Key Points
-
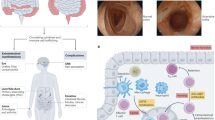
The pathophysiology of irritable bowel disease (IBD), including ulcerative colitis (UC) and Crohn's disease, reflects the convergence of genetic, environmental and immunological factors initiating an aberrant innate immune response and culminating in a T-cell-driven process.
-
Currently available therapies are inadequate for sizeable groups of patients with UC and Crohn's disease, as many patients are intolerant or unresponsive to existing medications.
-
Biologic therapies, particularly antibodies, have targeted cytokines which are involved in inflammation and T-cell differentiation.
-
Several additional agents directed against tumour-necrosis factor-α (TNFα) are likely to be approved soon for clinical use in Crohn's disease, including adalimumab, a fully human anti-TNFα antibody, and certolizumab (CDP870), a pegylated anti-TNFα fragment.
-
Anti-interleukin-12 (anti-IL-12) antibodies, which bind to a cytokine central to determining a TH1-type response, seem to be effective in Crohn's disease. Fontolizumab, an anti-interferon-γ (IFNγ) antibody, which blocks TH1 polarization, as well as activation of macrophages, monocytes and natural killer cells, is promising for the treatment of active Crohn's disease.
-
A CD3 antibody, visilizumab, appears beneficial in the treatment of UC, though there are concerns about viral activation and infusion reactions.
-
IL-10, though a central immunoregulatory cytokine, was not effective in several studies in Crohn's disease and UC, but continues to be investigated, with strategies which might provide more specific delivery to the gastrointestinal tract, including the use of engineered bacteria.
-
Blockade of selective adhesion molecules is an approach shared by several therapies. Although natalizumab, an α4 integrin antibody, might benefit a subset of patients with Crohn's disease and possibly sustain remission, development has been halted because of several cases of progressive, multifocal leukoencephalopathy (PML). An antibody directed against α4β7 integrin, designated MLN02, is more specific to the intestine, and seems to be promising for active UC.
-
Sargramostim, or recombinant human granulocyte–macrophage colony-stimulating factor (rhuGM-CSF), which may act to stimulate intestinal innate immunity, was effective in active Crohn's disease, and in contrast to most other therapies under investigation which act to suppress the immune response.
-
Modulation of the luminal flora has been investigated using probiotics and prebiotics, though these strategies are still early in development.
Abstract
With recent advances in the understanding of its pathophysiology, inflammatory bowel disease has become a very active area for the development of novel therapeutic agents. New targets for biologics include cytokines involved in T-cell activation, with antibodies directed against IL-12 and interferon-γ. Selective adhesion molecule blockade has produced promising, though mixed, results. Recombinant human granulocyte–macrophage colony-stimulating factor might be effective in active Crohn's disease, presumably through stimulation of intestinal innate immune responses. With increasing evidence for a crucial role for luminal flora in maintaining the health of the bowel, strategies to manipulate intestinal bacteria using probiotics and prebiotics are being actively investigated as well.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Podolsky, D. K. Inflammatory bowel disease. N. Engl. J. Med. 347, 417–429 (2002).
Hugot, J. P. et al. Association of NOD2 leucine-rich repeat variants with susceptibility to Crohn's disease. Nature 411, 599–603 (2001).
Ogura, Y. et al. A frameshift mutation in NOD2 associated with susceptibility to Crohn's disease. Nature 411, 603–606 (2001). The identification of the NOD mutation as a risk factor for the development of Crohn's disease has profoundly altered the understanding of Crohn's disease, though the full implications, with regard to insights into pathophysiology as well as clinical care, remain to be determined.
Stoll, M. et al. Genetic variation in DLG5 is associated with inflammatory bowel disease. Nature Genet. 36, 476–480 (2004).
Lamhonwah, A. M., Skaug, J., Scherer, S. W. & Tein, I. A third human carnitine/organic cation transporter (OCTN3) as a candidate for the 5q31 Crohn's disease locus (IBD5). Biochem. Biophys. Res. Commun. 301, 98–101 (2003).
Hisamatsu, T. et al. CARD15/NOD2 functions as an antibacterial factor in human intestinal epithelial cells. Gastroenterology 124, 993–1000 (2003).
Bonen, D. K. et al. Crohn's disease-associated NOD2 variants share a signaling defect in response to lipopolysaccharide and peptidoglycan. Gastroenterology 124, 140–146 (2003).
Watanabe, T., Kitani, A., Murray, P. J. & Strober, W. NOD2 is a negative regulator of Toll-like receptor 2-mediated T helper type 1 responses. Nature Immunol. 5, 800–808 (2004).
van Heel, D. A. et al. Muramyl dipeptide and toll-like receptor sensitivity in NOD2-associated Crohn's disease. Lancet 365, 1794–1796 (2005). The mechanisms by which the NOD mutation leads to the pathophysiology of Crohn's disease is controversial: whether it produces an innate immune defect or causes directly an excessive T-cell response is uncertain. Increasingly, an aberrant innate immune response is accepted as the initiating defect, supported by this study, among others.
van Heel, D. A. et al. Synergy between TLR9 and NOD2 innate immune responses is lost in genetic Crohn's disease. Gut 54, 1515–1518 (2005).
Favier, C. et al. Fecal β-D-galactosidase production and Bifidobacteria are decreased in Crohn's disease. Dig. Dis. Sci. 42, 817–822 (1997).
Seksik, P. et al. Alterations of the dominant faecal bacterial groups in patients with Crohn's disease of the colon. Gut 52, 237–242 (2003).
Mylonaki, M., Rayment, N. B., Rampton, D. S., Hudspith, B. N. & Brostoff, J. Molecular characterization of rectal mucosa-associated bacterial flora in inflammatory bowel disease. Inflamm Bowel Dis 11, 481–487 (2005).
Darfeuille-Michaud, A. et al. Presence of adherent Escherichia coli strains in ileal mucosa of patients with Crohn's disease. Gastroenterology 115, 1405–1413 (1998).
Ott, S. J. et al. Reduction in diversity of the colonic mucosa associated bacterial microflora in patients with active inflammatory bowel disease. Gut 53, 685–693 (2004).
Harrington, L. E. et al. Interleukin 17-producing CD4+ effector T cells develop via a lineage distinct from the T helper type 1 and 2 lineages. Nature Immunol. 6, 1123–1132 (2005).
Wynn, T. Th-17: a giant step from Th1 and Th2. Nature Immunol. 6, 1069–1070 (2005).
Canva-Delcambre, V. et al. Treatment of severe Crohn's disease with anti-CD4 monoclonal antibody. Aliment Pharmacol. Ther. 10, 721–727 (1996).
Stronkhorst, A. et al. CD4 antibody treatment in patients with active Crohn's disease: a phase 1 dose finding study. Gut 40, 320–327 (1997).
Plevy, S. et al. A Humanized anti-CD3 monoclonal antibody, visilizumab, for treatment of severe, steroid refractory ulcerative colitis: results of a Phase I study. Gastroenterology 126, A-75 (2004).
Creed, T. J. et al. Basiliximab (anti-CD25) in combination with steroids may be an effective new treatment for steroid-resistant ulcerative colitis. Aliment Pharmacol. Ther. 18, 65–75 (2003).
Van Assche, G. et al. A pilot study on the use of the humanized anti-interleukin-2 receptor antibody daclizumab in active ulcerative colitis. Am. J. Gastroenterol. 98, 369–376 (2003).
Hommes, D. et al. Daclizumab, an anti-CD25 antibody, for the treatment of moderate-to-severe ulcerative colitis. Digestive Dis. Week May 15–20, New Orleans, Louisiana (2004).
Mannon, P. J. et al. Anti-interleukin-12 antibody for active Crohn's disease. N. Engl. J. Med. 351, 2069–2079 (2004). A different mechanism of action has been utilized to produce a promising therapy for Crohn's disease by interfering with T-cell differentiation. An anti-IL-12 antibody, binding to a shared subunit with IL-23, inhibits the development of a T H 2 type response.
Ten Hove, T. et al. Blockade of endogenous IL-18 ameliorates TNBS-induced colitis by decreasing local TNF-α production in mice. Gastroenterology 121, 1372–1379 (2001).
Wirtz, S., Becker, C., Blumberg, R., Galle, P. R. & Neurath, M. F. Treatment of T cell-dependent experimental colitis in SCID mice by local administration of an adenovirus expressing IL-18 antisense mRNA. J. Immunol. 168, 411–420 (2002).
Hommes, D. et al. Fontolizumab (HuZAF[TM]), a humanized anti-IFN-γ antibody, has clinical activity and excellent tolerability in moderate to severe Crohn's disease (CD). Digestive Dis. Week May 15–20, New Orleans, Louisiana (2004).
Ito, H. et al. A pilot randomized trial of a human anti-interleukin-6 receptor monoclonal antibody in active Crohn's disease. Gastroenterology 126, 989–996; discussion 947 (2004).
Lopez-Cubero, S. O., Sullivan, K. M. & McDonald, G. B. Course of Crohn's disease after allogeneic marrow transplantation. Gastroenterology 114, 433–440 (1998).
Snowden, J. A. et al. Autologous hemopoietic stem cell transplantation in severe rheumatoid arthritis: a report from the EBMT and ABMTR. J. Rheumatol. 31, 482–488 (2004).
Oyama, Y. et al. Autologous hematopoietic stem cell transplantation in patients with refractory Crohn's disease. Gastroenterology 128, 552–563 (2005).
Yazdanbakhsh, M., Kremsner, P. & Ree, R. V. Allergy, parasites and the hygiene hypothesis. Science 296, 490–494 (2002).
Svetic, A. et al. A primary intestinal helminthic infection rapidly induces a gut-associated elevation of Th2-associated cytokines and IL-3. J. Immunol. 150, 3434–3441 (1993).
Doetze, A. et al. Antigen-specific cellular hyporesponsiveness in a chronic human helminth infection is mediated by T(h)3/T(r)1-type cytokines IL-10 and transforming growth factor-β but not by a T(h)1 to T(h)2 shift. Int. Immunol. 12, 623–630 (2000).
Elliott, D. et al. Helminths induce CD8+ regulatory T cell (Treg) in murine intestinal mucosa. Gastroenterology 128, A503 (2005).
Elliott, D. E. et al. Heligmosomoides polygyrus inhibits established colitis in IL-10-deficient mice. Eur. J. Immunol. 34, 2690–2698 (2004).
Summers, R. W., Elliott, D. E., Urban, J. F., Jr., Thompson, R. A. & Weinstock, J. V. Trichuris suis therapy for active ulcerative colitis: a randomized controlled trial. Gastroenterology 128, 825–832 (2005).
Summers, R. W., Elliott, D. E., Urban, J. F. Jr., Thompson, R. & Weinstock, J. V. Trichuris suis therapy in Crohn's disease. Gut 54, 87–90 (2005).
Targan, S. R. et al. A short-term study of chimeric monoclonal antibody cA2 to tumor necrosis factor α for Crohn's disease. Crohn's Disease cA2 Study Group. N. Engl. J. Med. 337, 1029–1035 (1997).
Sandborn, W. J. et al. Etanercept for active Crohn's disease: a randomized, double-blind, placebo-controlled trial. Gastroenterology 121, 1088–1094 (2001).
Sandborn, W. J. et al. CDP571, a humanised monoclonal antibody to tumour necrosis factor α, for moderate to severe Crohn's disease: a randomised, double blind, placebo controlled trial. Gut 53, 1485–1493 (2004).
Feagan, B. G. et al. A randomized, double-blind, placebo-controlled trial of CDP571, a humanized monoclonal antibody to tumour necrosis factor-α, in patients with corticosteroid-dependent Crohn's disease. Aliment Pharmacol. Ther. 21, 373–384 (2005).
Rutgeerts, P. et al. A randomized controlled trial of infliximab therapy for active ulvceraive colitis: Act 1 Trial. Gastroenterology 128, A105 (2005). Infliximab was considered unlikely by many to be a useful therapy for ulcerative colitis. Whether due to misunderstanding of the differences between Crohn's and UC, or due to an incomplete appreciation of the mechanisms of action of infliximab, this study demonstrated that infliximab is an effective treatment for UC as well.
Sandborn, W. et al. Infliximab induction and maintenance therapy for ulcerative colitis: the Act 2 Trial. Gastroenterology 128, A104 (2005).
Winter, T. A. et al. Intravenous CDP870, a PEGylated Fab' fragment of a humanized antitumour necrosis factor antibody, in patients with moderate-to-severe Crohn's disease: an exploratory study. Aliment Pharmacol. Ther. 20, 1337–1346 (2004).
Hanauer, S. B. et al. Human anti-tumor necrosis factor monoclonal antibody (adalimumab) in Crohn's disease: the CLASSIC-I Trial. Gatsroeneterology (in the press).
Schreiber, S. et al. A randomized, placebo-controlled trial of certolizumab pegol (CDP870) in active Crohn's Disease. Gastroenterology, 129, 807–818 (2005). A number of alternatives to infliximab, targeting TNF, have been developed including certolizumab, a pegylated anti-TNF antibody fragment and adalimumab, a fully human anti-TNF antibody, which both appear likely to receive regulatory approval for the treatment of Crohn's disease.
Baert, F. et al. Influence of immunogenicity on the long-term efficacy of infliximab in Crohn's disease. N. Engl. J. Med. 348, 601–608 (2003). Infliximab, an anti-TNF inhibitor, has rapidly become a mainstay of therapy for severe Crohn's disease. However, this study was critical in identifying the significant problem of immunogenicity to infliximab, likely due to the murine component, which leads to loss of response in a sizeable proportion of individuals.
Hommes, D. et al. Inhibition of stress-activated MAP kinases induces clinical improvement in moderate to severe Crohn's disease. Gastroenterology 122, 7–14 (2002).
Oettinger, C. & D'Souza, M. Microencapsulation of tumor necrosis factor oligomers: a new approach to proinflammatory cytokine inhibition. J. Interferon Cytokine Res. 23, 533–543 (2003).
Ehrenpreis, E. D., Kane, S. V., Cohen, L. B., Cohen, R. D. & Hanauer, S. B. Thalidomide therapy for patients with refractory Crohn's disease: an open-label trial. Gastroenterology 117, 1271–1277 (1999).
Vasiliauskas, E. A. et al. An open-label pilot study of low-dose thalidomide in chronically active, steroid-dependent Crohn's disease. Gastroenterology 117, 1278–1287 (1999).
van Deventer, S. J. A place for TACE. Gut 51, 5–6 (2002).
Prehn, J. L. et al. Potent inhibition of cytokine production from intestinal lamina propria T cells by phosphodiesterase-4 inhibitory thalidomide analogues. J. Clin. Immunol. 21, 357–364 (2001).
Bauditz, J. et al. Treatment with tumour necrosis factor inhibitor oxpentifylline does not improve corticosteroid dependent chronic active Crohn's disease. Gut 40, 470–474 (1997).
Reimund, J. M. et al. In vitro effects of oxpentifylline on inflammatory cytokine release in patients with inflammatory bowel disease. Gut 40, 475–480 (1997).
Buchman, A. et al. Semapimod treatment in Crohn's disease. Gastroenterology 126, A-464 (2004).
Iyer, S., Lahana, R. & Buelow, R. Rational design and development of RDP58. Curr. Pharm. Des. 8, 2217–2229 (2002).
Travis, S. et al. RDP58 is a novel and potentially effective oral therapy for ulcerative colitis. Inflamm. Bowel Dis. 11, 713–719 (2005).
Lewis, J. D. et al. An open-label trial of the PPAR-γ ligand rosiglitazone for active ulcerative colitis. Am. J. Gastroenterol. 96, 3323–3328 (2001).
Chinetti, G., Fruchart, J. C. & Staels, B. Peroxisome proliferator-activated receptors (PPARs): nuclear receptors at the crossroads between lipid metabolism and inflammation. Inflamm. Res. 49, 497–505 (2000).
Chinetti, G. et al. Activation of proliferator-activated receptors α and γ induces apoptosis of human monocyte-derived macrophages. J. Biol. Chem. 273, 25573–25580 (1998).
Faveeuw, C. et al. Peroxisome proliferator-activated receptor γ activators inhibit interleukin-12 production in murine dendritic cells. FEBS Lett. 486, 261–266 (2000).
Su, C. G. et al. A novel therapy for colitis utilizing PPAR-γ ligands to inhibit the epithelial inflammatory response. J. Clin. Invest. 104, 383–389 (1999).
Fedorak, R. N. et al. Recombinant human interleukin 10 in the treatment of patients with mild to moderately active Crohn's disease. The Interleukin 10 Inflammatory Bowel Disease Cooperative Study Group. Gastroenterology 119, 1473–1482 (2000).
Schreiber, S. et al. Safety and efficacy of recombinant human interleukin 10 in chronic active Crohn's disease. Crohn's Disease IL-10 Cooperative Study Group. Gastroenterology 119, 1461–1472 (2000).
Sandborn, W. J. et al. Lack of effect of intravenous administration on time to respond to azathioprine for steroid-treated Crohn's disease. North American Azathioprine Study Group. Gastroenterology 117, 527–535 (1999).
van Deventer, S. J., Elson, C. O. & Fedorak, R. N. Multiple doses of intravenous interleukin 10 in steroid-refractory Crohn's disease. Crohn's Disease Study Group. Gastroenterology 113, 383–389 (1997).
Colombel, J. F. et al. Interleukin 10 (Tenovil) in the prevention of postoperative recurrence of Crohn's disease. Gut 49, 42–46 (2001).
Steidler, L. et al. Treatment of murine colitis by Lactococcus lactis secreting interleukin-10. Science 289, 1352–1355 (2000).
Van Montfrans, C. et al. Prevention of colitis by interleukin 10-transduced T lymphocytes in the SCID mice transfer model. Gastroenterology 123, 1865–1876 (2002).
Sasaki, M. et al. Transfection of IL-10 expression vectors into endothelial cultures attenuates α4β7-dependent lymphocyte adhesion mediated by MAdCAM-1. BMC Gastroenterol. 3, 3 (2003).
Braat, H. et al. Interleukin-10 producing Lactococcis lactis for the treatment of Crohn's disease. Gastroenterology 128, A104 (2005).
Yacyshyn, B. R. et al. A placebo-controlled trial of ICAM-1 antisense oligonucleotide in the treatment of Crohn's disease. Gastroenterology 114, 1133–1142 (1998).
Yacyshyn, B. R. et al. Double blind, placebo controlled trial of the remission inducing and steroid sparing properties of an ICAM-1 antisense oligodeoxy-nucleotide, alicaforsen (ISIS 2302), in active steroid dependent Crohn's disease. Gut 51, 30–36 (2002).
Chey, W., Volfova, M., Konecny, M., Rydzewska, G. & Fogel, R. Two Phase 3 Studies of Alicaforsen (ISIS-2302), An antisense oligonucleotide to human ICAM-1, in the treatment of moderate to severe Crohn's disease. Gastroenterology A112 (2005).
van Deventer, S. J., Tami, J. A. & Wedel, M. K. A randomised, controlled, double blind, escalating dose study of alicaforsen enema in active ulcerative colitis. Gut 53, 1646–1651 (2004).
van Deventer, S. J. et al. A Phase 2 dose ranging double blind placebo controlled trial of alicaforsen enema in subjects with acute exacerbation of mild to moderateleft-sided ulcerative colitis. Gastroenterology 128 (Suppl. 2), A–74 Abstract 490 (2005).
Podolsky, D. K. et al. Attenuation of colitis in the cotton-top tamarin by anti-α4 integrin monoclonal antibody. J. Clin. Invest. 92, 372–380 (1993).
Ghosh, S. et al. Natalizumab for active Crohn's disease. N. Engl. J. Med. 348, 24–32 (2003).
Miller, D. H. et al. A controlled trial of natalizumab for relapsing multiple sclerosis. N. Engl. J. Med. 348, 15–23 (2003).
Sandborn, W. et al. Natalizumab induction and maintenance therapy for Crohn's disease. N. Engl. J. Med. 353, 1912–1925 (2005). An antibody directed to integrin α4 subunit has been highly effective for preventing flares of multiple sclerosis and has also been effective for maintenance of remission in Crohn's disease, though treatment of acute flares was not demonstrated in this study.
Sandborn, W. et al. A phase III, double-blind, placebo-controlled study of the efficacy, safety, and tolerability of Antegren (Natalizumab) in maintaining clinical response and remission in Crohn's disease (ENACT-2). Digestive Dis. Week May 15–20, New Orleans, Louisiana (2004).
Berger, J. R. & Koralnik, I. J. Progressive multifocal leukoencephalopathy and natalizumab — unforeseen consequences. N. Engl. J. Med. 353, 414–416 (2005).
Van Assche, G. et al. Progressive multifocal leukoencephalopathy after natalizumab therapy for Crohn's disease. N. Engl. J. Med. 353, 362–368 (2005). An unanticipated adverse event documented in association with natalizumab was the development of progressive multifocal leukencephalopathy (PML) in those treated for multiple sclerosis as well as one patient with Crohn's disease.
Kleinschmidt-Demasters, B. K. & Tyler, K. L. Progressive multifocal leukoencephalopathy complicating treatment with natalizumab and interferon β-1a for multiple sclerosis. N. Engl. J. Med. 353, 367–374 (2005).
Langer-Gould, A., Atlas, S. W., Bollen, A. W. & Pelletier, D. Progressive multifocal leukoencephalopathy in a patient treated with natalizumab. N. Engl. J. Med. 353, 375–381 (2005).
Laghi, L. et al. JC virus DNA is present in the mucosa of the human colon and in colorectal cancers. Proc. Natl Acad. Sci. USA 96, 7484–7489 (1999).
Feagan, B., Greenberg, G. & Wild, G. Efficacy and safety of a humanized α4β7 antibody in active Crohn's disease. Gastroenterology 124, A25 (2003). A different selective adhesion molecule blockade has targeted integrin α4β7, more specific for the gastrointestinal tract, and appears promising for UC, though not effective in Crohn's disease.
Feagan, B. G. et al. Treatment of ulcerative colitis with a humanized antibody to the α4β7 integrin. N. Engl. J. Med. 352, 2499–2507 (2005).
Ayabe, T. et al. A pilot study of centrifugal leukocyte apheresis for corticosteroid-resistant active ulcerative colitis. Intern. Med. 36, 322–326 (1997).
Kawamura, A. et al. New technique of leukocytapheresis by the use of nonwoven polyester fiber filter for inflammatory bowel disease. Ther. Apher. 3, 334–337 (1999).
Reinisch, W. et al. Extracorporeal photochemotherapy in patients with steroid-dependent Crohn's disease: a prospective pilot study. Aliment Pharmacol. Ther. 15, 1313–1322 (2001).
Shimoyama, T. et al. Safety and efficacy of granulocyte and monocyte adsorption apheresis in patients with active ulcerative colitis: a multicenter study. J Clin Apheresis 16, 1–9 (2001).
Suzuki, Y., Yoshimura, N., Saniabadi, A. R. & Saito, Y. Selective granulocyte and monocyte adsorptive apheresis as a first-line treatment for steroid naive patients with active ulcerative colitis: a prospective uncontrolled study. Dig. Dis. Sci. 49, 565–571 (2004).
Sinha, A., Nightingale, J., West, K. P., Berlanga-Acosta, J. & Playford, R. J. Epidermal growth factor enemas with oral mesalamine for mild-to-moderate left-sided ulcerative colitis or proctitis. N. Engl. J. Med. 349, 350–357 (2003). Augmenting intestinal repair, promoted here through epidermal growth factor enemas for distal UC, produced highly effective results in a small study.
Mahmood, A., Melley, L., Fitzgerald, A. J., Ghosh, S. & Playford, R. J. Trial of trefoil factor 3 enemas, in combination with oral 5-aminosalicylic acid, for the treatment of mild-to-moderate left-sided ulcerative colitis. Aliment Pharmacol. Ther. 21, 1357–1364 (2005).
Sandborn, W. J. et al. Repifermin (keratinocyte growth factor-2) for the treatment of active ulcerative colitis: a randomized, double-blind, placebo-controlled, dose-escalation trial. Aliment Pharmacol. Ther. 17, 1355–1364 (2003).
Jeffers, M. et al. A novel human fibroblast growth factor treats experimental intestinal inflammation. Gastroenterology 123, 1151–1162 (2002).
Slonim, A. E. et al. A preliminary study of growth hormone therapy for Crohn's disease. N. Engl. J. Med. 342, 1633–1637 (2000).
Decker, D. et al. Perioperative treatment with human growth hormone down-regulates apoptosis and increases superoxide production in PMN from patients undergoing infrarenal abdominal aortic aneurysm repair. Growth Horm. IGF Res. 15, 193–199 (2005).
Korzenik, J. R. & Dieckgraefe, B. K. Is Crohn's disease an immunodeficiency? A hypothesis suggesting possible early events in the pathogenesis of Crohn's disease. Dig. Dis. Sci. 45, 1121–1129 (2000).
Dieckgraefe, B. K., Korzenik, J. R., Husain, A. & Dieruf, L. Association of glycogen storage disease 1b and Crohn disease: results of a North American survey. Eur. J. Pediatr. 161 (Suppl 1), S88–S92 (2002).
Korzenik, J. R. & Dieckgraefe, B. K. An open-labelled study of granulocyte colony-stimulating factor in the treatment of active Crohn's disease. Aliment Pharmacol. Ther. 21, 391–400 (2005).
Dieckgraefe, B. K. & Korzenik, J. R. Treatment of active Crohn's disease with recombinant human granulocyte-macrophage colony-stimulating factor. Lancet 360, 1478–1480 (2002).
Korzenik, J. R., Dieckgraefe, B. K., Valentine, J. F., Hausman, D. F. & Gilbert, M. J. Sargramostim for active Crohn's disease. N. Engl. J. Med. 352, 2193–2201 (2005). A different hypothesis considered Crohn's as an innate immune deficiency and formed the basis for the study of granulocyte-macrophage colony stimulating factor, or sargramostim, a novel agent for the treatment of Crohn's disease.
Wehkamp, J. et al. Inducible and constitutive β-defensins are differentially expressed in Crohn's disease and ulcerative colitis. Inflamm. Bowel. Dis. 9, 215–223 (2003).
Klein, W. et al. A polymorphism of the bactericidal/permeability increasing protein (BPI) gene is associated with Crohn's disease. J. Clin. Gastroenterol. 39, 282–283 (2005).
Rachmilewitz, D. et al. Toll-like receptor 9 signaling mediates the anti-inflammatory effects of probiotics in murine experimental colitis. Gastroenterology 126, 520–528 (2004).
Rigby, R. J., Knight, S. C., Kamm, M. A. & Stagg, A. J. Production of interleukin (IL)-10 and IL-12 by murine colonic dendritic cells in response to microbial stimuli. Clin. Exp. Immunol. 139, 245–256 (2005).
Hart, A. L. et al. Modulation of human dendritic cell phenotype and function by probiotic bacteria. Gut 53, 1602–1609 (2004).
Gionchetti, P. et al. Oral bacteriotherapy as maintenance treatment in patients with chronic pouchitis: a double-blind, placebo-controlled trial. Gastroenterology 119, 305–309 (2000). The benefit of probiotics was most dramatically demonstrated for use in pouchitis, a very antibiotic sensitive subgroup of IBD, though the promise of this approach is yet to be established for Crohn's disease or UC.
Boudeau, J., Glasser, A. L., Julien, S., Colombel, J. F. & Darfeuille-Michaud, A. Inhibitory effect of probiotic Escherichia coli strain Nissle 1917 on adhesion to and invasion of intestinal epithelial cells by adherent-invasive E. coli strains isolated from patients with Crohn's disease. Aliment Pharmacol. Ther. 18, 45–56 (2003).
Sturm, A. et al. Escherichia coli Nissle 1917 distinctively modulates T-cell cycling and expansion via toll-like receptor 2 signaling. Infect Immun 73, 1452–1465 (2005).
Rembacken, B. J., Snelling, A. M., Hawkey, P. M., Chalmers, D. M. & Axon, A. T. Non-pathogenic Escherichia coli versus mesalazine for the treatment of ulcerative colitis: a randomised trial. Lancet 354, 635–639 (1999).
Schultz, M. et al. Lactobacillus GG in inducing and maintaining remission of Crohn's disease. BMC Gastroenterol 4, 5 (2004).
Prantera, C., Scribano, M. L., Falasco, G., Andreoli, A. & Luzi, C. Ineffectiveness of probiotics in preventing recurrence after curative resection for Crohn's disease: a randomised controlled trial with Lactobacillus GG. Gut 51, 405–409 (2002).
Guslandi, M., Mezzi, G., Sorghi, M. & Testoni, P. A. Saccharomyces boulardii in maintenance treatment of Crohn's disease. Dig. Dis. Sci. 45, 1462–1464 (2000).
Guslandi, M., Giollo, P. & Testoni, P. A. A pilot trial of Saccharomyces boulardii in ulcerative colitis. Eur J Gastroenterol Hepatol 15, 697–698 (2003).
Videla, S. et al. Dietary inulin improves distal colitis induced by dextran sodium sulfate in the rat. Am. J. Gastroenterol. 96, 1486–1493 (2001).
Lindsay, J. et al. The clinical, microbiological and immunological effects of fructo-oligosaccharide in patients with active ileocolonic Crohn's disease. Gastroenterology 128, A112 (2005).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
J.R.K. has received consulting and lecture fees from Proctor & Gamble, Shire Pharmaceuticals, Isis Pharmaceuticals, Cytokine Pharmasciences, Berlex and Centocor, and research support from Danisco. A US patent entitled 'Stimulating neutrophil function to treat inflammatory bowel disease' (6,500,418) was issued 31 December 2002, on which J.R.K. is an inventor. The patent is owned by Washington University and licensed by Berlex Laboratories. D.K.P. has equity in and serves as a consultant to The GI Company.
Related links
Glossary
- Ulcerative colitis
-
One of the two main forms of IBD with unknown aetiology, which causes an inflammatory response restricted to the colon, beginning at the rectum and spreading proximally to differing extents.
- Crohn's disease
-
One of the two main forms of IBD with unknown aetiology, characterized by inflammation that can occur anywhere in the gastrointestinal tract, affecting the terminal ileum in more than 70% of individuals.
- Probiotic
-
The use of live bacteria as a therapeutic agent to induce a benefit by altering the microbial balance.
- Innate immune response
-
The innate immune system comprises elements of the immune system that generate a nonspecific reaction to a potential pathogen (for example, superoxide burst for bactericidal function), which contrasts with an adaptive response (for example, an antibody produced by a B cell against a particular antigen).
- CARD15
-
The first gene identified as a susceptibility factor for the development of CD. How the defective gene leads to intestinal inflammation and CD remains an area of controversy.
- Toll-like receptors
-
(TLRs). A group of transmembrane receptors featuring specific pattern-recognition receptors (PRRs) that bind to pathogen-associated molecular patterns (PAMPs) to direct an appropriate immune response.
- Type 1 helper T-cells (TH1)
-
A subclass of CD4+ cells that produce a characteristic immune response with a cytokine profile which includes IL-2, IFNγ and IL-12.
- Type 2 helper T-cells (TH2)
-
A subclass of CD4+ cells that produce a characteristic immune response with a cytokine profile which includes IL-4, IL-5 and IL-13.
- Crohn's Disease Activity Index (CDAI)
-
A composite score determined from various symptoms, clinical complications, the physician's exam, haematocrit and weight, which forms the standard scoring of disease severity used in trials of therapeutic agents for CD. A score below 150 is considered remission and above 220 is considered moderately active disease. A decrease in 70–100 points is considered the minimum reduction for a 'therapeutic' response.
- Tregs
-
A subpopulation of T cells which function to suppress differentiation and activation of other T-cell subsets.
- Anti-idiotype antibodies
-
Antibodies generated against another antibody.
- Pouchitis
-
Patients with UC can undergo an operation in which the colon is removed and a new rectum 'pouch' is fashioned from the terminal ileum. As many as 50% of people will have one episode of inflammation in the pouch, termed pouchitis.
- Proctocolectomy
-
A surgical procedure in which the entire colon and rectum are resected.
- Prebiotic
-
A non-digested product, usually a complex carbohydrate, which enhances the proliferation of certain bacteria to change the microbial composition and induce a therapeutic effect.
Rights and permissions
About this article
Cite this article
Korzenik, J., Podolsky, D. Evolving knowledge and therapy of inflammatory bowel disease. Nat Rev Drug Discov 5, 197–209 (2006). https://doi.org/10.1038/nrd1986
Issue Date:
DOI: https://doi.org/10.1038/nrd1986
This article is cited by
-
Efficient production of levan using a recombinant yeast Saccharomyces cerevisiae hypersecreting a bacterial levansucrase
Journal of Industrial Microbiology and Biotechnology (2019)
-
Biologic treatment of Japanese patients with inflammatory bowel disease
BMC Gastroenterology (2018)
-
Inflammatory bowel disease in patients with Hirschsprung’s disease: a systematic review and meta-analysis
Pediatric Surgery International (2018)
-
Tocilizumab in the treatment of twelve cases with aa amyloidosis secondary to familial mediterranean fever
Orphanet Journal of Rare Diseases (2017)
-
Predicting Pre-emptive Discussions of Biologic Treatment: Results from an Openness and Preference Survey of Inflammatory Bowel Disease Patients and Their Prescribers
Advances in Therapy (2017)