Abstract
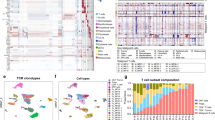
Cutaneous T cell lymphoma (CTCL) is a non-Hodgkin lymphoma of skin-homing T lymphocytes. We performed exome and whole-genome DNA sequencing and RNA sequencing on purified CTCL and matched normal cells. The results implicate mutations in 17 genes in CTCL pathogenesis, including genes involved in T cell activation and apoptosis, NF-κB signaling, chromatin remodeling and DNA damage response. CTCL is distinctive in that somatic copy number variants (SCNVs) comprise 92% of all driver mutations (mean of 11.8 pathogenic SCNVs versus 1.0 somatic single-nucleotide variant per CTCL). These findings have implications for new therapeutics.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Girardi, M., Heald, P.W. & Wilson, L.D. The pathogenesis of mycosis fungoides. N. Engl. J. Med. 350, 1978–1988 (2004).
Guenova, E. et al. TH2 cytokines from malignant cells suppress TH1 responses and enforce a global TH2 bias in leukemic cutaneous T-cell lymphoma. Clin. Cancer Res. 19, 3755–3763 (2013).
Kim, E.J. et al. Immunopathogenesis and therapy of cutaneous T cell lymphoma. J. Clin. Invest. 115, 798–812 (2005).
Wong, H.K., Mishra, A., Hake, T. & Porcu, P. Evolving insights in the pathogenesis and therapy of cutaneous T-cell lymphoma (mycosis fungoides and Sezary syndrome). Br. J. Haematol. 155, 150–166 (2011).
Lin, W.M. et al. Characterization of the DNA copy-number genome in the blood of cutaneous T-cell lymphoma patients. J. Invest. Dermatol. 132, 188–197 (2012).
Vermeer, M.H. et al. Novel and highly recurrent chromosomal alterations in Sezary syndrome. Cancer Res. 68, 2689–2698 (2008).
Caprini, E. et al. Identification of key regions and genes important in the pathogenesis of Sezary syndrome by combining genomic and expression microarrays. Cancer Res. 69, 8438–8446 (2009).
Laharanne, E. et al. Genome-wide analysis of cutaneous T-cell lymphomas identifies three clinically relevant classes. J. Invest. Dermatol. 130, 1707–1718 (2010).
Neri, A., Fracchiolla, N.S., Migliazza, A., Trecca, D. & Lombardi, L. The involvement of the candidate proto-oncogene NFKB2/lyt-10 in lymphoid malignancies. Leuk. Lymphoma 23, 43–48 (1996).
Braun, F.C. et al. Tumor suppressor TNFAIP3 (A20) is frequently deleted in Sezary syndrome. Leukemia 25, 1494–1501 (2011).
Vaqué, J.P. et al. PLCG1 mutations in cutaneous T-cell lymphomas. Blood 123, 2034–2043 (2014).
Wong, H.K. Novel biomarkers, dysregulated epigenetics, and therapy in cutaneous T-cell lymphoma. Discov. Med. 16, 71–78 (2013).
Lawrence, M.S. et al. Mutational heterogeneity in cancer and the search for new cancer-associated genes. Nature 499, 214–218 (2013).
Mermel, C.H. et al. GISTIC2.0 facilitates sensitive and confident localization of the targets of focal somatic copy-number alteration in human cancers. Genome Biol. 12, R41 (2011).
Cancer Genome Atlas Research Network. Comprehensive molecular characterization of gastric adenocarcinoma. Nature 513, 202–209 (2014).
Schizophrenia Working Group of the Psychiatric Genomics Consortium. Biological insights from 108 schizophrenia-associated genetic loci. Nature 511, 421–427 (2014).
Kandoth, C. et al. Mutational landscape and significance across 12 major cancer types. Nature 502, 333–339 (2013).
Raychaudhuri, S. et al. Identifying relationships among genomic disease regions: predicting genes at pathogenic SNP associations and rare deletions. PLoS Genet. 5, e1000534 (2009).
Beroukhim, R. et al. The landscape of somatic copy-number alteration across human cancers. Nature 463, 899–905 (2010).
Sedwick, C.E. & Altman, A. Perspectives on PKCτ in T cell activation. Mol. Immunol. 41, 675–686 (2004).
Man, K. et al. The transcription factor IRF4 is essential for TCR affinity-mediated metabolic programming and clonal expansion of T cells. Nat. Immunol. 14, 1155–1165 (2013).
Palomero, T. et al. Recurrent mutations in epigenetic regulators, RHOA and FYN kinase in peripheral T cell lymphomas. Nat. Genet. 46, 166–170 (2014).
Sakata-Yanagimoto, M. et al. Somatic RHOA mutation in angioimmunoblastic T cell lymphoma. Nat. Genet. 46, 171–175 (2014).
Yoo, H.Y. et al. A recurrent inactivating mutation in RHOA GTPase in angioimmunoblastic T cell lymphoma. Nat. Genet. 46, 371–375 (2014).
Heidorn, S.J. et al. Kinase-dead BRAF and oncogenic RAS cooperate to drive tumor progression through CRAF. Cell 140, 209–221 (2010).
Rajala, H.L. et al. Discovery of somatic STAT5b mutations in large granular lymphocytic leukemia. Blood 121, 4541–4550 (2013).
Evans, E.J. et al. Crystal structure of a soluble CD28-Fab complex. Nat. Immunol. 6, 271–279 (2005).
Odorizzi, P.M. & Wherry, E.J. Inhibitory receptors on lymphocytes: insights from infections. J. Immunol. 188, 2957–2965 (2012).
Linsley, P.S. et al. Human B7-1 (CD80) and B7-2 (CD86) bind with similar avidities but distinct kinetics to CD28 and CTLA-4 receptors. Immunity 1, 793–801 (1994).
Slavik, J.M., Hutchcroft, J.E. & Bierer, B.E. CD80 and CD86 are not equivalent in their ability to induce the tyrosine phosphorylation of CD28. J. Biol. Chem. 274, 3116–3124 (1999).
Wang, K. et al. Whole-genome sequencing and comprehensive molecular profiling identify new driver mutations in gastric cancer. Nat. Genet. 46, 573–582 (2014).
Kakiuchi, M. et al. Recurrent gain-of-function mutations of RHOA in diffuse-type gastric carcinoma. Nat. Genet. 46, 583–587 (2014).
Mayer, T., Meyer, M., Janning, A., Schiedel, A.C. & Barnekow, A. A mutant form of the rho protein can restore stress fibers and adhesion plaques in v-src transformed fibroblasts. Oncogene 18, 2117–2128 (1999).
García-Mata, R. et al. Analysis of activated GAPs and GEFs in cell lysates. Methods Enzymol. 406, 425–437 (2006).
Legarda-Addison, D. & Ting, A.T. Negative regulation of TCR signaling by NF-κB2/p100. J. Immunol. 178, 7767–7778 (2007).
Kopp, K.L. et al. STAT5-mediated expression of oncogenic miR-155 in cutaneous T-cell lymphoma. Cell Cycle 12, 1939–1947 (2013).
Zhang, Q. et al. Cutaneous T cell lymphoma expresses immunosuppressive CD80 (B7-1) cell surface protein in a STAT5-dependent manner. J. Immunol. 192, 2913–2919 (2014).
Haddad, B.R. et al. STAT5A/B gene locus undergoes amplification during human prostate cancer progression. Am. J. Pathol. 182, 2264–2275 (2013).
Kelly, J. et al. A role for Stat5 in CD8+ T cell homeostasis. J. Immunol. 170, 210–217 (2003).
Wu, J.N. & Roberts, C.W. ARID1A mutations in cancer: another epigenetic tumor suppressor? Cancer Discov. 3, 35–43 (2013).
Hill, L., Browne, G. & Tulchinsky, E. ZEB/miR-200 feedback loop: at the crossroads of signal transduction in cancer. Int. J. Cancer 132, 745–754 (2013).
Hidaka, T. et al. Down-regulation of TCF8 is involved in the leukemogenesis of adult T-cell leukemia/lymphoma. Blood 112, 383–393 (2008).
Williams, T.M. et al. Identification of a zinc finger protein that inhibits IL-2 gene expression. Science 254, 1791–1794 (1991).
Grégoire, J.M. & Romeo, P.H. T-cell expression of the human GATA-3 gene is regulated by a non-lineage-specific silencer. J. Biol. Chem. 274, 6567–6578 (1999).
Rausch, T. et al. Genome sequencing of pediatric medulloblastoma links catastrophic DNA rearrangements with TP53 mutations. Cell 148, 59–71 (2012).
Zack, T.I. et al. Pan-cancer patterns of somatic copy number alteration. Nat. Genet. 45, 1134–1140 (2013).
Papaemmanuil, E. et al. RAG-mediated recombination is the predominant driver of oncogenic rearrangement in ETV6-RUNX1 acute lymphoblastic leukemia. Nat. Genet. 46, 116–125 (2014).
Gostissa, M. et al. Long-range oncogenic activation of Igh–c-myc translocations by the Igh 3′ regulatory region. Nature 462, 803–807 (2009).
Couronné, L., Bastard, C. & Bernard, O.A. TET2 and DNMT3A mutations in human T-cell lymphoma. N. Engl. J. Med. 366, 95–96 (2012).
Luo, B. et al. Highly parallel identification of essential genes in cancer cells. Proc. Natl. Acad. Sci. USA 105, 20380–20385 (2008).
Di Fiore, R., D'Anneo, A., Tesoriere, G. & Vento, R. RB1 in cancer: different mechanisms of RB1 inactivation and alterations of pRb pathway in tumorigenesis. J. Cell. Physiol. 228, 1676–1687 (2013).
Yao, S., Zhu, Y. & Chen, L. Advances in targeting cell surface signalling molecules for immune modulation. Nat. Rev. Drug Discov. 12, 130–146 (2013).
Morin, R.D. et al. Frequent mutation of histone-modifying genes in non-Hodgkin lymphoma. Nature 476, 298–303 (2011).
Meyer, S.C. & Levine, R.L. Molecular pathways: molecular basis for sensitivity and resistance to JAK kinase inhibitors. Clin. Cancer Res. 20, 2051–2059 (2014).
Vainchenker, W. & Constantinescu, S.N. JAK/STAT signaling in hematological malignancies. Oncogene 32, 2601–2613 (2013).
Pomerantz, J.L., Denny, E.M. & Baltimore, D. CARD11 mediates factor-specific activation of NF-κB by the T cell receptor complex. EMBO J. 21, 5184–5194 (2002).
Dang, C.V. MYC on the path to cancer. Cell 149, 22–35 (2012).
Larsen, C.P. et al. Rational development of LEA29Y (belatacept), a high-affinity variant of CTLA4-Ig with potent immunosuppressive properties. Am. J. Transplant. 5, 443–453 (2005).
Zinzani, P.L. et al. Phase II trial of proteasome inhibitor bortezomib in patients with relapsed or refractory cutaneous T-cell lymphoma. J. Clin. Oncol. 25, 4293–4297 (2007).
Genovese, M.C. et al. Abatacept for rheumatoid arthritis refractory to tumor necrosis factor α inhibition. N. Engl. J. Med. 353, 1114–1123 (2005).
Rangwala, S., Zhang, C. & Duvic, M. HDAC inhibitors for the treatment of cutaneous T-cell lymphomas. Future Med. Chem. 4, 471–486 (2012).
Dees, N.D. et al. MuSiC: identifying mutational significance in cancer genomes. Genome Res. 22, 1589–1598 (2012).
Getz, G. et al. Comment on “The consensus coding sequences of human breast and colorectal cancers.” Science 317, 1500 (2007).
Zhao, S. et al. Landscape of somatic single-nucleotide and copy-number mutations in uterine serous carcinoma. Proc. Natl. Acad. Sci. USA 110, 2916–2921 (2013).
Li, J. et al. CONTRA: copy number analysis for targeted resequencing. Bioinformatics 28, 1307–1313 (2012).
Kozarewa, I. & Turner, D.J. Amplification-free library preparation for paired-end Illumina sequencing. Methods Mol. Biol. 733, 257–266 (2011).
Li, H. & Durbin, R. Fast and accurate long-read alignment with Burrows-Wheeler transform. Bioinformatics 26, 589–595 (2010).
Mayrhofer, M., Dilorenzo, S. & Isaksson, A. Patchwork: allele-specific copy number analysis of whole-genome sequenced tumor tissue. Genome Biol. 14, R24 (2013).
Chen, K. et al. BreakDancer: an algorithm for high-resolution mapping of genomic structural variation. Nat. Methods 6, 677–681 (2009).
Goh, G. et al. Recurrent activating mutation in PRKACA in cortisol-producing adrenal tumors. Nat. Genet. 46, 613–617 (2014).
Trapnell, C. et al. Differential gene and transcript expression analysis of RNA-seq experiments with TopHat and Cufflinks. Nat. Protoc. 7, 562–578 (2012).
Grant, C.E., Bailey, T.L. & Noble, W.S. FIMO: scanning for occurrences of a given motif. Bioinformatics 27, 1017–1018 (2011).
Merelli, I. et al. RSSsite: a reference database and prediction tool for the identification of cryptic Recombination Signal Sequences in human and murine genomes. Nucleic Acids Res. 38, W262–W267 (2010).
Emsley, P. & Cowtan, K. Coot: model-building tools for molecular graphics. Acta Crystallogr. D Biol. Crystallogr. 60, 2126–2132 (2004).
Choi, J. et al. Identification of PLX4032-resistance mechanisms and implications for novel RAF inhibitors. Pigment Cell Melanoma Res. 27, 253–262 (2014).
Acknowledgements
We gratefully acknowledge the participation of the patients who made this research possible. We are grateful to I. Tikhonova and the staff of the Yale Center for Genome Analysis for their expert production of DNA and RNA sequence. Work was supported by the Dermatology Foundation and the Yale Specialized Program of Research Excellence (SPORE) in Skin Cancer Career Development Award (J.C.);. the Yale SPORE in Skin Cancer, P50 CA121974 (T.J.B.); the Agency for Science, Technology and Research, Singapore (G.G.); and US National Institutes of Health (NIH) grant RO1 CA102703 (M.G.). D.G.S. and R.P.L. are investigators of the Howard Hughes Medical Institute.
Author information
Authors and Affiliations
Contributions
J.C., M.G. and R.P.L. designed the experiments, analyzed data and wrote the manuscript. J.D.O. and R.D.B. directed nucleic acid sequencing and data management. J.C., G.G. and R.P.L. analyzed sequencing results. J.C., T. Walradt, B.S.H., T. Wang, K. Chen, K.J.L., J.M.L., L.B., K. Carlson, F.M.F., A.S., E.C.V., R.L.E. and M.G. collected and annotated clinical samples. C.G.B. and T.J.B. performed structural modeling. J.C., B.S.H., K. Chen and T. Walradt performed functional experiments. J.C., J.T. and T. Walradt assessed TCGA data. J.C. and L.D. performed flow cytometry. J.C., Y.M. and D.G.S. performed analysis of RAG sequences at deletion breakpoints.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–17 and Supplementary Tables 1–17. (PDF 5359 kb)
Rights and permissions
About this article
Cite this article
Choi, J., Goh, G., Walradt, T. et al. Genomic landscape of cutaneous T cell lymphoma. Nat Genet 47, 1011–1019 (2015). https://doi.org/10.1038/ng.3356
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ng.3356
This article is cited by
-
Transcriptomic and proteomic analysis of tumor suppressive effects of GZ17-6.02 against mycosis fungoides
Scientific Reports (2024)
-
SWI/SNF complexes in hematological malignancies: biological implications and therapeutic opportunities
Molecular Cancer (2023)
-
A genetic profiling guideline to support diagnosis and clinical management of lymphomas
Clinical and Translational Oncology (2023)
-
Development of Cutaneous T-Cell Lymphoma Following Biologic Treatment: A Systematic Review
American Journal of Clinical Dermatology (2023)
-
Two cases of mycosis fungoides with large cell transformation with KMT2A rearrangements
Journal of Hematopathology (2023)