Abstract
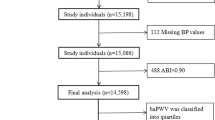
Little information is available on the association between brachial–ankle pulse wave velocity (baPWV) and the risk of stroke in Chinese H-type hypertension patients. Therefore, our study aimed to assess this association between baseline baPWV and short-term risk of first stroke and to propose a cutoff value of baPWV that could predict near cerebrovascular events. A total of 9787 hypertension patients without preexisting stroke who underwent baPWV measurement were included. The primary end points were first symptomatic stroke. Secondary end points were first ischemic stroke and first hemorrhagic stroke. During a median follow-up of 20.8 months, there was a total of 138 first strokes including 123 first ischemic strokes and 15 first hemorrhagic strokes. When baPWV was categorized in quartiles, the higher risks of first stroke (HR = 1.52; 95% CI: 1.05–2.21) and first ischemic stroke (HR = 1.53; 95% CI: 1.03–2.26) were found in participants in quartile 4 (≥21.31 m/s), compared with those in quartile 1–3 (<21.31 m/s). In receiver operating characteristic curve analysis, the best cutoff value of baPWV that could predict first stroke was 21.43 m/s. Higher baPWV (≥21.43 m/s) was significantly associated with increased risk of first stroke (HR = 1.60; 95% CI: 1.10–2.32) and first ischemic stroke (HR = 1.60; 95% CI: 1.08–2.37). In conclusion, higher baPWV levels were associated with an increased risk of first stroke among Chinese H-type hypertensive patients. In addition, a cutoff value of 21.43 m/s of baPWV was proposed that could predict the next two years’ cerebrovascular events.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 digital issues and online access to articles
$119.00 per year
only $9.92 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
Wang W, Jiang B, Sun H, Ru X, Sun D, Wang L, et al. Prevalence, incidence, and mortality of stroke in China: results from a nationwide population-based survey of 480 687 adults. Circulation 2017;135:759–71.
GBD SC. Global, regional, and national burden of stroke, 1990-2016: a systematic analysis for the Global Burden of Disease Study 2016. Lancet Neurol 2019;18:439–58.
Meschia JF, Bushnell C, Boden-Albala B, Braun LT, Bravata DM, Chaturvedi S, et al. Guidelines for the primary prevention of stroke: a statement for healthcare professionals from the American Heart Association/American Stroke Association. Stroke 2014;45:3754–832.
Huo Y, Li J, Qin X, Huang Y, Wang X, Gottesman RF, et al. Efficacy of folic acid therapy in primary prevention of stroke among adults with hypertension in China: the CSPPT randomized clinical trial. JAMA 2015;313:1325–35.
Liu LS. 2010 Chinese guidelines for the management of hypertension. Zhonghua Xin Xue Guan Bing Za Zhi 2011;39:579–615.
Towfighi A, Markovic D, Ovbiagele B. Pronounced association of elevated serum homocysteine with stroke in subgroups of individuals: a nationwide study. J Neurol Sci 2010;298:153–7.
Li J, Jiang S, Zhang Y, Tang G, Wang Y, Mao G, et al. H-type hypertension and risk of stroke in chinese adults: a prospective, nested case-control study. J Transl Int Med 2015;3:171–8.
Ohkuma T, Ninomiya T, Tomiyama H, Kario K, Hoshide S, Kita Y, et al. Brachial-ankle pulse wave velocity and the risk prediction of cardiovascular disease: an individual participant data meta-analysis. Hypertension 2017;69:1045–52.
Kim HL, Lim WH, Seo JB, Kim SH, Zo ZH, Kim MA. Prediction of cardiovascular events using brachial-ankle pulse wave velocity in hypertensive patients. J Clin Hypertens (Greenwich). 2020;22:1659–65.
Mancia G, Fagard R, Narkiewicz K, Redon J, Zanchetti A, Bohm M, et al. ESH/ESC Guidelines for the management of arterial hypertension: the Task Force for the management of arterial hypertension of the European Society of Hypertension (ESH) and of the European Society of Cardiology (ESC). J Hypertens. 2013;31:1281–357.
Tomiyama H, Matsumoto C, Shiina K, Yamashina A, Brachial-Ankle PWV. Current status and future directions as a useful marker in the management of cardiovascular disease and/or cardiovascular risk factors. J Atheroscler Thromb 2016;23:128–46.
Kim J, Song TJ, Kim EH, Lee KJ, Lee HS, Nam CM, et al. Brachial-ankle pulse wave velocity for predicting functional outcome in acute stroke. Stroke 2014;45:2305–10.
Song Y, Xu B, Xu R, Tung R, Frank E, Tromble W, et al. Independent and joint effect of brachial-ankle pulse wave velocity and blood pressure control on incident stroke in hypertensive adults. Hypertension 2016;68:46–53.
Kim YB, Park K, Chung P, Kim JM, Moon HS, Youn YC. Brachial-ankle pulse wave velocity is associated with both acute and chronic cerebral small vessel disease. Atherosclerosis 2016;245:54–59.
Kawai T, Ohishi M, Onishi M, Ito N, Takeya Y, Oguro R, et al. Prognostic impact of regional arterial stiffness in hypertensive patients. Heart Vessels 2015;30:338–46.
Munakata M, Konno S, Miura Y, Yoshinaga K. Prognostic significance of the brachial-ankle pulse wave velocity in patients with essential hypertension: final results of the J-TOPP study. Hypertens Res 2012;35:839–42.
Chen SC, Chang JM, Liu WC, Tsai YC, Tsai JC, Hsu PC, et al. Brachial-ankle pulse wave velocity and rate of renal function decline and mortality in chronic kidney disease. Clin J Am Soc Nephrol 2011;6:724–32.
Yamashina A, Tomiyama H, Takeda K, Tsuda H, Arai T, Hirose K, et al. Validity, reproducibility, and clinical significance of noninvasive brachial-ankle pulse wave velocity measurement. Hypertens Res 2002;25:359–64.
Liu Z, Yang Y, Zhang Y, et al. Association of brachial-ankle pulse wave velocity and carotid plaque in Chinese hypertensive adults: effect modification by age. Hypertension Res 2020;43:808–16.
Sun P, Liu L, Liu C, Zhang Y, Yang Y, Qin X, et al. Carotid intima-media thickness and the risk of first stroke in patients with hypertension. Stroke 2020;51:379–86.
Vanderweele TJ, Ding P. Sensitivity analysis in observational research: introducing the E-value. Ann Intern Med 2017;167:268–74.
Ohkuma T, Ninomiya T, Tomiyama H, Kario K, Hoshide S, Kita Y, et al. Brachial-ankle pulse wave velocity and the risk prediction of cardiovascular disease. Hypertension 2017;69:1045–52.
Li T, Wu XJ, Chen XM, Wang SB, Liu KD, Xing YQ. Ankle-brachial index and brachial-ankle pulse wave velocity are risk factors for ischemic stroke in patients with Type 2 diabetes. Neural Regen Res 2017;12:1853–9.
Ohkuma T, Tomiyama H, Ninomiya T, Kario K, Hoshide S, Kita Y, et al. Proposed cutoff value of brachial-ankle pulse wave velocity for the management of hypertension. Circ J 2017;81:1540–2.
Morimoto S, Yurugi T, Aota Y, Sakuma T, Jo F, Nishikawa M, et al. Prognostic significance of ankle-brachial index, brachial-ankle pulse wave velocity, flow-mediated dilation, and nitroglycerin-mediated dilation in end-stage renal disease. Am J Nephrol 2009;30:55–63.
Nakamura M, Yamashita T, Yajima J, Oikawa Y, Sagara K, Koike A, et al. Brachial-ankle pulse wave velocity as a risk stratification index for the short-term prognosis of type 2 diabetic patients with coronary artery disease. Hypertens Res 2010;33:1018–24.
Meguro T, Nagatomo Y, Nagae A, Seki C, Kondou N, Shibata M, et al. Elevated arterial stiffness evaluated by brachial-ankle pulse wave velocity is deleterious for the prognosis of patients with heart failure. Circ J 2009;73:673–80.
Kitahara T, Ono K, Tsuchida A, Kawai H, Shinohara M, Ishii Y, et al. Impact of brachial-ankle pulse wave velocity and ankle-brachial blood pressure index on mortality in hemodialysis patients. Am J Kidney Dis 2005;46:688–96.
Zeki AHA, Newman AB, Simonsick E, Sink KM, Sutton TK, Watson N, et al. Pulse wave velocity and cognitive decline in elders: the Health, Aging, and Body Composition study. Stroke 2013;44:388–93.
Webb AJ, Simoni M, Mazzucco S, Kuker W, Schulz U, Rothwell PM. Increased cerebral arterial pulsatility in patients with leukoaraiosis: arterial stiffness enhances transmission of aortic pulsatility. Stroke 2012;43:2631–6.
Palombo C, Kozakova M. Arterial stiffness, atherosclerosis and cardiovascular risk: pathophysiologic mechanisms and emerging clinical indications. Vasc Pharmacol 2016;77:1–7.
Liu X, Sun N, Yu T, Fan F, Zheng M, Qian G, et al. The independent and joint association of blood pressure, serum total homocysteine, and fasting serum glucose levels with brachial-ankle pulse wave velocity in chinese hypertensive adults. Int Heart J 2016;57:627–33.
Saji N, Kimura K, Kawarai T, Shimizu H, Kita Y. Arterial stiffness and progressive neurological deficit in patients with acute deep subcortical infarction. Stroke 2012;43:3088–90.
Acknowledgements
We acknowledge the contribution of all staff who participated in this study as well as the study participants who shared their time with us.
Funding
The study was supported by funding from the following: Peking University Medicine Fund of Fostering Young Scholars’ Scientific & Technological Innovation [grant 34254]; the National Key Research and Development Program of China [2016YFE0205400, 2018ZX09739010, 2018ZX09301034003]; the Science and Technology Program of Guangdong, China [2020B121202010]; the Science and Technology Planning Project of Guangzhou, China [201707020010]; the Science, Technology, and Innovation Committee of Shenzhen, China [GJHS20170314114526143, JSGG20180703155802047]; the Economic, Trade, and Information Commission of Shenzhen Municipality, China [20170505161556110, 20170505160926390, 201705051617070]; Peking University Medicine Fund of Fostering Young Scholars’ Scientific & Technological Innovation (grant 34254) Peking University Medicine Fund of Fostering Young Scholars’ Scientific & Technological Innovation (grant 34254).
Author information
Authors and Affiliations
Contributions
Conceptualization and methodology: XPX, YH, JPL. Software: LHH, LSL. Validation: YS, YZ. Formal analysis: LHH, YZ. Investigation: LHH, CLB, LSL, BYW, CQF, HM, XH, YZ. Data curation: LSL, YS, YZ. Writing (original draft preparation): LHH. Writing (review and editing): CLB, LSL, YS, BYW, CQF, HM, XH, YZ, XPX, XBW, YH, JPL. Supervision: XPX, YH, JPL. Project administration: CLB, LSL, YS, BYW, HM, JPL. Funding acquisition: XPX, XH, LHH. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Ethical approval
The study was approved by the Ethics Committee of the Institute of Biomedicine, Anhui Medical University, Hefei, China.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Hu, L., Bi, C., Liu, L. et al. Association between baseline brachial–ankle pulse wave velocity and short-term risk of first stroke among Chinese hypertensive adults. J Hum Hypertens 36, 1085–1091 (2022). https://doi.org/10.1038/s41371-021-00611-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41371-021-00611-7