Abstract
Objective:
To evaluate the preparedness of pediatric residents entering accredited neonatal–perinatal medicine (NPM) fellowships in the United States.
Study design:
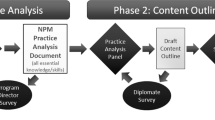
A multi-domain, validated survey was distributed to Program Directors (PDs) of US NPM fellowship programs. The 47-item survey explored 5 domains: professionalism, independent practice, psychomotor ability, clinical evaluation, and academia. A systematic, qualitative analysis on free-text comments was also performed.
Results:
Sixty-one PDs completed the survey, for a response rate of 62% (61/98). For entering fellows, PDs assessed performance in professionalism positively, including 76% as communicating effectively with parents and 90% treating residents/house-staff with respect. In contrast, most PDs rated performance in psychomotor abilities negatively, including 59% and 79% as deficient in bag-and-mask ventilation and neonatal endotracheal intubation, respectively. Although 62% of PDs assessed entering fellows positively for genuine interest in academic projects, fewer than 10% responded positively that entering fellows understood research protocol design, basic statistics, or were capable of writing a cohesive manuscript well. Thematic clustering of qualitative data revealed deficits in psychomotor ability and academia/scholarship.
Conclusions:
On the basis of the perspective of front line educators, graduating pediatric residents are underprepared for subspecialty fellowship training in NPM. To provide the best preparation for pediatric graduates who pursue advanced training, changes to residency education to address deficiencies in these important competencies are warranted.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Lieberman L, Hilliard RI . How well do paediatric residency programmes prepare residents for clinical practice and their future careers? Med Educ 2006; 40 (6): 539–546.
American Board of Pediatrics Inc., 2015–2016 Workforce Data. 2016 Available at https://www.abp.org/sites/abp/files/pdf/workforcebook.pdf (accessed on 15 May 2016).
Council of Pediatric Subspecialties. Recommendations from the CoPS Fellowship Readiness Action Team. 2014 Available at http://www.pedsubs.org/taskforce/pdfs/FinalRecommendations_fromFellowhsipReadinessActionTeam%201_6_14.pdf (accessed on 23 May 2016).
Landrigan CP, Fahrenkopf AM, Lewin D, Sharek PJ, Barger LK, Eisner M et al. Effects of the accreditation council for graduate medical education duty hour limits on sleep, work hours, and safety. Pediatrics 2008; 122 (2): 250–258.
Freed GL, Dunham KM, Moran LM, Spera L . Research Advisory Committee of the American Board of P. Resident work hour changes in children's hospitals: impact on staffing patterns and workforce needs. Pediatrics 2012; 130 (4): 700–704.
Freed GL, Dunham KM, Lamarand KE, Loveland-Cherry C, Martyn KK, The American Board of Pediatrics RAC. Neonatal nurse practitioners: distribution, roles and scope of practice. Pediatrics 2010; 126 (5): 856–860.
Mattar SG, Alseidi AA, Jones DB, Jeyarajah DR, Swanstrom LL, Aye RW et al. General surgery residency inadequately prepares trainees for fellowship: results of a survey of fellowship program directors. Ann Surg 2013; 258 (3): 440–449.
Guntupalli SR, Doo DW, Guy M, Sheeder J, Omurtag K, Kondapalli L et al. Preparedness of obstetrics and gynecology residents for fellowship training. Obstet Gynecol 2015; 126 (3): 559–568.
Association of American Medical Colleges: Physician Specialty Data Book (2014). Available at https://members.aamc.org/eweb/upload/PhysicianSpecialtyDatabook2014.pdf.
Althouse LA, Stockman JA 3rd The American Board of Pediatrics. Pediatric workforce: a look at neonatal-perinatal medicine data from the American Board of Pediatrics. J Pediatr 2006; 148 (6): 727–729.
Schumacher DJ, Frintner MP, Jain A, Cull W . The 2011 ACGME standards: impact reported by graduating residents on the working and learning environment. Acad Pediatr 2014; 14 (2): 149–154.
Schumacher DJ, Frintner MP, Winn A, Cull W . Graduating pediatrics residents' reports on the impact of fatigue over the past decade of duty hour changes. Acad Pediatr 2015; 15 (4): 362–366.
Harris PA, Taylor R, Thielke R, Payne J, Gonzalez N, Conde JG . Research electronic data capture (REDCap)—a metadata-driven methodology and workflow process for providing translational research informatics support. J. Biomed Inform 2009; 42 (2): 377–381.
Accreditation Council for Graduate Medical Education (ACGME). ACGME program requirements for graduate medical education in pediatrics. 2015. Available at http://www.acgme.org/Portals/0/PFAssets/ProgramRequirements/320_pediatrics_07012015.pdf (accessed on 23 May 2016).
Kourembanas S, Steinhorn R . In-house neonatology: what are we waiting for? Am J Respir Crit Care Med 2010; 182 (6): 728–729.
Burke AE, Rushton J, Guralnick S, Hicks P . Resident work duty hour requirements: medical educators' perspectives. Acad Pediatr 2010; 10 (6): 369–371.
Haubner LY, Barry JS, Johnston LC, Soghier L, Tatum PM, Kessler D et al. Neonatal intubation performance: room for improvement in tertiary neonatal intensive care units. Resuscitation 2013; 84 (10): 1359–1364.
Lee HC, Chitkara R, Halamek LP, Hintz SR . A national survey of pediatric residents and delivery room training experience. J Pediatr 2010; 157 (1): 158–161 e153.
O'Donnell CP, Kamlin CO, Davis PG, Morley CJ . Endotracheal intubation attempts during neonatal resuscitation: success rates, duration, and adverse effects. Pediatrics 2006; 117 (1): e16–e21.
Downes KJ, Narendran V, Meinzen-Derr J, McClanahan S, Akinbi HT . The lost art of intubation: assessing opportunities for residents to perform neonatal intubation. J Perinatol 2012; 32 (12): 927–932.
Bismilla Z, Finan E, McNamara PJ, LeBlanc V, Jefferies A, Whyte H . Failure of pediatric and neonatal trainees to meet Canadian Neonatal Resuscitation Program standards for neonatal intubation. J Perinatol 2010; 30 (3): 182–187.
Sanders RC, Giuliano JS, Sullivan JE, Brown CA, Walls RM, Nadkarni V et al. Level of Trainee and Tracheal Intubation Outcomes. Pediatrics 2013; 131 (3): E821–E828.
Lee HC, Rhee CJ, Sectish TC, Hintz SR . Changes in attendance at deliveries by pediatric residents 2000 to 2005. Am J Perinatol 2009; 26 (2): 129–134.
DeMeo SD, Katakam L, Goldberg RN, Tanaka D . Predicting neonatal intubation competency in trainees. Pediatrics 2015; 135 (5): e1229–e1236.
Sawyer T, French H, Ades A, Johnston L . Neonatal-perinatal medicine fellow procedural experience and competency determination: results of a national survey. J Perinatol 2016; 36 (7): 570–574.
Freed GL, Dunham KM, Switalski KE, Jones MD Jr., McGuinness GA . The American Board of Pediatrics RAC. Recently trained pediatric subspecialists: perspectives on training and scope of practice. Pediatrics 2009; 123 (Suppl 1): S44–S49.
Jones MD Jr., McGuinness GA, Residency R . Redesign in Pediatrics C. The future of pediatric residency education: prescription for more flexibility. J Pediatrics 2009; 154 (2): 157–158.
Parker TA, Aucott SW, Bendel CM, Dammann CE, Rice WR, Savich RD et al. The new 6-unit individualized curriculum for pediatric residents: the perspective of neonatology fellowship program directors. J Perinatol 33 (12): 910–913.
Ericsson KA . Deliberate practice and acquisition of expert performance: a general overview. Acad Emerg Med 2008; 15 (11): 988–994.
Finan E, Bismilla Z, Campbell C, Leblanc V, Jefferies A, Whyte HE . Improved procedural performance following a simulation training session may not be transferable to the clinical environment. J Perinatol 2012; 32 (7): 539–544.
Gaies MG, Landrigan CP, Hafler JP, Sandora TJ . Assessing procedural skills training in pediatric residency programs. Pediatrics 2007; 120 (4): 715–722.
Gilhooly J, Redden HR, Leonard DT . Competency in neonatal endotracheal intubation: mission impossible? Pediatrics 2015; 135 (5): e1290–e1291.
Schumacher DJ, Spector ND, Calaman S, West DC, Cruz M, Frohna JG et al. Putting the pediatrics milestones into practice: a consensus roadmap and resource analysis. Pediatrics 2014; 133 (5): 898–906.
Schumacher DJ, Lewis KO, Burke AE, Smith ML, Schumacher JB, Pitman MA et al. The pediatrics milestones: initial evidence for their use as learning road maps for residents. Academic pediatrics 2013; 13 (1): 40–47.
Carraccio C, Englander R, Gilhooly J, Mink R, Hofkosh D, Barone MA et al. Building a framework of entrustable professional activities, supported by competencies and milestones, to bridge the educational continuum. Acad Med 2016. (e-pub ahead of print).
Zemlo TR, Garrison HH, Partridge NC, Ley TJ . The physician-scientist: career issues and challenges at the year 2000. FASEB J 2000; 14 (2): 221–230.
Penn AA . Perspectives of recent trainees on career choices in neonatology. J Perinatol 2006; 26 (Suppl 2): S53–S56.
Nasca TJ, Day SH, Amis ES Jr. . The new recommendations on duty hours from the ACGME Task Force. N Engl J Med 2010; 363 (2): e3.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Backes, C., Bonachea, E., Rivera, B. et al. Preparedness of pediatric residents for fellowship: a survey of US neonatal–perinatal fellowship program directors. J Perinatol 36, 1132–1137 (2016). https://doi.org/10.1038/jp.2016.153
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2016.153
This article is cited by
-
Essentials of Neonatal-Perinatal Medicine fellowship: an overview
Journal of Perinatology (2022)
-
Essentials of Neonatal-Perinatal Medicine fellowship: part 2 - clinical education and experience
Journal of Perinatology (2022)