Abstract
Background
Physical activity (PA) and discretionary screen time (DST; television and computer use during leisure) are both associated with obesity risk, but little longitudinal evidence exists on their combined influence. This study examined the independent and joint associations of changes in PA and DST with incident obesity, body mass index (BMI) and waist circumference (WC).
Methods
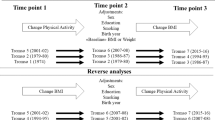
We analysed the data of individuals aged 40–69 years from the UK Biobank, a large-scale, population-based prospective cohort study. PA was measured using the International Physical Activity Questionnaire and DST was defined as the total of daily TV viewing and non-occupational computer use. Changes in PA and DST over time were defined using departure from sex-specific baseline tertiles and categorised as worsened (PA decreased/DST increased), maintained, and improved (PA increased/DST decreased). We then used each exposure change to define a joint PA-DST change variable with nine mutually exclusive groups. We used multivariable adjusted mixed-effects linear and Poisson models to examine the independent and joint associations between PA and DST changes with BMI and WC and incident obesity, respectively. Development of a BMI ≥ 30 kg/m2 was defined as incident obesity.
Results
Among 30,735 participants, 1,628 (5.3%) developed incident obesity over a mean follow-up of 6.9 (2.2) years. In the independent association analyses, improving PA (Incident Rate Ratio (IRR) 0.46 (0.38–0.56)) was associated with a lower risk of incident obesity than maintaining PA, maintaining DST, or improving DST. Compared to the referent group (both PA and DST worsened), all other combinations of PA and DST changes were associated with lower incident obesity risk in the joint association analyses. We observed substantial beneficial associations in the improved PA groups, regardless of DST change [e.g., DST worsened (IRR 0.31 (0.21–0.44)), maintained (IRR 0.34 (0.25–0.46)), or improved (IRR 0.35 (0.22–0.56)]. The most pronounced decline in BMI and WC was observed when PA was maintained or improved and DST was maintained.
Conclusion
We found that improved PA had the most pronounced beneficial associations with incident obesity, irrespective of DST changes. Improvements in PA or DST mutually attenuated the deleterious effects of the other behaviour’s deterioration.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
Dai H, Alsalhe TA, Chalghaf N, Riccò M, Bragazzi NL, Wu J. The global burden of disease attributable to high body mass index in 195 countries and territories, 1990–2017: An analysis of the Global Burden of Disease Study. PLoS Med. 2020;17:e1003198.
Bentham J, Di Cesare M, BIlano V, Boddy L. Worldwide trends in children’s and adolescents’ body mass index, underweight and obesity, in comparison with adults, from 1975 to 2016: a pooled analysis of 2,416 population-based measurement studies with 128.9 million participants. Lancet. 2017.
GBD Obesity Collaborators. Health effects of overweight and obesity in 195 countries over 25 years. New England J Med. 2017;377:13–27.
Dwivedi AK, Dubey P, Cistola DP, Reddy SY. Association between obesity and cardiovascular outcomes: updated evidence from meta-analysis studies. Curr Cardiol Rep. 2020;22:1–19.
Riaz H, Khan MS, Siddiqi TJ, Usman MS, Shah N, Goyal A, et al. Association between obesity and cardiovascular outcomes: a systematic review and meta-analysis of Mendelian randomization studies. JAMA Network Open. 2018;1:e183788–e.
Wade KH, Carslake D, Sattar N, Davey Smith G, Timpson NJ. BMI and mortality in UK Biobank: revised estimates using mendelian randomization. Obesity. 2018;26:1796–806.
Friedenreich CM, Ryder‐Burbidge C, McNeil J. Physical activity, obesity and sedentary behavior in cancer etiology: epidemiologic evidence and biologic mechanisms. Mol Oncol. 2021;15:790–800.
Lam T, Ho D. Worldwide trends in body-mass index, underweight, overweight. The Lancet. 2017;390:2627–42.
Tremblay MS, Aubert S, Barnes JD, Saunders TJ, Carson V, Latimer-Cheung AE, et al. Sedentary behavior research network (SBRN)–terminology consensus project process and outcome. Int J Behav Nutr Phys Activity. 2017;14:1–17.
Spanier PA, Marshall SJ, Faulkner GE. Tackling the obesity pandemic. Can J Public Health. 2006;97:255–7.
Bell JA, Hamer M, Batty GD, Singh-Manoux A, Sabia S, Kivimaki M. Combined effect of physical activity and leisure time sitting on long-term risk of incident obesity and metabolic risk factor clustering. Diabetologia. 2014;57:2048–56.
Shibata A, Oka K, Sugiyama T, Salmon J, Dunstan DW, Owen N. Physical activity, television viewing time, and 12-year changes in waist circumference. Med Sci Sports Exercise. 2016;48:633.
Chastin SF, De Craemer M, De Cocker K, Powell L, Van Cauwenberg J, Dall P, et al. How does light-intensity physical activity associate with adult cardiometabolic health and mortality? Systematic review with meta-analysis of experimental and observational studies. Br J Sports Med. 2019;53:370–6.
Martins C, Morgan L, Truby H. A review of the effects of exercise on appetite regulation: an obesity perspective. Int J Obesity. 2008;32:1337–47.
Biddle SJ, Garcia EB, Pedisic Z, Bennie J, Vergeer I, Wiesner G. Screen time, other sedentary behaviours, and obesity risk in adults: a review of reviews. Curr Obesity Rep. 2017;6:134–47.
Campbell SD, Brosnan BJ, Chu AK, Skeaff CM, Rehrer NJ, Perry TL, et al. Sedentary behavior and body weight and composition in adults: a systematic review and meta-analysis of prospective studies. Sports Med. 2018;48:585–95.
British Heart Foundation. Physical inactivity and sedentary behaviour report. British Heart Foundation; 2017.
Celis-Morales CA, Lyall DM, Steell L, Gray SR, Iliodromiti S, Anderson J, et al. Associations of discretionary screen time with mortality, cardiovascular disease and cancer are attenuated by strength, fitness and physical activity: findings from the UK Biobank study. BMC Medicine. 2018;16:1–14.
Bauman AE, Petersen CB, Blond K, Rangul V, Hardy LL. The descriptive epidemiology of sedentary behaviour. Sedentary behaviour epidemiology: Springer; 2018. p. 73–106.
Shields M, Tremblay MS. Sedentary behaviour and obesity. Health Reports. 2008;19:19.
Duncan MJ, Vandelanotte C, Caperchione C, Hanley C, Mummery WK. Temporal trends in and relationships between screen time, physical activity, overweight and obesity. BMC Public Health. 2012;12:1–9.
DiPietro L, Al-Ansari SS, Biddle SJ, Borodulin K, Bull FC, Buman MP, et al. Advancing the global physical activity agenda: recommendations for future research by the 2020 WHO physical activity and sedentary behavior guidelines development group. Int J Behav Nutr Phys Activity. 2020;17:1–11.
Knaeps S, Bourgois JG, Charlier R, Mertens E, Lefevre J, Wijndaele K. Ten-year change in sedentary behaviour, moderate-to-vigorous physical activity, cardiorespiratory fitness and cardiometabolic risk: independent associations and mediation analysis. Br J Sports Med. 2018;52:1063–8.
Maher CA, Mire E, Harrington DM, Staiano AE, Katzmarzyk PT. The independent and combined associations of physical activity and sedentary behavior with obesity in adults: NHANES 2003‐06. Obesity. 2013;21:E730–E7.
Liao Y, Harada K, Shibata A, Ishii K, Oka K, Nakamura Y, et al. Joint associations of physical activity and screen time with overweight among Japanese adults. Int J Behav Nutr Phys Activity. 2011;8:1–5.
Thakkar N, Jamnik V, Ardern CI. Cross-associations between physical activity and sedentary time on metabolic health: a comparative assessment using self-reported and objectively measured activity. J Public Health. 2018;40:e464–e73.
Cleland VJ, Patterson K, Breslin M, Schmidt MD, Dwyer T, Venn AJ. Longitudinal associations between TV viewing and BMI not explained by the ‘mindless eating’ or ‘physical activity displacement’ hypotheses among adults. BMC Public Health. 2018;18:1–12.
Piirtola M, Kaprio J, Waller K, Heikkilä K, Koskenvuo M, Svedberg P, et al. Leisure-time physical inactivity and association with body mass index: a Finnish Twin Study with a 35-year follow-up. Int J Epidemiol. 2017;46:116–27.
Leskinen T, Stenholm S, Pulakka A, Pentti J, Kivimäki M, Vahtera J. Comparison between recent and long-term physical activity levels as predictors of cardiometabolic risk: a cohort study. BMJ Open. 2020;10.
Sudlow C, Gallacher J, Allen N, Beral V, Burton P, Danesh J, et al. UK biobank: an open access resource for identifying the causes of a wide range of complex diseases of middle and old age. PLoS Med. 2015;12:e1001779.
Collins R. What makes UK Biobank special? Lancet (London, England). 2012;379:1173–4.
Allen NE, Sudlow C, Peakman T, Collins R. UK BioBank data: come and get it. Sci Transl Med. 2014;6:224ed4.
Carreras-Torres R, Johansson M, Haycock PC, Relton CL, Smith GD, Brennan P, et al. Role of obesity in smoking behaviour: Mendelian randomisation study in UK Biobank. Bmj. 2018;361.
World Health Organization. Body Mass Index (BMI) classifications 2021. Available from: https://www.euro.who.int/en/health-topics/disease-prevention/nutrition/a-healthy-lifestyle/body-mass-index-bmi.
Craig CL, Marshall AL, Sjöström M, Bauman AE, Booth ML, Ainsworth BE, et al. International physical activity questionnaire: 12-country reliability and validity. Med Sci Sports Exercise. 2003;35:1381–95.
The IPAQ Group. IPAQ-scoring protocol-International Physical Activity Questionnaire. Available from: https://sites.google.com/site/theipaq/scoring-protocol.
Townsend P, Phillimore P, Beattie A. Health and deprivation: inequality and the North: Routledge; 1988.
Su C, Jia X, Wang Z, Wang H, Ouyang Y, Zhang B. Longitudinal association of leisure time physical activity and sedentary behaviors with body weight among Chinese adults from China Health and Nutrition Survey 2004–2011. Eur J Clin Nutr. 2017;71:383–8.
Cleven L, Krell-Roesch J, Nigg CR, Woll A. The association between physical activity with incident obesity, coronary heart disease, diabetes and hypertension in adults: a systematic review of longitudinal studies published after 2012. BMC Public Health. 2020;20:1–15.
Leskinen T, Stenholm S, Heinonen OJ, Pulakka A, Aalto V, Kivimäki M, et al. Change in physical activity and accumulation of cardiometabolic risk factors. Prev Med. 2018;112:31–7.
Wanner M, Martin BW, Autenrieth CS, Schaffner E, Meier F, Brombach C, et al. Associations between domains of physical activity, sitting time, and different measures of overweight and obesity. Prev Med Rep. 2016;3:177–84.
Proper KI, Singh AS, Van Mechelen W, Chinapaw MJ. Sedentary behaviors and health outcomes among adults: a systematic review of prospective studies. Am J Prev Med. 2011;40:174–82.
Williams DM, Raynor HA, Ciccolo JT. A review of TV viewing and its association with health outcomes in adults. Am J Lifestyle Med. 2008;2:250–9.
Bayon V, Leger D, Gomez-Merino D, Vecchierini M-F, Chennaoui M. Sleep debt and obesity. Ann Med. 2014;46:264–72.
Cristi-Montero C, Steell L, Petermann F, Garrido-Méndez A, Díaz-Martínez X, Salas-Bravo C, et al. Joint effect of physical activity and sedentary behaviour on cardiovascular risk factors in Chilean adults. J Public Health. 2018;40:485–92.
Sugiyama T, Healy GN, Dunstan DW, Salmon J, Owen N. Joint associations of multiple leisure-time sedentary behaviours and physical activity with obesity in Australian adults. Int J Behav Nutr Phys Activity. 2008;5:1–6.
Heshmat R, Qorbani M, Shahr Babaki AE, Djalalinia S, Ataei-Jafari A, Motlagh ME, et al. Joint association of screen time and physical activity with cardiometabolic risk factors in a national sample of Iranian adolescents: the CASPIANIII study. PLoS ONE. 2016;11:e0154502.
Loprinzi PD, Lee H, Cardinal BJ. Daily movement patterns and biological markers among adults in the United States. Prev Med. 2014;60:128–30.
Bakrania K, Edwardson CL, Bodicoat DH, Esliger DW, Gill JM, Kazi A, et al. Associations of mutually exclusive categories of physical activity and sedentary time with markers of cardiometabolic health in English adults: a cross-sectional analysis of the Health Survey for England. BMC Public Health. 2015;16:1–10.
Ekelund U, Steene-Johannessen J, Brown WJ, Fagerland MW, Owen N, Powell KE, et al. Does physical activity attenuate, or even eliminate, the detrimental association of sitting time with mortality? A harmonised meta-analysis of data from more than 1 million men and women. The Lancet. 2016;388:1302–10.
Marques A, Santos DA, Peralta M, Sardinha LB, Valeiro MG. Regular physical activity eliminates the harmful association of television watching with multimorbidity. A cross-sectional study from the European Social Survey. Prev Med. 2018;109:28–33.
Whitaker KM, Pettee Gabriel K, Buman MP, Pereira MA, Jacobs DR Jr, Reis JP, et al. Associations of accelerometer‐measured sedentary time and physical activity with prospectively assessed cardiometabolic risk factors: the CARDIA study. J Am Heart Assoc. 2019;8:e010212.
Lee YY, Kamarudin KS, Muda WAMW. Associations between self-reported and objectively measured physical activity and overweight/obesity among adults in Kota Bharu and Penang, Malaysia. BMC Public Health. 2019;19:1–12.
da Silva BGC, da Silva ICM, Ekelund U, Brage S, Ong KK, Rolfe EDL, et al. Associations of physical activity and sedentary time with body composition in Brazilian young adults. Sci Rep. 2019;9:1–10.
Warren JM, Ekelund U, Besson H, Mezzani A, Geladas N, Vanhees L. Assessment of physical activity–a review of methodologies with reference to epidemiological research: a report of the exercise physiology section of the European Association of Cardiovascular Prevention and Rehabilitation. Eur J Prev Cardiol. 2010;17:127–39.
Prince SA, Adamo KB, Hamel ME, Hardt J, Gorber SC, Tremblay M. A comparison of direct versus self-report measures for assessing physical activity in adults: a systematic review. Int J Behav Nutr Phys Activity. 2008;5:1–24.
Prince SA, Cardilli L, Reed JL, Saunders TJ, Kite C, Douillette K, et al. A comparison of self-reported and device measured sedentary behaviour in adults: a systematic review and meta-analysis. Int J Behav Nutr Phys Activity. 2020;17:1–17.
Fry A, Littlejohns TJ, Sudlow C, Doherty N, Adamska L, Sprosen T, et al. Comparison of sociodemographic and health-related characteristics of UK Biobank participants with those of the general population. Am J Epidemiol. 2017;186:1026–34.
Stamatakis E, Owen KB, Shepherd L, Drayton B, Hamer M, Bauman AE. Is Cohort Representativeness Passé? Poststratified associations of lifestyle risk factors with mortality in the UK Biobank. Epidemiology (Cambridge, Mass). 2021;32:179.
Acknowledgements
This research has been conducted using the UK Biobank Resource under Application Number 25813. The authors would like to thank the participants of the UK Biobank study.
Funding
This work was supported by a National Health and Medical Research Council Investigator Grant (APP1194510; ES).
Author information
Authors and Affiliations
Contributions
ES and EIE conceptualised the study. BPC and SP carried out the analysis. SP prepared the original manuscript. ES, EIE, MA and BPC contributed to the composition and editing of the final manuscript. All authors have read and agreed to the final version of the manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Paudel, S., del Pozo Cruz, B., Inan-Eroglu, E. et al. Associations of changes in physical activity and discretionary screen time with incident obesity and adiposity changes: longitudinal findings from the UK Biobank. Int J Obes 46, 597–604 (2022). https://doi.org/10.1038/s41366-021-01033-8
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41366-021-01033-8