Abstract
The decline of tissue regenerative potential is a hallmark of ageing and may be due to age-related changes in tissue-specific stem cells1,2,3,4,5. A decline in skeletal muscle stem cell (satellite cell) activity due to a loss of Notch signalling results in impaired regeneration of aged muscle1,6. The decline in hepatic progenitor cell proliferation owing to the formation of a complex involving cEBP-α and the chromatin remodelling factor brahma (Brm) inhibits the regenerative capacity of aged liver7. To examine the influence of systemic factors on aged progenitor cells from these tissues, we established parabiotic pairings (that is, a shared circulatory system) between young and old mice (heterochronic parabioses), exposing old mice to factors present in young serum. Notably, heterochronic parabiosis restored the activation of Notch signalling as well as the proliferation and regenerative capacity of aged satellite cells. The exposure of satellite cells from old mice to young serum enhanced the expression of the Notch ligand (Delta), increased Notch activation, and enhanced proliferation in vitro. Furthermore, heterochronic parabiosis increased aged hepatocyte proliferation and restored the cEBP-α complex to levels seen in young animals. These results suggest that the age-related decline of progenitor cell activity can be modulated by systemic factors that change with age.
Similar content being viewed by others
Main
Ageing of metazoans can be generally characterized as a progressive decline of tissue and organ function, accompanied by increased oxidative damage8, mitochondrial dysfunction9, endocrine imbalance10 and genome instability11. Tissue regenerative capacity also declines with age, and in tissues such as muscle, blood, liver and brain this decline has been attributed to a diminished responsiveness of tissue-specific stem and progenitor cells1,3,4,5. Our previous work demonstrated that signalling through the Notch pathway is essential for the activation, proliferation and myogenic lineage progression of satellite cells necessary for muscle repair6, and that the decline in the regenerative potential of muscle with age is due to the failure of this pathway to be activated1. However, the activation of aged satellite cells and the regenerative potential of aged muscle can be restored by forced activation of Notch, demonstrating that the intrinsic regenerative capacity of aged satellite cells remains intact1. Aged muscle successfully regenerates when grafted into muscle in a young host, but young muscle displays impaired regeneration when grafted into an aged host12,13. We hypothesized that there are systemic factors that support the robust regeneration of tissues in young animals and/or inhibit regeneration in old animals, and that these factors act to modulate the key molecular pathways that control the regenerative properties of progenitor cells. The implication of this hypothesis is that old tissues might be made to regenerate as well as young tissues if, by means of systemic influences, the molecular pathways could be ‘rejuvenated’ from an old state to a young state.
To test this hypothesis we set up an experimental system in which—in contrast to transplantation—regenerating tissues in aged animals could be exposed only to the circulating factors of young animals, and vice versa. We established parabiotic pairings between young and old mice (heterochronic parabioses)14, with parabiotic parings between two young mice or two old mice (isochronic parabioses) as controls. In parabiosis, animals develop vascular anastomoses and thus a single, shared circulatory system. Previous work examining the effects of heterochronic parabiosis showed that such pairings may alter tissue function15,16,17, but the effects on progenitor cell activity or tissue regeneration have not been examined.
We examined the efficacy of muscle regeneration in young (2–3 months) and aged (19–26 months) mice in heterochronic and isochronic pairings. Young partners were either transgenic for green fluorescent protein (GFP), expressed from the constitutive β-actin promoter, or expressed a distinct CD45 allele (Ly5.2/CD45.1), allowing confirmation of blood chimaerism (Supplementary Fig. S1)18. The use of GFP-transgenic mice as one member of a pair also allowed us to distinguish the cells from each animal participating in tissue regeneration. After 5 weeks of parabiosis the hindlimb muscles of each mouse were injured and the mice were given 5-bromodeoxyuridine (BrdU) injections6. After muscle injury, satellite cells activate and give rise to proliferative myoblasts, which ultimately fuse to form nascent myofibres (myotubes) that maintain centrally located nuclei and express embryonic myosin heavy chain (eMHC), a specific marker of regenerating myotubes in adult animals. Five days after injury, muscles in young mice in both isochronic and heterochronic parabioses had regenerated robustly, as demonstrated by the appearance of centrally nucleated, eMHC-expressing myotubes (Fig. 1a) formed from proliferating progenitor cells (Supplementary Fig. S2). In contrast, injured muscle from old isochronic parabionts regenerated poorly, typical of aged animals1, with a failure of myotube formation, prominent fibrosis at the site of injury, and evidence of proliferating cells predominantly in the interstitial spaces (Supplementary Fig. S2). Notably, parabiosis with young mice significantly enhanced the regeneration of muscle in old partners (Fig. 1a, b; see also Supplementary Fig. S2). The appearance of nascent myotubes in these old mice was similar to that seen in young mice.
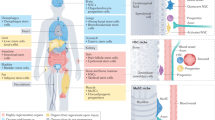
a, Five days after injury, muscles from parabiotic mice were analysed for indices of regeneration and nascent myotube formation by conventional histological analysis (top panels: haematoxylin and eosin staining) and by immunostaining for eMHC (bottom panels: eMHC (red); Hoechst dye (blue) labels all nuclei). Representative fields are shown. b, Quantification of the effectiveness of the regenerative responses from experiments represented in a (see Methods). Data are from three or more pairs for each parabiotic condition (asterisk, P < 0.005). c, After 5 weeks of parabiosis, bulk muscle fibres were isolated and cultured ex vivo for 1 day. Satellite cells were prepared and analysed by flow cytometry for Delta and CD34 expression to determine the percentage of activated satellite cells (that is, those CD34+ cells with high Delta expression6) (n = 4–6 for each condition; asterisk, P < 0.005). Error bars indicate standard deviation.
Importantly, the enhanced regeneration of aged muscle was due almost exclusively to the activation of resident, aged progenitor cells, not to the engraftment of circulating progenitor cells from the young partner. Less than 0.1% of regenerated myotubes in aged muscle were GFP-positive (Supplementary Fig. S4a–c), consistent with comparable studies testing for the contribution of circulating cells to muscle regeneration18,19,20. The GFP transgene has been shown not only to be expressed robustly in mature myofibres of the transgenic strain, but cells isolated from this strain express GFP after incorporation into a GFP-negative recipient18,19,21. Therefore, this is clearly a sensitive and accurate measure of engraftment. Nearly all GFP-positive cells present at the site of the injury were located in the interstitial spaces (Supplementary Fig. S4b), and these cells were probably infiltrating leukocytes, as has been described previously18,21. These results indicate that the impaired regenerative potential of aged satellite cells can be improved by a modification of the systemic environment, by means of an increase of positive factors in young mouse serum, a decrease or dilution of inhibitory factors present in old mouse serum, or both.
The loss of muscle regeneration with age is due at least in part to an age-related impairment in the upregulation of the Notch ligand Delta after muscle injury1. Therefore, we tested whether heterochronic parabiosis restored Delta upregulation in aged satellite cells and thus enhanced their activation and proliferation. Using myofibre explantation to assess satellite cell activation6,22, we analysed satellite cells for the expression of Delta. In young isochronic and heterochronic parabionts there was a marked upregulation of Delta in satellite cells, whereas Delta induction was lacking in the old, isochronic parabionts (Fig. 1c), typical of the response of aged muscle1. Notably, satellite cells from the aged partners of heterochronic parabionts showed a marked upregulation of Delta, comparable to that found in their young partners (Fig. 1c) and in young mice not subjected to parabiotic pairings1. There was a slight inhibition of Delta upregulation in satellite cells from young mice in heterochronic parabioses compared with young isochronic parabionts (Fig. 1c). Thus, heterochronic parabiosis not only enhances the proliferative response of the resident aged progenitor cells, it also restores the key molecular signalling in these cells that is necessary for muscle regeneration1.
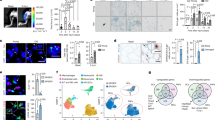
To determine whether the rejuvenating effects of heterochronic parabiosis could be replicated in an in vitro system, satellite cells, cultured either alone or in association with myofibre explants6, were prepared from young and old mice and were cultured in the presence of young or old mouse serum, thus recapitulating the humoral aspects of heterochronic parabioses. Compared with young satellite cells cultured in either young or old serum, there was much less upregulation of Delta in old satellite cells cultured with old mouse serum (Fig. 2a, b); however, young mouse serum restored the upregulation of Delta (Fig. 2a, b) and the activation of Notch (Figs 2c, d) in aged satellite cells. There was an inhibitory effect of the old mouse serum on young satellite cells in terms of the upregulation of Delta (Fig. 2b). Serum from young mice also significantly enhanced the proliferation of myofibre-associated satellite cells in the old cultures compared with serum from old mice (Supplementary Fig. S3). There was reduced proliferation of both young and old satellite cells cultured in young mouse serum when Notch signalling was inhibited (Supplementary Fig. S3). Therefore, enhanced activation and proliferation of aged myogenic progenitor cells by serum from young mice is Notch dependent. Together, these in vivo and in vitro data demonstrate that components in young serum alone are capable of reversing the molecular and cellular aspects of age-related decline in muscle stem cell activation. In addition, it also seems that factors in old serum negatively affect the processes required for satellite cell activation and muscle repair.
a, Myofibre-associated satellite cells were isolated from young or old mice, cultured overnight in media containing either young or old serum, and then analysed by flow cytometry for the expression of Delta and CD34, as described1. The data clearly discriminate between Delta-positive (above the horizontal line) and Delta-negative cells. Satellite cells are CD34-positive (to the right of the vertical line) upon isolation, but CD34 expression declines in the population with time in culture, as described1, After 24 h ex vivo, some cells have already become CD34-negative, an effect accentuated in old serum. b, Quantification of satellite cell activation from experiments represented in a. n = 4; asterisk, P < 0.005. c, Fibre-associated cells from young or old mice were plated in media containing young or old serum for 1 day before fixation. Cells were immunostained for active Notch-1 (green) and M-cadherin (a satellite cell marker26; red). Hoechst dye (blue) labels all nuclei. d, Cells from experiments such as in c were quantified to determine the number of satellite cells (M-cadherin-positive cells) in which activated Notch was detected (n ≥ 3; asterisk, P < 0.005). Error bars indicate standard deviation.
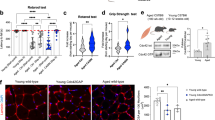
Encouraged by these findings, we then examined liver from aged mice subjected to heterochronic parabiosis to test for evidence of a more general capability to rejuvenate aged, resident progenitor cells. In liver, there are multiple types of progenitor cells that participate in regeneration and homeostasis, depending on the physiological or pathological condition23. Here, we studied proliferating hepatocytes involved in normal tissue turnover, because there is a well documented decline in hepatocyte proliferation with age4,7,24. Heterochronic and isochronic parabionts were examined for hepatocyte proliferation by two independent criteria: the incorporation of BrdU or expression of the proliferation marker Ki67 in albumin-positive cells. In young isochronic parabionts (Fig. 3a), the levels of basal hepatocyte proliferation were two- to threefold greater than in non-parabiosed controls (see Supplementary Fig. S5a), consistent with previous reports of effects of parabiosis on hepatocytes15,16. Also, clusters of BrdU-positive proliferating cells that were not hepatocytes were observed in aged livers (Supplementary Fig. S5b). Proliferation of albumin-positive cells in old isochronic parabionts was less than that observed in young isochronic parabionts (Fig. 3a), consistent with previous reports4,7 and our observation (Supplementary Fig. S5a) that there is an age-related decline in the basal rate of hepatocyte proliferation in non-parabiosed animals. However, parabiosis to a young partner significantly increased hepatocyte proliferation in aged mice (Fig. 3a). As in muscle, a reproducible reduction of progenitor cell proliferation was detected in livers of young mice after parabiotic pairing with old mice (Fig. 3a). Also as in muscle, the enhancement of hepatocyte proliferation in aged mice was due to resident cells and not the engraftment of circulating cells from the young partner. Consistent with previous observations18, less than 0.1% of hepatocytes expressed GFP in the non-transgenic, parabiotic partners.
a, After 5 weeks of parabiotic pairing, mice were given BrdU injections 5, 3 and 1 day before they were killed. Liver sections were analysed for hepatocyte proliferation based on co-staining with albumin and either BrdU or Ki67 (arrows point to nuclei of double-labelled cells). Hoechst dye (blue) labels all nuclei. Quantification of hepatocyte proliferation (see Methods) is shown to the right of each panel (asterisk, P < 0.05; double asterisk, P < 0.005; n = 3–5). b, Extracts from liver sections of parabionts were immunoprecipitated with an anti-cEBP-α antibody and the levels of Brm and cEBP-α were assessed by western blot analysis. Similar amounts of cEBP-α were detected after immunoprecipitation and similar levels of total Brm were present in all liver extracts (not shown), confirming that the formation of the complex, not the levels of the individual components, was affected by age and modified by heterochronic parabiosis. Similar results were obtained in four independent experiments. Error bars indicate standard deviation.
The age-related decline in hepatocyte proliferation is due to the formation of an age-specific complex of cell cycle regulators associated with cEBP-α that inhibits E2F-driven gene expression7. One of the proteins detected in this complex in old, but not young, liver is the chromatin remodelling factor Brm. Levels of the cEBP-α–Brm complex increase in the livers of old rodents, leading to a decline of hepatocyte proliferation7. We tested whether the enhancement of aged hepatocyte proliferation correlated with reduced levels of cEBP-α–Brm complex formation in the aged mice subjected to heterochronic parabiosis. The cEBP-α–Brm protein complex was detected in liver extracts from old isochronic parabionts but not from young isochronic parabionts (Fig. 3b), similar to previous reports in non-parabiosed rodents7. Notably, the formation of the cEBP-α–Brm complex was diminished in liver extracts from old heterochronic parabionts (Fig. 3b). Thus, the molecular determinant had reverted to the ‘youthful’ phenotype, consistent with the enhanced proliferative activity of hepatocytes in these mice. The complex was present at elevated levels in young heterochronic parabionts compared with young controls, also consistent with the modest inhibition of hepatocyte proliferation in young heterochronic parabionts. These data show that the young systemic environment restores a younger profile of molecular signalling to the aged progenitor cells in the liver and also enhances their proliferation.
Our experiments suggest that there are systemic factors that can modulate the molecular signalling pathways critical to the activation of tissue-specific progenitor cells, and that the systemic environment of a young animal is one that promotes successful regeneration, whereas that of an older animal either fails to promote or actively inhibits successful tissue regeneration. It will be of great interest to identify the factors that have such a critical influence on tissue-specific progenitor cells. Our studies also demonstrate that the decline of tissue regenerative potential with age can be reversed through the modulation of systemic factors, suggesting that tissue-specific stem and progenitor cells retain much of their intrinsic proliferative potential even when old, but that age-related changes in the systemic environment and niche in which progenitor cells reside preclude full activation of these cells for productive tissue regeneration.
Methods
Animal strains and parabiosis
Young C57Bl/Ka-Ly5.2 and β-actin–eGFP transgenic mice were bred and maintained by the Weissman Laboratory at the Stanford University Research Animal Facility. GFP-transgenic mice were generated as described25, and were backcrossed for at least ten generations to C57BL/Ka-Thy1.1 mice. Old C57Bl/6 mice were obtained from the National Institutes of Aging or aged on site; young C57Bl/6 mice were obtained from Jackson Laboratories. Animals were housed and handled in accordance with the guidelines of Veterinary Medical Unit of the VA Palo Alto Health Care System and the Administrative Panel on Laboratory Animal Care of Stanford University. Parabiosis was performed as published18; the viability of the pairs was similar to published data14.
Reagents
Antibodies to Delta and cEBP-α were purchased from Santa Cruz Biotechnology, to Ki67 from DakoCytomation, to CD34 and Brm from Beckton-Dickinson, to albumin and laminin from Sigma, and to active Notch-1 from Novus Biologicals/ABCAM. The antibody to eMHC was provided by G. Pavlath. The anti-BrdU staining kit was from Beckton-Dickinson and the BrdU-labelling reagent was from Zymed and was used at a dose of 50 µg g-1. Soluble Delta-4 and Jagged-1 were from R&D systems. Fluorophore-conjugated secondary antibodies for flow cytometry and immunofluorescence were obtained from Caltag and used as previously described6.
Muscle injury
In order to analyse satellite cell activation and muscle regeneration in vivo, a small focal injury was made by an application of dry ice for 5 s directly to the tibialis anterior muscle1. This generates a reproducible ‘wedge’ injury in the muscle with a discrete border between uninjured and injured muscle, and this border remains clear and distinct during the regeneration of the injured tissue.
Immunofluorescence and histological analysis
Muscles were dissected, embedded, cryo-sectioned and immunostained as previously described6. Liver was similarly prepared for cryo-sectioning and immunohistological analysis. Livers that showed signs of gross pathological abnormalities were excluded before analysis.
The effectiveness of the muscle regeneration was assessed by counting the number of eMHC-positive fibres at the injury site, and normalizing this to the total number of nuclei in the field of view in 7–12 randomly selected sections. This is presented as the ‘regeneration index’ and reflects both the positive (myotube formation) and negative (persistent inflammatory cell infiltration and fibroblast proliferation) aspects of regeneration that are present in young and aged mice.
To quantify hepatocyte proliferation, the total number of albumin-positive cells that were also either BrdU-positive or Ki67-positive were counted and expressed as a percentage of total albumin-positive cells in random fields. Ki67-positive or BrdU-positive cells that were negative for albumin were not included (see Supplementary Fig. S5b).
Satellite cell activation and isolation
In order to induce activation of satellite cells reproducibly and robustly, hindlimb muscles (tibialis anterior, gastrocnemius, biceps femoris and quadriceps) were dissected, digested into bulk fibres, and cultured overnight ex vivo1. Satellite cells were purified from bulk fibres as described1. The resulting preparation contained mononucleated cells that were >95% CD34+/M-cadherin+ satellite cells, which could be distinguished from remaining debris using flow cytometry by the characteristic forward scatter and side scatter properties of cells1.
Satellite cell culture in vitro
For in vitro studies of satellite cell activation in the presence of mouse serum, bulk fibres were cultured at a ratio of one volume of loosely settled fibres to no less than 20 volumes of OptiMem (plus penicillin/streptomycin (Gibco/Invitrogen)), supplemented with 5% serum from mice of the indicated age1. No additional matrix or growth factors were added to the fibres.
For detection of activated Notch, satellite cells were digested from muscle fibres as described1 and plated onto ECM-coated (ECM gel, Sigma; diluted 1:1,000 in ice-cold PBS, applied at 1 µg cm-2) chamber slides (Permanox or glass 8-well, Nalge-Nunc), and cultured at low density in OptiMEM with 5% mouse serum as above until fixation in 4% paraformaldehyde/PBS for 5 min for analysis.
For satellite cell proliferation, fibres were cultured as above with one-half of the media replaced every day. After addition of BrdU to the medium for 2 h, the percentages of BrdU-positive cells were determined as the total number of BrdU-positive nuclei per the total number of nuclei in fibres with associated BrdU-positive cells.
Flow cytometry
Cells were analysed either live or after fixation with 4% paraformaldehyde. Cells were stained with primary antibodies or with isotype-matched control antibodies (1 µg in 100 µl), followed by incubation with fluorochrome-labelled secondary antibodies (1:200–1:500 dilutions). Incubations were performed for 30 min on ice (live cells) or for 1 h at room temperature (fixed cells). Cells were analysed by flow cytometry (FACScan, Beckton Dickinson) using compensation for green and red fluorescence and doublet discrimination parameters.
Immunoprecipitation and western blotting
Immunoprecipitation of cEBP-α was from collected liver sections as described7. Western analysis was performed as previously described1.
Statistical analysis
Data are presented as means and standard deviations. Comparisons between groups were done using Student's t-test assuming two-tailed distribution and unequal variances.
References
Conboy, I. M., Conboy, M. J., Smythe, G. M. & Rando, T. A. Notch-mediated restoration of regenerative potential to aged muscle. Science 302, 1575–1577 (2003)
Morrison, S. J., Wandycz, A. M., Akashi, K., Globerson, A. & Weissman, I. L. The aging of hematopoietic stem cells. Nature Med. 2, 1011–1016 (1996)
Fuller, J. Hematopoietic stem cells and aging. Sci. Aging Knowledge Environ., e11 (2002)
Sigal, S. H., Brill, S., Fiorino, A. S. & Reid, L. M. The liver as a stem cell and lineage system. Am. J. Physiol. 263, G139–G148 (1992)
Kuhn, H. G., Dickinson-Anson, H. & Gage, F. H. Neurogenesis in the dentate gyrus of the adult rat: age-related decrease of neuronal progenitor proliferation. J. Neurosci. 16, 2027–2033 (1996)
Conboy, I. M. & Rando, T. A. The regulation of Notch signaling controls satellite cell activation and cell fate determination in postnatal myogenesis. Dev. Cell 3, 397–409 (2002)
Iakova, P., Awad, S. S. & Timchenko, N. A. Aging reduces proliferative capacities of liver by switching pathways of C/EBPα growth arrest. Cell 113, 495–506 (2003)
Golden, T. R., Hinerfeld, D. A. & Melov, S. Oxidative stress and aging: beyond correlation. Aging Cell 1, 117–123 (2002)
Hekimi, S. & Guarente, L. Genetics and the specificity of the aging process. Science 299, 1351–1354 (2003)
Tatar, M., Bartke, A. & Antebi, A. The endocrine regulation of aging by insulin-like signals. Science 299, 1346–1351 (2003)
Hasty, P., Campisi, J., Hoeijmakers, J., van Steeg, H. & Vijg, J. Aging and genome maintenance: lessons from the mouse? Science 299, 1355–1359 (2003)
Carlson, B. M. & Faulkner, J. A. Muscle transplantation between young and old rats: age of host determines recovery. Am. J. Physiol. 256, C1262–C1266 (1989)
Carlson, B. M., Dedkov, E. I., Borisov, A. B. & Faulkner, J. A. Skeletal muscle regeneration in very old rats. J. Gerontol. A 56, B224–B233 (2001)
McCay, C. M., Pope, F., Lunsford, W., Sperling, G. & Sambhavaphol, P. Parabiosis between old and young rats. Gerontologia 1, 7–17 (1957)
Finerty, J. Parabiosis in physiological studies. Physiol. Rev. 32, 277–302 (1952)
Tauchi, H. & Hasegawa, K. Change of the hepatic cells in parabiosis between old and young rats. Mech. Ageing Dev. 6, 333–339 (1977)
Sidorenko, A. V., Gubrii, I. B., Andrianova, L. F., Macsijuk, T. V. & Butenko, G. M. Functional rearrangement of lymphohemopoietic system in heterochronically parabiosed mice. Mech. Ageing Dev. 36, 41–56 (1986)
Wagers, A. J., Sherwood, R. I., Christensen, J. L. & Weissman, I. L. Little evidence for developmental plasticity of adult hematopoietic stem cells. Science 297, 2256–2259 (2002)
Sherwood, R. I. et al. Isolation of adult mouse myogenic progenitors: Functional heterogeneity of cells within and engrafting skeletal muscle. Cell 119, 543–554 (2004)
Partridge, T. A. Cells that participate in regeneration of skeletal muscle. Gene Ther. 9, 752–753 (2002)
Sherwood, R. I., Christensen, J. L., Weissman, I. L. & Wagers, A. J. Determinants of skeletal muscle contributions from circulating cells, bone marrow cells, and hematopoietic stem cells. Stem Cells 22, 1292–1304 (2004)
Rosenblatt, J. D., Lunt, A. I., Parry, D. J. & Partridge, T. A. Culturing satellite cells from living single muscle fiber explants. In Vitro Cell. Dev. Biol. Anim. 31, 773–779 (1995)
Sell, S. Heterogeneity and plasticity of hepatocyte lineage cells. Hepatology 33, 738–750 (2001)
Timchenko, N. A. et al. Regenerating livers of old rats contain high levels of C/EBPα that correlate with altered expression of cell cycle associated proteins. Nucleic Acids Res. 26, 3293–3299 (1998)
Wright, D. E. et al. Cyclophosphamide/granulocyte colony-stimulating factor causes selective mobilization of bone marrow hematopoietic stem cells into the blood after M phase of the cell cycle. Blood 97, 2278–2285 (2001)
Beauchamp, J. R. et al. Expression of CD34 and Myf5 defines the majority of quiescent adult skeletal muscle satellite cells. J. Cell Biol. 151, 1221–1234 (2000)
Acknowledgements
We thank L. Chan and K. Robinson for technical help, and T. Wyss-Coray, T. Palmer, B. Omary and M. Buckwalter for discussions. The work was supported by grants from the Burroughs Wellcome Fund Career Award to A.J.W., and from the NIH, the American Federation for Aging Research (Paul Beeson Faculty Scholar in Aging) and the Department of Veterans Affairs (Merit Review) to T.A.R.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
I.L.W. was a member of the SAB and owns significant stock in Amgen, Inc., and is a Director and owns founders stock in Stem Cells, Inc. and Cellerant, Inc.
Supplementary information
Supplementary Figure 1
Blood chimerism between parabiosed partners. (PPT 25 kb)
Supplementary Figure 2
Heterochronic parabiosis restores fiber regeneration in old mice. (PPT 100 kb)
Supplementary Figure 3
The enhancement of aged satellite cell proliferation by young serum is dependent on Notch signaling. (PPT 18 kb)
Supplementary Figure 4
Muscle regeneration in parabionts is mediated by endogenous, resident muscle stem cells, not by circulating progenitor cells. (PPT 2650 kb)
Supplementary Figure 5
Proliferating cells in livers of non-parabiotic and parabiotic mice. (PPT 1353 kb)
Rights and permissions
About this article
Cite this article
Conboy, I., Conboy, M., Wagers, A. et al. Rejuvenation of aged progenitor cells by exposure to a young systemic environment. Nature 433, 760–764 (2005). https://doi.org/10.1038/nature03260
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/nature03260
This article is cited by
-
Biologically informed deep learning for explainable epigenetic clocks
Scientific Reports (2024)
-
Pituitary stem cells: past, present and future perspectives
Nature Reviews Endocrinology (2024)
-
Epigenome-wide analysis of aging effects on liver regeneration
BMC Biology (2023)
-
Ageing and rejuvenation of tissue stem cells and their niches
Nature Reviews Molecular Cell Biology (2023)
-
Multi-omic rejuvenation and lifespan extension on exposure to youthful circulation
Nature Aging (2023)
Comments
By submitting a comment you agree to abide by our Terms and Community Guidelines. If you find something abusive or that does not comply with our terms or guidelines please flag it as inappropriate.