Abstract
Regions of the normal arterial intima predisposed to atherosclerosis are sites of ongoing monocyte trafficking and also contain resident myeloid cells with features of dendritic cells. However, the pathophysiological roles of these cells are poorly understood. Here we found that intimal myeloid cells underwent reverse transendothelial migration (RTM) into the arterial circulation after systemic stimulation of pattern-recognition receptors (PRRs). This process was dependent on expression of the chemokine receptor CCR7 and its ligand CCL19 by intimal myeloid cells. In mice infected with the intracellular pathogen Chlamydia muridarum, blood monocytes disseminated infection to the intima. Subsequent CCL19-CCR7–dependent RTM was critical for the clearance of intimal C. muridarum. This process was inhibited by hypercholesterolemia. Thus, RTM protects the normal arterial intima, and compromised RTM during atherogenesis might contribute to the intracellular retention of pathogens in atherosclerotic lesions.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout








Similar content being viewed by others
Change history
20 March 2017
In the version of this article initially published, the label along the horizontal axis of the graph in Figure 1a ('Dose (mg)') is incorrect. The correct label is 'Dose (μg)'. The error has been corrected in the HTML and PDF versions of the article.
References
Cybulsky, M.I., Cheong, C. & Robbins, C.S. Macrophages and dendritic cells: partners in atherogenesis. Circ. Res. 118, 637–652 (2016).
Millonig, G. et al. Network of vascular-associated dendritic cells in intima of healthy young individuals. Arterioscler. Thromb. Vasc. Biol. 21, 503–508 (2001).
Jongstra-Bilen, J. et al. Low-grade chronic inflammation in regions of the normal mouse arterial intima predisposed to atherosclerosis. J. Exp. Med. 203, 2073–2083 (2006).
Choi, J.H. et al. Identification of antigen-presenting dendritic cells in mouse aorta and cardiac valves. J. Exp. Med. 206, 497–505 (2009).
Paulson, K.E. et al. Resident intimal dendritic cells accumulate lipid and contribute to the initiation of atherosclerosis. Circ. Res. 106, 383–390 (2010).
Kawai, T. & Akira, S. The roles of TLRs, RLRs and NLRs in pathogen recognition. Int. Immunol. 21, 317–337 (2009).
Soloff, A.C. & Barratt-Boyes, S.M. Enemy at the gates: dendritic cells and immunity to mucosal pathogens. Cell Res. 20, 872–885 (2010).
Martel, C. et al. Lymphatic vasculature mediates macrophage reverse cholesterol transport in mice. J. Clin. Invest. 123, 1571–1579 (2013).
Huttenlocher, A. & Poznansky, M.C. Reverse leukocyte migration can be attractive or repulsive. Trends Cell Biol. 18, 298–306 (2008).
Xu, X. & Ge, Q. Maturation and migration of murine CD4 single positive thymocytes and thymic emigrants. Comput. Struct. Biotechnol. J. 9, e201403003 (2014).
Serbina, N.V. & Pamer, E.G. Monocyte emigration from bone marrow during bacterial infection requires signals mediated by chemokine receptor CCR2. Nat. Immunol. 7, 311–317 (2006).
Fujimura, N. et al. CCR2 inhibition sequesters multiple subsets of leukocytes in the bone marrow. Sci. Rep. 5, 11664 (2015).
Condeelis, J. & Pollard, J.W. Macrophages: obligate partners for tumor cell migration, invasion, and metastasis. Cell 124, 263–266 (2006).
Woodfin, A. et al. The junctional adhesion molecule JAM-C regulates polarized transendothelial migration of neutrophils in vivo. Nat. Immunol. 12, 761–769 (2011).
Campbell, L.A. & Kuo, C.C. Chlamydia pneumoniae--an infectious risk factor for atherosclerosis? Nat. Rev. Microbiol. 2, 23–32 (2004).
Grayston, J.T. Infections caused by Chlamydia pneumoniae strain TWAR. Clin. Infect. Dis. 15, 757–761 (1992).
Grayston, J.T. & Campbell, L.A. The role of Chlamydia pneumoniae in atherosclerosis. Clin. Infect. Dis. 28, 993–994 (1999).
Filardo, S., Di Pietro, M., Farcomeni, A., Schiavoni, G. & Sessa, R. Chlamydia pneumoniae-mediated inflammation in atherosclerosis: a meta-analysis. Mediators Inflamm. 2015, 378658 (2015).
Zimmer, S., Grebe, A. & Latz, E. Danger signaling in atherosclerosis. Circ. Res. 116, 323–340 (2015).
Moazed, T.C., Kuo, C.C., Grayston, J.T. & Campbell, L.A. Evidence of systemic dissemination of Chlamydia pneumoniae via macrophages in the mouse. J. Infect. Dis. 177, 1322–1325 (1998).
Gieffers, J. et al. Chlamydia pneumoniae infection in circulating human monocytes is refractory to antibiotic treatment. Circulation 103, 351–356 (2001).
Evani, S.J. & Ramasubramanian, A.K. Biophysical regulation of Chlamydia pneumoniae-infected monocyte recruitment to atherosclerotic foci. Sci. Rep. 6, 19058 (2016).
Kuo, C.C. et al. Chlamydia pneumoniae (TWAR) in coronary arteries of young adults (15-34 years old). Proc. Natl. Acad. Sci. USA 92, 6911–6914 (1995).
Kuo, C. & Campbell, L.A. Detection of Chlamydia pneumoniae in arterial tissues. J. Infect. Dis. 181 (Suppl. 3), S432–S436 (2000).
Belland, R.J., Ouellette, S.P., Gieffers, J. & Byrne, G.I. Chlamydia pneumoniae and atherosclerosis. Cell. Microbiol. 6, 117–127 (2004).
Zhu, S.N., Chen, M., Jongstra-Bilen, J. & Cybulsky, M.I. GM-CSF regulates intimal cell proliferation in nascent atherosclerotic lesions. J. Exp. Med. 206, 2141–2149 (2009).
Gautier, E.L. et al. Enhanced dendritic cell survival attenuates lipopolysaccharide-induced immunosuppression and increases resistance to lethal endotoxic shock. J. Immunol. 180, 6941–6946 (2008).
Förster, R., Davalos-Misslitz, A.C. & Rot, A. CCR7 and its ligands: balancing immunity and tolerance. Nat. Rev. Immunol. 8, 362–371 (2008).
Nibbs, R.J. & Graham, G.J. Immune regulation by atypical chemokine receptors. Nat. Rev. Immunol. 13, 815–829 (2013).
Gracey, E. et al. Pulmonary Chlamydia muridarum challenge activates lung interstitial macrophages which correlate with IFN-γ production and infection control in mice. Eur. J. Immunol. 45, 3417–3430 (2015).
Rajaram, K. & Nelson, D.E. Chlamydia muridarum infection of macrophages elicits bactericidal nitric oxide production via reactive oxygen species and cathepsin B. Infect. Immun. 83, 3164–3175 (2015).
de Bruijn, M.F. et al. High-level expression of the ER-MP58 antigen on mouse bone marrow hematopoietic progenitor cells marks commitment to the myeloid lineage. Eur. J. Immunol. 26, 2850–2858 (1996).
Choi, J.H. et al. Flt3 signaling-dependent dendritic cells protect against atherosclerosis. Immunity 35, 819–831 (2011).
Link, A. et al. Fibroblastic reticular cells in lymph nodes regulate the homeostasis of naive T cells. Nat. Immunol. 8, 1255–1265 (2007).
Poznansky, M.C. et al. Thymocyte emigration is mediated by active movement away from stroma-derived factors. J. Clin. Invest. 109, 1101–1110 (2002).
Lee, J.Y., Buzney, C.D., Poznansky, M.C. & Sackstein, R. Dynamic alterations in chemokine gradients induce transendothelial shuttling of human T cells under physiologic shear conditions. J. Leukoc. Biol. 86, 1285–1294 (2009).
Worbs, T., Mempel, T.R., Bölter, J., von Andrian, U.H. & Förster, R. CCR7 ligands stimulate the intranodal motility of T lymphocytes in vivo. J. Exp. Med. 204, 489–495 (2007).
Matloubian, M. et al. Lymphocyte egress from thymus and peripheral lymphoid organs is dependent on S1P receptor 1. Nature 427, 355–360 (2004).
Zachariah, M.A. & Cyster, J.G. Neural crest-derived pericytes promote egress of mature thymocytes at the corticomedullary junction. Science 328, 1129–1135 (2010).
Randolph, G.J., Beaulieu, S., Lebecque, S., Steinman, R.M. & Muller, W.A. Differentiation of monocytes into dendritic cells in a model of transendothelial trafficking. Science 282, 480–483 (1998).
Weiss, G. & Schaible, U.E. Macrophage defense mechanisms against intracellular bacteria. Immunol. Rev. 264, 182–203 (2015).
van Gils, J.M. et al. The neuroimmune guidance cue netrin-1 promotes atherosclerosis by inhibiting the emigration of macrophages from plaques. Nat. Immunol. 13, 136–143 (2012).
Angeli, V. et al. Dyslipidemia associated with atherosclerotic disease systemically alters dendritic cell mobilization. Immunity 21, 561–574 (2004).
Park, Y.M., Febbraio, M. & Silverstein, R.L. CD36 modulates migration of mouse and human macrophages in response to oxidized LDL and may contribute to macrophage trapping in the arterial intima. J. Clin. Invest. 119, 136–145 (2009).
Llodrá, J. et al. Emigration of monocyte-derived cells from atherosclerotic lesions characterizes regressive, but not progressive, plaques. Proc. Natl. Acad. Sci. USA 101, 11779–11784 (2004).
Keiper, T. et al. The role of junctional adhesion molecule-C (JAM-C) in oxidized LDL-mediated leukocyte recruitment. FASEB J. 19, 2078–2080 (2005).
Moore, K.J., Sheedy, F.J. & Fisher, E.A. Macrophages in atherosclerosis: a dynamic balance. Nat. Rev. Immunol. 13, 709–721 (2013).
Daley, J.M., Thomay, A.A., Connolly, M.D., Reichner, J.S. & Albina, J.E. Use of Ly6G-specific monoclonal antibody to deplete neutrophils in mice. J. Leukoc. Biol. 83, 64–70 (2008).
Ensan, S. et al. Self-renewing resident arterial macrophages arise from embryonic CX3CR1(+) precursors and circulating monocytes immediately after birth. Nat. Immunol. 17, 159–168 (2016).
Acknowledgements
We thank P. Lesnik (University of Pierre and Marie Curie) for CD11c–hBcl-2 mice; M.C. Nussenzweig (The Rockefeller University) for CD11c-eYFP mice; S. Nunes de Vasconcelos (Toronto General Research Institute) for Rag1−/− mice; J. Gommerman (University of Toronto) for Nos2−/− mouse bones; and N. van Rooijen (Vrije Universiteit) for CLs and PLs. Supported by the Canadian Institutes of Health Research (MOP-84446, MOP-106522 and MOP-89740 to M.I.C.).
Author information
Authors and Affiliations
Contributions
M.R. designed and performed most of the experiments, analyzed the data and contributed to writing the manuscript; E.G. and R.D.I. contributed to experiments with C. muridarum; A.S. and M.A. performed BrdU assays; S.-N.Z. performed ex vivo cannulation and perfusion of the aorta; A. Lau performed TUNEL staining and analysis; H.I. imaged live aortas ex vivo; K.T. performed qPCR analysis of mRNA in the intima; S.J.H. and K.O.C. contributed to function-blocking antibody experiments; S.E., A. Li and R.B. contributed to flow-cytometry sorting studies; H.M.B. contributed to the experimental design and editing; H.X. performed mouse husbandry; S.A.L. provided intellectual input and Ccl19−/− BM; C.S.R. provided intellectual input and contributed to flow-cytometry sorting studies; J.J.-B. contributed to the experimental design, project supervision and writing of the manuscript; and M.I.C. provided overall project supervision, including oversight of experiments and writing of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Integrated supplementary information
Supplementary Figure 1 Quantification of intimal CD11c+ DCs.
Representative composite en face confocal microscopy images of the ascending aortic arch lesser curvature from wild-type mice stained for CD11c (green) and nuclei (blue). Aortas were harvested 24 h after injection of PBS (upper panel) or LPS (lower panel). The abundance of intimal CD11c+ cells is reduced in LPS-injected mice Scale bars, 400 μm.
Supplementary Figure 2 Depletion of circulating monocytes via CLs and apoptosis of CD11c+ DCs in the intima.
(a) Representative flow cytometry plots of blood obtained from wild-type C57BL/6 mice 18 h after i.v. injection of PBS or clodronate liposomes (PL or CL, respectively). Classical monocytes were identified as CD11bhighGr-1+ cells (circled). The CD11bhighGr-1high cells are neutrophils. Absolute numbers of classical monocytes per ml of blood is shown in the graph (mean ± s.e.m.; n = 3; * P < 0.05 (two-tailed Student’s T-test)). (b) Representative en face confocal microscopy images of CD11c-DTR transgenic mouse intima 8 h after injection of DTx (left panel), and wild-type C57BL/6 intima 12 h after LPS injection (right panel). DTx induced extensive apoptosis, which depleted CD11c+ cells, and served as a positive control for TUNEL staining. Only occasional TUNEL+CD11c+ cells were found in the intima of LPS-injected mice (arrowhead). TUNEL+ nuclei (red) CD11c+ cells (green), nuclei (blue). Scale bars, 20 μm.
Supplementary Figure 3 Establishing the efficacy of function-blocking antibodies.
(a) In vitro CD8+ T cell chemotaxis assays. CD8+ T cells were purified from wild-type mouse lymph nodes. A chemotactic gradient was established by adding recombinant murine CCL21 (100 nM) to the bottom wells of a chemotactic chamber. T cells in the top wells were incubated with function-blocking antibodies to CCL21 or CCL19, or isotype-matched IgG. Three independent experiments were performed, each with triplicate wells. Values were normalized to the IgG-treated control group. mean ± s.e.m. ** P < 0.01 (one-way ANOVA with Tukey’s comparison). (b) In vivo adoptive transfer of UBC-GFP lymph node cells into wild-type and plt mice. One hour before the adoptive transfer, mice were injected with function-blocking antibody to CCL19 or CCL21, or isotype-matched IgG. Two hours after adoptive transfer, blood, spleen, and lymph nodes were isolated, cell suspensions were stained for CD3 and CD4 and analyzed by flow cytometry. Values represent GFP+CD4+ T cells (that were gated from CD3+ events in lymph nodes) relative to wild-type mice injected with IgG. Data were normalized to blood and spleen values in order to control for variability in adoptive transfer efficiency. ** P < 0.01, *** P < 0.001 (one-way ANOVA with Tukey’s comparison). Data are from three independent experiments (mean ± s.e.m. (a,b)).
Supplementary Figure 4 Determining the dose of Chlamydia in intranasal and i.v. inoculation models.
(a) Wild-type mice received an intranasal inoculation of C. muridarum. The dose, shown as inclusion forming units (IFU), is indicated. C. muridarum 16s rRNA expression in blood leukocytes was determined by qPCR 2.5 days after inoculation. Comparable infection of blood leukocytes is observed. The lower dose was selected for future studies. (b) Wild-type mice were injected i.v. with the indicated dose of C. muridarum and intimal CD11c+ cells per ascending aorta were quantified at 24 h. The highest dose was selected since it induces the greatest decrease in intimal CD11c+ cells. (c) The maximal Chlamydia infection in the intima was comparable after intranasal and i.v. injections. *** P < 0.001 (two-tailed Student’s T-test (a,c), one-way ANOVA with Tukey’s comparison (b)). Data are from three independent experiments (mean + s.e.m. (a-c)).
Supplementary Figure 5 IL-1β and TNF induce a decrease in intimal CD11c+ cells.
(a, c) In vivo assays: Cytokines were injected i.v. at the indicated doses and intimal CD11c+ cells per ascending aorta were quantified at 24 h. (b, d) Ex vivo assays: Ascending aortas were incubated with different concentrations of cytokines and intimal CD11c+ cells were determined at 12 h. ** P < 0.01, *** P < 0.001 (one-way ANOVA with Tukey’s comparison (a,c), two-tailed Student’s T-test (b,d)). Data are from three independent experiments (mean + s.e.m. (a-d)).
Supplementary Figure 6 Detection of C. muridarum in the plasma and blood leukocytes.
(a) Wild-type C57BL/6 mice were injected with PBS liposomes (PL) or clodronate liposomes (CL) 12 h prior to C. muridarum (107 EB i.v. per mouse). Blood was collected at 24 h after C. muridarum injection, cells were removed by centrifugation, and elementary bodies in the plasma were enumerated by assessing IFU in fibroblast cultures. mean ± s.e.m.; n = 10 for PL and n =5 for CL; *** P < 0.001 (two-tailed Student’s T-test). (b) Representative flow cytometry plots showing the sorting strategy for isolating blood B cells, T cells, neutrophils, classical and non-classical monocytes. Blood samples were obtained from wild-type mice 24 h after i.v. injection of C. muridarum and cells were stained for CD3, B220, Gr-1, and CD11b. The CD3- B220- gate from the upper plot was analyzed for Gr-1 and CD11b in the lower plot. Cells were sorted directly into Trizol reagent for RNA isolation and detection of C. muridarum 16s rRNA. Plots are from one experiment representative of three experiments (n = 6 mice).
Supplementary Figure 7 RTM of intimal CD11c+ cells removes C. muridarum from the arterial intima.
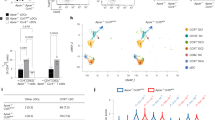
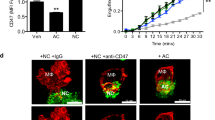
(a) Assessment of C. muridarum EB clearance from the plasma of Ccr7-/- and wild-type (WT) mice after i.v. injection of C. muridarum EBs (107 IFU per mouse). (b,c) Quantification of C. muridarum 16s rRNA by qPCR in blood leukocytes (b) and splenocytes (c) of wild-type and Ccr7-/- mice (key) after i.v. injection of C. muridarum EBs.. Data are expressed relative to values on day 1, set as 1. (d) Quantification of C. muridarum 16s rRNA in BM-derived macrophages after infection in vitro with C. muridarum EBs.. Data are expressed relative to 6 h values in wild-type cells. (e) Quantification of C. muridarum 16s rRNA in the intima (left) and the number of intimal CD11c+ cells (right) in wild-type mice injected i.v. with C. muridarum EBs on day 0 and PTx or B-oligomer on day 3. Aortas were analyzed on days 3 and 4. (f) Assessment of systemic inflammatory response after C. muridarum infection. Wild-type (dashed red) and Ccr7-/- (solid blue) mice were injected i.v. with C. muridarum EBs on day 0 and daily blood samples were collected for serum analysis. Cytokines and chemokines were analyzed using a LUMINEX MULTIPLEX ELISA. IL-3, IL-4, IL-17, and VEGF were not detectable in mouse serum. (g) Quantification of intimal CD11c+ cells in wild-type mice reconstituted with wild-type (WT) or Nos2-/- BM (key). After engraftment, mice were injected i.v. with C. muridarum EBs and intimal CD11c+ cells were quantified at the indicated time points by confocal microscopy.. (h) Quantification of intimal CD11c+ cells in wild-type mice injected i.v. with C. muridarum EBs and either iNOS inhibitor 1400W (10 mg/kg, i.v. 24 h prior to tissue harvesting) or DMSO (carrier control). (i) Quantification of intimal CD3+ cells in wild-type mice at the indicated time points after i.v. injection of C. muridarum EBs. (j ) Quantification of C. muridarum 16s rRNA in the intima of CD11c-DTR mice on day 3 after i.v. injection of C. muridarum EBs and depletion of intimal CD11c+ cells by injecting DTx on day 2. Controls received PBS instead of DT. (k) Quantification of C. muridarum 16s rRNA in the intima of CD11c-hBcl2 mice on days 3 and 4 after i.v. injection of C. muridarum EBs. (l) PCR analysis of mRNA in the aortic intima of wild-type (red) and Ccr7-/- (blue) mice at various times after i.v. injection of C. muridarum EBs. Data are expressed relative to values on day 0, set as 1..* P < 0.05, ** P < 0.01, *** P < 0.001 (one-way ANOVA (i) with Tukey’s post hoc test (c,d,e,g,h), two-way ANOVA (b) with Bonferroni’s post-hoc comparisons (f,l)), or unpaired Student’s t-test (a,j,k)). Data are from three independent experiments (a-l; mean ± s.e.m.).
Supplementary Figure 8 Hypercholesterolemia inhibits RTM induced by TLR4 ligands.
Quantification of intimal CD11c+ cells in Ldlr-/- mice (10 – 12 weeks old) that were fed either SCD or CRD for 1 week (key), then injected i.v. with PBS, LPS (100 μg) or poly(I:C) (150 μg), and aortas were harvested after 24 h. mean ± s.e.m.; n = 5 mice per group; *** P < 0.001 (one-way ANOVA (P < 0.0001) with Tukey’s comparison (within each diet group); two-way ANOVA (P = 0.0001) with Bonferroni’s comparison (between diet groups)). Data are from three independent experiments.
Supplementary information
Supplementary Text and Figures
Supplementary Figures 1–8 and Supplementary Table 1 (PDF 1043 kb)
Rights and permissions
About this article
Cite this article
Roufaiel, M., Gracey, E., Siu, A. et al. CCL19-CCR7–dependent reverse transendothelial migration of myeloid cells clears Chlamydia muridarum from the arterial intima. Nat Immunol 17, 1263–1272 (2016). https://doi.org/10.1038/ni.3564
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ni.3564