Abstract
Adiponectin is an adipocyte-derived hormone. Recent genome-wide scans have mapped a susceptibility locus for type 2 diabetes and metabolic syndrome to chromosome 3q27, where the gene encoding adiponectin is located. Here we show that decreased expression of adiponectin correlates with insulin resistance in mouse models of altered insulin sensitivity. Adiponectin decreases insulin resistance by decreasing triglyceride content in muscle and liver in obese mice. This effect results from increased expression of molecules involved in both fatty-acid combustion and energy dissipation in muscle. Moreover, insulin resistance in lipoatrophic mice was completely reversed by the combination of physiological doses of adiponectin and leptin, but only partially by either adiponectin or leptin alone. We conclude that decreased adiponectin is implicated in the development of insulin resistance in mouse models of both obesity and lipoatrophy. These data also indicate that the replenishment of adiponectin might provide a novel treatment modality for insulin resistance and type 2 diabetes.
Similar content being viewed by others
Main
Insulin resistance induced by high-fat diet and associated with obesity is a major risk factor for diabetes and cardiovascular diseases. Adipose tissue is not simply a store of excess energy, but also secretes a variety of proteins into circulating blood that influence systemic metabolism. These include leptin1, tumor necrosis factor (TNF)-α (ref. 2), plasminogen-activator inhibitor type 1 (PAI-1)3, adipsin4 and resistin5; these are collectively known as adipocytokines6.
One of adipocytokines, adiponectin7,8,9,10, was originally identified independently by four groups using different approaches. Adiponectin cDNA was isolated by large-scale random sequencing of a 3′-directed, human-adipose–tissue cDNA library7. Mouse cDNAs for adiponectin termed Acrp30 (ref. 8) and AdipoQ (ref. 9) were cloned by differential display before and after differentiation of mouse 3T3-L1 and 3T3-F442A cells, respectively. Human adiponectin was also purified from plasma as gelatin-binding protein-28 (ref. 10). The mRNA expression of adiponectin and its plasma level are significantly reduced in obese/diabetic mice and humans9,11. Lodish and colleagues12 have recently reported that a proteolytic cleavage product of Acrp30 increases fatty-acid oxidation in muscle and causes weight loss in mice. Froguel and colleagues13 have mapped a diabetes-susceptibility locus to human chromosome 3q27, where the adiponectin gene is located, in a native French cohort, and Comuzzie and colleagues14 have demonstrated a quantitative-trait locus on 3q27 strongly linked to the metabolic syndrome in individuals of European descent14.
Here we show that the decreased expression levels of adiponectin coinicide with insulin resistance in murine models of altered insulin sensitivity. We also show that physiological doses of adiponectin improve insulin resistance in mouse models of obesity and type 2 diabetes. Moreover, in peroxisome proliferator-activated receptor-γ (PPAR-γ)+/− mice15,16 treated with an inhibitor of PPAR-γ/retinoid-X receptor (RXR)17, which lack adipose tissue, insulin resistance was completely reversed by a combination of physiological doses of adiponectin and leptin, but only partially by either adiponectin or leptin alone We conclude that adiponectin is decreased in obesity and deficient in mice without adipose tissues, which play a casual role in the development of insulin resistance in these models. These data also suggest that replenishment of adiponectin may provide a novel treatment modality for insulin resistance and type 2 diabetes.
Adiponectin expression correlates with insulin sensitivity
Because adiponectin is reported to be decreased in obesity9,11, we investigated the role of altered adiponectin expression in obesity and insulin resistance. To this end, we used the PPAR-γ agonist rosiglitazone, which stimulates adipogenesis and at the same time reduces insulin resistance18,19. A high-fat diet reduced the mRNA levels in white adipose tissue (WAT) (Fig. 1a) and serum levels of adiponectin (Fig. 1b) in mice with hyperglycemia (Fig. 1c) and hyperinsulinemia (Fig. 1d). Rosiglitazone significantly increased the mRNA levels in WAT (Fig. 1a) and serum levels of adiponectin (Fig. 1b) in mice on high-fat diet, and at the same time ameliorated hyperglycemia (Fig. 1c) and hyperinsulinemia (Fig. 1d). There was, however, a slight increase in adipose tissue mass (vehicle-treated: 2.72 ± 0.11 g; Rosi-treated: 2.84 ± 0.16 g) and body weight (vehicle-treated: 46.5 ± 0.70 g; Rosi-treated: 47.9 ± 1.0 g) in db/db mice. We obtained similar results with wild-type controls (C57) (Web Supplement, Table A). In differentiated 3T3L1 adipocytes in vitro, rosiglitazone also increased adiponectin expression (Fig. 1e). These data raise the possibility that the expression of adiponectin mRNA might be partially regulated by a PPAR-γ–dependent pathway, and more closely related to insulin sensitivity than obesity.
a and b, Amounts of the mRNA in WAT (a) or serum levels of adiponectin (b) of db/db mice on the high-carbohydrate (HC), or high-fat diet untreated (HF) or treated with rosiglitazone (HF+Rosi). c and d, Values of area under the glucose curve (c) and area under the insulin curve (d) during glucose tolerance test in db/db mice subjected to indicated treatments. Results are expressed as the percentage of the value of untreated mice on the HC diet. The basal glucose levels (time = 0 of the glucose tolerance test) of untreated db/db mice on the HC diet were 244.8 ± 23.3 mg/dl (c). Each bar represents the mean ± s.e. (n = 5–10). *, P < 0.05; **, P < 0.01; compared with untreated mice on the HF diet. e, Amounts of adiponectin mRNA in 3T3L1 adipocytes untreated (−) or treated with 1 μM rosiglitazone (Rosi) for 24 hours.
Adiponectin is depleted in mice without adipose tissue
To clarify the causal relationship between adiponectin expression and insulin sensitivity, we attempted to deplete adipose tissue and hence adiponectin. We developed a mouse model without adipose tissue by severely reducing PPAR-γ/RXR activity (Fig. 2). Treatment of PPAR-γ+/− mice with a PPAR-γ/RXR inhibitor such as the RXR antagonist HX531 (ref. 17) for three weeks markedly decreased expression of PPAR-γ/RXR-responsive genes such as lipoprotein lipase (LPL)20 in WAT (∼90% or further; Fig. 2a), indicating that PPAR-γ/RXR activity was likely to be severely decreased. Four weeks of this treatment resulted in disappearance of visible WAT (Fig. 2b and c). This loss presumably results from decreased expression of molecules involved in triglyceride accumulation in WAT, the expression of which is dependent on PPAR-γ/RXR activity.
PPAR-γ+/− mice were untreated (−) or treated with HX531 (+) for 6 wk or PPAR-γ+/− mice were treated with recombinant full-length adiponectin (Ad), gAd or leptin (Lep) at the doses indicated (μg/day). Unless indicated, treatment as continuous systemic infusion (pump) in combination for the last 12 days of the 6-wk HX531 treatment while on the high-fat (HF) diet. a, Amounts of LPL mRNA in WAT. b, Epididymal WAT weight. c, Exposed ventral view of the mice illustrating ablation of WAT. d, Serum adiponectin levels were determined by immunoblotting with anti-adiponectin antibody10 with recombinant adiponectin as standards. Lane 9 shows the serum adiponectin level when mice were treated with 50 μg Ad as an intraperitoneal (ip) injection. e, Insulin resistance indices. The results are expressed as the percentage of the value of untreated PPAR-γ+/− mice on the high-fat diet. The basal glucose level (time = 0 of the glucose tolerance test) of untreated PPAR-γ+/− mice on the high-fat diet was 110.7 ± 12.8 mg/dl. Each bar represents the mean ± s.e. (n = 5–10). *, P < 0.05; **, P < 0.01; compared with untreated PPAR-γ+/− mice or treated with HX531 alone for 6 wk or treated with both leptin and adiponectin.
As expected, adiponectin was completely absent in sera from the lipoatrophic mice, whereas adiponectin was detected as a 35-kD protein with an antibody against adiponectin in sera from control mice (Fig. 2d, lanes 6&7). The lipoatrophic mice showed increased free-fatty acid (FFA) in serum, increased triglyceride levels, increased tissue triglyceride content in skeletal muscle and liver (Table 1) as well as hyperinsulinemia and hyperglycemia (Fig. 2e); these observations are consistent with the phenotypes reported for lipoatrophic diabetes21,22,23.
Adiponectin reverses insulin resistance of lipoatrophic mice
To determine the role of adiponectin deficiency in the development of insulin resistance in lipoatrophic mice, we administered adiponectin to these mice. Continuous systemic infusion of a physiological dose of recombinant adiponectin (Fig. 2d, lanes 6–8) significantly ameliorated hyperglycemia and hyperinsulinemia (Fig. 2e).
Globular domain of adiponectin exerts more potent effects
Adiponectin is composed of an N-terminal collagen-like sequence (cAd) and a C-terminal globular region (gAd)24,25. We next analyzed which domain mediates these biological effects. gAd ameliorated hyperglycemia and hyper-insulinemia much more potently than full-length adiponectin (Fig. 2e). Interestingly, a 25-kD protein recognized by an antibody against C-terminal portion of adiponectin was present in the serum, albeit in a very small amount (data not shown), suggesting that full-length adiponectin might undergo proteolytic processing. These data corroborate a recent finding that a small amount of gAd was indeed present in plasma and the C-terminal globular region of Acrp30 increased fatty-acid oxidation more potently than the full-length form12.
Adiponectin/leptin deficiency explains insulin resistance
Insulin resistance in lipoatrophic diabetes might be due to deficiency of adipocytokines which sensitize tissues to insulin. The results above indicate that adiponectin is one of such adipocytokines. It should also be noted that the physiological dose of adiponectin was not sufficient to completely ameliorate insulin resistance in mice without adipose tissue. Leptin has also been shown to be such an adipocytokine21. Serum leptin levels were undetectable in these mice (upper limit: 0.2 ng/ml). Treatment of these mice with physiological doses of leptin did indeed alleviate their insulin resistance, albeit partially (Fig. 2e). Interestingly, combining physiological doses of adiponectin and leptin almost completely abolished the insulin resistance in an additive fashion (Fig. 2e).
Adiponectin leads to decreased tissue triglyceride content
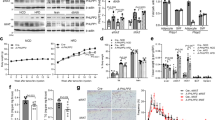
To determine the mechanisms by which adiponectin exerts its anti-diabetic effects, we examined its effects in individual organs. In skeletal muscle, low doses of gAd increased expression of molecules involved in fatty-acid transport, combustion and energy dissipation such as CD36 (refs. 26,27), acyl-CoA oxidase (ACO)28,29 and uncoupling protein (UCP)2 (refs. 30,31), respectively (Fig. 3a). In turn, these processes lead to decreased tissue triglyceride content in skeletal muscle (Table 1). Possible mechanism(s) underlying these alterations in gene expression might include increased expression of PPAR-α/γ and/or increased endogenous ligands, given that these genes possess the peroxisome proliferator-response element in their promoter regions18,19,26,27,28,29,30,31. Indeed, expression of PPAR-α (refs. 18,28,29) was increased (Fig. 3a). In contrast to skeletal muscle, in the liver, low doses of gAd decreased the expression of molecules involved in fatty-acid transport into tissues such as CD36 (Fig. 3b), thereby reducing fatty-acid influx into the liver, which might lead to decreased hepatic triglyceride content (Table 1). Thus, even though triglyceride content was decreased in both muscle and liver, the mechanisms involved are apparently quite different in the two tissues. These data indicate that adiponectin acts primarily on skeletal muscle to increase influx and combustion of FFA, thereby reducing muscle triglyceride content. As a consequence of decreased serum FFA and triglyceride levels (Table 1), hepatic triglyceride content is decreased.
a and b, mRNAs of fatty-acid translocase (FAT)/CD36, ACO, UCP2 and PPAR-α in mouse skeletal muscle (a) and liver (b). c, Insulin-induced tyrosine phosphorylation of insulin receptor (IR) and insulin receptor substrate (IRS)-1, and insulin-stimulated phosphorylation of Akt in skeletal muscle. HX531 was given as a 0.1% food admixture. Mice were stimulated with or without 1 U/g body weight of insulin for 2 min. Lysates were immunoprecipitated (IP), followed by immunoblotting, with the antibodies indicated36.
Decreased triglyceride content improves insulin signaling
Increased tissue triglyceride content has been reported to interfere with insulin-stimulated activation of phosphatidylinositol-3–kinase and subsequent translocation of glucose-transporter protein 4 and uptake of glucose, which leads to insulin resistance32. Thus, decreased triglyceride content in muscle might contribute to the improved insulin signal transduction, as demonstrated by increases in insulin-induced tyrosine phosphorylation of insulin receptor and insulin-receptor substrate 1, as well as increases in insulin-stimulated phosphorylation of Akt kinase in skeletal muscle of adiponectin-treated lipoatrophic mice (Fig. 3c).
Adiponectin reverses insulin resistance of obese mice
We next studied whether adiponectin can improve insulin resistance and diabetes in db/db and KKAy mice (KK mice overexpressing agouti), two different mouse models of type 2 diabetes characterized by obesity, hyperlipidemia, insulin resistance and hyperglycemia1,33. Serum adiponectin levels were decreased in wild-type mice on a high-fat diet (Fig. 4a, lane 3) compared with those in mice on a high-carbohydrate diet (Fig. 4a, lane 1). Serum adiponectin levels in db/db mice (Fig. 4a, lanes 5&7) were also decreased compared with wild-type controls on either high-carbohydrate or high-fat diet (Fig. 4a, lanes 1&3). Lower serum adiponectin levels in wild-type mice on the high-fat diet were partially restored to those of wild-type controls on the high-carbohydrate diet by continuous systemic infusion of low doses of recombinant adiponectin (Fig. 4a, lanes 1,3,4), which significantly ameliorated hyperglycemia induced by high-fat diet (Fig. 4b, lanes 1,3,4) and hyperinsulinemia (Fig. 4c, lanes 1,3,4). Lower serum adiponectin levels in db/db mice on either high-carbohydrate or high-fat diet were also partially restored to those in respective wild-type controls by the adiponectin replenishment (Fig. 4a), which also significantly ameliorated leptin receptor deficiency-induced hyperglycemia (Fig. 4b) and hyperinsulinemia (Fig. 4c). We obtained similar results when using KKAy mice and their wild-type controls (Fig. 4d–f). These data indicate that high-fat feeding, leptin-receptor deficiency or agouti overexpression causes insulin resistance, partially through decreases in adiponectin, and that adiponectin has potential as an anti-diabetic drug.
a–f, Serum levels of adiponectin (a and d), the values of area under the glucose curve (b and e) and area under the insulin curve (c and f) during glucose tolerance test (GTT) of C57 or db/db mice (a–c) or of KK or KKAy mice (d–f). Mice were on HC or HF diet untreated or Ad- or gAd-treated at indicated doses (μg/day). Serum adiponectin levels were determined by immunoblotting with anti-adiponectin antibody10 with recombinant adiponectin as standards (a and d). The results are expressed as the percentage of the value of untreated wild-type mice on the HC diet (b, c, e, f). The basal glucose level (time = 0 of the GTT) of untreated C57 mice on the HC diet was 62.3 ± 3.1 mg/dl (b) and that of KK mice was 93.0 ± 6.1 mg/dl (e). Each bar represents the mean ± s.e. (n = 5–10). *, P < 0.05; **, P < 0.01; C57 versus db/db, or KK versus KKAy, HC versus HF, or compared with untreated mice.
Adiponectin increases β-oxidation
In skeletal muscle, adiponectin-treated KKAy mice showed increased expression of enzymes involved in β-oxidation and UCP2 (Web Supplement, Table B). In mice treated with adiponectin, ACO activities and fatty-acid combustion were increased in skeletal muscle but not liver (Table 2). These alterations decreased tissue triglyceride content, associated with decreased serum FFA and triglyceride levels (Table 2). In turn, these reductions in serum FFA and triglyceride levels seemed to cause decreased expression of molecules involved in fatty-acid transport into hepatic tissues (Web Supplement, Table B), thereby also reducing tissue triglyceride content in liver (Table 2).
In contrast, treatment of normal C57 mice with adiponectin for two weeks slightly, but not significantly, reduced the increases in WAT mass (untreated mice: 0.53 ± 0.03 g; gAd-treated: 0.48 ± 0.04 g) and body weight associated with the high-fat diet as compared with vehicle (vehicle-treated: 22.8 ± 2.0 g; gAd-treated: 20.6 ± 2.1 g). Food intake tended to be higher in adiponectin-treated mice versus control on the high-fat diet (vehicle-treated: 5.71 ± 0.56 g/day; gAd-treated: 6.28 ± 0.51 g/day), and the rectal temperature was significantly higher in mice treated with adiponectin (Table 2), consistent with increased expression of molecules involved in fatty-acid combustion and energy dissipation in muscle and brown adipose tissue (Web Supplement, Table B). In this regard, leptin might have a role in the increased energy expenditure and improvement of insulin resistance in adiponectin-treated mice. However, the anti-diabetic effects of adiponectin were not attenuated in db/db mice, which lack leptin receptors1 (Fig. 4a–c). Moreover, treatment of wild-type mice with adiponectin did not alter the expression of leptin in WAT and serum leptin levels (vehicle-treated: 11.1 ± 2.1 ng/ml; gAd-treated: 10.4 ± 2.6 ng/ml). We obtained essentially similar results of serum leptin levels by using KK (vehicle-treated: 15.1 ± 2.5 ng/ml; gAd-treated: 13.4 ± 2.7 ng/ml), KKAy (vehicle-treated: 61.5 ± 5.4 ng/ml; gAd-treated: 57.9 ± 5.7 ng/ml), and db/db mice (vehicle-treated: 153.9 ± 20.4 ng/ml; gAd-treated: 145.2 ± 14.7 ng/ml). These findings indicate that adiponectin exerted its anti-diabetic effects through leptin-independent pathways.
Discussion
Here we show that replenishment of the fat-derived hormone adiponectin can reverse insulin resistance not only in lipoatrophic diabetic mice but also in murine models of obesity and type 2 diabetes. Our data support a mechanism of increased expression of molecules involved in fatty-acid combustion and energy dissipation in skeletal muscle, leading to decreased tissue triglyceride content in muscle and liver, independent of leptin signaling. Our data also indicate that adiponectin is decreased in both obesity and lipoatrophy; this decrease has a causal role in development of insulin resistance, possibly pointing to a common molecular mechanism of insulin resistance in the two opposite adiposity states. Although adiponectin slightly but not significantly reduced weight gain induced by high-fat diet during our study period, treatment with adiponectin for a longer duration might allow its anti-obesity effects to be exerted12.
In lipoatrophic diabetes, lack of fat is associated with insulin resistance and diabetes. This is in striking contrast to the usual association of diabetes with obesity. Previous studies have shown that transplantation of adipose tissue into lipoatrophic mice corrects diabetes22 and leptin treatment reverses the diabetes in a murine model of lipoatrophic diabetes21. We now show that the insulin resistance observed in lipoatrophic mice due to severely reduced PPAR-γ/RXR activity is completely ameliorated by complementation of physiological doses of adiponectin and leptin, but only partially by either adiponectin or leptin alone. Our results support the idea that combined adiponectin and leptin deficiency can account for insulin resistance in lipoatrophic diabetes in mice and possibly in humans.
Type 2 diabetes results from an interaction between genetic and environmental factors34. In this context, we have found that genetic variation resulting in reduced serum adiponectin levels is associated with increased risk for type 2 diabetes in the Japanese population (Hara et al., manuscript submitted). We also showed here that obesity induced by high-fat diet leads to reduced expression and serum levels of adiponectin, thereby causing insulin resistance. Replenishment of adiponectin, in patients with type 2 diabetes associated with decreased adiponectin levels due to either genetic or environmental factors, might represent a novel treatment strategy for insulin resistance and type 2 diabetes. In this respect, we speculate that adiponectin has several therapeutic advantages over anti-diabetic drugs now used clinically. First, in addition to hypolipidemic and anti-diabetic effects, adiponectin might prevent atherogenesis as an anti-inflammatory factor35. Second, adiponectin exerts anti-diabetic effects without increasing body weight. Third, in contrast to the usual association of obesity with insulin and leptin resistance, we observed no adiponectin resistance in the models of obesity and type 2 diabetes studied here.
Methods
Chemicals.
Rosiglitazone, a PPAR-γ agonist, and HX531, a PPAR-γ/RXR inhibitor, were synthesized as described17,28. All other materials were from sources already decribed10,15,28.
Animals.
PPAR-γ+/− mice have been described15. All other animals were purchased from Nippon CREA (Shizuoka, Japan). 6-wk-old mice were fed powdered chow as described15. Drugs were given as food admixtures15.
RNA preparation, northern-blot analysis and immunoblotting.
Total RNA was prepared from tissues with TRIzol (GIBCO-BRL, Grand Island, New York) according to the manufacturer's instructions. Total RNA from 5–10 mice in each group was pooled, and aliquots were subjected to northern-blot analysis26,28 with the probes for rat ACO (from T. Hashimoto), mouse CD36, UCP2, PPAR-α (from K. Motojima) or mouse adiponectin cDNA. The radioactivity in each band was quantified, and the fold change in each mRNA was calculated after correction for loading differences by measuring the amount of 28S rRNA. Serum adiponectin levels were determined by immunoblotting with the polyclonal antibody against gelatin-binding protein-28 (raised against the peptide of CYADNDNDSTFTGFLLYHDTN, which corresponded to the C-terminal 20 aa of human adiponectin with one extra cysteine at its N terminus)10 with recombinant adiponectin as standards. The procedures used for immunoprecipitation, and immunoblotting have been described36. Representative data from 1 of 3 independent experiments are shown.
Blood sample assays.
Plasma glucose, serum FFA and triglyceride levels were determined by glucose B-test, nonesterified fatty acid (NEFA) C-test and triglyceride L-type (Wako, Osaka, Japan), respectively. Plasma insulin was measured by insulin immunoassay (Morinaga Institute of Biological Science, Yokohama, Japan)28. Leptin was assayed with the ELISA-based Quantikine M mouse leptin immunoassay kit (R&D Systems, Minneapolis, Minnesota) according to the manufacturer's instructions.
Generation of 6xHis–adiponectin fusion proteins.
Each full-length mouse adiponectin, cAd or gAd was introduced into the pQE-30 bacterial expression vector (Qiagen, Hilden, Germany). The expression of histidine-tagged adiponectin, cAd and gAd in JM-109 was induced by the addition of isopropyl β-thiogalactopyranoside to growth medium. Bacterial extracts were prepared using standard methods, and the fusion proteins were purified by elution through a nickel-ion agarose column28. ActiClean Etox affinity columns (Sterogene Bioseparations, Carlsbad, California) were used to remove potential endotoxin contaminations.
Adiponectin or leptin treatment.
Mice were treated with adiponectin or leptin as an intraperitoneal injection or continuous systemic infusion as described21. An Alzet micro-osmotic pump (model 1002, Alza, Palo Alto, California) was inserted subcutaneously in the back of each mouse. The pumps delivered the doses indicated in figures and tables of mouse recombinant leptin (Sigma) or adiponectin per day for 12 days in a total volume of 0.1 ml of PBS.
Insulin-resistance index.
The areas of glucose and insulin curves were calculated by multiplying the cumulative mean height of the glucose values (1 mg/ml = 1 cm) and insulin values (1 ng/ml = 1 cm), respectively, by time (60 min = 1 cm)37. The insulin resistance index was calculated from the product of the areas of glucose and insulin × 10−2 in glucose tolerance test15 The results are expressed as the percentage of the value of each control.
Lipid metabolism and enzymatic activity of ACO.
The measurements of [14C]CO2 production from [1-14C]palmitic acid were performed using liver and muscle slices as described28. Liver and muscle homogenates were extracted , and tissue triglyceride content was determined as described28 with an extract solution (CHCl3:CH3OH = 2:1). The remainder of the liver and muscle was immediately frozen in liquid nitrogen and stored at −80 °C until measurements of the enzymatic activity of ACO were performed. ACO activity in the light mitochondrial fraction of liver and muscle was measured by assay that was based on the H2O2-dependent oxidation of leuco-dichlorofluorescein28.
Note: Supplementary information is available on the Nature Medicine website (http://www.nature.com/nm/supplementary_info/).
References
Friedman, J.M. Obesity in the new millennium. Nature 404, 632–634 (2000).
Hotamisligil, G.S. The role of TNFα and TNF receptors in obesity and insulin resistance. J. Intern. Med. 245, 621–625 (1999).
Shimomura, I. et al. Enhanced expression of PAI-1 in visceral fat: Possible contributor to vascular disease in obesity. Nature Med. 2, 800–803 (1996).
White, R.T. et al. Human adipsin is identical to complement factor D and is expressed at high levels in adipose tissue. J. Biol. Chem. 267, 9210–9213 (1992).
Steppan, C.M. et al. The hormone resistin links obesity to diabetes. Nature 409, 307–312 (2001).
Matsuzawa, Y., Funahashi, T. & Nakamura, T. Molecular mechanism of metabolic syndrome X: Contribution of adipocytokines adipocyte-derived bioactive substances. Ann. NY Acad. Sci. 892, 146–154 (1999).
Maeda, K. et al. cDNA cloning and expression of a novel adipose specific collagen-like factor, apM1 (AdiPose Most abundant Gene transcript 1). Biochem. Biophys. Res. Commun. 221, 286–296 (1996).
Scherer, P.E., Williams, S., Fogliano, M., Baldini, G. & Lodish, H.F. A novel serum protein similar to C1q, produced exclusively in adipocytes. J. Biol. Chem. 270, 26746–26749 (1995).
Hu, E., Liang, P. & Spiegelman, B.M. AdipoQ is a novel adipose-specific gene dysregulated in obesity. J. Biol. Chem. 271, 10697–10703 (1996).
Nakano, Y., Tobe, T., Choi-Miura, N.H., Mazda, T. & Tomita M. Isolation and characterization of GBP28, a novel gelatin-binding protein purified from human plasma. J. Biochem. (Tokyo) 120, 802–812 (1996).
Arita, Y. et al. Paradoxical decrease of an adipose-specific protein, adiponectin, in obesity. Biochem. Biophys. Res. Commun. 257, 79–83 (1999).
Fruebis, J. et al. Proteolytic cleavage product of 30-kDa adipocyte complement-related protein increases fatty acid oxidation in muscle and causes weight loss in mice. Proc. Natl. Acad. Sci. USA 98, 2005–2010 (2001).
Vionnet, N. et al. Genomewide search for type 2 diabetes-susceptibility genes in French whites: Evidence for a novel susceptibility locus for early-onset diabetes on chromosome 3q27-qter and independent replication of a type 2-diabetes locus on chromosome 1q21-q24. Am. J. Hum. Genet. 67, 1470–1480 (2000).
Kissebah, A.H. et al. Quantitative trait loci on chromosomes 3 and 17 influence phenotypes of the metabolic syndrome. Proc. Natl. Acad. Sci. USA 97, 14478–14483 (2000).
Kubota, N. et al. PPAR-γ mediates high-fat diet-induced adipocyte hypertrophy and insulin resistance. Mol. Cell 4, 597–609 (1999).
Miles, P.D., Barak, Y., He, W., Evans, R.M. & Olefsky, J.M. Improved insulin-sensitivity in mice heterozygous for PPAR-gamma deficiency. J. Clin. Invest. 105, 287–292 (2000).
Ebisawa, M. et al. Retinoid X receptor-antagonistic diazepinylbenzoic acids. Chem. Pharm. Bull. (Tokyo) 47, 1778–1786 (1999).
Kersten, S., Desvergne, B. & Wahli, W. Roles of PPARs in health and disease. Nature 405, 421–424 (2000).
Spiegelman, B.M. & Flier, J.S. Adipogenesis and obesity: Rounding out the big picture. Cell 87, 377–389 (1996).
Schoonjans, K. et al. PPARα and PPARγ activators direct a distinct tissue-specific transcriptional response via a PPRE in the lipoprotein lipase gene. EMBO J. 15, 5336–5348 (1996).
Shimomura, I., Hammer, R.E., Ikemoto, S., Brown, M.S. & Goldstein, J.L. Leptin reverses insulin resistance and diabetes mellitus in mice with congenital lipodystrophy. Nature 401, 73–76 (1999).
Gavrilova, O. et al. Surgical implantation of adipose tissue reverses diabetes in lipoatrophic mice. J. Clin. Invest. 105, 271–278 (2000).
Seip, M. & Trygstad, O. Generalized lipodystrophy, congenital and acquired (lipoatrophy). Acta Paediatr. Suppl. 413, 2–28 (1996).
Eggleton, P., Reid, K.B. & Tenner, A.J. C1q—how many functions? How many receptors? Trends Cell. Biol. 8, 428–431 (1998).
Shapiro, L. & Scherer, P.E. The crystal structure of a complement-1q family protein suggests an evolutionary link to tumor necrosis factor. Curr. Biol. 8, 335–338 (1998).
Motojima, K., Passilly, P., Peters, J.M., Gonzalez, F.J. & Latruffe, N. Expression of putative fatty acid transporter genes are regulated by peroxisome proliferator-activated receptor α and γ activators in a tissue- and inducer-specific manner. J. Biol. Chem. 273, 16710–16714 (1998).
Tontonoz, P., Nagy, L., Alvarez, J.G., Thomazy, V.A. & Evans, R.M. PPARγ promotes monocyte/macrophage differentiation and uptake of oxidized LDL. Cell 93, 241–252 (1998).
Murakami, K. et al. A novel insulin sensitizer acts as a coligand for peroxisome proliferator-activated receptor-α (PPAR-α) and PPAR-γ: Effect of PPAR-α activation on abnormal lipid metabolism in liver of Zucker fatty rats. Diabetes 47, 1841–1847 (1998).
Kersten, S. et al. Peroxisome proliferator-activated receptor α mediates the adaptive response to fasting. J. Clin. Invest. 103, 1489–1498 (1999).
Lowell, B.B. & Spiegelman, B.M. Towards a molecular understanding of adaptive thermogenesis. Nature 404, 652–660 (2000).
Kelly, L.J. et al. Peroxisome proliferator-activated receptors γ and α mediate in vivo regulation of uncoupling protein (UCP-1, UCP-2, UCP-3) gene expression. Endocrinology 139, 4920–4927 (1998).
Shulman, G.I. Cellular mechanisms of insulin resistance. J. Clin. Invest. 106, 171–176 (2000).
Masuzaki, H. et al. Glucose metabolism and insulin sensitivity in transgenic mice overexpressing leptin with lethal yellow agouti mutation: Usefulness of leptin for the treatment of obesity-associated diabetes. Diabetes 48, 1615–1622 (1999).
Kahn, C.R., Vicent, D. & Doria, A. Genetics of non-insulin-dependent (type-II) diabetes mellitus. Annu. Rev. Med. 47, 509–31 (1996).
Ouchi, N. et al. Adiponectin, an adipocyte-derived plasma protein, inhibits endothelial NF-κB signaling through a cAMP-dependent pathway. Circulation 102, 1296–301 (2000).
Yamauchi, T. et al. Insulin signalling and insulin actions in the muscles and livers of insulin-resistant, insulin receptor substrate 1-deficient mice. Mol. Cell. Biol. 16, 3074–3084 (1996).
Mondon, C.E., Dolkas, C.B. & Oyama, J. Enhanced skeletal muscle insulin sensitivity in year-old rats adapted to hypergravity. Am. J. Physiol. 240, E482–488 (1981).
Acknowledgements
We thank I. Shimomura for helpful suggestions; T. Hashimoto for the generous gift of a DNA probe for ACO; K. Motojima for kindly providing CD36, UCP2 and PPAR-α cDNA probes; and S. Uchida, K. Kirii, S. Sakata and T. Nagano for technical assistance. This work was supported by a grant from the Research Fellowships of the Japan Society for the Promotion of Science for Young Scientists (to T.Y.); a Grant-in-Aid for the Development of Innovative Technology from the Ministry of Education, Culture, Sports, Science and Technology (to T.K.); and a Grant-in-Aid for Creative Scientific Research 10NP0201 from Japan Society for the Promotion of Science (to T.K.); and by Health Science Research Grants (Research on Human Genome and Gene Therapy) from the Ministry of Health and Welfare (to T.K.).
Author information
Authors and Affiliations
Corresponding author
Supplementary information
Rights and permissions
About this article
Cite this article
Yamauchi, T., Kamon, J., Waki, H. et al. The fat-derived hormone adiponectin reverses insulin resistance associated with both lipoatrophy and obesity. Nat Med 7, 941–946 (2001). https://doi.org/10.1038/90984
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1038/90984
This article is cited by
-
Adiponectin attenuates H2O2-induced apoptosis in chicken skeletal myoblasts through the lysosomal-mitochondrial axis
In Vitro Cellular & Developmental Biology - Animal (2024)
-
Familial partial lipodystrophy type 2 and obesity, two adipose tissue pathologies with different inflammatory profiles
Diabetology & Metabolic Syndrome (2023)
-
Experimental periodontitis induced hypoadiponectinemia by IRE1α-mediated endoplasmic reticulum stress in adipocytes
BMC Oral Health (2023)
-
Relevance and consequence of chronic inflammation for obesity development
Molecular and Cellular Pediatrics (2023)
-
Novel targets for potential therapeutic use in Diabetes mellitus
Diabetology & Metabolic Syndrome (2023)