagi DK, Pettitt DJ, Bennett PH, Klein R, Knowler WC . Diabetic retinopathy assessed by fundus photography in Pima Indians with impaired glucose tolerance and NIDDM. Diabetic Med 1997; 14: 449–456.
Nakagami T, Kawahara R . Glycaemic control and prevention of retinopathy in Japanese NIDDM patients. A 10-year follow-up study. Diabetes Care 1997; 20: 621–622.
Newell SW, Tolbert B, Bennett J, Parsley TL . The prevalence and risk of diabetic retinopathy among Indians of southwest Oklahoma. J Oklahoma State Med Assoc 1989; 82: 414–424.
Nielsen NV, Ditzel J . Prevalence of macro- and microvascular disease as related to glycosylated hemoglobin in type I and II diabetic subjects. An epidemiologic study in Denmark. Horm Metab Res Suppl 1985; 15: 19–23.
Norymberg C, Shenkman L . Prevalence of overt diabetic nephropathy in patients with non insulin-dependent diabetes mellitus. Isr J Med Sci 1991; 27: 124–130.
Nwosu SN . Low vision in Nigerians with diabetes mellitus. Doc Ophthalmol 2000; 101: 51–57.
Nwosu SN . Prevalence and pattern of retinal diseases at the Guinness Eye Hospital, Onitsha, Nigeria. Ophthalmic Epidemiol 2000; 7: 41–48.
Olsen BS, Johannesen J, Sjolie AK, Borch-Johnsen K, Hougarrdss P, Thorsteinsson B et al. Metabolic control and prevalence of microvascular complications in young Danish patients with type I diabetes mellitus. Danish Study Group of Diabetes in Childhood. Diabetic Med 1999; 16: 79–85.
Parving HH, Hommel E, Mathiesen E, Skott P, Edsberg B, Bahnsen M et al. Prevalence of microalbuminuria, arterial hypertension, retinopathy and neuropathy in patients with insulin dependent diabetes. Br Med J Clin Res Ed 1988; 296: 156–160.
Patel KL, Mhetras SB, Varthakavi PK, Merchant PC, Nihalani KD . Microalbuminuria in non-insulin dependent diabetes mellitus. J Assoc Physicians India 1999; 47: 596–601.
Pinto-Figueiredo L, Moita J, Genro V, Vinagre M, Laires R, Rosa MJ et al. Diabetic retinopathy in a population of 1,302 insulin dependent diabetics (IDDM) diagnosed before 30 years of age. Int Ophthalmol 1992; 16: 429–437.
Pisu E, Vitelli F, Coggi G, Franzone M, Cavallo M, Chiara E et al. Univariate and multivariate analysis of associated factors of retinopathy in 894 Italian adult diabetics. Diabete Metab 1988; 14: 700–705.
Raheja B, Barua J, Jain S, Phatak R . Prevalence of diabetic retinopathy in Indian subjects with NIDDM. J Med Assoc Thailand 1987; 70 (Suppl 2): 135–138.
Rajala U, Laakso M, Qiao Q, Keinanen-Kiukaanniemi S . Prevalence of retinopathy in people with diabetes, impaired glucose tolerance, and normal glucose tolerance. Diabetes Care 1998; 21: 1664–1669.
Ramachandran A, Snehalatha C, Sasikala R, Satyavani K, Vijay V . Vascular complications in young Asian Indian patients with type I diabetes mellitus. Diabetes Res Clin Pract 2000; 48: 51–56.
Ramachandran A, Snehalatha C, Satyavani K, Latha E, Sasikala R, Vijay V . Prevalence of vascular complications and their risk factors in type 2 diabetes. J Assoc Physicians India 1999; 47: 1152–1156.
Ramachandran A, Snehalatha C, Vijay V, Viswanathan M . Diabetic retinopathy at the time of diagnosis of NIDDM in south Indian subjects. Diabetes Res Clin Pract 1996; 32: 111–114.
Rate RG, Knowler WC, Morse HG, Bonnell MD, McVey J, Chervenak CL et al. Diabetes mellitus in Hopi and Navajo Indians. Prevalence of microvascular complications. Diabetes 1983; 32: 894–899.
Rema M, Deepa R, Mohan V . Prevalence of retinopathy at diagnosis among type 2 diabetic patients attending a diabetic centre in South India. Br J Ophthalmol 2000; 84: 1058–1060.
Rema M, Ponnaiya M, Mohan V . Prevalence of retinopathy in non insulin dependent diabetes mellitus at a diabetes centre in southern India. Diabetes Res Clin Pract 1996; 34: 29–36.
Reuterving CO, Kratholm J, Wachtmeister L . Ophthalmic health care in diabetes mellitus: a cross-sectional study in northern Sweden. Ophthal Epidemiol 1999; 6: 267–278.
Rolfe M . Diabetic eye disease in Central Africa. Diabetologia 1998; 31: 88–92.
Roy MS . Diabetic retinopathy in African Americans with type I diabetes: the New Jersey 725: I. Methodology, population, frequency of retinopathy, and visual impairment. Arch Ophthalmol 2000; 118: 97–104.
Samanta A, Burden AC, Jagger C . A comparison of the clinical features and vascular complications of diabetes between migrant Asians and Caucasians in Leicester, UK. Diabetes Res Clin Pract 1991; 14: 205–213.
Schleiffer T, Holken H, Brass H . Morbidity in 565 type 2 diabetic patients according to stage of nephropathy. J Diabetes Complicat 1998; 12: 103–109.
Schranz AG, Villalpando EG, Villalpando CG, Perez BA, Stern MP . The epidemiology of diabetes in Malta. Diabetes Metab Rev 1997; 13: 181–199.
Segal P, Treister G, Yalon M, Sandak R, Berezin M, Modan M . The prevalence of diabetic retinopathy: effect of sex, age, duration of disease and mode of therapy. Diabetes Care 1983; 6: 149–151.
Segato T, Midena E, Grigoletto F, Zucchetto M, Fedele D, Piermarocchi S et al. The epidemiology and prevalence of diabetic retinopathy in the Veneto region of north east Italy. Veneto Group for Diabetic Retinopathy. Diabetic Med 1991; 8: S11–S66.
Sobngwi E, Mbanya KB, Moukouri EN, Ngu KB . Microalbuminuria and retinopathy in a diabetic population of Cameroon. Diabetes Res Clin Pract 1999; 44: 191–196.
Sparrow JM, McLeod BK, Smith TD, Birch MK, Rosenthal AR . The prevalence of diabetic retinopathy and maculopathy and their risk factors in the non-insulin-treated diabetic patients of an English town. Eye 1993; 7: 158–163.
Sprafka JM, Fritsche TL, Baker R, Kurth D, Whipple D . Prevalence of undiagnosed eye disease in high-risk diabetic individuals. Arch Intern Med 1990; 150: 857–861.
Suzuki K, Watanabe K, Motegi T, Kajinuma H . High prevalence of proliferative retinopathy in diabetic patients with low pancreatic B-cell capacity. Diabetes Res Clin Pract 1989; 6: 45–52.
Tabak AG, Tamas G, Zgibor J, Wilson R, Becker D, Kerenyi Z et al. Targets and reality: a comparison of health care indicators in the U.S. (Pittsburgh Epidemiology of Diabetes Complications Study) and Hungary (DiabCare Hungary). Diabetes Care 2000; 23: 1284–1289.
Telmer S, Christiansen JS, Andersen AR, Nerup J, Deckert T . Smoking habits and prevalence of clinical diabetic microangiopathy in insulin-dependent diabetics. Acta Med Scand 1984; 215: 63–68.
Toeller M, Buyken AE, Heitkamp G, Berg G, Scherbaum WA . Prevalence of chronic complications, metabolic control and nutritional intake in type I diabetes: comparison between different European regions. EURODIAB Complications Study group. Horm Metab Res 1999; 31: 680–685.
Verhoeven S, van Ballegooie E, Casparie AF . Impact of late complications in type 2 diabetes in a Dutch population. Diabetic Med 1991; 8: 435–438.
Wan Nazaimoon WM, Letchuman R, Noraini N, Ropilah AR, Zainal M, Ismail I et al. Systolic hypertension and duration of diabetes mellitus are important determinants of retinopathy and microalbuminuria in young diabetics. Diabetes Res Clin Pract 1999; 46: 213–221.
Wang WQ, Ip TP, Lam KS . Changing prevalence of retinopathy in newly diagnosed non-insulin dependent diabetes mellitus patients in Hong Kong. Diabetes Res Clin Pract 1998; 39: 185–191.
Wat N, Michon J, Lam KS . High prevalence of retinopathy among type 2 diabetic patients with no visual complaint. Aust N Z J Med 1998; 28: 459–461.
Weerasuriya N, Siribaddana S, Dissanayake A, Subasinghe Z, Wariyapola D, Fernando DJ . Long-term complications in newly diagnosed Sri Lankan patients with type 2 diabetes mellitus. Q J Med 1998; 91: 439–443.
West SK, Klein R, Rodriguez J, Munoz B, Broman AT, Sanchez R et al. Diabetes and diabetic retinopathy in a Mexican-American population. Diabetes Care 2001; 24: 1204–1209.
Williams AS, Sobngwi E, Mbanya JC, Moukouri EN, Ngu KB . Visual impairment with diabetes: estimates of lower and upper limits of prevalence in the United States. Diabetes Educator 1999; 25: 23–24.
Wirta OR, Pasternack AI, Oksa HH, Mustonen JT, Koivula TA, Helin HJ et al. Occurrence of late specific complications in type 2 (non-insulin-dependent) diabetes mellitus. J Diabetes Complicat 1995; 9: 177–185.
Yokoyama H, Okudaira M, Otani T, Takaike H, Miura J, Saeki A et al. Existence of early-onset NIDDM Japanese demonstrating severe diabetic complications. Diabetes Care 1997; 20: 844–847.
Zainal M, Masran L, Ropilah AR . Blindness and visual impairment amongst rural Malays in Kuala Selangor, Selangor. Med J Malaysia 1998; 53: 46–50.
Zander E, Seidlein I, Herfurth S, Heinke P, Chlup R, Badendick K et al. Increased prevalence of proliferative retinopathy and cardiovascular autonomic dysfunction in IDDM patients with proteinuria. Exp Clin Endocrinol 1992; 99: 102–107.
Ramachandran A, Snehalatha C, Vijay V, Viswanathan M . Diabetic retinopathy at the time of diagnosis of NIDDM in south Indian subjects. Diabetes Res Clin Pract 1996; 32: 111–114.
Klein R . The epidemiology of diabetic retinopathy: findings from the Wisconsin Epidemiologic Study of Diabetic Retinopathy. Int Ophthalmol Clin 1987; 27: 230–238.
Malone JI, Morrison AD, Pavan PR, Cuthbertson DD, The Diabetic Control Complications Trial. Prevalence and significance of retinopathy in subjects with type I diabetes of less than 5 years' duration screened for the diabetes control and complications trial. Diabetes Care 2001; 24: 522–526.
Klein R, Klein BEK, Moss SE, Cruickshanks KJ . The Wisconsin Epidemiological Study of Diabetic Retinopathy: XVII. The 14-year incidence and progression of diabetic retinopathy and associated risk factors in type I diabetes. Ophthalmology 1998; 105: 1801–1815.
Agardh CD, Agardh E, Torffvit O . The association between retinopathy, nephropathy, cardiovascular disease and long-term metabolic control in type I diabetes mellitus: a 5 year follow-up study of 442 adult patients in routine care. Diabetes Res Clin Pract 1997; 35: 113–121.
Agardh E, Agardh CD, Hansson-Lundblad C . The five-year incidence of blindness after introducing a screening programme for early detection of treatable diabetic retinopathy. Diabetic Med 1993; 10: 555–559.
Agardh E, Agardh CD, Koul S, Torffvit O . A four-year follow-up study on the incidence of diabetic retinopathy in older onset diabetes mellitus. Diabetic Med 1994; 11: 273–278.
Agardh E, Agardh C-D, Torffvit O . A 5-year follow-up study on the incidence of retinopathy in type I diabetes mellitus in relation to medical risk. J Intern Med 1994; 235: 353–358.
Arfken CL, Salicrup AE, Meuer SM, Del Priore V, Klein R, McGill JB et al. Retinopathy in African Americans and Whites with insulin-dependent diabetes melitus. Arch Intern Med 1994; 154: 2597–2602.
Axer-Siegel R, Hod M, Fink-Cohen S, Kramer M, Weinberger D, Schindel B et al. Diabetic retinopathy during pregnancy. Ophthalmology 1996; 103: 1815–1819.
Backlund LB, Algvere PV, Rosenqvist U . New blindness in diabetes reduced by more than one-third in Stockholm County. Diabetic Med 1997; 14: 732–740.
Bojestig M, Arnqvist HJ, Karlberg BE, Ludvigsson J . Unchanged incidence of severe retinopathy in a population of type I diabetic patients with marked reduction of nephropathy. Diabetic Med 1998; 15: 863–869.
Burger W, Hovener G, Dusterhus R, Hartmann R, Weber B . Prevalence and development of retinopathy in children and adolescents with type I (insulin-dependent) diabetes mellitus. A longitudinal study. Diabetologia 1986; 29: 17–22.
Chaturvedi N, Sjoelie AK, Porta M, Aldington SJ, Fuller JH, Songini M . The EURODIAB Prospective Complications Study. Markers of insulin resistance are strong risk factors for retinopathy incidence in type I diabetes. Diabetes Care 2001; 24: 284–289.
Chen MS, Kao CS, Fu CC, Chen CJ, Tai TY . Incidence and progression of diabetic retinopathy among non-insulin-dependent diabetic subjects: a 4-year follow-up. Int J Epidemiol 1995; 24: 787–795.
Cohen DL, Neil HA, Thorogood M, Mann JI . A population-based study of the incidence of complications associated with type 2 diabetes in the elderly. Diabetic Med 1991; 8: 928–933.
Cormack TG, Grant B, Macdonald MJ, Steel J, Campbell IW . Incidence of blindness due to diabetic eye disease in Fife 1990–9. Br J Ophthalmol 2001; 85: 354–356.
DCCT. The effect of intensive treatment of diabetes on the development and progression of long-term complications in insulin-dependent diabetes mellitus. N Engl J Med 1993; 329: 977–986.
Dibble CM, Kochenour NK, Worley RJ, Tyler FH, Swartz M . Effect of pregnancy on diabetic retinopathy. Obstet Gynecol 1982; 59: 699–704.
Dwyer MS, Melton III LJ, Ballard DJ . Incidence of diabetic retinopathy and blindness: a population-based study in Rochester, Minnesota. Diabetes Care 1985; 8: 316–322.
Flack A, Kaar ML, Laatikainen L . A prospective, longitudinal study examining the development of retinopathy in children with diabetes. Acta Paediatr 1996; 85: 313–319.
Gomes MB, Dorigo D, Silva Jr GR, Goncalves MF, Neves R . Prospective study of development of microalbuminuria and retinopathy in Brazilian IDDM patients. Acta Diabetol 2000; 37: 19–25.
Guillausseau PJ, Massin P, Charles MA, Allaguy H, Guvenli Z, Virally M . Glycaemic control and development of retinopathy in type 2 diabetes mellitus: a longitudinal study. Diabetic Med 1998; 15: 151–155.
Herse P, Gothwal VK . Survey of visual impairment in an Indian tertiary eye hospital. Indian J Ophthalmol 1997; 45: 189–193.
Icks A, Trautner C, Haastert B, Berger M, Giani G . Blindness due to diabetes: population-based age- and sex-specific incidence rates. Diabetic Med 1997; 14: 571–575.
Ito C, Maeda R, Ishida S, Harada H, Inoue N, Sasaki H . Importance of OGTT for diagnosing diabetes mellitus based on prevalence and incidence of retinopathy. Diabetes Res Clin Pract 2000; 49: 181–186.
Janghorbani M, Jones RB, Allison SP . Incidence of and risk factors for proliferative retinopathy and its association with blindness among diabetes clinic attenders. Ophthalmic Epidemiol 2000; 7: 225–241.
Kalter-Leibovici O, Leibovici L, Loya N, Kremer I, Axer-Siegel R, Karp M et al. The development and progression of diabetic retinopathy in type I diabetic patients: a cohort study. Diabetic Med 1997; 14: 858–866.
Kim HK, Kim CH, Kim SW, Park JY, Hong SK, Yoon YH et al. Development and progression of diabetic retinopathy in Koreans with NIDDM. Diabetes Care 1998; 21: 134–138.
Kitamura Y, Suto C, Funatsu H, Hori S, Totani R . The incidence of diabetic ocular complications. Folia Ophthalmol Jpn 1993; 44: 729–735.
Klein BE, Davis MD, Segal P, Long JA, Harris WA, Haug GA et al. Diabetic retinopathy. Assessment of severity and progression. Ophthalmology 1984; 91: 10–17.
Klein BE, Klein R, Moss SE, Palta M . A cohort study of the relationship of diabetic retinopathy to blood pressure. Arch Ophthalmol 1995; 113: 601–606.
Klein R, Klein BE, Jensen SC, Moss SE . The relation of socioeconomic factors to the incidence of proliferative diabetic retinopathy and loss of vision. Ophthalmology 1994; 101: 68–76.
Klein R, Klein BE, Moss SE, Cruickshanks KJ . Relationship of hyperglycemia to the long-term incidence and progression of diabetic retinopathy. Arch Intern Med 1994; 154: 2169–2178.
Klein R, Klein BE, Moss SE, Cruickshanks KJ . The Wisconsin Epidemiologic Study of Diabetic Retinopathy. XIV. Ten-year incidence and progression of diabetic retinopathy. Arch Ophthalmol 1994; 112: 1217–1228.
Klein R, Klein BE, Moss SE, Davis MD, DeMets DL . Glycosylated hemoglobin predicts the incidence and progression of diabetic retinopathy. JAMA 1988; 260: 2864–2871.
Klein R, Klein BE, Moss SE, Davis MD, DeMets DL . Is blood pressure a predictor of the incidence or progression of diabetic retinopathy? Arch Intern Med 1989; 149: 2427–2432.
Klein R, Klein BE, Moss SE, Davis MD, DeMets DL . The Wisconsin Epidemiologic Study of Diabetic Retinopathy. IX. Four-year incidence and progression of diabetic retinopathy when age at diagnosis is less than 30 years. Arch Ophthalmol 1989; 107: 237–243.
Klein R, Klein BE, Moss SE, Davis MD, DeMets DL . The Wisconsin Epidemiologic Study of Diabetic Retinopathy. X. Four-year incidence and progression of diabetic retinopathy when age at diagnosis is 30 years or more. Arch Ophthalmol 1989; 107: 244–249.
Klein R, Klein BE, Moss SE . How many steps of progression of diabetic retinopathy are meaningful? The Wisconsin Epidemiologic Study of Diabetic Retinopathy. 5. Arch Ophthalmol 2001; 119: 547–553.
Klein R, Klein BE, Moss SE . Is obesity related to microvascular and macrovascular complications in diabetes? The Wisconsin Epidemiologic Study of Diabetic Retinopathy. Arch Intern Med 1997; 157: 650–656.
Klein R, Klein BE, Moss SE . Relation of glycemic control to diabetic microvascular complications in diabetes mellitus. Ann Int Med 1996; 124: 90–96.
Klein R, Klein BE, Moss SE . The Wisconsin Epidemiologic Study of Diabetic Retinopathy. XVI. The relationship of C-peptide to the incidence and progression of diabetic retinopathy. Diabetes 1995; 44: 796–801.
Klein R, Klein BE, Moss SE . The Wisconsin epidemiologic study of diabetic retinopathy: an update. Aust NZ J Ophthalmol 1990; 18: 19–22.
Klein R, Moss SE, Klein BE, Davis MD, DeMets DL . The Wisconsin epidemiologic study of diabetic retinopathy. XI. The incidence of macular edema. Ophthalmology 1989; 96: 1501–1510.
Knowler WC, Bennett PH, Ballintine EJ . Increased incidence of retinopathy in diabetics with elevated blood pressure. A six-year follow-up study in Pima Indians. N Engl J Med 1980; 302: 645–650.
Kofoed-Enevoldsen A, Jensen T, Borch-Johnsen K, Deckert T . Incidence of retinopathy in type I (insulin-dependent) diabetes: association with clinical nephropathy. J Diabetes Complicat 1987; 1: 96–99.
Kohner EM, Stratton IM, Aldington SJ, Holman RR, Matthews DR, the UK Prospective Diabetes Study (UKPDS) Group. Relationship between the severity of retinopathy and progression to photocoagulation in patients with type 2 diabetes mellitus in the UKPDS (UKPDS 52). Diabetic Med 2001; 18: 178–184.
Kristinsson JK, Hauksdottir H, Stefansson E, Jonasson F, Gislason I . Active prevention in diabetic eye disease. A 4-year follow-up. Acta Ophthalmol Scand 1997; 75: 249–254.
Lee ET, Lee VS, Kingsley RM, Lu M, Russell D, Asal NR . Diabetic retinopathy in Oklahoma Indians with NIDDM. Incidence and risk factors. Diabetes Care 1992; 15: 1620–1627.
Lloyd CE, Klein R, Maser RE, Kuller LH, Becker DJ, Orchard TJ . The progression of retinopathy over 2 years: the Pittsburgh Epidemiology of Diabetes Complications (EDC) Study. J Diabetes Complicat 1995; 9: 140–148.
Lloyd CE, Orchard TJ, Lovestam-Adrian M, Agardh E, Agardh CD . The prevalence of complications of insulin-dependent diabetes mellitus in the United States — the temporal development of retinopathy and nephropathy in type I diabetes mellitus during 15 years diabetes duration. Practical Diabetes 1992; 9: 171–173.
Mitchell P, Moffitt P . Update and implications from the Newcastle diabetic retinopathy study. Aust N Z J Ophthalmol 1990; 18: 13–17.
Mitchell P . Development and progression of diabetic eye disease in Newcastle (1977–1984): rates and risk factors. Aust N Z J Ophthalmol 1985; 13: 39–44.
Moss SE, Klein R, Klein BE . Cigarette smoking and ten-year progression of diabetic retinopathy. Ophthalmology 1996; 103: 1438–1442.
Moss SE, Klein R, Klein BE . Ocular factors in the incidence and progression of diabetic retinopathy. Ophthalmology 1994; 101: 77–83.
Moss SE, Klein R, Klein BE . Ten-year incidence of visual loss in a diabetic population. Ophthalmology 1994; 101: 1061–1070.
Moss SE, Klein R, Klein BE . The 14-year incidence of visual loss in a diabetic population. Ophthalmology 1998; 105: 998–1003.
Moss SE, Klein R, Klein BE . The association of alcohol consumption with the incidence and progression of diabetic retinopathy. Ophthalmology 1994; 101: 1962–1968.
Moss SE, Klein R, Klein BE . The incidence of vision loss in a diabetic population. Ophthalmology 1988; 95: 1340–1348.
Nelson RG, Wolfe JA, Horton MB, Pettitt DJ, Bennett PH, Knowler WC . Proliferative retinopathy in NIDDM. Incidence and risk factors in Pima Indians. Diabetes 1989; 38: 435–440.
Nielsen NV . Diabetic retinopathy I. The course of retinopathy in insulin-treated diabetics. A one year epidemiological cohort study of diabetes mellitus. The Island of Falster, Denmark. Acta Ophthalmol 1984; 62: 256–265.
Okudaira M, Yokoyama H, Otani T, Uchigata Y, Iwamoto Y . Slightly elevated blood pressure as well as poor metabolic control are risk factors for the progression of retinopathy in early-onset Japanese type 2 diabetes. J Diabetes Complicat 2000; 14: 281–287.
Porta M, Tomalino MG, Santoro F, Ghigo LD, Cairo M, Aimone M . Diabetic retinopathy as a cause of blindness in the province of Turin, north-west Italy, in 1967–1991. Diabetic Med 1995; 12: 355–361.
Rith-Najarian SJ, Valway SE, Gohdes DM . Diabetes in a northern Minnesota Chippewa Tribe. Prevalence and incidence of diabetes and incidence of major complications, 1986–1988. Diabetes Care 1993; 16: 266–270.
Rossing K, Jacobsen P, Rossing P, Lauritzen E, Lund-Andersen H, Parving HH . Improved visual function in IDDM patients with unchanged cumulative incidence of sight-threatening diabetic retinopathy. Diabetes Care 1998; 21: 2007–2015.
Sasaki A, Horiuchi N, Hasewgawa K, Uehara M . Development of diabetic retinopathy and its associated risk factors in type 2 diabetic patients in Osaka district, Japan: a long-term prospective study. Diabetes Res Clin Pract 1990; 10: 257–263.
Stratton IM, Kohner EM, Aldington SJ, Turner RC, Holman RR, Manley SE et al. UKPDS 50: risk factors for incidence and progression of retinopathy in type 2 diabetes over 6 years from diagnosis. Diabetologia 2001; 44: 156–163.
Tudor SM, Hamman RF, Baron A, Johnson DW, Shetterly SM . Incidence and progression of diabetic retinopathy in Hispanics and non-Hispanic whites with type 2 diabetes. San Luis Valley Diabetes Study, Colorado. Diabetes Care 1998; 21: 53–61.
Wang Q, Dills DG, Klein R, Klein BE, Moss SE . Does insulin-like growth factor I predict incidence and progression of diabetic retinopathy? Diabetes 1995; 44: 161–164.
Yanko L, Goldbourt U, Michaelson IC, Shapiro A, Yaari S . Prevalence and 15-year incidence of retinopathy and associated characteristics in middle-aged and elderly diabetic men. Br J Ophthalmol 1983; 67: 759–765.
Yokoyama H, Uchigata Y, Otani T, Aoki K, Maruyama A, Maruyama H . Development of proliferative retinopathy in Japanese patients with IDDM: Tokyo Women's Medical College Epidemiologic Study. Diabetes Res Clin Pract 1994; 24: 113–119.
ETDRS. Photocoagulation for diabetic macular edema. Early Treatment Diabetic Retinopathy Study report number 1. Early Treatment Diabetic Retinopathy Study research group. Arch Ophthalmol 1985; 103: 1796–1806.
Hipwell JH, Strachan F, Olson JA, McHardy KC, Sharp PF, Forrester JV . Automated detection of microaneurysms in digital red-free photographs: a diabetic retinopathy screening tool. Diabetic Med 2000; 17: 588–594.
Bailey CC, Sparrow JM, Grey RH, Cheng H . The National Diabetic Retinopathy Laser Treatment Audit. III. Clinical outcomes. Eye 1999; 13: 151–159.
DCCT. The effect of intensive diabetes treatment on the progression of diabetic retinopathy in insulin-dependent diabetes mellitus. Arch Ophthalmol 1995; 113: 36–51.
Bachmann MO, Nelson SJ . Impact of diabetic retinopathy screening on a British district population: case detection and blindness prevention in an evidence-based model. J Epidemiol Community Health 1998; 52: 45–52.
Schoenfeld ER, Greene JM, Wu SY, Leske MC . Patterns of adherence to diabetes vision care guidelines: baseline findings from the Diabetic Retinopathy Awareness Program. Ophthalmology 2001; 108: 563–571.
Moss SE, Klein R, Klein BE . Factors associated with having eye examinations in persons with diabetes. Arch Fam Med 1995; 4: 529–534.
Legorreta AP, Hasan MM, Peters AL, Pelletier KR, Leung KM . An intervention for enhancing compliance with screening recommendations for diabetic retinopathy. A bicoastal experience. Diabetes Care 1997; 20: 520–523.
McCarty CA, Taylor KI, McKay R, Keeffe JE . Diabetic retinopathy: effects of national guidelines on the referral, examination and treatment practices of ophthalmologists and optometrists. Clin Exp Ophthalmol 2001; 29: 52–58.
Bailey CJ . Potential new treatments for type 2 diabetes. Trends Pharmacol Sci 2000; 21: 259–265.
Cunha-Vaz J . Lowering the risk of visual impairment and blindness. Diabetic Med 1998; 15 (Suppl 4): S47–S50.
Flynn Jr HW, Chew EY, Simons BD, Barton FB, Remaley NA, Ferris III FL . Pars plana vitrectomy in the Early Treatment Diabetic Retinopathy Study. ETDRS report number 17. The Early Treatment Diabetic Retinopathy Study Research Group. Ophthalmology 1992; 99: 1351–1357.
Emanuele N, Klein R, Abraira C, Colwell J, Comstock J, Henderson WG et al. Evaluations of retinopathy in the VA Cooperative Study on Glycemic Control and Complications in Type 2 Diabetes (VA CSDM). A feasibility study. Diabetes Care 1996; 19: 1375–1381.
Tomlinson DR . Mitogen-activated protein kinases as glucose transducers for diabetic complications. Diabetologia 1999; 42: 1271–1281.
Frank RN . Potential new medical therapies for diabetic retinopathy: protein kinase C inhibitors. Am J Ophthalmol 2002; 133: 693–698.
Ways K, King G, Aiello L . Amelioration of retinal hemodynamic dysfunction using a protein kinase C-beta inhibitor in patients with diabetes. 35th Annual Meeting of the European Association for the Study of Diabetes, 28 September–02 October 1999, Brussels, Belgium.
Acknowledgements
We thank Iris Gordon (who provided expert advice on development of electronic search strategies) and Katy Nocher (for assistance with literature hand searching). The review was built on the previous work of TK-M and Peter Hudson. The support of Jessamy Watkins and Alan Oglesby is gratefully acknowledged. The review was supported by a grant from Lilly.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Williams, R., Airey, M., Baxter, H. et al. Epidemiology of diabetic retinopathy and macular oedema: a systematic review. Eye 18, 963–983 (2004). https://doi.org/10.1038/sj.eye.6701476
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.eye.6701476