Abstract
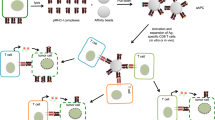
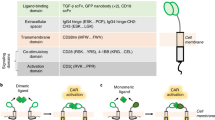
Artificial antigen presentation aims to accelerate the establishment of therapeutic cellular immunity. Artificial antigen-presenting cells (AAPCs) and their cell-free substitutes are designed to stimulate the expansion and acquisition of optimal therapeutic features of T cells before therapeutic infusion, without the need for autologous antigen-presenting cells. Compelling recent advances include fibroblast AAPCs that process antigens, magnetic beads that are antigen specific, novel T-cell costimulatory combinations, the augmentation of therapeutic potency of adoptively transferred T lymphocytes by interleukin-15, and the safe use of dendritic cell-derived exosomes pulsed with tumor antigen. Whereas the safety and potency of the various systems warrant further preclinical and clinical studies, these emerging technologies are poised to have a major impact on adoptive T-cell therapy and the investigation of T cell–mediated immunity.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Bob Crimi

Bob Crimi
Similar content being viewed by others
References
Riddell, S.R., Murata, M., Bryant, S. & Warren, E.H. T-cell therapy of leukemia. Cancer Control 9, 114–122 (2002).
Papadopoulos, E.B. et al. Infusions of donor leukocytes to treat Epstein-Barr virus-associated lymphoproliferative disorders after allogeneic bone marrow transplantation. N. Engl. J. Med. 330, 1185–1191 (1994).
Savoldo, B., Heslop, H.E. & Rooney, C.M. The use of cytotoxic T cells for the prevention and treatment of Epstein-Barr virus induced lymphoma in transplant recipients. Leukemia Lymphoma 39, 455–464 (2000).
Yee, C. et al. Adoptive T cell therapy using antigen-specific CD8+ T cell clones for the treatment of patients with metastatic melanoma: in vivo persistence, migration, and antitumor effect of transferred T cells. Proc. Natl. Acad. Sci. USA 99, 16168–16173 (2002).
Dudley, M.E. et al. Cancer regression and autoimmunity in patients after clonal repopulation with antitumor lymphocytes. Science 298, 850–854 (2002).
Hori, S., Takahashi, T. & Sakaguchi, S. Control of autoimmunity by naturally arising regulatory CD4+ T cells. Adv. Immunol. 81, 331–371 (2003).
Karim, M., Kingsley, C.I., Bushell, A.R., Sawitzki, B.S. & Wood, K.J. Alloantigen-induced CD25+CD4+ regulatory T cells can develop in vivo from CD25−CD4+precursors in a thymus-independent process. J. Immunol. 172, 923–928 (2004).
Janeway, C.A. Jr., Walport, M. & Shlomchik, M.J. Immunobiology, edn. 5 (Garland Publishing, New York, 2001).
Janetzki, S., Song, P., Gupta, V., Lewis, J.J. & Houghton, A.N. Insect cells as HLA-restricted antigen-presenting cells for the IFN-gamma elispot assay. J. Immunol. Methods 234, 1–12 (2000).
Cai, Z. et al. Transfected Drosophila cells as a probe for defining the minimal requirements for stimulating unprimed CD8+ T cells. Proc. Natl. Acad. Sci. USA 93, 14736–14741 (1996).
Jackson, M.R., Song, E.S., Yang, Y. & Peterson, P.A. Empty and peptide-containing conformers of class I major histocompatibility complex molecules expressed in Drosophila melanogaster cells. Proc. Natl. Acad. Sci. USA 89, 12117–12121 (1992).
Sun, S. et al. Dual function of Drosophila cells as APCs for naive CD8+ T cells: implications for tumor immunotherapy. Immunity 4, 555–564 (1996).
Schoenberger, S.P. et al. Efficient direct priming of tumor-specific cytotoxic T lymphocyte in vivo by an engineered APC. Cancer Res. 58, 3094–3100 (1998).
Latouche, J.B. & Sadelain, M. Induction of human cytotoxic T lymphocytes by artificial antigen-presenting cells. Nat. Biotechnol. 18, 405–409 (2000).
Papanicolaou, G.A. et al. Rapid expansion of cytomegalovirus-specific cytotoxic T lymphocytes by artificial antigen-presenting cells expressing a single HLA allele. Blood 102, 2498–2505 (2003).
Maus, M.V. et al. Ex vivo expansion of polyclonal and antigen-specific cytotoxic T lymphocytes by artificial APCs expressing ligands for the T-cell receptor, CD28 and 4-1BB. Nat. Biotechnol. 20, 143–148 (2002).
Thomas, A.K., Maus, M.V., Shalaby, W.S., June, C.H. & Riley, J.L. A cell-based artificial antigen-presenting cell coated with anti-CD3 and CD28 antibodies enables rapid expansion and long-term growth of CD4 T lymphocytes. Clin. Immunol. 105, 259–272 (2002).
Levine, B.L. et al. Effects of CD28 costimulation on long-term proliferation of CD4+ T cells in the absence of exogenous feeder cells. J. Immunol. 159, 5921–5930 (1997).
Levine, B.L. et al. Large-scale production of CD4+ T cells from HIV-1-infected donors after CD3/CD28 costimulation. J. Hematother. 7, 437–448 (1998).
Levine, B.L. et al. Adoptive transfer of costimulated CD4+ T cells induces expansion of peripheral T cells and decreased CCR5 expression in HIV infection. Nat. Med. 8, 47–53 (2002).
Laux, I. et al. Response differences between human CD4(+) and CD8(+) T-cells during CD28 costimulation: implications for immune cell-based therapies and studies related to the expansion of double-positive T-cells during aging. Clin. Immunol. 96, 187–197 (2000).
Oelke, M. et al. Ex vivo induction and expansion of antigen-specific cytotoxic T cells by HLA-Ig-coated artificial antigen-presenting cells. Nat. Med. 9, 619–624 (2003).
Maus, M.V., Riley, J.L., Kwok, W.W., Nepom, G.T. & June, C.H. HLA tetramer-based artificial antigen-presenting cells for stimulation of CD4+ T cells. Clin. Immunol. 106, 16–22 (2003).
Prakken, B. et al. Artificial antigen-presenting cells as a tool to exploit the immune 'synapse' Nat. Med. 6, 1406–1410 (2000).
Zitvogel, L. et al. Eradication of established murine tumors using a novel cell-free vaccine: dendritic cell-derived exosomes. Nat. Med. 4, 594–600 (1998).
Wolfers, J. et al. Tumor-derived exosomes are a source of shared tumor rejection antigens for CTL cross-priming. Nat. Med. 7, 297–303 (2001).
Thery, C., Zitvogel, L. & Amigorena, S. Exosomes: composition, biogenesis and function. Nat. Rev. Immunol. 2, 569–579 (2002).
Andre, F. et al. Malignant effusions and immunogenic tumour-derived exosomes. Lancet 360, 295–305 (2002).
Chaput, N. et al. Exosomes as potent cell-free peptide-based vaccine. II. Exosomes in CpG adjuvants efficiently prime naive Tc1 lymphocytes leading to tumor rejection. J. Immunol. 172, 2137–2146 (2004).
Chaput, N., Schartz, N.E., Andre, F. & Zitvogel, L. Exosomes for immunotherapy of cancer. Adv. Exp. Med. Biol. 532, 215–221 (2003).
Raposo, G. et al. B lymphocytes secrete antigen-presenting vesicles. J. Exp. Med. 183, 1161–1172 (1996).
Hsu, D.H. et al. Exosomes as a tumor vaccine: enhancing potency through direct loading of antigenic peptides. J. Immunother. 26, 440–450 (2003).
Banchereau, J. & Steinman, R.M. Dendritic cells and the control of immunity. Nature 392, 245–252 (1998).
Pardoll, D.M. Spinning molecular immunology into successful immunotherapy. Nat. Rev. Immunol. 2, 227–238 (2002).
Stoll, S., Delon, J., Brotz, T.M. & Germain, R.N. Dynamic imaging of T cell-dendritic cell interactions in lymph nodes. Science 296, 1873–1876 (2002).
Jung, S. et al. In vivo depletion of CD11c(+) dendritic cells abrogates priming of CD8(+) T cells by exogenous cell-associated antigens. Immunity 17, 211–220 (2002).
Riddell, S.R. & Greenberg, P.D. T-cell therapy of cytomegalovirus and human immunodeficiency virus infection. J. Antimicrob. Chemother. 45 Suppl T3, 35–43 (2000).
Bender, A., Sapp, M., Schuler, G., Steinman, R.M. & Bhardwaj, N. Improved methods for the generation of dendritic cells from nonproliferating progenitors in human blood. J. Immunol. Methods 196, 121–135 (1996).
Reddy, A., Sapp, M., Feldman, M., Subklewe, M. & Bhardwaj, N. A monocyte conditioned medium is more effective than defined cytokines in mediating the terminal maturation of human dendritic cells. Blood 90, 3640–3646 (1997).
Mitchell, M.S. et al. Phase I trial of adoptive immunotherapy with cytolytic T lymphocytes immunized against a tyrosinase epitope. J. Clin. Oncol. 20, 1075–1086 (2002).
Krause, A. et al. Antigen-dependent CD28 signaling selectively enhances survival and proliferation in genetically modified activated human primary T lymphocytes. J. Exp. Med. 188, 619–626 (1998).
Gong, M.C. et al. Cancer patient T cells genetically targeted to prostate-specific membrane antigen specifically lyse prostate cancer cells and release cytokines in response to prostate-specific membrane antigen. Neoplasia 1, 123–127 (1999).
Johnson, D.R. Differential expression of human major histocompatibility class I loci: HLA-A, -B, and -C. Hum. Immunol. 61, 389–396 (2000).
Delbrück, A. in Structural Chemistry and Molecular Biology. (eds. Davidson, N. & Rich, A.) 198–215 (Freeman, San Francisco, 1968).
Kim, J., Mosior, M., Chung, L.A., Wu, H. & McLaughlin, S. Binding of peptides with basic residues to membranes containing acidic phospholipids. Biophys. J. 60, 135–148 (1991).
Kim, J., Shishido, T., Jiang, X., Aderem, A. & McLaughlin, S. Phosphorylation, high ionic strength, and calmodulin reverse the binding of MARCKS to phospholipid vesicles. J. Biol. Chem. 269, 28214–28219 (1994).
McLaughlin, S., Wang, J., Gambhir, A. & Murray, D. PIP(2) and proteins: interactions, organization, and information flow. Annu. Rev. Biophys. Biomol. Struct. 31, 151–175 (2002).
Mosior, M. & McLaughlin, S. Electrostatics and reduction of dimensionality produce apparent cooperativity when basic peptides bind to acidic lipids in membranes. Biochim. Biophys. Acta. 1105, 185–187 (1992).
Lee, S.J., Hori, Y., Groves, J.T., Dustin, M.L. & Chakraborty, A.K. The synapse assembly model. Trends Immunol. 23, 500–502 (2002).
Lee, S.J., Hori, Y., Groves, J.T., Dustin, M.L. & Chakraborty, A.K. Correlation of a dynamic model for immunological synapse formation with effector functions: two pathways to synapse formation. Trends Immunol. 23, 492–499 (2002).
Hwang, I., Shen, X. & Sprent, J. Direct stimulation of naive T cells by membrane vesicles from antigen-presenting cells: distinct roles for CD54 and B7 molecules. Proc. Natl. Acad. Sci. USA 100, 6670–6675 (2003).
Gett, A.V., Sallusto, F., Lanzavecchia, A. & Geginat, J. T cell fitness determined by signal strength. Nat. Immunol. 4, 355–360 (2003).
Sadelain, M., Riviere, I. & Brentjens, R. Targeting tumours with genetically enhanced T lymphocytes. Nat. Rev. Cancer 3, 35–45 (2003).
Lohr, J., Knoechel, B., Jiang, S., Sharpe, A.H. & Abbas, A.K. The inhibitory function of B7 costimulators in T cell responses to foreign and self-antigens. Nat. Immunol. 4, 664–669 (2003).
Topp, M.S. et al. Restoration of CD28 expression in CD28+-CD8+ memory effector T cells reconstitutes antigen-induced IL-2 production. J. Exp. Med. 198, 947–955 (2003).
Wen, T., Bukczynski, J. & Watts, T.H. 4-1BB ligand-mediated costimulation of human T cells induces CD4 and CD8 T cell expansion, cytokine production, and the development of cytolytic effector function. J. Immunol. 168, 4897–4906 (2002).
Melero, I. et al. Amplification of tumor immunity by gene transfer of the co-stimulatory 4-1BB ligand: synergy with the CD28 co-stimulatory pathway. Eur. J. Immunol. 28, 1116–1121 (1998).
Rogers, P.R., Song, J., Gramaglia, I., Killeen, N. & Croft, M. OX40 promotes Bcl-xL and Bcl-2 expression and is essential for long-term survival of CD4 T cells. Immunity 15, 445–455 (2001).
Kikuchi, T., Moore, M.A. & Crystal, R.G. Dendritic cells modified to express CD40 ligand elicit therapeutic immunity against preexisting murine tumors. Blood 96, 91–99 (2000).
Kikuchi, T., Worgall, S., Singh, R., Moore, M.A. & Crystal, R.G. Dendritic cells genetically modified to express CD40 ligand and pulsed with antigen can initiate antigen-specific humoral immunity independent of CD4+ T cells. Nat. Med. 6, 1154–1159 (2000).
Overwijk, W.W. et al. Tumor regression and autoimmunity after reversal of a functionally tolerant state of self-reactive CD8+ T cells. J. Exp. Med. 198, 569–580 (2003).
Rottman, J.B. et al. The costimulatory molecule ICOS plays an important role in the immunopathogenesis of EAE. Nat. Immunol. 2, 605–611 (2001).
Salama, A.D. et al. Interaction between ICOS-B7RP1 and B7-CD28 costimulatory pathways in alloimmune responses in vivo. Am. J. Transplant. 3, 390–395 (2003).
Sporici, R.A. & Perrin, P.J. Costimulation of memory T-cells by ICOS: a potential therapeutic target for autoimmunity? Clin. Immunol. 100, 263–269 (2001).
Villegas, E.N. et al. A role for inducible costimulator protein in the CD28- independent mechanism of resistance to Toxoplasma gondii. J. Immunol. 169, 937–943 (2002).
Yoshinaga, S.K. et al. T-cell co-stimulation through B7RP-1 and ICOS. Nature 402, 827–832 (1999).
Rosenberg, S.A. et al. Use of tumor-infiltrating lymphocytes and interleukin-2 in the immunotherapy of patients with metastatic melanoma. A preliminary report. N. Engl. J. Med. 319, 1676–1680 (1988).
Bhardwaj, N., Seder, R.A., Reddy, A. & Feldman, M.V. IL-12 in conjunction with dendritic cells enhances antiviral CD8+ CTL responses in vitro. J. Clin. Invest. 98, 715–722 (1996).
Gajewski, T.F. Integrating IL-12 into therapeutic cancer vaccines. Cancer Chemother. Biol. Response Modif. 20, 343–349 (2002).
Portielje, J.E., Gratama, J.W., van Ojik, H.H., Stoter, G. & Kruit, W.H. IL-12: a promising adjuvant for cancer vaccination. Cancer Immunol. Immunother. 52, 133–144 (2003).
Puccetti, P., Belladonna, M.L. & Grohmann, U. Effects of IL-12 and IL-23 on antigen-presenting cells at the interface between innate and adaptive immunity. Crit. Rev. Immunol. 22, 373–390 (2002).
Schluns, K.S. & Lefrancois, L. Cytokine control of memory T-cell development and survival. Nat. Rev. Immunol. 3, 269–279 (2003).
Fehniger, T.A., Cooper, M.A. & Caligiuri, M.A. Interleukin-2 and interleukin-15: immunotherapy for cancer. Cytokine Growth Factor Rev. 13, 169–183 (2002).
Waldmann, T. The contrasting roles of IL-2 and IL-15 in the life and death of lymphocytes: implications for the immunotherapy of rheumatological diseases. Arthritis Res. 4 Suppl 3, S161–S167 (2002).
Waldmann, T.A., Dubois, S. & Tagaya, Y. Contrasting roles of IL–2 and IL-15 in the life and death of lymphocytes: implications for immunotherapy. Immunity 14, 105–110 (2001).
Alpdogan, O. et al. IL-7 enhances peripheral T cell reconstitution after allogeneic hematopoietic stem cell transplantation. J. Clin. Invest. 112, 1095–1107 (2003).
Kaech, S.M. et al. Selective expression of the interleukin 7 receptor identifies effector CD8 T cells that give rise to long-lived memory cells. Nat. Immunol. 4, 1191–1198 (2003).
Nugeyre, M.T. et al. IL-7 stimulates T cell renewal without increasing viral replication in simian immunodeficiency virus-infected macaques. J. Immunol. 171, 4447–4453 (2003).
Strengell, M., Sareneva, T., Foster, D., Julkunen, I. & Matikainen, S. IL-21 up-regulates the expression of genes associated with innate immunity and Th1 response. J. Immunol. 169, 3600–3605 (2002).
Wong, P. & Pamer, E.G. Cutting edge: antigen-independent CD8 T cell proliferation. J. Immunol. 166, 5864–5868 (2001).
Brentjens, R.J. et al. Eradication of systemic B-cell tumors by genetically targeted human T lymphocytes co-stimulated by CD80 and interleukin-15. Nat. Med. 9, 279–286 (2003).
Shand, A. & Forbes, A. Potential therapeutic role for cytokine or adhesion molecule manipulation in Crohn's disease: in the shadow of infliximab? Int. J. Colorectal. Dis. 18, 1–11 (2003).
Parrish-Novak, J., Foster, D.C., Holly, R.D. & Clegg, C.H. Interleukin-21 and the IL-21 receptor: novel effectors of NK and T cell responses. J. Leukoc. Biol. 72, 856–863 (2002).
Wurster, A.L. et al. Interleukin 21 is a T helper (Th) cell 2 cytokine that specifically inhibits the differentiation of naive Th cells into interferon gamma-producing Th1 cells. J. Exp. Med. 196, 969–977 (2002).
Andre, F. et al. Tumor-derived exosomes: a new source of tumor rejection antigens. Vaccine 20 Suppl 4, A28–A31 (2002).
Chaput, N. et al. Exosomes and anti-tumour immunotherapy. Bull. Cancer 90, 695–698 (2003).
Wang, H.Y. et al. Tumor-specific human CD4+ regulatory T cells and their ligands: implications for immunotherapy. Immunity 20, 107–118 (2004).
Laport, G.G. et al. Adoptive transfer of costimulated T cells induces lymphocytosis in patients with relapsed/refractory non-Hodgkin lymphoma following CD34+-selected hematopoietic cell transplantation. Blood 102, 2004–2013 (2003).
Rapoport, A.P. et al. Molecular remission of CML after autotransplantation followed by adoptive transfer of costimulated autologous T cells. Bone Marrow Transplant. 33, 53–60 (2004).
Andre, F. et al. Exosomes as potent cell-free peptide-based vaccine. I. Dendritic cell-derived exosomes transfer functional MHC class I/peptide complexes to dendritic cells. J. Immunol. 172, 2126–2136 (2004).
Hurwitz, A.A., Yanover, P., Markowitz, M., Allison, J.P. & Kwon, E.D. Prostate cancer: advances in immunotherapy. BioDrugs 17, 131–138 (2003).
Hurwitz, A.A., Yu, T.F., Leach, D.R. & Allison, J.P. CTLA-4 blockade synergizes with tumor-derived granulocyte-macrophage colony-stimulating factor for treatment of an experimental mammary carcinoma. Proc. Natl. Acad. Sci. USA 95, 10067–10071 (1998).
Phan, G.Q. et al. Cancer regression and autoimmunity induced by cytotoxic T lymphocyte-associated antigen 4 blockade in patients with metastatic melanoma. Proc. Natl. Acad. Sci. USA 100, 8372–8377 (2003).
van Elsas, A., Hurwitz, A.A. & Allison, J.P. Combination immunotherapy of B16 melanoma using anti-cytotoxic T lymphocyte-associated antigen 4 (CTLA-4) and granulocyte/macrophage colony-stimulating factor (GM-CSF)-producing vaccines induces rejection of subcutaneous and metastatic tumors accompanied by autoimmune depigmentation. J. Exp. Med. 190 355–366 (1999).
Seder, R.A. & Ahmed, R. Similarities and differences in CD4+ and CD8+ effector and memory T cell generation. Nat. Immunol. 4, 835–842 (2003).
Ahn, H.J. et al. A mechanism underlying synergy between IL-12 and IFN-gamma-inducing factor in enhanced production of IFN-gamma. J. Immunol. 159, 2125–2131 (1997).
Robinson, D. et al. IGIF does not drive Th1 development but synergizes with IL-12 for interferon-gamma production and activates IRAK and NFkappaB. Immunity 7, 571–581 (1997).
Tatsumi, T. et al. Intratumoral delivery of dendritic cells engineered to secrete both interleukin (IL)-12 and IL-18 effectively treats local and distant disease in association with broadly reactive Tc1-type immunity. Cancer Res. 63, 6378–6386 (2003).
Watford, W.T., Moriguchi, M., Morinobu, A. & O'Shea, J.J. The biology of IL-12: coordinating innate and adaptive immune responses. Cytokine Growth Factor Rev. 14, 361–368 (2003).
Bromley, S.K. et al. The immunological synapse. Annu. Rev. Immunol. 19, 375–396 (2001).
Acknowledgements
Our work is supported by National Institutes of Health grants CA-59350, CA-08748 and CA-09512 to J.V.K., I.R. and M.S.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Kim, J., Latouche, JB., Rivière, I. et al. The ABCs of artificial antigen presentation. Nat Biotechnol 22, 403–410 (2004). https://doi.org/10.1038/nbt955
Published:
Issue Date:
DOI: https://doi.org/10.1038/nbt955
This article is cited by
-
Precise surface functionalization of PLGA particles for human T cell modulation
Nature Protocols (2023)
-
Optimizing interleukin-2 concentration, seeding density and bead-to-cell ratio of T-cell expansion for adoptive immunotherapy
BMC Immunology (2021)
-
Engineered red blood cells as an off-the-shelf allogeneic anti-tumor therapeutic
Nature Communications (2021)
-
Biomaterials for Engineering Immune Responses
Journal of the Indian Institute of Science (2018)
-
Hurdles Associated with the Translational Use of Genetically Modified Cells
Current Stem Cell Reports (2018)