Abstract
Diabetic nephropathy ranks as the most devastating kidney disease worldwide. It characterizes in the early onset by glomerular hypertrophy, hyperfiltration and mesangial expansion. Experimental models show that overproduction of vascular endothelial growth factor (VEGF) is a pathogenic condition for podocytopathy; however the mechanisms that regulate this growth factor induction are not clearly identified. We determined that the adenosine A2B receptor (A2BAR) mediates VEGF overproduction in ex vivo glomeruli exposed to high glucose concentration, requiring PKCα and Erk1/2 activation. The glomerular content of A2BAR was concomitantly increased with VEGF at early stages of renal disease in streptozotocin-induced diabetic rats. Further, in vivo administration of an antagonist of A2BAR in diabetic rats blocked the glomerular overexpression of VEGF, mesangial cells activation and proteinuria. In addition, we also determined that the accumulation of extracellular adenosine occurs in glomeruli of diabetic rats. Correspondingly, raised urinary adenosine levels were found in diabetic rats. In conclusion, we evidenced that adenosine signaling at the onset of diabetic kidney disease is a pathogenic event that promotes VEGF induction.
Similar content being viewed by others
Main
Diabetes mellitus is a metabolic disease showing a dramatic increase of affected people worldwide.1 Diabetic nephropathy (DN) is a diabetes-derived complication that continues to be the primary cause of terminal renal illness throughout the world,2 affecting up to 30% of diabetic people. Patients with DN live with a high risk of developing cardiovascular disease and their quality of life worsens with progression of the disease. The economic and social impacts of the illness are high, as DN predisposes patients to undergo hemodialysis programs and possible renal transplant at advanced stages. Up to date, strict controls of glycemia and arterial blood pressure, as well as the use of the renin–angiotensin system blockers have been only modestly successful in retarding DN progression.3, 4 Thus, identification of new therapeutic alternatives remains to be a challenge for research in this field.
It has been shown at the onset of DN that podocytopathy and alterations of the filtration barrier occur, which clinically correspond to hyperfiltration and microalbuminuria. In addition, mesangial expansion with exacerbated extracellular matrix accumulation is a remarkable feature of this disease, which histologically appears as glomeruloesclerosis.5 The disruption of the vascular endothelial growth factor (VEGF)/nitric oxide axis has been recognized as a key event leading to the progression of DN.6 Further, overproduction of VEGF in transgenic animals is sufficient to resemble the glomerular alterations seen in DN.7, 8 Moreover, biopsies from type 1 and type 2 diabetic patients with early renal damage show an increased glomerular VEGF.9, 10, 11, 12, 13 Therefore, identification of upstream mediators of VEGF overproduction is critical for identifying the pathogenesis of this disease.
Interestingly, early observations in the diabetic rat kidney showed that adenosine levels were significantly increased in the renal vein plasma compared with the renal artery.14 It has been described that the equilibrative nucleoside transporters (ENTs), characterized by its sodium-independent facilitative transport activity, could have a major contribution on adenosine availability for signaling through adenosine receptor (AR).15, 16, 17, 18, 19, 20, 21 ENTs activity mediates adenosine uptake to be either metabolized intracellularly, or to accumulate outside when the uptake activity is reduced. We have previously determined that the ENT1’s activity decreased in diabetic rats’ glomeruli22 therefore, the handling of the nucleoside could be altered in this pathologic condition.
The cellular effects of adenosine are mediated by the P1 purinoceptor family enclosing A1, A2A, A2B and A3 AR subtypes.23 Studies about the role of AR in the progression of DN in rats have attributed to the A2A subtype, a possible protective role in preventing inflammation-associated renal injury,24 while a controversial role has been attributed to A1 subtype in mediating glomerular hyperfiltration.25, 26 We have determined that the nucleoside adenosine is a regulator of the VEGF production in glomeruli of rat in vitro.27 Therefore, the correlation of adenosine levels and alterations of glomerular functions in the diabetic state, as well as the possible pharmacological intervention remain to be explored in vivo.
In this study, we show the role of adenosine A2B receptor (A2BAR) in mediating glomerular VEGF induction, which could be relevant in the pathological context because it correlates both the activity of a low-affinity receptor and the increased adenosine levels with the establishment of the diabetic glomerulopathy.
MATERIALS AND METHODS
Ex Vivo Glomeruli Assays
Glomeruli were isolated from rat kidney cortex using a differential sieving method.28 Freshly purified glomeruli (10 000 per well) were incubated in 2 ml of HAM-F10 medium (Invitrogen, Grand Island, NY, USA) supplemented with 1 μmol/l NECA (non-selective P1 receptors agonist), 50 nmol/l MRS1754 (A2BAR antagonist), 30 nmol/l CPA (A1AR agonist), 30 nmol/l DPCPX (A1AR antagonist), all from Tocris Cookson (Ellisville, MO, USA) at standard conditions (37 °C and 5% CO2) for 6 h. Also, supplementation with D-glucose 25 mM was carried out for 24 h. Five millimoles of D-glucose and supplementation with D-mannitol were included as controls. Following incubation, the glomeruli were collected by centrifugation and supernatants were stored at −70 °C. Total protein extracts were obtained from glomeruli resuspended in 150 μl RIPA buffer containing protease inhibitors 1 mM PMSF, 2 μM aprotinin, 1 μg/μl leupeptin and pepstatin (Roche, Indianapolis, IN, USA).
Short Interfering RNA
The generation of an adenoviral vector that codes a short interfering RNA targeting the sequence 5′-AACAGUAAAGACCGUGCCACC-3′ of rat A2BAR mRNA (nucleotides 540–560) or the scrambled sequence 5′-ACGUGAGACACCGAACCUAAC-3′ were constructed using pSilencer adeno 1.0-CMV System (Ambion, Austin, TX, USA). Efficient inhibition of A2BAR expression was obtained following 48 h from adenoviral infection of glomeruli in HAM-F10 medium (see Supplementary Figure 2).
Western Blots
Total proteins extracts (50 μg) fractionated by polyacrylamide gel (10%) electrophoresis were transferred to nitrocellulose membranes and probed with anti-VEGF antibody (1:1000) (ab46154 from Abcam, Cambridge, MA, USA). Membranes were washed in Tris buffer saline 0.1% Tween, and incubated 1 h in TBST/0.1% BSA containing HRP-conjugated goat anti-rabbit IgG antibody. Immunodetections were revealed by enhanced chemiluminescence and quantitated by densitometry. Following the stripping procedure, the membranes were probed with a monoclonal anti-β actin antibody (1:5000) (Sigma–Aldrich, St Louis, MO, USA) and revealed, as described above.
Enzyme-Linked Immunosorbent Assay
The amounts of VEGF secreted by glomeruli were measured by a quantitative solid-phase Enzyme-Linked Immunosorbent Assay enzyme immunoassay designed to recognize rat VEGF164 (R&D Systems, Minneapolis, MN, USA). The sensitivity of the assay was 8.4 pg/ml.
Adenine Nucleotides and Adenosine Quantifications
Total glomeruli freshly purified from individual rat were incubated in 1 ml of tyrode’s buffer at 37 °C and 5% CO2 for 1 h. Incubation medium and glomeruli were separated by centrifugation at 2000 g for 5 min. The adenine nucleotides and adenosine contents in supernatants were quantified using derivatization with chloroacetaldehyde and HPLC with fluorometric detection.22 For determination of the urinary nucleoside levels the urines of rats were recollected in metabolic cages for 24 h. Samples were processed according to previously described29 and derivatized for HPLC analysis.
Animals and Treatments
All animal studies were approved by the institutional animal care and use committee at Universidad Austral de Chile according to the NIH Guide for the Care and Use of Laboratory Animals. Diabetes was induced in male rats (Sprague-Dawley) weighing 250 g by single intravenous injection of streptozotocin 65 mg/kg (Merck, Darmstadt, Germany), dissolved in citrate buffer, pH 4.5. The diabetic groups included animals showing blood glucose levels ⩾25 mmol/l. Following 4 weeks of diabetes induction, the rats were treated with the antagonist of A2BAR MRS1754 (0.2 or 1.0 mg/kg) for 2 weeks administered via intra peritoneal, every 2 days. Control rats received an equivalent volume of vehicle. Urines of rat were recollected in metabolic cage for 24 h and protein contents were quantified by the pyrogallol red molybdate method (Proti U/LCR, Wiener Lab, Rosario, Argentina).
Immunohistochemistry
Rat kidney tissues were fixed in formalin, paraffin embedded and 5 μm sections were mounted on sylanized slides. Immunodetection was performed as described previously22 using the primary anti-A2BAR, anti-A1AR, anti-VEGF and anti-nephrin polyclonal antibodies (ab40002, ab46154 and ab58968 from Abcam), and the monoclonal anti-α-smooth muscle actin (αSMA) (sc130617 from Santa Cruz Biotechnology, Santa Cruz, CA, USA). The immunosignals were revealed using the LSAB+System–HRP system (Dako, Carpinteria, CA, USA). The podocytes number was estimated by counting Wilms tumor protein (WT)-1-stained nuclei in 30 glomeruli representatives of each group. Glomerular injury characterized by mesangial expansion was graded on the basis of the extent of glomerular staining using Periodic-acid Schiff (PAS) on a scale of 1–3 as follows: 1, normal; 2, mild; 3, moderate to severe.
Statistical Method
Values are means±s.e.m., where n indicates number of animals. Statistical analyses were carried out on raw data using the Peritz F multiple means comparison test. Student’s t-test was applied for unpaired data.
RESULTS
A2BAR Mediates VEGF Production in Rat Glomeruli
Using isolated glomeruli from rat kidney we determined the role of A2BAR on VEGF production ex vivo. The treatment of glomeruli with the general agonist of ARs induces an increase in the content of VEGF, which is in line with the previously determined increase in mRNA levels.27 This increase was blocked by MRS1754, the selective antagonist of the A2B and it was not observed when glomeruli were infected with an adenoviral vector expressing a short RNA that interferes with the expression of this AR subtype (Figure 1a). No significant changes in the glomerular content of VEGF have been observed with pharmacological modulators of other ARs.27 We determined that A2BAR-mediated VEGF production required p42/44 MAPK and PKC signaling molecules activation (Figure 1a). Particularly, we determined that p42/44 MAPK and PKCα isoform were phosphorylated upon A2BAR activation (Figures 1b and c).
Adenosine A2B receptor signaling mediates vascular endothelial growth factor (VEGF) overexpression in rat glomeruli. (a) The content of VEGF was quantified in glomeruli exposed ex vivo to the general adenosine receptor (ARs) agonist NECA (non-selective P1 receptors agonist) alone or in combination with a selective antagonist of adenosine A2B receptor (A2BAR) (MRS1754), a general inhibitor of PKC (Calphostin C) or the MAPK activation inhibitor (PD98059) for 24 h. Also, the inhibition of the A2BAR expression by siRNA (siRNA A2BAR) was evaluated. When indicated glomeruli were exposed to 25 mM D-glucose (HG) as control of increased VEGF production. The upper images show a representative western blot detection of VEGF content in total protein extracts (50 μg) from treated glomeruli. The graph depicts the ratio between immune signals of VEGF vs β-actin. (b, c) The activation of PKCα and ERK1/2 was quantified by the detection of phosphorylated forms in total protein extracts of glomeruli (50 μg) by western blots. The graphs show the ratio between phosphorylated vs total content of the signaling proteins. (d) Representative western blot analysis of the effect of siRNA-mediated inhibition of A2BAR and scrambled siRNA on VEGF induction by NECA. All graphs represent the means±s.e.m. *P<0.01 vs control without treatment; #P<0.01 vs NECA; a–c n=9, d n=4.
Released VEGF was also increased when the general AR agonist NECA was used. This effect was blocked by MRS1754 the selective antagonist of A2BAR (Figure 2a). In contrast, the selective agonist of A1AR decreased the basal release of VEGF from glomeruli. This effect could be blocked by using DPCPX, the selective antagonist of A1AR (Figure 2b).
Role of A1AR and adenosine A2B receptor (A2BAR) on VEGF release. The release of VEGF from glomeruli was assessed by Enzyme-Linked Immunosorbent Assay. (a) Rat glomeruli were incubated by 6 h in the absence (control) or presence of the general AR agonist (non-selective P1 receptors agonist) alone or in combination with a selective A2BAR antagonist (MRS1754). (b) The role of A1AR on VEGF release was assayed using the selective agonist CPA and the antagonist DPCPX. The graphs show the means±s.e.m. of VEGF content values in the supernatants. *P<0.01 vs control without treatment; #P<0.01 vs NECA or CPA; n=9.
Experimental Diabetes Increases the Expression of A2BAR and VEGF in Kidney Glomeruli
The distribution of A2BAR was assessed in rats’ kidney by immunohistochemistry. The expression pattern of A2BAR resembles that of VEGF in the glomeruli of healthy rats (Figure 3). As early as 3 weeks following diabetes induction, we detected a stronger immunosignal and a wide distribution of A2BAR in glomerular cells. Similarly, VEGF content was notably increased (Figure 3). In contrast, the expression of the adenosine A1 receptor subtype appears to decrease in diabetic rats glomeruli (Figure 3).
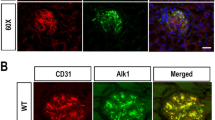
Glomerular changes in the expression of adenosine receptors (ARs) induced by experimental diabetes. Following 3 weeks of diabetes induction the expression of ARs in glomeruli were detected by immunohistochemistry. Similarly, the increased glomerular expression of vascular endothelial growth factor (VEGF) at this stage was evidenced in kidney sections. Original magnification × 400. Scale bars 50 μm. The analyses of 50 glomeruli per slide in each condition were performed using the UN-SCANIT 2.0 software. The graphs depict the quantification of intensity of immune signals in glomeruli of rats, normalizing the value of vehicle-treated rats to 1. *P<0.01 vs vehicle, n=6.
Glomerular Adenosine Availability
Owing to the fact that the A2BAR exhibits a low affinity for the ligand,23 changes in the extracellular adenosine availability should occur to mediate the physiologic effects. We quantified the extracellular concentration of adenine nucleotides and adenosine in glomeruli isolated from healthy and STZ-induced diabetic rats. Following 3 weeks of diabetes induction the contents of ATP, ADP and AMP were not different to the levels seen in normal rats glomeruli (Figure 4a). However, a notably increase in the extracellular levels of adenosine were quantified in glomeruli of STZ-induced diabetic rats (Figure 4a).
Adenosine contents in streptozotocin-induced diabetic rat. (a) Adenine nucleotides and adenosine levels were quantified by HPLC in glomeruli of control (□) and diabetic rats (▪) following 3 weeks of diabetes induction. The graph shows the means±s.e.m. from individual determinations normalized to 1 μg of total glomerular proteins. *P<0.01, n=7. (b) The adenosine contents in urine of rats were quantified following 4 weeks of diabetes induction. The graph shows individual determinations and horizontal line represents the mean value for control or diabetic group. P=0.038, n=7.
Furthermore, there was a correlation between the altered glomerular adenosine handling and the urinary excretion of the nucleoside. The mean adenosine urinary excretion rate was increased more than twofold in diabetic rats (Figure 4b).
Blockage of Diabetes-Induced VEGF Overproduction in MRS1754-Treated Rats
The exposure of ex vivo glomeruli to high glucose concentration induced an overproduction of VEGF (Figure 5a). This result was specific to high glucose levels as using mannitol as osmotic control did not alter the content of VEGF (Figure 5b). We observed that this high glucose effect was blocked when using the A2BAR antagonist, by knocking down the receptor expression or using the PKC and ERK activation inhibitors (Figure 5a).
Role of adenosine in high glucose-induced vascular endothelial growth factor (VEGF) overproduction. (a) The content of VEGF was quantified in glomeruli exposed ex vivo to D-glucose 25 mM in combination with a selective antagonist of adenosine A2B receptor (A2BAR) (MRS1754), a siRNA interfering with A2BAR expression, a general inhibitor of PKC (Calphostin C) or the MAPK activation inhibitor (PD98059) for 24 h. The upper image shows a representative western blot detection of VEGF content in total protein extracts (50 μg) from treated glomeruli. The graph depicts the ratio between immune signals of VEGF vs β-actin. Control experiments contained D-glucose 5 mM. The graph represents the means±s.e.m. *P<0.01 vs D-glucose 5 mM; #P<0.01 vs D-glucose 25 mM; n=5. (b) The content of VEGF was evaluated in isolated glomeruli exposed to glucose 5 mM, glucose 25 mM and glucose 5 mM supplemented with mannitol 20 mM as osmotic control for 24 h. The figure is a representative western blot analysis showing that increased expression of VEGF was specific to high glucose concentration. The graph shows the means±s.e.m. *P<0.01 vs D-glucose 5 mM; n=4.
In vivo analysis of the A2BAR role on VEGF production were carried out in STZ-induced diabetic rats treated with the selective antagonist MRS1754. Following 4 weeks of diabetes induction, the administration of MRS1754 for 14 days blocked the glomerular increase in the expression of VEGF compared with vehicle-treated diabetic group (Figures 6a and b). The expression of the slit diaphragm protein nephrin was partially recovered following the treatment with the antagonist (Figures 6a and c, and Supplementary Figure 1), and the increase in the urinary excretion of proteins induced by diabetes was blocked by the treatment using MRS1754 (Figure 6e).
In vivo evaluation of an adenosine A2B receptor (A2BAR) antagonist in experimental diabetic rats. Following 4 weeks of diabetes induction the rats were treated by 14 days with the selective A2BAR antagonist MRS1754 in doses of 0.2 and 1.0 mg/kg of body weight (see Materials and Methods). (a) Glomerulopathy was detected by vascular endothelial growth factor (VEGF), nephrin, α-smooth muscle actin (α-SMA) and Wilms tumor protein (WT-1) immunohistochemistry. Also Periodic acids-Schiff staining (PAS) was included. Original magnification × 400. Scale bars 50 μm. (b, c) The graphs depict the quantification of immune signals intensity in rats glomeruli, normalizing the value of normal rats to 1. #P<0.01 vs diabetes, n=12. (d) The graph shows the percentage of α-SMA-stained glomeruli from total glomeruli on each slide. #P<0.01 vs diabetes, n=12. (e) Total urinary protein contents were quantified in STZ-induced diabetic rats treated with MRS1754. *P<0.01, n=7. (f) Podocyte number was estimated from immunohistochemical staining of nuclear WT-1. The graph depicts the means of positive nuclei in 30 glomeruli of each group. *P<0.01, n=12. (g) The grade of mesangial expansion from normal to severe (1–3) was estimated in PAS-stained glomeruli of each group. The graph shows the means of 30 glomeruli graded in each group.
Furthermore, the glomerular expression of αSMA, a mesangial cells myofibroblast transdifferentiation marker, was also blocked in the kidney of diabetic rats under the treatment with the A2BAR antagonist (Figures 6a and d). The blockade of VEGF induction and mesangial cells activation was in an early stage of glomerular dysfunction as only a decrease in the podocytes number was quantified while mesangial expansion has not yet occurred. A significant difference was detected in the patterns of glomerular WT-1 in all diabetic groups compared with healthy rats (Figures 6a and f). The treatment with MRS1754 did not modify the decreased glomerular WT-1 imnunosignals in diabetic rats. PAS staining was not changed by diabetes or treatment with the antagonist of A2BAR in our experimental conditions (Figures 6a and g).
The treatment with the A2BAR antagonist did not alter the increased levels of plasma glucose in the STZ-induced diabetic rats. However, partial recovery of body weight was observed in rats following treatment with the antagonist (Table 1).
DISCUSSION
We demonstrate that the activity of A2BAR has a pathogenic effect in the early glomerular dysfunctions observed in STZ-induced diabetic rats and it can be blocked by using a selective antagonist in vivo. These alterations mediated by A2BAR correlate with an increased expression of this receptor in rats’ diabetic glomerulus. Furthermore, the pathogenic state also involves a decrease in the content of A1AR subtype in glomerular cells. This event, first described by Pawelczyk et al,30 probably turns off the inhibitory effects on glomerular VEGF release accompanied with an increased production of this growth factor, as a consequence of the modulation of ARs activities by differential expression in the diabetic state.
We also correlate the activity of a low-affinity AR with an increase in the ligand availability in glomeruli of diabetic rats. Interestingly, it was found elevated adenosine levels in plasma of clinically manifest DN patients compared with the basal levels of diabetic patients without DN and in healthy individuals.31 Probably, the measurement of adenosine levels in plasma or urine could represent a novel specific marker to evaluate the progression of DN.
Recently, the pathogenic role of adenosine in mediating renal dysfunction and fibrosis in the adenosine desaminase knockout (ADA−/−) mice model, with increased levels of the nucleoside, was described.32 In addition, the progression of renal fibrosis generated in the ADA−/− animals or in mice infused with angiotensin II (Ang II)or subjected to unilateral ureteral obstruction can be blocked using an A2BAR antagonist, suggesting a common pathogenic pathway involving adenosine signaling in chronic kidney disease.32 Our major contribution is to demonstrate that this pathogenic pathway also occurs early in the progression of the renal disease derived from diabetes thus supporting the option of a DN pharmacological A2BAR target intervention.
The pathomechanisms of DN converge in inducing a host of growth factors in the kidney. The fibrogenic cytokine transforming growth factor-beta 1 (TGF-β), through its Smad3 signaling pathway, is the etiologic agent of renal hypertrophy and the accumulation of mesangial extracellular matrix components and tubule-interstitial fibrosis in diabetes. However, there is limited evidence to support a role for TGF-β in the development of albuminuria. Podocyte-derived VEGF is a permeability and angiogenic factor whose expression is also increased in diabetic kidney diseases animal models. It appears to act in an autocrine signaling mode to induce the podocytopathy of diabetes, especially the genesis of proteinuria.33 Therefore, currently strategies for DN therapy may need to involve interception of both the TGF-β and the VEGF signaling pathways. In this way, the A2BAR antagonist could be a valuable tool because it was demonstrated that it is able to block the increased release of TGF-β from diabetic glomeruli in vitro22 and the myofibroblast transdifferentiation of masangial cells in vivo, as reported in this work. Similarly, interception of VEGF induction was a remarkable feature.
Studies have shown that the VEGF expression in renal podocytes increased upon exposure to high glucose concentration and it is intracellularly mediated by PKC-alpha and ERK1/2 signaling molecules.34, 35 In addition, cultured podocytes exposed to high glucose concentration exhibit increased levels of extracellular adenosine.36 Previously, we showed that the VEGF production increase in ex vivo glomeruli exposed to high glucose concentration could be blocked by MRS1754.27 In consequence, our study in vivo suggests that A2BAR could be a transducer of hyperglycemic conditions to mediate VEGF increase. Up to date, Ang II has been recognized as the major factor to increase VEGF expression in diabetic glomerular podocytes.37 Intra-renal renin and angiotensinogen levels are induced in diabetic animals,38, 39 and high glucose has been shown to stimulate renin and Ang II synthesis in mesangial cells and podocytes.37, 40, 41 Further, the role of notch I signaling have also been recently associated with pathogenic VEGF induction and podocytopathy.42 It remains to be determined if the use of A2BAR antagonist could also intercept the activation of the renin–angiotensin system or notch I signaling.
The extracellular adenosine availability was shown to increase in diabetic glomeruli as shown by the higher urinary nucleoside levels. This effect could be linked to a decreased activity of ENT1 measured in isolated diabetic glomeruli.22 Similar to our finding, ENT1 activity was found to be decreased in human endothelial cells isolated from gestational diabetes pregnancy43 or in cells exposed to high glucose concentrations.44, 45 This decreased activity of ENT1 elicits adenosine signaling by ARs as previously described, using inhibitors of ENT1 activity or in ENT1−/− mice.10, 19, 20 Interestingly, a correlation between ENT1 decreased activity with epithelium mesenchymal transition (EMT) of renal proximal tubule epithelial cells in vitro, was recently demonstrated.46 EMT is a requisite for progression of tubule-interstitial fibrosis in the diabetic kidney disease.
Collectively, these findings support a pathogenic role of adenosine and A2B receptor subtype in mediating early states of renal dysfunction in DN, and also suggest a possible pharmacological target for intervention. Furthermore, it has been described that A2BAR blockade reverses insulin resistance in type II diabetes animal models.47 Therefore, A2BAR blockers useful in humans such as CVT-6883 are being developed,18 and would represent a novel alternative for management of DN patients.
References
Yach D, Stuckler D, Brownell KD . Epidemiologic and economic consequences of the global epidemics of obesity and diabetes. Nat Med 2006;12:62–66.
Gross JL, De Azevedo MJ, Silveiro SP et al. Diabetic nephropathy: diagnosis, prevention, and treatment. Diab Care 2005;28:164–176.
Brenner BM, Cooper ME, De Zeeuw D et al. Effects of losartan on renal and cardiovascular outcomes in patients with type 2 diabetes and nephropathy. N Engl J Med 2001;345:861–869.
Lewis EJ, Hunsicker LG, Clarke WR et al. Renoprotective effect of the angiotensin-receptor antagonist irbesartan in patients with nephropathy due to type 2 diabetes. N Engl J Med 2001;345:851–860.
Cooper M . Pathogenesis, prevention, and treatment of diabetic nephropathy. Lancet 1998;352:213–219.
Nakagawa T . A new mouse model resembling human diabetic nephropathy: uncoupling of VEGF with eNOS as a novel pathogenic mechanism. Clin Nephrol 2009;71:103–109.
Liu E, Morimoto M, Kitajima S et al. Increased expression of vascular endothelial growth factor in kidney leads to progressive impairment of glomerular functions. J Am Soc Nephrol 2007;18:2094–2104.
Veron D, Bertuccio C, Marlier A et al. Podocyte vascular endothelial growth factor (Vegf164) overexpression causes severe nodular glomerulosclerosis in a mouse model of type 1 diabetes. Diabetologia 2011;54:1227–1241.
Cha DR, Kim NH, Yoon JW et al. Role of vascular endothelial growth factor in diabetic nephropathy. Kidney Int Suppl 2000;77:S104–S112.
Gröne HJ, Simon M, Gröne EF . Expression of VEGF in renal vascular disease and renal allografts. J Pathol 1995;177:259–267.
Shulman K, Rosen S, Tognazzi K et al. Expression of vascular permeability factor (VPF/VEGF) is altered in many glomerular diseases. J Am Soc Nephrol 1996;7:661–666.
Kanesaki Y, Suzuki D, Uehara G et al. VEGF gene expression is correlated with glomerular neovascularization in human diabetic nephropathy. Am J Kidney Dis 2005;45:288–294.
Baelde H, Eikmans M, Lappin D et al. Reduction of VEGF-A and CTGF expression in diabetic nephropathy is associated with podocyte loss. Kidney Int 2007;71:637–645.
Angielski S, Jakubowski Z, Pawelczyk T et al. Renal handling and metabolism of adenosine in diabetic rats. Contrib Nephrol 1989;73:52–57.
Mubagwa K, Flameng W . Adenosine, adenosine receptors and myocardial protection: an updated overview. Cardiovasc Res 2001;52:25–39.
Ackley MA, Governo RJ, Cass CE et al. Control of glutamatergic neurotransmission in the rat spinal dorsal horn by the nucleoside transporter ENT1. J Physiol 2003;548:507–517.
Sonoki K, Iwase M, Iino K et al. Dilazep and fenofibric acid inhibit MCP-1 mRNA expression in glycoxidized LDL-stimulated human endothelial cells. Eur J Pharmacol 2003;475:139–147.
Gadalla AE, Pearson T, Currie AJ et al. AICA riboside both activates AMP-activated protein kinase and competes with adenosine for the nucleoside transporter in the CA1 region of the rat hippocampus. J Neurochem 2004;88:1272–1282.
Choi DS, Cascini MG, Mailliard W et al. The type 1 equilibrative nucleoside transporter regulates ethanol intoxication and preference. Nat Neurosci 2004;7:855–861.
Riksen NP, Rongen GA, Boers GH et al. Enhanced cellular adenosine uptake limits adenosine receptor stimulation in patients with hyperhomocysteinemia. Arterioscler Thromb Vasc Biol 2005;25:109–114.
Carrier EJ, Auchampach JA, Hillard CJ . Inhibition of an equilibrative nucleoside transporter by cannabidiol: a mechanism of cannabinoid immunosuppression. Proc Natl Acad Sci USA 2006;103:7895–7900.
Roa H, Gajardo C, Troncoso E et al. Adenosine mediates transforming growth factor-beta 1 release in kidney glomeruli of diabetic rats. FEBS Lett 2009;583:3192–3198.
Fredholm B, IJzerman A, Jacobson K et al. International Union of Basic and Clinical Pharmacology. LXXXI. Nomenclature and classification of adenosine receptors—an update. Pharmacol Rev 2011;63:1–34.
Awad A, Huang L, Ye H et al. Adenosine A2A receptor activation attenuates inflammation and injury in diabetic nephropathy. Am J Physiol Renal Physiol 2006;290:F828–F837.
Vallon V, Schroth J, Satriano J et al. Adenosine A1 receptors determine glomerular hyperfiltration and the salt paradox in early streptozotocin diabetes mellitus. Nephron Physiol 2009;111:30–38.
Faulhaber-Walter R, Chen L, Oppermann M et al. Lack of A1 adenosine receptors augments diabetic hyperfiltration and glomerular injury. J Am Soc Nephrol 2008;19:722–730.
Valladares D, Quezada C, Montecinos P et al. Adenosine A2B receptor mediates an increase on VEGF-A production in rat kidney glomeruli. Biochem Biophys Res Commun 2008;366:180–185.
Quezada C, Alarcón S, Cárcamo JG et al. Increased expression of the multidrug resistance-associated protein 1 (MRP1) in kidney glomeruli of streptozotocin induced diabetic rats. Biol Chem 2011;392:529–537.
Zhang Y, Geiger J, Lautt W . Improved high-pressure liquid chromatographic-fluorometric assay for measurement of adenosine in plasma. Am J Physiol 1999;260:G658–G664.
Pawelczyk T, Grden M, Rzepko R et al. Region-specific alterations of adenosine receptors expression level in kidney of diabetic rat. Am J Pathol 2005;167:315–325.
Xia JF, Liang QL, Hu P et al. Correlations of six related purine metabolites and diabetic nephropathy in Chinese type 2 diabetic patients. Clin Biochem 2009;42:215–220.
Dai Y, Zhang W, Wen J et al. A2B adenosine receptor–mediated induction of IL-6 promotes CKD. J Am Soc Nephrol 2011;22:890–901.
Ziyadeh FN . Different roles for TGF-beta and VEGF in the pathogenesis of the cardinal features of diabetic nephropathy. Diabetes Res Clin Pract 2008;82:S38–S41.
Hoshi S, Nomoto K, Kuromitsu J et al. High glucose induced VEGF expression via PKC and ERK in glomerular podocytes. Biochem Biophys Res Commun 2002;290:177–184.
Lee EY, Chung CH, Kim JH et al. Antioxidants ameliorate the expression of vascular endothelial growth factor mediated by protein kinase C in diabetic podocytes. Nephrol Dial Transplant 2006;21:1496–1503.
Karczewska J, Piwkowska A, Rogacka D et al. Purinergic modulation of glucose uptake into cultured rat podocytes: effect of diabetic milieu. Biochem Biophys Res Commun 2011;404:723–727.
Yoo TH, Li JJ, Kim JJ et al. Activation of the renin-angiotensin system within podocytes in diabetes. Kidney Int 2007;71:1019–1027.
Anderson S, Jung FF, Ingelfinger JR . Renal renin-angiotensin system in diabetes: functional, immunohistochemical, and molecular biological correlations. Am J Physiol 1993;265:F477–F486.
Zimpelmann J, Kumar D, Levine DZ et al. Early diabetes mellitus stimulates proximal tubule renin mRNA expression in the rat. Kidney Int 2000;58:2320–2330.
Singh R, Singh AK, Alavi N et al. Mechanism of increased angiotensin II levels in glomerular mesangial cells cultured in high glucose. J Am Soc Nephrol 2003;14:873–880.
Vidotti DB, Casarini DE, Cristovam PC et al. High glucose concentration stimulates intracellular renin activity and angiotensin II generation in rat mesangial cells. Am J Physiol 2004;286:F1039–F1045.
Lin CL, Wang FS, Hsu YC et al. Modulation of notch-1 signaling alleviates vascular endothelial growth factor-mediated diabetic nephropathy. Diabetes 2010;59:1915–1925.
Farías M, San Martín R, Puebla C et al. Nitric oxide reduces adenosine transporter ENT1 gene (SLC29A1) promoter activity in human fetal endothelium from gestational diabetes. J Cell Physiol 2006;208:451–460.
Sakowicz M, Szutowicz A, Pawelczyk T . Insulin and glucose induced changes in expression level of nucleoside transporters and adenosine transport in rat T lymphocytes. Biochem Pharmacol 2004;68:1309–1320.
Aguayo C, Casado J, Gonzalez M et al. Equilibrative nucleoside transporter 2 is expressed in human umbilical vein endothelium, but is not involved in the inhibition of adenosine transport induced by hyperglycaemia. Placenta 2005;26:641–653.
Guillén-Gómez E, Pinilla-Macua I, Pérez-Torras S et al. New Role of the human equilibrative nucleoside transporter 1 (hENT1) in epithelial-to-mesenchymal transition in renal tubular cells. J Cell Physiol 2012;227:1521–1528.
Rüsing D, Müller C, Verspohl E . The impact of adenosine and A2B receptors on glucose homoeostasis. J Pharm Pharmacol 2006;58:1639–1645.
Acknowledgements
This work was funded by grants FONDECYT 1100484 and CONICYT-PIA ANILLO ACT73.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The author declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Laboratory Investigation website
A new pathogenic mechanism for the onset of diabetic kidney disease is proposed. Aberrant adenosine signaling in glomeruli promotes excessive VEGF production, leading to the progression of diabetic glomerulopathy. The adenosine A2B receptor is thus a new target for pharmacological intervention in diabetic kidney disease.
Supplementary information
Rights and permissions
About this article
Cite this article
Cárdenas, A., Toledo, C., Oyarzún, C. et al. Adenosine A2B receptor-mediated VEGF induction promotes diabetic glomerulopathy. Lab Invest 93, 135–144 (2013). https://doi.org/10.1038/labinvest.2012.143
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/labinvest.2012.143
Keywords
This article is cited by
-
Deficient Insulin-mediated Upregulation of the Equilibrative Nucleoside Transporter 2 Contributes to Chronically Increased Adenosine in Diabetic Glomerulopathy
Scientific Reports (2017)
-
Adenosine signalling in diabetes mellitus—pathophysiology and therapeutic considerations
Nature Reviews Endocrinology (2015)
-
The role of adenosine receptors A2A and A2B signaling in renal fibrosis
Kidney International (2014)
-
Therapeutic approaches to diabetic nephropathy—beyond the RAS
Nature Reviews Nephrology (2014)