Abstract
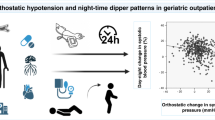
In the pre-awakening hours, diastolic blood pressure (DBP) is normally at its lowest, and diastolic hypotension is a risk factor for cardiac ischemia. We investigated pre-awakening DBP values and its predictors in treated hypertensive patients who underwent ambulatory blood pressure monitoring. The pre-awakening period was defined as the 3-h period ending 1 h before awakening (most frequently 03:00–06:00). In 269 included subjects, office DBP was 86.4±12.0 mm Hg, 24-h DBP was 78.6±9.6 mm Hg, mean pre-awakening DBP was 70.3±10.9 mm Hg, and trough pre-awakening DBP was 62.5±11.2 mm Hg. Half of the patients (51%) had a mean pre-awakening DBP <70 mm Hg, and 14% had <60 mm Hg. Trough pre-awakening DBP <60 mm Hg was seen in 36% and <50 mm Hg in 12% of patients. Office DBP was the most important predictor of mean and trough pre-awakening DBP (both beta=0.4; P<0.001), and of pre-awakening DBP <70 mm Hg and <60 mm Hg (both P⩽0.001). Diabetes mellitus was associated with a lower trough pre-awakening DBP (beta=−3.2; P=0.02). Among variables that failed to independently predict low pre-awakening DBP were age, a history of vascular disease, and classes and number of antihypertensive drugs. We found that many hypertensive patients have low DBP in the pre-awakening period. Office DBP is the main predictor of low pre-awakening DBP. Further studies are needed to define the prognostic relevance and potential risks of low pre-awakening DBP.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Muller JE, Stone PH, Turi ZG, Rutherford JD, Czeisler CA, Parker C et al. Circadian variation in the frequency of onset of acute myocardial infarction. N Eng J Med 1985; 313: 1315–1322.
White WB . Cardiovascular risk and therapeutic intervention for the early morning surge in blood pressure and heart rate. Blood Press Monit 2001; 6: 63–72.
Millar-Craig MW, Bishop CN, Raftery EB . Circadian variation of blood-pressure. Lancet 1978; 1: 795–797.
Mancia G, Sega R, Milesi C, Cesana G, Zanchetti A . Blood-pressure control in the hypertensive population. Lancet 1997; 349: 454–457.
Kario K . Morning surge in blood pressure and cardiovascular risk: evidence and perspectives. Hypertension 2010; 56: 765–773.
O’Brien E, Sheridan J, O’Malley K . Dippers and non-dippers. Lancet 1988; 2: 397.
Ohkubo T, Hozawa A, Yamaguchi J, Kikuya M, Ohmori K, Michimata M et al. Prognostic significance of the nocturnal decline in blood pressure in individuals with and without high 24-h blood pressure: the Ohasama study. J Hypertens 2002; 20: 2183–2189.
De la Sierra A, Redon J, Banegas JR, Segura J, Parati G, Gorostidi M et al. Prevalence and factors associated with circadian blood pressure patterns in hypertensive patients. Hypertension 2009; 53: 466–472.
Kario K, Matsuo T, Kobayashi H, Imiya M, Matsuo M, Shimada K . Nocturnal fall of blood pressure and silent cerebrovascular damage in elderly hypertensive patients. Advanced silent cerebrovascular damage in extreme dippers. Hypertension 1996; 27: 130–135.
Pierdomenico SD, Bucci A, Costantini F, Lapenna D, Cuccurullo F, Mezzetti A . Circadian blood pressure changes and myocardial ischemia in hypertensive patients with coronary artery disease. J Am Cardiol 1998; 31: 1627–1634.
Owens P, O’Brien E . Hypotension in patients with coronary disease: can profound hypotensive events cause myocardial ischaemic events? Heart 1999; 82: 477–481.
James Pa, Oparil S, Carter BL, Cushman WC, Dennison-Himmelfarb C, Handler J et al. 2014 evidence-based guideline for the management of high blood pressure in adults. JAMA 2013; 1097: 1–14.
Banach M, Aronow WS . Blood pressure J-curve: current concepts. Curr Hypertens Rep 2012; 14: 556–566.
Fogari R, Zoppi A, Malamani GD, Lazzari P, Destro M, Corradi L . Ambulatory blood pressure monitoring in normotensive and hypertensive type 2 diabetics prevalence of impaired diurnal blood pressure patterns. Am J Hypertens 1993; 6: 1–7.
Dost A, Klinkert C, Kapellen T, Lemmer A, Naeke A, Grabert M et al. Arterial hypertension determined by ambulatory blood pressure profiles: contribution to microalbuminuria risk in a multicenter investigation in 2105 children and adolescents with type 1 diabetes. Diabetes Care 2008; 31: 720–725.
Acknowledgements
We gratefully acknowledge vascular nurse specialist Catherine Combee who greatly assisted in the data collection.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Journal of Human Hypertension website
Supplementary information
Rights and permissions
About this article
Cite this article
Zheng, K., Serné, E., Kooter, A. et al. Pre-awakening diastolic hypotension in treated hypertensive patients: prevalence and predictors. J Hum Hypertens 30, 322–327 (2016). https://doi.org/10.1038/jhh.2015.80
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jhh.2015.80