Abstract
Background
Although it is well established that obesity is a risk factor for chronic kidney disease, the impact of distinct long-term body mass index (BMI) developmental patterns on renal function in later life is poorly understood.
Methods
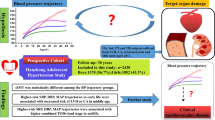
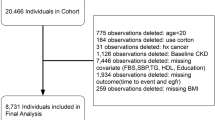
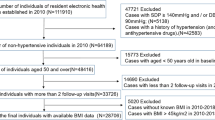
This study utilized data derived from the Hanzhong Adolescent Hypertension Cohort, a prospective cohort followed over 30 years. We used latent class growth mixture modeling method to identify the BMI trajectories of participants who had received BMI measurements at least three times from childhood (age: 6–15 years) to adulthood (age: 36–45 years). The modified Poisson regression model was used to identify potential associations between BMI trajectories and subclinical renal damage (SRD) in midlife.
Results
Within a total of 2162 individuals, we identified four distinct long-term BMI trajectories: stable normal (54.72%), moderately increasing overweight (32.42%), resolving (10.27%), and progressively increasing obese (2.59%). By the latest follow-up in 2017, a total of 257 (13.1%) individuals were diagnosed with SRD. Compared with the stable normal group, the moderately increasing overweight group and the progressively increasing obese group exhibited significantly a higher urinary albumin-to-creatinine ratio and a higher odd of existing SRD in 2017 (risk ratio [RR], 1.70 [95% confidence interval (CI), 1.33–2.19] and 4.35 [95% CI, 3.00–6.30], respectively). However, individuals who resolved their elevated BMI in early life had a similar risk for SRD as those who had never been obese or overweight (RR, 1.17 [95% CI, 0.77–1.79]).
Conclusions
Child-to-adult BMI trajectories that worsen or persist at high levels were associated with an increased risk for SRD in midlife. Maintaining a normal BMI or reversing an elevated BMI in early life may be beneficial to renal function over the long term.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Code availability
The code used in this study are available from the corresponding author, upon reasonable request.
References
Levin A, Tonelli M, Bonventre J, Coresh J, Donner J-A, Fogo AB, et al. Global kidney health 2017 and beyond: a roadmap for closing gaps in care, research, and policy. Lancet. 2017;390:1888–917.
Saran R, Robinson B, Abbott KC, Agodoa LYC, Bragg-Gresham J, Balkrishnan R, et al. US Renal Data System 2018 Annual Data Report: epidemiology of kidney disease in the United States. Am J Kidney Dis. 2019;73:A7–A8.
Webster AC, Nagler EV, Morton RL, Masson P. Chronic kidney disease. Lancet. 2017;389:1238–52.
Chen TK, Knicely DH, Grams ME. Chronic kidney disease diagnosis and management: a review. JAMA. 2019;322:1294–304.
MacLaughlin HL, Hall WL, Sanders TA, Macdougall IC. Risk for chronic kidney disease increases with obesity: Health Survey for England 2010. Public Health Nutr. 2015;18:3349–54.
Zheng W, Mu J, Chu C, Hu J, Yan Y, Ma Q, et al. Association of blood pressure trajectories in early life with subclinical renal damage in middle age. J Am Soc Nephrol. 2018;29:2835–46.
Whaley-Connell A, Sowers JR. Obesity and kidney disease: from population to basic science and the search for new therapeutic targets. Kidney Int. 2017;92:313–23.
Andres-Hernando A, Lanaspa MA, Kuwabara M, Orlicky DJ, Cicerchi C, Bales E, et al. Obesity causes renal mitochondrial dysfunction and energy imbalance and accelerates chronic kidney disease in mice. Am J Physiol Renal Physiol. 2019;317:F941–8.
Wang Y, Chen X, Klag MJ, Caballero B. Epidemic of childhood obesity: implications for kidney disease. Adv Chronic Kidney Dis. 2006;13:336–51.
Tullus K. Is there an obesity-related epidemic of CKD starting already in childhood?. Nephrol Dial Transplant. 2013;28(Suppl 4):iv114–6.
Kovesdy CP, Furth S, Zoccali C. Obesity and kidney disease: hidden consequences of the epidemic. Physiol Int. 2017;104:1–14.
Hsu C-Y, McCulloch CE, Iribarren C, Darbinian J, Go AS. Body mass index and risk for end-stage renal disease. Ann Intern Med. 2006;144:21–28.
Hsu C-Y, Iribarren C, McCulloch CE, Darbinian J, Go AS. Risk factors for end-stage renal disease: 25-year follow-up. Arch Intern Med. 2009;169:342–50.
Mu J, Zheng S, Lian Q, Liu F, Liu Z. Evolution of blood pressure from adolescents to youth in salt sensitivies: a 18-year follow-up study in Hanzhong children cohort. Nutr J. 2012;11:70.
Chu C, Dai Y, Mu J, Yang R, Wang M, Yang J. et al. Associations of risk factors in childhood with arterial stiffness 26 years later: the Hanzhong adolescent hypertension cohort. J Hypertens. 2017;35(Suppl 1):S10–5.
Liao Y-Y, Ma Q, Chu C, Wang Y, Zheng W-L, Hu J-W, et al. The predictive value of repeated blood pressure measurements in childhood for cardiovascular risk in adults: the Hanzhong Adolescent Hypertension Study. Hypertens Res. 2020:969–78.
Yuan Y, Chu C, Zheng W-L, Ma Q, Hu J-W, Wang Y. et al. Body mass index trajectories in early life is predictive of cardiometabolic risk. J Pediatr.2020;219:31–37.
Wang Y, Chen C, Yan Y, Yuan Y, Wang K, Chu C, et al. Association of uric acid in serum and urine with subclinical renal damage: Hanzhong Adolescent Hypertension Study. PLoS ONE. 2019;14:e0224680.
Leoncini G, Viazzi F, Conti N, Baratto E, Tomolillo C, Bezante GP, et al. Renal and cardiac abnormalities in primary hypertension. J Hypertens. 2009;27:1064–73.
Mulè G, Calcaterra I, Costanzo M, Geraci G, Guarino L, Foraci AC, et al. Relationship between short-term blood pressure variability and subclinical renal damage in essential hypertensive patients. J Clin Hypertens (Greenwich). 2015;17:473–80.
Ma Y-C, Zuo L, Chen J-H, Luo Q, Yu X-Q, Li Y, et al. Modified glomerular filtration rate estimating equation for Chinese patients with chronic kidney disease. J Am Soc Nephrol. 2006;17:2937–44.
Zhang L, Wang F, Wang L, Wang W, Liu B, Liu J, et al. Prevalence of chronic kidney disease in China: a cross-sectional survey. Lancet. 2012;379:815–22.
Proust-Lima C, Philipps V, Liquet B. Estimation of extended mixed models using latent classes and latent processes: the R Package lcmm. J Statistics. 2017;078:1–56.
Buscot M-J, Thomson RJ, Juonala M, Sabin MA, Burgner DP, Lehtimäki T, et al. Distinct child-to-adult body mass index trajectories are associated with different levels of adult cardiometabolic risk. Eur Heart J. 2018;39:2263–70.
Fan B, Yang Y, Dayimu A, Zhou G, Liu Y, Li S, et al. Body mass index trajectories during young adulthood and incident hypertension: a longitudinal cohort in Chinese population. J Am Heart Assoc. 2019;8:e011937.
Marioni RE, Proust-Lima C, Amieva H, Brayne C, Matthews FE, Dartigues J-F, et al. Cognitive lifestyle jointly predicts longitudinal cognitive decline and mortality risk. Eur J Epidemiol. 2014;29:211–9.
Zhang J, Yu KF. What’s the relative risk? A method of correcting the odds ratio in cohort studies of common outcomes. JAMA. 1998;280:1690–1.
Zou GY, Donner A. Extension of the modified Poisson regression model to prospective studies with correlated binary data. Stat Methods Med Res. 2013;22:661–70.
Kramer H, Luke A, Bidani A, Cao G, Cooper R, McGee D. Obesity and prevalent and incident CKD: the Hypertension Detection and Follow-Up Program. A J Kidney Dis. 2005;46:587–94.
Gelber RP, Kurth T, Kausz AT, Manson JE, Buring JE, Levey AS, et al. Association between body mass index and CKD in apparently healthy men. Am J Kidney Dis. 2005;46:871–80.
Iseki K, Ikemiya Y, Kinjo K, Inoue T, Iseki C, Takishita S. Body mass index and the risk of development of end-stage renal disease in a screened cohort. Kidney Int. 2004;65:1870–6.
Vivante A, Golan E, Tzur D, Leiba A, Tirosh A, Skorecki K, et al. Body mass index in 1.2 million adolescents and risk for end-stage renal disease. Arch Intern Med. 2012;172:1644–50.
Yun H-R, Kim H, Park JT, Chang TI, Yoo T-H, Kang S-W, et al. Obesity, metabolic abnormality, and progression of CKD. Am J Kidney Dis. 2018;72:400–10.
Chang AR, Grams ME, Ballew SH, Bilo H, Correa A, Evans M, et al. Adiposity and risk of decline in glomerular filtration rate: meta-analysis of individual participant data in a global consortium. BMJ. 2019;364:k5301.
Piché M-E, Poirier P, Lemieux I, Després J-P. Overview of epidemiology and contribution of obesity and body fat distribution to cardiovascular disease: an update. Prog Cardiovasc Dis. 2018;61:103–13.
Chughtai HL, Morgan TM, Rocco M, Stacey B, Brinkley TE, Ding J, et al. Renal sinus fat and poor blood pressure control in middle-aged and elderly individuals at risk for cardiovascular events. Hypertension. 2010;56:901–6.
Hall JE, do Carmo JM, da Silva AA, Wang Z, Hall ME. Obesity-induced hypertension: interaction of neurohumoral and renal mechanisms. Circ Res. 2015;116:6.
Robertson J, Schaufelberger M, Lindgren M, Adiels M, Schiöler L, Torén K, et al. Higher body mass index in adolescence predicts cardiomyopathy risk in midlife. Circulation. 2019;140:117–25.
Koning M, Hoekstra T, de Jong E, Visscher TLS, Seidell JC, Renders CM. Identifying developmental trajectories of body mass index in childhood using latent class growth (mixture) modelling: associations with dietary, sedentary and physical activity behaviors: a longitudinal study. BMC Public Health. 2016;16:1128.
Mattsson M, Maher GM, Boland F, Fitzgerald AP, Murray DM, Biesma R. Group-based trajectory modelling for BMI trajectories in childhood: a systematic review. Obes Rev.2019;20:998–1015.
Buscot M-J, Thomson RJ, Juonala M, Sabin MA, Burgner DP, Lehtimäki T, et al. BMI trajectories associated with resolution of elevated youth BMI and incident adult obesity. Pediatrics. 2018;141:e20172003.
Juonala M, Magnussen CG, Berenson GS, Venn A, Burns TL, Sabin MA, et al. Childhood adiposity, adult adiposity, and cardiovascular risk factors. N Engl J Med. 2011;365:1876–85.
Charakida M, Khan T, Johnson W, Finer N, Woodside J, Whincup PH, et al. Lifelong patterns of BMI and cardiovascular phenotype in individuals aged 60-64 years in the 1946 British birth cohort study: an epidemiological study. Lancet Diabetes Endocrinol. 2014;2:648–54.
Expert panel on integrated guidelines for cardiovascular health and risk reduction in children and adolescents: summary report. Pediatrics. 2011;128 Suppl 5:S213–56.
Xie W, Lundberg DJ, Collins JM, Johnston SS, Waggoner JR, Hsiao C-W, et al. Association of weight loss between early adulthood and midlife with all-cause mortality risk in the US. JAMA Netw Open. 2020;3:e2013448.
Jia G, Shu X-O, Liu Y, Li H-L, Cai H, Gao J, et al. Association of adult weight gain with major health outcomes among middle-aged Chinese persons with low body weight in early adulthood. JAMA Netw Open. 2019;2:e1917371.
Jezewska-Zychowicz M, Gębski J, Plichta M, Guzek D, Kosicka-Gębska M. Diet-related factors, physical activity, and weight status in Polish adults. Nutrients. 2019;11:2532.
Mushtaq MU, Gull S, Mushtaq K, Shahid U, Shad MA, Akram J. Dietary behaviors, physical activity and sedentary lifestyle associated with overweight and obesity, and their socio-demographic correlates, among Pakistani primary school children. Int J Behav Nutr Phys Act. 2011;8:130.
Zheng W, McLerran DF, Rolland B, Zhang X, Inoue M, Matsuo K, et al. Association between body-mass index and risk of death in more than 1 million Asians. N Engl J Med. 2011;364:719–29.
Wang C, He Y, Xu P, Yang Y, Saito K, Xia Y, et al. TAp63 contributes to sexual dimorphism in POMC neuron functions and energy homeostasis. Nat Commun. 2018;9:1544.
Formanek P, Salisbury-Afshar E, Afshar M. Helping patients with ESRD and earlier stages of CKD to quit smoking. Am J Kidney Dis. 2018;72:255–66.
Cosola C, Sabatino A, di Bari I, Fiaccadori E, Gesualdo L. Nutrients, nutraceuticals, and xenobiotics affecting renal health. Nutrients. 2018;10:808.
Locatelli F, Pozzoni P, Del Vecchio L. Renal manifestations in the metabolic syndrome. J Am Soc Nephrol. 2006;17:S81–5.
Afshinnia F, Pennathur S. Lipids and cardiovascular risk with CKD. Clin J Am Soc Nephrol. 2020;15:5–7.
Chen J, Muntner P, Hamm LL, Jones DW, Batuman V, Fonseca V, et al. The metabolic syndrome and chronic kidney disease in U.S. adults. Ann Intern Med. 2004;140:167–74.
Sharaf El Din UAA, Salem MM, Abdulazim DO. Uric acid in the pathogenesis of metabolic, renal, and cardiovascular diseases: a review. J Adv Res. 2017;8:537–48.
Benjamin EJ, Virani SS, Callaway CW, Chamberlain AM, Chang AR, Cheng S, et al. Heart disease and stroke statistics-2018 update: a report from the American Heart Association. Circulation. 2018;137:e67–e492.
Hall JE, do Carmo JM, da Silva AA, Wang Z, Hall ME. Obesity, kidney dysfunction and hypertension: mechanistic links. Nat Rev Nephrol. 2019;15:367–85.
Chen CM. Overview of obesity in Mainland China. Obes Rev. 2008;9(Suppl 1):14–21.
Acknowledgements
This work was supported by the National Natural Science Foundation of China No. 81870319 and No. 81700368 (CC), National Key R&D Program of China (2016YFC1300100); Grant 2017YFC1307604 from the Major Chronic Non-communicable Disease Prevention and Control Research Key Project of the Ministry of Science and Technology of the People’s Republic of China; Grant 2017ZDXM-SF-107 from the Key Research Project of Shaanxi Province, and Clinical Research Award of the First Affiliated Hospital of Xi’an Jiaoton University, China (No.XJTU1AF-CRF-2019-004). The authors thank Ruihai Yang, Jun Yang, Yong Ren, Bo Yan, and Ying Deng for assistance with data collection, and Fangyao Chen for statistical advice.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Yan, Y., Zheng, W., Ma, Q. et al. Child-to-adult body mass index trajectories and the risk of subclinical renal damage in middle age. Int J Obes 45, 1095–1104 (2021). https://doi.org/10.1038/s41366-021-00779-5
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-021-00779-5
This article is cited by
-
Alterations of DNA methylation profile in peripheral blood of children with simple obesity
Health Information Science and Systems (2024)
-
Childhood modifiable risk factors and later life chronic kidney disease: a systematic review
BMC Nephrology (2023)
-
Children who appeared or remained overweight or obese predict a higher follow-up blood pressure and higher risk of hypertension: a 6-year longitudinal study in Yantai, China
Hypertension Research (2023)
-
Relation between obesity-related comorbidities and kidney function estimation in children
Pediatric Nephrology (2023)
-
Triglyceride-glucose index trajectory and arterial stiffness: results from Hanzhong Adolescent Hypertension Cohort Study
Cardiovascular Diabetology (2022)