Abstract
Few prospective studies have examined the combined impact of blood pressure (BP) categories and glucose abnormalities on the incidence of cardiovascular disease (CVD) in the general Asian population. This study aimed to examine the effect of the combined risks of these factors on the incidence of CVD in a general Japanese population. We studied 5321 Japanese individuals (aged 30–79 years), without CVD at baseline, who received follow-up for an average of 11.7 years. Serum fasting glucose categories were defined according to the 2003 American Diabetes Association recommendations. BP categories were defined by the 2009 Japanese Society of Hypertension Guidelines for the Management of Hypertension. The Cox proportional hazard ratios (HRs) for CVD according to the serum glucose and BP categories were calculated. In 62 036 person-years of follow-up, we documented 364 CVD events (198 stroke and 166 coronary heart disease (CHD)). Compared with normoglycemic subjects, the multivariable HRs (95% confidence intervals (CIs)) for CVD, CHD and stroke were 1.25 (1.00–1.58), 1.46 (1.04–2.04) and 1.11 (0.81–1.52), respectively, in individuals with impaired fasting glucose (IFG), whereas these values were 2.13 (1.50–3.03), 2.28 (1.34–3.88) and 2.08 (1.29–3.35), respectively, in individuals with diabetes mellitus (DM). Compared with normoglycemic and optimal blood pressure (BP) subjects, increased risks of CVD were observed in the normoglycemic subjects with high-normal BP or hypertension, the IFG subjects with normal or higher BP, and the DM subjects regardless of BP category (P-value for interaction=0.046). In conclusion, the high-normal BP subjects in all glucose categories and the normal BP subjects with IFG showed increased risk of CVD in this Japanese population. Further investigation of larger cohorts of DM subjects should be conducted to better understand this phenomenon.
Similar content being viewed by others
Introduction
Hypertension is one of the strongest risk factors for increased incidence of cardiovascular disease (CVD) worldwide.1, 2, 3 Recently, high-normal blood pressure (BP)1, 2 and prehypertension3 have also been recognized as risk factors for CVD.4, 5, 6 Increased BP is the most likely precipitator of CVD and stroke.5, 7, 8 Furthermore, the prevalence of glucose intolerance and obesity has increased greatly in recent years.9, 10 Diabetes mellitus (DM) has become a major public health problem11, 12 as well as a risk factor for all-cause mortality11 and CVD.10, 13, 14, 15 Recently, prediabetic hyperglycemia has been recognized to confer an increased risk for CVD.16 However, a few population studies17 have reported a positive association between CVD and impaired fasting glucose (defined as blood glucose of 5.6–6.9 mmol l−1 according to the 2003 American Diabetes Association definition).18
Evaluation of the combined impact of these two major borderline risk factors is essential in preventing CVD because elevated BP is the highest population attributable fraction (PAF) of CVD incidence, and the incidence of hyperglycemia is increasing in Asian and Western countries. There have been a few population studies on the association between the occurrence of hypertension together with DM and the risk of stroke19, 20, 21 and coronary heart disease (CHD).22 However, few population cohort studies have evaluated the impact of the combination of BP categories (optimal BP, normal BP, high-normal BP (or prehypertension) and hypertension) and fasting glucose categories (normoglycemia, impaired fasting glucose (IFG) and DM) on the risk of CVD. Thus, the aim of this study was to examine the combined impact of BP categories and blood glucose abnormalities on the incidence of CVD in a general urban Japanese population.
Methods
Study subjects
The Suita Study, a cohort study for CVD in urban residents, was established in 1989. The details of this study have been described elsewhere.5, 23, 24, 25, 26, 27, 28, 29 Briefly, 6485 individuals (aged 30 to 79 years) underwent regular health checkups between September 1989 and March 1994. Some cohort members were excluded for the following reasons: past or present history of CVD at baseline (n=208); missing data (n=170); nonfasting blood collections (n=173); or lost from follow-up (n=613). After applying these exclusions, a total of 5321 subjects (aged 30 to 79 years) participated in the baseline examination. Informed consent was obtained from all participants. This study was approved by the institutional review board of the National Cardiovascular Center.
Measurement of BP and fasting glucose
Measurement of BP has been described elsewhere.5 In brief, well-trained physicians measured the BP of each individual three times in a seated position using a mercury column sphygmomanometer, an appropriately sized cuff and a standard protocol. Before the initial BP reading was obtained, participants were seated at rest for at least 5 min. Systolic (SBP) and diastolic (DBP) blood pressures were recorded as the average of the second and third measurements, which were taken more than 1 min apart.
At the time of the baseline examination, subjects were classified into one of the following BP categories based on the 2009 Japanese Society of Hypertension Guidelines for the Management of Hypertension:2 optimal BP (SBP, <120 mm Hg and DBP, <80 mm Hg); normal BP (SBP, 120 to 129 mm Hg and DBP, 80 to 84 mm Hg); high-normal BP (SBP, 130 to 139 mm Hg and DBP, 85 to 89 mm Hg); and hypertension (SBP, ⩾140 mm Hg or DBP, ⩾90 mm Hg or antihypertensive drug use). If the SBP and DBP readings for a subject were in different categories, then the subject was categorized into the higher of the two categories.
We performed routine fasting blood collection and immediately measured serum glucose and total cholesterol levels using the same autoanalyzer (Toshiba TBA-80, Toshiba, Tokyo, Japan). Fasting serum glucose categories were defined as follows:18 DM (fasting serum glucose ⩾7.0 mmol l−1 (126 mg per 100 ml) or medications for DM); IFG (fasting serum glucose levels 5.6 to 6.9 mmol l−1 (100 to 125 mg per 100 ml)); and normoglycemia (fasting serum glucose levels <5.6 mmol l−1 (<100 mg per 100 ml)). Hypercholesterolemia was defined as total serum cholesterol levels ⩾5.7 mmol l−1 (220 mg per 100 ml) or current use of antihyperlipidemic medications. Physicians or nurses administered questionnaires addressing personal habits and present illness at the baseline examination. Body mass index was calculated as weight (kg) divided by height (m) squared.
Confirmation of stroke and coronary heart disease and end point determination
Medical records were reviewed by registered hospital physicians or research physicians who were blinded to the baseline data. Strokes were defined according to the US National Survey of Stroke criteria.30 For each stroke subtype (that is, cerebral infarction (thrombotic or embolic infarction), intracerebral hemorrhage and subarachnoid hemorrhage), a definite diagnosis was established based on examination of computed tomographic scans, magnetic resonance images or autopsies. Definite and probable myocardial infarctions were defined according to the criteria set out by the MONICA project.31 The criteria for a diagnosis of CHD included first ever acute myocardial infarction, sudden cardiac death within 24 h after the onset of acute illness or coronary artery disease followed by coronary artery bypass surgery or angioplasty. In this study, CVD was defined as stroke or CHD.
To detect CHD and stroke occurrences, each participant's health status was checked during clinical visits to the National Cardiovascular Center every 2 years. Yearly questionnaires by mail or telephone were also completed by all participants. In addition, to complete our surveillance for fatal strokes and CHD, we conducted a systematic search for death certificates. All data were checked against medical records to confirm the incidence of CVD. When informed consent could not be obtained for a medical records survey (19.5%), we identified possible strokes or CHD using information from (1) questionnaires for present illness of stroke and CHD at the health examination and/or (2) death certificates bearing a diagnosis of probable stroke or CHD. The end point of the follow-up period for each participant was, whichever of the following options occurred first: (1) date of the first diagnosis of CHD or stroke event; (2) date of death; (3) date of leaving Suita; or (4) 31 December, 2005.
Statistical analysis
Analyses of variance and χ2-tests were used to compare mean values and frequencies. The Cox proportional hazard ratios (HRs) and 95% confidence intervals (95% CIs) were fitted to each glucose category (normoglycemia, IFG and DM) after adjusting for sex and age in 5-year increments as stratified variables and other potential confounding factors at baseline, including BP category (optimal, normal, and high-normal BP and hypertension), hypercholesterolemia (positive or negative), body mass index (continuous variable), smoking status (never, ex-smoker and current smoker) and drinking status (never, ex-drinker and current drinker). Test for effect modification by glucose category was conducted with an interaction term generated by multiplying BP category by glucose category. We conducted tests for trend across the BP categories and tested the significance of this variable.
To express the combined impact of glucose and BP categories on the incidence of CVD in these participants, we estimated the PAF as follows:

where Pe is the proportion of incident cases in the combination of glucose and BP categories, and HR is the multivariable-adjusted hazard ratio.32 All statistical analyses were conducted using the SAS statistical software package (release version 8.2; SAS Institute, Cary, NC, USA).
Results
The frequencies of IFG and DM increased with age in both men and women (Figure 1). Table 1 shows the distribution of CVD risk factors at baseline according to fasting glucose categories at baseline. Both men and women with DM were older and had a higher body mass index as well as a higher prevalence of hypertension, hypercholesterolemia and medication for hypertension than those without DM. Men with DM had a lower frequency of never drinking than men without DM.
In 62 036 person-years of follow-up (an average of 11.7 years of follow-up), we documented 364 CVD (198 strokes and 166 CHD) events. Table 2 shows the age- and sex-adjusted HRs and multivariable-adjusted HRs for incidence of CVD according to glucose categories in men and women. Compared with normoglycemic subjects, the multivariable HRs (95% CIs) for CVD, CHD and stroke were 1.25 (1.00–1.58), 1.46 (1.04–2.04) and 1.11 (0.81–1.52), respectively in IFG subjects, whereas these values were 2.13 (1.50–3.03), 2.28 (1.34–3.88) and 2.08 (1.29–3.35), respectively in DM subjects. Compared with normoglycemic subjects, IFG and DM were risk factors for CVD and CHD in women, and DM was a risk factor for CVD and stroke in men.
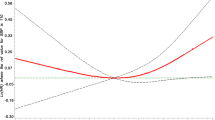
Figure 2 shows the multivariable HRs of CVD for the combined impact of the fasting glucose and BP categories. Compared with normoglycemic subjects with optimal BP, the following groups showed increased risk of CVD: the normoglycemic subjects with high-normal BP or hypertension (P-value for trend of BP category<0.001); the IFG subjects with normal or higher BP (P-value for trend of BP category=0.001); and the DM subjects in any BP category (P-value for trend of BP category=0.41). After excluding subjects taking diabetic medication, the P-value for the BP category trend was not statistically significant in the DM subjects. The significant interaction terms between fasting blood glucose and BP categories were observed in CVD (P=0.046); however, the interaction term was not significant after exclusion of DM subjects.
The influence of fasting glucose and BP categories on multivariable-adjusted hazard ratios and 95% confidence intervals for the incidence of cardiovascular disease. *P<0.05, compared with normoglycemic subjects with optimal BP. †P<0.05, compared with normoglycemic subjects in the same BP category. ‡P<0.05, compared with normoglycemic subjects with hypertension.
Using the HRs, we estimated the PAF for CVD to exposure to the combined impact of fasting glucose and BP categories at baseline (Figure 3). The population-attributable risk percentage for CVD incidence was estimated at 3.7% for subjects with normoglycemia and high-normal BP, 5.7% for subjects with IFG and normal or high-normal BP group and 8.2% for subjects with DM and any BP category group, when comparing these groups with the normoglycemic and optimal BP group.
The hazard ratios and population attributable fractions for CVD to exposure to the combined impact of glucose (normoglycemia, impaired fasting glucose and diabetes) and blood pressure categories (optimal, normal, and high-normal blood pressures and hypertension) at baseline were estimated. The gray and black areas represent excessive incidence of CVD in the high blood glucose and high blood pressure categories compared with the subjects with normoglycemia and optimal blood pressure as a reference.
Discussion
In this population cohort study, we found that DM was a risk factor for CVD, stroke and CHD, whereas an IFG of 5.6 to 6.9 mmol l−1 was a risk factor for CVD and CHD only. A combined effect of IFG and prehypertension on the incidence of CVD was observed. The high-normal BP subjects in any glucose category and the normal BP subjects with IFG in the Japanese population showed increased risks of CVD. To our knowledge, this study is the first on the combined impact of these borderline risk factors, IFG and prehypertension on the incidence of CVD in a general Asian population.
Previous cohort studies have shown that DM is a risk factor for CVD, stroke14, 15 and CHD.13 The results of our study are also essentially compatible with the previous cohort studies in Japan. The Hisayama Study demonstrated that glucose intolerance for 2421 participants was a risk factor for increased incidence of stroke and CHD.15 Iso et al.20 reported that glucose abnormalities were a risk factor for ischemic stroke in a Japanese population by using nonfasting glucose levels. The NIPPON DATA 80 Study indicated that DM, defined by nonfasting blood glucose levels, was a risk factor for CVD mortality.33 In the Funagata Diabetes Study, IFG was not a risk factor for CVD mortality, although impaired glucose tolerance was a risk factor for CVD.34
Compared with previous studies, our study has several methodological strengths. First, our cohort population was relatively large and was selected at random from an urban population in contrast to most other cohort populations in Asia, which were selected from rural populations.15, 20, 34 Second, all of our cohort participants were examined at one place and measured using the same autoanalyzer at one laboratory. Finally, our study examined the risk of CVD incidence, not CVD mortality.
In our study, we used the definitions of IFG and CVD/CHD set forth by the 2003 American Diabetes Association recommendations. In the Framingham Heart Study, the 2003 IFG definition was predictive of CHD in women but not in men,17 a finding which was similar to our results. However, fewer studies have examined the association of the 2003 IFG definitions for CHD and stroke. Kanaya et al.35 showed that the 2003 defination for IFG was not associated with increased risk of CHD or stroke among postmenopausal women with coronary artery disease.Kim et al.36 reported that one-third of the population has IFG according to the 2003 definition. However, many of these individuals do not have increased prevalence of CHD.
Hu et al.19 reported that hypertension and DM increased stroke risk independently and that their combination additively increased stroke risk. In our study, the risks of CVD in the normoglycemic and IFG groups were linearly related to the BP category (P-value for trend<0.001). However, the risks of CVD in the DM group did not change with BP category (P-value for trend=0.4), which was compatible with a previous result for trends between glucose category and hypertension status.20 Recently, the ACCORD BP Study has shown that targeting an SBP <120 mm Hg, as opposed to an SBP <140 mm Hg, did not reduce the rate of a composite outcome of fatal and nonfatal major cardiovascular events in patients with type 2 diabetes.37 Although present studies suggest that decreasing BP may be an effective way to prevent CVD in normoglycemic or IFG subjects, further investigations are required to clarify the interaction between the BP categories of DM subjects at risk for CVD in other large cohorts.
The percentage of the PAF for CVD incidence in normoglycemic subjects with high-normal BP or IFG subjects with normal or high-normal BP (PAF=12.6%) was 1.5 times higher than that in the DM subjects in any BP category (PAF=8.2%). Also, the PAF suggested that 12.6% of CVD cases would be preventable if the borderline glucose and blood pressure levels were controlled to within normoglycemic and optimal BP ranges.
Our results showed that hyperglycemia conferred a slightly higher risk of CVD incidence in women than in men, although men had greater absolute event rates for CVD. Previous studies have shown that the impact of DM on the risk of CVD is significantly greater in women than in men.13, 17, 38 Lee et al. reported that the HRs of coronary heart disease for DM were 2.6 for women and 1.9 for men. In the Framingham Heart Study, 17 IFG was associated with increased CHD risk only in women (HR=1.7; 95% CI, 1.0–3.0). The reason for these sex differences in the association between DM and CVD remains unclear.
Our study has several limitations. The primary limitation is the regression dilution bias; this study was based on a single day measurement of serum glucose and BP levels.39 That is, the fasting serum glucose and BP levels might have been misclassified. Second, as we did not perform glucose tolerance tests, we may have missed subjects with impaired glucose tolerance. Finally, we did not examine the combined effect of BP categories and glucose abnormalities after stratification by CVD subtypes, such as stroke and CHD because of the small sample size.
In conclusion, DM is a risk factor for CVD, stroke, and CHD, whereas an IFG of 5.6 to 6.9 mmol l−1 is a risk factor for CVD and CHD in women. The risks of CVD in the normoglycemic and IFG groups were linearly related to the BP category. The high-normal BP subjects in any glucose categories and the normal BP subjects with IFG showed increased risks of CVD in this Japanese population. Further investigations of larger cohorts of DM subjects are needed.
References
Mancia G, De Backer G, Dominiczak A, Cifkova R, Fagard R, Germano G, Grassi G, Heagerty AM, Kjeldsen SE, Laurent S, Narkiewicz K, Ruilope L, Rynkiewicz A, Schmieder RE, Boudier HA, Zanchetti A, Vahanian A, Camm J, De Caterina R, Dean V, Dickstein K, Filippatos G, Funck-Brentano C, Hellemans I, Kristensen SD, McGregor K, Sechtem U, Silber S, Tendera M, Widimsky P, Zamorano JL, Erdine S, Kiowski W, Agabiti-Rosei E, Ambrosioni E, Lindholm LH, Viigimaa M, Adamopoulos S, Bertomeu V, Clement D, Farsang C, Gaita D, Lip G, Mallion JM, Manolis AJ, Nilsson PM, O'Brien E, Ponikowski P, Redon J, Ruschitzka F, Tamargo J, van Zwieten P, Waeber B, Williams B . 2007 guidelines for the management of arterial hypertension: the task force for the management of arterial hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). J Hypertens 2007; 25: 1105–1187.
Ogihara T, Kikuchi K, Matsuoka H, Fujita T, Higaki J, Horiuchi M, Imai Y, Imaizumi T, Ito S, Iwao H, Kario K, Kawano Y, Kim-Mitsuyama S, Kimura G, Matsubara H, Matsuura H, Naruse M, Saito I, Shimada K, Shimamoto K, Suzuki H, Takishita S, Tanahashi N, Tsuchihashi T, Uchiyama M, Ueda S, Ueshima H, Umemura S, Ishimitsu T, Rakugi H . The Japanese Society of Hypertension Guidelines for the Management of Hypertension (JSH 2009). Hypertens Res 2009; 32: 3–107.
Chobanian AV, Bakris GL, Black HR, Cushman WC, Green LA, Izzo Jr JL, Jones DW, Materson BJ, Oparil S, Wright Jr JT, Roccella EJ . The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: the JNC 7 Report. JAMA 2003; 289: 2560–2572.
Vasan RS, Larson MG, Leip EP, Evans JC, O'Donnell CJ, Kannel WB, Levy D . Impact of high-normal blood pressure on the risk of cardiovascular disease. N Engl J Med 2001; 345: 1291–1297.
Kokubo Y, Kamide K, Okamura T, Watanabe M, Higashiyama A, Kawanishi K, Okayama A, Kawano Y . Impact of high-normal blood pressure on the risk of cardiovascular disease in a Japanese urban cohort: the Suita Study. Hypertension 2008; 52: 652–659.
Kokubo Y, Kamide K . High-normal blood pressure and the risk of cardiovascular disease. Circ J 2009; 73: 1381–1385.
Ohira T, Shahar E, Chambless LE, Rosamond WD, Mosley Jr TH, Folsom AR . Risk factors for ischemic stroke subtypes: the Atherosclerosis Risk in Communities study. Stroke 2006; 37: 2493–2498.
Imano H, Kitamura A, Sato S, Kiyama M, Ohira T, Yamagishi K, Noda H, Tanigawa T, Iso H, Shimamoto T . Trends for blood pressure and its contribution to stroke incidence in the middle-aged Japanese population: the Circulatory Risk in Communities Study (CIRCS). Stroke 2009; 40: 1571–1577.
Kubo M, Hata J, Doi Y, Tanizaki Y, Iida M, Kiyohara Y . Secular trends in the incidence of and risk factors for ischemic stroke and its subtypes in Japanese population. Circulation 2008; 118: 2672–2678.
Fox CS, Coady S, Sorlie PD, D′Agostino Sr RB, Pencina MJ, Vasan RS, Meigs JB, Levy D, Savage PJ . Increasing cardiovascular disease burden due to diabetes mellitus: the Framingham Heart Study. Circulation 2007; 115: 1544–1550.
Garcia MJ, McNamara PM, Gordon T, Kannel WB . Morbidity and mortality in diabetics in the Framingham population. Sixteen year follow-up study. Diabetes 1974; 23: 105–111.
Manuel DG, Schultz SE . Health-related quality of life and health-adjusted life expectancy of people with diabetes in Ontario, Canada, 1996–1997. Diabetes Care 2004; 27: 407–414.
Lee WL, Cheung AM, Cape D, Zinman B . Impact of diabetes on coronary artery disease in women and men: a meta-analysis of prospective studies. Diabetes Care 2000; 23: 962–968.
Folsom AR, Rasmussen ML, Chambless LE, Howard G, Cooper LS, Schmidt MI, Heiss G . Prospective associations of fasting insulin, body fat distribution, and diabetes with risk of ischemic stroke. The Atherosclerosis Risk in Communities (ARIC) Study Investigators. Diabetes Care 1999; 22: 1077–1083.
Doi Y, Ninomiya T, Hata J, Fukuhara M, Yonemoto K, Iwase M, Iida M, Kiyohara Y . Impact of glucose tolerance status on development of ischemic stroke and coronary heart disease in a general Japanese population: the Hisayama Study. Stroke 2010; 41: 203–209.
Wingard DL, Barrett-Connor EL, Scheidt-Nave C, McPhillips JB . Prevalence of cardiovascular and renal complications in older adults with normal or impaired glucose tolerance or NIDDM. A population-based study. Diabetes Care 1993; 16: 1022–1025.
Levitzky YS, Pencina MJ, D′Agostino RB, Meigs JB, Murabito JM, Vasan RS, Fox CS . Impact of impaired fasting glucose on cardiovascular disease: the Framingham Heart Study. J Am Coll Cardiol 2008; 51: 264–270.
Genuth S, Alberti KG, Bennett P, Buse J, Defronzo R, Kahn R, Kitzmiller J, Knowler WC, Lebovitz H, Lernmark A, Nathan D, Palmer J, Rizza R, Saudek C, Shaw J, Steffes M, Stern M, Tuomilehto J, Zimmet P . Follow-up report on the diagnosis of diabetes mellitus. Diabetes Care 2003; 26: 3160–3167.
Hu G, Sarti C, Jousilahti P, Peltonen M, Qiao Q, Antikainen R, Tuomilehto J . The impact of history of hypertension and type 2 diabetes at baseline on the incidence of stroke and stroke mortality. Stroke 2005; 36: 2538–2543.
Iso H, Imano H, Kitamura A, Sato S, Naito Y, Tanigawa T, Ohira T, Yamagishi K, Iida M, Shimamoto T . Type 2 diabetes and risk of non-embolic ischaemic stroke in Japanese men and women. Diabetologia 2004; 47: 2137–2144.
Kissela BM, Khoury J, Kleindorfer D, Woo D, Schneider A, Alwell K, Miller R, Ewing I, Moomaw CJ, Szaflarski JP, Gebel J, Shukla R, Broderick JP . Epidemiology of ischemic stroke in patients with diabetes: the greater Cincinnati/Northern Kentucky Stroke Study. Diabetes Care 2005; 28: 355–359.
Hu G, Jousilahti P, Tuomilehto J . Joint effects of history of hypertension at baseline and type 2 diabetes at baseline and during follow-up on the risk of coronary heart disease. Eur Heart J 2007; 28: 3059–3066.
Kokubo Y, Nakamura S, Okamura T, Yoshimasa Y, Makino H, Watanabe M, Higashiyama A, Kamide K, Kawanishi K, Okayama A, Kawano Y . The relationship between blood pressure category and incidence of stroke and myocardial infarction in an urban Japanese population with and without chronic kidney disease: the Suita Study. Stroke 2009; 40: 2674–2679.
Kokubo Y, Okamura T, Yoshimasa Y, Miyamoto Y, Kawanishi K, Kotani Y, Okayama A, Tomoike H . Impact of metabolic syndrome components on the incidence of cardiovascular disease in a general urban Japanese population: the Suita Study. Hypertens Res 2008; 31: 2027–2035.
Okamura T, Kokubo Y, Watanabe M, Higashiyama A, Miyamoto Y, Yoshimasa Y, Okayama A . Low-density lipoprotein cholesterol and non-high-density lipoprotein cholesterol and the incidence of cardiovascular disease in an urban Japanese cohort study: the Suita Study. Atherosclerosis 2009; 203: 587–592.
Watanabe M, Kokubo Y, Higashiyama A, Ono Y, Okayama A, Okamura T . New diagnosis criteria for diabetes with hemoglobin A1c and risks of macro-vascular complications in an urban Japanese cohort: the Suita Study. Diabetes Res Clin Pract 2010; 88: e20–e23.
Okamura T, Kokubo Y, Watanabe M, Higashiyama A, Ono Y, Miyamoto Y, Yoshimasa Y, Okayama A . Triglycerides and non-high-density lipoprotein cholesterol and the incidence of cardiovascular disease in an urban Japanese cohort: the Suita Study. Atherosclerosis 2010; 209: 290–294.
Higashiyama A, Okamura T, Ono Y, Watanabe M, Kokubo Y, Okayama A . Risk of smoking and metabolic syndrome for incidence of cardiovascular disease—comparison of relative contribution in urban Japanese population: the Suita Study. Circ J 2009; 73: 2258–2263.
Furukawa Y, Kokubo Y, Okamura T, Watanabe M, Higashiyama A, Ono Y, Kawanishi K, Okayama A, Date C . The relationship between waist circumference and the risk of stroke and myocardial infarction in a Japanese urban cohort: the Suita Study. Stroke 2010; 41: 550–553.
Walker AE, Robins M, Weinfeld FD . The national survey of stroke. Clinical findings. Stroke 1981; 12: I13–I44.
Tunstall-Pedoe H, Kuulasmaa K, Amouyel P, Arveiler D, Rajakangas AM, Pajak A . Myocardial infarction and coronary deaths in the World Health Organization MONICA Project. Registration procedures, event rates, and case-fatality rates in 38 populations from 21 countries in four continents. Circulation 1994; 90: 583–612.
Rockhill B, Newman B, Weinberg C . Use and misuse of population attributable fractions. Am J Public Health 1998; 88: 15–19.
Kadowaki S, Okamura T, Hozawa A, Kadowaki T, Kadota A, Murakami Y, Nakamura K, Saitoh S, Nakamura Y, Hayakawa T, Kita Y, Okayama A, Ueshima H . Relationship of elevated casual blood glucose level with coronary heart disease, cardiovascular disease and all-cause mortality in a representative sample of the Japanese population. NIPPON DATA 80. Diabetologia 2008; 51: 575–582.
Tominaga M, Eguchi H, Manaka H, Igarashi K, Kato T, Sekikawa A . Impaired glucose tolerance is a risk factor for cardiovascular disease, but not impaired fasting glucose. The Funagata Diabetes Study. Diabetes Care 1999; 22: 920–924.
Kanaya AM, Herrington D, Vittinghoff E, Lin F, Bittner V, Cauley JA, Hulley S, Barrett-Connor E . Impaired fasting glucose and cardiovascular outcomes in postmenopausal women with coronary artery disease. Ann Intern Med 2005; 142: 813–820.
Kim SH, Chunawala L, Linde R, Reaven GM . Comparison of the 1997 and 2003 American Diabetes Association classification of impaired fasting glucose: impact on prevalence of impaired fasting glucose, coronary heart disease risk factors, and coronary heart disease in a community-based medical practice. J Am Coll Cardiol 2006; 48: 293–297.
ACCORD Study Group. Cushman WC, Evans GW, Byington RP, Goff Jr DC, Grimm Jr RH, Cutler JA, Simons-Morton DG, Basile JN, Corson MA, Probstfield JL, Katz L, Peterson KA, Friedewald WT, Buse JB, Bigger JT, Gerstein HC, Ismail-Beigi F . Effects of Intensive blood-pressure control in type 2 diabetes mellitus. N Engl J Med 2010; 362: 1575–1585.
Barrett-Connor EL, Cohn BA, Wingard DL, Edelstein SL . Why is diabetes mellitus a stronger risk factor for fatal ischemic heart disease in women than in men? The Rancho Bernardo Study. JAMA 1991; 265: 627–631.
MacMahon S, Peto R, Cutler J, Collins R, Sorlie P, Neaton J, Abbott R, Godwin J, Dyer A, Stamler J . Blood pressure, stroke, and coronary heart disease. Part 1, Prolonged differences in blood pressure: prospective observational studies corrected for the regression dilution bias. Lancet 1990; 335: 765–774.
Acknowledgements
We thank Dr Yasushi Kotani, all members of the Suita City Health Center and the Suita Medical Association. We also thank all researchers and the staff of the Division of Preventive Cardiology for performing the medical examinations and study follow-up. We also thank Satsuki-Junyukai, the volunteers who administered the Suita Study. Source of Funding: This study was supported by a Grant-in-Aid from the Ministry of Health, Labor and Welfare of Japan (H20-SeiShu-013 and H19-SeiShu-017); a research grant for cardiovascular disease from the Ministry of Health, Labor and Welfare (19S-6, 21S-1); and the Mitsui Life Social Welfare Foundation.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Kokubo, Y., Okamura, T., Watanabe, M. et al. The combined impact of blood pressure category and glucose abnormality on the incidence of cardiovascular diseases in a Japanese urban cohort: the Suita Study. Hypertens Res 33, 1238–1243 (2010). https://doi.org/10.1038/hr.2010.174
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/hr.2010.174
Keywords
This article is cited by
-
Factors Associated with the Antihypertensive Effect of Esaxerenone and Serum Potassium Elevation: A Pooled Analysis of Seven Phase III Studies
Advances in Therapy (2023)
-
Liver enzymes, alcohol consumption and the risk of diabetes: the Suita study
Acta Diabetologica (2022)
-
Effect of metabolic syndrome on coronary heart disease in rural minorities of Xinjiang: a retrospective cohort study
BMC Public Health (2020)
-
Impact of hypertension stratified by diabetes on the lifetime risk of cardiovascular disease mortality in Japan: a pooled analysis of data from the Evidence for Cardiovascular Prevention from Observational Cohorts in Japan study
Hypertension Research (2020)
-
Recent status of self-measured home blood pressure in the Japanese general population: a modern database on self-measured home blood pressure (MDAS)
Hypertension Research (2020)