Abstract
Cell-free human T-lymphotropic virus type 1 (HTLV-1) virions are poorly infectious in vitro for their primary target cells, CD4+ T cells. Here, we show that HTLV-1 can efficiently infect myeloid and plasmacytoid dendritic cells (DCs). Moreover, DCs exposed to HTLV-1, both before and after being productively infected, can rapidly, efficiently and reproducibly transfer virus to autologous primary CD4+ T cells. This DC-mediated transfer of HTLV-1 involves heparan sulfate proteoglycans and neuropilin-1 and results in long-term productive infection and interleukin-2–independent transformation of the CD4+ T cells. These studies, along with observations of HTLV-1–infected DCs in the peripheral blood of infected individuals, indicate that DCs have a central role in HTLV-1 transmission, dissemination and persistence in vivo. In addition to altering the current paradigm concerning how HTLV-1 transmission occurs, these studies suggest that impairment of DC function after HTLV-1 infection plays a part in pathogenesis.
Similar content being viewed by others
Main
HTLV-1 (ref. 1) is the causal agent of adult T cell leukemia (ATL) and HTLV-1–associated myelopathy and tropical spastic paraparesis (HAM/TSP) and is associated with other inflammatory disorders and immunosuppression. Unlike most retroviruses, cell-free virions of HTLV-1 and other deltaretroviruses are very poorly infectious in vitro2. Cell-free HTLV-1 does not stably infect its primary target cells, CD4+ T cells, in vitro, although transient infection has been reported3. Cell-free virions are also thought to be poorly infectious in vivo, as post-transfusion infection studies indicate that HTLV-1 transmission requires cell passage4. Although infected and uninfected lymphocytes can form a virological synapse that transfers HTLV-1 to the uninfected cells5, it is not clear whether this reflects a major pathway of productive cell-mediated transmission of HTLV-1 (ref. 6). Factors that contribute to HTLV-1 dissemination, persistence and pathogenesis remain poorly understood2,6.
DCs are potent antigen-presenting cells that are central in immune responses against viral infections. DCs are located at the sites of viral entry: mucosal membranes and peripheral blood. Although the functional characteristics of the two blood DC subsets, myeloid DCs (myDCs) and plasmacytoid DCs (pDCs), are distinct, both subsets are capable of taking up antigen, migrating to lymphoid organs and presenting antigen to T cells7. In addition to their role in adaptive immunity, pDCs are potent mediators of innate immune responses.
Many viruses infect DCs to facilitate their transmission, including the retroviruses HIV-1 and mouse mammary tumor virus8,9,10. Some viruses do this directly, hijacking the trafficking properties of DCs to facilitate their transport from the periphery to lymph nodes, where they infect target cells. Viral infection of DCs can also indirectly facilitate spread by impairing the ability of DCs to mount an appropriate immune response9.
We investigated the role of DCs in the transmission of HTLV-1 and discovered that, in contrast to all other primary cells examined to date, freshly isolated myDCs and pDCs are efficiently and productively infected by cell-free HTLV-1. Infected DCs rapidly and reproducibly transfer HTLV-1 to autologous primary CD4+ T cells, resulting in chronic productive infection of CD4+ T cells and generation of interleukin-2 (IL-2)-independent transformed cells.
Results
Primary dendritic cells are productively infected by HTLV-1
To investigate the role of DCs in HTLV-1 transmission, we isolated immature myDCs and pDCs from human peripheral blood and cultured them ex vivo. Owing to the low abundance of DCs in vivo10,11, we also generated monocyte-derived dendritic cells (MDDCs) from isolated monocytes. Both myDCs and pDCs bound cell-free HTLV-1 (Fig. 1a and Supplementary Fig. 1 online). HTLV-1 virions were efficiently internalized by myDCs and pDCs, as judged by intracellular staining for the viral proteins MA and SU (Fig. 1b). MDDCs also internalized cell-free HTLV-1 (Fig. 1b), consistent with earlier reports that these in vitro generated cells can bind12, internalize13 and be transiently infected by14 HTLV-1.
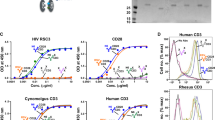
(a) Binding of HTLV-1 virions (10 μg/ml) to freshly isolated immature myDCs and pDCs, as analyzed by flow cytometry using antibodies specific for the HTLV envelope protein SU. In all figures, the gray line represents the isotype control unless otherwise noted. (b) Flow cytometric analysis of internalized virions. Left, myDCs, pDCs and MDDCs were exposed to HTLV-1, and the cells permeabilized and stained with antibody to the core protein MA 24 h later. Right, pDCs exposed to HTLV-1 from two different HTLV-1 producer cell lines (DB1, 50 ng, and MT-2, 100 ng). In all graphs of flow cytometry analysis, protein expression was determined by subtracting the mean fluorescence intensity (MFI) of the isotype control cells from the MFI of cells treated with specific antibodies. (c) MDDCs were exposed to HTLV-1 for 3 h, and the intracellular abundance of viral proteins was determined 6, 16 and 48 h later. (d) HTLV-1 protein expression in DCs. Left, myDCs and pDCs were incubated with HTLV-1 in the presence or absence of 5 μM zidovudine (AZT), and the intracellular amount of MA was determined 3, 24 and 48 h later. Right, MDDCs were exposed to HTLV-1 that had either been inactivated by incubation at 56 °C or left on ice for 30 min. Intracellular amounts of protein were determined 3 and 24 h later. Data represent three to six independent experiments. Values in all graphs are means ± s.e.m.
To distinguish de novo infection from internalization, DCs were stained for the HTLV-1 regulatory protein Tax, which is not present in the virion15 and can be detected in cells only after proviral integration and de novo production of viral proteins. Tax was detected in MDDCs 16 h after exposure to cell-free virus, with the majority of the DCs expressing Tax by 48 h (Fig. 1c). Tax was also rapidly expressed in myDCs and pDCs after exposure to HTLV-1 (Fig. 1d). Blocking infection by treating DCs with reverse transcriptase inhibitors or by inactivating HTLV-1 virions reduced intracellular staining for Tax by over 95% (Fig. 1d), verifying that Tax staining reflected productive infection. We next examined whether the infected DCs produced HTLV-1 virions. This could not be examined at early times after infection, because, as shown for other viruses, both productively and nonproductively infected DCs release internalized viral core proteins for 3 d after HTLV-1 exposure (Supplementary Fig. 2 online). At later times after viral exposure, we detected virus in culture supernatants of DCs exposed to HTLV-1, verifying that infected DCs produce virus (Fig. 2a). Similar amounts of HTLV-1 were produced by infected pDCs, myDCs and MDDCs (Fig. 2a). Intracellular staining and western blot analysis confirmed de novo production of viral proteins in DCs 1 week after exposure to HTLV-1 virions (Fig. 2b). This is in contrast to CD4+ T cells, which, consistently with previous reports2,3, were not chronically infected after exposure to cell-free HTLV-1 (Supplementary Fig. 3 online). Moreover, HTLV-1 produced by infected DCs could infect other DCs (Fig. 2c), confirming that the virus was produced by DCs was infectious.
(a) pDCs were exposed to HTLV-1, trypsinized, washed thoroughly and cultured. Left, pDCs were exposed for 3 h to HTLV-1 (50 ng). At 3, 6, 9 and 13 d after infection, cultures were refed, and the supernatant was harvested 24 h later. Right, pDCs were exposed to HTLV-1 for 24 h and cultured for 2 weeks. Extracellular virus concentration, as measured by HTLV-1 MA (p19) abundance and shown as mean ± s.e.m., is shown in linear scale in the left panel and log scale in the right panel. (b) DCs were infected with HTLV-1 and harvested 7 d later. Left, flow cytometric analysis of MA and Tax (by intracellular staining) and SU (by surface staining). Right, HTLV-1–infected pDCs were lysed, and western blot analysis was performed with sera from HTLV-1–infected individuals (top) and antibodies to gp46 (SU; middle) and Tax (bottom), and with plasma pooled from HTLV-1–infected individuals, which, consistently with previous reports, recognizes p24 (CA) Gag and p53 (Gag precursor protein; top). As expected, Tax is present in both MT-2 cells and cells infected by virus from MT-2 as an Env-Tax fusion protein. Lane 1, HTLV-1–infected pDCs; lanes 2 and 3, uninfected CD4+ T cell lines (MOLT4 and SupT1, respectively); lane 4, HTLV-1–infected CD4+ T cell line (MT-2). (c) pDCs were exposed to HTLV-1 (10 ng) isolated from stably infected pDCs. Left, virus production. Data represent means ± s.e.m. Right, expression of viral proteins. (d) Cells were isolated from an individual with HAM-TSP, stimulated by culturing overnight in media containing phytohemagglutinin (CD4+ T cells) or CD40L (pDCs), and analyzed for expression of viral proteins. Data shown represent three to ten independent experiments.
MDDCs generated from monocytes isolated from individuals with HAM/TSP have been shown to express viral proteins14. To examine viral protein expression in pDCs infected in vivo, we obtained peripheral blood mononuclear cells (PBMCs) from an individual with HAM/TSP and isolated pDCs and CD4+ T cells. After 1 d, both CD40 ligand (CD40L)-stimulated pDCs and phytohemagglutinin-stimulated CD4+ T cells expressed HTLV-1 viral proteins (Fig. 2d).
CD4+ T cells are productively infected by HTLV-1–infected DCs
Because several viruses have been shown to spread by DC–T cell interactions, we reasoned that primary CD4+ T cells may be infected after contact with HTLV-1–infected DCs. To examine this, we exposed pDCs and myDCs to HTLV-1 virions and then cultured the DCs with autologous, activated CD4+ T cells. The CD4+ T cells internalized virus and became infected, as judged by the intracellular presence of MA and Tax (Fig. 3a). CD4+ T cells exposed to heat-inactivated virus via DCs expressed <3% of the amount of Tax expressed by cells exposed to infectious virus (Fig. 3a). Further characterization of DC-mediated infection by real-time PCR revealed that the HTLV-1 proviral copy number in CD4+ T cells 1 week after infection varied with the individual donors, ranging between 0.8 and 7.6 copies per 100 cells (Fig. 3b and data not shown). These levels are similar to the proviral loads observed in PBMCs isolated from asymptomatic HTLV-1-infected individuals (2–3 copies per 100 cells)16,17,18. Moreover, CD4+ T cells infected via DCs produced high amounts of HTLV-1 virus (Fig. 3c). This is in contrast to the relatively low amount of HTLV-1 produced by infected DCs, both when they have been separated after coculture with CD4+ T cells (Supplementary Table 1 online) and when they have not been exposed to T cells (Fig. 2). DCs from all of the individual donors examined (19 pDC donors, 7 myDC donors and 28 MDDC donors) were able to transfer HTLV-1 to, and productively infect, CD4+ T cells under these conditions (exposing DCs to 50–100 ng/ml of HTLV-1 virions, 1:5 ratio of DCs to T cells). Either exposing DCs to lower amounts of virus or decreasing the ratio of DCs to T cells also resulted in productive infection (Supplementary Figs. 4 and 5 online).
(a–c) DCs were exposed for 3–4 h to HTLV-1, trypsinized and cultured with CD4+ T cells. (a) Left, viral protein abundance, as measured by flow cytometry, 24 h after coculture. Right, DCs were exposed to heat-inactivated or untreated control HTLV-1 before coculture. Three hours later, T cells were isolated and Tax levels determined 48 h later. (b) DCs were exposed for 30 s (uninfected) or 4 h (infected) to HTLV-1 before coculture, and proviral load was determined in T cells isolated 1 week later. (c) T cells were separated after coculture as in a, and virus concentration was determined 7 d later. (d) Left, DCs were exposed to virus and cultured 3 d later with T cells as indicated, and virus internalization was measured 24 h later. Top, myDCs; bottom, pDCs. Right, DCs were exposed to HTLV-1 for 3 d and cultured with SupT1 or C8166. Six days later, T cells were isolated, and virus concentration was determined 24 h later. (e,f) Infection of SupT1/18x21-EGFP cells, as determined by flow cytometry from the percentage of EGFP-positive cells. (e) SupT1/18x21-EGFP cells cultured for 48 h with HTLV-1–infected pDCs (top row) or cell-free virus from the same cells (bottom row). Gray line, SupT1/18x21-EGFP cells incubated with supernatant from uninfected pDC cultures. (f) SupT1/18x21-EGFP cells cultured with the in vivo–infected, activated pDCs described in Figure 2d for 48 h. Data represent three to six independent experiments, except data in f, which represent triplicates of a single experiment. Graphs show mean ± s.e.m.
DCs transferred HTLV-1 virions to CD4+ T cell lines (SupT1, C8166) to a degree similar to that achieved with primary CD4+ T cells (Fig. 3d). These cell lines produced high amounts of virus 1 week after infection (Fig. 3d). To better characterize the early events after DC-mediated HTLV-1 transfer, we used an indicator cell line (SupT1/18x21-EGFP cells) in which EGFP expression is dependent on the expression of Tax19. Control studies verified that SupT1/18x21-EGFP cells infected via DCs expressed high amounts of EGFP, that EGFP expression required de novo viral expression and that the cells were productively infected with HTLV-1 (Supplementary Fig. 6 online). The majority of SupT1/18x21-EGFP cells were infected 2 d after exposure to HTLV-1–infected DCs (Fig. 3e). When pDCs isolated from an HTLV-1–infected individual were cultured with SupT1/18x21-EGFP cells, we observed that, like pDCs infected in vitro, in vivo–infected pDCs were able to productively infect CD4+ T cells (Fig. 3f).
Infection of CD4+ T cells via DCs occurs in cis and in trans
Another human retrovirus, HIV-1, infects CD4+ T cells via immature DCs in a biphasic manner. During the first day after viral exposure, before becoming infected, DCs capture and transfer virions to CD4+ T cells (trans infection). At later times, T cells are primarily infected by transmission of de novo–produced virus from infected DCs (cis infection)10,20. Our observation that HTLV-1 can be transmitted to T cells within 7 h after exposure of DCs to virus (Fig. 3a–c) indicates that DCs can also transfer HTLV-1 to T cells before becoming infected. To verify this, we incubated pDCs for 3 h with HTLV-1, cultured them with activated autologous CD4+ T cells and then separated the cells 3 h later. Analysis of the CD4+ T cells revealed internalized HTLV-1 immediately after isolation (Fig. 4a) and de novo viral protein expression within 48 h (Fig. 4a). As expected, because this transfer occurs before the infection of DCs, blocking infection with reverse transcriptase inhibitors did not lower the abundance of viral proteins in T cells infected via DCs (Fig. 4a). CD4+ T cells after such trans infection were productively infected with HTLV-1, expressing high amounts of virus by 1 week after coculture (Fig. 4b).
(a,b) pDCs were incubated with HTLV-1 for 3 h and cocultured with CD4+ T cells. The T cells were isolated 3 h later. (a) Left, internalization of virus into T cells, as determined from the amount of MA immediately after isolation. Right, pDCs were incubated for 30 min in the presence or absence of 5 μM AZT before a 3-h incubation with HTLV-1. The pDCs were then thoroughly washed and cultured with T cells that had been either treated 30 min with 10 μM AZT or left untreated. T cells were isolated 3 h later, and the amount of viral proteins was determined 48 h later. (b) Virus concentration in supernatants of T cell cultures 1, 2 and 3 weeks after exposure to pDCs. (c) MDDCs (top panels) or pDCs (bottom panels) were exposed to HTLV-1 for 3 d in the presence or absence of 5 μM AZT. They were then washed and cultured with CD4+ T cells, and virus internalization was determined 4 h later. (d) HTLV-1–infected DCs were exposed to HTLV-1, washed and cultured for 14 d. Infected DCs were cultured with CD4+ T cells for 24 h, the T cells were isolated and the virus concentration was determined 1 week later. Data represent three or four independent experiments. Graphs show mean ± s.e.m.
Next, to investigate whether infection of T cells at later times after exposure to HTLV-1–infected DCs involves virus produced by DCs, we exposed DCs to HTLV-1 for 3 d in the presence or absence of a reverse transcriptase inhibitor and determined their ability to transmit virus to T cells. Both untreated MDDCs and pDCs efficiently transferred virus to CD4+ T cells within 4 h of coculture (Fig. 4c). Blocking infection of DCs substantially reduced the transfer of HTLV-1 to CD4+ T cells (Fig. 4c), indicating that transmission to T cells at this later time involves de novo–synthesized virus. Further studies revealed that stably infected DCs can also productively infect autologous CD4+ T cells (Fig. 4d). Thus, whereas trans infection can occur soon after exposure of DCs to HTLV-1, at later times, CD4+ T cells are infected by de novo–produced virus from HTLV-1-infected DCs. Thus, like HIV-1, HTLV-1 uses both mechanisms in a biphasic manner to infect CD4+ T cells via immature DCs.
Role of NP-1 and HSPGs in DC–T cell transmission of HTLV-1
Two molecules involved in the initial interactions of HTLV-1 with CD4+ T cells and other cells are neurophilin-1 (NP-1) and heparan sulfate proteoglygans (HSPGs)21,22,23. Because NP-1 and HSPGs also have a role in DC–T cell interactions24,25, we reasoned that these two molecules might be important for DC–T cell transfer of HTLV-1. DC-mediated infection of SupT1/18x21-EGFP cells was reduced by approximately 50% when HSPGs were enzymatically removed before culture with HTLV-1–infected DCs (Fig. 5a). Incubating the cells with a peptide that blocks interactions with NP-1 (ref. 26) during culture also reduced infection by approximately 50%, and blocking interactions with both molecules further decreased infection (by 80%; Fig. 5b).
(a) SupT1/18x21-EGFP cells were treated to remove HSPGs or left untreated as described previously22 and then cultured for 3 h with HTLV-1–infected pDCs. The percentage of infected cells was determined 1 week later as in Figure 3f. p.i., post-infection. (b) SupT1/18x21-EGFP cells were treated and cultured as in a, and then SupT1/18x21-EGFP cells were incubated with either a peptide homologous to a portion of the NP-1 binding domain of the NP-1 ligand VEGF165 (exon 7) or a control peptide of the same length (ACTH). Left, percentage of infected cells. Right, virus concentration. (c) HTLV-1–infected pDCs were cultured with autologous naive (left) or activated (right) CD4+ T cells. Virus internalization into T cells was determined 3 h later. (d) Naive CD4+ T cells were incubated with either uninfected pDCs (left) or pDCs infected with HTLV-1 1 week beforehand (right). Cell surface expression of HSPGs and NP-1 was determined by flow cytometry 3 h later. (e) Left, naive CD4+ T cells were incubated for 30 min with either the exon 7 peptide and an antibody directed against HSPG (10E4) or appropriate controls (ACTH peptide and isotype control). They were cocultured 3 h with HTLV-1–infected DCs, and virus internalization was determined 24 h later. Right, activated CD4+ T cells treated as in b were cultured with HTLV-1–infected pDCs. Three hours later, T cells were isolated, and Tax abundance was determined 1 week later. Data shown represent three to five independent experiments. Graphs show mean ± s.e.m.
Previous studies have indicated that cell-free HTLV-1 can bind and enter activated, but not quiescent, CD4+ T cells27. Because T cells are activated during interactions with DCs, we examined whether DCs could transmit virus to quiescent CD4+ T cells. HTLV-1 was internalized by naive T cells within 3 h after coculture with HTLV-1–exposed DCs, although at a lower level than by activated cells from the same individual (Fig. 5c). T cell surface expression of both NP-1 and HSPGs was rapidly induced after coculture of infected pDCs with autologous quiescent T cells (Fig. 5d), consistently with previous observations that these molecules are induced after in vitro activation of T cells21,22. Blocking interactions with HSPG and NP-1 blocked the DC-mediated transfer of HTLV-1 to both naive CD4+ T cells and activated CD4+ T cells (Fig. 5e). Thus, two molecules needed for initial binding of HTLV-1 to CD4+ T cells are also important for DC–T cell transmission of HTLV-1.
Transformation of CD4+ T cells infected with HTLV-1 via DCs
In previous in vitro studies, chronic infection and IL-2–independent transformation of T cells by HTLV-1 required coculture with irradiated virus-producer cells28,29. To examine whether T cells infected via DCs could also be transformed by HTLV-1, we removed IL-2 from CD4+ T cells cultures 6 weeks after infection. Whereas cells in the uninfected cultures died rapidly, cells in the HTLV-1–infected cultures continued to proliferate. The IL-2–independent cultures continued to produce virus in amounts (15–120 ng/ml) similar to those produced by T cell lines transformed by T cell–T cell transmission of virus or established from the cells of infected individuals. Similarly, the HTLV-1 proviral copy number in the transformed CD4+ T cell cultures (0.45–4.7 proviral copies per cell, data not shown) was similar to the range reported for other HTLV-1–transformed cell lines (0.9–5.2 proviral copies per cell)30. To verify that individual cells in these cultures were transformed, we subjected the cells to limiting-dilution cloning. Cultures derived from single cells remained IL-2–independent and continued to produce high amounts of virus (Fig. 6a). These cloned transformed cells expressed high amounts of viral proteins (Fig. 6b), did not express DC markers (CD123 in Fig. 6b and data not shown) and shared phenotypic characteristics (CD3+, CD4+) with malignant T cells from individuals with ATL (Fig. 6b).
(a) HTLV-1–infected pDCs and MDDCs were cultured with CD4+ T cells for 1 week, and then CD4+ T cells were removed. Six weeks later, IL-2 was removed from the T cell cultures, and IL-2–independent cultures of T cells were subjected to limiting dilution cloning 28 weeks later. Four weeks later, the concentration of HTLV-1 was determined in six clones each from two independent cultures transformed via MDDCs (M1 and M2) and pDCs (P1 and P2). (b) Phenotype of cloned IL-2–independent cells generated as described in a, as determined by flow cytometry 40 weeks after infection. Shown are one clone from each of the four cultures (left to right: M1, M2, P1, P2) in a representative experiment out of four performed.
Discussion
Because cell-free HTLV-1 cannot efficiently infect T cells in vitro, it has been widely believed that transmission of HTLV-1 is qualitatively and/or quantitatively different from that of most other retroviruses. Here, we demonstrate that HTLV-1 is not poorly infectious and that the mechanism of HTLV-1 transmission is similar to that of other retroviruses. Exposure of primary DCs to cell-free HTLV-1 virions at concentrations similar to those used for other retroviral infections3,31 results in efficient, productive infection. Moreover, CD4+ T cells are efficiently infected after contact with HTLV-1–exposed DCs, paralleling recent observations that HIV-1, although highly infectious as a cell-free particle, is more efficiently transmitted by DC–T cell interactions31,32,33. This study raises the possibility that other viruses thought to be poorly infectious because of their poor infectivity in vitro may also utilize DCs to efficiently infect their target cells.
Previous studies of infection of DCs by HTLV-1, performed with in vitro–derived MDDCs, yielded conflicting results. Various laboratories reported observing binding but no internalization34, internalization by cell-associated but not cell-free virus13, and cell-free infection but no transfer to or immortalization of CD4+ T cells14. The differing results obtained in previous studies with MDDCs underscore the importance of performing infection studies with ex vivo primary cell cultures. Our studies, using freshly isolated myDCs and pDCs as well as MDDCs, are the first (to our knowledge) to report production of infectious virus by DCs, DC–T cell virus transfer, and infection and immortalization of T cells by HTLV-1 via DCs.
These in vitro observations are supported by earlier in vivo studies11,14,35, indicating that they are directly relevant to HTLV-1 transmission in vivo. Our observations that HTLV-1 productively infects DCs and pDCs from an individual with HAM-TSP express HTLV-1 proteins confirm and extend earlier reports that MDDCs generated from monocytes from some individuals with HAM-TSP express viral proteins14 and that DCs in infected individuals contain viral sequences11,35. High HTLV-1 proviral loads (4–37 copies per 100 cells) have been observed in pDCs isolated from asymptomatic individuals11. Studies of DCs isolated from HTLV-1–infected individuals, along with our observations of efficient ex vivo infection of pDCs and myDCs (Figs. 1 and 2), suggest that cell-free HTLV-1 can also infect DCs in vivo. These studies thus alter the current paradigm concerning HTLV-1 infection, which involves cell-cell transmission of the virus between T cells.
For many viruses, infection of DCs affects the host's ability to mount an appropriate immune response by interfering with DC development, maturation, function and/or viability9. A number of aspects of HTLV-1–induced immunosuppression are consistent with alterations in DC function. Adaptive immunity is impaired in asymptomatic HTLV-1–infected individuals36,37,38,39. Both MDDCs generated from monocytes of HTLV-1–infected individuals36 and MDDCs infected in vitro38 are poor stimulators of autologous T cell differentiation. CD4+ T cells from individuals with ATL are deficient in expression of CD40L36,40, a molecule with a central role in activation by antigen-presenting cells. HTLV-1 infection of DCs also interferes with innate immunity: pDCs isolated from HTLV-1–infected individuals are impaired in their ability to produce type I interferon11, an important antiviral mechanism of the innate immune system.
HTLV-1 infection of DCs may have an important role in the development of ATL and HAM-TSP. Individuals with ATL, like asymptomatic carriers, have impaired immune systems41 and development of ATL is associated with an increase in the number of HTLV-1–infected cells not recognized by CD8+ CTLs42,43. In individuals with HAM/TSP, high viral loads are associated with decreased degeneracy of T cell recognition44. These observations suggest that, in both of these diseases, infection of DCs modifies the presentation of HTLV-1 antigens and thus generates a repertoire of CD8+ T cells that do not efficiently recognize the virally infected cells. Development of ATL is also associated with the loss of pDCs and myDCs11, consistent with observations from other viruses that infection of DCs can induce cytopathic effects9.
In addition to providing insights into transmission and pathogenesis, this work describes an efficient system to transmit HTLV-1 in vitro. Here this approach was used to show that NP-1 and HSPGs, two crucial molecules for efficient binding of HTLV-1 to CD4+ T cells21,22,23, are also involved in the transfer of HTLV-1 from DCs to T cells. This approach could be also used to investigate the role of other molecules previously reported to be involved in HTLV-1 Env-mediated transmission and fusion, including GLUT-1 (ref. 45) and DC-SIGN12,13. Moreover, because DC-mediated trans infection of T cells eliminates the need for HTLV-1–infected cells, and because T cells can be easily separated from DCs after coculture, this system represents a new approach for dissection of the early events in HTLV-1–induced transformation and HTLV-1 infection.
Our data indicate that the previous models of HTLV-1 transmission, persistence and pathogenesis should be revisited. Because DCs have a pivotal role in antiviral immunity, methods to efficiently infect these cells in culture should allow for further dissection of the effect of HTLV-1 infection on pDC- and myDC-mediated immune function and pathogenesis.
Methods
Isolation, separation and culture of primary cells.
We obtained informed consent from all subjects. We collected leukopaks of peripheral blood from healthy donors and an individual with HAM/TSP, as well as cord blood from healthy donors, according to US National Institutes of Health Institutional Review Board protocols, and we separated PBMCs as previously described46. We isolated CD4+ T cells, pDCs, myDCs and monocytes from PBMCs with immunomagnetic beads (Miltenyi Biotec). We isolated naive unactivated CD4+ T cells, and isolated, activated and cultured CD4+ T cells as previously described46. Details on isolation, culture and phenotyping of pDCs, myDCs and monocytes are provided in the Supplementary Methods online.
Cell culture and reagents.
We obtained and maintained SupT1, C8166, MT-2 and 729/ACH cells as described previously46,47. DB-1 is a newly derived HTLV-1 producer cell line generated after DC-mediated infection of primary CD4+ T cells. We obtained the SupT1/18x21-EGFP cell line, generated by limiting-dilution cloning following transduction of SupT1 cells with a lentivirus vector encoding EGFP under control of a Tax-dependent promoter19 from L. Yang, M. Liu and C.-Z. Giam. We obtained heparan sulfate lyase from Seikagaku and the 24–amino acid peptide homologous to the NP-1–binding portion of the ligand VEGF165 (exon 7)26 and a control peptide of the same length (ACTH) from GenScript.
Flow cytometric analysis.
We performed flow cytometry analyses and measured specific binding of HTLV-1 virions to target cells as previously described22,48. Antibodies directed against CCR7 were from R&D Systems, antibodies to HSPGs (F58-10E4) were from Seikagaku and the remainder were from BD Pharmingen. We measured virus internalization as previously described46 with the following modifications. We obtained virus from HTLV-1 producer cell lines resuspended in fresh media 16 h beforehand at 2 × 106 cells/ml. After incubating target cells with virus, we incubated them in trypsin for 10 min at 37 °C to remove virus bound to the cell surface. We stained the cells for either HTLV-1 MA or SU as described previously47 or, to measure de novo viral protein production, with an antibody to Tax49 (gift of C.-Z. Giam). For experiments in which the DCs and CD4+ T cells were not separated, we stained the cells with an antibody to CD3 and analyzed the T cells by gating on the CD3+ subset.
Infection of dendritic cells and dendritic cell–to–T cell transmission.
We plated DCs in six-well plates at 50,000 cells/well, then harvested them with Cell Dissociation Solution (Sigma) after the appropriate interval: for myDCs and pDCs, 24 h later; for MDDCs, 7–10 d later. We incubated the DCs with HTLV-1 (100 ng unless otherwise indicated) for 3 h unless otherwise indicated. We then incubated the cells in trypsin for 10 min at 37 °C and washed twice with media containing 20% FCS. For studies of DC infection, we either harvested the cells immediately or replated the cells in six-well plates at 500,000 cells/well. For studies of DC–T cell transmission, we replated DCs in six-well plates at 500,000 cells/well unless otherwise noted. We added T cells (2,500,000/well in a six-well plate) to the DCs after the interval indicated in Figures 3 and 4 (3 h to 3 d), and refed the cultures with a 1:1 ratio of the medium for DCs to the medium for CD4+ T cells. Target cells in DC–T cell transmission studies were autologous, activated CD4+ T cells unless otherwise indicated. We separated CD4+ T cells from the DCs by positive selection for CD3+ cells with immunomagnetic beads.
Quantification of HTLV-1 viral production and proviral load.
We determined the concentration of HTLV-1 in the supernatant of infected cell cultures by measuring the amount of MA (p19) protein by ELISA (Zeptometrix). We extracted DNA from cells using the QIAamp DNA Blood Mini Kit (Qiagen) and quantified HTLV-1 proviral load by real-time PCR as described previously50. We performed western blot analysis as previously described22 with the following modifications. We incubated the immunoblots overnight at 4 °C with either plasma pooled from HTLV-1–infected individuals (Scripps Laboratories) or with antibodies directed against either HTLV-1 Tax or HTLV-1 SU (Zeptometrix).
Transformation assay.
We assayed for T cell transformation as described previously28 with the following modifications. We cultured HTLV-1–exposed DCs for 1 week with activated CD4+ T cells, then separated the T cells and cultured them at 500,000 cells/ml in 24-well or six-well plates. Five weeks later, we refed the cells with medium without IL-2 and cultured an additional 6–28 weeks. Some transformed cells were cloned 12–16 weeks after infection at a cell density of 0.3 cells/well.
Statistical analyses.
For analyses involving multiple samples, the mean and the s.e.m. were determined, and data are presented as the mean ± s.e.m.
Note: Supplementary information is available on the Nature Medicine website.
References
Poiesz, B.J. et al. Detection and isolation of type C retrovirus particles from fresh and cultured lymphocytes of a patient with cutaneous T-cell lymphoma. Proc. Natl. Acad. Sci. USA 77, 7415–7419 (1980).
Feuer, G. & Green, P.L. Comparative biology of human T-cell lymphotropic virus type 1 (HTLV-1) and HTLV-2. Oncogene 24, 5996–6004 (2005).
Fan, N. et al. Infection of peripheral blood mononuclear cells and cell lines by cell-free human T-cell lymphoma/leukemia virus type I. J. Clin. Microbiol. 30, 905–910 (1992).
Donegan, E. et al. Transfusion transmission of retroviruses: human T-lymphotropic virus types I and II compared with human immunodeficiency virus type 1. Transfusion 34, 478–483 (1994).
Igakura, T. et al. Spread of HTLV-I between lymphocytes by virus-induced polarization of the cytoskeleton. Science 299, 1713–1716 (2003).
Overbaugh, J. HTLV-1 sweet-talks its way into cells. Nat. Med. 10, 20–21 (2004).
Steinman, R.M. & Hemmi, H. Dendritic cells: translating innate to adaptive immunity. Curr. Top. Microbiol. Immunol. 311, 17–58 (2006).
Courreges, M.C., Burzyn, D., Nepomnaschy, I., Piazzon, I. & Ross, S.R. Critical role of dendritic cells in mouse mammary tumor virus in vivo infection. J. Virol. 81, 3769–3777 (2007).
Pohl, C., Shishkova, J. & Schneider-Schaulies, S. Viruses and dendritic cells: enemy mine. Cell. Microbiol. 9, 279–289 (2007).
Wu, L. & KewalRamani, V.N. Dendritic-cell interactions with HIV: infection and viral dissemination. Nat. Rev. Immunol. 6, 859–868 (2006).
Hishizawa, M. et al. Depletion and impaired interferon-α–producing capacity of blood plasmacytoid dendritic cells in human T-cell leukaemia virus type I–infected individuals. Br. J. Haematol. 125, 568–575 (2004).
Kampani, K. et al. A novel high throughput quantum dot–based fluorescence assay for quantitation of virus binding and attachment. J. Virol. Methods 141, 125–132 (2007).
Ceccaldi, P.E. et al. DC-SIGN facilitates fusion of dendritic cells with human T-cell leukemia virus type 1–infected cells. J. Virol. 80, 4771–4780 (2006).
Makino, M., Shimokubo, S., Wakamatsu, S.I., Izumo, S. & Baba, M. The role of human T-lymphotropic virus type 1 (HTLV-1)-infected dendritic cells in the development of HTLV-1–associated myelopathy/tropical spastic paraparesis. J. Virol. 73, 4575–4581 (1999).
Ehrlich, G.D. et al. Detection of anti–HTLV-I Tax antibodies in HTLV-I enzyme-linked immunosorbent assay–negative individuals. Blood 74, 1066–1072 (1989).
Shinzato, O. et al. Semiquantitative analysis of integrated genomes of human T-lymphotropic virus type I in asymptomatic virus carriers. Blood 78, 2082–2088 (1991).
Silva, M.T. et al. Human T lymphotropic virus type 1 (HTLV-1) proviral load in asymptomatic carriers, HTLV-1–associated myelopathy/tropical spastic paraparesis, and other neurological abnormalities associated with HTLV-1 infection. Clin. Infect. Dis. 44, 689–692 (2007).
Ureta-Vidal, A. et al. Human T cell leukemia virus type I (HTLV-I) infection induces greater expansions of CD8 T lymphocytes in persons with HTLV-I–associated myelopathy/tropical spastic paraparesis than in asymptomatic carriers. J. Infect. Dis. 183, 857–864 (2001).
Zhang, L., Liu, M., Merling, R. & Giam, C.Z. Versatile reporter systems show that transactivation by human T-cell leukemia virus type 1 Tax occurs independently of chromatin remodeling factor BRG1. J. Virol. 80, 7459–7468 (2006).
Turville, S.G. et al. Immunodeficiency virus uptake, turnover, and 2-phase transfer in human dendritic cells. Blood 103, 2170–2179 (2004).
Ghez, D. et al. Neuropilin-1 is involved in human T-cell lymphotropic virus type 1 entry. J. Virol. 80, 6844–6854 (2006).
Jones, K.S., Petrow-Sadowski, C., Bertolette, D.C., Huang, Y. & Ruscetti, F.W. Heparan sulfate proteoglycans mediate attachment and entry of human T-cell leukemia virus type 1 virions into CD4+ T cells. J. Virol. 79, 12692–12702 (2005).
Pinon, J.D. et al. Human T-cell leukemia virus type 1 envelope glycoprotein gp46 interacts with cell surface heparan sulfate proteoglycans. J. Virol. 77, 9922–9930 (2003).
Chung, J.S., Dougherty, I., Cruz, P.D., Jr. & Ariizumi, K. Syndecan-4 mediates the coinhibitory function of DC-HIL on T cell activation. J. Immunol. 179, 5778–5784 (2007).
Tordjman, R. et al. A neuronal receptor, neuropilin-1, is essential for the initiation of the primary immune response. Nat. Immunol. 3, 477–482 (2002).
Barr, M.P. et al. A peptide corresponding to the neuropilin-1-binding site on VEGF(165) induces apoptosis of neuropilin-1–expressing breast tumour cells. Br. J. Cancer 92, 328–333 (2005).
Nath, M.D., Ruscetti, F.W., Petrow-Sadowski, C. & Jones, K.S. Regulation of the cell-surface expression of an HTLV-I binding protein in human T cells during immune activation. Blood 101, 3085–3092 (2003).
Green, P.L., Ross, T.M., Chen, I.S. & Pettiford, S. Human T-cell leukemia virus type II nucleotide sequences between env and the last exon of tax/rex are not required for viral replication or cellular transformation. J. Virol. 69, 387–394 (1995).
Persaud, D., Munoz, J.L., Tarsis, S.L., Parks, E.S. & Parks, W.P. Time course and cytokine dependence of human T-cell lymphotropic virus type 1 T-lymphocyte transformation as revealed by a microtiter infectivity assay. J. Virol. 69, 6297–6303 (1995).
Li, M. & Green, P.L. Detection and quantitation of HTLV-1 and HTLV-2 mRNA species by real-time RT-PCR. J. Virol. Methods 142, 159–168 (2007).
Thomas, J.A., Ott, D.E. & Gorelick, R.J. Efficiency of human immunodeficiency virus type 1 postentry infection processes: evidence against disproportionate numbers of defective virions. J. Virol. 81, 4367–4370 (2007).
Gummuluru, S., KewalRamani, V.N. & Emerman, M. Dendritic cell–mediated viral transfer to T cells is required for human immunodeficiency virus type 1 persistence in the face of rapid cell turnover. J. Virol. 76, 10692–10701 (2002).
Piguet, V. & Sattentau, Q. Dangerous liaisons at the virological synapse. J. Clin. Invest. 114, 605–610 (2004).
Zucker-Franklin, D., Fraig, M. & Grusky, G. Interaction of human immunodeficiency virus type 1, human T-cell leukemia/lymphoma virus type I (HTLV-I), and HTLV-II with in vitro–generated dendritic cells. Clin. Diagn. Lab. Immunol. 2, 343–348 (1995).
Macatonia, S.E., Cruickshank, J.K., Rudge, P. & Knight, S.C. Dendritic cells from patients with tropical spastic paraparesis are infected with HTLV-1 and stimulate autologous lymphocyte proliferation. AIDS Res. Hum. Retroviruses 8, 1699–1706 (1992).
Al-Dahoodi, Z.M., Takemoto, S., Kataoka, S. & Taguchi, T. Dysfunction of dendritic and T cells as the cause of immune suppression in HTLV-I infected individuals. J. Clin. Exp. Hematop. 43, 43–48 (2003).
Katsuki, T., Katsuki, K., Imai, J. & Hinuma, Y. Immune suppression in healthy carriers of adult T-cell leukemia retrovirus (HTLV-I): impairment of T-cell control of Epstein-Barr virus–infected B cells. Jpn. J. Cancer Res. 78, 639–642 (1987).
Makino, M., Wakamatsu, S., Shimokubo, S., Arima, N. & Baba, M. Production of functionally deficient dendritic cells from HTLV-I–infected monocytes: implications for the dendritic cell defect in adult T cell leukemia. Virology 274, 140–148 (2000).
Mascarenhas, R.E. et al. Peripheral blood mononuclear cells from individuals infected with human T-cell lymphotropic virus type 1 have a reduced capacity to respond to recall antigens. Clin. Vaccine Immunol. 13, 547–552 (2006).
Makino, M. et al. Association of CD40 ligand expression on HTLV-I–infected T cells and maturation of dendritic cells. Scand. J. Immunol. 54, 574–581 (2001).
Taguchi, H. & Miyoshi, I. Immune suppression in HTLV-I carriers: a predictive sign of adult T-cell leukemia. Acta Med. Okayama 43, 317–321 (1989).
Arnulf, B. et al. Loss of the ex vivo but not the reinducible CD8. T-cell response to Tax in human T-cell leukemia virus type 1-infected patients with adult T-cell leukemia/lymphoma. Leukemia 18, 126–132 (2004).
Furukawa, Y., Kubota, R., Tara, M., Izumo, S. & Osame, M. Existence of escape mutant in HTLV-I tax during the development of adult T-cell leukemia. Blood 97, 987–993 (2001).
Kubota, R., Furukawa, Y., Izumo, S., Usuku, K. & Osame, M. Degenerate specificity of HTLV-1–specific CD8. T cells during viral replication in patients with HTLV-1-associated myelopathy (HAM-TSP). Blood 101, 3074–3081 (2003).
Manel, N. et al. The HTLV receptor is an early T-cell activation marker whose expression requires de novo protein synthesis. Blood 101, 1913–1918 (2003).
Jones, K.S. et al. Induction of human T cell leukemia virus type I receptors on quiescent naive T lymphocytes by TGF-β. J. Immunol. 174, 4262–4270 (2005).
Jones, K.S. et al. Human T-cell leukemia virus type 1 (HTLV-1) and HTLV-2 use different receptor complexes to enter T cells. J. Virol. 80, 8291–8302 (2006).
Hague, B.F., Zhao, T.M. & Kindt, T.J. Binding of HTLV-1 virions to T cells occurs by a temperature- and calcium-dependent process and is blocked by certain type 2 adenosine receptor antagonists. Virus Res. 93, 31–39 (2003).
Liu, B., Hong, S., Tang, Z., Yu, H. & Giam, C.Z. HTLV-I Tax directly binds the Cdc20-associated anaphase-promoting complex and activates it ahead of schedule. Proc. Natl. Acad. Sci. USA 102, 63–68 (2005).
Yamano, Y. et al. Correlation of human T-cell lymphotropic virus type 1 (HTLV-1) mRNA with proviral DNA load, virus-specific CD8. T cells, and disease severity in HTLV-1-associated myelopathy (HAM-TSP). Blood 99, 88–94 (2002).
Acknowledgements
We are grateful to L. Yang, M. Liu and C.-Z. Giam (Uniformed Services University of Health Sciences) for reagents; O. Unsong and S. Jacobson (National Institute of Neurological Disorders and Stroke, National Institutes of Health) for PBMCs from the HTLV-1–infected individual; C. Pique, G. Trinchieri and D. Klinman for critical review of the manuscript; S. Reynolds for technical assistance; and P. Green, V. KewalRamani and C.-Z. Giam for helpful discussions. This project has been funded in whole or in part with federal funds from the US National Cancer Institute and US National Institutes of Health under contract N01-CO-12400. The content of this publication does not necessarily reflect the views or policies of the Department of Health and Human Services, nor does mention of trade names, commercial products or organizations imply endorsement by the US government. This research was supported in part by the Intramural Research Program of the US National Institutes of Health, US National Cancer Institute and Center for Cancer Research.
Author information
Authors and Affiliations
Contributions
K.S.J. and F.W.R. designed the experiments, performed data analysis and wrote the manuscript. C.P.-S., Y.K.H. and D.C.B. prepared the reagents, conducted the experiments and edited the manuscript.
Corresponding author
Supplementary information
Supplementary Text and Figures
Supplementary Figs. 1–6, Supplementary Table 1 and Supplementary Methods (PDF 611 kb)
Rights and permissions
About this article
Cite this article
Jones, K., Petrow-Sadowski, C., Huang, Y. et al. Cell-free HTLV-1 infects dendritic cells leading to transmission and transformation of CD4+ T cells. Nat Med 14, 429–436 (2008). https://doi.org/10.1038/nm1745
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nm1745
This article is cited by
-
An acquired phosphatidylinositol 4-phosphate transport initiates T-cell deterioration and leukemogenesis
Nature Communications (2022)
-
HTLV-1 infection of myeloid cells: from transmission to immune alterations
Retrovirology (2019)
-
Viral antigens detectable in CSF exosomes from patients with retrovirus associated neurologic disease: functional role of exosomes
Clinical and Translational Medicine (2018)
-
Inhibition of Tunneling Nanotube (TNT) Formation and Human T-cell Leukemia Virus Type 1 (HTLV-1) Transmission by Cytarabine
Scientific Reports (2018)
-
Stability of the HTLV-1 glycoprotein 46 (gp46) gene in an endemic region of the Brazilian Amazon and the presence of a significant mutation (N93D) in symptomatic patients
Virology Journal (2018)