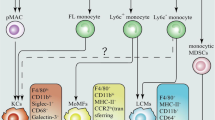
Abstract
Until now, the Food and Drug Administration (FDA)-approved iron supplement ferumoxytol and other iron oxide nanoparticles have been used for treating iron deficiency, as contrast agents for magnetic resonance imaging and as drug carriers. Here, we show an intrinsic therapeutic effect of ferumoxytol on the growth of early mammary cancers, and lung cancer metastases in liver and lungs. In vitro, adenocarcinoma cells co-incubated with ferumoxytol and macrophages showed increased caspase-3 activity. Macrophages exposed to ferumoxytol displayed increased mRNA associated with pro-inflammatory Th1-type responses. In vivo, ferumoxytol significantly inhibited growth of subcutaneous adenocarcinomas in mice. In addition, intravenous ferumoxytol treatment before intravenous tumour cell challenge prevented development of liver metastasis. Fluorescence-activated cell sorting (FACS) and histopathology studies showed that the observed tumour growth inhibition was accompanied by increased presence of pro-inflammatory M1 macrophages in the tumour tissues. Our results suggest that ferumoxytol could be applied ‘off label’ to protect the liver from metastatic seeds and potentiate macrophage-modulating cancer immunotherapies.
Similar content being viewed by others
Main
Iron oxide nanoparticles have been widely used as contrast agents and drug carriers in preclinical and clinical settings1,2,3,4,5. We recently revealed a hidden intrinsic therapeutic effect of the FDA-approved iron oxide nanoparticle compound ferumoxytol on ‘untreated’ tumours: tumour cells co-injected with ferumoxytol exhibited a markedly delayed growth rate compared with tumour cells injected without addition of ferumoxytol. Here, we elucidate pathophysiological mechanisms that led to the observed tumour growth inhibition by ferumoxytol.
It is well known that systemically or locally administered nanoparticles are internalized by tumour-associated macrophages (TAMs) in the tumour microenvironment2. This effect has been utilized to image tumour response to immune-modulating cancer therapies with diagnostic nanoparticles3,4,6 or to shuttle nanoparticle-conjugated therapeutic drugs to tumours7,8. However, the intrinsic impact of nanoparticles on macrophage physiology is not well understood. We hypothesized that ferumoxytol nanoparticles inhibited cancer growth by inducing a pro-inflammatory immune response with M1 macrophage polarization. Since iron oxide nanoparticles are increasingly used in clinical practice for cancer diagnosis9, cancer therapy10 and anaemia treatment11, effects of nanoparticles on the tumour microenvironment would have immediate and broad clinical implications.
Results
Effects of ferumoxytol on cancer cells and macrophages in vitro
We incubated several malignant and non-malignant cell types with ferumoxytol (0–30 mg ml–1) for 24 h, and measured cell death via caspase-3/7 activity. The results revealed no direct cytotoxic effects of ferumoxytol at 3 mg Fe ml–1 (Supplementary Fig. 1), which is equivalent to locally administered doses in vivo (2.73 mg Fe ml–1, see below) and the calculated plasma concentration after a typical intravenous injection of 5–10 mg kg–1 in rodents12. MMTV PyMT-derived mammary carcinoma cells did not exhibit any significant change in caspase-3 expression up to 12 mg Fe ml–1 ferumoxytol. Thus, ferumoxytol demonstrated no direct cytotoxic effects on cancer cells at clinically relevant doses.
To determine whether ferumoxytol nanoparticles attract macrophages, we investigated their chemotactic properties in vitro13. It has been previously reported that nanoparticles attract alveolar macrophages14. Using a dual-chamber transwell system with 3-µm-sized microporous membranes (macrophages are able to migrate through 3-µm pores), we evaluated the migration of DiD-labelled macrophages towards ferumoxytol nanoparticles, malignant cells, or both (Supplementary Fig. 2). Ferumoxytol and tumour cells attracted macrophages, and their combination led to an additive effect on macrophage recruitment (P < 0.05).
It has been reported that pro-inflammatory M1 macrophages in wounds release hydrogen peroxides, which elicit iron to generate highly toxic hydroxyl radicals (OH•) via the Fenton reaction15. To investigate if the Fenton reaction occurred in our co-cultures, we measured the level of reactive oxygen species (ROS) and cancer cell apoptosis in co-cultures of MMTV-PyMT cancer cells and macrophages, incubated with or without ferumoxytol. We found significantly increased caspase-3 expression by cancer cells incubated with macrophages plus ferumoxytol, compared with cancer cells incubated with either macrophages or ferumoxytol alone (P < 0.05; Fig. 1a–c). Co-cultures of cancer cells, macrophages and ferumoxytol demonstrated an 11-fold increase in hydrogen peroxide and a 16-fold increase in hydroxyl radical production compared with co-cultures of cancer cells and macrophages alone (P < 0.05; Fig. 1d,e). Thus, ferumoxytol enhances the production of ROS by macrophages, which increases cancer cell cytotoxicity.
RAW264.7 macrophages were co-cultured with MMTV-PyMT cancer cells in a transwell system for 24 h, with or without ferumoxytol (2.73 mg ml–1). Macrophages in the upper chamber and cancer cells in the lower chamber were separated by a 0.4-µm-sized microporous membrane, which allowed for exchange of molecules, but not cells. Cancer cells in the lower chamber were stained for caspase expression using green fluorescent protein (GFP)-conjugated antibodies against active caspase 3 (green). F-actin and the cell nuclei were counterstained with phalloidin rodamine (red) and DAPI (blue), respectively. a, Co-culture of cancer cells, macrophages and ferumoxytol leads to increased caspase-3 expression of cancer cells. Co-incubations of cancer cells and macrophages only or cancer cells and ferumoxytol only do not lead to significant apoptosis induction. Scale bars, 20 µm. b, Corresponding quantitative data, displayed as mean data of three experiments per experimental group and standard deviation. Apoptotic cancer cell counts in each experiment were averaged from 15–20 fields of view (FOV) using a fluorescence microscope. c, Graph shows corresponding quantitative data after co-incubation of mouse bone-marrow-derived macrophages and MMTV-PyMT tumour cells under the same conditions as described above. d,e, Pro-inflammatory M1 macrophages release hydrogen peroxides, which elicit iron to generate highly toxic hydroxyl radicals: graph shows quantitative measures of hydrogen peroxide (d) and hydroxyl radicals (e) in above-mentioned co-cultures, as determined with colorimetric hydrogen peroxide and hydroxyphenyl fluorescein (HPF) detection kits. f, Co-culture of cancer cells, macrophages and ferumoxytol show signs of pro-inflammatory macrophage activation: TNFa gene expression of cells shown in a and b, as measured by quantitative RT-PCR (qRT-PCR). g,h, Macrophages in co-cultures with cancer cells and ferumoxytol demonstrated increased TNFa expression (g) and decreased IL-10 secretion (h) compared with controls. All data are representative of at least three (N = 3) independent experiments for each experimental group and are displayed as mean ± standard deviation. *P < 0.05, indicates statistically significant difference (Student's t-test).
Next, we treated cancer cells in the bottom chamber with 100 µM caspase-3 inhibitor to block apoptosis and noted a six- and sevenfold decrease in hydrogen peroxide and hydroxyl radicals, respectively (Fig. 1d,e). This suggests an additive effect of dying cancer cells on macrophage activation and ROS production.
To further determine if ferumoxytol nanoparticles induce M1 macrophages, we isolated macrophages from above described co-cultures and audited their transcriptomes for expression differences of M1- versus M2-type mRNAs via quantitative real-time polymerase chain reaction (RT-PCR). This analysis revealed that ferumoxytol-exposed macrophages upregulated M1-related TNFα and CD86 markers (Fig. 1f) significantly compared with macrophages only (P < 0.05). In addition, mRNA levels of M2-related CD206 and IL10 markers were significantly decreased after exposure to ferumoxytol (P < 0.05). Similarly, an ELISA (enzyme-linked immunosorbent assay) of ferumoxytol-exposed cancer cell and macrophage co-cultures demonstrated a significantly increased production of tumour-necrosis factor-α (TNFα), a classical M1 marker (Fig. 1g, P = 0.021), but no significant production of M2-related interleukin-10 (IL-10) (Fig. 1h). This suggests that ferumoxytol-induced cancer cytotoxicity is coupled to M1 macrophage polarization.
In vivo inhibition of mammary tumour growth
To determine if ferumoxytol exposure would impact tumour growth in vivo, we implanted 2.3 × 106 MMTV-PyMT-derived cancer cells into the bilateral mammary fat pads of female FVB/N mice, with or without addition of ferumoxytol (2.73 mg Fe ml–1; group 1, see Methods). We found significantly suppressed tumour growth (57% at 21 days post-inoculation; P = 0.038) of ferumoxytol co-implanted cancer cells compared with non-ferumoxytol-treated controls (Fig. 2a). Tumour growth inhibition was the same for both high (8.37 mg Fe ml–1; group 2) and low (2.73 mg Fe ml–1; group 1) concentrations of ferumoxytol (tumour size 53% at day 21 compared with controls; Fig. 2a) (P = 0.070). Tumour growth was suppressed by ferumoxytol, without significant dose response at the given concentrations.
Mice were implanted with 2.3 × 106 MMTV-PyMT-derived cancer cells in the mammary fat pad with and without ferumoxytol. a, Ferumoxytol inhibited tumour growth compared with untreated controls at two different local Fe concentrations of 2.73 mg Fe ml–1 (n = 7 mice) and 8.37 mg Fe ml–1 (n = 7 mice). Data are displayed as mean tumour volume of seven tumours per group. b, Tumour growth was significantly inhibited compared with untreated controls by two different iron oxide nanoparticle compounds, ferumoxytol (n = 7 mice) and ferumoxytran-10 (n = 7 mice). No significant tumour growth inhibition was observed after injection of dextran only (negative control). Data are displayed as mean tumour volume of seven tumours per group. In a,b, error bars represent standard deviation. c, To exclude cross-talk of two tumours in the same mouse, mice were either implanted unilaterally or bilaterally with 2.3 × 106 MMTV-PyMT-derived cancer cells in the mammary fat pad, with and without co-implantation of ferumoxytol at a concentration of 2.73 mg Fe ml–1. Each data point represents the mean tumour volume of seven mice ± standard deviation. No significant difference in tumour volume was observed between mice inoculated unilaterally and those inoculated bilaterally. One-way ANOVA was used to compare data of ferumoxytol-treated groups and controls (P < 0.05, n = 7 mice per group). d, Corresponding serial quantitative MR signal of ferumoxytol-co-implanted and untreated cancer inoculation sites, as quantified by mean T2* relaxation rates of seven tumours in each group and standard deviation. Paraspinal muscle served as internal control. A slow decline in T2* shortening at the co-implantation site, apparently due to local iron metabolization, coincides with tumour growth. e, Corresponding representative T2*-weighted axial gradient echo MR images. Red arrows indicate ferumoxytol-induced negative (dark) T2* signal effects at cancer-ferumoxytol co-implantation sites and black arrows indicate lack of T2* signal effects at cancer implantation only sites. Tumour growth is delayed at the ferumoxytol-cancer cell co-implantion site. One-way ANOVA was used to compare results of different experimental groups for statistically significant difference (P < 0.05).
To investigate the possible role of the carboxymethyldextran coating of ferumoxytol nanoparticles, we compared tumour growth inhibition effects of ferumoxytol with the dextran-coated nanoparticle compound ferumoxtran-10 (Sinerem/Combidex, group 3). Results showed significant tumour growth inhibition of both ferumoxytol- and ferumoxytran-10 co-implanted cancer cells when compared with controls (P < 0.05; Fig. 2b) without any significant difference between the two compounds (P > 0.05). Additional mice were co-implanted with low-molecular-weight dextran (50 mg ml–1) and cancer cells (group 7, see Methods). Results showed no significant effect of iron-free dextran on tumour growth inhibition when compared with untreated controls (P > 0.05; Fig. 2b). Therefore, the coating of ferumoxytol does not play a significant role in tumour inhibition.
It has been reported that when multiple tumours are present in the same subject, one tumour can affect another tumour's growth through competition for vascular supply and the expression of cytokines and growth factors16. To exclude the possibility of cross-talk between multiple tumours within the same animal, 14 FVB/N mice received unilateral injections of either 2.3 × 106 MMTV-PyMT-derived cancer cells (n = 7 mice) or cancer cells plus 100 µl of ferumoxytol (2.73 mg Fe ml–1; n = 7 mice) into the mammary fat pad of the left lower abdomen (group 4, see Methods). Results confirmed significant growth inhibition of cancer cells co-implanted with ferumoxytol compared with cancer cells alone (P < 0.05; Fig. 2c). Within each group, there was no significant difference in tumour volumes of mice with unilateral or bilateral tumours (P > 0.05).
To evaluate if ferumoxytol co-injection could completely suppress tumour growth, we implanted decreasing quantities of MMTV-PyMT-derived cancer cells (2.3, 1, 0.1 and 0.01 × 106) with ferumoxytol at a concentration of 2.73 mg Fe ml–1 into 21 additional mice (group 5, see Methods). Tumour formation was investigated by near-infrared fluorescence optical imaging using the IVIS Spectrum optical imaging system at 2, 7, 14 and 21 days, followed by histopathological evaluation. We found significant tumour growth inhibition for all ferumoxytol-treated mice compared with untreated controls, with maximum tumour growth inhibition for the lowest quantity of ferumoxytol-exposed cancer cells (0.01 × 106; Supplementary Fig. 3).
Ferumoxytol nanoparticles can be detected and quantified with magnetic resonance (MR) imaging based on their effects on tissue T2* relaxation times17. To correlate tumour growth inhibition with ferumoxytol metabolization, we measured T2* relaxation times of ferumoxytol-co-implanted MMTV-PyMT cancers and controls (group 1, see Methods). Local administration of ferumoxytol induced a marked hypointense (dark) signal effect at the implantation sites on T2*-weighted MR images (Fig. 2e), which was significantly lower than the T2* signal of ipsilateral muscle (P < 0.05) and contralateral control cancers (P < 0.05). T2* relaxation times at the co-implantation sites increased gradually over 21 days after ferumoxytol administration (P < 0.05), which coincided with slow iron metabolization and developing tumours (Fig. 2d). Thus, the inhibitory effect of ferumoxytol on cancer growth is limited by ferumoxytol metabolism.
Ferumoxytol-treated tumours and untreated controls (group 1, see Methods), were evaluated by multicolour flow cytometry and immunofluorescence. Immunofluorescence analysis of tumour sections obtained at day 7 after implantation showed increased presence of CD80+ cells within ferumoxytol-co-implanted tumours compared with controls, representing increased quantities of pro-inflammatory M1 macrophages in ferumoxytol-co-implanted cancers (Fig. 3a,d). Later-stage tumours, 21 days after implantation, demonstrated high quantities of CD206+ cells in both ferumoxytol-treated and untreated cancers (Fig. 3b,d), suggesting an M2-type macrophages in the ferumoxytol-treated group.
a,b, Representative immunofluorescence stainings for CD11b (red), CD206 (red) and CD80 (green) of MMTV-PyMT tumour sections obtained at 7 days (a) and 21 days (b) after implantation of 2.3 × 106 cancer cells with or without ferumoxytol (2.73 mg Fe ml–1). Scale bars, 100 µm (a); 50 µm (b). c, Flow cytometric analysis of leukocyte populations within tumour samples (n = 7 tumour samples per group) obtained at 14 days and 21 days after implantation of 2.3 × 106 cancer cells with or without ferumoxytol (2.73 mg Fe ml–1; n = 7 tumour samples per group). Results are shown as a per cent of total CD45+. Note that tumour tissue at day 7 was too small for flow cytometric analyses. d, Quantitation of M1- and M2-macrophage-associated markers on immunofluorescence stainings at day 7 and 21. The number of positive cells in 10 high-power fields were counted and quantified for seven tumours per group. e, Corresponding flow cytometry analysis of CD3−CD49b−CD19−CD11b+Ly6C−Ly6G−F4/80+ (TAMs) and CD3−CD49b−CD19−CD11b+Ly6C+Ly6G−F4/80− (monocytes) in ferumoxytol co-implanted and control tumours at 14 and 21 days. All quantitative data are displayed as mean of seven tissue samples per group ± standard deviation. *P < 0.05, indicates a statistically significant difference (Student's t-test) from cancer cell injected controls.
MMTV-PyMT tumours were detectable as 4–5-mm subcutaneous nodules at day 14 after implantation. At this time, CD45-positive immune cell infiltrates were detected in both ferumoxytol-co-injected cancers and untreated controls. We evaluated immune cell subsets by FACS analyses at day 14 and 21, using a combination of lineage markers as shown in Fig. 3c. At day 14 after implantation, early-stage tumours of the control group contained leukocyte infiltrates dominated by TAMs (CD3−CD9b−CD19−CD11b+Ly6G−Ly6C−F4/80+), with minor populations of T cells, B cells, monocytes and natural killer cells. In comparison, the ferumoxytol co-injected group demonstrated a higher quantity of monocytes and TAMs (Fig. 3e). This difference diminished in later-stage tumours at day 21.
To prove that tumour growth in our MMTV-PYMT mouse model was driven by TAMs, another group of mice (n = 7; group 6, see Methods) was treated with anti-colony stimulating factor monoclonal antibody (α-CSF1 mAb), which depletes TAMs2. We found significant tumour growth inhibition in both α-CSF1 mAb and ferumoxytol co-implanted tumours compared with untreated controls (P > 0.05; Supplementary Fig. 4), even though the underlying mechanisms were different: depletion of TAMs in α-CSF1 mAb co-implanted tumours and M1 macrophage activation in ferumoxytol co-implanted tumours. As expected, there was no significant synergistic effect of α-CSF1 mAb and ferumoxytol treatment. Control mice (n = 7 mice per group) receiving cancer cells plus immunoglobulin-G (IgG), or cancer cells plus 2.73 mg ml-1 ferumoxytol plus IgG showed no significant tumour growth inhibition (Supplementary Fig. 4a). These results further validate TAM-dependent mechanisms of tumour growth inhibition.
Inhibition of metastases in the liver and lungs
To evaluate whether ferumoxytol has similar therapeutic benefit when delivered systemically to mice with visceral metastases, we investigated a second mouse model of small-cell lung cancer (SCLC) liver metastases18. We chose the liver as the target organ, because it accumulates high concentrations of intravenously administered iron oxide nanoparticles. 2 × 104 KP1-GFP-Luc cells were intravenously injected into NOD.Cg-Prkdcscid Il2rgtm1Wjl/SzJ mice and allowed to grow for 1 week, at which time tumour formation in the liver was confirmed by bioluminescence imaging (Fig. 4a). Then, ferumoxytol at a dose of 10 mg Fe kg–1 or saline (control) was administered intravenously, followed by serial bioluminescence imaging up to day 14. Ferumoxytol-treated mice demonstrated significantly inhibited tumour bioluminescence and significantly decreased total histopathologic tumour load compared with untreated control mice (P < 0.05; Fig. 4b).
Mice were intravenously injected with 2 × 104 KP1-GFP-Luc cancer cells. a, Seven days later, seven mice each received a single intravenous injection of ferumoxytol at a dose of 10 mg Fe kg–1 or no treatment, followed by serial bioluminescence imaging studies in weekly intervals. At baseline (week 1) both ferumoxytol-treated and control mice demonstrated equal liver bioluminescence, indicative of equal tumour burden. However, follow-up imaging studies at weeks 2 and 3 demonstrated diminished tumour bioluminescence of treated livers compared with controls. b, Corresponding quantitative liver luminescence of ferumoxytol-treated and control mice, displayed as mean data of seven mice in each group and standard deviation. c, FACS analysis of lung tissue of the same mice, gated on CD45−GFP+ live singlets to assess tumour load in control (left) and ferumoxytol-treated (right) Cg-Prkdcscid Il2rgtm1Wjl/SzJ (NSG) mice. Tumour load was significantly reduced in the treated group. d, Characterization of lung macrophages/dendritic cells in control (left) and ferumoxytol-treated (right) NSG mice with metastatic disease showed a significant increase of interstitial lung macrophages under treatment; subsets (gated on CD45+ Ly6G− live singlets) were characterized based on CD11b and CD11c expression as interstitial macrophages (CD11bhighCD11cint), inflammatory monocytes (CD11bhigh,CD11cneg), alveolar macrophages (CD11chigh,CD11bneg) and lung dendritic cells (CD11cintCD11bint). e, The frequencies of infiltrating Ly6C+ lung monocytes (gated on CD45+ Ly6G− live singlets) did not differ in the control and ferumoxytol-treated groups. f, M1- and M2-polarization phenotypes of CD45+CD11b+F4/80+ cells in control and ferumoxytol-treated lung macrophages indicates a significant reduction of CD206 expression on treatment. Numbers in boxes in c–f represent frequencies of the subset within the respective parent gate. Frequencies and statistical analysis of the respective gates for c–f are plotted on the corresponding graphs at the right side of the panel. All quantitative data are displayed as mean of seven mice per tissue samples per group ± standard deviation. *P < 0.05, indicates a statistically significant difference (Student's t-test) from untreated controls.
Systemic delivery of ferumoxytol also significantly reduced pulmonary metastasis in the same mouse model (Fig. 4c). This was associated with significant increase of interstitial macrophages (CD11bhighCD11cint) in the lungs of ferumoxytol-injected mice while the amount of pro-inflammatory Ly6C+ monocytes (CD11bhigh, CD11cneg), alveolar macrophages (CD11chigh, CD11bneg) and lung dendritic cells (CD11cintCD11bint) remained constant (Fig. 4d,e). Most importantly, lung macrophages showed a significant loss of the M2 marker CD206 in the treatment group, which could indicate M1 polarization (Fig. 4f). Ferumoxytol was also effective in inhibiting established liver tumours in a TAM-dependent manner.
In vivo prevention of hepatic metastasis
To provide an immediate practical application of our findings, we next sought to prevent liver tumour formation by pretreatment with ferumoxytol, using the above-described mouse model of SCLC liver metastases18. We pretreated NOD.Cg-Prkdcscid Il2rgtm1Wjl/SzJ mice with three ferumoxytol tail-vein injections at a dose of 10 mg Fe kg–1 and an interval of 4 days, followed by intravenous injection of 1 × 104 KP1-GFP-Luc cells. Non-ferumoxytol-treated mice served as controls (Fig. 5a,b). Ferumoxytol-pretreated mice showed significantly reduced tumour formation in the liver, as quantified by significantly lower liver photon flux values compared with untreated controls (P < 0.05; Fig. 5c,d,i). Histopathology confirmed a significant reduction of tumour lesions in ferumoxytol-treated livers compared with the untreated controls (P < 0.05; Fig. 5e–h,j). Flow cytometry analyses revealed increased quantities of CD11bhighF4/80low macrophages in ferumoxytol-pretreated mice compared to untreated controls (Fig. 6a,c,d). The tumour load was 6 times lower in ferumoxytol-treated animals compared with control animals (Fig. 6b and Supplementary Fig. 5). Further, the polarization of infiltrating macrophages shifted towards M1 phenotypes (Fig. 6f), whereas tissue-resident macrophages lost their M2 polarization (Fig. 6e). Thus, pretreatment with ferumoxytol can inhibit tumour metastases.
a,b, Experimental set-up: mice were injected with either saline (left) or ferumoxytol (3 × 10 mg Fe per kg–1; right), followed by intravenous injection of 1 × 104 KP1-GFP-Luc cells. c,d, Liver tumour growth was monitored by bioluminescence imaging: at day 21 after tumour cell injection, untreated livers (c) showed strong bioluminescence while ferumoxytol pretreated livers did not (d). e–h, Corresponding histopathology: representative hematoxylin and eosin (H&E) stained images show marked tumour cell infiltration (yellow arrows) of an untreated control liver (e) but not of a ferumoxytol-treated liver (g). Prussian blue stains show minor iron deposition in normal livers (f) and markedly positive iron deposition in ferumoxytol-treated livers (h). Scale bars,1 mm. i,j, Luminescence radiance (i) and corresponding quantitative tumour area (j) of ferumoxytol-treated livers and untreated controls, displayed as mean of seven livers in each group ± standard deviation. *P < 0.05, indicates a statistically significant difference (Student's t-test) from untreated controls.
a, Livers of the same mice described in Fig. 5 were further analysed with FACS for infiltrating leukocyte populations. b, Accordingly, the relative number of GFP+ cells within the liver gate (%) was significantly reduced in ferumoxytol–treated livers compared with untreated controls. c, CD11blowF4/80high tissue-resident macrophages were increased in ferumoxytol-treated livers compared to controls and d, CD11bhighF4/80low peripheral-derived macrophages were increased in ferumoxytol-treated livers compared with controls. e,f, The polarization of both tissue-resident and infiltrating macrophages shifted towards the M1 phenotype as measured by CD80 and CD206 markers: median fluorescent intensity ratios (MFI) of M1/M2 associated markers (CD80/CD206) in CD11blowF4/80high tissue-resident macrophages (e) and infiltrating F4/80low CD11bhigh liver macrophages (f) isolated from ferumoxytol-treated livers and untreated controls. All quantitative data are displayed as the mean of seven livers per group ± standard deviation. *P < 0.05, indicates a statistically significant difference (Student's t-test) from untreated controls.
Discussion
Our data demonstrate that ferumoxytol nanoparticles significantly suppressed tumour growth by inducing pro-inflammatory macrophage responses. Since ferumoxytol is FDA-approved for treatment of iron deficiency19, it could be applied ‘off label’ to protect the liver from metastatic seeds and potentiate TAM-modulating cancer immunotherapies in patients.
Elemental iron plays a complex role in both progression and suppression of malignancies20,21. Low doses of iron ions are essential for cell replication and DNA synthesis22. However, iron overexposure can lead to an increased incidence of human cancers through increased oxidative stress and DNA damage20,23. Thus, it seems logical to counteract this process by iron depletion. In fact, iron depletion has led to tumour growth arrest in mouse models24. Conversely, high iron doses have been reported to have direct cytotoxic effects on malignant tumours in vitro25 and in vivo26,27,28. However, clinically approved nanoparticles are produced with semi-synthetic coatings that minimize direct toxic effects. Ferumoxytol is coated with carboxymethyldextran, which leads to low toxicity29 and lysosomal uptake and degradation30, with little or no effect on cell function and viability31.
Our data show that ferumoxytol nanoparticles rather cause tumour growth inhibition through indirect effects on the tumour microenvironment: monocytes are recruited to malignant tumours through local expression of chemotactic cytokines32 and are typically polarized to anti-inflammatory M2 phenotypes33. Previous in vitro studies showed that superparamagnetic iron oxides induce a phenotypic shift in M2 macrophages towards a high CD86+, TNFα positive M1 macrophage subtype34. This M1 polarization can induce a Fenton reaction15. Our data showed that the Fenton reaction can induce cancer cell apoptosis. Continued M1 polarization triggered by apoptotic cancer cells can then create an autocrine feedback loop that maintains the production of TNFα and nitric oxide (NO)35.
It has been found15 that in wound healing iron exposure leads to M1 polarization and that concomitant anti-inflammatory M2 responses are overpowered. The value of CD206 as a marker for M2 macrophages, used in our study and in ref. 15, is controversial and might be tissue-specific15. In the study described in ref. 36, tumour-promoting macrophages with a CD206 expression marker were not detected, but rather a CD11bhi MHCII+ population derived from inflammatory monocytes. We confirmed M1 polarization in our tumours by significant expression of M1-associated genes.
Potential clinical applications of ferumoxytol-mediated pro-inflammatory immune responses could entail potentiating the efficacy of other M1-activating cancer immunotherapies, such as anti-CD47 mAbs (ref. 37) or antibodies blocking IL-4 or IL-13 signalling38. In addition, ferumoxytol could be locally delivered to unresectable tumours via interventional procedures, to micrometastases in confined spaces (for example, peritoneal seeds) or to tumour resection margins at the end of a tumour surgery with positive resection margins. Finally, patients with primary tumours that typically metastasize to the liver could receive protective ferumoxytol medications to prevent early metastatic seeds. Ferumoxytol can be conjugated or functionalized to anciliary molecules to further amplify the desired immune-modulating properties39,40.
The current recommended dose of ferumoxytol (Feraheme) for the treatment of anaemia is 510 mg iron, followed by a second administration of 510 mg iron 3–8 days later. Ferumoxytol should not be administered to patients with signs of iron overload19,41. But it has been shown that ferumoxytol does not cause liver toxicity in animal models42 or patients19. Feraheme is typically metabolized within 6–8 weeks19. Therefore, maintenance treatment could continue in 2–3 month intervals. Future studies have to show if ferumoxytol can suppress liver metastases in patients. Of note, there is a large population of patients with liver metastases who received similar iron oxide nanoparticle compounds, it would be worthwhile to review their imaging studies and clinical outcomes.
Conclusions
We discovered an intrinsic therapeutic effect of ferumoxytol on cancer growth due to macrophage polarization into pro-inflammatory M1 phenotypes. These results have major implications for diagnostic and therapeutic applications of iron oxide nanoparticles. Because ferumoxytol is FDA-approved, our approach is immediately accessible for cancer patients through ‘off label’ use19.
Methods
Detailed methodology is described in the Supplementary methods.
Cell culture
MMTV-PyMT (mouse mammary tumour virus - Polyoma middle T antigen) mammary cancer cells were isolated from 90- to 95-day-old transgenic MMTV-PyMT mice. MDA-MB-468 human breast carcinoma cells, HT1080 human fibrosarcoma cells, RAW264.7 macrophages, human dermal fibroblasts (ATCC, PCS-201–012) and human umbilical vein endothelial cells (HUVECs) were purchased from the American Type Culture Collection (ATCC; Bethesda, MD, USA). These cell lines are not listed in the database of commonly misidentified cell lines maintained by ICLAC and were directly purchased from ATCC. All cell lines used in this study are quarterly authenticated by unique STR profile and results indicated no cross-contamination. All cancer cells were cultured in Dulbecco's Modified Eagle's Medium (DMEM, Gibco, Grand Island, NY, USA), supplemented with 10% fetal bovine serum (FBS, Gibco) and 1% penicillin/streptomycin (Gibco). Human fibroblasts were maintained in fibroblast basal media (Gibco), supplemented with a fibroblast growth kit (Gibco). HUVECs were grown in endothelial basal medium (Clonetics) supplemented with SingleQuots (Clonetics) and 1% penicillin/streptomycin.
Murine and human cancer cells were incubated with ferumoxytol nanoparticles and cell cytotoxicity was evaluated using the SensoLyte Homogeneous AMC Caspase-3/7 assay kit (AnaSpec, Fremont, CA, USA), according to the manufacturer's instructions. Briefly, 1 × 105 cells per well were treated with ferumoxytol at various concentrations for 6 h. Then, 50 µl per well of AMC caspase 3/7 substrate solution was added to the cells and incubated at room temperature for 30 min. The fluorescent signal was measured by a fluorescence microplate reader (FlexStation II384, MolecularDevice, CA) with excitation/emission 354 nm/442 nm, cutoff 430 nm. Results were expressed as n-fold increases in caspase activity compared with untreated controls (defined as 1). For each concentration of ferumoxytol, a Student's t-test was employed to determine the significance of caspase 3/7 activity levels between different cell samples. P values of less than 0.05 were considered to indicate statistically significant differences.
Animal model
Animal handling, surveillance, and experimentation were performed in accordance with and approval from the Stanford University Administrative Panel on Laboratory Animal Care (protocol no. 24965). FVB/N mice were purchased from Charles River (Wilmington, MA, USA) and NOD.Cg-Prkdcscid Il2rgtm1Wjl/SzJ mice were purchased from Jackson Laboratory (Bar Harbor, ME, USA). Ninety-eight 8–10-week-old female FVB/N mice were randomly divided into seven groups, which were implanted with MMTV-PyMT cancer cells and/or ferumoxytol nanoparticles into 1 or more mammary fat pads, followed by daily tumour size measurements with a caliper for 7–21 days, followed by histopathological evaluation.
Group 1
To evaluate whether local ferumoxytol administration causes tumour growth inhibition, 21 FVB/N mice were implanted with 2.3 × 106 MMTV-PyMT-derived cancer cells into the left mammary fat pad and 2.3 × 106 MMTV-PyMT-derived cancer cells co-injected with 100 µl ferumoxytol at a concentration of 2.73 mg Fe ml–1 into the right mammary fat pads (9.1 µl ferumoxytol at a concentration of 30 mg Fe ml–1 in 90.9 µl of cancer cells in PBS). Cancer growth was monitored for up to 7 days (n = 7 mice), 14 days (n = 7 mice) and 21 days (n = 7 mice) after implantation, followed by histopathology.
Group 2
To evaluate effects of different ferumoxytol concentrations, seven additional FVB/N mice were implanted with 2.3 × 106 MMTV-PyMT-cancer cells into the left mammary fat pads and an equal number of cells plus 100 µl of ferumoxytol at a concentration of 8.37 mg Fe ml–1 into the right mammary fat pads.
Group 3
To evaluate effects of different nanoparticle compositions, seven additional FVB/N mice were implanted with 2.3 × 106 MMTV-PyMT-derived cancer cells into the left mammary fat pads and 2.3 × 106 of MMTV-PyMT cancer cells plus 100 µl of ferumoxtran-10 (Sinerem/Combidex; 2.73 mg Fe ml–1) into the right mammary fat pads.
Group 4
To exclude the possibility that tumours in the same animal interact with each other, a set of 14 FVB/N mice were implanted unilaterally with either 2.3 × 106 MMTV-PyMT-derived cancer cells (n = 7) or cancer cells plus 100 µl of ferumoxytol (2.73 mg Fe ml–1; n = 7).
Group 5
To determine which tumour cell quantity could be completely suppressed by ferumoxytol treatment, 21 additional FVB/N mice were implanted with decreasing quantities of cancer cells (1 × 106 (n = 7), 0.1 × 106 (n = 7) and 0.01 × 106 (n = 7)) into the left mammary fat pads and the same quantity of MMTV-PyMT-derived cancer cells plus 100 µl of ferumoxytol (2.73 mg Fe ml–1) into the right mammary fat pads. To monitor tumour formation, all mice underwent near-infrared fluorescence optical imaging after intravenous injection of 100 µl of indocyanine green (ICG, Acros Organics, Pittsburgh, Pennsylvania, 50 µM), using the IVIS Spectrum Optical Imaging System (Xenogen Corporation, Caliper Life Sciences, Hopkinton, MA, USA) with an excitation filter of 745 nm, an emission filter of 820 nm, and an exposure time of 1 s. Fluorescence data were processed using Living Image software (version 4.3.1, Perkin Elmer, MA, USA).
Group 6
To evaluate the effect of macrophages on tumour growth, seven additional FVB/N mice were implanted with 2.3 × 106 MMTV-PyMT-derived cancer cells into the left mammary fat pad and 2.3 × 106 MMTV-PyMT-derived cancer plus 100 µl ferumoxytol (2.73 mg Fe ml–1) into the right mammary fat pad. After tumour cell implantation, mice were treated with anti-colony stimulating factor (CSF)-1 monoclonal antibody (mAb), clone 5A1 (ATCC, USA) at a total dose of 2 mg, consisting of an initial dose of 1 mg followed by 0.5 mg chaser doses on days 5 and 8. Two additional groups of mice (n = 7 mice per group) served as controls by receiving cancer cells + IgG (IgG1 Isotype control, Bio X Cell, USA) and cancer cells + ferumoxytol + IgG.
Group 7
To address whether the ferumoxytol-induced tumour growth inhibition is specific to the iron oxide core of ferumoxytol nanoparticles, seven additional FVB/N mice were implanted with 2.3 × 106 MMTV-PyMT-derived cancer cells into the left mammary fat pad and 2.3 × 106 MMTV-PyMT-derived cancer cells plus 100 µl dextran (FD10S; Molecular Weight 10,000 Da; Sigma-Aldrich, St. Louis, MO) at a concentration of 50 mg ml–1.
Statistical analyses
Data are presented as mean ± standard deviation. Comparison between two groups was performed using paired or unpaired t-tests. Multiple experimental groups were compared by a one-way analysis of variance (ANOVA) followed by an appropriate post-hoc test. Results were considered statistically significant when P < 0.05. All in vitro work has been repeated at least three times by independent experiments. The sample size was not predetermined in in vitro studies. Sample sizes for animal studies were estimated and randomization was applied. Blinding was used for group allocation between the non-ferumoxytol control group and ferumoxytol treatment group.
References
Corot, C., Robert, P., Idee, J. M. & Port, M. Recent advances in iron oxide nanocrystal technology for medical imaging. Adv. Drug Deliv. Rev. 58, 1471–1504 (2006).
Daldrup-Link, H. E. et al. MRI of tumor-associated macrophages with clinically applicable iron oxide nanoparticles. Clin. Cancer Res. 17, 5695–5704 (2011).
Klenk, C. et al. Ionising radiation-free whole-body MRI versus 18F-fluorodeoxyglucose PET/CT scans for children and young adults with cancer: a prospective, non-randomised, single-centre study. Lancet Oncol. 15, 275–285 (2014).
Ansari, C. et al. Development of novel tumor-targeted theranostic nanoparticles activated by membrane-type matrix metalloproteinases for combined cancer magnetic resonance imaging and therapy. Small 10, 566–575 (2014).
Neuwelt, E. A. et al. The potential of ferumoxytol nanoparticle magnetic resonance imaging, perfusion, and angiography in central nervous system malignancy: a pilot study. Neurosurgery 60, 601–611 (2007).
Daldrup-Link, H. & Coussens, L. M. MR imaging of tumor-associated macrophages. Oncoimmunology 1, 507–509 (2012).
Vinogradov, S., Warren, G. & Wei, X. Macrophages associated with tumors as potential targets and therapeutic intermediates. Nanomedicine 9, 695–707 (2014).
Miller, M. A. et al. Tumour-associated macrophages act as a slow-release reservoir of nano-therapeutic Pt(IV) pro-drug. Nat. Commun. 6, 8692 (2015).
Weissleder, R., Nahrendorf, M. & Pittet, M. J. Imaging macrophages with nanoparticles. Nat. Mater. 13, 125–138 (2014).
Li, C. A targeted approach to cancer imaging and therapy. Nat. Mater. 13, 110–115 (2014).
Futterer, S., Andrusenko, I., Kolb, U., Hofmeister, W. & Langguth, P. Structural characterization of iron oxide/hydroxide nanoparticles in nine different parenteral drugs for the treatment of iron deficiency anaemia by electron diffraction (ED) and X-ray powder diffraction (XRPD). J. Pharm. Biomed. Anal. 86, 151–160 (2013).
Ittrich, H., Peldschus, K., Raabe, N., Kaul, M. & Adam, G. Superparamagnetic iron oxide nanoparticles in biomedicine: applications and developments in diagnostics and therapy. RoFo 185, 1149–1166 (2013).
Richards, J. M. et al. In vivo mononuclear cell tracking using superparamagnetic particles of iron oxide: feasibility and safety in humans. Circ. Cardiovasc. Imaging 5, 509–517 (2012).
Warheit, D. B. & Hartsky, M. A. Role of alveolar macrophage chemotaxis and phagocytosis in pulmonary clearance responses to inhaled particles: comparisons among rodent species. Microsc. Res. Tech 26, 412–422 (1993).
Sindrilaru, A. et al. An unrestrained proinflammatory M1 macrophage population induced by iron impairs wound healing in humans and mice. J. Clin. Invest. 121, 985–997 (2011).
Wodarz, D. & Anton-Culver, H. Dynamical interactions between multiple cancers. Cell Cycle 4, 764–771 (2005).
Nejadnik, H. et al. Somatic differentiation and MR imaging of magnetically labeled human embryonic stem cells. Cell Transplant. 21, 2555–2567 (2012).
Jahchan, N. S. et al. A drug repositioning approach identifies tricyclic antidepressants as inhibitors of small cell lung cancer and other neuroendocrine tumors. Cancer Discov. 3, 1364–1377 (2013).
Lu, M., Cohen, M. H., Rieves, D. & Pazdur, R. FDA report: ferumoxytol for intravenous iron therapy in adult patients with chronic kidney disease. Am. J. Hematol. 85, 315–319 (2010).
Choi, J. Y. et al. Iron intake, oxidative stress-related genes (MnSOD and MPO) and prostate cancer risk in CARET cohort. Carcinogenesis 29, 964–970 (2008).
Poljak-Blazi, M. et al. Effect of ferric ions on reactive oxygen species formation, cervical cancer cell lines growth and E6/E7 oncogene expression. Toxicol. In Vitro 25, 160–166 (2011).
Crowe, W. E., Maglova, L. M., Ponka, P. & Russell, J. M. Human cytomegalovirus-induced host cell enlargement is iron dependent. Am. J. Physiol. Cell Physiol. 287, C1023–C1030 (2004).
Petersen, D. R. Alcohol, iron-associated oxidative stress, and cancer. Alcohol 35, 243–249 (2005).
Nie, G., Chen, G., Sheftel, A. D., Pantopoulos, K. & Ponka, P. In vivo tumor growth is inhibited by cytosolic iron deprivation caused by the expression of mitochondrial ferritin. Blood 108, 2428–2434 (2006).
Knobel, Y., Glei, M., Osswald, K. & Pool-Zobel, B. L. Ferric iron increases ROS formation, modulates cell growth and enhances genotoxic damage by 4-hydroxynonenal in human colon tumor cells. Toxicol. In Vitro 20, 793–800 (2006).
Basel, M. T. et al. Cell-delivered magnetic nanoparticles caused hyperthermia-mediated increased survival in a murine pancreatic cancer model. Int. J. Nanomedicine 7, 297–306 (2012).
Chung, T. H. et al. Iron oxide nanoparticle-induced epidermal growth factor receptor expression in human stem cells for tumor therapy. ACS Nano 5, 9807–9816 (2011).
Foy, S. P. & Labhasetwar, V. Oh the irony: iron as a cancer cause or cure? Biomaterials 32, 9155–9158 (2011).
Reinisch, W., Staun, M., Bhandari, S. & Munoz, M. State of the iron: how to diagnose and efficiently treat iron deficiency anemia in inflammatory bowel disease. J. Crohns Colitis 7, 429–440 (2013).
Lunov, O. et al. Lysosomal degradation of the carboxydextran shell of coated superparamagnetic iron oxide nanoparticles and the fate of professional phagocytes. Biomaterials 31, 9015–9022 (2010).
Gupta, A. K. & Wells, S. Surface-modified superparamagnetic nanoparticles for drug delivery: preparation, characterization, and cytotoxicity studies. IEEE Trans. Nanobioscience 3, 66–73 (2004).
Mou, W. et al. Expression of Sox2 in breast cancer cells promotes the recruitment of M2 macrophages to tumor microenvironment. Cancer Lett. 358, 115–123 (2015).
Becker, M., Muller, C. B., De Bastiani, M. A. & Klamt, F. The prognostic impact of tumor-associated macrophages and intra-tumoral apoptosis in non-small cell lung cancer. Histol. Histopathol. 29, 21–31 (2014).
Laskar, A., Eilertsen, J., Li, W. & Yuan, X. M. SPION primes THP1 derived M2 macrophages towards M1-like macrophages. Biochem. Biophys. Res. Commun. 441, 737–742 (2013).
Solinas, G., Germano, G., Mantovani, A. & Allavena, P. Tumor-associated macrophages (TAM) as major players of the cancer-related inflammation. J. Leukoc. Biol. 86, 1065–1073 (2009).
Franklin, R. A. et al. The cellular and molecular origin of tumor-associated macrophages. Science 344, 921–925 (2014).
Edris, B. et al. Antibody therapy targeting the CD47 protein is effective in a model of aggressive metastatic leiomyosarcoma. Proc. Natl Acad. Sci. USA 109, 6656–6661 (2012).
Shiao, S. L. et al. TH2-polarized CD4+ T cells and macrophages limit efficacy of radiotherapy. Cancer Immunol. Res. 3, 518–525 (2015).
Hadjipanayis, C. G. et al. EGFRvIII antibody-conjugated iron oxide nanoparticles for magnetic resonance imaging-guided convection-enhanced delivery and targeted therapy of glioblastoma. Cancer Res. 70, 6303–6312 (2010).
Thorek, D. L. et al. Non-invasive mapping of deep-tissue lymph nodes in live animals using a multimodal PET/MRI nanoparticle. Nat. Commun. 5, 3097 (2014).
Rosner, M. H. & Auerbach, M. Ferumoxytol for the treatment of iron deficiency. Expert Rev. Hematol. 4, 399–406 (2011).
Cheng, K. et al. Magnetic antibody-linked nanomatchmakers for therapeutic cell targeting. Nat. Commun. 5, 4880 (2014).
Acknowledgements
The authors acknowledge support from the National Institute of Health/National Cancer Institute (NIH/NCI), grant numbers R21CA156124 and R21CA176519, and the Department of Defense BCRP Era of Hope Scholar Expansion Award (BC10412). S.Z. was supported by the Stanford Cancer Imaging Training (SCIT) T32 fellowship programme. We also thank the Stanford Center for Innovation and In-Vivo Imaging (SCI 3) supported by the NCI Cancer Center (P30 CA124435–02) and NCI ICMIC (P50 CA114747) for providing the infrastructure for mouse imaging. G.H. was supported by a Swiss National Science Foundation Grant P-155336 (www.snf.ch) and the Novartis Foundation for Medical-Biological Research (www.stiftungmedbiol.novartis.com). In addition, we thank E. Misquez for her excellent administrative assistance throughout this project, D. Yang for assistance with cell culture and M. Winslow's laboratory (Stanford University) for their generous gift of the SCLC KP1-GFP-Luc cell lines.
Author information
Authors and Affiliations
Contributions
The study concept and design was developed by H.E.D.-L., L.M.C. and S.Z. The acquisition of data was performed by S.Z., R.S., G.H., M.Ma., S.G. and A.S. (cell experiments, tissue experiments and immunohistochemistry), S.Z., J.S.P., O.L. and H.N. (animal experiments), S.Z., O.L., M.Mo. (magnetic resonance imaging), and S.Z., G.H., A.S. (flow cytometry). All authors contributed to the analysis of the data and discussed the results. H.E.D.-L. and S.Z. wrote the manuscript. All authors edited the manuscript and approved the final version. Funding was obtained by H.E.D.-L. and all studies were supervised by H.E.D.-L.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
Supplementary information
Supplementary information (PDF 1038 kb)
Rights and permissions
About this article
Cite this article
Zanganeh, S., Hutter, G., Spitler, R. et al. Iron oxide nanoparticles inhibit tumour growth by inducing pro-inflammatory macrophage polarization in tumour tissues. Nature Nanotech 11, 986–994 (2016). https://doi.org/10.1038/nnano.2016.168
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/nnano.2016.168
This article is cited by
-
circ-TFRC downregulation suppresses ovarian cancer progression via miR-615-3p/IGF2 axis regulation
Cancer Cell International (2024)
-
The application of nanoparticles-based ferroptosis, pyroptosis and autophagy in cancer immunotherapy
Journal of Nanobiotechnology (2024)
-
“All in one” nanoprobe Au-TTF-1 for target FL/CT bioimaging, machine learning technology and imaging-guided photothermal therapy against lung adenocarcinoma
Journal of Nanobiotechnology (2024)
-
Arsenic album 30C exhibits crystalline nano structure of arsenic trioxide and modulates innate immune markers in murine macrophage cell lines
Scientific Reports (2024)
-
Nanomedicine targeting ferroptosis to overcome anticancer therapeutic resistance
Science China Life Sciences (2024)