Abstract
The urea cycle is a metabolic pathway for the disposal of excess nitrogen, which arises primarily as ammonia. Nitrogen is essential for growth and life-maintenance, but excessive ammonia leads to life-threatening conditions. The urea cycle disorders (UCDs) comprise diseases presenting with hyperammonemia that arise in either the neonatal period (about 50% of cases) or later. Congenital defects of the enzymes or transporters of the urea cycle cause the disease. This cycle utilizes five enzymes, two of which, carbamoylphosphate synthetase 1 and ornithine transcarbamylase are present in the mitochondrial matrix, whereas the others (argininosuccinate synthetase, argininosuccinate lyase and arginase 1) are present in the cytoplasm. In addition, N-acetylglutamate synthase and at least two transporter proteins are essential to urea cycle function. Severity and age of onset depend on residual enzyme or transporter function and are related to the respective gene mutations. The strategy for therapy is to prevent the irreversible toxicity of high-ammonia exposure to the brain. The pathogenesis and natural course are poorly understood because of the rarity of the disease, so an international registry system and novel clinical trials are much needed. We review here the current concepts of the pathogenesis, diagnostics, including genetics and treatment of UCDs.
Similar content being viewed by others
Introduction
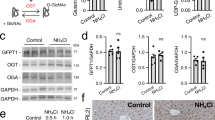
The human body normally maintains protein and amino acid homeostasis by means of processes such as protein synthesis, protein degradation, amino acid oxidation and urea production. Proteins from our nutrition or endogenous sources are constantly degraded back to amino acids and utilized to reconstitute proteins with very little loss (<10%). The daily rate of protein turnover in humans (250–400 g/day) largely exceeds the level of protein intake (50–80 g/day) [1]. Amino acid turnover in the body results in excessive ammonia production. In addition, ammonia is produced by intestinal urease-positive bacteria as well as constantly during amino acid metabolism. Hence, ammonia needs to be detoxified appropriately and the urea cycle performs the critical function of converting ammonia into urea. If this cycle is defective, patients develop diseases presenting with severe hyperammonemia, typically in the neonatal period, caused by congenital or secondary defects in the metabolic enzymes or transporters that comprise the urea cycle (urea synthesis pathway) (Fig. 1). Hyperammonemia leads to cerebral edema, lethargy, anorexia, vomiting, hyperventilation (or hypoventilation), hypothermia, neurologic posturing, and coma. Preventing ammonia toxicity of the nervous system is a major target in treating both primary and secondary hyperammonemia.
A metabolic cascade of the urea cycle in the liver. NH3 enters the urea cycle in the form of carbamoyl phosphate and the reaction leads to urea production, which can be excreted in the urine. In the case of OTC deficiency, excess carbamoyl phosphate leaks into the cytosol and is metabolized to orotic acid. ASL argininosuccinic acid lyase, ASS argininosuccinic acid synthetase, ATP adenosine triphosphate, AcCoA acetyl-CoA, CoASH co-enzyme A, CPS1 carbamoylphosphate synthetase, NAGS N-acetylglutamate synthase, ORNT1 mitochondrial ornithine transporter 1, OTC ornithine transcarbamylase
The enzymes associated with ammonia production
Ammonia is generated by the following enzymes and pathways (Figs. 2, 3). Under baseline conditions, ammonia is produced through the catabolism of glutamine by glutaminase (mucosal epithelial cells) [2], glutamate dehydrogenase (GDH; small intestine) and bacterial deaminase (large intestine) [3]. In addition, urea is metabolized to ammonia by bacterial urease (large intestine) [4]. Ammonia produced in the gastrointestinal tract accumulates in the portal vein where the concentration is 2–5 times higher than in the systemic circulation, which explains the hyperammonemia caused by portosystemic shunts [5]. The second route of ammonia production is the nitrogen metabolism associated with amino acid catabolism (mainly in the brain and skeletal muscle) [5]. An important reaction for releasing ammonia is GDH, that reacts as an oxidative deamination. Because ammonia releasing is critical, GDH is regulated by many substances. For example, adenosine diphosphate and l-leucine are well-known as allosteric activators, whereas guanosine triphosphate, adenosine triphosphate (ATP), long-chain fatty acids, estrogens, epigallocatechin gallate, and nicotinamide adenine dinucleotide act as allosteric inhibitors [6]. Under normal conditions, GDH predominantly catabolize glutamate, producing α-ketoglutarate and ammonia, probably due to the relatively high concentration of glutamate and the low concentration of ammonia present in the mitochondria; in contrast, under catabolic conditions high concentration of α-ketoglutarate and ammonia inside the mitochondria is thought to trigger biosynthesis of glutamate by GDH [6,7,8]. In addition, high concentration of α-ketoglutarate and ammonia promote glutamine production from glutamate by glutamine synthetase (GS) [9]. The ammonia produced in various tissues of the body is transported as glutamine to the liver, in which these amino acids are converted into glutamate via a process called transamination, and the released ammonia is metabolized to urea by the urea cycle. Glutamine is broken down into ammonia and glutamate by glutaminase, which is important especially in liver and kidney. If catabolism is accelerated under the condition of liver dysfunctions such as cirrhosis or in UCDs, this reaction increases and ammonia can raise to levels capable to cause brain damage. Hence, it is mainstay of treatment for UCD patients to prevent catabolism and control the plasma glutamine level, which can be seen as an important biomarker for the total nitrogen metabolism, and, if elevated, as an indicator for too high levels of protein intake.
Human ammonia generation and metabolism. In the gastro-intestinal tract, ammonia is produced by mucosal glutaminase (intestine), mucosal adenosine deaminase, glutamate dehydrogenase (intestine), bacterial deaminase (colon), and bacterial urease (colon). Ammonia from the portal vein and systemic blood is metabolized into urea by the urea cycle. Ammonia is also metabolized into glutamine by glutamine synthetase in the brain and in skeletal muscle. Synthesized glutamine is catalyzed to ammonia and glutamate by glutaminase in the liver
The enzymes associated with the urea cycle and its disorders
Krebs and Henseleit [10] reported in 1932 that ornithine activates urea synthesis and described the urea cycle as the pathway, which converts ammonia into urea prior to excretion via the kidney. The biochemical reaction that produces urea from ammonia is performed mainly in the liver and to a much lesser extent in the kidney. The overall energy flux of the urea cycle is shown in the following equation [10].
The conversion of two molecules of ammonia to urea requires 3 ATP, and ~10% of the ATP produced in the mitochondria is consumed by the urea cycle. In the mammalian organisms, ammonia is excreted as fixed nitrogen in the form of urea.
Carbamoylphosphate synthetase 1 (CPS1: EC 6.3.5.5)
CPS1 is the first enzyme in the urea cycle, and the gene located in 2q25 (Table 1). CPS1 catalyzes the condensation of ammonia and bicarbonate into carbamoylphosphate in the mitochondrial matrix, which requires an allosteric activator, N-acetylglutamate (NAG), magnesium (Mg2+), and ATP (Fig. 1). CPS1 is the rate limiting enzyme of the urea cycle. CPS1 deficiency is an autosomal recessive disorder and is one of the most severe UCDs. The estimated prevalence is 1/975,000 in the US [11] and 1/800,000 in Japan [12]. Usually, clinical symptoms are seen during the neonatal period already a few days after birth along with hyperammonemia, sometimes resulting in death, or neurological damage if patients survive. Laboratory findings demonstrate hyperammonemia, elevated plasma glutamine, and alanine concentrations without increased urinary orotic acid (Table 1). In case of a suggestive biochemical profile, however, molecular testing is required to distinguish CPS1 deficiency from NAG synthase (NAGS) deficiency.
N-acetylglutamate synthase (NAGS: EC 2.3.1.1)
NAGS catalyzes the conversion of glutamate and acetyl-CoA to NAG, which is the allosteric activator of CPS1 (Fig. 1). Mutations of the NAGS gene, located on 17q21.3 (Table 1), lead to a deficiency of NAG and a defect of CPS1, which cannot convert ammonia into carbamoylphosphate in the absence of NAG. Hence, NAGS deficiency leads to a functional deficiency in CPS1. Laboratory investigations and clinical findings cannot distinguish NAGS from CPS1 deficiency, thus molecular testing is required. NAGS deficiency is an ultra-rare autosomal recessive disorder, and the exact prevalence is unknown. Because there is an effective treatment available, a drug that is an analog of NAG (N-carbamoylglutamate), it is very important to fast and reliably diagnose NAGS deficiency by gene analysis for early intervention.
Ornithine transcarbamylase (OTC: EC 2.1.3.3)
OTC catalyzes the synthesis of citrulline from carbamoylphosphate and ornithine (Fig. 1). The OTC gene is located on Xp21.1 (Table 1). Thus, OTC deficiency is, as the only UCD, an X-linked genetic disease [12]. OTC deficiency is the most common UCD with a prevalence of 1/63,000 in the US [7] and 1/80,000 in Japan [12]. Mutations that abrogate OTC activity result in a severe form of disease with neonatal onset, as usually seen in hemizygous male patients. In contrast, mutations that decrease OTC activity but allow for some residual enzyme function result in the late-onset form, as often seen in heterozygous females. In fact, female carriers may rarely be affected, depending on the level of X-inactivation. Clinical symptoms observed in male neonates, include severe hyperammonemia that typically manifests already a few days after birth. Patients with late-onset OTC deficiency often present with episodic symptoms, but acute hyperammonemia can manifest at any age. Laboratory findings during an episode of hyperammonemia, include elevated plasma glutamine and alanine concentrations, along with particularly elevated urinary orotic acid (Table 1 and Fig. 1). Definitive diagnosis can be achieved by genetic analysis or, at least in males, measurement of OTC enzyme activity in the liver.
Argininosuccinate synthetase 1 (ASS1: EC 6.3.4.5)
ASS1 conjugates citrulline and aspartate in the cytosol of hepatocytes to generate argininosuccinate (Fig. 1). Citrulline and aspartate are transported to the cytoplasm from the mitochondrial matrix through the ornithine transporter ORNT1 and the aspartate-glutamate carrier (called citrin), respectively. The ASS1 gene is located on 9q34, and ASS1 deficiency (called citrullinemia type I) is an autosomal recessive disorder with broad phenotypic variability, ranging from severely affected patients with neonatal hyperammonemia to asymptomatic children or adults with only biochemical manifestations of the disease. Laboratory findings include marked elevation of the plasma citrulline concentration, elevation of the plasma glutamine and alanine concentrations, and mild elevation of urinary orotic acid (Table 1).
Citrin (aspartate–glutamate carrier)
Citrin acts as a mitochondrial membrane aspartate–glutamate transporter encoded by SLC25A15, a gene localized on 7q21.3 (Table 1). Mutations in this gene result in defective citrin activity, reducing aspartate export from the mitochondria to the cytosol, leading to a condition in which aspartate is not available as ASS substrate to generate argininosuccinate in the liver [13]. During the neonatal period in affected individuals, the levels of various amino acids in the blood are high, including citrulline, phenylalanine, threonine, tyrosine, and methionine, and patients also present with increased galactose in blood and urine. In the neonatal period and infancy, patients typically present with intrahepatic cholestasis, which often improves spontaneously to some degree. After an often-asymptomatic period during childhood, some patients become symptomatic again in adolescence or adulthood, presenting mainly neuropsychiatric symptoms, recurrent hyperammonemia and increased plasma citrulline (hence the condition is called citrullinemia type 2), although this is mainly reported in Asia.
Argininosuccinate lyase (ASL; EC: 4.3.2.1)
ASL is a cytosolic enzyme which catalyzes argininosuccinate to arginine and fumarate. The ASL gene is located on 7cen-q11.2 [14]. Mutations of this gene result in argininosuccinic aciduria, which is an autosomal recessive disorder, and tissue accumulation of argininosuccinate. There is a wide range in the severity of ASL deficiency with clinical and biochemical findings likely caused by a combination of tissue specific deficiency of arginine and/or elevation of argininosuccinate [15, 16]. In cases of neonatal onset, severe hyperammonemia appears starting from a few days after birth, and the mortality rate is high. The late-onset form is associated with cognitive impairment, stunted growth, and liver dysfunction with hepatomegaly and fibrosis/cirrhosis. Hair abnormalities (called trichorrhexis nodosa) are observed that are specific to this disease. Furthermore, the sequelae frequently observed in ASL deficiency, include chronic hepatopathy with a bleeding tendency caused by mild elevation of transaminases and coagulation factor abnormalities. Acute episodes of severe hyperammonemia occur when the patient is in a catabolic state, such as during the course of an infection. Laboratory findings include hyperammonemia, mild elevation of transaminases, non-specific elevated plasma glutamine and alanine concentrations, moderate elevation of the plasma citrulline concentration, and marked elevation of plasma argininosuccinate (Table 1). Argininosuccinate is also found in the urine and cerebrospinal fluid, with the concentrations higher in the cerebrospinal fluid than in plasma.
Arginase 1 (ARG1; EC: 3.5.3.1)
Arginase 1 (ARG1) catalyzes the hydrolysis of arginine to ornithine and urea as the final step in the urea cycle. The ARG1 gene is located on 6q23 (Table 1). Mutations of this gene cause defective ARG1 activity and comprise an autosomal recessive disorder that exhibits phenotypic variability. ARG1 deficiency is not typically characterized by acute onset hyperammonemia. Instead, patients often present with developmental delay and progressive spasticity. They often develop seizures, hepatomegaly and gradually loose prior intellectual attainments. Laboratory findings include marked elevation of arginine in the plasma and cerebrospinal fluid, and moderate elevation of urinary orotic acid. The plasma ammonia concentration is either normal or only slightly elevated. Excretion of arginine, lysine, cystine, and ornithine in the urine may be elevated, but can also be normal. Urinary guanidino compounds (α-keto guanidino valerate and alginate) are significantly elevated.
Mitochondrial ornithine transporter (ORNT1)
The transport of ornithine from the cytosol to the mitochondrial matrix and the export of citrulline from the mitochondrion into the cytosol is carried out by ORNT1, which is encoded by SLC25A15 located on 13q1 (Table 1). Mutations of this gene cause ornithine translocase deficiency (also called hyperornithinemia, hyperammonemia, and homocitrullinuria syndrome, HHH syndrome). The plasma ornithine concentrations in this condition become extremely high. Homocitrulline is thought to originate from the carbamylation of lysine. Most affected patients have intermittent hyperammonemia accompanied by coagulation disorders, signs of spasticity, vomiting, lethargy, and coma. Growth is abnormal and intellectual development is negatively affected.
Ammonia toxicity
Ammonia easily crosses the blood-brain barrier in its non-ionized form. Once a metabolic crisis has developed, a large amount of ammonia can accumulate in the blood and also the brain. Hyperammonemia causes neurological dysfunction such as tremor, ataxia, seizures, coma, and death. However, the mechanisms of the brain damage induced by hyperammonemia still remain to be fully elucidated. In the normal state, ammonia is rapidly metabolized to glutamine by GS, mainly in astrocytes, liver and skeletal muscle. Hence, the plasma glutamine concentration can be seen as an indicator for the total nitrogen load of the organism. In patients with OTC deficiency, the brain glutamine level was reported to be twofold increased [17]. The accumulation of intracellular glutamine in astrocytes is believed to be a major cause of brain damage, because glutamine is osmotically active and thus leads to astrocyte swelling [18]. In addition, hyperammonemia disturbs glutamatergic neurotransmission and affects other neurotransmitter systems [19, 20]. The acute hyperammonemia was reported to cause excitotoxic cell death, decrease in astrocyte transporters, increased extracellular glutamate, decreased brain glutamate and loss of α-amino-3-hydroxy-5-methyl-4-isoxazolepropionic acid (AMPA) receptors [19,20,21]. Excess extracellular glutamate is known to be an excitotoxic agent that activates N-methyl-D-aspartate (NMDA) receptors, which leads to disturbed nitric oxide (NO) metabolism, Na+/K+-ATPase, ATP shortage, mitochondrial dysfunction, free radical accumulation and oxidative stress [22]. Imbalances of amino acids can also contribute to the brain damage that occurs in UCDs. Spf mice, which have a single point mutation in the Otc gene, presented with some neutral amino acids accumulation in the brain (i.e., tryptophan, tyrosine, phenylalanine, methionine, and histidine), and it was suggested that the accumulation of tryptophan may cause an abnormality in serotoninergic neurotransmission [23]. In addition, ATP content was shown to be decreased in the brain of spf mice [24]. Recently, it is reported that acute hyperammonemia in vivo caused the extracellular potassium concentration in neurons and activated the Na+-K+−2Cl− cotransporter isoform 1 (NKCC1) in neurons without brain edema, that may be a main pathophysiology to trigger neuronal disinhibition and seizures [25].
Symptoms
UCD symptoms correlate to some extent with the ammonia level in the body. Typically, patients with primary UCDs present with neurological abnormalities such as abnormal posturing, vomiting, ataxia, confusion and irritability during the neonatal period. Hyperventilation is a common symptom and causes respiratory alkalosis, which worsens brain edema. If appropriate intervention does not take place, the patients develop seizures, enter into coma and die. In milder cases, clinical symptoms may be recognized by loss of appetite, cyclical vomiting, lethargy, behavioral abnormalities, sleep disorders, delusions, hallucinations, and psychosis. Liver involvement is a frequent finding in UCDs [26]. Liver involvement can result in acute liver failure but also in long-term complications such as cirrhosis (described in NICCD, CTLN2, OTCD, and ASLD) and hepatocellular carcinoma (described in CTLN2, citrullinemia type 1, and ASLD).
UCDs can be classified according to the form of onset
- 1.
Presymptomatic form: identified by predelivery diagnosis (see the “prenatal testing”) or neonatal screening tests (see the “neonatal screening tests).
- 2.
Neonatal-onset form: neurological symptoms (written above) associated with hyperammonemia during the neonatal period.
- 3.
Late-onset form: neurological symptoms with hyperammonemia persist from infancy through adulthood, and are triggered by several triggers leading to catabolic states (Table 2).
Table 2 Potential triggers of hyperammonemia in UCD patients
Clinical investigation and the laboratory tests for diagnosis
UCDs should be primarily suspected when a patient presents with hyperammonemia without metabolic acidosis and with a normal blood glucose level. Consortia for UCDs in the EU, USA, and Japan have published guidelines and a diagnostic flowchart is shown in Fig. 4. Most cases do not present with liver dysfunction. However, there were cases with liver dysfunction reported and summarized in a review in 2017 [26]. ARG and ASL deficiencies are distinguished by elevated concentrations of arginine and argininosuccinic acid, respectively. Hypercitrullinemia without increased argininosuccinic acid is suggestive of ASS deficiency. A patient who presents with urinary orotic acid along with low plasma concentrations of citrulline and arginine, is likely to be diagnosed as having OTC deficiency. If urinary orotic acid is low-normal or even decreased in cases with low plasma concentrations of citrulline and arginine, CPS1 or NAGS deficiency is suspected. HHH syndrome should be suspected in cases of hyperammonemia associated with high blood ornithine and urinary homocitrulline. For the purpose of differential diagnosis, other important diseases should be considered, such as mitochondrial disorders, fatty acid oxidation disorders, systemic sepsis, liver failure, and portosystemic shunt.
Testing for plasma ammonia levels
Plasma ammonia levels should be measured in patients during any age, presenting (1) an unexplained change in consciousness; (2) unusual or unexplained neurological illness; (3) liver failure; and (4) suspected intoxication.
Normal levels, according to the Association of Clinical Biochemistry [27], are written below:
Premature neonates: <150 μmol/L (255 μg/dl)
Term neonates: <100 μmol/L (170 μg/dl)
Infants and children: <40 μmol/L (68 μg/dl)
Adolescents and adults: 11–32 μmol/L (19–54 μg/dl)
Differential diagnoses should be investigated when plasma ammonia levels are increased with any symptoms related to hyperammonemia (see “symptoms”). Ammonia levels exceeding 300 μmol/L are a sign of severity, leading often to poor prognosis.
Amino acid analysis
The plasma and urinary amino acid profiles in patients with UCDs can show specific changes. In particular, the analysis of amino acids can reveal an accumulation of a precursor amino acid or a reduction of urea cycle intermediary amino acids resulting from and thereby specifying the defective enzyme. Hence, amino acid analysis is used for the initial biochemical diagnosis of UCDs. For example, in patients with OTC deficiency, the plasma glutamine, alanine, and glycine levels are increased, with a decrease in citrulline and arginine levels [28, 29]. Typical examples of the amino acid profiles in UCDs are provided in Table 1.
Urinary orotic acid
Orotic acid is an intermediate in pyrimidine biosynthesis. The urinary excretion of orotic acid is increased in many UCDs including defects of OTC, ASS, ASL, ARG1, and ORNT1 (Table 1), because of accumulated carbamoylphosphate. In UCDs, orotic acid is mainly a marker of OTC deficiency that distinguishes it from CPS1 deficiency (Table 1 and Fig. 1). Biochemically, orotic acid is a biosynthetic intermediate of pyrimidine bases that is produced by dihydroorotate dehydrogenase from dihydroorotate, and is converted to orotidine monophosphate by orotate phosphoribosyltransferase. Orotic acid is not elevated in CPS1 or NAGS deficiency. Notably, urinary orotic acid correlates with the clinical course and metabolic status in the body. In particular, urinary orotic acid excretion increases in allopurinol loading tests, which are performed to detect “non-symptomatic” female carriers of OTC deficiency or to select living donors for liver transplantation (LT). However, the low sensitivity of this test is an issue of concern about which clinicians should be aware.
Enzyme activity analysis
Although genetic analysis is the method of choice for diagnostic confirmation and prenatal testing, enzyme activity assays can help confirming the diagnosis and the residual activity if the genetic test does not give a clear result. Liver tissue, the intestinal mucosa, erythrocytes, and fibroblasts can be used for enzyme activity assay in some of the UCDs. Specifically, the urea cycle is fully expressed only in the liver, with CPS1, OTC, and NAGS expressed primarily in liver cells. It should be noted that in OTC deficiency, as it constitutes an X-linked disorder, the enzyme activities in female patients can largely vary within in the liver, in accordance with the Lyonization principle (i.e., it will vary depending on the proportion of wild-type to mutant X-chromosomes having undergone X-inactivation in the sample site).
Genetic analysis
Genetic testing is the method of choice to confirm the diagnosis of a UCD nowadays. The sensitivity of genetic analysis varies between the different disorders but is at least 80%. The confirmation of the causative mutation is essential in order to offer prenatal diagnosis and family counseling. Gene analysis is also needed to distinguish CPS1 and NAGS deficiencies, because these cannot be distinguished by biochemical data alone (unless liver biopsy-based enzyme analysis is done).
Prenatal testing
Prenatal testing in UCDs is available in several countries for pregnancy termination in the severe cases. This may also be indicated in milder UCDs or for NAGS deficiency (which has a curable therapy) for psychological reasons and to prepare for perinatal management [30,31,32]. The genetical techniques of mutation- or disease allele-tracking using chorionic villus samples, amniotic fluid cells or cultures [33, 34] are useful because it gives rapid and clear-cut results in a short term with little fetal risk. Prenatal tests using amniotic fluid citrulline and ASA are also suitable for respective ASS and ASL deficiencies [34,35,36]. In all these cases, prenatal testing requires joint careful counseling by clinical geneticists and metabolic specialists.
Newborn screening (NBS)
NAGS, CPS1, and OTC deficiencies are generally not yet screened in most countries because of the low specificity and sensitivity for detection of decreasing citrulline levels by tandem mass screening with dried blood spots [37]. The screening for ASS, ASL, and ARG1 deficiencies are operated in most US states, Taiwan, and Australia by assessing respectively citrulline, ASA and arginine levels in dried blood spots. Although there are few false positives and no false negatives for severe ASS and ASL deficiencies [38,39,40], ASL deficiency screening was stopped in Austria because many newborns who remained asymptomatic were detected [41]. All jurisdictions in US screening for hyperargininemia take arginine as the initial action indicator. Several programs reported to use the Arg/Orn ratio as a secondary discriminator.
Treatment
It is urgent to reduce the plasma ammonia level and protect against brain damage when hyperammonemia is noted. The reader is referred to the readily available guidelines for diagnosis and treatment of UCDs in the US, Europe, and Japan. Each guideline (in Europe and the US) is available online [42, 43]. Collaboration with metabolic specialist centers is essential (Tables 2, 3). The following sections describe the essentials of UCD treatment.
Clinical treatment
In the acute phase, hemodialysis or hemodiafiltration are the most efficient treatments for reducing the plasma ammonia concentration. The dialysis method depends on the condition of the affected patient, the available equipment, and the experience of the dialysis team. For instance, continuous hemodiafiltration is often used in neonates because of the greater safety and tolerability. However, any of the hemodialysis methods are recommended for ammonia clearance, while peritoneal dialysis is ineffective and not recommended in any of the guidelines. It is also important that it takes a few hours to prepare hemodialysis and the loss of time correlates with brain damage. Hence, other treatment options should be performed in parallel in order to achieve fast ammonia reduction. Reducing ammonia production can be achieved with intravenous administration of l-arginine hydrochloride and nitrogen-removing agents (e.g., sodium phenylacetate and sodium benzoate) [44,45,46]. After a loading dose of the latter, the patient receives an intravenous maintenance dose, which is switched to oral administration once patients have stabilized (Table 3). In the acute phase, protein intake should be stopped. However, complete protein removal for more than 24–48 h is not recommended, because endogenous protein catabolism may occur. Thus, it is important to administer small amounts of protein (0.1–0.3 g/kg/day) starting from an early stage (2 or 3 days after diagnosis). Dietary management during acute decompensation is shown in Table 4. Carbohydrates and lipids can be used as calories during the acute phase, such as through intravenous administration of glucose (use at least 10% solutions) and lipids and/or administration of a protein-free milk via a gastric tube. It is considered best practice to transition from parenteral to enteral administration as early as possible.
In the chronic phase, preventing both a catabolic condition and a recurrence of hyperammonemia is important. The drugs recommended for long-term treatment are shown in Table 5. Any form of catabolism, tissue damage and bleeding are triggering events to prevent. It is also important to educate the family about the way to prevent a catabolic state. A protein-restricted diet and formula should be maintained and high-caloric intake is needed, which is the mainstay of long-term management that is based on minimizing the nitrogen load on the urea cycle life-long unless LT is performed. The suitable amount of natural protein depends on individual demand and residual enzyme or transporter function. The FAO/WHO/UNU 2007 report (summarized in Table 6) could be useful for energy intake. Nasogastric (NG) tube or gastrostomy feeding may be necessary to ensure sufficient energy intake. It is sometimes difficult to determine the balance of nutritional requirements. Therefore, a metabolic specialist should be involved in the management on a regular basis.
Dehydration, for instance related to alcohol intake, exercise and long flights, should be avoided. Use of valproic acid or steroids, long-term periods of fasting, and high intake of protein or amino acids can induce hyperammonemia and should also be avoided.
Liver transplant
The first cases of LT for UCDs, reported by Largilliere et al. in 1989 [48] and Tuchman et al. in 1989 [49], demonstrated that LT is able to normalize the plasma ammonia levels in UCD patients. Leonard and McKiernan reported on a total of 59 patients (32 OTC deficiency, 9 citrullinemia type I, 9 citrullinemia type II, 6 CPS1 deficiency, 2 ASL deficiency and 1 arginase deficiency), with a 5-year survival rate of 93% after LT (55/59 patients) [50]. The quality of life substantially improved in all of these surviving children. A normalization of diet and a reduction in hospital admissions were observed. Kasahara et al. reported a retrospective analysis in Japan on organ sharing data for liver recipients who had undergone LT at an age <18 years in the period 1989–2010 [51]. In Japan, LT is performed as living-related LT (LRLT) in almost all cases. In this period in Japan, 2224 pediatric patients underwent LRLT including 57 UCD patients (40 OTC deficiency, 6 citrullinemia type I, 9 CPS1 deficiency, and 2 ASL deficiency). For children with UCDs, the 20 years survival rate was 95.9%. Almost all of the cases improved or completely recovered after LT. Of course, LT is not a perfect therapy because there are small amounts of defective enzymes that are still present in the kidney, gut and brain. The physiological importance of cerebral expression of some urea cycle enzymes, such as ASL and ARG, has been reported. In addition, the plasma concentration of citrulline (e.g., in case of OTC or CPS1 deficiency) is not corrected by LT, so citrulline supplementation is still required for OTC or CPS1 deficiency patients after LT.
Indications for LT
Liver transplantation is a curable therapy for all UCDs (except NAGS deficiency that can bet treated with medication), and allows termination of protein restriction and alternative pathway therapy. In all patients with severe neonatal onset (except NAGS deficiency), LT should be considered and done before 1 year of age in order to achieve the best neurological outcome [52]. To prevent irreversible brain damage, earlier LT is recommended. However, it should be deferred at least before 3 months and/or 5 kg body weight because of the increased LT-related complications and lower survival rates [53, 54]. On the other hand, since technical advancement is promoting constantly, the recommended age and body weight for LT is changing and depend on the skills and experience in every institute. Each LT candidate is assigned a score that reflects the probability of death within a 3-month period as determined by the model for end-stage liver disease (MELD) scoring system or the pediatric end stage liver disease scoring system. It is clear that a disease severity scoring system that is focused on liver biochemical levels will disadvantage patients with life-threatening diseases where liver synthetic capacity is not affected (such as UCDs and hepatocellular carcinoma), or patients with manifestations that are not immediately life-threatening but contribute significantly to morbidity such as ascites and hepatic encephalopathy. To deal with this limitation, allocation policies allow MELD exceptions in the case of inherited metabolic disorders. In Japan, almost all cases underwent LDLT. The indications for LDLT were retrospectively evaluated according to a grading score system based on the guidelines recommended by the Japanese Ministry of Health, Labor and Welfare [55]. With regard to X-linked OTC deficiency, symptomatic heterozygous maternal donors should not be considered potential donor candidates.
Neurological outcome after LT
Uchino et al. [56] and Kido et al. [57] reported the long-term outcome of large cohorts of UCDs in Japan. In comparison of the two study periods, the 5-year survival rate of patients with OTC deficiency improved to 86% for those with the neonatal-onset type and to 92% for those with the late-onset type. Severe brain damage was observed in patients who presented with more than 360 μmol/L of plasma ammonia [57]. Early LT was thus shown to be able to prevent severe brain damage and thus provides a chance for an improved cognitive outcome. Developmental outcome after early LT was prospectively investigated by McBride et al. [47]. They evaluated three infants (age at LT 5, 11, and 3 months, respectively) and one female OTC deficient child with LT performed in early childhood using the Griffiths Mental Developmental Scale. After LT, only mild to moderate psychomotor delay (average overall score 66.7, normal range 100 ± 10.8) was found.
Experimental therapies
-
1.
Hypothermia therapy is now under investigation for treatment of hyperammonemic encephalopathy [58, 59]. Mild systemic hypothermia (34–35 ℃ for 48 h) combined with hemofiltration in neonatal UCD patients resulted in a rapid reduction in the plasma ammonia concentration [60]. Animal experiments and a small number of clinical trials in hepatic encephalopathy caused by acute liver failure both suggest that therapeutic hypothermia provides neuroprotection in hyperammonemia-associated encephalopathy. However, it cannot be recommended until randomized controlled studies confirm these findings.
-
2.
Liver cell therapy (LCT) was studied in an open, multicenter trial in the US and Canada that aimed to demonstrate the safety and efficacy of LCT in children with UCDs [61]. Children aged 0–5 years suffering from OTC deficiency, CPS1 deficiency or citrullinemia were admitted to the trial. Five treatment centers and ten additional centers recruited patients and offered them continuing treatment in the SELICA III trial. Unfortunately, the SELICA III clinical trial program was terminated and no further trial was approved in the US or Canada. In Japan, the first UCD case treated with LCT was reported in 2013 by the National Center for Child Health and Development (newspaper reports) and this is still ongoing.
-
3.
Stem/progenitor cell-based therapy should be a hopeful therapy for UCDs. In 2007, Najimi and Sokal reported that liver mesenchymal-like cells were isolated from adult human liver [62]. These isolated adult-derived liver mesenchymal stem-cells proliferated and differentiated into hepatocyte-like cells both in vitro and in vivo, making them an attractive expandable cell source for stem cell therapy in human liver diseases.
-
4.
Gene therapy is reported in animal models of defects of OTC [63,64,65], ASS [66, 67], and ASL [68, 69]. OTC deficiency has been a major target for a preclinical gene therapy trial. Ye et al. [70] reported that using an improved adenovirus-mediated gene transfer in OTC deficient (OTC spf-ash) mice was associated with a complete normalization of liver OTC enzyme activity that persisted for at least 2 months. This early preclinical success led to an ill-fated phase 1 clinical trial for partial OTC deficiency in 1999 [71]. The first 17 patients recruited to this dose escalation safety study were treated without any complications. However, the 18th patient developed a fatal systemic inflammatory response with disseminated intravascular coagulation and multi-organ failure which culminated in his death [72]. This event was linked to the immunobiology of adenoviral vectors and led to a greater focus on the preclinical evaluation of vector safety. In 2017, a safety and dose-finding study (DTX301; ClinicalTrials.gov Identifier: NCT02991144) with AAV8 in adults with late onset OTC deficiency has started and is now ongoing [73, 74].
Closing remarks
Individual guidelines in the US, Europe and Japan have been established and are being used in many countries. Patient registries have been established in Europe and the US and in some parts of Japan. However, UCDs are rare disorders and no guideline can be considered perfect. There is no doubt that hemodialysis and LT improve the prognosis. Further improvement will require new therapies, but additional effort is needed to make them become a reality.
References
Schutz Y. Protein turnover, ureagenesis and gluconeogenesis. Int J Vitam Nutr Res. 2011;81:101–7.
Haberle J, Gorg B, Rutsch F, et al. Congenital glutamine deficiency with glutamine synthetase mutations. N Engl J Med. 2005;353:1926–33.
James LA, Lunn PG, Middleton S and Elia M. Distribution of glutaminase and glutamine synthetase activities in the human gastrointestinal tract. Clin Sci. 1998;94:313–9.
Levitt DG and Levitt MD. Gastrointestinal urease in man. I Activity of mucosal urease. Gut. 1966;7:631–5.
Levitt DG, Levitt MD. A model of blood-ammonia homeostasis based on a quantitative analysis of nitrogen metabolism in the multiple organs involved in the production, catabolism, and excretion of ammonia in humans. Clin Exp Gastroenterol. 2018;11:193–215.
Maria MAdevaa, Gema Soutob, Natalia Blancoc, Cristóbal Donapetrya. Ammonium metabolism in humans. Metabolism. 2012;61:1495–511.
Plaitakis A, Zaganas I. Regulation of human glutamate dehydrogenases: implications for glutamate, ammonia and energy metabolism in brain. J Neurosci Res. 2001;66:899–908.
Stanley CA, Lieu YK, Hsu BY, Burlina AB, Greenberg CR, Hopwood NJ, et al. Hyperinsulinism and hyperammonemia in infants with regulatory mutations of the glutamate dehydrogenase gene. N Engl J Med. 1998;338:1352–7.
Cooper AJ, Jeitner TM. Contral role of glutamate metabolism in the maintenance of nitrogen homeostasis in normal and hyperammonemic brain. Biomolecules. 2016;6:1–33. 16
Krebs HA, Henseleit K. Untersuchungen über die Harnstoffbildung im Tierkörper. Klin Woche. 1932;ume 11(Issue 18):757–9. pp
Batshaw ML, Tuchman M, Summar M, Seminara J. Members of the urea cycle disorders consortium. A longitudinal study of urea cycle disorders. Mol Genet Metab. 2014;113:127–30.
Nagata N, Matsuda I, Oyanagi K. Estimated frequency of urea cycle enzymopathies in Japan. Am J Med Genet. 1991;39:228–9.
Kobayashi K, Sinasac DS, Iijima M, Boright AP, Begum L, Lee JR, et al. The gene mutated in adult-onset type II citrullinaemia encodes a putative mitochondrial carrier protein. Nat Genet. 1999;22:159–63.
Abramson RD, Barbosa P, Kalumuck K and O’Brien WE. Characterization of the human argininosuccinate lyase gene and analysis of exon skipping. Genomics. 1991;10:126–32.
Keskinen P, Siitonen A, Salo M. Hereditary urea cycle diseases in Finland. Acta Paediatr. 2008;97:1412–9.
Erez A, Nagamani SC, Lee B. Argininosuccinate lyase deficiency-argininosuccinic aciduria and beyond. Am J Med Genet C Semin Med Genet. 2011;157:45–53.
Connelly A, Cross JH, Gadian DG, Hunter JV, Kirkham FJ and Leonard JV. Magnetic resonance spectroscopy shows increased brain glutamine in ornithine carbamoyl transferase deficiency. Pediatr Res. 1993;33:77–81.
Brusilow SW, Koehler RC, Traystman RJ, Cooper AJ. Astrocyte glutamine synthetase: importance in hyperammonemic syndromes and potential target for therapy. Neurotherapeutics. 2010;7:452–470.
Butterworth RF. Effects of hyperammonaemia on brain function. J Inherit Metab Dis. 1998;21:6–20.
Felipo V, Butterworth RF. Neurobiology of ammonia. Prog Neurobiol. 2002;67:259–79.
Robinson MB, Hopkins K, Batshaw ML, McLaughlin BA, Heyes MP, Oster-Granite ML. Evidence of excitotoxicity in the brain of the ornithine carbamoyltransferase deficient sparse fur mouse. Brain Res Dev Brain Res. 1995;90:35–44.
Rodrigo R1, Cauli O, Boix J, ElMlili N, Agusti A and Felipo V. Role of NMDA receptors in acute liver failure and ammonia toxicity: therapeutical implications. Neurochem Int. 2009;55:113–8.
Bachmann C, Colombo JP. Increase of tryptophan and 5-hydroxyindole acetic acid in the brain of ornithine carbamoyltransferase deficient sparse-fur mice. Pedia Res. 1984;18:372–5.
Ratnakumari L, Qureshi IA, Butterworth RF. Effects of congenital hyperammonemia on the cerebral and hepatic levels of the intermediates of energy metabolism in spf mice. Biochem Biophys Res Commun. 1992;184:746–51.
Rangroo ThraneV1, Thrane AS, Wang F, Cotrina ML, Smith NA, Chen M, et al. Ammonia triggers neuronal disinhibition and seizures by impairing astrocyte potassium buffering. Nat Med. 2013;19:1643–8.
Bigot A, Tchan MC, Thoreau B, Blasco H, Maillot F. Liver involvement in urea cycle disorders: a review of the literature. J Inherit Metab Dis. 2017;40:757–69.
Hawke L. Ammonia (plasma, blood). http://www.acb.org.uk/whatwedo/science/-AMALC.aspx. Published 2012. Accessed 26 March 2019.
Maestri NE, McGowan KD, Brusilow SW. Plasma glutamine concentration: a guide in the management of urea cycle disorders. J Pediatr. 1992;121:259–61.
Berry GT, Steiner RD. Long-term management of patients with urea cycle disorders. J Pediatr. 2001;138(Suppl 1):S56–60.
Leonard JV, Ward Platt MP, Morris AA. Hypothesis: proposals for the management of a neonate at risk of hyperammonaemia due to a urea cycle disorder. Eur J Pedia. 2008;167:305–9.
Maestri NE, Hauser ER, Bartholomew D, Brusilow SW. Prospective treatment of urea cycle disorders. J Pedia. 1991;119:923–8.
Sniderman King L, Singh RH, Rhead WJ, Smith W, Lee B, Summar ML. Genetic counseling issues in urea cycle disorders. Crit Care Clin. 2005;21:S37–S44.
Häberle J, Koch HG. Genetic approach to prenatal diagnosis in urea cycle defects. Prenat Diagn. 2004;24:378–83.
Kamoun P, Fensom AH, Shin YS, Bakker E, Colombo JP, Munnich A, et al. Prenatal diagnosis of the urea cycle diseases: a survey of the European cases. Am J Med Genet. 1995;55:247–50.
Chadefaux-Vekemans B, Rabier D, Chabli A, Blanc A, Aupetit J, Bardet J et al. Improving the prenatal diagnosis of citrullinemia using citrulline/ornithine+arginine ratio in amniotic fluid. Prenat Diagn. 2002;22:456–8.
Mandell R, Packman S, Laframboise R, Golbus MS, Schmidt K, Workman L, et al. Use of amniotic fluid amino acids in prenatal testing for argininosuccinic aciduria and citrullinaemia. Prenat Diagn. 1996;16:419–24.
Cavicchi C, Malvagia S, la Marca G, Gasperini S, Donati MA, Zammarchi E, et al. Hypocitrullinemia in expanded newborn screening by LC-MS/MS is not a reliable marker for ornithine transcarbamylase deficiency. J Pharm Biomed Anal. 2009;49:1292–5.
Naylor EW, Chace DH. Automated tandem mass spectrometry for mass newborn screening for disorders in fatty acid, organic acid, and amino acid metabolism. J Child Neurol. 1999;14(Suppl 1):S4–S8.
Rashed MS. Clinical applications of tandem mass spectrometry: ten years of diagnosis and screening for inherited metabolic diseases. J Chromatogr B Biomed Sci Appl. 2001;758:27–48.
Sander J, Janzen N, Sander S, Steuerwald U, Das AM, Scholl S, et al. Neonatal screening for citrullinaemia. Eur J Pedia. 2003;162:417–20.
Mercimek-Mahmutoglu S, Moeslinger D, Häberle J, Engel K, Herle M, Strobl MW, et al. Long-term outcome of patients with argininosuccinate lyase deficiency diagnosed by newborn screening in Austria. Mol Genet Metab. 2010;100:24–28.
Häberle J, Boddaert N, Burlina A, Chakrapani A, Dixon M, Huemer M, et al. Suggested guidelines for the diagnosis and management of urea cycle disorders. Orphanet J Rare Dis. 2012;7:32.
NORD Physician Guide to the UCDs. Available at https://rarediseases.org/physician-guide/urea-cycle-disorders/. Accessed 25 Feb 2019.
Brusilow SW. Phenylacetylglutamine may replace urea as a vehicle for waste nitrogen excretion. Pedia Res. 1991;29:147–50.
Brusilow SW, Horwich AL. Urea cycle enzymes. In: Scriver CR, Beaudet AL, Sly WS, et al. editors. The metabolic and molecular basis of inherited disease, 8th ed. New York: McGraw-Hill; 2001. p. 1909–63.
Brusilow SW, Valle DL, Batshaw M. New pathways of nitrogen excretion in inborn errors of urea synthesis. Lancet. 1979;2:452–4.
McBride KL1, Miller G, Carter S, Karpen S, Goss J and Lee B. Developmental outcomes with early orthotopic liver transplantation for infants with neonatal-onset urea cycle defects and a female patient with late-onset ornithine transcarbamylase deficiency. Pediatrics. 2004;114:e523–e526.
Largillière C, Houssin D, Gottrand F, Mathey C, Checoury A, Alagille D, et al. Liver transplantation for ornithinine transcarboxylase deficiency in a girl. J Pedaitr. 1989;115:415–7.
Tuchman M. Persistent acitrullinemia after liver transplantation for carbamylphosphate synthetase deficiency. N Engl J Med. 1989;320:1498–9.
Leonard JV, McKiernan PJ. The role of liver transplantation in urea cycle disorders. Mol Genet Metab. 2004;81(Suppl 1):S74–8.
Kasahara M, Umeshita K, Inomata Y, et al. Long-term outcomes of pediatric living donor liver transplantation in Japan: an analysis of more than 2200 cases listed in the Registry of the Japanese Liver Transplantation Society. Am J Transplant. 2013;13:1830–9.
McBride KL, Miller G, Carter S, Karpen S, Goss J, Lee B. Developmental outcomes with early orthotopic liver transplantation for infants with neonatal-onset urea cycle defects and a female patient with late-onset ornithine transcarbamylase deficiency. Pediatrics. 2004;114:e523–e526.
Noujaim HM, Mayer DA, Buckles JA, Beath SV, Kelly DA, McKiernan PJ, et al. Techniques for and outcome of liver transplantation in neonates and infants weighing up to 5 kilograms. J Pedia Surg. 2002;37:159–64.
Sundaram SS, Alonso EM, Whitington PF. Liver transplantation in neonates. Liver Transpl. 2003;9:783–8.
Kasahara M, Sakamoto S, Horikawa R, Koji U, Mizuta K, Shinkai M, et al. Living donor liver transplantation for pediatric patients with metabolic disorders: the Japanese multicenter registry. Pedia Transplant. 2014;18:6–15.
Uchino T, Endo F, Matsuda I. Neurodevelopmental outcome of long-term therapy of urea cycle disorders in Japan. J Inherit Metab Dis. 1998;21(Suppl 1):151–9.
Kido J, Nakamura K, Mitsubuchi H, Ohura T, Takayanagi M, Matsuo M, et al. Long-term outcome and intervention of urea cycle disorders in Japan. J Inherit Metab Dis. 2012;35:777–85.
Jalan R, Rose C. Hypothermia in acute liver failure. Metab Brain Dis. 2004;19:215–21.
Rabinstein AA. Treatment of brain edema in acute liver failure. Curr Treat Options Neurol. 2010;12:129–41.
Whitelaw A, Bridges S, Leaf A, Evans D. Emergency treatment of neonatal hyperammonaemic coma with mild systemic hypothermia. Lancet. 2001;358:36–38.
Clinical Trials.gov. eterogous Liver Cells for Infusion in Children with Urea Cycle Disorders (SELICA III). NCT01195753. Available at: http://clinicaltrials.gov/ct2/show/NCT01195753. Accessed 25 Feb 2019.
Najimi M, Khuu DN, Lysy PA, et al. Adult-derived human liver mesenchymal-like cells as a potential progenitor reservoir of hepatocytes? Cell Transpl. 2007;16:717–28.
Brunetti-Pierri N, Clarke C, Mane V, Palmer DJ, Lanpher B, Sun Q, et al. Phenotypic correction of ornithine transcarbamylase deficiency using low dose helper-dependent adenoviral vectors. J Gene Med. 2008;10:890–6.
Moscioni D, Morizono H, McCarter RJ, Stern A, Cabrera-Luque J, Hoang A, et al. Long-term correction of ammonia metabolism and prolonged survival in ornithine transcarbamylase- deficient mice following liver-directed treatment with adeno-associated viral vectors. Mol Ther. 2006;14:25–33.
Cunningham SC, Spinoulas A, Carpenter KH, Wilcken B, Kuchel PW, Alexander IE. AAV2/8-mediated correction of OTC deficiency is robust in adult but not neonatal Spf(ash) mice. Mol Ther. 2009;17:1340–6.
Patejunas G, Lee B, Dennis JA, Healy PJ, Reeds PJ, Yu H, et al. Evaluation of gene therapy for citrullinaemia using murine and bovine models. J Inherit Metab Dis. 1998;21(Suppl 1):138–50.
Lee B, Dennis JA, Healy PJ, Mull B, Pastore L, Yu H, et al. Hepatocyte gene therapy in a large animal: a neonatal bovine model of citrullinemia. Proc Natl Acad Sci USA. 1999;96:3981–6.
Baruteau J, Perocheau DP, Hanley J, Lorvellec M, Rocha-Ferreira E, Karda R, et al. Argininosuccinic aciduria fosters neuronal nitrosative stress reversed by Asl gene transfer. Nat Commun. 2018;9:3505.
Ashley SN, Nordin JML, Buza EL, Greig JA, Wilson JM, Adeno-associated viral gene therapy corrects a mouse model of argininosuccinic aciduria. Mol Genet Metab. 2018 Nov;125:241–250.
Ye X1, Robinson MB, Batshaw ML, Furth EE, Smith I, Wilson JM. Prolonged metabolic correction in adult ornithine transcarbamylase-deficient mice with adenoviral vectors. J Biol Chem. 1996;271:3639–46.
Raper SE, Yudkoff M, Chirmule N, et al. A pilot study of in vivo liver-directed gene transfer with an adenoviral vector in partial ornithine transcarbamylase deficiency. Hum Gene Ther. 2002;13:163–75.
Wilson JM. Lessons learned from the gene therapy trial for ornithine transcarbamylase deficiency. Mol Genet Metab. 2009;96:151–7.
Clinical Trials.gov: Long Term Follow Up to Evaluate DTX301 in Adults With Late-Onset OTC Deficiency (CAPtivate) https://clinicaltrials.gov/ct2/show/NCT03636438. Accessed 16 May 2019.
WHO Technical Report Series: Protein and amino acid requirement in human nutrition. In Report of a joint WHO/FAO/UNU expert consultation Series 935; 2007.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note: Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Matsumoto, S., Häberle, J., Kido, J. et al. Urea cycle disorders—update. J Hum Genet 64, 833–847 (2019). https://doi.org/10.1038/s10038-019-0614-4
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s10038-019-0614-4
This article is cited by
-
Persistent basal ganglia involvement in aminoacylase-1 deficiency: expanding imaging findings and review of literature
Irish Journal of Medical Science (1971 -) (2024)
-
Ammonia detoxification promotes CD8+ T cell memory development by urea and citrulline cycles
Nature Immunology (2023)
-
Gas Chromatography–Mass Spectrometry Technology: Application in the Study of Inflammatory Mechanism in COVID-19 Patients
Chromatographia (2023)
-
Ammonia scavenger and glutamine synthetase inhibitors cocktail in targeting mTOR/β-catenin and MMP-14 for nitrogen homeostasis and liver cancer
Medical Oncology (2023)
-
Modelling urea cycle disorders using iPSCs
npj Regenerative Medicine (2022)