Abstract
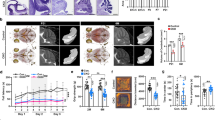
Loss-of-function mutations in the gene (CSTB) encoding human cystatin B, a widely expressed cysteine protease inhibitor, are responsible for a severe neurological disorder known as Unverricht-Lundborg disease (EPM1). The primary cellular events and mechanisms underlying the disease are unknown. We found that mice lacking cystatin B develop myoclonic seizures and ataxia, similar to symptoms seen in the human disease. The principal cytopathology appears to be a loss of cerebellar granule cells, which frequently display condensed nuclei, fragmented DNA and other cellular changes characteristic of apoptosis. This mouse model of EPM1 provides evidence that cystatin B, a non-caspase cysteine protease inhibitor, has a role in preventing cerebellar apoptosis.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout







Similar content being viewed by others
References
Berkovic, S.F., Andermann, F., Carpenter, S. & Wolfe, L.S. Progressive myoclonus epilepsies: specific causes and diagnosis. New Eng. J. Med. 315, 296–305 (1985).
Schoffner, J.M., Lott, M.T. & Lezza, A.M.S. Myoclonus epilepsy and red-ragged fiber disease (MERRF) is associated with a mitochondrial DNA tRNAlys mutation. Cell 61, 931–937 (1990).
Vesa, J. et al. Mutations in the palmitoyl protein thioesterase gene causing infantile neuronal ceroid lipofuscinosis. Nature 376, 584–587 (1995).
International Batten Disease Consortium. Isolation of a novel gene underlying Batten disease, CLN3. Cell 82, 949–957 (1995).
Bonten, E., van der Spoel, A., Fornerod, M., Grosveld, G. & d'Azzo, A. Characterization of human lysosomal neuraminidase defines the molecular basis of the metabolic storage disorder sialidosis. Genes Dev. 10, 3156– 3169 (1996).
Pennacchio, L.A. et al. Mutations in the gene encoding cystatin B in progressive myoclonus epilepsy (EPM1). Science 271, 1731–1734 (1996).
Lalioti, M.D. et al. Identification of mutations in cystatin B, the gene responsible for the Unverricht-Lundborg type of Progressive Myoclonus Epilepsy (EPM1). Am. J. Hum. Genet. 60, 342– 351 (1997).
Sleat, D.E. et al. Association of mutations in a lysosomal protein with classical late-infantile neuronal ceroid lipofuscinosis. Science 277, 1802–1805 (1997).
Savukoski, M. et al. CLN5, a novel gene encoding a putative transmembrane protein mutated in Finnish variant late infantile neuronal ceroid lipofuscinosis. Nature Genet. 19, 286– 288 (1998).
Harriman, D.G.F. & Millar, J.H.D. Progressive familial myoclonic epilepsy in 3 families: its clinical features and pathological basis. Brain 78, 325–349 (1955).
Zeman, W. & Alpert, M. On the nature of the "stored" lipid substances in juvenile amaurotic idiocy (Batten-Spielmeyer-Vogt). Ann. Histochim. 8, 255–257 (1963).
Carpenter, S., Karpati, G., Andermann, F., Jacob, J.C. & Andermann, E. Lafora's disease: peroxisomal storage in skeletal muscle. Neurol. 24, 531–538 (1974).
O'Brien, J.S. The cherry red spot-myoclonus syndrome: a newly recognized inherited lysosomal storage disease due to acid neuraminidase deficiency. Clin. Genet. 14, 55–60 ( 1978).
Wallace, D.C. et al. Familial mitochondrial encephalomyopathy (MERRF): genetic, pathophysiological, and biochemical characterization of a mitochondrial DNA disease. Cell 55, 601–610 (1988).
Bindoff, L.A. et al. Multiple defects of the mitochondrial respiratory chain in a mitochondrial encephalopathy (MERRF): a clinical, biochemical and molecular study. J. Neurol. Sci. 102, 17– 24 (1991).
Koskiniemi, M., Donner, M., Majuri, H., Haltia, M. & Norio, R. Progressive myoclonus epilepsy: a clinical and histopathological study. Acta Neurol. Scand. 50, 307– 332 (1974).
Koskiniemi, M., Toivakka, E. & Donner, M. Progressive myoclonus epilepsy: electroencephalographical findings. Acta Neurol. Scand. 50, 333– 359 (1974).
Norio, R. & Koskiniemi, M. Progressive myoclonus epilepsy: genetic and nosological aspects with special reference to 107 Finnish patients. Clin. Genet. 15, 382–398 (1979).
Koskiniemi, M. in Paediatric Epilepsy (eds Sillanpää, M., Johannessen, S.I., Blennow, G. & Dam, D.) 37–144 (Wrightson, Hampshire, 1990).
Haltia, M., Kristensson, K. & Sourander, P. Neuropathological studies in three Scandanavian cases of progressive myoclonus epilepsy. Acta Neurol. Scand. 45, 63–77 (1969).
Eldridge, R., Iivanainen, M., Stern, R., Koerber, T. & Wilder, B.J. "Baltic" myoclonus epilepsy: hereditary disorder of childhood made worse by phenytoin. Lancet 2, 838–842 (1983).
Barrett, A.J. et al. Nomenclature and classification of the proteins homologous with the cysteine-proteinase inhibitor chicken cystatin. Biochem. J. 236, 312 (1986).
Turk, V. & Bode, W. The cystatins: protein inhibitors of cysteine proteinases. FEBS Lett. 285, 213–219 (1991).
Rawlings, N.D. & Barrett, A.J. Evolution of proteins of the cystatin superfamily. J. Mol. Evol. 30, 60–71 (1990).
Ritonja, A., Machleidt, W. & Barrett, A.J. Amino acid sequence of the intracellular cysteine proteinase inhibitor cystatin B from human liver. Biochem. Biophys. Res. Comm. 131, 1187–1192 (1985).
Barrett, A.J. et al. Inhibitors of cysteine proteases. in Proteinease Inhibitors (eds Barrett, A.J. & Salvesen, G.) 515–569 (Elsevier Publishing, New York, 1986).
Barrett, A.J. & Kirschke, H. Cathepsin B, cathepsin H, and cathepsin L. in Methods in Enzymology Vol. 80 (ed. Lorand, L.) 535–561 (Academy Press, New York, 1981).
Bohley, P. & Seglen, P.O. Proteases and proteolysis in the lysosome. Experientia 48, 151– 157 (1992).
Marks, N., Berg, M.J. & Benuck, M. Preferential action of rat brain cathepsin B as a peptidyl dipeptidase converting pro-pioid oligopeptides. Arch. Biochem. Biophys. 249, 489–499 (1986).
Pennacchio, L.A. & Myers, R.M. Isolation and characterization of the mouse cystatin B gene. Genome Res. 6, 1103–1109 (1996).
Gavrieli, Y., Sherman, Y. & Ben-Sasson, S.A. Identification of programmed cell death in situ via specific labeling of nuclear DNA fragmentation. J. Cell Biol. 119, 493–501 (1992).
Kyllerman. M., Sommerfelt, K., Hedstrom, A., Wennergren, G. & Holmgren, D. Clinical and neurophysiological development of Unverricht-Lundborg disease in four Swedish siblings. Epilepsia 32, 900–909 (1991).
Sax, D.S., Hirano, A. & Shofer, R.J. Staggerer, a neurological murine mutant. An electron microscopic study of the cerebellar cortex in the adult. Neurol. 18, 1093–1100 (1968).
Rakic, P. & Sidman, R.L. Organization of cerebellar cortex secondary to deficit of granule cells in weaver mutant mice. J. Comp. Neurol. 152, 133–161 (1973).
Caddy, K.W.T. & Biscoe, C.H. Structural and quantitative studies on the normal C3H and lurcher mutant mouse. Philosoph. Trans. R. Soc. London 287, 167–201 (1979).
Kuida, K. et al. Decreased apoptosis in the brain and premature lethality in CPP32-deficient mice. Nature 384, 368–372 (1996).
Du, Y. et al. Activation of a caspase 3-related cysteine protease is required for glutamate-mediated apoptosis of cultured cerebellar granule neurons. Proc. Natl Acad. Sci. USA 94, 11657– 11662 (1997).
Williams, M.S. & Henkart, P.A. Apoptotic cell death induced by intracellular proteolysis. J. Immunol. 153, 4247–4255 (1994).
Salvesen, G.S. & Dixit, V.M. Caspases: Intracelluar signaling by proteolysis. Cell 91, 443– 446 (1997).
Zhou, Q. & Salvesen, G.S. Activation of pro-caspase-7 by serine proteases includes a non-canonical specificity. Biochem. J. 324, 361–364 (1997).
Tsung, P.K. & Holly, F.J. Protease activity in human tears. Curr. Eye Res. 1, 351– 355 (1981).
Barka, T., Asbell., P.A., van der Noen, H. & Prasad, A. Cystatins in human tear fluid. Curr. Eye Res. 10, 25–34 (1991).
Cejkova, J., Lojda, Z., Salonen, E.M. & Vaheri, A. Histochemical study of alkali-burned rabbit anterior eye segment in which severe lesions were prevented by aprotinin treatment. Histochemistry 92, 441–448 (1989).
Salonen, E.M., Tervo, T., Torma, E., Tarkkanen, A. & Vaheri, A. Plasmin in tear fluid of patients with corneal ulcers: basis for new therapy. Acta Ophthalmol. 65, 3–12 (1987).
Tervo, T. et al. Contact lens wear is associated with the appearance of plasmin in the tear fluid-preliminary results. Graefes Arch. Clin. Exp. Ophthalmol. 227, 42–44 (1989).
Luetteke, N.C. et al. TGFα deficiency results in hair follicle and eye abnormalities in targeted and waved-1 mice. Cell 73, 263–278 (1993).
Lane, S.C., Jolly, R.D., Schmechel, D.E., Alroy, J. & Boustany, R.-M. Apoptosis as a mechanism of neurodegeneration in Batten's disease. J. Neurochem. 67, 677–683 (1996).
Bradley, A. Production and analysis of chimaeric mice. in Teratocarcinomas and Embryonic Stem Cells: A Practical Approach (ed. Robertson, E.J.) 113–151 (IRL Press, Oxford, 1987).
Mangiarini, L. et al. Exon 1 of the HD gene with an expanded CAG repeat is sufficient to cause a progressive neurological phenotype in transgenic mice. Cell 87, 493–506 (1996).
Laemmli, U.K. Cleavage of structural proteins during the assembly of the head of bacteriophage T4. Nature 227, 680–685 (1970).
Acknowledgements
We thank D. Cox, D. Vollrath, C. Prange Pennacchio, C. Iannicola, C. Karlovich, G. Barsh and members of the Myers laboratory for discussions and support, F. Davies for use of the rotorod, A. Nagy for the R1 ES cells donation, N. Ghouri for EM sample preparation, S. Krajewski for assistance with EM interpretations and C. Davis for his help with ECoG recordings. This work is supported by grant NIH NS29709 and HD24064 (J.L.N.).
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Pennacchio, L., Bouley, D., Higgins, K. et al. Progressive ataxia, myoclonic epilepsy and cerebellar apoptosis in cystatin B-deficient mice. Nat Genet 20, 251–258 (1998). https://doi.org/10.1038/3059
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/3059
This article is cited by
-
Pathological Deficit of Cystatin B Impairs Synaptic Plasticity in EPM1 Human Cerebral Organoids
Molecular Neurobiology (2023)
-
Cerebellar Involvement in Patients with Mild to Moderate Myoclonus Due to EPM1: Structural and Functional MRI Findings in Comparison with Healthy Controls and Ataxic Patients
Brain Topography (2017)
-
Biomarkers of Epileptogenesis: The Focus on Glia and Cognitive Dysfunctions
Neurochemical Research (2017)
-
Brain inflammation is accompanied by peripheral inflammation in Cstb −/− mice, a model for progressive myoclonus epilepsy
Journal of Neuroinflammation (2016)
-
The network sustaining action myoclonus: a MEG-EMG study in patients with EPM1
BMC Neurology (2016)