Abstract
BACKGROUND:
Variation in care and outcomes of very low birth weight infants (VLBW) in neonatal intensive care units (NICU) has been widely reported in the past decade. Less is known about care provided to healthy premature infants born between 30 and 35 weeks gestational age (GA). We have previously reported inter-NICU variation in discharge (D/C) timing and achievement of maturational milestones in this population.
OBJECTIVE:
To compare inter-NICU growth outcomes and feeding practices in healthy, moderately premature infants.
METHODS:
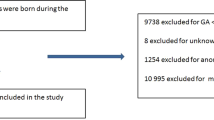
Records of 450 infants, 30 to 35 weeks gestation, without medical or surgical complications, and consecutively discharged from 15 Massachusetts NICUs (nine Level II and six Level III) were reviewed. Final analyses included 382 infants with hospital length of stay >6 days (d).
RESULTS:
GA at birth and birth weight (BW) were 33.2 weeks (SD 1.2) and 2024?g (389). Mean Z-score decreased 0.67z (0.37) from birth to D/C. Weight loss from birth to 7?d averaged 4.0%. Mean growth velocity from 7?d to D/C was 13.3?g/k/d (5.2) with net growth velocity of 5.5?g/k/d (5.6). Mean net growth velocity ranged from 0.1 to 8.4?g/k/d (p<0.001) among study NICUs. Time of initiation, rate of advancement and caloric density of feedings also varied significantly between NICUs.
CONCLUSION:
Mean NICU growth velocity of healthy, moderately premature infants did not achieve in utero growth standards. There was significant inter-NICU variation in growth outcomes and feeding practices. Further study is needed to identify practices associated with better growth in this healthy moderately premature infant population.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Morley R, Lucas A . Randomized diet in the neonatal period and growth performance until 7.5–8?y of age in preterm children. Am J Clin Nutr 2000;71(3):822–828.
Gordon N . Nutrition and cognitive function. Brain Dev 1997;19(3):165–170.
Cooper PA, Rothberg AD, Davies VA, Horn J, Vogelman L . Three year growth and developmental follow-up of very low birth weight infants fed own mother's milk, a premature infant formula, or one of two standard formulas. J Pediatr Gastroenterol Nutr 1989;8(3):348–354.
Georgieff MK, Hoffman JS, Pereira GR, Bernbaum J, Hoffman-Williamson M . Effect of caloric deprivation on head growth and 1 year developmental status in preterm infants. J Pediatr 1985;107(4):581–587.
American Academy of Pediatrics, Committee on Nutrition. Nutritional needs of low birth weight infants. Pediatrics 1985;75:976–986.
Clark RH, Thomas P, Peabody J . Extrauterine growth restriction remains a serious problem in prematurely born neonates. Pediatrics 2003;111:986–990.
Lemons JA, Bauer CR, Oh W, et al. Very low birth weight outcomes of the National Institute of Child Health and Human Development Neonatal Research Network, January 1995 through December 1996. NICHD Neonatal Research Network. Pediatrics 2001;107(1):E1.
Bloom BT, Mulligan J, Arnold C, et al. Improving growth of very low birth weight infants in the first 28 days. Pediatrics 2003;112(1, Part 1):8–14.
Lee SK, McMillan DD, Ohlsson A, et al. Variations in practice and outcomes in the Canadian NICU network: 1996–1997. Pediatrics 2000;106(5):1070–1079.
Horbar JD, Badger GJ, Lewit EM, Rogowski J, Shiono PH . Hospital and patient characteristics associated with variation in 28-day mortality rates for very low birth weight infants. Vermont Oxford Network. Pediatrics 1997;99(2):149–156.
Olsen IE, Richardson DK, Schmid CH, Ausman LM, Dwyer JT . Intersite differences in weight growth velocity of extremely premature infants. Pediatrics 2002;110(6):1125–1132.
Arias E, MacDorman MF, Strobino DM, Guyer B . Annual summary of vital statistics. Pediatrics 2003;112(6):1215–1230.
Kramer MS, Demissie K, Yang H, Platt RW, Sauve R, Liston R . The contribution of mild and moderate preterm birth to infant mortality. Fetal and Infant Health Study Group of the Canadian Perinatal Surveillance System. JAMA 2000;284(7):843–849.
Lee JS, Richardson DK, Clark RH . Postnatal growth of infants 30–34 weeks gestational age: A comparison of 63 neonatal intensive care units (NICUs). Pediatr Res 2001;49(4 pt 2 suppl):358A.
Eichenwald EC, Blackwell M, Lloyd JS, Tran T, Wilker R, Richardson DK . Inter-NICU variation in discharge timing: effects of relationship between apnea and feeding management. Pediatrics. 2001;108(4):928–933.
Brenner WE, Edelman DA, Hendricks CH . A standard of fetal growth for the United States of America. Am J Obstet Gynecol 1976;126(5):555–564.
Tsang R, Lucas A, Uauy R, Zlotkin S, editors. Nutritional Needs of the Preterm Infant. Baltimore, MD: William & Wilkins; 1993.
Embleton NE, Pang N, Cooke RJ . Postnatal nutrition and growth retardation: an inevitable consequence of current recommendations in preterm infants? Pediatrics. 2001;107(2):270–273.
Cooke RJ, Griffin IJ, McCormick K, et al. Feeding preterm infants after hospital discharge: effect of dietary manipulation on nutrient intake and growth. Pediatr Res 1998;43(3):355–360.
Kliethermes PA, Cross ML, Lanese MG, Johnson KM, Simon SD . Transitioning preterm infants with nasogastric tube supplementation: increased likelihood of breastfeeding. J Obstetr Gynecol Neonatal Nurs 1999;28(3):264–273.
Wauben IP, Atkinson SA, Shah JK, Paes B . Growth and body composition of preterm infants: influence of nutrient fortification of mother's milk in hospital and breast-feeding post-hospital discharge. Acta Paediatr 1998;87(7):780–785.
Schanler RJ . Suitability of human milk for the low birth weight infant. Clin Perinatol 1995;22(1):207–222.
Lucas A, King F, Bishop NB . Post-discharge formula consumption in infants born preterm. Arch Dis Child 1992;67(6):691–692.
Acknowledgements
We thank our co-investigators Drs. Tai Tran (Beverly Hospital), Janet S. Lloyd (South Shore Hospital) and Richard Wilker (Newton-Wellesley Hospital). We are grateful for review and advice from Irene Olsen, PhD (Cincinnati Children's Hospital). Special thanks are due to Martin Horowitz, MD (Pediatrics, Harvard Vanguard Medical Associates) for organizing and supporting this project.
Author information
Authors and Affiliations
Additional information
Funding was provided by Harvard Pilgrim Health Care, Neighborhood Health Plan, Tufts Health Plan, Fallon Community Health Plan, and Blue Cross-Blue Shield of Massachusetts.
Rights and permissions
About this article
Cite this article
Blackwell, M., Eichenwald, E., McAlmon, K. et al. Interneonatal Intensive Care Unit Variation in Growth Rates and Feeding Practices in Healthy Moderately Premature Infants. J Perinatol 25, 478–485 (2005). https://doi.org/10.1038/sj.jp.7211302
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.jp.7211302
This article is cited by
-
Early infancy growth, body composition and type of feeding in late and moderate preterms
Pediatric Research (2023)
-
Poor weight gain and its predictors among preterm neonates admitted at Muhimbili National Hospital in Dar-es-salaam, Tanzania: a prospective cohort study
BMC Pediatrics (2021)
-
The efficacy and safety of peripheral intravenous parenteral nutrition vs 10% glucose in preterm infants born 30 to 33 weeks’ gestation: a randomised controlled trial
BMC Pediatrics (2020)
-
Implications of continuity of care on infant caloric intake in the neonatal intensive care unit
Journal of Perinatology (2020)
-
Inadequate oral feeding as a barrier to discharge in moderately preterm infants
Journal of Perinatology (2019)