Abstract
Activating mutations of the Ca2+-sensing receptor (CaR) gene cause autosomal dominant hypoparathyroidism. Functional expression studies have been reported for several mutations, but have produced conflicting results. Thus, the mechanism by which these mutations activate the receptor is unclear. We describe here a new family with autosomal dominant hypoparathyroidism. The mother and three daughters experienced muscle spasms and/or seizures from early childhood. They were treated with oral calcium and vitamin D analogs, and all four patients developed hypercalciuria, nephrocalcinosis, and renal insufficiency. In this family, we identified a heterozygous missense mutation(F612S) involving the extracellular region of the CaR. The mutation cosegregated with disease. It was not present in 50 normal control individuals. We used site-directed mutagenesis to introduce this mutation into the CaR cDNA, and then expressed the mutant receptor in human embryonic kidney(HEK)-293 cells. In these cells, the accumulation of inositol phosphates was measured as a function of extracellular Ca2+ concentration. Compared with the wild-type receptor, the mutant receptor showed a left-shift in the concentration-response curve and an increase in the maximal response to high Ca2+ concentrations. These effects did not appear to be mediated by changes in levels of receptor expression, as judged by ELISA, or by changes in receptor glycosylation, as judged by Western analysis. We conclude that this CaR mutation causes hypoparathyroidism by a dual increase in receptor sensitivity to extracellular Ca2+ and maximal signal transduction capacity.
Similar content being viewed by others
Main
The CaR is a 7-transmembrane domain, G protein-coupled receptor that binds the extracellular calcium ion. The activated receptor, acting through a G protein, stimulates phospholipase C activity thus increasing inositol 1,4,5-trisphosphate production and secondarily increasing cytoplasmic Ca2+ concentrations(1, 2).
The CaR is expressed in parathyroid, kidney, and other tissues. In parathyroid, the receptor negatively regulates PTH secretion. In kidney, the receptor is thought to negatively regulate Ca2+ reabsorption in the thick ascending limb(3). Thus, inactivating mutations in the CaR increase PTH secretion and decrease urinary Ca2+ excretion, leading to familial hypocalciuric hypercalcemia(4, 5).
We and others recently reported missense mutations in the CaR gene in autosomal dominant hypoparathyroidism and in sporadic hypoparathyroidism(6–10). These patients also manifest a characteristic hypercalciuria, which can lead to renal complications(6, 10). To explain the phenotype, it was hypothesized that these mutations activate the receptor. To test that hypothesis and to elucidate the mechanism of activation, the WT receptor and four of these mutant receptors have been expressed in cultured mammalian cells(10–12). When exposed to increasing Ca2+ concentrations, cells expressing the mutant receptor have shown altered concentration-response curves. When cytoplasmic Ca2+ response was assessed, all four of the mutations thus far studied showed a left-shift in the concentration-response curve. However, when the IP response was assessed, the mutations produced an unusual biphasic concentration-response curve with maximal response occurring at a Ca2+ concentration of 1.0-2.0 mM and a decreasing response at higher Ca2+ concentrations. Furthermore, these studies did not quantitate cell surface expression of the mutant receptors. For these reasons, the mechanism by which these mutations activate the receptor is unclear.
METHODS
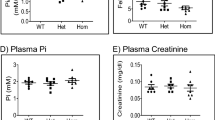
Patients. We studied a family in which the mother and three daughters had hypoparathyroidism. The mother had a history of intermittent tremors, muscle spasms, and paresthesias since early childhood. A diagnosis of hypoparathyroidism was not reached until 39 y of age. The three daughters, who were 10, 11, and 12 y of age at diagnosis, had a history of seizures, cramps, and paresthesias throughout childhood. Laboratory studies at the time of diagnosis showed hypocalcemia and hyperphosphatemia. PTH levels were inappropriately low for the calcium level. Serum creatinine levels were normal(Table 1). The father, who was clinically unaffected, had normal serum calcium and phosphorus levels. The affected family members were treated with vitamin D analogs and calcium supplementation for 16 years. They were then referred to the National Institutes of Health (NIH) Clinical Center for further evaluation. At that time, while receiving oral calcium and calcitriol, serum calcium levels were in the normal range, PTH levels were suppressed, and urine calcium excretion was elevated. All four women showed increased serum creatinine concentrations and decreased creatinine clearance rates (Table 1). Computed tomography scans showed nephrocalcinosis in all four patients.
Informed consent was obtained from all subjects included in the study. This study was approved by the NICHD institutional review board.
DNA amplification and sequence analysis. Genomic DNA was isolated from white blood cells, and portions of the CaR gene were PCR-amplified using primer pairs previously described(4). Screening for mutations was performed by heteroduplex analysis using MDE gels(AT Biochem)(13). The double-stranded PCR products were heated to 95 °C to produce single-stranded DNA and then cooled slowly to 37 °C to reanneal the DNA. The reannealed PCR products were then subjected to PAGE using 0.5 × MDE gels containing 0.6 × Tris-borate EDTA buffer and 15% urea. Gels were run at 15 V/cm for 14-18 h. When genomic DNA containing a heterozygous base pair substitution is PCR-amplified, it yields a mixture of two different homoduplexes. Melting and reannealing produces a mixture of two homoduplexes and two heteroduplexes visualized as two or more bands on the MDE gel. PCR products that showed heteroduplex bands were sequenced from both strands by the dideoxy method using an automated fluorescent sequencing system(14).
Site-directed mutagenesis. The mutated receptor sequence was created by site-directed mutagenesis using the Altered Sites II system(Promega). The human CaR cDNA, inserted into the mutagenesis vector pAlterI(Promega), was obtained from NPS Pharmaceuticals. Oligonucleotides were synthesized containing the single base pair mismatch corresponding to the mutated nucleotide. These nucleotides were annealed to the CaR cDNA constructs, extended with T4 DNA polymerase, and ligated. The resultant constructs were used to transform Escherichia coli strain XLMutS and were then transferred to strain JM109. Restriction enzymes XbaI and Hin dIII were used to isolate the mutated cDNA from the vector pAlterI. The cDNA was then inserted into the vector pcDNAI/Amp (Invitrogen, San Diego, CA). Automated DNA sequencing was used to confirm the presence of the mutation.
Cell culture and transfection. HEK-293 cells were cultured in DMEM (Biofluids Inc., Rockville, MD). Approximately 1 × 105 cells were transiently transfected with 0.5 μg of the mutant or WT CaR cDNA construct and 5 μL of Lipofectamine (Life Technologies Inc., Gaithersburg, MD) per dish.
Preparation of cell membranes. Partially purified plasma membranes were prepared by washing the transfected cells with PBS. After addition of extraction buffer (50 mM Tris-HCl, pH 6.8, 0.32 M sucrose, 1 mM EDTA, 1 mM phenylmethylsulfonyl fluoride, 10 μg/mL aprotinin, 5 μg/mL leupeptin, 0.7 μg/mL pepstatin) at 4 °C, the cells were lysed by passing through 22-gauge needles and sedimented at 16 000 × g for 30 min to remove nuclei and mitochondria. Plasma membranes were pelleted at 50 000 × g for 30 min and then solubilized with 1% Triton X-100.
Western analysis. Membrane proteins (25 μg/well, determined by Pierce BCA protein assay) were subjected to SDS-PAGE with a linear gradient of polyacrylamide (5-15%) and transferred to a nitrocellulose membrane. The blot was incubated with 2 μg/mL affinity-purified monoclonal anti-ADD antibody (made against residues 214-235 of human CaR, and kindly provided by Dr. Paul K. Goldsmith, Metabolic Diseases Branch, National Institute of Diabetes, Digestive and Kidney Diseases, National Institutes of Health), and then with a secondary, goat anti-mouse antibody conjugated to alkaline phosphatase (Kierkegaard & Perry Laboratories Inc., Gaithersburg, MD; diluted 1:1000). 4-Chloronaphthol was used to visualize the CaR protein bands.
Assessment of cell surface expression by ELISA. A monoclonal 7F8 antibody was made by immunization with the purified extracellular domain of the human CaR (P. K. Goldsmith, manuscript in preparation). Transfected cells were suspended in 1% BSA-DMEM and blocked for 30 min at 4 °C. Cells were then incubated with 7F8 MAb (20 μg/mL) for 1 h at 4 °C. After washing, cells were further incubated with a 1:1000 dilution of peroxidase-conjugated goat anti-mouse secondary antibody (Kierkegaard & Perry Laboratories; 1:1000 dilution). After washing, peroxidase substrate was added to cells, and absorbance was measured at 405 nm. The ELISA was performed on three independent transfections. The ELISA value thus reflects cell surface expression, but the two quantities may not be linearly related.
Measurement of phosphoinositides. Forty-eight hours after transfection, HEK-293 cells were labeled with myo-[3H]inositol (New England Biolab) at 3 μCi/mL in DMEM for 16-24 h. These cells were then incubated in PI buffer (99 mM NaCl, 5 mM KCl, 5.6 mM glucose, 0.4 mM MgCl2) containing 20 mM LiCl for 1 h. Cells were exposed to graded extracellular concentrations of Ca2+ for 30 min at 37 °C, and the reactions were terminated with the addition of acid methanol (167 μL of HCl in 120 mL of methanol). Dowex AG1-X8 columns were used to separate the total IPs as described previously(15). Labeled IPs were then counted by liquid scintillation. Nine separate transfections were performed at each Ca2+ concentration for IP measurement.
Statistical analysis. Results are expressed as mean ± SEM. Significance was assessed using a t test.
RESULTS
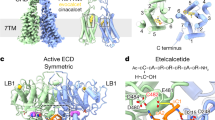
Sequence analysis. To screen for mutations in the CaR, we PCR-amplified individual exons from genomic DNA and used heteroduplex analysis. All affected members showed heteroduplex bands in exon 6(Fig. 1). Sequencing of the PCR-amplified genomic DNA showed a heterozygous T to C transition at position 1835 [numbered according to Garrett et al.(16)] in all four patients (Fig. 2). This mutation produces a phenylalanine to serine substitution at residue 612 in the extracellular region of the receptor, adjacent to the first transmembrane domain (Fig. 3). It was not present in any of 50 normal control subjects evaluated by heteroduplex analysis or sequencing (data not shown).
Heteroduplex analysis of CaR gene. Exon 6 of the CaR gene was PCR-amplified, denatured, slowly reannealed, and subjected to MDE-PAGE. Lane 1 represents a normal control showing a single band. Lanes 2, 3, 4, and 5 represent the affected mother and three daughters, respectively, showing double bands that correspond to the heteroduplexes and homoduplexes.
Base pair substitution in the CaR gene. PCR amplified genomic DNA was sequenced directly using fluorescent dideoxynucleotides in an automated DNA sequencing system. The DNA sequence for the third daughter, shown below that for a normal control subject, revealed a heterozygous T to C transition at position 1835. The numbers indicate position based on the human sequence. The arrow indicates the site of the mutation.
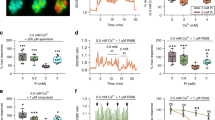
Functional analysis. HEK-293 cells transiently transfected with WT and mutant receptors were exposed to Ca2+ at concentrations of 0.5 to 16 mM, and IP accumulation was measured. Although mean IP accumulation was slightly higher for the mutant receptor than for the WT receptor at low Ca2+ concentration, this difference did not reach statistical significance (p = 0.18, Table 2). IP accumulation increased for the WT and mutant receptor in response to an increasing Ca2+ concentration and came to a plateau at high Ca2+ concentrations (Fig. 4). The concentration-response curve for the mutated receptor was left-shifted with a decreased EC50 compared with the WT receptor (p < 0.001 Table 2). The mutant receptor also produced a greater maximal response at high Ca2+ concentration than did the WT receptor (p < 0.02Table 2, Fig. 4).
IP response to extracellular Ca2+ in transfected HEK-293 cells. Cells were transfected with WT or mutant (F612S) CaR cDNA expression plasmids. After 48 h, cells were labeled with myo-[3H]inositol for 16-24 h and then exposed to graded extracellular concentrations of Ca2+ for 30 min. IPs were isolated and counted by liquid scintillation. Nine separate transfections were performed at each Ca2+ concentration.
Western analysis. Western analysis of plasma membrane preparations from cells transfected with the WT and mutant receptors produced the same pattern of two bands between 100 and 200 kD and a third band at about 250 kD (Fig. 5). Western analysis was performed twice, producing consistent results.
Western analysis of WT and mutant (F612S) CaR. Twenty-five micrograms of purified membrane protein from transfected HEK-293 cells were subjected to SDS-PAGE on a linear gradient running gel(5-15%). An affinity-purified MAb (against residues 214-235 of the human CaR) was used to identify the CaR bands. 293 represents protein from the untransfected HEK-293 cells.
Cell surface protein expression. Expression of mutant and WT receptors in plasma membranes of HEK-293 cells was assessed by ELISA. The mean cell surface expression was lower for the mutant than for the WT receptor(Table 2). However, this difference did not reach statistical significance (p = 0.06). To confirm assay specificity, ELISA was also performed on cells transfected with vector alone (0.34 ± 0.002, mean ± SEM, OD units).
DISCUSSION
We identified a CaR mutation in a family with autosomal dominant hypoparathyroidism. On treatment, affected family members developed hypercalciuria and nephrocalcinosis. This phenotype is characteristic of autosomal dominant hypoparathyroidism due to CaR mutations. The mutation identified in this family produced an amino acid substitution in the aminoterminal extracellular domain of the receptor near the first transmembrane domain. This same missense mutation was recently reported in another family with a similar phenotype, but the functional effects of the sequence alteration were not studied(10). It is difficult to predict the conformational change induced by this mutation because the three-dimensional structure of the protein is not known.
To determine whether the mutation activates the receptor and to study the mechanism of activation, we expressed mutant and WT receptors in HEK-293 cells. For both the WT and mutant CaR, increasing extracellular Ca2+ concentrations elicited an increase in IP production. For both receptors the IP response reached a plateau at high Ca2+ concentrations. This shape of the concentration-response curve is typical of ligand-receptor interactions. However, it differs from the IP response of three activating mutations recently reported(10). All three of these mutations produced a biphasic concentration-response curve with maximal activity at 1-2 mM Ca2+ and decreased response at higher Ca2+ concentrations. This difference in observed responses could reflect differences either in methodology or in the functional effects of the specific mutations.
The EC50 of the mutant receptor was significantly less than that of the WT receptor. This left-shift in the concentration-response curve indicates that the mutant receptor is more sensitive to extracellular Ca2+ than is the WT receptor. This increased sensitivity may result from an increase in receptor affinity for Ca2+. However, methods for directly assessing the affinity of the receptor for Ca2+ have not been reported.
The mutant receptor also showed greater signal transduction at high Ca2+ concentrations. Because the expression of the mutant receptor on the surface of HEK-293 cells was actually less than that of the WT receptor, the observed difference in total activity could not be explained by differences in receptor expression. Thus, the data suggest that the activity per receptor was increased. Previous expression studies have not quantitated cell surface expression and thus could not distinguish these variables.
The F612S amino acid substitution could increase receptor activity indirectly by altering posttranslational modification. However, there was no evidence of altered glycosylation or protein size of the mutant receptor by Western analysis, suggesting that the amino acid substitution directly alters receptor activity. Western analysis does not exclude more subtle alterations in posttranslational modification.
A dual increase in receptor sensitivity and maximal signal transduction, similar to that of F612S, has been observed for mutations in other G protein-coupled receptors. Mutations in the β2-adrenergic receptor, the α1B-adrenergic receptor, and the platelet-activating factor receptor have produced similar effects(17, 18). Conversely, inactivating mutations of the CaR in familial hypocalciuric hypercalcemia, the mirror image of autosomal dominant hypoparathyroidism, have been observed to cause a dual decrease in sensitivity and maximal activity(11, 12).
In summary, we identified a mutation in the CaR in a family with autosomal dominant hypoparathyroidism. This mutation activates the receptor by increasing both sensitivity to extracellular Ca2+ and maximal activity. The observed activation explains the clinical phenotype of hypoparathyroidism with disproportionate hypercalciuria.
Abbreviations
- CaR:
-
Ca2+-sensing receptor
- DMEM:
-
Dulbecco's minimal essential medium
- WT:
-
wild-type
- HEK:
-
human embryonic kidney cell line
- IP:
-
inositol phosphate
- MDE:
-
mutation detection enhancement
References
Chattopadhyay N, Mithal A, Brown EM 1996 The calcium-sensing receptor: a window into the physiology and pathophysiology of mineral ion metabolism. Endocr Rev 17: 289–307.
Brown EM, Gamba G, Riccardi D, Lombardi M, Butters R, Kifor O, Sun A, Hedlger MA, Lytton J, Hebert SC 1993 Cloning and characterization of an extracellular Ca2+-sensing receptor from bovine parathyroid. Nature 366: 575–580.
Aida K, Koishi S, Tawata M, Onaya T 1995 Molecular cloning of a putative Ca2+-sensing receptor cDNA from human kidney. Biochem Biophys Res Commun 214: 524–529.
Pollack MR, Brown EM, Yan-Huei WC, Hebert SC, Marx SJ, Steinmann B, Levi T, Seidman CE, Seidman JG 1993 Mutations in the human Ca2+-sensing receptor gene cause familial hypocalciuric hypercalcemia and neonatal severe hyperparathyroidism. Cell 75: 1297–1303.
Bai M, Pearce SHS, Kifor O, Trivedi S, Stauffer UG, Thakker RV, Brown EM, Steinmann B 1997 In vivo and in vitro characterization of neonatal hyperparathyroidism resulting from a de novo heterozygous mutation in the Ca2+ -sensing receptor gene: normal maternal homeostasis as a cause of secondary hyperparathyroidism in familial benign hypocalciuric hypercalcemia. J Clin Invest 99: 88–96.
Baron J, Winer KK, Yanovski JA, Cunningham AW, Laue L, Zimmerman D, Cutler GB Jr 1996 Mutations in the Ca2+-sensing receptor gene cause autosomal dominant and sporadic hypoparathyroidism. Hum Mol Gen 5: 601–606.
Pollack MR, Brown EM, Estep HL, McLaine PN, Kifor O, Park J, Hebert SC, Seidman CE, Seidman JG 1994 Autosomal dominant hypocalcaemia caused by a Ca2+-sensing receptor gene mutation. Nat Genet 8: 303–307.
Lovlie R, Eiken HG, Sorheim JI, Boman H 1996 The Ca2+-sensing receptor gene (PCAR1) mutation T151M in isolated autosomal dominant hypoparathyroidism. Hum Genet 98: 129–133.
Perry YM, Finegold DN, Armiteage MM, Ferrell RE 1994 A missense mutation in the Ca-sensing receptor gene causes familial autosomal dominant hypoparathyroidism. Am J Hum Genet(suppl) 55: 3( abstr 1700).
Pearce SHS, Williamson C, Kifor O, Bai M, Coulthard MG, Davies M, Lewis-Barned N, Mc Credie D, Powell H, Kendall-Taylor P, Brown EM, Thakker RV 1996 A familial syndrome of hypocalcemia with hypercalciuria due to mutations in the calcium-sensing receptor. N Engl J Med 335: 1115–1125.
Pearce SHS, Bai M, Quinn SJ, Kifor O, Broen EM, Thakker RV 1996 Functional characterization of calcium-sensing receptor mutations expressed in human embryonic kidney cells. J Clin Invest 98: 1860–1866.
Bai M, Quinn S, Trivedi S, Kifor O, Pearce SHS, Pollack MR, Krapcho K, Hebert SC, Brown EM 1996 Expression and characterization of inactivating and activating mutations in the human Ca2+-sensing receptor. J Biol Chem 271: 19537–19545.
White MB, Carvalho M, Derse D, O'Brien SJ, Dean M 1992 Detecting single base substitutions as heteroduplex polymorphisms. Genomics 12: 301–306.
Smith LM, Sanders JZ, Kaiser RJ, Hughes P, Dodd C, Connell CR, Heiner C, Kent SBH, Hood LE 1986 Fluorescence detection in automated DNA sequence analysis. Nature 321: 674–679.
Berridge MJ, Dawson RM, Downes CP, Heslop JP, Irvine RF 1983 Changes in levels of inositol phosphates after agonist dependent hydrolysis of membrane phosphoinositides. Biochem J 212: 473–482.
Garrett JE, Capuano IV, Hammerland LG, Hung BCP, Brown EM, Hebert SC et al 1995 Molecular cloning and functional expression of human parathyroid calcium receptor cDNAs. J Biol Chem 270: 12919–12925.
Lefkowitz RJ, Cotecchia S, Samama P, Costa T 1993 Constitutive activity of receptors coupled to guanine nucleotide regulatory proteins. Trends Pharmacol Sci 14: 303–307.
Parent J, Le Gouill C, de Brum-Fernandes AJ, Rola-Pleszczynski M, Stankova J 1996 Mutations of two adjacent amino acids generate inactive and constitutively active forms of the human platelet-activating factor receptor. J Biol Chem 271: 7949–7955.
Acknowledgements
The authors thank Dr. Paul K. Goldsmith for providing the MAb, and Dr. Regina Collins for tissue culture assistance. We also thank NPS pharmaceutical for providing the WT CaR cDNA construct.
Author information
Authors and Affiliations
Additional information
Presented in part at the 10th International Congress of Endocrinology, San Francisco, 1996.
Rights and permissions
About this article
Cite this article
Mancilla, E., De Luca, F., Ray, K. et al. A Ca2+-Sensing Receptor Mutation Causes Hypoparathyroidism by Increasing Receptor Sensitivity to Ca2+ and Maximal Signal Transduction. Pediatr Res 42, 443–447 (1997). https://doi.org/10.1203/00006450-199710000-00004
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-199710000-00004