Abstract
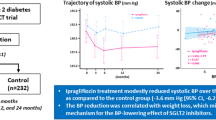
High blood pressure variability (BPV) has been associated with increased cardiovascular (CV) risk. The effect of dietary salt and renin–angiotensin–aldosterone system (RAAS) activity on short-term BPV in type 2 diabetes mellitus (T2DM) is not well characterised. We aimed to determine the effect of dietary salt (sodium chloride, NaCl) supplementation on 24-h mean arterial BPV (24hBPV) during angiotensin II receptor blocker (telmisartan) use and to evaluate the effects of age, sex, plasma renin activity (PRA) and serum aldosterone on 24hBPV. In a randomised, double-blind, crossover study, patients with T2DM (n = 28), treated with telmisartan received NaCl (100 mmol/24 h) or placebo capsules during 2 weeks of telmisartan. Following a 6-week washout, the protocol was repeated in reverse. 24hBPV was evaluated as a co-efficient of variation [CV (%) = mean/standard deviation] × 100). Twenty-four hour urinary sodium excretion, ambulatory BP and biochemical tests were performed at each phase. Results were analysed using a linear mixed model to generate predicted values for 24hBPV. Predicted 24hBPV was higher with telmisartan vs baseline (p = 0.01), with a trend towards reduced 24hBPV with salt (p = 0.052). Predicted 24hBPV was lower in females (p = 0.017), increasing age (p = 0.001) and increasing PRA (p = 0.011). In patients with T2DM, predicted 24hBPV increased from baseline with telmisartan, but there was no additional increase in predicted 24hBPV with salt supplementation. This suggests that in the short-term, salt supplementation has no apparent deleterious effects on 24hBPV. Long-term studies are required to evaluate the effect of 24hBPV on CV outcomes in patients with T2DM.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Garcia MJ, McNamara PM, Gordon T, Kannell WB. Morbidity and mortality in diabetics in the framingham population: sixteen year follow-up study. Diabetes. 1974;23:105–11.
Parati G, Ochoa JE, Salvi P, Lombardi C, Bilo G. Prognostic value of blood pressure variability and average blood pressure levels in patients with hypertension and diabetes. Diabetes Care. 2013;36 Suppl. 2:S312–24.
Rothwell PM, Howard SC, Dolan E, O’Brien E, Dobson JE, Dahlöf B, et al. Prognostic significance of visit-to-visit variability, maximum systolic blood pressure, and episodic hypertension. Lancet. 2010;375:895–905.
Poortvliet RK, Ford I, Lloyd SM, Sattar N, Mooijaart SP, de Craen AJ, et al. Blood pressure variability and cardiovascular risk in the PROspective Study of Pravastatin in the Elderly at Risk (PROSPER). PLoS ONE. 2012;7:e52438.
Okada H, Fukui M, Tanaka M, Matsumoto S, Mineoka Y, Nakanishi N, et al. Visit-to-visit blood pressure variability is a novel risk factor for the development and progression of diabetic nephropathy in patients with type 2 diabetes. Diabetes Care. 2013;36:1908–12.
Sohn M-W, Epstein N, Huang ES, Huo Z, Emanuele N, Stukenborg G, et al. Visit-to-visit systolic blood pressure variability and microvascular complications among patients with diabetes. J Diabetes Complicat. 2017;31:195–201.
Stevens SL, Wood S, Koshiaris C, Law K, Glasziou P, Stevens RJ, et al. Blood pressure variability and cardiovascular disease: systematic review and meta-analysis. Br Med J. 2016;354:i4098.
Veerman DP, Imholz BP, Wieling W, Karemaker JM, van Montfrans GA. Effects of aging on blood pressure variability in resting conditions. Hypertension. 1994;24:120–30.
Thayer JF, Sollers JJ, Friedman BH, Koenig J. Gender differences in the relationship between resting heart rate variability and 24-hour blood pressure variability. Blood Press. 2016;25:58–62.
Webb AJ, Fischer U, Mehta Z, Rothwell PM. Effects of antihypertensive-drug class on interindividual variation in blood pressure and risk of stroke: a systematic review and meta-analysis. Lancet. 2010;375:906–15.
Chen AX, Jerums G, Baqar S, Lambert E, Somarajah G, Thomas G, et al. Short-term dietary salt supplementation blunts telmisartan induced increases in plasma renin activity in hypertensive patients with type 2 diabetes mellitus. Clin Sci. 2015;129:415–22.
Ekinci EI, Thomas G, Thomas D, Johnson C, MacIsaac RJ, Houlihan CA, et al. Effects of salt supplementation on the albuminuric response to telmisartan with or without hydrochlorothiazide therapy in hypertensive patients with type 2 diabetes are modulated by habitual dietary salt intake. Diabetes Care. 2009;32:1398–403.
Ekinci EI, Thomas G, MacIsaac RJ, Johnson C, Houlihan C, Panagiotopoulos S, et al. Salt supplementation blunts the blood pressure response to telmisartan with or without hydrochlorothiazide in hypertensive patients with type 2 diabetes. Diabetologia. 2010;53:1295–303.
Houlihan CA, Allen TJ, Baxter AL, Panangiotopoulos S, Casley DJ, Cooper ME, et al. A low-sodium diet potentiates the effects of losartan in type 2 diabetes. Diabetes Care. 2002;25:663–71.
Parati G, Ochoa JE, Lombardi C, Bilo G. Assessment and management of blood-pressure variability. Nat Rev Cardiol. 2013;10:143–55.
Mallinckrod CH, Lane PW, Schnell D, Peng Y, Mancuso JP. Recommendations for the primary analysis of continuous endpoints in longitudinal clinical trials. Drug Inf J. 2008;42:303–19.
Williams R. Using the margins command to estimate and interpret adjusted predictions and marginal effects. Stata J. 2012;12:308.
Burnier M, Brunner H. Angiotensin II receptor antagonists. Lancet. 2000;355:637–45.
Mancia G. Blood pressure variability: mechanisms and clinical significance. J Cardiovasc Pharmacol. 1990;16:S1–6.
Zhang Y, Agnoletti D, Safar ME, Blacher J. Effect of antihypertensive agents on blood pressure variability. Hypertension. 2011;58:155–60.
Omboni S, Kario K, Bakris G, Parati G. Effect of antihypertensive treatment on 24-h blood pressure variability: pooled individual data analysis of ambulatory blood pressure monitoring studies based on olmesartan mono or combination treatment. J Hypertens. 2018;36:720–33.
Ushigome E, Fukui M, Hamaguchi M, Tanaka T, Atsuta H, Mogami S, et al. Factors affecting variability in home blood pressure in patients with type 2 diabetes: post hoc analysis of a cross-sectional multicenter study. J Hum Hypertens. 2014;28:594–9.
Vogiatzakis N, Tsioufis C, Georgiopoulos G, Thomopoulos C, Dimitriadis K, Kasiakogias A, et al. Effect of renal sympathetic denervation on short-term blood pressure variability in resistant hypertension: a meta-analysis. J Hypertens. 2017;35:1750–7.
Mente A, O’Donnell M, Rangarajan S, McQueen M, Dagenais G, Wielgosz A, et al. Urinary sodium excretion, blood pressure, cardiovascular disease, and mortality: a community-level prospective epidemiological cohort study. Lancet. 2018;392:496–506.
Brian MS, Dalpiaz A, Matthews EL, Lennon-Edwards S, Edwards DG, Farquhar WB. Dietary sodium and nocturnal blood pressure dipping in normotensive men and women. J Hum Hypertens. 2017;31:145–50.
Iuchi H, Sakamoto M, Suzuki H, Kayama Y, Ohashi K, Hayashi T, et al. Effect of one-week salt restriction on blood pressure variability in hypertensive patients with type 2 diabetes. PloS ONE. 2016;11:e0144921.
Grassi G, Dell’Oro R, Seravalle G, Foglia G, Trevano FQ, Mancia G. Short-and long-term neuroadrenergic effects of moderate dietary sodium restriction in essential hypertension. Circulation. 2002;106:1957–61.
Hall JE. Control of sodium excretion by angiotensin II: intrarenal mechanisms and blood pressure regulation. Am J Physiol. 1986;250:R960–72.
Ozkayar N, Dede F, Akyel F, Yildirim T, Ateş I, Turhan T, et al. Relationship between blood pressure variability and renal activity of the renin–angiotensin system. J Hum Hypertens. 2016;30:297.
Chau NP, Chanudet X, Larroque P. Inverse relationship between upright plasma renin activity and twenty-four hour blood pressure variability in borderline hypertension. J Hypertens. 1990;8:913–8.
Campbell DJ, Nussberger J, Stowasser M, Danser AHJ, Morganti A, Frandsen E, et al. Activity assays and immunoassays for plasma renin and prorenin: information provided and precautions necessary for accurate measurement. Clin Chem. 2009;55:867–77.
Deppe S, Böger RH, Weiss J, Benndorf RA. Telmisartan: a review of its pharmacodynamic and pharmacokinetic properties. Exp Opi Drug Metab Toxicol. 2010;6:863–71.
Imai Y, Aihara A, Ohkubo T, Nagai K, Tsuji I, Minami N, et al. Factors that affect blood pressure variability. Am J Hypertens. 1997;10:1281–9.
Migneco A, Ojetti V, Covino M, Mettimano M, Montebelli MR, Leone A, et al. Increased blood pressure variability in menopause. Eur Rev Med Pharm Sci. 2008;12:89.
Holbrook J, Patterson K, Bodner J, Douglas L, Veillon C, Kelsay J, et al. Sodium and potassium intake and balance in adults consuming self-selected diets. Am J Clin Nutr. 1984;40:786–93.
di Rienzo M, Grassi G, Pedotti A, Mancia G. Continuous vs intermittent blood pressure measurements in estimating 24-hour average blood pressure. Hypertension. 1983;5:264–9.
Acknowledgements
The authors would like to acknowledge the support of Department 310 of Endocrinology, Austin Health, University of Melbourne in undertaking this study.
Funding
This work was supported by an NHMRC Postgraduate Research Scholarship (grant number APP466611 to EIE), NHRMC Early Career Fellowship (grant number APP1054312 to EIE) and Heart Foundation Scholarship (grant number 100287 to SB).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Chen, A.X., Moran, J.L., Libianto, R. et al. Effect of angiotensin II receptor blocker and salt supplementation on short-term blood pressure variability in type 2 diabetes. J Hum Hypertens 34, 143–150 (2020). https://doi.org/10.1038/s41371-019-0238-3
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41371-019-0238-3