Abstract
Objective
To assess the impact of chlorhexidine gluconate (CHG) bathing on skin bacterial burden in neonates.
Study design
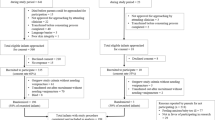
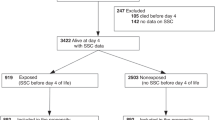
In this prospective observational study, arm and groin skin bacterial growth was measured in 40 CHG-exposed and nonexposed neonates admitted to the NICU. Exposed neonates received 2% CHG baths per protocol for central line-associated bloodstream infection (CLABSI) prevention or Staphylococcus aureus decolonization.
Results
Forty neonates were enrolled, 18 of whom were CHG-exposed. Mean baseline Gram-positive (GP) bacterial burden was 2.19 log CFU/ml on the arm and 1.81 log CFU/ml on the groin. Bacterial burden decreased after the first bath, but returned to baseline by 72 h. Residual skin CHG concentration declined over time, with a corresponding increase in GP bacterial burden.
Conclusions
CHG bathing reduces skin bacterial burden, but burden returns to baseline after 72 h. Twice weekly CHG bathing may be inadequate to suppress skin bacterial growth in hospitalized neonates.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Ponnusamy V, Venkatesh V, Clarke P. Skin antisepsis in the neonate: what should we use? Curr Opin Infect Dis. 2014;27:244–50.
Klevens RM, Edwards JR, Richards CL, Horan TC, Gaynes RP, Pollock DA, et al. Estimating health care-associated infections and deaths in U.S. hospitals, 2002. Public Health Rep. 2007;122:160–6.
Milstone AM, Passaretti CL, Perl TM. Chlorhexidine: expanding the armamentarium for control and prevention. Clin Infect Dis. 2008;46:274–81.
Vernon MO, Hayden MK, Trick WE, Hayes RA, Blom DW, Weinstein RA. Chlorhexidine gluconate to cleanse patients in a medical intensive care unit: the effectiveness of source control to reduce the bioburden of vancomycin-resistant enterococci. Arch Intern Med. 2006;166:306–12.
Bleasdale SC, Trick WE, Gonzalez IM, Lyles RD, Hayden MK, Weinstein RA. Effectiveness of chlorhexidine bathing to reduce catheter-associated bloodstream infections in medical intensive care unit patients. Arch Intern Med. 2007;167:2073–9.
Climo MW, Sepkowitz KA, Zuccotti G, Fraser VJ, Warren DK, Perl TM, et al. The effect of daily bathing with chlorhexidine on the acquisition of methicillin-resistant Staphylococcus aureus, vancomycin-resistant Enterococcus, and healthcare-associated bloodstream infections: results of a quasi-experimental multicenter trial. Crit Care Med. 2009;37:1858–65.
Marschall J, Mermel LA, Fakih M, Hadaway L, Kallen A, O’Grady NP, et al. Strategies to prevent central line-associated bloodstream infections in acute care hospitals: 2014 update. Infect Control Hosp Epidemiol. 2014;35:753–71.
Mullany LC, Saha SK, Shah R, Islam MS, Rahman M, Islam M, et al. Impact of 4.0% chlorhexidine cord cleansing on the bacteriologic profile of the newborn umbilical stump in rural Sylhet district, Bangladesh. Pediatr Infect Dis J. 2012;31:440–50.
Arifeen SE, Mullany LC, Shah R, Mannan I, Rahman SM, Talukder MR, et al. The effect of cord cleansing with chlorhexidine on neonatal mortality in rural Bangladesh: a community-based, cluster-randomized trial. Lancet. 2012;379:1022–8.
Sinha A, Sazawal S, Pradhan A, Ramji S, Opiyo N. Chlorhexidine skin or cord care for prevention of mortality and infections in neonates. Cochrane Database Syst Rev. 2015;3:CD007835.
Johnson J, Bracken R, Tamma PD, Aucott SW, Bearer C, Milstone AM. Trends in chlorhexidine use in US Neonatal Intensive Care Units: results from a follow-up national survey. Infect Control Hosp Epidemiol. 2016;37:1116–8.
Tamma PD, Aucott SW, Milstone AM. Chlorhexidine use in the neonatal intensive care unit: results from a national survey. Infect Control Hosp Epidemiol. 2010;31:846–9.
Quach C, Milstone AM, Perpête C, Bonenfant M, Moore DL, Perreault T. Chlorhexidine bathing in a tertiary care neonatal intensive care unit: impact on central line-associated bloodstream infections. Infect Control Hosp Epidemiol. 2014;35:158–63.
Chapman AK, Aucott SW, Milstone AM. Safety of chlorhexidine gluconate used for skin antisepsis in the preterm infant. J Perinatol. 2012;32:4–9.
Popovich KJ, Lyles R, Hayes R, Hota B, Trick W, Weinstein RA, et al. Relation of chlorhexidine gluconate skin concentration to microbial density on skin of critically ill patients bathed daily with chlorhexidine gluconate. Infect Control Hosp Epidemiol. 2012;33:889–96.
Popoola VO, Budd A, Wittig SM, Ross T, Aucott SW, Perl TM, et al. MRSA transmission and infections in a neonatal intensive care unit despite active surveillance cultures and decolonization—challenges for infection prevention. Infect Control Hosp Epidemiol. 2014;35:412–8.
Angeletti S. Matrix assisted laser desorption time of flight mass spectrometry (MALDI-TOF MS) in clinical microbiology. J Microbiol Methods. 2017;138:20–29.
Climo MA, Wong ES. Daily chlorhexidine bathing and hospital-acquired infection. N Engl J Med. 2013;368:2332.
Milstone AM, Elward A, Song X, Zerr DM, Orscheln R, Speck K, et al. Daily chlorhexidine bathing to reduce bacteraemia in critically ill children: a multicenter, cluster-randomised, crossover trial. Lancet. 2013;381:1099–106.
Sankar MJ, Paul VK. Efficacy and safety of whole body skin cleansing with chlorhexidine in neonates—a systemic review. Pediatr Infect Dis J. 2013;32:e227–e234.
Gupta B, Vaswani ND, Sharma D, Chaudhary U, Lekhwani S. Evaluation of efficacy of skin cleansing with chlorhexidine in prevention of neonatal nosocomial sepsis—a randomized controlled trial. J Matern Fetal Neonatal Med. 2016;29:242–7.
Acknowledgements
The authors wish to thank the study’s participants and their families, as well as Annie Voskertchian and Anne King for their study support, and Dr. Mary K. Hayden and her colleagues at Rush University for sharing their colorimetric assay protocol.
Funding
This study was supported by an investigator-initiated research grant from Sage Products, LLC, and NIH Training Grant Award T32 HL 125239-1 (JJ).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Johnson, J., Suwantarat, N., Colantuoni, E. et al. The impact of chlorhexidine gluconate bathing on skin bacterial burden of neonates admitted to the Neonatal Intensive Care Unit. J Perinatol 39, 63–71 (2019). https://doi.org/10.1038/s41372-018-0231-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-018-0231-7
This article is cited by
-
Myelin toxicity of chlorhexidine in zebrafish larvae
Pediatric Research (2023)
-
Neonatal sepsis and the skin microbiome
Journal of Perinatology (2022)
-
Chlorhexidine baths in preterm infants — are we there yet?
Journal of Perinatology (2019)