Key Points
-
Estimates of incidence of endometriosis vary from <10 to >20% of women
-
Although considered rare, endometriosis of the urinary tract might be more common than previously thought, owing to changing definitions and a lack of recognition by surgeons
-
Endometriosis of the ureter can result in silent kidney loss if not effectively managed
-
Treatment options differ depending on whether the endometriosis is superficial or deep infiltrating, and also on the site of the lesions
-
Laparoscopy with or without robotic assistance is feasible and advisable to treat urinary tract endometriosis
Abstract
Endometriosis predominantly affects the pelvic reproductive organs but can also affect the urinary tract. A number of theories for the pathogenesis of endometriosis have been suggested, but the exact mechanisms remain elusive. Endometriotic lesions can be found on both the ureter and bladder, and the optimal therapeutic approach depends on the extent, depth, and location of these lesions. Medical approaches, including hormonal therapies such as GnRH agonists and oral contraceptives, tend to be a temporary measure, but can be useful in a preoperative setting or if the patient is unsuitable for surgery, and are also useful as a postoperative treatment. If surgical resection is deemed appropriate, laparoscopic management with or without robotic assistance of urological endometriosis is feasible and advisable. Newer techniques, such as nerve-sparing surgery, might help to decrease the risk of urinary complications following resection of deeply infiltrating endometriosis.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout









Similar content being viewed by others
References
Veeraswamy, A. et al. Extragenital endometriosis. Clin. Obstet. Gynecol. 53, 449–466 (2010).
Nezhat, C. et al. in Nezhat's Video-Assisted and Robotic-Assisted Laparoscopy and Hysteroscopy 4th edn (eds Nezhat, C., Nezhat, F. & Nezhat, C.) 265–302 (Cambridge Univ. Press, 2013).
Nezhat, C., Modest, A. M. & King, L. P. The role of the robot in treating urinary tract endometriosis. Curr. Opin. Obstet. Gynecol. 25, 308–311 (2013).
Nezhat, C., Nezhat, F. & Green, B. Laparoscopic treatment of obstructed ureter due to endometriosis by resection and ureteroureterostomy: a case report. J. Urol. 148, 865–868 (1992).
Nezhat, C. & Winer, W. Is endoscopic treatment of endometriosis and endemetrioma associated with better results than laparotomy. Am. J. Gynecol. Health 2, 10–16 (1987).
Nezhat, C. R., Winer, W., Nezhat, F. & Nezhat, C. Laparoscopic treatment of endometriosis with laser and videocamera augmentation (videolaseroscopy). J. Gynecol. Surg. 5, 163–169 (2009).
Donnez, J. CO2 laser laparoscopy in infertile women with endometriosis and women with adnexal adhesions. Fertil. Steril. 48, 390–394 (1987).
Fedele, L. et al. Long-term follow-up after conservative surgery for bladder endometriosis. Fertil. Steril. 83, 1729–1733 (2005).
Guntupalli, S. et al. Preparedness of obstetrics and gynecology residents for fellowship training. Obstet. Gynecol. 126, 559–568 (2015).
Bosev, D. et al. Laparoscopic management of ureteral endometriosis: the Stanford University hospital experience with 96 consecutive cases. J. Urol. 182, 2748–2752 (2009).
Bateman, B., Kolp, L. & Mills, S. Endoscopic versus laparotomy management of endometriomas. Fertil. Steril. 62, 690–695 (1994).
Hart, R., Hickey, M., Maouris, P. & Buckett, W. Excisional surgery versus ablative surgery for ovarian endometriomata. Cochrane Database Syst. Rev. 16, CD004992 (2008).
Scioscia, M., Molon, A., Grosso, G. & Minelli, L. Laparoscopic management of ureteral endometriosis. Curr. Opin. Obstet. Gynecol. 21, 325–328 (2009).
Sanfilippo, J., Wakim, N., Schikler, K. & Yussman, M. Endometriosis in association with uterine anomaly. Am. J. Obstet. Gynecol. 154, 39–43 (1986).
Halme, J., Hammond, M., Hulka, J., Raj, S. & Talbert, L. Retrograde menstruation in healthy women and in patients with endometriosis. Obstet. Gynecol. 64, 151–154 (1984).
Burney, R. O. & Giudice, L. C. Pathogenesis and pathophysiology of endometriosis. Fertil. Steril. 98, 511–519 (2012).
Dmowski, W. & Radwanska, E. Current concepts on pathology, histogenesis and etiology of endometriosis. Acta Obstet. Gynecol. Scand. Suppl. 123, 29–33 (1984).
Harada, T., Iwabe, T. & Terakawa, N. Role of cytokines in endometriosis. Fertil. Steril. 76, 1–10 (2001).
Burney, R. O. & Giudice, L. C. in Nezhat's Video-Assisted and Robotic-Assisted Laparoscopy and Hysteroscopy 4th edn (eds Nezhat, C., Nezhat, F. & Nezhat, C.) 252–258 (Cambridge Univ. Press, 2013).
Cavaco-Gomes, B. et al. Laparoscopic management of ureteral endometriosis: a systematic review. Eur. J. Obstet. Gynecol. Reprod. Biol. 210, 94–101 (2017).
Berlanda, N. et al. Ureteral and vesical endometriosis. Two different clinical entities sharing the same pathogenesis. Obstet. Gynecol. Surv. 64, 830–842 (2009).
Sinaii, N., Cleary, S. D., Ballweg, M. L., Nieman, L. K. & Stratton, P. High rates of autoimmune and endocrine disorders, fibromyalgia, chronic fatigue syndrome and atopic diseases among women with endometriosis: a survey analysis. Hum. Reprod. 17, 2715–2724 (2002).
Price, D. et al. Vesical endometriosis: report of two cases and review of the literature. Urology 48, 639–643 (1996).
Vercellini, P., Meschia, M. & De Giorgi, O. Bladder detrusor endometriosis: clinical and pathogenetic implications. J. Urol. 155, 84–86 (1996).
Buka, N. Vesical endometriosis after cesarean section. Am. J. Obstet. Gynecol. 158, 1117–1118 (1988).
Simpson, J. L., Elias, S., Malinak, L. R. & Buttram, V. C. Heritable aspects of endometriosis. I. Genetic studies. Am. J. Obstet. Gynecol. 137, 327–331 (1980).
Rahmioglu, N., Missmer, S., Montgomery, G. & Zondervan, K. Insights into assessing the genetics of endometriosis. Curr. Obstet. Gynecol. Rep. 1, 124–137 (2012).
Saha, R. et al. Heritability of endometriosis. Fertil. Steril. 104, 947–952 (2015).
Zondervan, K. et al. Significant evidence of one or more susceptibility loci for endometriosis with near-Mendelian inheritance on chromosome 7p13-15. Hum. Reprod. 22, 717–728 (2007).
Rahmioglu, N. et al. Genetic variants underlying risk of endometriosis: insights from meta-analysis of eight genome-wide association andreplication datasets. Hum. Reprod. Update 20, 702–716 (2014).
Sapkota, Y. et al. Independent replication and meta-analysis for endometriosis risk loci. Twin Res. Hum. Genet. 18, 518–525 (2015).
Kamergorodsky, G., Ribeiro, A. & Galvao, L. Histologic classification of specimens from women affected by superficial endometriosis, deeply infiltrating endometriosis, and ovarian endometriomas. Fertil. Steril. 92, 2074–2077 (2009).
Nisolle, M. & Donnez, J. Peritoneal endometriosis ovarian endometriosis, and adenomyotic nodules of the rectovaginal septum are three different entities. Fertil. Steril. 68, 585–596 (1997).
Carrarelli, P. et al. Increased expression of antimüllerian hormone and its receptor in endometriosis. Fertil. Steril. 101, 1353–1358 (2014).
Tosti, C., Pinzauti, S., Santulli, P., Chapron, C. & Petraglia, F. Pathogenetic mechanisms of deep infiltrating endometriosis. Reprod. Sci. 22, 1053–1059 (2015).
Gustilo-Ashby, A. & Paraiso, M. Treatment of urinary tract endometriosis. J. Minim. Invasive Gynecol. 13, 559–565 (2006).
Donnez, J., Nisolle, M. & Squifflet, J. Ureteral endometriosis: a complication of rectovaginal endometriotic (adenomyotic) nodules. Fertil. Steril. 77, 32–37 (2002).
Shook, T. & Nyberg, L. Endometriosis of the urinary tract Urology. Urology 31, 1–6 (1988).
Nezhat, C., Paka, C., Gomaa, M. & Schipper, E. Silent loss of kidney seconary to ureteral endometriosis. JSLS 16, 451–455 (2012).
Kołodziej, A., Krajewski, W., Dołowy, Ł. & Hirnle, L. Urinary tract endometriosis. Urol. J. 12, 2213–2217 (2015).
Al-Fozan, H. & Tulandi, T. Left lateral predisposition of endometriosis and endometrioma. Obstet. Gynecol. 101, 164–166 (2003).
Vercellini, P. et al. Is ureteral endometriosis an asymmetric disease? BJOG 107, 559–561 (2000).
Comiter, C. V. Endometriosis of the urinary tract. Urol. Clin. North Am. 29, 625–635 (2002).
Donnez, J. & Brosens, I. Definition of ureteral endometriosis? Fertil. Steril. 68, 178–180 (1997).
Clement, P. B. in Blaustein's Pathology of the Female Genital Tract 3rd edn (ed. Kurman, R. J.) 516–559 (Springer, 1987).
Yohannes, P. Ureteral endometriosis. J. Urol. 170, 20–25 (2003).
Berlanda, N. et al. Surgery versus hormonal therapy for deep endometriosis: is it a choice of the physician? Eur. J. Obstet. Gynecol. Reprod. Biol. 209, 67–71 (2016).
Iosca, S. et al. Multislice computed tomography with colon water distension (MSCT-c) in the study of intestinal and ureteral endometriosis. Clin. Imaging 37, 1061–1068 (2013).
Medeiros, L. et al. Accuracy of magnetic resonance in deeply infiltrating endometriosis: a systematic review and meta-analysis. Arch. Gynecol. Obstet. 291, 611–621 (2015).
Kinkel, K., Frei, K. A., Balleyguier, C. & Chapron, C. Diagnosis of endometriosis with imaging: a review. Eur. Radiol. 16, 285–298 (2006).
Pateman, K. et al. Visualization of ureters on standard gynecological transvaginal scan: a feasibility study. Ultrasound Obstet. Gynecol. 41, 696–701 (2013).
Guerriero, S. et al. Systematic approach to sonographic evaluation of the pelvis in women with suspected endometriosis, including terms, definitions and measurements: a consensus opinion from the International Deep Endometriosis Analysis (IDEA) group. Ultrasound Obstet. Gynecol. 48, 318–332 (2016).
Shokeir, A., Provoost, A. & Nijman, R. Recoverability of renal function after relief of chronic partial upper urinary tract obstruction. BJU Int. 83, 11–17 (1999).
Sillou, S., Poirée, S., Millischer, A. E., Chapron, C. & Hélénon, O. Urinary endometriosis: MR imaging appearance with surgical and histological correlations. Diagn. Interv. Imaging 96, 373–381 (2015).
Nisenblat, V., Bossuyt, P. M., Farquhar, C., Johnson, N. & Hull, M. L. Imaging modalities for the non-invasive diagnosis of endometriosis. Cochrane Database Syst. Rev. 26, CD009591 (2016).
Takeuchi, M., Matsuzaki, K. & Harada, M. Susceptibility-weighted MRI of extra-ovarian endometriosis: preliminary results. Abdom. Imaging 40, 2512–2516 (2015).
Knabben, L. et al. Urinary tract endometriosis in patients with deep infiltrating endometriosis: prevalence, symptoms, management, and proposal for a new clinical classification. Fertil. Steril. 103, 147–152 (2015).
Uccella, S. et al. Laparoscopy for ureteral endometriosis: surgical details, long-term follow-up, and fertility outcomes. Fertil. Steril. 102, 160–166 (2014).
Nezhat, C. & Nezhat, F. Operative laparoscopy (minimally invasive surgery): state of the art. J. Gynecol. Surg. 8, 111–141 (1992).
Nezhat, C. H., Malik, S., Nezhat, F. & Nezhat, C. Laparoscopic ureteroneocystostomy and vesicopsoas hitch for infiltrative endometriosis. JSLS 8, 3–7 (2004).
Nezhat, C. H., Malik, S., Osias, J., Nezhat, F. & Nezhat, C. Laparoscopic management of 15 patients with infiltrating endometriosis of the bladder and a case of primary intravesical endometrioid adenosarcoma. Fertil. Steril. 78, 872–875 (2002).
Nezhat, C. et al. Robotic versus standard laparoscopy for the treatment of endometriosis. Fertil. Steril. 94, 2758–2760 (2010).
Nezhat, C., Nezhat, F., Seidman, D. & Nezhat, C. Laparoscopic ureteroureterostomy: a prospective follow-up of 9 patients. Prim. Care Update Ob. Gyns. 5, 200 (1998).
Nezhat, C. et al. Urinary tract endometriosis treated by laparoscopy. Fertil. Steril. 66, 920–924 (1996).
Isac, W. et al. Robot-assisted ureteroneocystostomy: technique and comparative outcomes. J. Endourol. 27, 318–323 (2013).
Autorino, R., Zargar, H. & Kaouk, J. H. Robotic-assisted laparoscopic surgery: recent advances in urology. Fertil. Steril. 102, 939–949 (2014).
Efe, E. et al. Hormonal treatment for severe hydronephrosis caused by bladder endometriosis. Case Rep. Urol. 2014, 891295 (2014).
De Cicco, C., Ussia, A. & Koninckx, P. R. Laparoscopic ureteral repair in gynaecological surgery. Curr. Opin. Obstet. Gynecol. 23, 296–300 (2011).
Nezhat, C. & Nezhat, F. Laparoscopic repair of ureter resected during operative laparoscopy. Obstet. Gynecol. 80, 543–544 (1992).
Nezhat, C., Hajhosseini, B. & King, L. P. Robotic-assisted laparoscopic treatment of bowel, bladder, and ureteral endometriosis. JSLS 15, 387–392 (2011).
Fadhlaoui, A., Gillon, T., Lebbi, I., Bouquet de Jolinière, J. & Feki, A. Endometriosis and vesico-sphincteral disorders. Front. Surg. 2, 23 (2015).
Symons, S., Kurien, A. & Desai, M. Laparoscopic ureteral reimplantation: a single center experience and literature review. J. Endourol. 23, 269–274 (2009).
Phillips, E. A. & Wang, D. S. Current status of robot-assisted laparoscopic ureteral reimplantation and reconstruction. Curr. Urol. Rep. 13, 190–194 (2012).
Kondo, W. et al. Surgery for deep infiltrating endometriosis: technique and rationale. Front. Biosci. (Elite Ed.) 5, 316–332 (2013).
Mu, D., Li, X., Zhou, G. & Guo, H. Diagnosis and treatment of ureteral endometriosis: study of 23 cases. Urol. J. 11, 1806–1812 (2014).
Camanni, M. et al. Laparoscopic conservative management of ureteral endometriosis: a survey of eighty patients submitted to ureterolysis. Reprod. Biol. Endocrinol. 7, 109 (2009).
Nezhat, C. & Nezhat, F. Safe laser endoscopic excision or vaporization of peritoneal edometriosis. Fertil. Steril. 52, 149–151 (1989).
Nezhat, C., Winer, W. & Nezhat, F. A. Comparison of the CO2, argon, and KTP/532 lasers in the videolaseroscopic treatment of endometriosis. J. Gynecol. Surg. 4, 41–47 (2009).
Azioni, G. et al. Laparoscopic ureteroneocystostomy and vesicopsoas hitch for infiltrative ureteral endometriosis. Minim. Invasive Ther. Allied Technol. 19, 292–297 (2010).
Stepniewska, A. et al. Ureteral endometriosis: clinical and radiological follow-up after laparoscopic ureterocystoneostomy. Hum. Reprod. 26, 112–116 (2011).
Antonelli, A. Urinary tract endometriosis. Urologia 79, 167–170 (2012).
Nezhat, C. H., Nezhat, F. R., Freiha, F. & Nezhat, C. R. Laparoscopic vesicopsoas hitch for infiltrative ureteral endometriosis. Fertil. Steril. 71, 376–379 (1999).
Thonnon, C. et al. Three-dimensional ultrasound in the management of bladder endometriosis. J. Minim. Invasive Gynecol. 22, 403–409 (2015).
Nezhat, C. & Nezhat, F. Laparoscopic segmental bladder resection for endometriosis: a report of two cases. Obstet. Gynecol. 81, 882–884 (1993).
Cornell, K. Cystotomy, partial cystectomy, and tube cystostomy. Clin. Tech. Small Anim. Pract. 15, 11–16 (2000).
Hastings, J. C., Van Winkle, W., Barker, E., Hines, D. & Nichols, W. The effect of suture materials on healing wounds of the bladder. Surg. Gynecol. Obstet. 140, 933–937 (1975).
Maggiore, L. R. et al. Bladder endometriosis: a systematic review of pathogenesis, diagnosis, treatment, impact on fertility, and risk of malignant transformation. Eur Urol. 71, 790–807 (2017).
Noël, J.-C. et al. Estrogen and progesterone receptors in smooth muscle component of deep infiltrating endometriosis. Fertil. Steril. 93, 1774–1777 (2010).
Westney, O. L., Amundsen, C. L. & McGuire, E. J. Bladder endometriosis: conservative management. J. Urol. 163, 1814–1817 (2000).
Angioni, S. et al. Dienogest. A possible conservative approach in bladder endometriosis. Results of a pilot study. Gynecol. Endocrinol. 31, 406–408 (2015).
Bourdel, N. et al. Laparoscopic ureteroneocystostomy: be prepared! J. Minim. Invasive Gynecol. 22, 827–833 (2015).
Chamsy, D., King, C. & Lee, T. The use of barbed suture for bladder and bowel repair. J. Minim. Invasive Gynecol. 22, 648–652 (2015).
Chapron, C. et al. Surgery for bladder endometriosis: long-term results and concomitant management of associated posterior deep lesions. Hum. Reprod. 25, 884–889 (2010).
Antonelli, A. et al. Clinical aspects and surgical treatment of urinary tract endometriosis: our experience with 31 cases. Eur. Urol. 49, 1093–1098 (2006).
Panel, P. et al. Bladder symptoms and urodynamic observations of patients with endometriosis confirmed by laparoscopy. Int. Urogynecol. J. 27, 445–451 (2016).
Serati, M. et al. Deep endometriosis and bladder and detrusor functions in women without urinary symptoms: a pilot study through an unexplored world. Fertil. Steril. 100, 1332–1336 (2013).
Lemos, N. et al. Laparoscopic anatomy of the autonomic nerves of the pelvis and the concept of nerve-sparing surgery by direct visualization of autonomic nerve bundles. Fertil. Steril. 104, e11–e12 (2015).
Possover, M., Quakernack, J. & Chiantera, V. The LANN technique to reduce postoperative functional morbidity in laparoscopic radical pelvic surgery. J. Am. Coll. Surg. 201, 913–917 (2005).
Ceccaroni, M. et al. Nerve-sparing laparoscopic eradication of deep endometriosis with segmental rectal and parametrial resection: the Negrar method. A single-center, prospective, clinical trial. Surg. Endosc. 26, 2029–2045 (2012).
de Resende, J. A. Jr, Cavalini, L. T., Crispi, C. P. & de Freitas Fonseca, M. Risk of urinary retention after nerve-sparing surgery for deep infiltrating endometriosis: a systematic review and meta-analysis. Neurourol. Urodyn. 36, 57–61 (2015).
Nezhat, F., Pejovic, T., Reis, F. & Guo, S. The link between endometriosis and ovarian cancer: clinical implications. Int. J. Gynecol. Cancer. 24, 623–628 (2014).
Kim, H., Kim, T., Chung, H. & Song, Y. Risk and prognosis of ovarian cancer in women with endometriosis: a meta-analysis. Br. J. Cancer 110, 1878–1890 (2014).
Melin, A., Sparén, P., Persson, I. & Bergqvist, A. Endometriosis and the risk of cancer with special emphasis on ovarian cancer. Hum. Reprod. 21, 1237–1242 (2006).
Brinton, L., Gridley, G., Persson, I., Baron, J. & Bergqvist, A. Cancer risk after a hospital discharge diagnosis of endometriosis. Am. J. Obstet. Gynecol. 176, 572–579 (1997).
Nezhat, F., Apostal, R., Nezhat, C. & Pejovic, T. New insights in the pathophysiology of ovarian cancer and implications for screening and prevention. Am. J. Obstet. Gynecol. 213, 262–267 (2015).
Acknowledgements
We would like to thank Sahar Houshdaran of the University of California at San Francisco for her contributions to the genetics portion of this paper. For their review of the manuscript, we would also like to thank Ceana Nezhat of the Atlanta Center for Minimally Invasive Surgery and Reproductive Medicine, and Farr Nezhat of Nezhat Surgery for Gynecology/Oncology in New York. We also thank Gity Meshkat Razavi for her help with drawing up the original figures in this article.
Author information
Authors and Affiliations
Contributions
All four authors researched data for the article and wrote the manuscript. C.N., R.F., and L.K. took part in discussions of content. C.N. and R.F. reviewed and edited the manuscript before submission.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Supplementary information
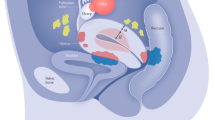
DIE at the bladder base.
The sonographer evaluates the size, location, and extent of a deeply infiltrative endometriosis lesion at the bladder base. This type of assessment can aid a physician in understanding endometriosis as the cause of a patient's UTI-like symptoms and help them counsel the patient on operative planning. Preoperative knowledge of a bladder endometrioma informs the surgeon of whom to gather for an interdisciplinary surgical team, often including a laparoscopically trained urologist and/or minimally invasively trained gynaecology expert. Permission obtained from ISUOG; published by John Wiley and Sons Ltd. © Guerriero, S. et al. Ultrasound Obstet. Gynecol. 48, 318–332 (2016). (MP4 6757 kb)
Laparoscopic treatment of endometriosis of the ureter with and without robotic assistance.
In this video, multiple forms of urinary tract endometriosis are classified and laparoscopic management strategies described. First, ureterolysis of extrinsic (superficial) disease of the ureter is shown, using robotic assistance. Next, release of a choked ureter constricted by endometriosis is demonstrated and then ureteroureterostomy for intrinsic (deeply invasive) endometriosis necessitating excision of a segment of ureter is shown. Next, ureterolysis and peritoneal stripping with robotic assistance is described. Use of the CO2 laser for excision and vaporization of endometriotic lesions as well as the role of hydrodissection in protecting the ureter and other vital structures from harm is shown in all cases. Finally, two cases of laparoscopic segmental bladder resection of deeply infiltrating endometriosis are shown, one performed with robotic assistance and one without. In both cases, cystoscopy is routinely performed to guide operative cystotomy. Complete excision of the deeply infiltrating endometriosis is required, with a 5 mm margin. Following the excision, bilateral stents are placed in the ureters, and the bladder is closed with 4–0 through-and-through. With or without robot assistance, the operative surgeon must be comfortable and adept at laparoscopic suturing of the bladder. (MP4 107967 kb)
Rights and permissions
About this article
Cite this article
Nezhat, C., Falik, R., McKinney, S. et al. Pathophysiology and management of urinary tract endometriosis. Nat Rev Urol 14, 359–372 (2017). https://doi.org/10.1038/nrurol.2017.58
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrurol.2017.58
This article is cited by
-
Acute abdominal pain in women of reproductive age: keys to suggest a complication of endometriosis
Insights into Imaging (2023)
-
Comprehensive surgical treatment for obstructive rectal endometriosis: a case report and review of the literature
BMC Women's Health (2022)
-
Laparoscopic Resection of Renal Capsular Endometriosis in a Woman with Menstrual-Related Flank Pain: Case Report
African Journal of Urology (2021)
-
Protective effect of cabergoline on mitochondrial oxidative stress-induced apoptosis is mediated by modulations of TRPM2 in neutrophils of patients with endometriosis
Journal of Bioenergetics and Biomembranes (2020)
-
Total laparoscopic bladder resection in the management of deep endometriosis: “take it or leave it.” Radicality versus persistence
International Urogynecology Journal (2020)