Abstract
Mast cells can function as effector and immunoregulatory cells in immunoglobulin E–associated allergic disorders, as well as in certain innate and adaptive immune responses. This review focuses on exciting new developments in the field of mast cell biology published in the past year. We highlight advances in the understanding of FcɛRI-mediated signaling and mast cell–activation events, as well as in the use of genetic models to study mast cell function in vivo. Finally, we discuss newly identified functions for mast cells or individual mast cell products, such as proteases and interleukin 10, in host defense, cardiovascular disease and tumor biology and in settings in which mast cells have anti-inflammatory or immunosuppressive functions.
Similar content being viewed by others
Main
Mast cells are derived from hematopoietic progenitor cells but do not ordinarily circulate in mature form; instead, the differentiation and maturation of mast cells occurs locally, after migration of their precursors to the vascularized tissues or serosal cavities in which the mast cells will ultimately reside1,2,3,4,5,6. Mast cells are key effector cells in immunoglobulin E (IgE)-associated immune responses, including allergic disorders and certain protective immune responses to parasites2,6,7,8. IgE-dependent activation of mast cells leads to the secretion of three classes of mediators. Degranulation of activated cells results in the secretion of preformed mediators (such as vasoactive amines and neutral proteases) that are stored in the cells' cytoplasmic granules. In contrast, proinflammatory lipid mediators are synthesized anew. Finally, growth factors, cytokines and chemokines are secreted. However, mast cells can be activated to perform important effector and immunomodulatory functions by many mechanisms that are independent of IgE, and the type of stimulus can determine the kinetics, amounts and/or spectrum of mediators that are released6,7,9.
Signaling through the receptor FcɛRI
Mast cells can participate in a wide variety of physiological and pathological processes as a result of their activation by any of an array of receptors. However, the best-studied mechanism by which mast cells accomplish immunologically specific function is through antigen- and IgE-dependent aggregation of the high-affinity IgE receptor FcɛRI (refs. 7,9,10,11,12,13,14; Fig. 1). FcɛRI is expressed on mast cells as a heterotetrameric receptor composed of an IgE-binding α-subunit, the membrane-tetraspanning β-subunit and two identical disulfide-linked γ-subunits. The γ-subunits are important for initiating signaling events 'downstream' of this receptor because each γ-subunit contains one immunoreceptor tyrosine-based activation motif (ITAM)7,9,11,13. The stability of FcɛRI on the mast cell surface, which is a chief determinant of FcɛRI expression, can be influenced both by external factors (such as IgE binding2,7) and intracellular molecules such as rabaptin 5 (ref. 15). Antigen- and IgE-induced crosslinking of cell surface FcɛRI triggers activation of the kinase Lyn, which phosphorylates FcɛRI ITAMs and activates the kinase Syk after ITAM binding. Lyn and Syk phosphorylate several adaptor molecules and enzymes to regulate mast cell activation. In addition to activating Lyn, FcɛRI aggregation activates a second Src family kinase, Fyn, that phosphorylates the adaptor Gab2 to activate the phosphatidylinositol-3-OH kinase (PI(3)K) pathway.
Antigen (Ag)-induced crosslinking of FcɛRI induces activation of Lyn, which phosphorylates FcɛRI ITAMs (green) and activates Syk after ITAM binding, and Fyn, which phosphorylates the adaptor Gab2 to activate the PI(3)K pathway. Lyn and Syk phosphorylate many adaptor molecules, such as Lat and NTAL, and enzymes to regulate activation of the GTPase Ras, phospholipase C-γ (PLC-γ) and PI(3)K pathways, as well as other pathways. Grb2 and SOS (son of sevenless homolog) activate the Ras-Erk (extracellular signal–regulated kinase) pathway, which regulates the activation of transcription factors and metabolism of arachidonic acid (through activation of phospholipase A2 (PLA2)). Phospholipase C-γ can be activated through the coordinated function of the adaptor molecules Lat, Gads, SLP-76 and Vav and the tyrosine kinase Btk or independently of Lat through a PI(3)K-Btk–dependent pathway. Activation of phospholipase C-γ regulates the activation of classical protein kinase C (through the generation of diacylglycerol (DAG)) and calcium responses (through the generation of inositol-1,4,5-trisphosphate (IP3)). The binding of inositol-1,4,5-trisphosphate to its receptor (IP3R) triggers Ca2+ release from the endoplasmic reticulum (ER); STIM1 couples depletion of endoplasmic reticulum Ca2+ stores with activation of CRAC channels, which leads to the influx of extracellular Ca2+ and a calcium release–activated current (ICRAC). The PI(3)K product phosphatidylinositol-3,4,5-trisphosphate (PI(3,4,5)P3) is an important lipid mediator that regulates the activity of various enzymes, such as Btk, the serine-threonine kinase Akt, the phosphoinositide-dependent kinase PDK1, phospholipase D (PLD) and sphingosine kinase (SK), and the formation of other lipid mediators, such as diacylglycerol and sphingosine 1-phosphate (S1P). Sphingosine 1-phosphate can act intracellulary to regulate Ca2+ influx and degranulation (independently of phospholipase C and inositol-1,4,5-trisphosphate) and extracellularly (after secretion from the cell) by binding to the S1P1 or S1P2 surface receptor, thereby inducing cytoskeletal rearrangement or enhancing degranulation, respectively. The IKK complex consists of two catalytic subunits, IKKα (IKK1) and IKKβ (IKK2), and a regulatory subunit, NEMO (IKKγ); this complex phosphorylates IκB to activate NF-κB. IKKβ also phosphorylates SNAP-23 to facilitate formation of the SNARE complex. Arrows indicate the contributions of these signaling pathways to the degranulation of mast cells, the metabolism of arachidonic acid, and the production of cytokines, chemokines and growth factors (some arrows do not indicate direct interactions or targets). Bcl-10, adaptor protein; CaM, calmodulin; Gads, adaptor protein; Jnk, Janus kinase; MALT1, adaptor protein; MEK, mitogen-activated protein kinase (MAPK) kinase; MEKK, MAPK kinase kinase; PAK65, serine kinase; PKC-δ, protein kinase C- δ; Rac, small GTPase; Raf, Ras effector molecule; RasGRP, Ras guanyl nucleotide–releasing protein; SEK1, MAPK kinase; Sph, sphingosine.
In addition to its aforementioned signal-initiating activity, Lyn also negatively regulates FcɛRI-induced signaling events (including Fyn activation)9. Indeed, Lyn-deficient mast cells and mice are hyper-responsive to stimulation with IgE plus antigen9,16,17. A third Src family kinase, Hck, has a positive regulatory function in FcɛRI-induced mast cell degranulation and cytokine release through Lyn-dependent and Lyn-independent mechanisms (both of which are dependent, at least in part, on phosphorylation of the FcɛRI β-chain)18. The Lyn-dependent mechanism involves Hck-mediated suppression of Lyn's negative regulatory kinase activity. Hck−/− bone marrow–derived cultured mast cells (BMCMCs) have more Lyn activity and phosphorylation of various Lyn targets, such as the phosphatase SHIP, whereas they have less phosphorylation of various positive regulatory molecules such as Syk18. On the basis of those findings, the following hierarchical relationship among the Src family kinases downstream of FcɛRI has been proposed: Hck negatively regulates Lyn, which negatively regulates Fyn18. Additional studies are needed to understand more fully the interaction among Src family kinases downstream of FcɛRI. For example, why is Fyn activity normal in Hck−/− BMCMCs despite the greater activity of Lyn?
Phospholipase C-γ hydrolyzes phosphatidylinositol-4,5-bisphosphate to form soluble inositol-1,4,5-trisphosphate and membrane-bound diacylglycerol7,9,11,12,13. The binding of inositol-1,4,5-trisphosphate to its receptor in the endoplasmic reticulum rapidly induces the first stage of calcium (Ca2+) mobilization, which is the transient release of Ca2+ from endoplasmic reticulum stores; this in turn induces prolonged influx of Ca2+ through store-operated calcium release–activated calcium (CRAC) channels in the plasma membrane (Fig. 1). The identification of STIM1, a sensor of endoplasmic reticulum Ca2+ concentrations that couples depletion of endoplasmic reticulum Ca2+ stores with activation of CRAC channels19,20, and CRACM1 (also called Orai1), the pore-forming subunit of the CRAC channel21,22,23,24, has increased the understanding of CRAC currents at the molecular level. Researchers studying STIM1-deficient mice have found that STIM1 is required for FcɛRI-induced Ca2+ influx, degranulation, activation of the transcription factors NF-κB and NFAT, and IgE-dependent anaphylaxis in vivo25. Others have used CRACM1-deficient mice to show that CRACM1 is required for FcɛRI-induced degranulation, synthesis of lipid mediators, cytokine release and IgE-dependent allergic responses in vivo26. Such studies have demonstrated conclusively that the second stage of FcɛRI-induced Ca2+ mobilization, which is the influx of Ca2+ mediated by STIM1 and CRACM1, is essential for mast cell activation in vitro and in vivo25,26.
Other work indicates that canonical transient receptor potential channels (TRPCs), which are calcium-permeable nonselective cation channels, may associate with STIM1 and CRACM1 to enhance Ca2+ entry27,28. Researchers using inhibitory RNA in a rat mast cell line (RBL-2H3) have identified an additional requirement for TRPC5, in addition to STIM1 and CRACM1, for optimal FcɛRI-induced Ca2+ influx and degranulation29. They propose that strontium-permeable TRPC5 associates with STIM1 and CRACM1 in a stoichiometric way to enhance FcɛRI-induced Ca2+ influx and degranulation in mast cells29.
The rate of Ca2+ influx through store-operated channels is also dependent on the membrane potential, which is regulated by calcium-activated nonselective cation channels30 such as TRPM4. TRPM4 activates a calcium-activated nonselective current that depolarizes membrane potential and limits the driving force for Ca2+ entry through CRAC channels in BMCMCs31. FcɛRI-induced degranulation, release of leukotrienes and production of tumor necrosis factor (TNF), but not interleukin 6 (IL-6), are higher in TRPM4-deficient BMCMCs, and TRPM4-deficient mice develop more-severe acute (but not late-phase) inflammation during IgE-mediated passive cutaneous anaphylaxis responses31. Accordingly, it has been proposed that TRPM4 acts as a 'molecular brake' on Ca2+ influx after FcɛRI-induced activation of mast cells in vitro and in vivo31.
Downstream of early FcɛRI-induced signaling events (such as Ca2+ influx), the final stages of mast cell degranulation require membrane fusion events. The exocytosis of mast cell granules, or secretory lysosomes, is mediated by membrane fusion proteins called SNAREs (soluble N-ethyl-maleimide-sensitive factor–attachment protein receptors)32,33,34,35,36. These are categorized as t-SNAREs (such as syntaxins and SNAPs (soluble N-ethyl-maleimide-sensitive factor–attachment proteins)), which are located on the target membrane, and v-SNAREs (such as vesicle-associated membrane proteins (VAMPs), which are located on the vesicle membrane. Rodent and human mast cells express VAMP-2, VAMP-3, VAMP-7 and VAMP-8, and both VAMP-7 and VAMP-8 localize together with secretory granules in RBL-2H3 cells34,37. Two groups have shown that FcɛRI-induced exocytosis is diminished in VAMP-8-deficient mast cells38,39. One group has reported that this defect is limited to a distinct subset of secretory granules that contain serotonin and cathepsin D38. However, in that study, VAMP-8-deficient mast cells did not show any defects in the regulated exocytosis of granules containing histamine38. In contrast, the other group has shown that FcɛRI-induced β-hexosaminidase and histamine release in vitro is approximately 50% lower in the absence of VAMP-8 (ref. 39). Moreover, they show that VAMP-8-deficient mice have lower concentrations of blood histamine during passive systemic anaphylaxis39. Although these groups used different VAMP-8-deficient mice, the reason for the discrepancies in their findings remains to be determined. Another study has shown that inhibition of syntaxin 4, SNAP23, VAMP-7 or VAMP-8 blocks FcɛRI-induced release of histamine in primary human mast cells but inhibition of VAMP-2 or VAMP-3 does not40.
The t-SNAREs syntaxin 4 and SNAP-23 regulate FcɛRI-induced exocytosis from mast cells32,34, and phosphorylation of SNAP-23 on the serine residues at positions 120 and 95 has been shown to modulate exocytic events41. Inhibitory κB kinase-β (also called IKK2), one of two catalytically active subunits of the IKK complex, phosphorylates SNAP-23 on those serine residues42. Although the IKK complex is best known for its involvement in activating the transcription factor NF-κB, this IKKβ-mediated phosphorylation of SNAP-23 upregulates FcɛRI-induced degranulation in vitro in an NF-κB-independent way42. Moreover, IKKβ in mast cells is critical in enhancing IgE-mediated acute local or systemic reactions in vivo independently of NF-κB42. Conversely, the IKKβ-mediated enhancement of cutaneous late-phase reactions in vivo (which are promoted by the release of proinflammatory cytokines) occurs in an NF-κB-dependent way42. These results suggest that IKKβ may have additional substrates that allow this kinase to regulate NF-κB-independent mast cell activation events, such as the formation of SNARE complexes.
In addition to SNAREs, Rab GTPases regulate exocytic events33,35,36. Rab27a and its effector, Munc13-4, enhance FcɛRI-induced degranulation of mast cells43. The calcium sensor Doc2α, previously thought to be a brain-specific isoform of the Doc2 family that regulates calcium-dependent synaptic vesicle exocytosis, is expressed in mast cells44. Doc2α localizes together with Munc13-4 on secretory granules in RBL-2H3 cells, and BMCMCs from Doc2α-deficient mice have less FcɛRI-induced calcium-dependent exocytosis of secretory lysosomes44.
Mast cell activation through FcɛRI can be enhanced when the cells are exposed to certain ligands recognized by other receptors expressed on the mast cell surface7,11. For example, stem cell factor, the ligand for c-Kit, can both enhance FcɛRI-dependent activation of mouse or human mast cells and, in certain circumstances, directly induce mast cell degranulation7,11,45. The IL-1 family receptor T1 (also called ST2), which is the receptor for IL-33 (ref. 46), is expressed by mouse47,48,49 and human50,51 mast cells. ST2 is also expressed on T helper type 2 cells, and IL-33–ST2 interactions can induce T helper type 2 cells to produce IL-4, IL-5 and IL-13 (ref. 46). IL-33 can also induce mast cells to produce IL-13 (refs. 48,50,51) and several other cytokines48,49,50,51 and can substantially enhance the production of such cytokines by mouse48 or human51 mast cells that are costimulated through FcɛRI. Although the importance of IL-33–ST2 interactions in mast cell biology in vivo remains mostly undefined, evidence indicates that activation of mast cells that is dependent on IL-33–ST2 may exacerbate collagen-induced arthritis in mice52. This finding suggests that IL-33–mast cell interactions may have important functions in settings beyond immune responses or allergic disorders associated with T helper type 2 cells and IgE.
Negative regulation of mast cell activation through FcɛRI
Several negative intracellular regulators, such as the lipid phosphatase SHIP, can diminish FcɛRI-induced signaling events (Fig. 2). Some signaling molecules initiate both activating and inhibitory signals, for example, Lyn phosphorylates FcɛRI ITAMs as well as inhibitory receptor immunoreceptor tyrosine-based inhibitory motifs (ITIMs). The latter leads to recruitment of inhibitory signaling molecules such as SHIP. Other signaling molecules can negatively regulate FcɛRI-induced mast cell–activation events by altering the rate of FcɛRI internalization; for example, one function of RabGEF1 is to enhance FcɛRI internalization53,54. RGS13 (regulator of G protein signaling (RGS) 13) has been identified as a negative regulator of FcɛRI-induced degranulation (but not of production of the cytokines TNF, IL-6 and IL-13) in vitro and IgE-dependent passive cutaneous and systemic anaphylaxis in vivo55. RGS proteins typically inhibit G protein–coupled receptor signaling events through GTPase-accelerating protein activity on Gα subunits. Although G protein–coupled receptor signaling can amplify FcɛRI-mediated responses through activation of PI(3)Kγ56, RGS13-mediated inhibition of FcɛRI-induced activation occurs independently of RGS13's GTPase-accelerating protein activity55. Instead, it has been proposed that RGS13, which is upregulated after antigen stimulation, binds to the p85α subunit of PI(3)K and disrupts its association with an FcɛRI-activated signaling complex containing Gab2 and Grb2 (ref. 55; Fig. 2).
FcɛRI aggregation activates many proteins that negatively regulate the positive signaling pathways activated downstream of this receptor. For example, Lyn, which initiates both activating and inhibitory signals, negatively regulates Fyn activity and, thus, Gab2 phosphorylation. Other negative regulators include c-Cbl (which facilitates the ubiquitination of FcɛRI, Lyn and Syk), the tyrosine phosphatase SHP-1 (which dephosphorylates Syk), the lipid phosphatases SHIP (which catalyzes the hydrolysis of phosphatidylinositol-3,4,5-trisphosphate to phosphatidylinositol-3,4-bisphosphate (PI(3,4)P2)) and PTEN (which catalyzes the hydrolysis of phosphatidylinositol-3,4,5-trisphosphate to phosphatidylinositol-4,5-bisphosphate (PI(4,5)P2)), RasGAP (which enhances the intrinsic GTPase activity of Ras), RabGEF1 (which enhances FcɛRI internalization and can bind to GTP-bound Ras) and RGS13 (which binds to the p85α subunit of PI(3)K and disrupts its association with Gab2 and Grb2). Antigen-induced aggregation of FcɛRI with FcγRIIB inhibits FcɛRI-induced signaling events and mast cell activation through Lyn-mediated phosphorylation of the FcγRIIB ITIM (red) and the subsequent recruitment of SHIP and the docking protein DOK1. Finally, ES-62 (a glycoprotein secreted by filanial neatodes) forms a complex with Toll-like receptor 4 (TLR4), which causes the sequestration and subsequent proteosome-independent degradation of protein kinase C-α (PKC-α) to block FcɛRI-induced phospholipase D–coupled, sphingosine kinase–mediated Ca2+ flux and NF-κB activation.
In addition to negative intracellular regulators, signaling events initiated by FcɛRI and other ITAM-containing immunoreceptors are negatively regulated by their aggregation together with ITIM-containing receptors. Mast cells express several inhibitory receptors, including FcγRIIB, gp49B1, MAFA and PIR-B7,13. FcγRIIB, the first ITIM-containing receptor identified, is a likely therapeutic target for mast cell–activation events because it recruits SHIP after aggregation together with FcɛRI in vivo57 (Fig. 2).
It has been reported that ES-62, a glycoprotein secreted by filarial nematodes, might also be investigated as a new therapeutic agent for allergy58. ES-62 inhibits the activation of many immune cells, including B cells, T cells, dendritic cells and macrophages. ES-62 also inhibits FcɛRI-induced degranulation, the metabolism of arachidonic acid and the production of TNF, IL-3 and IL-6 (but not IL-13 or IL-5) in human BMCMCs. ES-62 mediates these effects by forming a complex with Toll-like receptor 4, which causes sequestration and proteasome-independent degradation of protein kinase C-α, resulting in less phospholipase D–coupled, sphingosine kinase–mediated Ca2+ influx and NF-κB activation58 (Fig. 2). Moreover, in model systems, ES-62 decreases the magnitude of oxazolone-induced cutaneous immediate-type hypersensitivity as well as ovalbumin-induced airway hyper-reactivity to methacholine and of airway allergic inflammation in mice sensitized to ovalbumin admixed with aluminum hydroxide as an adjuvant58. According to the authors of these studies, ES-62-mediated suppression of mast cell activation may contribute to the lower incidence of allergic disorders in people harboring worms and, because ES-62 seems to be well tolerated by millions of infected people, ES-62 derivatives might represent a new type of therapeutic agent for diseases such as asthma.
New developments in mast cell models
Human mast cell populations and mouse BMCMCs, as well as cultured mast cells derived from other hematopoietic tissues (such as fetal liver) or embryonic stem cells, are powerful tools for investigating the mechanisms by which mast cells might influence various immunological or other biological responses in vitro. Although there are many similarities between mast cell populations in humans and in mice, there are also some differences in their anatomical distributions, phenotypes and functions that may influence the specific roles of mast cells in various biological responses in the two species2,59. However, the ability to manipulate the number, phenotype or function of human mast cells in vivo is limited. Thus, many investigators have attempted to analyze mast cell function with more tractable experimental species, especially the mouse.
The in vivo relevance and biological importance of in vitro observations about mast cell function, as well as the contributions of mast cells to the expression of particular biological responses in vivo, can be assessed with Kit mutant mice (either WBB6F1-KitW/W-v or C57BL/6-KitW-sh/W-sh mice) that almost completely lack mast cell populations60,61,62,63,64,65. The mast cell deficiency of these mice can be selectively 'repaired' through the adoptive transfer of genetically compatible, in vitro–derived mast cells from congenic wild-type mice or various transgenic or mutant mice62,64,65 or from mouse embryonic stem cells63, or mast cells that have been transduced with short hairpin RNA to decrease the expression of proteins of interest66. Such 'mast cell–knock-in' mice are now in wide use to assess the contributions of mast cells or specific mast cell products to diverse biological responses in vivo.
C57BL/6-KitW-sh/W-sh mice are gaining popularity for such studies because these mice have fewer or less-severe phenotypic abnormalities than those of WBB6F1-KitW/W-v mice. For example, unlike WBB6F1-KitW/W-v mice, C57BL/6-KitW-sh/W-sh mice are neither anemic nor sterile, and they seem to have normal numbers of bone marrow and blood neutrophils64,67. It is important to consider the genetic background of the mice and the effects of the different Kit mutations on other cell lineages when studying various disease models. For example, whereas one group has shown that WBB6F1-KitW/W-v mice are resistant to the development of joint inflammation in a model of autoantibody-induced arthritis68, another group has reported that mast cell–deficient C57BL/6-KitW-sh/W-sh mice develop autoantibody-mediated, neutrophil-dependent immune-complex arthritis but mast cell–deficient WBB6F1-KitW/W-v mice do not67. The authors attribute this difference to the relative neutrophil deficiency of WBB6F1-KitW/W-v mice67.
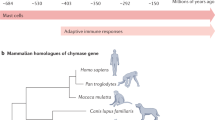
Two groups have reported the generation of mast cell–specific 'Cre' mice. Transgenic mice have been generated that express Cre recombinase under the control of the promoter of the gene encoding mast cell protease 5 (Cma1, called 'Mcpt5' here)69. Using ROSA26-EYFP mice69, these authors show that efficient Cre-mediated recombination occurs in mast cells from the peritoneal cavity and skin, whereas only minimal reporter gene expression is detected outside the mast cell compartment. Cre expressed under the control of the promoter of the gene encoding baboon α-chymase in ROSA26R mice results in Cre-mediated recombination in mast cells of the lungs and colon tissue but not in mast cells isolated from the peritoneal cavity or in vitro–generated BMCMCs70. Care must be taken both in characterizing the phenotypic features of such mice (as expressed in mast cells and possibly in other cell types) and in interpreting the results of experiments with such mice. However, mice with confirmed mast cell–specific Cre expression and mice with inducible mast cell–specific Cre expression may well become powerful genetic models for investigating the contributions of mast cells or mast cell–specific products to health and disease.
Mast cell proteases and host defense
Mast cells are strategically located very near sites where the body comes in contact with the external environment, which is a prime location for the initiation and modulation of innate immune responses. Indeed, mast cells can provide important contributions to innate bacterial clearance, at least in part by enhancing the recruitment of neutrophils to the site of infection71,72. Many in vitro or in vivo studies have provided additional evidence that mast cells can enhance host defense through direct effects on pathogens by initiating and modulating the inflammation associated with innate immune responses and perhaps by initiating adaptive immune responses to pathogens.
Another protective function of mast cells during innate responses to bacterial infection is to limit the toxicity of certain products generated by the host, which can have adverse effects at high concentrations. For example, mast cells can limit the toxicity of the peptide endothelin 1 (ET-1), whose concentrations are much higher during acute bacterial peritonitis and sepsis, by releasing proteases stored in their granules that can degrade this peptide73,74. ET-1 has high homology to sarafotoxins (the most toxic components of venom from the Israeli mole viper (Atractaspis engaddensis)). Mast cells can substantially enhance resistance to the pathology and mortality induced in mice by the venoms from A. engaddensis and two other poisonous snakes and that of the honeybee66. Both short hairpin RNA and pharmacological methods have been used to show that a mast cell–mediated decrease in endogenous (ET-1) and exogenous (sarafotoxin) toxic peptides is dependent on the activity of carboxypeptidase A3 (CPA3); however, mast cells that lack CPA3 concomitantly lack mast cell protease 5 (MCP-5; refs. 66,74). In an elegant study, a mutant mouse has been generated bearing two amino acid substitutions that render CPA3 catalytically inactive without affecting the expression of other proteases74. Using this mutant, the authors confirm that mast cell–mediated innate defense against ET-1 and sarafotoxin is dependent on CPA3 activity, and they define the molecular mechanism by which CPA3 inactivates these toxins74.
In addition to ET-1, concentrations of neurotensin (a peptide known to induce hypotension) have been shown to be higher in a mouse model of sepsis75. In mice, neurotensin can contribute to sepsis-related mortality, whereas mast cells can lower neurotensin concentrations in vivo by degrading neurotensin through the protease neurolysin75. Mast cells can decrease neurotensin-induced hypotension as well as sepsis-related mortality75. Moreover, a pilot study of human patients with sepsis (or with cardiogenic shock) has shown that their plasma concentrations of neurotensin are increased to concentrations similar to those in mice with acute bacterial peritonitis75. Because sepsis is the most common cause of death in intensive care units in the United States, there is considerable interest in identifying additional biomarkers and therapeutic targets in this disorder. The findings reported above75 raise the possibility that neurotensin might contribute to the pathology of patients with sepsis; therefore, inhibiting the pathological actions of neurotensin may confer a benefit in this setting.
Although IL-15 is known to be critical in innate immunity, IL-15-deficient mice are actually less susceptible to sepsis-related mortality76. Moreover, WBB6F1-KitW/W-v mice engrafted with IL-15-deficient mast cells survive better than those engrafted with wild-type mast cells. Mast cells express intracellular IL-15, both constitutively and after stimulation with lipopolysaccharide, which seems to function as a negative transcriptional regulator of the mast cell chymase MCP-2 (ref. 76). The authors propose that this IL-15-mediated repression of MCP-2 activity limits the bactericidal activity of mast cells and the recruitment of neutrophils needed to clear the bacterial infection.
Further emphasizing the importance of mast cell proteases in innate host defense, others have reported that the mast cell tryptase MCP-6 (also called Tpsb2) can have a critical protective function in bacterial infection77. MCP-6-deficient mice are less able to clear Klebsiella pneumoniae injected into their peritoneal cavities, probably because of less recruitment of neutrophils77. The authors suggest that MCP-6 is the main preformed granule mediator of mast cells that can protect mice during acute bacterial infection77; however, the mechanism by which MCP-6 induces the recruitment of neutrophils to the site of infection remains to be determined.
Mast cell proteases also can contribute to resistance to infection with parasites. For example, delayed expulsion of the adult helminth and increased deposition of larvae in muscles occur in MCP-1-deficient mice infected with Trichinella spiralis78. MCP-6 is important for the clearance of chronic T. spiralis infection79; the recruitment of eosinophils to T. spiralis larvae and the elimination of larvae in chronically infected skeletal muscle are lower in MCP-6-deficient mice. Because eosinophil infiltration around T. spiralis larvae is also lower in IgE-deficient mice, the authors suggest that mast cells and, more specifically, MCP-6 link adaptive and innate immunity in the chronic phase of T. spiralis infection79.
Mast cell proteases: limiting allergic reactions
In addition to helping out in host defense, mast cell proteases may have beneficial functions during allergic disorders. Mast cells are typically thought of as troublesome cells because of their prominent function as effector cells in IgE-dependent allergic hypersensitivity reactions such as allergic rhinitis (hay fever), atopic dermatitis (eczema), allergic (or 'atopic') asthma and some food allergies. However, β-tryptase, a protease released by mast cells, can cleave IgE80. IgE cleavage products can be detected in tissue fluids collected from sites of allergic inflammation, and protamine, an inhibitor of heparin-dependent proteases, enhances IgE-mediated allergic skin inflammation induced by skin-prick testing in human subjects80. Although protamine treatment may have other effects that influence the magnitude of the biological responses analyzed, the findings suggest that mast cell protease–dependent degradation of IgE may help limit this type of allergic inflammation. The extent to which this mechanism can contribute to the decrease in local (or systemic) IgE concentrations during other examples of allergic inflammation remains to be determined.
Immunomodulatory functions of mast cells: slowing things down
Mast cells can exert positive or negative immunomodulatory effects on immune cells by influencing the recruitment, survival, development, phenotype or function of immune cells and thereby enhance or suppress the initiation, magnitude and/or duration of immune responses6. Because they might at first seem counterintuitive, given the mast cell's well-deserved reputation as a promoter of inflammation, we will first discuss some negative immunomodulatory functions of this cell. An early study showed that the ability of ultraviolet B irradiation of the skin to induce systemic immunosuppression of contact hypersensitivity responses was mast cell dependent81. Ultraviolet irradiation–induced migration of mast cells from the skin to the draining lymph nodes, which is mediated by the chemokine receptor CXCR4 on mast cells, is a key step in the induction of ultraviolet irradiation–induced immunosuppression82. Mast cells have also been shown to mediate immunosuppressive functions after bites by anopheles mosquitos83 and in peripheral tolerance to skin allografts (which requires the participation of CD4+CD25+Foxp3+ regulatory T cells)84. However, the mechanisms by which mast cells mediate immunosuppressive functions in each of these studies remain to be elucidated.
Mast cells can mediate negative immunomodulatory functions in vivo by producing IL-10 (ref. 85). Mast cells and mast cell–derived IL-10 limit the magnitude of and promote the resolution of contact hypersensitivity responses induced in response to the hapten DNFB (2,4-dinitro-1-fluorobenzene) or urushiol (Fig. 3), which is the hapten-containing sap of poison ivy (Toxicodendron radicans) or poison oak (Toxicodendron diversilobum)85. Mast cells and mast cell–derived IL-10 also suppress innate cutaneous responses to chronic low-dose ultraviolet B irradiation85. Although mast cells limit many aspects of these responses, including inflammation, epidermal hyperplasia and skin ulceration, the pathways that link mast cell–derived IL-10 (or other mast cell mediators that are relevant in this setting) to the observed tissue changes remain to be defined. Mast cells and mast cell–derived IL-10 may influence these responses through a complex combination of direct and indirect effector and immunomoregulatory functions.
Cross-sections of ears (stained with Masson's Trichrome) from WBB6F1-Kit+/+ (wild-type) mice (a,b), WBB6F1-KitW/W-v mice (c,d) and WBB6F1-KitW/W-v mice engrafted 8 weeks before the experiment with wild-type BMCMCs (WT BMCMC→KitW/W-v; e,f) or Il10−/− BMCMCs (Il10−/− BMCMC→KitW/W-v; g,h), obtained 5 d after challenge with vehicle only (100% acetone; a,c,e,g) or 5 mg/ml of urushiol (b,d,f,h). Focal full-thickness necrosis of the epidermis and/or ulceration occurred in association with contact hypersensitivity responses to urushiol at 5 d after challenge in eight of ten mast cell–deficient WBB6F1-KitW/W-v mice and in eight of eight KitW/W-v mice given Il10−/− BMCMCs but in none of ten WBB6F1-Kit+/+ mice or seven KitW/W-v mice given wild-type BMCMCs. P < 0.05, WBB6F1-Kit+/+ versus WBB6F1-KitW/W-v or WT BMCMC→KitW/W-v versus Il10−/− BMCMC→KitW/W-v (Chi-squared test). Similar results were obtained for contact hypersensitivity responses to urushiol in five of seven C57BL/6-KitW-sh/W-sh mice in response to the hapten DNFB (data not shown). In contrast, epidermal necrosis and ulceration occurred in none of the corresponding congenic wild-type mice or C57BL/6-KitW-sh/W-sh mice engrafted with wild-type BMCMCs (10 or 8 for urushiol and 19 or 16 for DNFB, respectively). P < 0.05, wild-type mice or C57BL/6-KitW-sh/W-sh mice engrafted with wild-type BMCMC versus the corresponding mast cell–deficient C57BL/6-KitW-sh/W-sh mice (Chi-squared test). Double-headed yellow arrows (d) indicate the thickness of the dermis (D) or epidermis (Ep); arrows in insets indicate ulcers with adherent exudates (red). C*, cartilage. Scale bars, 100 μm (main image) or 1,000 μm (inset). Results are representative of three experiments (n = 3–7 mice per group per experiment) and are from ref. 85.
Immunomodulatory functions of mast cells: revving things up
Mast cells also can enhance the development of various T cell–associated immune responses in mice, including models of multiple sclerosis (experimental autoimmune encephalomyelitis)86 and bullous pemphigoid87. Mast cells and mast cell–derived TNF have been shown to contribute to disease pathology in a model of lung inflammation dependent on IL-17-producing T helper cells and associated with neutrophil recruitment in ovalbumin-challenged, ovalbumin-specific T cell receptor–transgenic mice88. Moreover, mast cells contribute to the development of delayed-type contact hypersensitivity (also called allergic contact dermatitis) in some but not all experimental conditions5,89,90. Using various immunizing doses of the hapten oxazolone, one group has shown that mast cells can act to diminish or enhance the inflammatory response in contact hypersensitivity reactions depending on the concentration of hapten used for immunization91.
Several mast cell–derived products can influence the development, recruitment, phenotype, proliferation and activation of T cells in vitro and in vivo5,6,86,88,92,93. Mast cells can promote T cell activation indirectly through the stimulation of antigen-presenting cells in vivo; for example, mast cells induce the migration of dendritic cells93 and Langerhans cells92,94 to draining lymph nodes where antigen presentation occurs. Moreover, antigen incorporated into mast cells through FcɛRI can activate antigen-specific T cell responses in vitro95; this mechanism is independent of the expression of major histocompatibility complex class II by mast cells but requires that such mast cells undergo apoptosis and then ingestion by antigen-presenting cells.
Because mast cells can help to initiate adaptive immune responses by inducing or enhancing the migration of antigen-presenting cells to draining lymph nodes and through lymphocyte activation, one group has hypothesized that the administration of small-molecule mast cell activators (such as compound 48/80) with vaccine antigens might enhance the development of a protective antigen-specific immune response96. Indeed, they have found that subcutaneous or nasal administration of such activators enhances the trafficking of dendritic cells and lymphocytes to draining lymph nodes and increases antigen-specific serum IgG responses96. Moreover, nasal administration of compound 48/80 with B5R poxvirus protein protects immunized mice against infection with vaccinia virus in vivo but B5R poxvirus protein alone does not. The authors show that mast cells and mast cell–derived TNF are required for the enhancement of immune responses in WBB6F1-KitW/W-v mice engrafted with mast cells in the footpad and then vaccinated at the same site; however, their efforts to engraft mast cells in the nasal cavity of mast cell–deficient mice were unsuccessful. As noted above, WBB6F1-KitW/W-v mice have defects beyond a profound deficiency of mast cells, including neutrophil defects, and mast cell activators can have effects on cell types other than mast cells. However, from a clinical perspective, if this new vaccination approach can be shown to be effective and, just as important, safe (as mast cell activation in the context of vaccination could result in clinical toxicities), this approach may be of considerable value even if the method works because of effects on cells in addition to (or other than) mast cells.
Mast cells in cardiovascular disorders
Several lines of evidence have linked mast cells to the development of a variety of chronic inflammatory disorders, including cardiovascular disease. Because mast cells are found in the heart and, in humans, around coronary arteries and in atherosclerotic lesions, several groups have proposed that mast cells may contribute to the pathogenesis of atherogenesis97,98,99. Indeed, targeted activation of perivascular mast cells promotes atherogenesis and plaque destabilization in apolipoprotein E–deficient mice97. By crossing atherosclerosis-prone mice deficient in low-density lipoprotein receptor with C57BL/6-KitW-sh/W-sh mice, others have provided in vivo evidence that mast cells can contribute to atherosclerosis99, as smaller lesions with fewer inflammatory cell (macrophage and T cell) infiltrates are noted in the absence of mast cells. There is evidence that mast cells promote atherosclerosis in this setting by releasing proinflammatory cytokines (IL-6 and interferon-γ) that augment the expression of matrix-degrading proteases99. This group has also reported that mast cells contribute to the pathogenesis of elastase-induced abdominal aortic aneurysms in mice, as C57BL/6-KitW-sh/W-sh mice fail to develop such aneurysms100. They show that the formation of such aneurysms in this model requires mast cell–derived IL-6 and IFN-γ, but not TNF, and that mast cells increase the expression of matrix-degrading proteases, the apoptosis of smooth muscle cells and microvessel growth100. Similarly, others have shown that the formation of such aneurysms after periaortic application of calcium chloride (accompanied by more mast cells and T cells, activation of matrix metalloproteinase 9, and angiogenesis in the aortic tissue) is impaired in mast cell–deficient Ws/Ws rats101.
Mast cells in cancer
The importance of a possible functional link between chronic inflammation and cancer has long been recognized; for example, treatment with nonsteroidal anti-inflammatory drugs, which can inhibit chronic inflammation, decreases the risk of several cancers102. Most tumors contain inflammatory cells, including mast cells, which have potential effects that might either benefit the tumor or contribute to tumor resistance or rejection. Experiments with WBB6F1-KitW/W-v mice have provided evidence that mast cells can facilitate angiogenesis during early stages of skin carcinogenesis103. Pharmacological approaches (cromolyn) and genetic approaches (C57BL/6-KitW-sh/W-sh mice) suggest that mast cells also may be required for the angiogenesis and macroscopic expansion of c-Myc-induced pancreatic β-cell tumors104. Although cromolyn is widely characterized as a 'mast cell stabilizer' (as an agent that blocks the release of mast cell mediators after appropriate activation of the cell) that suppresses mouse mast cell function in vivo, its molecular targets are neither fully defined nor restricted to mast cells6. Moreover, because c-Kit signaling has been shown to be important for angiogenesis105 and cell lineages other than mast cells are affected by the Kit mutation in C57BL/6-KitW-sh/W-sh mice, it will be useful to assess whether engraftment of the C57BL/6-KitW-sh/W-sh mice with mast cells can restore wild-type responsiveness in this model of tumor progression. However, these results and others collectively indicate that certain tumors may 'hijack' certain functions of mast cells to facilitate angiogenesis and contribute to tumor survival.
Mutations of the gene encoding the tumor suppressor adenomatous polyposis coli are necessary and sufficient for the initiation of hereditary and many spontaneous human colorectal cancers106,107. Angiogenesis and tissue remodeling are also required for tumor expansion. One group has shown that mast cells accumulate in adenomatous polyps (in a lymphocyte-independent way) and are required for polyp formation106, the initiating step of colon cancer. Polyp-prone mice with a mutant adenomatous polyposis coli protein reconstituted with bone marrow from wild-type, C57BL/6-KitW-sh/W-sh or Cd34−/−Cd43−/− mice have demonstrated a tight correlation between the number of mast cells and mast cell progenitors and the frequency and size of polyps in these mice (wild-type > C57BL/6-KitW-sh/W-sh > Cd34−/−Cd43−/−). Blood vessel density was higher in mice transplanted with wild-type marrow than in those transplanted with Cd34−/−Cd43−/− marrow106. The authors show that TNF is required for the growth of adenomatous polyps and propose that mast cell–derived TNF acts in an autocrine way to amplify the local mast cell pool at the site of tumor formation106. They conclude that mast cells contribute importantly to the development of colon cancer. The preceding results are consistent with those in a study reporting lower susceptibility of WBB6F1-KitW/W-v mice to chemically induced intestinal tumors108. Engraftment of the WBB6F1-KitW/W-v mice with wild-type bone marrow cells increases carcinogen-induced tumorigenesis to nearly wild-type amounts, consistent with involvement of mast cells in this process. However, engraftment of wild-type BMCMCs fails to result in mucosal mast cells in WBB6F1-KitW/W-v recipients and also fails to 'normalize' the response of the mice to the carcinogen108.
Although other evidence also suggests that mast cells can promote tumorigenesis and tumor progression, there are some tumor models in which mast cells seem to have functions that favor the host. For example, one report has demonstrated a protective a function for mast cells in colorectal tumorigenesis107. Mice resulting from the crossing of C57BL/6-KitW-sh/W-sh mice with mice that have multiple intestinal neoplasia (a model for early intestinal tumorigenesis) have a greater frequency and size of adenomas, whereas they have less tumor cell apoptosis and eosinophil infiltration107. The authors of that study suggest that the net contributions of mast cells in various tumor models may favor the host or the tumor depending on the specific tumor model, genetic variables (both germline and tumor specific) and microenvironmental factors (such as intestinal flora in gastrointestinal tumors). The story is probably as complicated (if not more so) in humans, given that humans, as well as their colonic neoplasms, are so diverse.
Conclusions
New evidence indicating that mast cells can contribute to the pathology of cardiovascular diseases and certain cancers (at least in rodents) continues to tarnish the reputation of this enigmatic cell. However, this 'bad guy' image is increasingly being challenged and, to some extent, overshadowed by identification of the many protective functions mast cells can serve in both innate and adaptive immune responses and even in host responses to some tumors (Fig. 4). But many issues of mast cell biology remain to be resolved. For example, certain features of mouse mast cell phenotype and/or function can vary considerably among different strains of mice109,110. It will be useful to define how and to what extent various genetic factors can influence aspects of mast cell biology in humans. However, this is likely to be a challenging topic to investigate. Another goal is to understand how the mast cell lineage can accomplish so many distinct functions depending on the setting, either promoting or limiting innate or adaptive immune responses6,111,112. Can mast cells, like T cells, generate developmentally, phenotypically and functionally distinct 'subsets', or do individual mast cells have sufficient plasticity to develop distinct features on the basis of their responsiveness to particular local and/or systemic environmental signals? Do both mechanisms occur? Finally, it will be important to assess how the understanding of mast cell biology can be exploited clinically. Defining to what extent the positive functions of mast cells can be enhanced safely or their harmful activities can be inhibited will continue to be an important goal, both for achieving a fuller understanding of this fascinating cell and for exploiting such knowledge to decrease disease and promote health.
Newly identified protective (green) or detrimental (red) functions of mast cells (MC) and mast cell products in biological responses in mice. Red inverted 'T', inhibition of MCP-2 mRNA expression by intracellular IL-15. AAA, abdominal aortic aneurysm; NLN, neurolysin; NT, neurotensin; SMC, smooth muscle cell.
References
Kitamura, Y. Heterogeneity of mast cells and phenotypic change between subpopulations. Annu. Rev. Immunol. 7, 59–76 (1989).
Mekori, Y.A. & Metcalfe, D.D. Mast cells in innate immunity. Immunol. Rev. 173, 131–140 (2000).
Kawakami, T. & Galli, S.J. Regulation of mast-cell and basophil function and survival by IgE. Nat. Rev. Immunol. 2, 773–786 (2002).
Marone, G., Galli, S.J. & Kitamura, Y. Probing the roles of mast cells and basophils in natural and acquired immunity, physiology and disease. Trends Immunol. 23, 425–427 (2002).
Metz, M. et al. Mast cells in the promotion and limitation of chronic inflammation. Immunol. Rev. 217, 304–328 (2007).
Galli, S.J., Grimbaldeston, M. & Tsai, M. Immunomodulatory mast cells: negative, as well as positive, regulators of immunity. Nat. Rev. Immunol. 8, 445–454 (2008).
Galli, S.J. et al. Mast cells as “tunable” effector and immunoregulatory cells: recent advances. Annu. Rev. Immunol. 23, 749–786 (2005).
Gurish, M.F. & Austen, K.F. The diverse roles of mast cells. J. Exp. Med. 194, F1–F5 (2001).
Rivera, J. & Gilfillan, A.M. Molecular regulation of mast cell activation. J. Allergy Clin. Immunol. 117, 1214–1225 (2006).
Nishida, K. et al. FcepsilonRI-mediated mast cell degranulation requires calcium-independent microtubule-dependent translocation of granules to the plasma membrane. J. Cell Biol. 170, 115–126 (2005).
Gilfillan, A.M. & Tkaczyk, C. Integrated signalling pathways for mast-cell activation. Nat. Rev. Immunol. 6, 218–230 (2006).
Kambayashi, T. & Koretzky, G.A. Proximal signaling events in FcɛRI-mediated mast cell activation. J. Allergy Clin. Immunol. 119, 544–552 (2007).
Kraft, S. & Kinet, J.P. New developments in FcɛRI regulation, function and inhibition. Nat. Rev. Immunol. 7, 365–378 (2007).
Rivera, J. & Olivera, A. Src family kinases and lipid mediators in control of allergic inflammation. Immunol. Rev. 217, 255–268 (2007).
Rios, E.J., Piliponsky, A.M., Ra, C., Kalesnikoff, J. & Galli, S.J. Rabaptin-5 regulates receptor expression and functional activation in mast cells. Blood published online, doi:10.1182/blood-2008-04-152660 (12 August 2008).
Hernandez-Hansen, V. et al. Dysregulated FcɛRI signaling and altered Fyn and SHIP activities in Lyn-deficient mast cells. J. Immunol. 173, 100–112 (2004).
Odom, S. et al. Negative regulation of immunoglobulin E-dependent allergic responses by Lyn kinase. J. Exp. Med. 199, 1491–1502 (2004).
Hong, H. et al. The Src family kinase Hck regulates mast cell activation by suppressing an inhibitory Src family kinase Lyn. Blood 110, 2511–2519 (2007).
Roos, J. et al. STIM1, an essential and conserved component of store-operated Ca2+ channel function. J. Cell Biol. 169, 435–445 (2005).
Liou, J. et al. STIM is a Ca2+ sensor essential for Ca2+-store-depletion-triggered Ca2+ influx. Curr. Biol. 15, 1235–1241 (2005).
Vig, M. et al. CRACM1 is a plasma membrane protein essential for store-operated Ca2+ entry. Science 312, 1220–1223 (2006).
Feske, S. et al. A mutation in Orai1 causes immune deficiency by abrogating CRAC channel function. Nature 441, 179–185 (2006).
Yeromin, A.V. et al. Molecular identification of the CRAC channel by altered ion selectivity in a mutant of Orai. Nature 443, 226–229 (2006).
Prakriya, M. et al. Orai1 is an essential pore subunit of the CRAC channel. Nature 443, 230–233 (2006).
Baba, Y. et al. Essential function for the calcium sensor STIM1 in mast cell activation and anaphylactic responses. Nat. Immunol. 9, 81–88 (2008).
Vig, M. et al. Defective mast cell effector functions in mice lacking the CRACM1 pore subunit of store-operated calcium release–activated calcium channels. Nat. Immunol. 9, 89–96 (2008).
Liao, Y. et al. Orai proteins interact with TRPC channels and confer responsiveness to store depletion. Proc. Natl. Acad. Sci. USA 104, 4682–4687 (2007).
Yuan, J.P., Zeng, W., Huang, G.N., Worley, P.F. & Muallem, S. STIM1 heteromultimerizes TRPC channels to determine their function as store-operated channels. Nat. Cell Biol. 9, 636–645 (2007).
Ma, H.T. et al. Canonical transient receptor potential 5 channel in conjunction with Orai1 and STIM1 allows Sr2+ entry, optimal influx of Ca2+, and degranulation in a rat mast cell line. J. Immunol. 180, 2233–2239 (2008).
Mohr, F.C. & Fewtrell, C. Depolarization of rat basophilic leukemia cells inhibits calcium uptake and exocytosis. J. Cell Biol. 104, 783–792 (1987).
Vennekens, R. et al. Increased IgE-dependent mast cell activation and anaphylactic responses in mice lacking the calcium-activated nonselective cation channel TRPM4. Nat. Immunol. 8, 312–320 (2007).
Guo, Z., Turner, C. & Castle, D. Relocation of the t-SNARE SNAP-23 from lamellipodia-like cell surface projections regulates compound exocytosis in mast cells. Cell 94, 537–548 (1998).
Jahn, R. & Sudhof, T.C. Membrane fusion and exocytosis. Annu. Rev. Biochem. 68, 863–911 (1999).
Paumet, F. et al. Soluble NSF attachment protein receptors (SNAREs) in RBL-2H3 mast cells: functional role of syntaxin 4 in exocytosis and identification of a vesicle-associated membrane protein 8-containing secretory compartment. J. Immunol. 164, 5850–5857 (2000).
Blank, U. et al. SNAREs and associated regulators in the control of exocytosis in the RBL-2H3 mast cell line. Mol. Immunol. 38, 1341–1345 (2002).
Logan, M.R., Odemuyiwa, S.O. & Moqbel, R. Understanding exocytosis in immune and inflammatory cells: the molecular basis of mediator secretion. J. Allergy Clin. Immunol. 111, 923–932 (2003).
Hibi, T., Hirashima, N. & Nakanishi, M. Rat basophilic leukemia cells express syntaxin-3 and VAMP-7 in granule membranes. Biochem. Biophys. Res. Commun. 271, 36–41 (2000).
Puri, N. & Roche, P.A. Mast cells possess distinct secretory granule subsets whose exocytosis is regulated by different SNARE isoforms. Proc. Natl. Acad. Sci. USA 105, 2580–2585 (2008).
Tiwari, N. et al. VAMP-8 segregates mast cell-preformed mediator exocytosis from cytokine trafficking pathways. Blood 111, 3665–3674 (2008).
Sander, L.E. et al. Vesicle associated membrane protein (VAMP)-7 and VAMP-8, but not VAMP-2 or VAMP-3, are required for activation-induced degranulation of mature human mast cells. Eur. J. Immunol. 38, 855–863 (2008).
Hepp, R. et al. Phosphorylation of SNAP-23 regulates exocytosis from mast cells. J. Biol. Chem. 280, 6610–6620 (2005).
Suzuki, K. & Verma, I.M. Phosphorylation of SNAP-23 by IκB kinase2 (IKK2/β) regulates anaphylactic reactions: NF-κB-independent regulation of mast cell exocytosis. Cell 134, 485–495 (2008).
Neeft, M. et al. Munc13–4 is an effector of rab27a and controls secretion of lysosomes in hematopoietic cells. Mol. Biol. Cell 16, 731–741 (2005).
Higashio, H. et al. Doc2alpha and Munc13-4 regulate Ca2+-dependent secretory lysosome exocytosis in mast cells. J. Immunol. 180, 4774–4784 (2008).
Costa, J.J. et al. Recombinant human stem cell factor (kit ligand) promotes human mast cell and melanocyte hyperplasia and functional activation in vivo. J. Exp. Med. 183, 2681–2686 (1996).
Schmitz, J. et al. IL-33, an interleukin-1-like cytokine that signals via the IL-1 receptor-related protein ST2 and induces T helper type 2-associated cytokines. Immunity 23, 479–490 (2005).
Moritz, D.R., Rodewald, H.R., Gheyselinck, J. & Klemenz, R. The IL-1 receptor-related T1 antigen is expressed on immature and mature mast cells and on fetal blood mast cell progenitors. J. Immunol. 161, 4866–4874 (1998).
Ho, L.H. et al. IL-33 induces IL-13 production by mouse mast cells independently of IgE-FcɛRI signals. J. Leukoc. Biol. 82, 1481–1490 (2007).
Moulin, D. et al. Interleukin (IL)-33 induces the release of pro-inflammatory mediators by mast cells. Cytokine 40, 216–225 (2007).
Allakhverdi, Z., Smith, D.E., Comeau, M.R. & Delespesse, G. Cutting edge: The ST2 ligand IL-33 potently activates and drives maturation of human mast cells. J. Immunol. 179, 2051–2054 (2007).
Iikura, M. et al. IL-33 can promote survival, adhesion and cytokine production in human mast cells. Lab. Invest. 87, 971–978 (2007).
Xu, D. et al. IL-33 exacerbates antigen-induced arthritis by activating mast cells. Proc. Natl. Acad. Sci. USA 105, 10913–10918 (2008).
Tam, S.Y. et al. RabGEF1 is a negative regulator of mast cell activation and skin inflammation. Nat. Immunol. 5, 844–852 (2004).
Kalesnikoff, J. et al. Roles of RabGEF1/Rabex-5 domains in regulating Fc epsilon RI surface expression and FcɛRI-dependent responses in mast cells. Blood 109, 5308–5317 (2007).
Bansal, G., Xie, Z., Rao, S., Nocka, K.H. & Druey, K.M. Suppression of immunoglobulin E-mediated allergic responses by regulator of G protein signaling 13. Nat. Immunol. 9, 73–80 (2008).
Laffargue, M. et al. Phosphoinositide 3-kinase γ is an essential amplifier of mast cell function. Immunity 16, 441–451 (2002).
Saxon, A., Kepley, C. & Zhang, K. “Accentuate the negative, eliminate the positive”: engineering allergy therapeutics to block allergic reactivity through negative signaling. J. Allergy Clin. Immunol. 121, 320–325 (2008).
Melendez, A.J. et al. Inhibition of FcɛRI-mediated mast cell responses by ES-62, a product of parasitic filarial nematodes. Nat. Med. 13, 1375–1381 (2007).
Bischoff, S.C. Role of mast cells in allergic and non-allergic immune responses: comparison of human and murine data. Nat. Rev. Immunol. 7, 93–104 (2007).
Kitamura, Y., Go, S. & Hatanaka, K. Decrease of mast cells in W/Wv mice and their increase by bone marrow transplantation. Blood 52, 447–452 (1978).
Lyon, M.F. & Glenister, P.H. A new allele sash (Wsh) at the W-locus and a spontaneous recessive lethal in mice. Genet. Res. 39, 315–322 (1982).
Nakano, T. et al. Fate of bone marrow-derived cultured mast cells after intracutaneous, intraperitoneal, and intravenous transfer into genetically mast cell-deficient W/Wv mice. Evidence that cultured mast cells can give rise to both connective tissue type and mucosal mast cells. J. Exp. Med. 162, 1025–1043 (1985).
Tsai, M. et al. In vivo immunological function of mast cells derived from embryonic stem cells: an approach for the rapid analysis of even embryonic lethal mutations in adult mice in vivo. Proc. Natl. Acad. Sci. USA 97, 9186–9190 (2000).
Grimbaldeston, M.A. et al. Mast cell-deficient W-sash c-kit mutant KitW-sh/W-sh mice as a model for investigating mast cell biology in vivo. Am. J. Pathol. 167, 835–848 (2005).
Wolters, P.J. et al. Tissue-selective mast cell reconstitution and differential lung gene expression in mast cell-deficient KitW-sh/KitW-sh sash mice. Clin. Exp. Allergy 35, 82–88 (2005).
Metz, M. et al. Mast cells can enhance resistance to snake and honeybee venoms. Science 313, 526–530 (2006).
Zhou, J.S., Xing, W., Friend, D.S., Austen, K.F. & Katz, H.R. Mast cell deficiency in KitW-sh mice does not impair antibody-mediated arthritis. J. Exp. Med. 204, 2797–2802 (2007).
Lee, D.M. et al. Mast cells: a cellular link between autoantibodies and inflammatory arthritis. Science 297, 1689–1692 (2002).
Scholten, J. et al. Mast cell-specific Cre/loxP-mediated recombination in vivo. Transgenic Res. 17, 307–315 (2008).
Musch, W., Wege, A.K., Mannel, D.N. & Hehlgans, T. Generation and characterization of α-chymase-Cre transgenic mice. Genesis 46, 163–166 (2008).
Echtenacher, B., Mannel, D.N. & Hultner, L. Critical protective role of mast cells in a model of acute septic peritonitis. Nature 381, 75–77 (1996).
Malaviya, R., Ikeda, T., Ross, E. & Abraham, S.N. Mast cell modulation of neutrophil influx and bacterial clearance at sites of infection through TNF-α. Nature 381, 77–80 (1996).
Maurer, M. et al. Mast cells promote homeostasis by limiting endothelin-1-induced toxicity. Nature 432, 512–516 (2004).
Schneider, L.A., Schlenner, S.M., Feyerabend, T.B., Wunderlin, M. & Rodewald, H.R. Molecular mechanism of mast cell mediated innate defense against endothelin and snake venom sarafotoxin. J. Exp. Med. 204, 2629–2639 (2007).
Piliponsky, A.M. et al. Neurotensin increases mortality and mast cells reduce neurotensin levels in a mouse model of sepsis. Nat. Med. 14, 392–398 (2008).
Orinska, Z. et al. IL-15 constrains mast cell-dependent antibacterial defenses by suppressing chymase activities. Nat. Med. 13, 927–934 (2007).
Thakurdas, S.M. et al. The mast cell-restricted tryptase mMCP-6 has a critical immunoprotective role in bacterial infections. J. Biol. Chem. 282, 20809–20815 (2007).
Knight, P.A., Wright, S.H., Lawrence, C.E., Paterson, Y.Y. & Miller, H.R. Delayed expulsion of the nematode Trichinella spiralis in mice lacking the mucosal mast cell-specific granule chymase, mouse mast cell protease-1. J. Exp. Med. 192, 1849–1856 (2000).
Shin, K. et al. Mouse mast cell tryptase mMCP-6 is a critical link between adaptive and innate immunity in the chronic phase of Trichinella spiralis infection. J. Immunol. 180, 4885–4891 (2008).
Rauter, I. et al. Mast cell-derived proteases control allergic inflammation through cleavage of IgE. J. Allergy Clin. Immunol. 121, 197–202 (2008).
Hart, P.H. et al. Dermal mast cells determine susceptibility to ultraviolet B-induced systemic suppression of contact hypersensitivity responses in mice. J. Exp. Med. 187, 2045–2053 (1998).
Byrne, S.N., Limon-Flores, A.Y. & Ullrich, S.E. Mast cell migration from the skin to the draining lymph nodes upon ultraviolet irradiation represents a key step in the induction of immune suppression. J. Immunol. 180, 4648–4655 (2008).
Depinay, N., Hacini, F., Beghdadi, W., Peronet, R. & Mecheri, S. Mast cell-dependent down-regulation of antigen-specific immune responses by mosquito bites. J. Immunol. 176, 4141–4146 (2006).
Lu, L.F. et al. Mast cells are essential intermediaries in regulatory T-cell tolerance. Nature 442, 997–1002 (2006).
Grimbaldeston, M.A., Nakae, S., Kalesnikoff, J., Tsai, M. & Galli, S.J. Mast cell-derived interleukin 10 limits skin pathology in contact dermatitis and chronic irradiation with ultraviolet B. Nat. Immunol. 8, 1095–1104 (2007).
Gregory, G.D., Raju, S.S., Winandy, S. & Brown, M.A. Mast cell IL-4 expression is regulated by Ikaros and influences encephalitogenic Th1 responses in EAE. J. Clin. Invest. 116, 1327–1336 (2006).
Chen, R. et al. Mast cells play a key role in neutrophil recruitment in experimental bullous pemphigoid. J. Clin. Invest. 108, 1151–1158 (2001).
Nakae, S., Suto, H., Berry, G.J. & Galli, S.J. Mast cell-derived TNF can promote Th17 cell-dependent neutrophil recruitment in ovalbumin-challenged OTII mice. Blood 109, 3640–3648 (2007).
Askenase, P.W. et al. Defective elicitation of delayed-type hypersensitivity in W/Wv and SI/SId mast cell-deficient mice. J. Immunol. 131, 2687–2694 (1983).
Galli, S.J. & Hammel, I. Unequivocal delayed hypersensitivity in mast cell-deficient and beige mice. Science 226, 710–713 (1984).
Norman, M.U. et al. Mast cells regulate the magnitude and the cytokine microenvironment of the contact hypersensitivity response. Am. J. Pathol. 172, 1638–1649 (2008).
Jawdat, D.M., Albert, E.J., Rowden, G., Haidl, I.D. & Marshall, J.S. IgE-mediated mast cell activation induces Langerhans cell migration in vivo. J. Immunol. 173, 5275–5282 (2004).
Suto, H. et al. Mast cell-associated TNF promotes dendritic cell migration. J. Immunol. 176, 4102–4112 (2006).
Bryce, P.J. et al. Immune sensitization in the skin is enhanced by antigen-independent effects of IgE. Immunity 20, 381–392 (2004).
Kambayashi, T. et al. Indirect involvement of allergen-captured mast cells in antigen presentation. Blood 111, 1489–1496 (2008).
McLachlan, J.B. et al. Mast cell activators: a new class of highly effective vaccine adjuvants. Nat. Med. 14, 489–490 (2008).
Bot, I. et al. Perivascular mast cells promote atherogenesis and induce plaque destabilization in apolipoprotein E-deficient mice. Circulation 115, 2516–2525 (2007).
Kovanen, P.T. Mast cells and degradation of pericellular and extracellular matrices: potential contributions to erosion, rupture and intraplaque haemorrhage of atherosclerotic plaques. Biochem. Soc. Trans. 35, 857–861 (2007).
Sun, J. et al. Mast cells promote atherosclerosis by releasing proinflammatory cytokines. Nat. Med. 13, 719–724 (2007).
Sun, J. et al. Mast cells modulate the pathogenesis of elastase-induced abdominal aortic aneurysms in mice. J. Clin. Invest. 117, 3359–3368 (2007).
Tsuruda, T. et al. Adventitial mast cells contribute to pathogenesis in the progression of abdominal aortic aneurysm. Circ. Res. 102, 1368–1377 (2008).
Coussens, L.M. & Werb, Z. Inflammation and cancer. Nature 420, 860–867 (2002).
Coussens, L.M. et al. Inflammatory mast cells up-regulate angiogenesis during squamous epithelial carcinogenesis. Genes Dev. 13, 1382–1397 (1999).
Soucek, L. et al. Mast cells are required for angiogenesis and macroscopic expansion of Myc-induced pancreatic islet tumors. Nat. Med. 13, 1211–1218 (2007).
Kopp, H.G., Ramos, C.A. & Rafii, S. Contribution of endothelial progenitors and proangiogenic hematopoietic cells to vascularization of tumor and ischemic tissue. Curr. Opin. Hematol. 13, 175–181 (2006).
Gounaris, E. et al. Mast cells are an essential hematopoietic component for polyp development. Proc. Natl. Acad. Sci. USA 104, 19977–19982 (2007).
Sinnamon, M.J. et al. A protective role of mast cells in intestinal tumorigenesis. Carcinogenesis 29, 880–886 (2008).
Wedemeyer, J. & Galli, S.J. Decreased susceptibility of mast cell-deficient KitW/KitW-v mice to the development of 1,2-dimethylhydrazine-induced intestinal tumors. Lab. Invest. 85, 388–396 (2005).
Nakae, S. et al. Mast cells enhance T cell activation: importance of mast cell costimulatory molecules and secreted TNF. J. Immunol. 176, 2238–2248 (2006).
Yamashita, Y. et al. Cutting edge: genetic variation influences FcɛRI-induced mast cell activation and allergic responses. J. Immunol. 179, 740–743 (2007).
Christy, A.L. & Brown, M.A. The multitasking mast cell: positive and negative roles in the progression of autoimmunity. J. Immunol. 179, 2673–2679 (2007).
Galli, S.J., Tsai, M. & Piliponsky, A.M. The development of allergic inflammation. Nature 454, 445–454 (2008).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Competing interests
S.J.G. occasionally consults for Amgen, Genentech, Novartis and other companies that are developing or producing agents to treat allergies, asthma and/or other disorders linked to mast cells. S.J.G. is also on the scientific advisory board of Tunitas Therapeutics, which plans to develop products that can be used to treat allergies and asthma.
Rights and permissions
About this article
Cite this article
Kalesnikoff, J., Galli, S. New developments in mast cell biology. Nat Immunol 9, 1215–1223 (2008). https://doi.org/10.1038/ni.f.216
Published:
Issue Date:
DOI: https://doi.org/10.1038/ni.f.216
This article is cited by
-
Single-cell analysis unveils activation of mast cells in colorectal cancer microenvironment
Cell & Bioscience (2023)
-
Drug Desensitization Update: Key Concepts and Mechanisms
Current Treatment Options in Allergy (2023)
-
Recent advances in GPR35 pharmacology; 5-HIAA serotonin metabolite becomes a ligand
Archives of Pharmacal Research (2023)
-
Arf1 facilitates mast cell proliferation via the mTORC1 pathway
Scientific Reports (2022)
-
A pharmacological approach assessing the role of mast cells in insulin infusion site inflammation
Drug Delivery and Translational Research (2022)