Abstract
Background/Objectives:
The impact of nutritional status on survival among community-dwelling older adults is unclear. We aimed to investigate the prevalence and association of poor nutritional status, including malnutrition and risk for malnutrition defined by the Mini-Nutritional Assessment-Short Form (MNA-SF) with survival, and to explore the role of relevant biomarkers (hemoglobin, albumin and C-reactive protein) in this association.
Subjects/Methods:
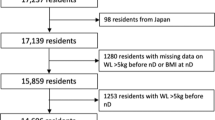
This study included 3041 participants aged ⩾60 in the Swedish National study on Aging and Care-Kungsholmen. On the basis of the total score in MNA-SF, nutritional status for each participant was assessed as normal (score 12–14), risk for malnutrition (8–11) or malnutrition (<8). Over an 11-year follow-up, survival status was observed. Data were analysed using logistic regression, flexible parametric survival and Laplace models.
Results:
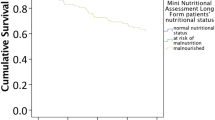
Of all the participants, 51 (1.7%) had malnutrition and 751 (24.7%) were at risk for malnutrition. The multi-adjusted hazard ratio (95% confidence interval) of mortality was 2.40 (1.56−3.67; P<0.001) for malnutrition and 1.49 (1.29−1.71; P<0.001) for risk for malnutrition. The median ages at death of participants with malnutrition and risk for malnutrition were ~3 and 1.5 years shorter than those with normal nutritional status, respectively, whereas malnutrition or risk for malnutrition together with abnormal biomarker (hemoglobin and albumin) levels was related to 1 year more shortened survival.
Conclusions:
Malnutrition and risk for malnutrition are highly prevalent and significantly associated with a shorter survival. Poor nutritional status in combination with abnormalities in the biomarkers is associated with even more shortened survival.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Norman K, Pichard C, Lochs H, Pirlich M . Prognostic impact of disease-related malnutrition. Clin Nutr 2008; 27: 5–15.
Furman EF . Undernutrition in older adults across the continuum of care: nutritional assessment, barriers, and interventions. J Gerontol Nurs 2006; 32: 22–27.
Meijers JM, van Bokhorst-de van der Schueren MA, Schols JM, Soeters PB, Halfens RJ . Defining malnutrition: mission or mission impossible? Nutrition 2010; 26: 432–440.
Wells JL, Dumbrell AC . Nutrition and aging: assessment and treatment of compromised nutritional status in frail elderly patients. Clin Interv Aging 2006; 1: 67–79.
Guigoz Y . The Mini Nutritional Assessment (MNA) review of the literature—What does it tell us? J Nutr Health Aging 2006; 10: 466–485; discussion 485–487.
Kaiser MJ, Bauer JM, Ramsch C, Uter W, Guigoz Y, Cederholm T et al. Frequency of malnutrition in older adults: a multinational perspective using the mini nutritional assessment. J Am Geriatr Soc 2010; 58: 1734–1738.
Sullivan DH . The role of nutrition in increased morbidity and mortality. Clin Geriatr Med 1995; 11: 661–674.
Correia MI, Waitzberg DL . The impact of malnutrition on morbidity, mortality, length of hospital stay and costs evaluated through a multivariate model analysis. Clin Nutr 2003; 22: 235–239.
Persson MD, Brismar KE, Katzarski KS, Nordenstrom J, Cederholm TE . Nutritional status using mini nutritional assessment and subjective global assessment predict mortality in geriatric patients. J Am Geriatr Soc 2002; 50: 1996–2002.
Lundin H, Saaf M, Strender LE, Mollasaraie HA, Salminen H . Mini nutritional assessment and 10-year mortality in free-living elderly women: a prospective cohort study with 10-year follow-up. Eur J Clin Nutr 2012; 66: 1050–1053.
Ferreira LS, do Amaral TF, Marucci Mde F, Nascimento LF, Lebrao ML, Duarte YA . Undernutrition as a major risk factor for death among older Brazilian adults in the community-dwelling setting: SABE survey. Nutrition 2011; 27: 1017–1022.
Kaiser MJ, Bauer JM, Ramsch C, Uter W, Guigoz Y, Cederholm T et al. Validation of the Mini Nutritional Assessment short-form (MNA-SF): a practical tool for identification of nutritional status. J Nutr Health Aging 2009; 13: 782–788.
Lagergren M, Fratiglioni L, Hallberg IR, Berglund J, Elmstahl S, Hagberg B et al. A longitudinal study integrating population, care and social services data. The Swedish National study on Aging and Care (SNAC). Aging Clin Exp Res 2004; 16: 158–168.
Folstein MF, Folstein SE, McHugh PR . 'Mini-mental state'. A practical method for grading the cognitive state of patients for the clinician. J Psychiatr Res 1975; 12: 189–198.
Patel KV . Epidemiology of anemia in older adults. Semin Hematol 2008; 45: 210–217.
Fried LP, Kronmal RA, Newman AB, Bild DE, Mittelmark MB, Polak JF et al. Risk factors for 5-year mortality in older adults: the Cardiovascular Health Study. JAMA 1998; 279: 585–592.
Rubenstein LZ, Harker JO, Salva A, Guigoz Y, Vellas B . Screening for undernutrition in geriatric practice: developing the short-form mini-nutritional assessment (MNA-SF). J Gerontol A Biol Sci Med Sci 2001; 56: M366–M372.
Ludvigsson JF, Otterblad-Olausson P, Pettersson BU, Ekbom A . The Swedish personal identity number: possibilities and pitfalls in healthcare and medical research. Eur J Epidemiol 2009; 24: 659–667.
Bottai M, Zhang J . Laplace regression with censored data. Biom J 2010; 52: 487–503.
Bottai M, Orsini N . A command for Laplace regression. Stata J 2013; 13: 1–13.
Cereda E . Mini nutritional assessment. Curr Opin Clin Nutr Metab Care 2012; 15: 29–41.
Johansson L, Sidenvall B, Malmberg B, Christensson L . Who will become malnourished? A prospective study of factors associated with malnutrition in older persons living at home. J Nutr Health Aging 2009; 13: 855–861.
Serrano-Urrea R, Garcia-Meseguer MJ . Malnutrition in an elderly population without cognitive impairment living in nursing homes in Spain: study of prevalence using the Mini Nutritional Assessment test. Gerontology 2013; 59: 490–498.
Morley JE . Undernutrition in older adults. Fam Pract 2012; 29: i89–i93.
Vandewoude MF, Alish CJ, Sauer AC, Hegazi RA . Malnutrition-sarcopenia syndrome: is this the future of nutrition screening and assessment for older adults? J Aging Res 2012; 2012: 651570.
Rendall MS, Weden MM, Favreault MM, Waldron H . The protective effect of marriage for survival: a review and update. Demography 2011; 48: 481–506.
Cowan DT, Roberts JD, Fitzpatrick JM, While AE, Baldwin J . Nutritional status of older people in long term care settings: current status and future directions. Int J Nurs Stud 2004; 41: 225–237.
Saletti A, Johansson L, Yifter-Lindgren E, Wissing U, Osterberg K, Cederholm T . Nutritional status and a 3-year follow-up in elderly receiving support at home. Gerontology 2005; 51: 192–198.
Soeters PB, Reijven PL, van Bokhorst-de van der Schueren MA, Schols JM, Halfens RJ, Meijers JM et al. A rational approach to nutritional assessment. Clin Nutr 2008; 27: 706–716.
Fuhrman MP . The albumin-nutrition connection: separating myth from fact. Nutrition 2002; 18: 199–200.
Fuhrman MP, Charney P, Mueller CM . Hepatic proteins and nutrition assessment. J Am Diet Assoc 2004; 104: 1258–1264.
Mitrache C, Passweg JR, Libura J, Petrikkos L, Seiler WO, Gratwohl A et al. Anemia: an indicator for malnutrition in the elderly. Ann Hematol 2001; 80: 295–298.
Carmel R . Nutritional anemias and the elderly. Semin Hematol 2008; 45: 225–234.
Acknowledgements
The Swedish National study on Aging and Care, SNAC, (www.snac.org) is financially supported by the Ministry of Health and Social Affairs, Sweden, the participating County Councils and Municipalities, and the Swedish Research Council for Health, Working Life and Welfare (grant 825-2011-6243 to LF; and grant 2012-0022 to WX). In addition, specific grants were obtained from the Gun och Bertil Stohnes Foundation; Demensfonden; Tornspiran Foundation; and Ragnhild och Einar Lundströms Minne Foundation (grant LA2012-0508 to BS; Sweden). We specially thank the staff of the SNAC-K project for their collaboration in data collection and management.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on European Journal of Clinical Nutrition website
Supplementary information
Rights and permissions
About this article
Cite this article
Shakersain, B., Santoni, G., Faxén-Irving, G. et al. Nutritional status and survival among old adults: an 11-year population-based longitudinal study. Eur J Clin Nutr 70, 320–325 (2016). https://doi.org/10.1038/ejcn.2015.109
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ejcn.2015.109
This article is cited by
-
Is the Utility of the GLIM Criteria Used to Diagnose Malnutrition Suitable for Bicultural Populations? Findings from Life and Living in Advanced Age Cohort Study in New Zealand (LiLACS NZ)
The Journal of nutrition, health and aging (2023)
-
Health management of malnourished elderly in primary health care: a scoping review
BMC Primary Care (2022)
-
Mortality risks of body mass index and energy intake trajectories in institutionalized elderly people: a retrospective cohort study
BMC Geriatrics (2022)
-
Nutritional risk screening in malignant tumors: a study of 375 cancer inpatients
Supportive Care in Cancer (2022)
-
County-Level Characteristics Driving Malnutrition Death Rates among Older Adults in Texas
The Journal of nutrition, health and aging (2021)