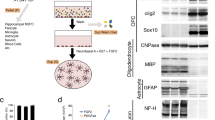
Abstract
Cerebral dopamine depletion is the hallmark of Parkinson disease. Because dopamine modulates ontogenetic neurogenesis, depletion of dopamine might affect neural precursors in the subependymal zone and subgranular zone of the adult brain. Here we provide ultrastructural evidence showing that highly proliferative precursors in the adult subependymal zone express dopamine receptors and receive dopaminergic afferents. Experimental depletion of dopamine in rodents decreases precursor cell proliferation in both the subependymal zone and the subgranular zone. Proliferation is restored completely by a selective agonist of D2-like (D2L) receptors. Experiments with neural precursors from the adult subependymal zone grown as neurosphere cultures confirm that activation of D2L receptors directly increases the proliferation of these precursors. Consistently, the numbers of proliferating cells in the subependymal zone and neural precursor cells in the subgranular zone and olfactory bulb are reduced in postmortem brains of individuals with Parkinson disease. These observations suggest that the generation of neural precursor cells is impaired in Parkinson disease as a consequence of dopaminergic denervation.
Similar content being viewed by others
Main
In Parkinson disease, dopaminergic midbrain neurons degenerate, leading to cerebral dopamine depletion1,2. Dopamine is implicated in the modulation of movements, mood and motivation. Consequently, individuals with Parkinson disease show characteristic impairments of these functions.
In the developing mammalian brain, dopamine contributes to morphogenesis by governing the activity of neural stem cells3. Dopamine appears early during ontogenesis4, as do its receptors5,6, and affects cell proliferation in the embryonic germinal zones7. Findings have suggested that there is a developmental continuum of germinal activity that links embryonic stem cells to neural stem cells located in restricted areas of the adult brain8. The regulation of precursor cells by dopamine might therefore persist into adulthood, and dopamine depletion, the hallmark of Parkinson disease, might affect adult neurogenesis.
Here we show experimentally that dopamine modulates adult neurogenesis in vivo and in vitro and that adult neurogenesis is impaired in individuals with Parkinson disease.
Results
Dopaminergic fibers in the subependymal zone
Neural stem cells are located in the adult mammalian subependymal zone9,10,11,12, immediately adjacent to the striatum, which is rich in dopaminergic afferents from the substantia nigra. Dopaminergic neurites, identified by their immunoreactivity for the dopamine transporter (DAT), were also present in the adult mouse subependymal zone (Fig. 1a). Neurites in the subependymal zone were detected with the catecholaminergic marker tyrosine hydroxylase, but not with the noradrenergic marker dopamine-β-hydroxylase, confirming that the tyrosine hydroxylase–expressing (TH+) fibers in the subependymal zone are indeed dopaminergic.
(a–e) Laser scanning confocal images of the subependymal zone of adult mice. (a) DAT+ (green) fibers in close contact with a BrdU+ cell (red) 3 weeks after BrdU labeling. (b) PSA-NCAM+ migrating neuroblasts (A-cells, red), separated from DAT+ fibers (green) by GFAP+ astrocytes (B-cells, blue). (c) DAT+ fibers (green) in contact with an EGFR+ cell (red) with nuclear expression of the proliferation marker PCNA (blue). (d) A DAT+ nerve ending (green) expressing synaptophysin (blue) and contacting an EGFR+ cell (red). (e) Detail from d, focusing on the DAT+ (green), synaptophysin+ (blue) nerve fiber (arrow) on the EGFR+ cell (red) at high magnification. Scale bars, 5 μm (a); 10 μm (b); 5 μm (c); 2 μm (d); 1 μm (e). (f–i) Electron microscopic image of a presynaptic structure apposed to a C-cell in the subependymal zone of an adult rat. (f) C-cell identified on the basis of published morphological criteria13. (g–i) Successive magnifications of the boxed areas in f–h, respectively. (h) Presynaptic element in contact with the plasma membrane of the C-cell (red) and containing mitochondria (blue) and vesicles (green). (i) Examples of the vesicles at higher magnification. Scale bars, 2 μm (f); 500 nm (g); 200 nm (h); 40 nm (i). (j–l) Immunoelectron microscopic image showing the relationship between TH+ fibers (electron-dense DAB precipitate) and the different cell types in the subependymal zone of adult rats. Arrows in j indicate TH+ fibers. (l) Detail from the boxed area in k, showing a TH+ structure containing mitochondria (blue) and vesicles (green) apposed to a C-cell. A, A-cells; B, B-cells; C, C-cells. Scale bars, 5 μm (j); 2 μm (k); 500 nm (l). (m–p) Immunoelectron microscopic image showing the presence of D1L (m,n) and D2L (o,p) receptors (electron-dense gold particles, arrows) on A- and C- but not B-cells in the subependymal zone of adult rats. Insets show details from the boxed areas. Scale bars, 2 μm (m–p). (q) Summary schema. Gray, ependymal cells; red, migrating neuroblasts (A-cells); blue, astrocytes (B-cells); green, transit-amplifying C-cell; black, dopaminergic fibers; ●, D1L receptors; ○, D2L receptors.
To determine the relationship between the dopaminergic fibers and proliferating subependymal zone cells, we injected adult mice with the thymidine analog 5-bromodeoxyuridine (BrdU) to label mitotic cells. To identify infrequently dividing precursors, we also injected mice eight times with 50 mg per kg (body weight) of BrdU at 6-h intervals over a 2-d period. The mice were killed 3 weeks later. The time lag between labeling and death was long enough for the bulk of restricted precursors to have migrated out of the subependymal zone12. The BrdU+ cells remaining in the subependymal zone were therefore likely to be upstream elements in the neural cell lineage. Confocal microscopy showed dopaminergic fibers in close contact with 80% of these BrdU+ subependymal zone cells (Fig. 1a).
Dopaminergic fibers preferentially contact EGFR+ cells
We next determined the identity of the subependymal zone cells receiving dopaminergic afferents. The subependymal zone stem cell lineage comprises several types of cell12,13,14. Specialized astrocytes (B-cells) are infrequently dividing stem cells, which generate frequently dividing, transit-amplifying C-cells, which in turn produce restricted neuroblasts (A-cells) destined to migrate via the rostral migratory stream (RMS) to the olfactory bulb, where they integrate as interneurons10,12,13,14.
A-cells are identified by their expression of polysialic neural cell-adhesion molecule (PSA-NCAM), and B-cells by their expression of glial fibrillary acidic protein (GFAP)13,14. By confocal microscopy, we found a minority (4.8 ± 0.8%) of PSA-NCAM+ A-cells in the vicinity of dopaminergic fibers (Fig. 1b). GFAP+ B-cells were more often found close to dopaminergic fibers, but their branched morphology precluded a meaningful quantification (Fig. 1b). However, most (87.2 ± 1.9%) of the cells expressing epidermal growth factor receptor (EGFR) were in contact with dopaminergic fibers (Fig. 1c). EGFR is expressed by all C-cells and a small subset of B-cells, but not by A-cells14. On confocal analysis, we found that 2.1 ± 0.6% of the EGFR+ cells expressed GFAP, suggesting that 97.9% of the EGFR+ cells were C-cells. Dopaminergic nerve endings contacting EGFR+ cells expressed synaptophysin, a marker of presynaptic exocytotic vesicles, suggesting that there was functional dopaminergic transmission (Fig. 1d,e).
Ultrastructure of dopaminergic afferents to C-cells
We verified the presence of afferents to subependymal zone cells in rat brains by electron microscopy. Nerve terminals were readily detected in contact with the plasma membrane of C-cells (Fig. 1f–i), which were identified by their smooth elliptical surface, deeply invaginated nuclei and prominent Golgi apparatus13. The apposed terminals contained mitochondria and numerous small vesicles with a diameter of 40.3 ± 1.3 nm (Fig. 1h,i), suggesting that they had the capacity to release a neurotransmitter. No postsynaptic densities, characteristic of excitatory synapses, were observed on C-cells. Presynaptic structures were not found in contact with A-cells, identified by their smooth elongated shape and dark cytoplasm containing many microtubules and free ribosomes13, or with B-cells, identified by their irregular shape and light cytoplasm containing dense bodies and many mitochondria13.
We analyzed the ultrastructural relationship between tyrosine hydroxylase–immunolabeled dopaminergic fibers and subependymal zone cells. TH+ fibers were not found in contact with the plasma membranes of A-cells, and a layer of B-cells was typically located between A-cells and the dopaminergic fibers (Fig. 1j). Dopaminergic fibers did, however, contact C-cells (Fig. 1k). As above, the dopaminergic terminals apposed to C-cells contained mitochondria and small vesicles, suggesting their capacity to release neurotransmitter (Fig. 1l).
D2L receptors predominate on C-cells
Dopamine receptors are classified into D1-like (D1L; D1 and D5 receptors) and D2L (D2, D3 and D4 receptors) subfamilies according to structural and functional homology. We studied the expression of D1L and D2L receptors in the rat subependymal zone by immunoelectron microscopy.
No D1L or D2L receptors were found in B-cells (Fig. 1m,n). D1L receptors were present in the cytoplasm of C-cells (Fig. 1m) and in the plasma membranes of A-cells (Fig. 1n). D2L receptors were most abundant in C-cells, in both the cytoplasm and plasma membranes (Fig. 1o), and less frequent in the plasma membranes of A-cells (Fig. 1p).
Dopamine denervation reduces subependymal zone proliferation
To test whether dopaminergic subependymal zone afferents are functionally implicated in the regulation of proliferation, we selectively ablated the dopaminergic forebrain innervation of adult mice by using the neurotoxin 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP)15. At the dose administered (four injections of 10 mg/kg at 2-h intervals), the dopaminergic denervation of the striatum and adjacent subependymal zone was almost complete during the first few days after MPTP injection, as assessed by immunolabeling for DAT and tyrosine hydroxylase (Fig. 2a–c,e). However, the number of dopaminergic neurons in the substantia nigra did not significantly decrease (control, 918 ± 77; MPTP, 799 ± 100), allowing complete recovery of the dopaminergic fibers in the striatum and subependymal zone during the 70 d after the lesion (Fig. 2a–c,e).
(a–c) Coronal sections of the anterior forebrain immunostained with antibodies to DAT (a,b) and tyrosine hydroxylase (TH; c), visualizing dopaminergic fibers in the striatum (a) and subependymal zone (b,c) of a control mouse and MPTP-lesioned mice killed 1, 2, 7, 21 and 70 d after the lesion. Broken lines in b and c indicate the ventricular surface. Scale bars, 1 mm (a); 10 μm (b,c). (d) Proliferating cells in the subependymal zone visualized by PCNA immunoreactivity. Scale bar, 20 μm. (e) Optical density of DAT+ fibers (arbitrary units) in the striatum adjacent to the subependymal zone as a function of time after the lesion. ▪, MPTP; □, control. *P < 0.05 versus corresponding control (n ≥ 3 per group); ANOVA followed by post-hoc LSD test. (f) Stereologically determined number of PCNA+ cells per subependymal zone as a function of time after the lesion. *P < 0.05 versus corresponding control (n ≥ 3 per group); ANOVA followed by post-hoc LSD test. (g) Number of PCNA+ cells in the subependymal zone (percentage of corresponding control group mean) as a function of the optical density of DAT+ fibers (percentage of corresponding control group mean). The control shown represents the pooled values of all five control groups. Linear regression of the MPTP group means: n = 5, Pearson's R = 0.95, P < 0.05.
The stereologically determined number of subependymal zone cells expressing the cell-cycle marker proliferating cell nuclear antigen (PCNA)16 decreased significantly after denervation and recovered in parallel with the dopaminergic re-innervation during the next 70 d (Fig. 2d,f). There was a significant correlation between the number of PCNA+ cells in the subependymal zone and the density of DAT+ fibers (Fig. 2g).
D2L transmission stimulates subependymal zone proliferation
Because a transient and bilateral decrease in subependymal zone proliferation occurred after transient and bilateral dopaminergic denervation with MPTP, we predicted that persistent and unilateral depletion of dopamine might induce a persistent and unilateral reduction in proliferation that could be restored by dopaminergic pharmacotherapy. To test this prediction, we ablated the right mesencephalic dopaminergic neurons of adult rats by stereotaxic injection of the toxic dopamine analog 6-hydroxydopamine (6-OHDA) into the right nigrostriatal pathway. Ablation resulted in a unilateral dopaminergic denervation of the striatum and subependymal zone that persisted for 6 weeks after the lesion (Fig. 3a, lesion group). At this time point, the number of PCNA+ cells in the subependymal zone ipsilateral to the lesion was reduced to 66.3 ± 6.0% of the control value (P < 0.05), but unchanged on the unlesioned side (Fig. 3b–d, control and lesion groups).
The right nigrostriatal dopaminergic projection in adult rats was destroyed by unilateral stereotaxic injection of 6-OHDA in the nigrostriatal pathway. Controls were injected with NaCl. Lesioned rats were either untreated and killed 6 weeks after the lesion (lesion), treated continuously for 3 weeks with levodopa starting 3 weeks after the lesion and then killed (lesion plus levodopa), or injected with a single dose of the D2L agonist ropinirole before being killed 6 weeks after the lesion (lesion plus ropinirole). (a) Coronal sections of the anterior forebrain immunostained for tyrosine hydroxylase (TH) showing a severe depletion of dopaminergic fibers in the striatum ipsilateral to the 6-OHDA injection side 6 weeks after the lesion. Scale bar, 1 mm. (b) Adjacent sections showing the subependymal zone immunostained for PCNA. Scale bar, 500 μm. (c) Details of the boxed areas in b showing PCNA staining in the subependymal zone at higher magnification. Scale bar, 100 μm. (d) Stereologically determined number of PCNA+ cells per subependymal zone. ▪, left subependymal zone; □, right subependymal zone.*P < 0.05 versus control group and #P < 0.05 versus 6-OHDA side in the lesion group (n = 6 per group); ANOVA followed by post-hoc LSD test.
To determine whether dopaminergic pharmacotherapy restores proliferation, we continuously infused rats, starting 3 weeks after the lesion, for 3 weeks with levodopa, the physiological precursor of dopamine. This treatment did not change the number of PCNA+ cells in the subependymal zone on the unlesioned side as compared with the controls, but it significantly increased the number on the lesioned side, to 84.0 ± 1.6% of the control value (P < 0.05 versus lesioned side in rats without levodopa treatment; Fig. 3a–d, lesion + levodopa group).
To determine whether the induction of proliferation by levodopa was immediate and mediated by dopamine receptors, we injected rats 6 weeks after the lesion with a single dose of ropinirole before killing them. This selective D2L agonist was chosen because of the preferential expression of D2L receptors on C-cells. This treatment significantly increased the number of PCNA+ cells on both the unlesioned (ropinirole, 135.3 ± 7.2, P < 0.05) and lesioned (ropinirole, 115.7 ± 9.2%, P < 0.05; Fig. 3a–d, lesion + ropinirole group) side. Taken together, these data suggest that cell proliferation in the adult subependymal zone is under dopaminergic control.
D2L activation increases proliferation in neurospheres
To verify that the changes in subependymal zone proliferation occurring after manipulation of the dopaminergic system in vivo resulted from the direct action of dopamine on precursor cells, we analyzed the effects of activation of the dopamine receptor on precursors that were explanted from the subependymal zone of adult mice and grown as neurosphere cultures9,11. The cells in neurospheres expressed the EGFR and both D1L and D2L receptors (Fig. 4a,b).
(a,b) D1L (a) and D2L (b) receptors (green) are expressed on EGFR+ cells (red) in neurosphere cultures derived from the subependymal zone of adult mice, as assessed by confocal microscopy. Nuclei are stained with Hoechst 33342 (blue). (c–f) To assess the effect of dopaminergic stimulation on neural precursor cell proliferation in vitro, the BrdU labeling index (LI) was determined in neurosphere cultures after 12 h of exposure to BrdU plus the D1L agonist SKF 38393 (c), the D2L agonist bromocriptine (d), a combination of 1 μM bromocriptine and 1 μM sulpiride, a D2L antagonist (e) or dopamine (f). *P < 0.05 versus control (n = 3–8 per group); ANOVA followed by post-hoc LSD test.
The BrdU labeling index (the number of BrdU-labeled cells divided by the total number of cells) in cultures grown for 12 h in presence of BrdU was determined as a measure of proliferation7. A 12-h treatment of the cultures with the D1L agonist SKF 38393 (1–10 μM) did not change the BrdU labeling index (Fig. 4c). The D2L agonist bromocriptine increased the BrdU labeling index in a concentration-dependent manner (Fig. 4d). The D2L antagonist sulpiride (0.3–3 μM) did not affect the BrdU labeling index alone, but it prevented the bromocriptine-induced increase (Fig. 4e). Dopamine, acting on both the D1L and D2L receptors, also increased the BrdU labeling index (Fig. 4f). These observations suggest that activation of the D2L receptor directly stimulates the proliferation of EGFR+ subependymal zone cells.
Dopamine denervation reduces EGFR+ cell proliferation
To assess the consequences of dopaminergic denervation on the cellular composition of the subependymal zone, we analyzed the changes occurring in mice treated with MPTP. We first excluded the possibility that an increase in cell death might underlie the reduced number of proliferating subependymal zone cells after dopamine denervation, because the numbers of cells that were labeled in a TdT-mediated dUTP nick end labeling (TUNEL) assay, indicating apoptosis (Fig. 5a), or that contained chromatin clumps visualized by cresyl violet, indicating pyknosis (Fig. 5b), did not differ between control and MPTP-treated mice.
Cellular changes in the mouse subependymal zone were analyzed after dopaminergic denervation by MPTP. (a) Illustration and quantification of TUNEL+ cells (green). (b) Illustration and quantification of pyknotic cells, identified as cresyl violet–stained, round, well-defined chromatin clumps of irregular size. (c) Illustration and quantification of GFAP+ cells (red) expressing the proliferation marker PCNA (green) in their nuclei. (d) Illustration and quantification of EGFR+ cells (red) expressing PCNA (green) in their nuclei. (e) Illustration and quantification of PSA-NCAM+ cells (red) expressing PCNA (green) in their nuclei. In a,c–e, orthogonal reconstructions of confocal microscopic images in the x-y, x-z and y-z planes are shown and cell nuclei are stained with Hoechst 33342 (blue). Scale bars, 5 μm (a,c–e). *P < 0.05 versus control (n ≥ 3 per group); t-test. *P < 0.05 versus control (n ≥ 3 per group); t-test.
Furthermore, we excluded the possibility that the proliferation of B-cells was reduced during dopaminergic denervation, because neither the number of GFAP+ B-cells in the subependymal zone nor the percentage of GFAP+ B-cells with nuclear expression of the proliferation marker PCNA differed between control and MPTP-treated mice (Fig. 5c). The total number of EGFR+ cells also remained unchanged (Fig. 5d). However, the percentage of EGFR+ cells expressing PCNA decreased significantly (Fig. 5d), suggesting that the mitotic activity of EGFR+ cells was reduced after dopamine depletion.
Consistently, there was a significant decrease in PSA-NCAM+ A-cells, the cell type generated by asymmetric division of C-cells. The vast majority of EGFR+ cells are C-cells14. The percentage of A-cells expressing PCNA, however, remained unchanged (Fig. 5e). These data indicate that dopaminergic denervation may selectively reduce the generation of A-cells by C-cells.
Fewer neurons in olfactory bulb after dopamine denervation
Most newborn subependymal zone cells migrate to the olfactory bulb to form new neurons10, whereas others generate glia17 or die18. To determine whether dopaminergic denervation decreases neuroblast migration to the olfactory bulb, we treated mice with MPTP and labeled cells undergoing mitosis during the next 2 d with BrdU (eight injections of 50 mg/kg at 6-h intervals; Fig. 6a). Significantly fewer BrdU+ cells were present in the subependymal zone and RMS during severe dopaminergic denervation 2 d after MPTP treatment as compared with controls, confirming the reduction in proliferation determined by PCNA labeling (Fig. 6b,c,e,f). At the same time, the number of BrdU+ cells in the parietal cortex, which reflects spontaneous glial and endothelial proliferation, remained unchanged (MPTP, 27.9 ± 0.6 cells/mm3; control, 28.3 ± 1.3 cells/mm3), showing that the decrease in BrdU+ cell number in the subependymal zone was region-specific and not the consequence of a nonspecific overall reduction in proliferation or reduced bioavailability of BrdU.
(a) Experimental model. Dopaminergic fibers in mice were ablated by four injections of MPTP. Thereafter, mitotic cells were labeled by eight injections of BrdU over 48 h. Mice were killed either 2 or 21 d after the lesion. (b) BrdU+ cells were analyzed in the subependymal zone (SZ) and RMS 2 d after the lesion (1 h after the last BrdU injection) and in the granular layer of the olfactory bulb (OB) 21 d after the lesion. (c) Stereologically determined number of BrdU+ cells at the three anatomical levels in control (□) and MPTP mice (▪), expressed as a percentage of the control (absolute control values: SZ, 30,158 ± 1,323; RMS, 4,235 ± 140; OB, 29,508 ± 2,905). *P < 0.05 versus control (n ≥ 3 per group); t-test. (d) Absolute number of newborn neurons in the OB 21 d after MPTP injection, identified as BrdU+ NeuN+ cells by confocal microscopy. *P < 0.05 versus control (n ≥ 3); t-test. (e–g) Photomicrographs showing BrdU+ cells in the SZ (e), RMS (f) and OB (g) of control (left) and MPTP (right) mice, 2 d (e,f) and 21 d (g) after the lesion. S, septum; St, striatum; V, ventricle. Brightfield illumination was used in g to identify the contour of the granular layer; BrdU+ cells appear as bright spots. Boxed areas in e and g indicate the location of the details shown as insets. Scale bars, 50 μm (e, inset; f); 100 μm (g, inset); 200 μm (e,g).
After 3 weeks, 32.9% fewer BrdU+ cells had migrated to the olfactory bulb in MPTP-lesioned than in control mice (Fig. 6b,c,g), and 33.2% fewer newborn neurons had integrated into the olfactory bulb, as assessed by the colocalization of BrdU with the neuronal marker neuronal nuclear antigen (NeuN) by confocal microscopy (Fig. 6d).
Dopamine denervation affects hippocampal precursors
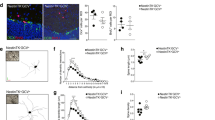
Neurogenesis also occurs in the subgranular zone of the hippocampus in adult mammals19. To assess whether progenitor cells in the subgranular zone are contacted by dopaminergic fibers, we injected mice with BrdU (eight injections of 50 mg/kg at 6-h intervals), killing them 1 h after the last injection, to label dividing cells before they had undergone neuronal differentiation. We identified DAT+ dopaminergic fibers in the subgranular zone of the dentate gyrus, where stem cells are located, but only sparse immunoreactivity in the adjacent hilus or granule cell layer (Fig. 7a). We found that DAT+ nerve endings (Fig. 7b) and TH+ fibers (Fig. 7c) contacted BrdU+ cells in the subgranular zone.
(a) DAT+ fibers (red) in the vicinity of BrdU+ cells (green) in the subgranular zone of the hippocampus of an adult mouse killed 1 h after BrdU injection. GCL, granule cell layer. Scale bar, 50 μm. (b,c) Laser scanning confocal images showing a DAT+ nerve ending (b, red, arrow) and TH+ nerve fibers (c, red) in the immediate vicinity of BrdU+ cells (green) in the subgranular zone. Scale bars, 3 μm. (d) Quantification of PCNA+ cells in the subgranular zone of control (□) and MPTP-treated mice (▪) killed after 1, 2, 7, 21 or 70 d. *P < 0.05 versus control (n ≥ 3 per group); ANOVA followed by post-hoc LSD test. (e) Photomicrographs of PCNA+ cells in the subgranular zone in a control mouse (C 1 d) and in MPTP-treated mice killed 2 d (M 2 d) or 70 d (M 70 d) after the lesion. Scale bar, 50 μm.
We analyzed the effect of dopaminergic denervation on proliferation in the subgranular zone in MPTP-treated mice. MPTP induced a complete loss of the DAT+ dopaminergic fibers in the subgranular zone that fully recovered within 70 d, as it did in the subependymal zone. Noradrenergic fibers positive for dopamine-β-hydroxylase in the dentate gyrus were not lost (data not shown). Proliferation in the subgranular zone, as assessed by counting PCNA+ cells, first decreased and then recovered in parallel with dopaminergic denervation and reinnervation, respectively (Fig. 7d,e). Taken together, these observations indicate that cell proliferation in the subgranular zone of the dentate gyrus may be also under dopaminergic control.
Fewer precursor cells in Parkinson disease
Because our experimental data suggested that adult neurogenesis might be impaired after dopamine depletion in rodent models of Parkinson disease, we determined whether the degeneration of dopaminergic neurons in individuals affected with Parkinson disease has similar consequences. We found EGFR+ cells in the normal human subependymal zone, located between the ependymal cell layer and the striatum with its dense dopaminergic innervation (Fig. 8a). Confocal microscopy showed that the close contact between dopaminergic fibers and EGFR+ cells is conserved in humans (Fig. 8b).
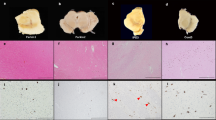
(a) EGFR+ cells are present in the human subependymal zone (SZ), located between the striatum (Str) and the ependymal cell layer (E), adjacent to the lateral ventricle (V), in the postmortem brain of an 84-year-old man who died with no neurological or psychiatric diseases. Scale bar, 20 μm. (b) Laser scanning confocal image showing a DAT+ nerve fiber contacting an EGFR+ cell, surrounded by GFAP+ astrocytic processes in the normal adult human SZ. Scale bar, 5 μm. (c) Representative photomicrographs showing PCNA+ cells in the human SZ of a control subject and an individual with PD (scale bar, 20 μm), and quantification of PCNA+ cells in the human SZ of the control and PD groups (n = 4 per group). *P < 0.05; t-test. (d) PSA-NCAM+ cells (arrows) in the normal adult human SZ. Note the absence of chain migration. Scale bar, 20 μm. (e) Individual PSA-NCAM+ cells are dispersed in the adult human olfactory bulb (OB; scale bar, 5 μm). PSA-NCAM+ cells in the OB coexpress nestin (scale bar, 2 μm). Quantification of nestin+ cells in the human OB of the control and PD groups (n = 4 per group). *P < 0.05; t-test. (f,g) The human dentate gyrus (DG) contains nestin+ cells and β-III-tubulin+ (b3T) cells (brown DAB precipitate). Nuclei are counterstained with cresyl violet. (f) Overview (scale bar, 50 μm) and detail showing the boxed area at higher magnification (scale bar, 10 μm), and quantification of nestin+ cells in the human DG of the control (n = 3), PD (n = 3) and PDD (n = 5) groups, expressed as thousands per mm3 of DG volume. (g) Overview showing two β-III-tubulin+ cells (arrows; scale bar, 40 μm) and detail showing the boxed area at higher magnification (scale bar, 10 μm), and quantification of β-III-tubulin+ cells in the human DG of the control (n = 3), PD (n = 3) and PDD (n = 5) groups, expressed as in f. *P < 0.05 and **P < 0.01 versus control; ANOVA followed by post-hoc LSD test.
To assess the influence of dopaminergic denervation on proliferation in humans, we compared the number of PCNA+ cells in the subependymal zone of individuals with clinically and pathologically diagnosed Parkinson disease and control subjects who had died without evidence of neurological or psychiatric disorders. The number of PCNA+ cells in the subependymal zone of individuals with Parkinson disease was reduced by 29.9% (P < 0.05, Fig. 8c).
We also found isolated PSA-NCAM+ cells in the human subependymal zone (Fig. 8d), suggesting the presence of migrating cells sharing similarity with the A-cells described in rodents. Isolated PSA-NCAM+ cells were also present in the human olfactory bulb (Fig. 8e). These PSA-NCAM+ cells coexpressed nestin, an intermediate filament characteristic of immature neural precursors20 (Fig. 8e), suggesting that neural precursors exist in the adult human olfactory bulb. The stereologically determined number of nestin+ precursors was reduced in the olfactory bulb of individuals with Parkinson disease (Fig. 8e).
Finally, we identified cells immunoreactive for nestin (Fig. 8f) and for β-III-tubulin, a marker for immature neurons (Fig. 8g), in the adult human dentate gyrus. We compared dentate gyri from control subjects, individuals with Parkinson disease without cognitive impairment, and individuals with Parkinson disease with dementia (PDD; Mini-Mental State Examination, 10.8 ± 2.0; range 5–15). The Parkinson disease and PDD groups did not differ significantly in the severity of their parkinsonian motor disability (unified Parkinson disease rating scale III score, 42.0 ± 17.6 versus 55.0 ± 8.3). Nestin+ cells in the dentate gyrus were reduced to 62.3 ± 15.4% (P < 0.05 versus control) in the Parkinson disease group and to 49.9 ± 5.3 % (P < 0.01) in the PDD group (Fig. 8f). Cells expressing β-III-tubulin were reduced to 67.5 ± 6.7% (P < 0.05) in the Parkinson disease and to 57.9 ± 8.3% (P < 0.01) in the PDD groups (Fig. 8g).
Discussion
We have shown that there are dopaminergic afferents in the adult mammalian subepen-dymal zone. We identified highly proliferative EGFR+ cells as the anatomical and functional targets of this dopaminergic innervation. Dopamine stimulated the proliferation of EGFR+ cells through D2L receptors. Dopamine seemed to control neuro-genesis in the dentate gyrus as well, as suggested by lesion experiments. We found that the dopaminergic innervation of EGFR+ subependymal zone cells is conserved in adult humans. Consistent with our experimental evidence showing that dopamine controls the proliferation of neural precursor cells, we found a reduction in mitotic activity in the subependymal zone and in the number of neural precursor cells in the olfactory bulb and dentate gyrus of individuals with Parkinson disease.
The origin of the dopamine fibers terminating in the subependymal zone remains to be precisely determined, but anterograde tracing in an adult primate has shown that they originate, at least in part, from the substantia nigra (C. François, personal communication). Dopaminergic fibers in the dentate gyrus have been described as originating in part from the substantia nigra but mainly from the ventral tegmental area21.
The EGFR+ cells were identified as a specific target of the dopaminergic afferents in the subependymal zone, on the basis of their frequent contacts with DAT+ synaptophysin+ axons. Most EGFR+ cells are transit-amplifying C-cells14: that is, highly proliferative intermediate precursors that generate neuroblasts12,13. Consistently, we found ultrastructural evidence for presynaptic dopaminergic structures apposed to C-cells and we have shown that C-cells express dopamine receptors, in particular receptors of the D2L subtype. The receptors were distributed diffusely on their plasma membranes, suggesting a paracrine mode of neurotransmission (volume transmission), which is typical of catecholamine signaling22.
Functionally, dopaminergic transmission in the subependymal zone seems to stimulate the proliferation of EGFR+ cells because, first, dopamine substitution increased the proliferation of subependymal zone–derived EGFR+ cells grown as neurospheres; and second, dopamine depletion reduced the proliferation of EGFR+ cells in living mice. This effect was mediated by D2L receptors because, first, a D2L-agonist increased proliferation in neurospheres; second, the effect was blocked by a D2L antagonist; and third, a D2L agonist restored proliferation in the dopamine-depleted subependymal zone of living rats. Levodopa was less effective in vivo, most probably because there were very few dopaminergic fibers left in the subependymal zone to transform levodopa into dopamine.
Previous studies have examined the effect of the dopamine receptor blocker haloperidol on neurogenesis. Haloperidol has been reported to decrease cell proliferation in the subependymal zone of early postnatal rats23, a finding compatible with our results suggesting that dopamine stimulates neurogenesis. Other studies have found no effect of haloperidol on neurogenesis in the adult rat subependymal zone24 or have reported an increase in neural progenitors in the adult rodent subependymal zone after chronic treatment with haloperidol (T.E. Kippin, S. Kapur and D. van der Kooy, Soc. Neurosci. Abstr. 753.10, 2003). With regard to precursor cell proliferation in the dentate gyrus, there are studies reporting an increase25, no effect26,27 or a decrease23 after haloperidol treatment. Although dopamine receptor blockade is the best known effect of haloperidol, this molecule also strongly activates sigma opiate receptors (which modulate NMDA glutamate receptors) and antagonizes α1-adrenergic and 5HT2-serotoninergic receptors. Because glutamate, noradrenaline and serotonin also influence progenitor cell proliferation in the adult mammalian brain28,29,30, haloperidol treatment may test more than just the effect of dopaminergic transmission, and the conflicting results reported in the literature may result from its many pharmacological properties.
The generation of new dopaminergic neurons in the substantia nigra of adult mice has been reported to occur spontaneously and to increase after MPTP lesion31. This lesion-induced phenomenon in the midbrain thus seems to be regulated differently from the forebrain neurogenesis that we analyzed and may depend on local signals generated by apoptotic cell death rather than on dopamine depletion.
There is now robust evidence for the presence of neural stem cells in the adult human subependymal zone, although there was no evidence of a massive chain migration of subependymal zone–derived precursors to the olfactory bulb32. It was concluded that precursors might not migrate from the subependymal zone to the olfactory bulb in humans or that they might migrate as individual cells32. Our observations confirm a previous report of the presence of individual neural precursors in the adult human olfactory bulb33, supporting the view that precursors in the olfactory bulb in adult humans may be rare in comparison to rodents, but not completely absent.
Most notably, our data indicate that the dopaminergic modulation of forebrain precursor proliferation may be conserved in adult humans: first, we found dopaminergic fibers contacting EGFR+ cells in the normal human subependymal zone; and second, we found reduced numbers of proliferating subependymal zone cells, neural precursors in the olfactory bulb, and neural precursors in the dentate gyrus in the brains of individuals with Parkinson disease, a disease characterized by the degeneration of the dopaminergic forebrain innervation originating in the substantia nigra and ventral tegmental area1,2. Because the individuals studied had all been treated with levodopa, the reduction in proliferation in drug-naive patients may be even more pronounced than the moderate decreases that we observed. It is thus likely that a subclinical depletion of dopamine in the early course of Parkinson disease, before the onset of motor symptoms, leads to a prolonged reduction in the generation of new neural cells in the diseased brain and may permanently alter its cytoarchitecture.
This raises the important issue of whether impaired generation of neural precursors may be clinically relevant to Parkinson disease. Evidence from experimental animals suggests that olfactory neurogenesis is implicated in the memorization of odors34,35. Hippocampal neurogenesis has been associated experimentally with the regulation of mood26,27 and mnestic functions36, particularly spatial memory37,38. However, those studies used rather acute experimental models, and the functional consequences of chronically impaired generation of adult precursors, as seems to occur in Parkinson disease, are not known. Intriguingly, olfactory dysfunction39, depression40 and impaired spatial memory41 are frequently observed in individuals with Parkinson disease and often occur before the onset of motor symptoms, which become apparent only after striatal dopamine levels have decreased by more than 70% (ref. 1).
With regard to olfactory dysfunction, impaired detection, identification and discrimination of odors affects more than 80% of people with Parkinson disease and coincides with the subclinical striatal depletion of dopamine39. Previous neuropathological examinations of the olfactory bulb of individuals with the disease have suggested continuous neurodegeneration42 and structural reorganization43 as a possible substrate of the hyposmia. Our data raise the possibility that chronic impairment of neural (neuronal or glial) regeneration might also contribute to olfactory impairment in Parkinson disease. Mnestic dysfunction, particularly that affecting spatial memory, occurs frequently and early in Parkinson disease41. Memory impairment or frank dementia have been associated with hippocampal atrophy in Parkinson disease44,45,46. Our data show that the number of neural precursors decreases in the dentate gyrus of individuals with Parkinson disease whether or not they have dementia. It is thus tempting to speculate that impaired neurogenesis may predispose individuals to the development of cognitive dysfunction during the course of Parkinson disease, although our data do not provide evidence for a functional implication of reduced neurogenesis in Parkinson disease symptoms.
In summary, we have shown that there is dopaminergic regulation of neural precursor cell proliferation in the adult mammalian brain, and that dopaminergic denervation may be responsible for the reduction in neural precursors observed in the brains of individuals with Parkinson disease. The neurobiological and clinical consequences of chronic reduction in neural precursors in Parkinson disease remain to be determined. However, the possibility of manipulating dopamine-regulated precursor cell proliferation by pharmacological means in humans opens exciting perspectives for the use of endogenous neural progenitor cells to repair the damaged brain.
Methods
Human brains.
Brains were obtained with written informed consent and in accordance with local law, and were dissected, fixed and frozen as described2. We cut coronal sections of the olfactory bulb (40 μm), subependymal zone (40 μm) and hippocampi (20 μm) on a freezing microtome in regularly spaced series. Four individuals with pathologically confirmed Parkinson disease and four individuals without neuropsychiatric disorders were matched for sex (50% females in each group), age (68.5 ± 3.2 versus 66.0 ± 11.1 years) and interval from death to tissue fixation (26.5 ± 4.8 versus 27.8 ± 10.5 h) to analyze the olfactory bulb and subependymal zone. Hippocampi were analyzed from three controls, three individuals with Parkinson disease and no cognitive impairment, and five individuals with Parkinson disease and cognitive dysfunction (Mini-Mental State Exam ≤15), who were matched for sex (66.6%, 66.6% and 40.0% females, respectively), age (87.7 ± 6.7, 71.3 ± 4.9 and 85.6 ± 5.0 years, respectively) and postmortem delay (31.5 ± 7.2, 25.1 ± 8.2 and 19.4 ± 5.9 h, respectively).
MPTP mice.
Mice were handled according to the European Union Council Directive 86/609/EEC. The appropriate ethical committee approved the experiments. Male C57BL/6J mice (CERJ), aged 10 weeks, received four injections of 10 mg/kg of MPTP (Sigma-Aldrich) or 0.9% NaCl (controls) intraperitoneally (i.p.) at 2-h intervals. Thereafter, mice received eight injections of 50 mg/kg of BrdU (Sigma) i.p. at 6-h intervals. MPTP-treated and control mice were killed at defined time points after the lesion (n ≥ 3 per group) with 100 mg/kg of pentobarbital i.p. and perfused transcardially with 50 ml of 0.1 M PBS and 100 ml of 4% paraformaldehyde. Brains were postfixed, frozen and cut on a freezing microtome (20 μm). We collected regularly spaced series of coronal sections containing the olfactory bulb, RMS, subependymal zone and adjacent striatum, hippocampi and substantia nigra.
6-OHDA-treated rats.
Under ketamine anesthesia (150 mg/kg), male Sprague-Dawley rats (CERJ), weighing 250–350 g, were injected stereotaxically with 6 μg of 6-OHDA (Sigma) stabilized with 0.2 μg/μl of L-ascorbate (lesion groups) or L-ascorbate in saline (controls) into the right nigrostriatal pathway (2.2 mm caudal, 1.9 mm lateral to bregma, 8.4 mm ventral to the skull surface). Thirty minutes earlier, they had received 25 mg/kg of desipramine (Sigma) to protect noradrenergic neurons. Lesioned rats were included only when loss of striatal tyrosine hydrolase immunoreactivity, measured post mortem, exceeded 90% (n = 6 per group). Three weeks after the lesion, we implanted 2ML4 minipumps (Alzet), which subcutaneously delivered 100 mg/kg/d of levodopa methyl ester (Chiesi) stabilized by 25 mg/kg/d of benserazide (Roche) and 0.02% L-ascorbate (lesion + levodopa group). Other rats received 3 mg/kg of ropinirole (GlaxoSmithKline; lesion + ropinirole group) 6 weeks after the lesion. The doses of levodopa and ropinirole were higher than those used in humans, but were standard for the rat. Six weeks after the lesion (3 weeks after pump implantation or 45 min after ropinirole injection), all rats were perfused and processed as described for MPTP mice. We cut 40-μm sections containing the subependymal zone and the adjacent striatum.
Neurosphere cultures.
Tissue containing the subventricular zone was dissected from the brains of 8-week-old SWISS mice (CERJ), incubated in L15 medium containing 10 U/ml of papain, 0.2 mg/ml of cysteine, 0.2 mg/ml of EDTA and 100 U/ml of DNase I on a rocking platform (30 min, 37 °C) and dissociated mechanically in DMEM/F-12 medium (Invitrogen) containing 0.7 mg/ml of ovomucoid (Sigma). Cells were grown in DMEM/F-12 medium supplemented with B27 (Invitrogen), 20 ng/ml of epidermal growth factor and 10 ng/ml of basic fibroblast growth factor (PeproTech). After 1 week, the primary neurospheres were dissociated mechanically, seeded at a density of 60 cells per μl in DMEM/F-12 medium containing B27 and 5 ng/ml EGF, and allowed to rest for 12 h. They were then exposed to 5 μM BrdU (Sigma) and dopamine receptor agonists or antagonists for 12 h, and fixed with 4% paraformaldehyde.
Immunohistochemistry.
Free-floating brain sections or neurosphere cultures were incubated (12 h, 4 °C) with the following primary antibodies in 0.1 M PBS, 0.2% Triton X-100 and 5% normal goat serum: rabbit anti–tyrosine hydroxylase, diluted 1/500 (Pel Freez); rabbit anti–rodent DAT, 1/100; rabbit anti–human DAT, 1/200; rabbit anti–dopamine β-hydroxylase, 1:500; mouse anti-NeuN, 1/1,000 (Chemicon); rat anti-BrdU, 1/200 (ImmunologicalsDirect); mouse anti-synaptophysin, 1/200; mouse anti-GFAP, 1/500; mouse anti–β-III-tubulin, 1/500 (Sigma); sheep anti-EGFR, 1/50 (Upstate Biotech); rabbit anti-GFAP, 1/1,000; mouse anti-PCNA, 1/500 (DAKO); mouse anti–PSA-NCAM, 1/1,000 (a gift of G. Rougon, Marseille, France); rabbit anti–human nestin, 1/1,000 (a gift of U. Lendahl, Stockholm, Sweden); rabbit anti–D1L receptor, 1/1,000 (a gift of B. Bloch, Bordeaux, France); and rabbit anti–D2L receptor, 1/200 (a gift of P. Vernier, Gif-sur-Yvette, France). Samples were pretreated with 2 N HCl (37 °C, 20 min) for BrdU detection or with 70% ethanol (−20 °C, 30 min) for PCNA detection. We visualized antibodies by the diaminobenzidine (DAB) method (Vectastain) or with fluorescent secondary antibodies: Cy3-, Cy5- or 5-(4,6-dichlorotriazinyl)aminofluorescein (DTAF)-conjugated anti–rabbit, anti–mouse, anti–sheep or anti–rat IgG; fluorescein isothiocyanate (FITC)-conjugated anti–mouse IgM, diluted 1/500 (Jackson ImmunoResearch); and Alexa Fluor 488–conjugated anti–mouse or rabbit IgG, 1/500 (Molecular Probes). Nuclei were stained with Hoechst 33342.
TUNEL assay.
Apoptotic nuclei were detected using an ApopTag TUNEL kit (Serologicals).
Image analysis.
The following cell counts were done on regularly spaced sections by using a semiautomatic stereology system (ExploraNova Mercator): PCNA+ or BrdU+ cells in the subependymal zone (defined from 2.4 to −0.8 mm relative to bregma)47, RMS (5.2 to 3.0 mm), olfactory bulb (7.4 to 5 mm) and dentate gyrus (−3.3 to −4.5 mm) of mice; PCNA+ cells in the rat subependymal zone (0.4 to 1.0 mm)48; and nestin+ cells along the whole rostrocaudal extent of the human olfactory bulb. We counted PCNA+ cells in the human subependymal zone from the corpus callosum to the vena thalamostriata on coronal sections taken at the level of the anterior commissure, to assure identical anatomical levels in all subjects. Nestin+ and β-III-tubulin+ cells were counted in the granular and subgranular zone of the human dentate gyrus. The optical density of striatal DAT+ fibers was quantified under bright-field illumination by the Mercator software. Pyknotic profiles in the subependymal zone were identified as cresyl violet–stained, round chromatin clumps of irregular size. Quantification of TUNEL+, GFAP+, EGFR+ and PSA-NCAM+ cells in the subependymal zone and colocalization with PCNA, as well as NeuN-BrdU colocalization along the rostrocaudal extent of the OB, were done with a Leica TCS SP2 AOBS confocal microscope, equipped with a Coherent multiphoton laser. We used three-dimensional reconstruction to verify colocalization in the x-y, x-z and y-z planes.
Electron microscopy.
Brain sections of untreated male Sprague-Dawley rats (CERJ) were immunolabeled with rabbit anti–D1L receptor, diluted 1/1,000 (a gift of B. Bloch), rabbit anti–D2L receptor, 1/200 (a gift of P. Vernier), and rabbit anti–tyrosine hydrolase, 1/500 (Pel Freez). Receptor antibodies were detected with a gold-coupled secondary antibody, particle size 0.8 nm, diluted 1/50 (Aurion), and tyrosine hydrolase antibodies were detected by the DAB technique. Ultrathin sections (50 nm) were analyzed on a JEOL 1200EXII electron microscope with Analysis Docu software (Soft Imaging System). No labeling was observed when the primary antibodies were omitted.
Statistics.
All data are reported as the mean ± s.e.m. Normal, parametric data were compared by a two-sided, unpaired t-test or by analysis of variance (ANOVA) followed by the post-hoc least significant difference (LSD) test. Pearson's correlation (R) was calculated for linear regression analysis. A value of P < 0.05 was considered to be statistically significant.
References
Bernheimer, H., Birkmayer, W., Hornykiewicz, O., Jellinger, K. & Seitelberger, F. Brain dopamine and the syndromes of Parkinson and Huntington. Clinical, morphological and neurochemical correlations. J. Neurol. Sci. 20, 415–455 (1973).
Hirsch, E., Graybiel, A.M. & Agid, Y.A. Melanized dopaminergic neurons are differentially susceptible to degeneration in Parkinson's disease. Nature 334, 345–348 (1988).
Cameron, H.A., Hazel, T.G. & McKay, R.D. Regulation of neurogenesis by growth factors and neurotransmitters. J. Neurobiol. 36, 287–306 (1998).
Lidow, M.S. & Rakic, P. Neurotransmitter receptors in the proliferative zones of the developing primate occipital lobe. J. Comp. Neurol. 360, 393–402 (1995).
Diaz, J. et al. Selective expression of dopamine D3 receptor mRNA in proliferative zones during embryonic development of the rat brain. J. Neurosci. 17, 4282–4292 (1997).
Ohtani, N., Goto, T., Waeber, C. & Bhide, P.G. Dopamine modulates cell cycle in the lateral ganglionic eminence. J. Neurosci. 23, 2840–2850 (2003).
Alvarez-Buylla, A., Garcia-Verdugo, J.M. & Tramontin, A.D. A unified hypothesis on the lineage of neural stem cells. Nat. Rev. Neurosci. 2, 287–293 (2001).
Reynolds, B.A. & Weiss, S. Generation of neurons and astrocytes from isolated cells of the adult mammalian central nervous system. Science 255, 1707–1710 (1992).
Luskin, M.B. Restricted proliferation and migration of postnatally generated neurons derived from the forebrain subventricular zone. Neuron 11, 173–189 (1993).
Morshead, C.M. et al. Neural stem cells in the adult mammalian forebrain: a relatively quiescent subpopulation of subependymal cells. Neuron 13, 1071–1082 (1994).
Doetsch, F., Caille, I., Lim, D.A., Garcia-Verdugo, J.M. & Alvarez-Buylla, A. Subventricular zone astrocytes are neural stem cells in the adult mammalian brain. Cell 97, 703–716 (1999).
Doetsch, F., Garcia-Verdugo, J.M. & Alvarez-Buylla, A. Cellular composition and three-dimensional organization of the subventricular germinal zone in the adult mammalian brain. J. Neurosci. 17, 5046–5061 (1997).
Doetsch, F., Petreanu, L., Caille, I., Garcia-Verdugo, J.M. & Alvarez-Buylla, A. EGF converts transit-amplifying neurogenic precursors in the adult brain into multipotent stem cells. Neuron 36, 1021–1034 (2002).
Przedborski, S. & Vila, M. The 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine mouse model: a tool to explore the pathogenesis of Parkinson's disease. Ann. NY Acad. Sci. 991, 189–198 (2003).
Curtis, M.A. et al. Increased cell proliferation and neurogenesis in the adult human Huntington's disease brain. Proc. Natl. Acad. Sci. USA 100, 9023–9027 (2003).
Nait-Oumesmar, B. et al. Progenitor cells of the adult mouse subventricular zone proliferate, migrate and differentiate into oligodendrocytes after demyelination. Eur. J. Neurosci. 11, 4357–4366 (1999).
Morshead, C.M. & van der Kooy, D. Postmitotic death is the fate of constitutively proliferating cells in the subependymal layer of the adult mouse brain. J. Neurosci. 12, 249–256 (1992).
van Praag, H. et al. Functional neurogenesis in the adult hippocampus. Nature 415, 1030–1034 (2002).
Lendahl, U., Zimmerman, L.B. & McKay, R.D. CNS stem cells express a new class of intermediate filament protein. Cell 60, 585–595 (1990).
Gasbarri, A., Sulli, A. & Packard, M.G. The dopaminergic mesencephalic projections to the hippocampal formation in the rat. Prog. Neuropsychopharmacol. Biol. Psychiatry 21, 1–22 (1997).
Ridet, I. & Privat, A. Volume transmission. Trends Neurosci. 23, 58–59 (2000).
Backhouse, B., Barochovsky, O., Malik, C., Patel, A.J. & Lewis, P.D. Effects of haloperidol on cell proliferation in the early postnatal rat brain. Neuropathol. Appl. Neurobiol. 8, 109–116 (1982).
Wakade, C.G., Mahadik, S.P., Waller, J.L. & Chiu, F.C. Atypical neuroleptics stimulate neurogenesis in adult rat brain. J. Neurosci. Res. 69, 72–79 (2002).
Dawirs, R.R., Hildebrandt, K. & Teuchert-Noodt, G. Adult treatment with haloperidol increases dentate granule cell proliferation in the gerbil hippocampus. J. Neural. Transm. 105, 317–327 (1998).
Malberg, J.E., Eisch, A.J., Nestler, E.J. & Duman, R.S. Chronic antidepressant treatment increases neurogenesis in adult rat hippocampus. J. Neurosci. 20, 9104–9110 (2000).
Santarelli, L. et al. Requirement of hippocampal neurogenesis for the behavioral effects of antidepressants. Science 301, 805–809 (2003).
Cameron, H.A., McEwen, B.S. & Gould, E. Regulation of adult neurogenesis by excitatory input and NMDA-receptor activation in the dentate gyrus. J. Neurosci. 15, 4687–4692 (1995).
Brezun, J.M. & Daszuta, A. Depletion in serotonin decreases neurogenesis in the dentate gyrus and the subventricular zone of adult rats. Neuroscience 89, 999–1002 (1999).
Kulkarni, V.A., Jha, S. & Vaidya, V.A. Depletion of norepinephrine decreases the proliferation, but does not influence the survival and differentiation, of granule cell progenitors in the adult rat hippocampus. Eur. J. Neurosci. 16, 2008–2012 (2002).
Zhao, M. et al. Evidence for neurogenesis in the adult mammalian substantia nigra. Proc. Natl. Acad. Sci. USA 100, 7925–7930 (2003).
Sanai, N. et al. Unique astrocyte ribbon in adult human brain contains neural stem cells but lacks chain migration. Nature 427, 740–744 (2004).
Liu, Z. & Martin, L.J. Olfactory bulb core is a rich source of neural progenitor and stem cells in adult rodent and human. J. Comp. Neurol. 459, 368–391 (2003).
Rochefort, C., Gheusi, G., Vincent, J.D. & Lledo, P.M. Enriched odor exposure increases the number of newborn neurons in the adult olfactory bulb and improves odor memory. J. Neurosci. 22, 2679–2689 (2002).
Scotto-Lomassese, S. et al. Suppression of adult neurogenesis impairs olfactory learning and memory in an adult insect. J. Neurosci. 23, 9289–9296 (2003).
Shors, T.J. et al. Neurogenesis in the adult is involved in the formation of trace memories. Nature 410, 372–376 (2001).
Nilsson, M., Perfilieva, E., Johansson, U., Orwar, O. & Eriksson, P.S. Enriched environment increases neurogenesis in the adult rat dentate gyrus and improves spatial memory. J. Neurobiol. 39, 569–578 (1999).
Drapeau, E., et al. Spatial memory performances of aged rats in the water maze predict levels of hippocampal neurogenesis. Proc. Natl. Acad. Sci. USA 100, 14385–14390 (2003).
Berendse, H.W. et al. Subclinical dopaminergic dysfunction in asymptomatic Parkinson's disease patients' relatives with a decreased sense of smell. Ann. Neurol. 50, 34–41 (2001).
Oertel, W.H. et al. Depression in Parkinson's disease. An update. Adv. Neurol. 86, 373–383 (2001).
Pillon, B. et al. Memory for spatial location in 'de novo' parkinsonian patients. Neuropsychologia 35, 221–228 (1997).
Braak, H. et al. Staging of brain pathology related to sporadic Parkinson's disease. Neurobiol. Aging 24, 197–211 (2003).
Hoogland, P.V., van den Berg, R. & Huisman, E. Misrouted olfactory fibres and ectopic olfactory glomeruli in normal humans and in Parkinson and Alzheimer patients. Neuropathol. Appl. Neurobiol. 29, 303–311 (2003).
Laakso, M.P. et al. Hippocampal volumes in Alzheimer's disease, Parkinson's disease with and without dementia, and in vascular dementia: an MRI study. Neurology 46, 678–681 (1996).
Riekkinen, P. Jr. et al. Hippocampal atrophy is related to impaired memory, but not frontal functions in non-demented Parkinson's disease patients. NeuroReport 9, 1507–1511 (1998).
Camicioli, R. et al. Parkinson's disease is associated with hippocampal atrophy. Mov. Disord. 18, 784–790 (2003).
Franklin, B.J. & Paxinos, G.T. The Mouse Brain in Stereotaxic Coordinates (Academic, London, 1996).
Paxinos, G.T. & Watson, C. The Rat Brain in Stereotaxic Coordinates (Academic, London, 1998).
Acknowledgements
We thank B. Mathieu and C. Cappe for technical assistance and M. Ruberg for discussions. This work was funded by the Institut National de la Santé et de la Recherche Médicale, the Deutsche Forschungsgemeinschaft (ho2402/2-1), the Fondation pour la Recherche Médicale (ACE20030307094), the Peter Hofmann research project and the Parkinson's Disease Foundation–National Parkinson Foundation Joint Research Grant Program.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Höglinger, G., Rizk, P., Muriel, M. et al. Dopamine depletion impairs precursor cell proliferation in Parkinson disease. Nat Neurosci 7, 726–735 (2004). https://doi.org/10.1038/nn1265
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nn1265
This article is cited by
-
A Diagnostic Model for Parkinson’s Disease Based on Anoikis-Related Genes
Molecular Neurobiology (2023)
-
Restoration of Adult Neurogenesis by Intranasal Administration of Gangliosides GD3 and GM1 in The Olfactory Bulb of A53T Alpha-Synuclein-Expressing Parkinson’s-Disease Model Mice
Molecular Neurobiology (2023)
-
The ventricular-subventricular, subgranular and subcallosal zones: three niches of neural stem cells in the postnatal brain
Experimental Brain Research (2023)
-
The Dialogue Between Neuroinflammation and Adult Neurogenesis: Mechanisms Involved and Alterations in Neurological Diseases
Molecular Neurobiology (2023)
-
Fecal Microbiota Transplantation from Aged Mice Render Recipient Mice Resistant to MPTP-Induced Nigrostriatal Degeneration Via a Neurogenesis-Dependent but Inflammation-Independent Manner
Neurotherapeutics (2023)