Abstract
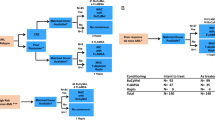
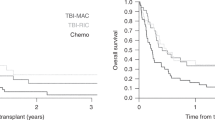
Sixty-two infants with MLL gene-rearrangement-positive acute lymphoblastic leukemia (MLL-r ALL) were treated with the MLL03 protocol of the Japanese Pediatric Leukemia/Lymphoma Study Group: short-course intensive chemotherapy followed by early allogeneic hematopoietic stem cell transplantation (HSCT) within 4 months of the initial induction. The 4-year event-free survival and overall survival rates were 43.2% (95% confidence interval (CI)=30.7–55.1%) and 67.2% (53.8–77.4%), respectively. A univariate analysis showed younger age (<90 days at diagnosis), central nervous system disease and poor response to initial prednisolone therapy significantly associated with poor prognosis (P<0.05). In a multivariate analysis, younger age at diagnosis tended to be associated with poor outcome (hazard ratio=1.969; 95% CI=0.903–4.291; P=0.088). Although the strategy of early use of HSCT effectively prevented early relapse and was feasible for infants with MLL-r ALL, the fact that substantial number of patients still relapsed even though transplanted in their first remission indicates the limited efficacy of allogeneic HSCT for infants with MLL-r ALL. Considering the risk of severe late effects, indications for HSCT should be restricted to specific subgroups with poor risk factors. An alternative approach incorporating molecular-targeted drugs should be established.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Pui CH, Kane JR, Crist WM . Biology and treatment of infant leukemias. Leukemia 1995; 9: 762–769.
Armstrong SA, Staunton JE, Silverman LB, Pieters R, den Boer ML, Minden MD et al. MLL translocations specify a distinct gene expression profile that distinguishes a unique leukemia. Nat Genet 2002; 30: 41–47.
Pieters R, Schrappe M, de Lorenzo P, Hann I, De Rossi G, Felice M et al. A treatment protocol for infants younger than 1 year with acute lymphoblastic leukaemia (Interfant-99): an observational study and a multicentre randomised trial. Lancet 2007; 370: 240–250.
Tomizawa D, Koh K, Sato T, Kinukawa N, Isoyama K, Kosaka Y et al. Outcome of risk-based therapy for infant acute lymphoblastic leukemia with or without an MLL gene rearrangement, with emphasis on late effects: a final report of two consecutive studies, MLL96 and MLL98, of the Japan Infant Leukemia Study Group. Leukemia 2007; 21: 2258–2263.
Hilden JM, Dinndorf PA, Meerbaum SO, Sather H, Villaluna D, Heerema NA et al. Analysis of prognostic factors of acute lymphoblastic leukemia in infants: report on CCG 1953 from the Children's Oncology Group. Blood 2006; 108: 441–451.
Silverman LB, McLean TW, Gelber RD, Donnelly MJ, Gilliland DG, Tarbell NJ et al. Intensified therapy for infants with acute lymphoblastic leukemia: results from the Dana-Farber Cancer Institute Consortium. Cancer 1997; 80: 2285–2295.
Biondi A, Rizzari C, Valsecchi MG, de Lorenzo P, Aricò M, Basso G et al. Role of treatment intensification in infants with acute lymphoblastic leukemia: results of two consecutive AIEOP studies. Haematologica 2006; 91: 534–537.
Dördelmann M, Reiter A, Borkhardt A, Ludwig WD, Götz N, Viehmann S et al. Prednisone response is the strongest predictor of treatment outcome in infant acute lymphoblastic leukemia. Blood 1999; 94: 1209–1217.
Ferster A, Benoit Y, Francotte N, Dresse MF, Uyttebroeck A, Plouvier E et al. Treatment outcome in infant acute lymphoblastic leukemia. Children Leukemia Cooperative Group—EORTC. European Organization for Research and Treatment of Cancer. Blood 2000; 95: 2729–2731.
Chessells JM, Harrison CJ, Watson SL, Vora AJ, Richards SM . Treatment of infants with lymphoblastic leukaemia: results of the UK Infant Protocols 1987-1999. Br J Haematol 2002; 117: 306–314.
Kosaka Y, Koh K, Kinukawa N, Wakazono Y, Isoyama K, Oda T et al. Infant acute lymphoblastic leukemia with MLL gene rearrangements: outcome following intensive chemotherapy and hematopoietic stem cell transplantation. Blood 2004; 104: 3527–3534.
Isoyama K, Eguchi M, Hibi S, Kinukawa N, Ohkawa H, Kawasaki H et al. Risk-directed treatment of infant acute lymphoblastic leukaemia based on early assessment of MLL gene status: results of the Japan Infant Leukaemia Study (MLL96). Br J Haematol 2002; 118: 999–1010.
Pieters R, den Boer ML, Durian M, Janka G, Schmiegelow K, Kaspers GJL et al. Relation between age, immunophenotype and in vitro drug resistance in 395 children with acute lymphoblastic leukemia–implications for treatment of infants. Leukemia 1998; 12: 1344–1348.
Nakamura H, Sato T, Okada K, Miura G, Ariyoshi N, Nakazawa K et al. Population pharmacokinetics of oral busulfan in young Japanese children before hematopoietic stem cell transplantation. Ther Drug Monit 2008; 30: 75–83.
Salzer WL, Jones TL, Devidas M, Hilden JM, Winick N, Hunger S et al. Modifications to induction therapy decrease risk of early death in infants with acute lymphoblastic leukemia treated on Children's Oncology Group P9407. Pediatr Blood Cancer 2012; 59: 834–839.
Tomizawa D, Koh K, Hirayama M, Miyamura T, Hatanaka M, Saikawa Y et al. Outcome of recurrent or refractory acute lymphoblastic leukemia in infants with MLL gene rearrangements: a report from the Japan Infant Leukemia Study Group. Pediatr Blood Cancer 2009; 52: 808–813.
Schechter T, Finkelstein Y, Doyle J, Verjee Z, Moretti M, Koren G et al. Pharmacokinetic disposition and clinical outcomes in infants and children receiving intravenous busulfan for allogeneic hematopoietic stem cell transplantation. Biol Blood Marrow Transplant 2007; 13: 307–314.
Pui C-H, Gaynon PS, Boyett JM, Chessells JM, Baruchel A, Kamps W et al. Outcome of treatment in childhood acute lymphoblastic leukaemia with rearrangements of the 11q23 chromosomal region. Lancet 2002; 359: 1909–1915.
Dreyer ZE, Dinndorf PA, Camitta B, Sather H, La MK, Devidas M et al. Analysis of the role of hematopoietic stem-cell transplantation in infants with acute lymphoblastic leukemia in first remission and MLL gene rearrangements: a report from the Children's Oncology Group. J Clin Oncol 2011; 29: 214–222.
Stumpel DJPM Schneider P, van Roon EHJ, Boer JM, de Lorenzo P, Valsecchi MG et al. Specific promoter methylation identifies different subgroups of MLL-rearranged infant acute lymphoblastic leukemia, influences clinical outcome, and provides therapeutic options. Blood 2009; 114: 5490–5498.
Bernt KM, Zhu N, Sinha AU, Vempati S, Faber J, Krivtsov AV et al. MLL-rearranged leukemia is dependent on aberrant H3K79 methylation by DOT1L. Cancer Cell 2011; 20: 66–78.
Daigle SR, Olhava EJ, Therkelsen CA, Majer CR, Sneeringer CJ, Song J et al. Selective killing of mixed lineage leukemia cells by a potent small-molecule DOT1L inhibitor. Cancer Cell 2011; 20: 53–65.
Mann G, Attarbaschi A, Schrappe M, De Lorenzo P, Peters C, Hann I et al. Improved outcome with hematopoietic stem cell transplantation in a poor prognostic subgroup of infants with mixed-lineage-leukemia (MLL)-rearranged acute lymphoblastic leukemia: results from the Interfant-99 Study. Blood 2010; 116: 2644–2650.
Acknowledgements
We thank all JPLSG investigators and the following investigators who contributed to the central diagnosis in this study: H Nakamura and S Yamagata (Chiba University, Chiba) for the BU pharmacokinetic study; Y Komada (Mie University Graduate School of Medicine, Mie) and H Ohta (Osaka University, Osaka) for immunophenotypic diagnostics; T Taki (Kyoto Prefectural University of Medicine, Kyoto) for the molecular biological analyses; and J Fujimoto (National Center for Child Health and Development, Tokyo) for the preservation of the diagnostic specimens. This work was supported by a Grant for Clinical Cancer Research and a Grant-in-Aid for Cancer Research from the Ministry of Health, Labour and Welfare of Japan.
Author Contributions
K Koh, DT, TM, MH, Y Takahashi, AO, K Kato, KS and EI (principal investigator) participated actively in the study conception and design; K Koh, DT and EI reviewed the data analysis and interpretation and were the main authors of the manuscript; AMS and TW conducted the statistical analysis; TS was responsible for the busulfan pharmacokinetic study; TD and MT were responsible for the immunophenotyping diagnostics; YH was responsible for coordinating the molecular biology analyses; K Koh, K Kato, JT and Y Takeshita recruited patients; MT, KH and SM contributed to the financial and administrative support of the study; and all authors contributed to the conduct of the trial and were involved in the review of the results and the final approval of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies this paper on the Leukemia website
Supplementary information
Rights and permissions
About this article
Cite this article
Koh, K., Tomizawa, D., Moriya Saito, A. et al. Early use of allogeneic hematopoietic stem cell transplantation for infants with MLL gene-rearrangement-positive acute lymphoblastic leukemia. Leukemia 29, 290–296 (2015). https://doi.org/10.1038/leu.2014.172
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/leu.2014.172
This article is cited by
-
Evolution and optimization of therapies for acute lymphoblastic leukemia in infants
International Journal of Hematology (2023)
-
Multi-omics analysis defines highly refractory RAS burdened immature subgroup of infant acute lymphoblastic leukemia
Nature Communications (2022)
-
Acute Leukemia in Infants
Current Oncology Reports (2021)
-
Panel-based next-generation sequencing identifies prognostic and actionable genes in childhood acute lymphoblastic leukemia and is suitable for clinical sequencing
Annals of Hematology (2019)
-
Personalized pharmacokinetic targeting with busulfan in allogeneic hematopoietic stem cell transplantation in infants with acute lymphoblastic leukemia
International Journal of Hematology (2019)