Abstract
It has been shown that glucocorticoids accelerate lung development by limiting alveolar formation resulting from a premature maturation of the alveolar septa. Based on these data, the aim of the present work was to analyze the influence of dexamethasone on cell cycle control mechanisms during postnatal lung development. Cell proliferation is regulated by a network of signaling pathways that converge to the key regulator of cell cycle machinery: the cyclin-dependent kinase (CDK) system. The activity of the various cyclin/CDK complexes can be modulated by the levels of the cyclins and their CDKs, and by expression of specific CDK inhibitors (CKIs). In the present study, newborn rats were given a 4-d treatment with dexamethasone (0.1–0.01 μg/g body weight dexamethasone sodium phosphate daily on d 1–4), or saline. Morphologically, the treatment caused a significant thinning of the septa and an acceleration of lung maturation on d 4. Study of cyclin/CDK system at d 1–36 documented a transient down-regulation of cyclin/CDK complex activities at d 4 in the dexamethasone-treated animals. Analysis of the mechanisms involved suggested a role for the CKIs p21CIP1 and p27KIP1. Indeed, we observed an increase in p21CIP1 and p27KIP1 protein levels on d 4 in the dexamethasone-treated animals. By contrast, no variations in either cyclin and CDK expression, or cyclin/CDK complex formation could be documented. We conclude that glucocorticoids may accelerate lung maturation by influencing cell cycle control mechanisms, mainly through impairment of G1 cyclin/CDK complex activation.
Similar content being viewed by others
Main
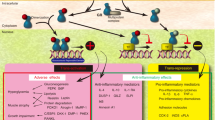
Glucocorticoids are essential anti-inflammatory molecules widely used in the treatment of a large variety of lung diseases. The early postnatal use of glucocorticoids is often motivated by a positive effect on lung maturation in preterm born babies, who otherwise stand a high risk of developing chronic lung disease also called bronchopulmonary dysplasia. However, as a side effect, it has been demonstrated in a number of animal models that glucocorticoids may impair postnatal lung maturation and growth (1–5).
The morphologic descriptions of the effects of glucocorticoids on postnatal lung development have established that the acceleration of alveolar wall thinning and microvascular maturation is associated with a reduction in the outgrowth of new interalveolar septa and, therefore, with an inhibition of alveolar formation (4). These data are consistent with the involvement of glucocorticoids in the processes of cellular differentiation and proliferation (6). In normal situations, the balanced action of endogenous glucocorticoids on both processes results in adequate lung maturation. In situations with increased levels of glucocorticoids, it is likely that this balance is no longer maintained resulting in an impairment in lung development.
The observations that glucocorticoid treatment was associated with decreased formation of new alveoli strongly suggests an inhibitory effect of these hormones on cell growth, and, therefore, on cell cycle progression. This finding points to the key regulators of the cell cycle machinery, the CDK system (7, 8). CDKs consist of a regulatory subunit, termed a cyclin, and a catalytic subunit. The G1 cyclins include D cyclins (D1, D2, and D3) and cyclin E (9–11). The D-type cyclins form complexes primarily with CDK4 and CDK6, and cyclin E with CDK2. The G1 CDKs phosphorylate substrates such as the product of the Rb tumor suppressor gene, which in turn regulates the initiation of DNA replication (12–14). Once cells have completed the G1 phase, progression toward mitosis involves the formation of other cyclin/CDK complexes, with the major CDK partner being CDC2. Activity of cyclin/CDK complexes can be modulated by several mechanisms, including changes in cyclin or CDK levels, residue phosphorylation, and association with CKI (13, 15, 16). Two families of CKIs have been characterized. The first one to be identified was the INK4 family, which acts principally on complexes formed with the D-type cyclins. This family includes p15INK4B, p16INK4A, p18INK4C, and p19INK4D. The second family, which includes p21CIP1 (also known WAF1), p27KIP1, and p57KIP2, has been reported to act on a wide range of cyclin/CDKs (13, 16).
To gain some insights into the mechanisms involved in the inhibition of lung growth in response to glucocorticoids, in the present study we focused on the effects of these hormones on the activity of the cyclin/CDK complexes and on the expression of the cyclins and their CDKs in the lungs of newborn rats that were given a 4-d treatment with dexamethasone. The lung tissues were analyzed on d 1, 4, 10, 16, 19, 21, and 36. The most dramatic modification observed after glucocorticoid administration was a profound decrease in the activity of the CDK complexes, associated with an increase in the levels of the CKIs, p21CIP1, and p27KIP1. These data suggest that glucocorticoids may alter postnatal lung growth by acting on specific targets of the cell cycle machinery, which results in an impairment in the activation of cyclin/CDK complexes.
MATERIALS AND METHODS
Animals and tissues.
On the first day after birth (postnatal d 1) female Zur:SD rat litters were reduced to eight pups per mother and the male pups were assigned to experimental and control groups. Glucocorticoid-treated animals received on postnatal d 1 0.1 μg/g body weight dexamethasone (Decadron phosphate, Merck Sharp Dohme AG, Glattbrugg, Switzerland, diluted in saline 1:200–1:400) by s.c. injection between 0900 and 1000 h, followed by 0.05 μg/g on d 2, 0.025 μg/g on d 3, and 0.01 μg/g on d 4. Control animals were injected with similar volumes of saline (4). The animals obtained at d 1 were not treated at all. Handling of the animals before and during the experiments, as well as the experiments themselves, were approved and supervised by the Swiss Agency for the Environment, Forests and Landscape and the Veterinary Service of the Canton of Bern. For each experimental condition, lung tissues from four to six animals were used.
Lungs were obtained on postnatal d 1, 4, 10, 16, 19, 21, and 36. For Western blot studies, the lung tissues were immediately frozen in liquid nitrogen and kept there until further processing. For morphologic and immunohistochemical studies, the lungs were prepared according to Schittny et al. (17). Briefly, the blood vessels were perfused with PBS (10 mM sodium phosphate, containing 127 mM sodium chloride, pH 7.4) containing 5 units/mL heparin, 10 mg/mL procaine, and 10 mM EDTA (Fluka Chemie AG, Buchs, Switzerland). The airspace was filled at a constant pressure of 20 cm water column by instillation via tracheotomy with PBS, containing 4% freshly prepared paraformaldehyde (Merck, Darmstadt, Germany). At the applied pressure, the lung reaches roughly its mid-respiratory volume. To prevent a recoiling of the lung, the pressure was maintained during removal of the lung from the still intact thoracic cage and during the 30-min fixation.
Morphologic and immunohistochemical studies.
After fixation, the lungs were washed three times in PBS and embedded in paraffin (Histosec, Merck) at 60°C after dehydration in a graded series of ethanol and using Histoclear (Life Science International, Frankfurt, Germany) as intermedium. Then, 3.5–5-μm-thick sections were cut, transferred onto silanized (aminopropyl-trimethoxy-silane) slides, and air dried over night at 37°C. All sections were dewaxed in three changes of Histoclear and a graded series of ethanol, followed by two changes of distilled water, or tris buffered saline (TBS), (50 mM Tris/HCl, pH 7.4, containing 100 mM sodium chloride), respectively.
For morphologic studies, sections were stained with hematoxylin-eosin. For immunoperoxidase staining, the sections were fixed for 20 min with 4% paraformaldehyde, freshly dissolved in TBS, washed three times with TBS, and cooked for 15–20 min in 0.01 M Sodium citrate (pH 6.0) in a microwave oven. After blocking for 30 min, using blocking buffer (TBS, containing 5 mg/mL BSA and 1% nonspecific rabbit IgG), the sections were incubated with the first antibody (goat anti-p21CIP1 or goat anti-p27KIP1 (Santa Cruz Biotechnology, Santa Cruz, CA, U.S.A.) diluted 1:20 in blocking buffer) for 15 h at 4°C, followed by an affinity purified biotinylated anti-goat IgG (Vector Laboratories, Burlingame, CA, U.S.A.; diluted 1:100 in blocking buffer), and by avidin-biotin-complex/horseradish peroxidase (Dakopatts, Glostrup, Denmark). The latter two incubations were done for 45 min at room temperature. After each incubation step, sections were washed three times with TBS. The slides were developed with 3-amino-9-ethylcarbazole (Sigma Chemical, St. Louis, MO, U.S.A.)/H2O2 and mounted in Aquatex (Merck). Negative controls were performed with nonspecific goat IgG and only very low levels nonspecific background were observed. The shown samples were taken from central parts of the lung.
Immunoblotting studies.
Total cellular lung proteins (150 μg) were lysed by addition of 40 μL lysis buffer (250 mM NaCl, 50 mM HEPES pH 7.0, 5 mM EDTA, 1 mM DTT, 0.1% Nonidet NP40, 10 μg/mL leupeptin, 10 μg/mL apoprotinin, 50 μg/mL phenylmethylsulfonyl fluoride, 2 mM sodium pyrophosphate, 1 mM sodium orthovanadate), as previously described (17–19). The lysates were clarified by centrifugation at 10,000 ×g for 10 min at 4°C. Equal quantities of samples were loaded for each experimental condition, and proteins were separated by SDS-PAGE (10% acrylamide). Western blots were prepared by transferring the proteins onto 0.45-μm nitro-cellulose membranes (NC), (Bio-Rad, Richmond, CA, U.S.A.) for 1 h 30 min at 130 V. Immunoblotting was performed by first saturating the NC sheet for 2 h at room temperature in TBS (20 mM Tris-HCL, pH 7.6, 137 mM NaCl) containing 0.2% Tween (TBS-T) and 10% powdered milk. This was followed by incubation with diluted antiserum in 5% milk-TBS for 20 h at 4°C. The antisera used were the following: rabbit anti-mouse cyclin D1, cyclin D2, and cyclin D3 antibodies and anti-rabbit CDK4 antibody from Dr. Sherr (Howard Hughes Medical Institute, Memphis, TN, U.S.A.); rabbit anti-CDK2 and rabbit anti-CDC2 antibodies from Dr. Guguen-Guillouzo; rabbit anti-cyclin E, anti-p21CIP1 and anti-p27KIP1 antibodies (Santa Cruz Biotechnology). The membranes were then washed three times in TBS-T buffer and incubated for 1 h at 37°C with horseradish peroxidase–conjugated goat anti-rabbit IgG (Amersham, England), diluted 1:1000 in milk-TBS. The membranes were then washed three times in TBS-T, after which they were incubated for 1 min at room temperature in chemiluminescence reaction detection reagents (ECL Western blotting, Amersham) and exposed to autoradiography film (Hyperfilm-ECL, Amersham).
Immunoprecipitation and kinase assays.
Total cellular lung proteins (100 μg) were lysed by addition of 40 μL lysis buffer (250 mM NaCl, 50 mM HEPES pH 7.0, 5 mM EDTA, 1 mM DTT, 0.1% Nonidet NP40, 10 μg/mL leupeptin, 10 μg/mL apoprotinin, 50 μg/mL phenylmethylsulfonyl fluoride, 2 mM sodium pyrophosphate, 1 mM sodium orthovanadate). The lysates were clarified by centrifugation at 10,000 ×g for 10 min at 4°C, and incubated at 4°C overnight with either anti-cyclin E antibody, anti-CDK2 antibody, anti-CDK4 antibody, or anti-CDC2 antibody, as previously described (17–19). Cyclin/CDK complexes were then isolated by incubation at 4°C for 2 h with 50 μL of either protein A-Sepharose beads 6MB (Pharmacia, Piscataway, NJ, U.S.A.) or glutathione S-transferase (GST)-agarose beads (Pharmacia). The beads were then washed with PBS and incubated for 30 min at 30°C in 25 μL reaction buffer (50 mM Tris-HCL pH 7.4, 10 mM MgCl2, 1 mM DTT, 1μM ATP) in the presence of either 5 μg histone H1 (Roche Molecular Biochemicals, Mannheim, Germany) or 1 μg of GST-retinoblastoma protein (pRb) substrate (a gift from Dr. Ewen, Dana Farber Institute, Boston, MA, U.S.A.), 1 μL (−32P) ATP (4500 mCi/mmol). Reactions were stopped by adding 40 μL 2× SDS sample buffer (62.5 mM Tris-HCL pH 6.8, 2% SDS, 10% glycerol, 0.025% bromophenol blue, 5% β-mercaptoethanol). The samples were then boiled for 5 min and analyzed by 10% SDS-PAGE. 32P-labeled proteins were detected by autoradiography and quantified with densitometry scanner.
Statistical analysis.
Results were reported as mean ± SE. Data were analyzed with standard tests of statistical significance including Mann-Whitney U test or Bonferroni t test. Significance was assigned for p < 0.05.
RESULTS
Morphologic observations.
The very short glucocorticoid treatment already induced structural alterations in the lungs detectable at light microscopical level. On postnatal d 4, the last day of treatment, the glucocorticoid treated animals showed a significant acceleration of lung maturation (Fig. 1, a and b ). Thinning of the inter-airspace septa, a process normally detected during the third postnatal week, could be observed. Furthermore, the cross-sectional areas of the respiratory airspaces appeared wider in the glucocorticoid group than in the controls, but it remains open how much of it is caused by the premature thinning of the septa and how much reflects a real widening of the airspaces. On postnatal d 10, the untreated animals exhibited a higher complexity of the lung parenchyma (Fig. 1, c and d ), which may be explained by a reduced formation of secondary septa in the dexamethasone-treated animals. These prominent differences disappeared, however, gradually with age. At the beginning of the third postnatal week, no significant differences were detectable anymore (Fig. 1, e and f ).
Morphologic observations. On postnatal d 4 (a and b), 10 (c and d), and 16 (e and f), lung sections of the control (a, c, and e) and dexamethasone groups (b, d, and f) were stained with hematoxylin-eosin. Especially on d 4, a significant acceleration of the lung maturation is visible in the dexamethasone group. Bar: 100 μm.
Cyclin/CDK activities.
To characterize the mechanisms involved in the impairment of lung growth in glucocorticoid-treated animals, we focused on the study of the cyclin and CDK system. Based on the results of previous experiments on lung epithelial cells demonstrating a down-regulation of G1 cyclin/CDK complex activities after dexamethasone treatment, we first performed in vitro kinase assays to assess the activity of several cyclin/CDK complexes. The cyclin D/CDK4 complexes were assayed for their kinase activity toward pRb. The complexes formed with either cyclin E, or CDC2 were evaluated using phosphorylation of histone H1. The patterns of cyclin/CDK complex activities in the control group are shown in Figures 2 and 3. Activities of the complexes formed with CDK4 displayed some variations during the study period. The activities of the complexes formed with either cyclin E, CDK2, or CDC2 were higher during the first postnatal days compared with d 36. For CDK2 complexes a prominent peak of activity was observed on d 4. When the patterns of the various cyclin/CDK complex activities in the dexamethasone group were compared with the control group, the most striking difference was a dramatic decrease in CDK activity for all the complexes studied on d 4. However, this reduction was transient. The activities of CDK4, CDK2, and cyclin E-associated complexes were found to be increased at d 10. For CDC2 complex activities, the increase was observed later, on d 16.
Analysis of CDK4 (A) and cyclin E-associated (B) kinase complex activities. Cell lysates were prepared from lung tissues of rats treated with saline (Control) or with dexamethasone (Dex) on postnatal d 1, 4, 10, 16, 19, 21, and 36. CDK4 complex activities were determined using purified bacterial GST-pRb fusion protein as a substrate, and cyclin E-associated kinase complex activities were evaluated using histone H1 as a substrate. Representative autoradiograms of signals are shown on the left. On the right, the histograms show a quantitative representation of CDK4 and cyclin E-associated kinase complex activities obtained from laser densitometric analysis of three independent experiments. Densitometry results were expressed in arbitrary units. *p < 0.05 vs control condition on the same day.
Analysis of CDK2 and CDC2 complex activities. Cell lysates were prepared from lung tissues of rats treated with saline (Control) or with dexamethasone (Dex) on postnatal d 4, 10, 16, 19, 21, and 36. Tissues from d 1 were obtained from untreated animals. CDK2 complex or CDC2 complex activities were evaluated using histone H1 as a substrate. The reaction products were electrophoretically separated on denaturing gels, and phosphorylated proteins were detected by autoradiography as described in “Materials and Methods.” Representative autoradiograms of signals are shown on the left. On the right, the histograms show a quantitative representation of CDK2 and CDC2 kinase complex activities obtained from laser densitometric analysis of three independent experiments. Densitometry results were expressed in arbitrary units. *p < 0.05 vs control condition on the same day.
Expression of CDK4, CDK2, and CDC2.
It is well established that the activity of cyclin/CDK complexes can be modulated either by changes in CDK or cyclin levels, changes in complex formation, or association with a CKI. To determine the mechanisms involved in the decrease in cyclin/CDK complex activity observed on d 4 in the dexamethasone group we first asked whether dexamethasone could induce changes in G1 CDK or cyclin protein levels. From the results obtained in the CDK complex activity experiments, we focused the study on d 1, 4, and 10. Lung proteins from the control group and from dexamethasone-treated rats were extracted and studied by Western blotting. The patterns of expression of CDK4, CDK2, and CDC2 are shown in Figure 4. Some variations in the levels of expression were observed in the various experimental conditions. In the control animals, the expression of CDK4 and CDK2 appeared higher on d 4 than on d 1 and remained higher on d 10. When the pattern of expression in the dexamethasone group was compared with the control group, the only difference observed was the peak of CDC2 that was documented on d 10 instead of on d 4. However, these variations did not reach statistical significance.
Study of CDK4, CDK2, and CDC2 expression. Total proteins were extracted from lung tissues on postnatal d 1, 4, and 10. On d 4 and 10, the rats were treated with saline (Control) or with dexamethasone (Dex). Proteins were then analyzed by immunoblotting: the materials were fractionated on SDS-PAGE, transferred to nitrocellulose, and probed with the corresponding antibody, as described in “Materials and Methods.” Autoradiograms of signals for CDK4 (33 kD), CDK2 (33 kD), and CDC2 (34 kD) proteins from a representative experiment are shown.
Expression of G1 cyclins.
The patterns of expression of cyclin D1, D3, and E are shown in Figure 5. In the control group, no major changes in the levels of cyclin D1 and D3 were observed from d 1 to d 10. As described, cyclin E migrated as a series of bands consistent with its normal processing. The expression of all cyclin E isoforms appeared higher on d 4 and 10. When the expression patterns in the dexamethasone group were compared with the control group, the major (only statistical) difference was the transient reduction in cyclin E isoform levels on d 4 compared with d 1. Cyclin D2 expression was barely detectable in all of the experimental conditions. These results were consistent with our previous data obtained from lung alveolar epithelial cells.
Study of cyclin D1, cyclin D3, and cyclin E expression. Total proteins were extracted from lung tissues on postnatal d 1, 4, and 10. On d 4 and 10, the rats were treated with saline (Control) or with dexamethasone (Dex). Proteins were then analyzed by immunoblotting: the materials were fractionated on SDS-PAGE, transferred to nitrocellulose, and probed with the corresponding antibody, as described in “Materials and Methods.” Autoradiograms of signals for cyclins D1 (36 kD), D3 (30 kD), and cyclin E (between 50kD and 60 kD) proteins from a representative experiment are shown.
Formation of cyclin E/CDK2 complexes.
Our observation of a decrease in cyclin/CDK complex activity on d 4 in association with a decrease in cyclin E isoforms levels led us to investigate the formation of cyclin E/CDK2 complexes. For these experiments, proteins were first immunoprecipitated with either anti-CDK2 antibody or anti-cyclin E antibody, and the levels of either cyclin E or CDK2 in the precipitates were analyzed by immunoblotting. This study was performed on d 1 and d 4. The results are shown in Figure 6. Despite the reduction of the cyclin/CDK complex activity on d 4 in dexamethasone-treated group, no changes in complex formation could be found. Similar results were obtained for complexes formed with CDK4 and CDC2 (data not shown).
Study of cyclin E/CDK2 complex formation. Cell lysates were prepared from lung tissues of rats on d 1 and of rats treated with dexamethasone on postnatal d 4. (A) Proteins were first immunoprecipitated with anti-CDK2 antibody, and cyclin E level in the precipitates was then analyzed by immunoblotting, as described in “Materials and Methods.” (B) Proteins were first immunoprecipitated with anti-cyclin E antibody, and CDK2 level in the precipitates was then analyzed by immunoblotting.
Expression of CKIs.
As shown above, the activity of cyclin/CDK complexes was significantly reduced on postnatal d 4 in the dexamethasone-treated animals despite a constant amount of cyclin/CDK complex formation. These results led us to focus on the possible involvement of CKIs. To determine whether the dexamethasone treatment could cause alterations in the expression of the two major inhibitors, p21CIP1 and p27KIP1, Western blotting and immunohistochemical studies were performed. Our interest in p21CIP1 and p27KIP1 was the result of the fact that only the CIP/KIP inhibitor family can act on the cyclin/CDK complexes that are already formed. As shown in Figure 7, a modest increase in p21CIP1 protein was observed on d 4 in the lungs of the control animals and a significant increase in the level of p27KIP1 on d 10 could be documented in comparison with d 1. In dexamethasone group, a progressive and significant increase in the levels of p21CIP1 was found from d 1 to d 10, whereas significant induction of p27KIP1 was only observed on d 4. Similar results were obtained by immunolocalization of p21CIP1 and p27KIP1 (Fig. 8). In lung tissues from dexamethasone-treated animals, an increase in the number of p21CIP1 and p27KIP1 positive cells and in the overall staining intensity was observed when compared with the control group. The increase was predominant at postnatal d 10 for p21CIP1 and at d 4 for p27KIP1. The dexamethasone-induced expression of p21CIP1 and p27KIP1 occurred in cells in the alveolar septa as well as in epithelial cells of the bronchioli.
Study of CKIs expression. Total proteins were extracted from lung tissues on postnatal d 1, 4, and 10. On d 4 and 10, the rats were treated with saline (Control) or with dexamethasone (Dex). Proteins were then analyzed by immunoblotting: the materials were fractionated on SDS-PAGE, transferred to nitrocellulose, and probed with the corresponding antibody, as described in “Materials and Methods.” Representative autoradiograms of signals for p21CIP1 and p27KIP1 proteins are shown on the left. On the right, the histograms show a quantitative representation of p21CIP1 and p27KIP1 obtained from laser densitometric analysis of three independent experiments. Densitometry results were expressed in arbitrary units. *p < 0.05 vs control condition on the same day; #p < 0.05 vs d 4 vs d 1 condition.
Immunolocalization of p21CIP1 and p27KIP1. Immunolocalization of p27KIP1 and p21CIP1 was done on postnatal d 4–36 in the control and glucocorticoid groups using the immunoperoxidase technique. Only the days with the most prominent differences between the two groups are shown. In the control group p27KIP1 (A) and p21CIP1 (C) were expressed at low levels. In the treated group, the expression of p27KIP1 was highest on postnatal d 4 (B) and the one of p21CIP1 on postnatal d 10 (D). Bar: 100 μm.
Association of p21CIP1 with cyclin E/CDK complexes.
Our observation of a decrease in cyclin/CDK complex activity on d 4 in the dexamethasone group in association with an elevated level of p21CIP1 led us to investigate the interaction between p21CIP1 and cyclin E/CDK complexes. For these experiments, proteins were first immunoprecipitated with anti-cyclin E antibody, and the level of p21CIP1 in the precipitates was analyzed by immunoblotting. This study was performed on d 1 and d 4. The results are shown in Figure 9. An increased association of p21CIP1 with cyclin E/CDK complexes was found on d 4 in the dexamethasone-treated group compared with d 1. For p27KIP1, the signals obtained under our experimental conditions were too weak to document a difference between control and dexamethasone groups.
Association of p21CIP1 with cyclin E/CDK complex. Cell lysates were prepared from lung tissues on postnatal d 1, and on postnatal d 4 in the dexamethasone-treated group. Proteins were first immunoprecipitated with anti-cyclin E antibody, and p21CIP1 level in the precipitates was then analyzed by immunoblotting, as described in “Materials and Methods.”
DISCUSSION
The present study provides information on the expression of the cyclin/CDK system during postnatal development of the lung, and on the changes in both activity and expression induced by glucocorticoid treatment. From the data reported herein, it appears that dexamethasone administration induced a decrease in several cyclin/CDK complex activities, which was associated with an increase in the levels of the CKIs, p21CIP1, and p27KIP1. Experiments reported herein addressed the question of the mechanisms used by glucocorticoids to alter postnatal lung development. Although some variations in the levels of expression of the various cyclins and CDKs were documented in the group of animals treated with dexamethasone, they did not appear to interfere with cyclin/CDK complex formation. These results are in agreement with previous data obtained in lung alveolar epithelial cells indicating that block of proliferation induced by dexamethasone did not affect the levels of the various G1 cyclins and their CDKs (19). In the present work, analysis of cyclin E/CDK2 complex formation indicated that the levels of the complexes remained unchanged upon dexamethasone treatment. These data clearly demonstrated that the decreased activity of the various complexes was not caused by an impairment in the association of the partners of the cyclin/CDK complexes. In the past few years, much has been learned of the mechanisms that can regulate the activity of cyclin/CDK complexes (20). Among the various regulation mechanisms are the associations of the complexes with the CKIs. The CKIs that have been reported to be involved in the actions of glucocorticoids are the proteins of the p21 family, which includes p21CIP1 and p27KIP1(20–22). Data reported herein support a role of these CKIs in the decreased activity of the various cyclin/CDK complexes, as an increase in p21CIP1 and p27KIP1 was found. In addition, we were able to document an increased association of p21CIP1 with cyclin E complexes.
The current understanding of the role of p21CIP1 and p27KIP1 in cell cycle progression emphasizes the importance of the relative abundance of these inhibitors (23). Indeed, Zhang et al. (24) demonstrated that active cyclin/CDK complexes contained a single p21CIP1 molecule whereas inactive complexes possessed multiple p21CIP1 subunits. It can be proposed, based on this model, that intermediate levels of p21CIP1 may favor proliferation. In contrast, the high levels of both p21CIP1 and p27KIP1 found in the dexamethasone group at d 4 could block the activity of most of the G1 cyclin/CDK complexes. Finally, the dramatic decrease in p27KIP1 documented at d 10 may participate in the transformation into active complexes. Several studies have provided data suggesting a role for p27KIP1 in the control of cell cycle exit. Durand et al. (25, 26) observed a progressive accumulation of p27KIP1 in proliferating oligodendrocytes precursor cells from rats, and showed that the highest p27KIP1 levels were found in the differentiated cells. In the present study, we found an accelerated maturation at postnatal day 4 in the group of animals treated with dexamethasone associated with high levels of p27KIP1 and decreased cyclin/CDK activities. These data suggest that p27KIP1 may play a role in the premature lung maturation induced by glucocorticoids.
During the early postnatal period, important modifications in rat lung structure are observed. They are the consequence of two processes, the formation of alveoli and the maturation of the alveolar septa including the capillary system (27–30). It is believed that alveolization occurs predominantly within the first 2 wk of postnatal life in rats, and then microvascular maturation occurs during the third postnatal week. At about 3 wk, the rat lung appears mature. Alveolization is characterized by rapid tissue proliferation culminating in the budding of small crests from the primary septa. It is also associated with a dramatic increase in alveolar surface density. Microvascular maturation, the second phase of postnatal lung development, is mainly characterized by the maturation of the alveolar septa including the capillary network and by proportionate growth that follows the bulk of alveoli formation. In addition to these morphometric descriptions, autoradiographic studies have provided data on mitotic activity of the various cell types that compose the alveolar wall (31–33). For mesodermally derived cells, which include fibroblasts and endothelial cells, a sharply rising peak of the labeling indices was observed on d 4, just before the intense tissue mass increase whereas the labeling index of type-2 epithelial cells, the stem cells of the alveolar epithelium, reached a peak on d 10 (34, 35).
Our results in the control group are consistent with the data on morphometric and autoradiographic studies performed during the postnatal phase of lung development. Indeed, analysis of the various cyclin/CDK activities indicated that the activities of the complexes formed with CDK2 reached a peak at d 4 and then decreased progressively. Similar observation was made for cyclin E and CDC2 activities, although the activities of these complexes were found already high at birth, and then gradually decreased after d 4. This pick of proliferative activity was also found by Al-Jumaily and co-workers (36), by using flow cytometric analysis of the DNA content of freshly isolated lung fibroblasts.
Data obtained in the dexamethasone-treated animals provide new information on the processes involved in the alteration of lung development following glucocorticoid treatment. We attempted mimicking the glucocorticoid treatment used for premature babies by administrating a short application of high-dosage dexamethasone during the saccular stage of lung development. As previously reported (34), the lungs showed a markedly accelerated maturation at postnatal d 4. In the treated animals, a premature thinning of the septa took place. In those treated animals, the cross-sectional areas of the respiratory airspaces appeared enlarged and the complexity of the lung parenchyma seemed to be reduced (Fig. 1). These notable changes disappeared gradually with age. The dexamethasone-induced reduction of secondary septa formation was observed in parallel to a strong suppression of overall cell proliferation at d 2–4 (34). The results obtained in the present study are consistent with this observation, inasmuch as cyclin/CDK activities were found to be decreased following glucocorticoid administration. The inhibitory effect of dexamethasone on cell proliferation has been documented in various cell systems, including both normal and transformed cells (37, 38). From these studies, it is believed that the antiproliferative actions of glucocorticoids result from a blockage of cell cycle progression during the G1 phase of the cell cycle or at the G1-S boundary (37, 39). In the present work, the reduction of the various cyclin/CDK complex activities in lung tissues upon dexamethasone treatment is consistent with the data obtained in cellular models.
From the data obtained in the present work, it is likely that p21CIP1 and p27KIP1 are important molecular targets of glucocorticoid actions during postnatal lung development. From the current knowledge of their functions and mechanisms of regulation, it can be proposed that these CKIs may contribute to glucocorticoid-induced impairment of postnatal lung parenchyma development by inhibiting the process of proliferation and therefore the outgrowth of new interalveolar septa, and by accelerating the process of differentiation resulting in an acceleration of microvascular maturation. Experiments are in progress to document the factors involved in the increase in p21CIP1 and p27KIP1 in response to glucocorticoid treatment. Characterization of the mechanisms of glucocorticoid-induced alterations of postnatal lung growth is critical for the development of therapeutical strategies aimed at preventing the deletion effects of glucocorticoids on lung maturation in infants.
Abbreviations
- CDK:
-
cyclin-dependent kinase
- Rb:
-
retinoblastoma
- CKI:
-
cyclin kinase inhibitor
References
Beck JC, Mitzner W, Johnson JWC, Hutchins JM, Foildart J, London WT, Palmer AE, Scott R 1981 Betamethasone and the rhesus fetus: effect on lung morphometry and connective tissue. Pediatr Res 15: 235–240
Massaro D, Massaro GD 1986 Dexamethasone accelerates postnatal alveolar wall thinning and alters wall composition. Am J Physiol 251: R218–R224
Tschanz SA, Burri PH 1997 Postnatal lung development and its impairment by glucocorticoids. Pediatr Pulmonol Suppl 16: 247–249
Tschanz SA, Damke BM, Burri PH 1995 Influence of postnatally administered glucocorticoids on rat lung growth. Biol Neonate 68: 229–245
Cherukupalli K, Larson JE, Puterman M, Sekhon HS, Thurlbeck WM 1997 Comparative biochemistry of gestational and postnatal lung growth and development in the rat and human. Pediatr Pulmonol 24: 12–21
Post M 1987 Maternal administration of dexamethasone stimulates cholinaphosphate cytidylyl transferase activity in fetal type II cells. Biochem J 241: 291–296
Pines J 1993 Cyclins and cyclin-dependent kinases: take your partners. Trends Biochem Sci 18: 195–197
Pines J 1994 The cell cycle kinases. Semin Cancer Biol 5: 305–313
Sherr CJ 1993 Mammalian G1 cyclins. Cell 73: 1059–1065
Sherr CJ 1994 G1 phase progression: cycling on cue. Cell 79: 551–555
Sherr CJ 1995 D-type cyclins. Trends Biochem Sci 20: 187–190
Bartek J, Bartkova J, Lukas J 1996 The retinoblastoma protein pathway and the restriction point. Curr Opin Cell Biol 8: 805–814
Sherr CJ 1996 Cancer cell cycles. Science 274: 1672–1677
Weinberg RA 1995 The retinoblastoma protein and cell cycle control. Cell 81: 323–330
Elledge SJ 1996 Cell cycle checkpoints: preventing and identity crisis. Science 274: 1664–1672
Sherr CJ, Roberts JM 1995 Inhibitors of mammalian G1 cyclin-dependent kinases. Genes Dev 9: 1149–1163
Schittny J, Paulson M, Vallan C, Burri PH, Kedei N, Aeschlimann D 1997 Protein cross-linking mediated by tissue transglutaminase correlates with the maturation of extracellular matrices during lung development. Am J Respir Cell Mol Biol 17: 334–343
Corroyer S, Maitre B, Cazals V, Clement A 1996 Oxidant-induced growth-arrest of lung alveolar epithelial cells involves inactivation of cyclin E-CDK2 complex. J Biol Chem 271: 25117–25125
Corroyer S, Nabeyrat E, Clement A 1997 Involvement of the cell cycle inhibitor CIP1/WAF1 in lung alveolar epithelial cell growth arrest induced by glucocorticoids. Endocrinology 138: 3677–3685
Lees E 1995 Cyclin dependent kinase regulation. Curr Opin Cell Biol 7: 773–780
Chen J, Jackson PK, Kirschner MW, Dutta A 1995 Separate domains of p21 involved in the inhibition of CDK kinase and PCNA. Nature 374: 386–388
Luo Y, Hurwitz J, Massagué J 1995 Cell-cycle inhibition by independent CDK and PCNA binding domains in p21Cip1. Nature 375: 159–161
Chang M, Olivier P, Diehl A, Fero M, Sherr CJ 1999 The p21/CIP1 and the p27/KIP1 CDK inhibitors are essential activators of cyclinD-dependent kinases in murine activators. EMBO J 18: 1571–1583
Zhang H, Hannon GJ, Beach D 1994b p21-containing cyclin kinases exist in both active and inactive states. Genes Dev 8: 1750–1758
Durand B, Gao F, Raff M 1997 Accumulation of the cyclin-dependent kinase inhibitor p27/KIP1 and the timing of oligodendrocyte differentiation. EMBO J 16: 306–317
Zhang P, Xong C, DePinho R, Harper J, Elledge S 1998 Cooperation between the CDK inhibitors p27/KIP1 and p57/KIP2 in the control of tissue growth and development. Genes Dev 12: 3162–3167
Burri PH, Dbaly J, Weibel ER 1974 The postnatal growth of the rat lung. I. Morphometry. Anat Rec 178: 711–730
Burri PH 1974 The postnatal growth of the rat lung. III. Morphology. Anat Rec 180: 77–98
Caduff JM, Fisher LC, Burri PH 1986 Scanning electron microscopic study of the developing microvasculature in the postnatal rat lung. Anat Rec 216: 154–164
Massaro D, Teich N, Maxwell S, Massaro GD, Whitney P 1985 Postnatal development of alveoli. Regulation and evidence for a critical period in rats. J Clin Invest 76: 1297–1305
Burri PH, Weibel E 1997 Ultrastructure and Morphometry of the Developing Lung. Raven, New York, pp 215–268.
Burri PH 1997 Postnatal Growth and Development. Raven, Philadelphia, pp 1013–1026.
Kauffman SL, Burri PH, Weibel ER 1974 The postnatal growth of the rat lung. Anat Rec 180: 63–76
Luyet C, Burri PH, Schittny JC 2002 Suppression of cell proliferation and programmed cell death by dexamethasone during postnatal lung developement. Am J Physiol ( in press)
Schittny J, Djonov V, Fine A, Burri PH 1998 Programmed cell death contributes to postnatal lung development. Am J Respir Cell Mol Biol 18: 786–793
Al-Jumaily W, Bruce M 1999 The postnatal age of rat lung fibroblasts influences G1/S phase transition in vitro. In Vitro Cell Dev Biol Anim 35: 410–416
Mouhieddine OB, Cazals V, Kuto E, Le Bouc Y, Clement A 1996 Glucocorticoid-induced growth arrest of lung alveolar epithelial cells is associated with increased production of insulin-like growth factor binding protein-2. Endocrinology 137: 287–295
Satoh M, Yamazaki M 1993 In vitro DNA synthesis of mouse hepatocytes stimulated by tumor necrosis factor is inhibited by glucocorticoids and prostaglandin D2 but enhanced by retinoic acid. J Cell Physiol 157: 104–109
Frost GH, Rhee K, Thompson EA 1993 Glucocorticoid regulation of thymidine kinase (Tk-1) expression in L929 cells. J Biol Chem 268: 6748–6754
Acknowledgements
The authors thank Dr. Jill Lahti for her help in the elaboration of the manuscript.
Author information
Authors and Affiliations
Corresponding author
Additional information
This work was financially supported by grants from Association Claude Bernard, Chancellerie des Universités de Paris (Legs Poix to A.C.), Ligue Nationale contre le Cancer (Fellowship to S.C.; grants 97/RS-BCM100 and 98/RS-BCM43 to A.C.), Ministère de la Santé (PHRC AOB94049 to A.C.), Association pour la Recherche sur le Cancer (grant 9970 to A.C.), Ambassade de France in Switzerland Service Culturel et Scientifique (grant 44-366/84), and the Swiss National Science Foundation (grant 31.55895.98).
Rights and permissions
About this article
Cite this article
Corroyer, S., Schittny, J., Djonov, V. et al. Impairment of Rat Postnatal Lung Alveolar Development by Glucocorticoids: Involvement of the p21CIP1 and p27KIP1 Cyclin-Dependent Kinase Inhibitors. Pediatr Res 51, 169–176 (2002). https://doi.org/10.1203/00006450-200202000-00008
Received:
Accepted:
Issue Date:
DOI: https://doi.org/10.1203/00006450-200202000-00008
This article is cited by
-
Development of the lung
Cell and Tissue Research (2017)
-
Neonatal steroids induce a down-regulation of tenascin-C and elastin and cause a deceleration of the first phase and an acceleration of the second phase of lung alveolarization
Histochemistry and Cell Biology (2014)