Abstract
Objectives
Quantify associations of human milk feeding with in-hospital growth and examine differences by human milk type (maternal or donor).
Study design
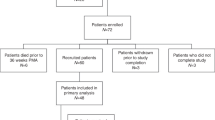
We included infants born <33 weeks’ gestation and <1500 g from 9 Neonatal Intensive Care Units (n = 1429). We estimated associations of percent of visit days fed any human milk (maternal or donor) and percent of days fed donor milk with weight, length, and head z-scores at discharge or transfer using a linear mixed model, adjusting for birth size and other covariates.
Results
Any human milk feeding was not associated with growth outcomes. Infants fed donor milk on ≥50% of days had less favorable growth vs. those fed <50% [z-scores—weight: −1.1 vs. −0.7 (p = 0.04); length: −1.5 vs. −1.1 (p = 0.04); head −1.0 vs. −0.3 (p < 0.01)].
Conclusions
Fortified human milk was not associated with impaired growth compared with preterm formula.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Section on Breastfeeding. Breastfeeding and the use of human milk. Pediatrics. 2012;129:e827–e841.
WHO. Born too soon: the global action report on preterm birth. Geneva: WHO; 2012. p. 126.
Cleminson JS, Zalewski SP, Embleton ND. Nutrition in the preterm infant: what’s new? Curr Opin Clin Nutr Metab Care. 2016;19:220–5.
Belfort MB, Anderson PJ, Nowak VA, Lee KJ, Molesworth C, Thompson DK, et al. Breast milk feeding, brain development, and neurocognitive outcomes: a 7-year longitudinal study in infants born at less than 30 weeks’ gestation. J Pediatr. 2016;177:133–9. e1.
Vohr BR, Poindexter BB, Dusick AM, McKinley LT, Wright LL, Langer JC, et al. Beneficial effects of breast milk in the neonatal intensive care unit on the developmental outcome of extremely low birth weight infants at 18 months of age. Pediatrics. 2006;118:e115–23.
Chowning R, Radmacher P, Lewis S, Serke L, Pettit N, Adamkin DH. A retrospective analysis of the effect of human milk on prevention of necrotizing enterocolitis and postnatal growth. J Perinatol. 2016;36:221–4.
Colaizy TT, Carlson S, Saftlas AF, Morriss FH Jr. Growth in VLBW infants fed predominantly fortified maternal and donor human milk diets: a retrospective cohort study. BMC Pediatr. 2012;12:124.
Maas C, Wiechers C, Bernhard W, Poets CF, Franz AR. Early feeding of fortified breast milk and in-hospital-growth in very premature infants: a retrospective cohort analysis. BMC Pediatr. 2013;13:178.
Hoban R, Schoeny ME, Esquerra-Zwiers A, Kaenkumchorn TK, Casini G, Tobin G, et al. Impact of donor milk on short- and long-term growth of very low birth weight infants. Nutrients. 2019;11:241.
Sisk PM, Lambeth TM, Rojas MA, Lightbourne T, Barahona M, Anthony E, et al. Necrotizing enterocolitis and growth in preterm infants fed predominantly maternal milk, pasteurized donor milk, or preterm formula: a retrospective study. Am J Perinatol. 2017;34:676–83.
Piemontese P, Liotto N, Mallardi D, Roggero P, Puricelli V, Giannì ML, et al. The effect of human milk on modulating the quality of growth in preterm infants. Front Pediatr. 2018;6:291.
Belfort MB, Edwards EM, Greenberg LT, Parker MG, Ehret DY, Horbar JD. Diet, weight gain, and head growth in hospitalized US very preterm infants: a 10-year observational study. Am J Clin Nutr. 2019;109:1373–9.
Quigley M, Embleton ND, McGuire W. Formula versus donor breast milk for feeding preterm or low birth weight infants. Cochrane Database Syst Rev. 2018;6:CD002971.
O’Connor DL, Gibbins S, Kiss A, Bando N, Brennan-Donnan J, Ng E, et al. Effect of supplemental donor human milk compared with preterm formula on neurodevelopment of very low-birth-weight infants at 18 months: a randomized clinical trial. JAMA. 2016;316:1897–905.
Gidrewicz DA, Fenton TR. A systematic review and meta-analysis of the nutrient content of preterm and term breast milk. BMC Pediatr. 2014;14:216.
Zachariassen G, Fenger-Gron J, Hviid MV, Halken S. The content of macronutrients in milk from mothers of very preterm infants is highly variable. Dan Med J. 2013;60:A4631.
Olsen IE, Groveman SA, Lawson ML, Clark RH, Zemel BS. New intrauterine growth curves based on United States data. Pediatrics. 2010;125:e214–24.
Patel AL, Engstrom JL, Meier PP, Kimura RE. Accuracy of methods for calculating postnatal growth velocity for extremely low birth weight infants. Pediatrics. 2005;116:1466–73.
Olsen IE, Richardson DK, Schmid CH, Ausman LM, Dwyer JT. The impact of early transfer bias in a growth study among neonatal intensive care units. J Clin Epidemiol. 2003;56:998–1005.
Perrin MT. Donor human milk and fortifier use in United States level 2, 3, and 4 neonatal care hospitals. J Pediatr Gastroenterol Nutr. 2018;66:664–9.
Montjaux-Régis N, Cristini C, Arnaud C, Glorieux I, Vanpee M, Casper C. Improved growth of preterm infants receiving mother’s own raw milk compared with pasteurized donor milk. Acta Paediatr. 2011;100:1548–54.
Brownell EA, Matson AP, Smith KC, Moore JE, Esposito PA, Lussier MM, et al. Dose-response relationship between donor human milk, mother’s own milk, preterm formula, and neonatal growth outcomes. J Pediatr Gastroenterol Nutr. 2018;67:90–6.
Neu J. Mother’s own milk: how does it differ from donor milk for the baby. Breastfeed Med. 2019;14 S1:S3–4.
Belfort MB, Ramel SE. NICU diet, physical growth and nutrient accretion, and preterm infant brain development. Neoreviews. 2019;20:e385–96.
Victora CG, de Onis M, Hallal PC, Blössner M, Shrimpton R. Worldwide timing of growth faltering: revisiting implications for interventions. Pediatrics. 2010;125:e473–80.
Foote JM, Brady LH, Burke AL, Cook JS, Dutcher ME, Gradoville KM, et al. Development of an evidence-based clinical practice guideline on linear growth measurement of children. J Pediatr Nurs. 2011;26:312–24.
Acknowledgements
Neonatal Quality Improvement Collaborative of Massachusetts (NeoQIC) includes: Bay State Medical Center, Beth Israel Deaconess Medical Center, Boston Medical Center, Brigham and Women’s Hospital, Massachusetts General Hospital, Boston Children’s Hospital, South Shore Hospital, St. Elizabeth’s Medical Center, Tufts Medical Center, and UMass Medical Center.
Funding
The study is supported by the CDC (1U38PD005373) and W.K. Kellogg Foundation (P3031871).
Author information
Authors and Affiliations
Contributions
MB, MP, and MG conceptualized the project. MB developed the research plan. BS and PM conducted the statistical analysis. MB, BS, MP, PM, and MG contributed to interpretation of the results. BS drafted the manuscript. MB, MP, PM and MG critically reviewed the manuscript. All authors are responsible for the final content of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
MB and MP report that they are volunteer members of the Research Advisory Board of the Mother’s Milk Bank Northeast (USA). We have no other conflicts of interest to disclose.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Soldateli, B., Parker, M., Melvin, P. et al. Human milk feeding and physical growth in very low-birth-weight infants: a multicenter study. J Perinatol 40, 1246–1252 (2020). https://doi.org/10.1038/s41372-020-0705-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41372-020-0705-2
This article is cited by
-
Effects of human milk on body composition and growth in very low birthweight infants
Pediatric Research (2023)