Abstract
Maternal immune activation (MIA) and poor maternal nutritional habits are risk factors for the occurrence of neurodevelopmental disorders (NDD). Human studies show the deleterious impact of prenatal inflammation and low n-3 polyunsaturated fatty acid (PUFA) intake on neurodevelopment with long-lasting consequences on behavior. However, the mechanisms linking maternal nutritional status to MIA are still unclear, despite their relevance to the etiology of NDD. We demonstrate here that low maternal n-3 PUFA intake worsens MIA-induced early gut dysfunction, including modification of gut microbiota composition and higher local inflammatory reactivity. These deficits correlate with alterations of microglia-neuron crosstalk pathways and have long-lasting effects, both at transcriptional and behavioral levels. This work highlights the perinatal period as a critical time window, especially regarding the role of the gut-brain axis in neurodevelopment, elucidating the link between MIA, poor nutritional habits, and NDD.
Similar content being viewed by others
Introduction
Neurodevelopmental disorders (NDD), such as Autism Spectrum Disorders (ASD), intellectual Disability or Attention Deficit Hyperactivity Disorder (ADHD), are a group of disabilities that arise from a disrupted development of the central nervous system (CNS) [1]. Individuals with NDD display cognitive deficits, associated with hippocampal dysfunction, among other symptoms [1]. Despite the identification of several genetic risk factors, they do not entirely explain NDDs. These disorders can also originate from complex interactions between various environmental factors [2]. Epidemiological studies reveal that maternal immune activation (MIA) or poor nutritional habits in the perinatal period are among the strongest of risk factors for NDD [3,4,5,6,7,8].
Long term structural and behavioral deficits relevant to NDD are commonly observed in the offspring of rodent models of MIA, including memory deficits and functional alterations in the hippocampus [6, 9,10,11,12,13,14,15]. Furthermore, some nutrients, including the polyunsaturated fatty acids (PUFAs), have a profound long-term influence on brain function [5, 16, 17]. PUFAs are essential fatty acids required for proper brain development and maturation [18,19,20,21,22,23,24,25]. Because they must be provided by alimentation, low dietary intake of these nutrients strongly affects neurodevelopment [8]. The principal forms of PUFAs in the CNS are the long chain (LC) arachidonic acid (AA, 20:4n-6) and the docosahexaenoic acid (DHA, 22:6n-3) [16]. Both clinical and preclinical studies show that low levels of LC n-3 PUFAs increase the risk of NDD and/or aggravate symptoms [8, 16, 26]. Recent clinical evidence suggests that n-3 PUFA homeostasis may be altered in ASD, either as a result of nutritional imbalance or genetic defect [27]. Finally, we and others already showed that decreasing n-3 PUFA dietary intake can affect the offspring’s susceptibility to MIA [8, 28]. However, the mechanisms linking the early-life nutritional status and inflammation to later life behavioral alterations are still unclear.
Microglia are essential for brain maturation, hence, interfering in their developmental activity gives rise to NDD-like symptoms in mice [9, 29,30,31]. In normal conditions, microglia guide axons, phagocyte apoptotic neurons, refine spines and synapses, in an activity-dependent manner [29, 30, 32,33,34,35,36,37,38,39,40,41,42,43]. Both MIA and nutritional imbalance have been shown to disrupt these processes, which might explain the long-term structural and behavioral defects [8, 9, 16, 44]. Myelination is also sensitive to early-life insults and a decrease in white matter integrity is a marker of most, if not all, NDDs [45, 46]. Both MIA and n-3 PUFAs can modulate myelination according to preclinical and clinical studies [47,48,49,50,51,52,53,54,55,56,57].
More recent literature highlights the role of the gut-brain axis in the occurrence of NDD [58,59,60,61]. Clinical studies have observed alterations in the composition of microbiota and associated metabolites in subjects with autism and schizophrenia [62,63,64,65,66,67,68]. The gut microbiome plays an important role in the modulation of microglial function and myelination and both PUFAs and MIA can alter its composition [69,70,71,72,73,74].
In the present study, we show that (1) n-3 PUFA deficiency reveals MIA-induced behavioral alterations in adult offspring but not in pups, (2) both n-3 PUFA deficiency and MIA affect brain lipid composition in adults, (3) this correlates to profound transcriptomic alterations in adulthood, especially for genes involved in CNS development, (4) n-3 PUFA deficiency worsens the impact of MIA on microglia-neuron crosstalk and alters the expression of oligodendrocyte and myelin markers in the developing brain, (5) n-3 PUFA deficiency worsens MIA-induced microbiota and gut alterations in pups, (6) microbial composition and gut inflammatory molecules correlate with neurobiological outcome during the post-natal period.
Material and methods
Animals
Animal husbandry and experimental procedures were in accordance with the EU Directive 2010/63/EU for animal experiments and approved by the Bioethical committee of our University (no. 50120186-A) and Région Aquitaine Veterinary Services (Direction Départementale de la Protection des Animaux, approval ID: A33-063-920). Every effort was made to minimize suffering and the number of animals used. All experiments were conducted in CD1 mice (Charles River, Arbresle, France). Mice were maintained under standard housing conditions in a temperature (23 ± 1 °C) and humidity (40–50%) controlled animal room with a 12h/12h light/dark cycle (07 h–19 h) and ad libitum access to food and water.
Diet and treatment
α-linolenic acid (ALA, 18:3 n-3) and linoleic acid (LA, 18:2 n-6) are the dietary precursors of omega-3 and omega-6 respectively. As soon as the male was introduced in the mating cage, female mice were fed isocaloric diets containing 5% fat with a high or low LA(n-6)/ALA(n-3) ratio (n-3 deficient group or “DEF” and n-3 sufficient group or “SUFF,” respectively) across gestation and lactation (i.e., from the first day of gestation until the post-natal day –PND-21) [28, 75,76,77,78,79]. These diets were custom-made and the pellets were prepared by the SAAJ-INRAE laboratory (Jouy-en-Josas, France).
Females were exposed to males for 48 h. Mating was further confirmed by the observation of a vaginal plug and by measuring weight gain across gestation. At embryonic day 17 (E17), pregnant females were given an intraperitoneal (i.p.) injection of lipopolysaccharide (LPS, E. Coli LPS0127:B8, Sigma Inc, St. Louis, MO, USA; 0.12 µg/g mouse/100 µl). We assessed the development of a sickness behavior in dams by comparing their body weight at E17 and E18 (24 h after the administration of LPS). As expected, we found a significant decrease in body weight in both n-3 sufficient and n-3 deficient mice (Supplementary Fig. 1). We previously showed that this dose of LPS was sufficient to induce an inflammatory response in fetuses’ brain, which was exacerbated by n-3 PUFA deficiency [28]. The administration of the corresponding volume of saline solution (NaCl 0.9%, “Saline”) was used as a control [28, 80, 81]. Sickness behavior and weight were monitored at E17 and E18 to confirm that dams treated with LPS displayed a significantly lower weight gain than saline-treated dams (see MIA checklist, Table S1; [82]).
At birth, litter size was limited to 10 pups. At PND21, the weaned males were housed in groups of 3–6 without mixing the litters. We generated between 2 and 5 litters per condition. Only 1–2 pups from each litter were tested, to avoid any litter effect.
Cohorts were organised as follows (Fig. 1a): (1) One cohort for neonates’ behavior (PND4-8) (Fig. 1); (2) One cohort to assess microglial density/phenotype, microglia-neuron crosstalk and neuronal morphology between PND14 and PND28 (Fig. 3); (3) One cohort dedicated to gut assessment (intestinal permeability, microbiota composition). The brains of these mice were used to conduct immunohistochemistry studies (Iba-1, myelin markers) and perform correlation studies (Figs. 4, 5); (4) 2 cohorts were used for the behavioral assessment of the adult offspring (one for locomotion and anxiety and another for memory testing by the Morris Water Maze) (Fig. 1); (5) one cohort for lipid and transcriptomic profiling in the hippocampus of adults (Fig. 2).
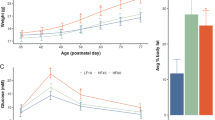
All graphs show Means ± SEM. a Experimental setup. b Average time spent by pups to achieve the Fox battery tests (negative geotaxis and righting reflex; 3 trials per day from PND4 to PND6). N = 14–19. Two-way ANOVA: MIA effect, F(1,62) = 11.67, p = 0.0011. c Average vocalization time (15-min sessions at PND7-8). N = 14–19. Kruskal–Wallis test followed by Mann–Whitney comparison; n-3 sufficient-Saline vs n-3 sufficient-LPS, **p < 0.01. d Neonate average locomotion measured as the distance traveled (in cm/min) during 1 min-session from PND5 to PND8. N = 14–19. Kruskal–Wallis test followed by Mann–Whitney comparison; n-3 sufficient-Saline vs n-3 deficient-saline, **p = 0.009, n-3 deficient-Saline vs n-3 deficient-LPS, ***p < 0.001. e Time course of locomotor activity of newborns from PND5 to PND8. N = 14–19. Two-way ANOVA on repeated measures followed by Bonferroni’s multiple comparisons test: n-3 deficient-Saline vs n-3 deficient-LPS, *p = 0.02. f Time course of the distance traveled in the Morris Water Maze during the learning phase (in cm). N = 10. Two-way ANOVA on repeated measures: diet effect, F(1,36) = 9.22, p = 0.004. g Percentage of time spent in the target quadrant. N = 10. One-sample t test; n-3 sufficient-Saline, ***p < 0.001; n-3 sufficient-LPS, **p = 0.004; n-3 deficient-saline, ***p < 0.001; n-3 deficient-LPS, p = 0.11. h. Time course of the distance traveled in the Morris Water Maze during the reversal learning phase (in cm). N = 10. Two-way ANOVA on repeated measures: MIA effect, F(1,36) = 3.27, p = 0.008; time effect, F(1,36) = 19, p < 0.001. i Basal locomotor activity (in cm). N = 12. Kruskal–Wallis test followed by Mann–Whitney comparison; n-3 deficient-Saline vs n-3 deficient-LPS, **p = 0.008. j Time spent in the light box (anxiogenic area) of the light-dark test. N = 11. Kruskal–Wallis test followed by Mann–Whitney comparison. k Percentage of time spent in the center of the open-field arena (anxiogenic area). N = 8–11. Kruskal–Wallis test followed by Mann–Whitney comparison.
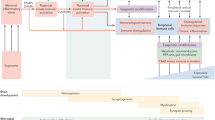
Quantification of the levels of total PUFAs (a), n-6 PUFAs (b), DTA n-6 (c) or DPAn-6 (d) in the hippocampus of adult mice, expressed as the percentage of total fatty acids. All graphs show Means ± SEM. N = 6. Two-way ANOVA followed by Bonferroni’s multiple comparisons test: Total PUFAs: n-3 sufficient-Saline vs n-3 deficient-Saline, ***p = 0.0001; n-3 deficient-Saline vs n-3 deficient-LPS, *p = 0.0156; n-3 deficient-Saline vs n-3 sufficient-LPS, ***p = 0.0003. Total n-6 PUFAs: n-3 sufficient-Saline vs n-3 deficient-Saline, ***p < 0.0001; n-3 deficient-Saline vs n-3 deficient-LPS, **p = 0.0055; n-3 deficient-Saline vs n-3 sufficient-LPS, ***p < 0.0001; n-3 sufficient-Saline vs n-3 deficient LPS, ***p < 0.0001; n-3 deficient-LPS vs n-3 sufficient-LPS, ***p < 0.0001. DTA n-6: n-3 sufficient-Saline vs n-3 deficient-Saline, ***p < 0.0001; n-3 deficient-Saline vs n-3 deficient-LPS, **p = 0.0013; n-3 deficient-Saline vs n-3 sufficient-LPS, ***p < 0.0001; n-3 sufficient-Saline vs n-3 deficient LPS, ***p = 0.0004; n-3 deficient-LPS vs n-3 sufficient-LPS, *p = 0.0158. DPA n-6: n-3 sufficient-Saline vs n-3 deficient-Saline, ***p < 0.0001; n-3 deficient-Saline vs n-3 deficient-LPS, **p = 0.0045; n-3 deficient-Saline vs n-3 sufficient-LPS, ***p < 0.0001; n-3 sufficient-Saline vs n-3 deficient LPS, ***p < 0.0001; n-3 deficient-LPS vs n-3 sufficient-LPS, ***p < 0.0001. e Venn diagram highlighting the number of genes that were modulated by MIA in the hippocampi of adult n-3 sufficient (blue) or n-3 deficient (red) mice. Lower panel: Number of genes that were up- or down-regulated in n-3 sufficient and n-3 deficient mice. Representation of the 20 most significantly dysregulated genes in n-3 sufficient (f) and n-3 deficient (g) mice. Genes that appear in both n-3 sufficient and n-3 deficient mice are bold. h PCA analysis of MIA-induced differentially expressed genes (DEG) in both dietary groups. Confidence ellipses appear around each group. i, j Gene Ontology analysis of DEGs (light red and blue: up-regulated genes; dark red and blue: down-regulated genes).
All methodological details appear as supplementary information.
Statistical analysis
All data are expressed as means ± SEM. Normality and homoscedasticity of distributions were assessed by Shapiro-Wilk test and Brown–Forsythe test respectively. Data were then analysed using parametric two-way analysis of variance (ANOVA) (diet and prenatal treatment as factors) followed by Bonferroni post-hoc test when applicable. If normality and/or homoscedasticity tests failed, data were analyzed with a non-parametric Kruskal–Wallis test followed by Mann–Whitney U test when applicable. To analyse recognition index results in the probe test of the Morris Water Maze, we performed a one sample t tests (comparison to chance level set at 25%). To calculate the inflammation Z-score, all cytokines were converted to Z-scores (each cytokine value subtracted by the mean of the group and divided by the SD), and the Z-scores were added. Spearman correlations were used to explore associations between microbial composition, the gut immune cells reactivity and markers of myelin and oligodendrocytes. All analyses were conducted with GraphPad Prism 7 (GraphPadSotfware, San Diego, USA) except for repeated measures analysis (learning and reversal phase in Morris Water Maze task; pups’ exploratory behavior), where we used Statistica 6.0 (StatSoft, Tulsa, USA) and for correlation matrix where we used R version 3.5.2. For all results, statistical significance was set at p < 0.05. Details for all statistical results are presented in Tables S2 and S3.
Results
Low maternal n-3 PUFA dietary intake results in MIA-induced locomotor and spatial memory deficits in adult offspring
We assessed short and long-term consequences of MIA and dietary manipulation on offspring’s behavior. Regardless of the diet, MIA negatively affected the psychomotor score of pups between PND4 and PND6, measured by the increase of time needed to perform the 2 tests of the Fox battery. In addition, MIA decreased the whistles time of vocalizing PND7-8 pups in response to maternal separation, independent of maternal diet. (Fig. 1b, c). The exploratory behavior of neonates was significantly decreased in n-3 deficient mice (Fig. 1d, e). Moreover, MIA significantly increased the mean exploratory behavior of n-3 deficient animals.
In adulthood, n-3 deficient mice displayed learning deficits during the training phase of the Morris Water Maze task (Fig. 1f). During the probe test, MIA-exposed n-3 deficient mice spent the same amount of time in all 4 quadrants of the maze, a marker of spatial memory deficits (Fig. 1g). When assessing locomotor activity, MIA-exposed n-3 deficient mice traveled significantly longer distances than n-3 deficient-Saline or n-3 sufficient mice during the 1 h-recording period (Fig. 1i).
Finally, we could not find any effect of MIA or diet on the reversal task in the Morris Water Maze, or on the anxiety levels as assessed in the light-dark box and the open-field (data not shown) (Fig. 1h–k).
Overall, our data showed that MIA induced spatial memory deficits and hyper-locomotion only in n-3 deficient adult offspring.
MIA-exposed n-3 deficient adult mice display alterations in the metabolism of n-6 PUFAs in the hippocampus
N-3 PUFA dietary deficiency significantly altered fatty acid composition of the hippocampus in the adult offspring (Fig. 2a–d, Table 1, Table S3), including an increase in the total amount of n-6 PUFAs, Saturated Fatty Acids and MonoUnsaturated Fatty Acids, and a decrease in n-3 PUFAs. MIA alone also increased SFA concentration and decreased total PUFAs, total n-6 PUFAs, DocosaTetraenoic Acid (DTA), and DPA levels (Table 1 and Table S3). Post-hoc analysis revealed that these effects were more pronounced in MIA-exposed n-3 deficient mice (Fig. 2a–d).
Dietary n-3 PUFA deficiency exacerbates MIA-mediated alterations of gene expression in the adult hippocampus
Next, we used transcriptomics to assess gene regulations sustaining the behavioral effects of n-3 PUFA deficiency and MIA in adults. We focused on the hippocampus, a critical structure for learning and memory abilities [83]. When comparing MIA-exposed mice to saline-treated individuals, 337 genes were significantly differentially expressed (DEGs) in n-3 sufficient mice vs 610 DEGs in n-3 deficient animals, among which 120 genes were common to both dietary groups (Tables 2, 3). This suggests that MIA had a greater impact on gene expression under low n-3 PUFA intake (Fig. 2e). Figure 2f, g illustrates the most significantly dysregulated genes in n-3 sufficient (Fig. 2f) and n-3 deficient mice (Fig. 2g). Principal component analysis (PCA), using DEGs between n-3 sufficient-LPS vs n-3 deficient-LPS mice, showed separation between dietary groups (Fig. 2h).
We then used the MGI database [84] to retrieve the non-redundant Gene-Ontology annotations of interest that are related to the set of DEGs identified above. We computed the number of genes for each selected GO-term, in every group of DEGs identified for each diet type (Fig. 2i, j). The analysis revealed that the majority of these genes belong to “Cell communication” (e.g., synaptic activity, neurotransmitter release), “Immune/defense response” (e.g., leukocyte activation/migration/homeostasis), “CNS development” (e.g., myelination, gliogenesis, neurogenesis) or “Lipid metabolism” (e.g., fatty acid metabolism, membrane lipid metabolic process) pathways (Fig. 2i, j). Based on these transcriptomic data, we further analysed the impact of low n-3 PUFA intake and exposure to MIA on: (1) microglia-neuron crosstalk in the developing hippocampus; (2) neuronal phenotype; (3) myelination.
MIA induces persistent neuronal morphology alterations in n-3 deficient mice, likely by modifying microglia-neuron interactions
During the first post-natal weeks, microglia prune nonfunctional and immature synapses as a maturation mechanism for neuronal networks [29, 30, 85]. We quantified the level of colocalization between microglia (Iba-1) and dendritic spines (PSD95) at PND14, when synaptic refinement peaks in the hippocampus [86]. Our data show that n-3 PUFA deficiency significantly increased the level of Iba-1/PSD95 colocalization at PND14, suggesting greater synaptic pruning activity (Fig. 3a). Prenatal exposure to LPS did not show any effect. However, MIA differentially affected the expression of c3, cd47, cx3cr1, cx3cl1 according to n-3 PUFA intake, all these genes being involved in microglia-mediated synaptic pruning in the developing brain (Fig. 3b). These effects could not be attributed to modifications of microglial density (quantification of Iba-1 immunoreactivity) and/or phenotype (flow cytometry analysis of phenotypic markers on sorted microglia) (Supplementary Fig. 2a, b). We could only observe a slight, yet significant, increase in the proportion of CD86+ microglia in MIA-exposed n-3 deficient mice at PND14, suggesting that the cells may be skewed towards a proinflammatory phenotype (Supplementary Fig. 2b) [87]. Prenatal LPS exposure also did not affect cytokine mRNA production in the hippocampus of the offspring (Supplementary Fig. 2c).
All graphs show Means ± SEM. a Colocalization of Iba-1 and PSD95 proteins immunoreactivity in the CA1 region of the hippocampus of PND14 pups. Representative confocal image of Iba-1 (green) PSD95 (red) costaining (Top panel: scale bar = 10 µm) and Imaris 3D reconstruction (Bottom panel, scale bar = 1 µm). N = 72–122. Kruskal–Wallis test followed by Mann–Whitney comparisons; n-3 deficient-Saline vs n-3 sufficient-Saline, ***p < 0.0001; n-3 deficient-LPS vs n-3 sufficient-LPS, ***p < 0.0001. b qRT-PCR quantification of microglia-neuron interaction mRNA markers in the hippocampus of PND14 mice (data normalized to the saline group, dotted line). N = 4–6. Kruskal–Wallis test followed by Mann–Whitney comparisons; *p < 0.05, **p < 0.01 (all comparisons in Table S2). c Quantification and representative images of Golgi staining spine density in the CA1 region of the hippocampus at PND28. N = 8–21. Kruskal–Wallis test followed by Mann–Whitney comparisons; n-3 deficient-Saline vs n-3 deficient-LPS, ***p < 0.0001; n-3 deficient-Saline vs n-3 sufficient-Saline, **p = 0.001; n-3 deficient-LPS vs n-3 sufficient-LPS, *p = 0.025. d Western blot-based quantification and representative images of PSD95 protein expression in the hippocampus of PND28 mice. N = 4–8. Kruskal–Wallis test followed by Mann–Whitney comparisons; n-3 deficient-Saline vs n-3 deficient-LPS, **p = 0.004; n-3 deficient-LPS vs n-3 sufficient-LPS, *p = 0.03. Quantification of Olig2 (e), PLP (f), APC (g), MAG (h) and MBP (i) immunoreactivity in the hippocampus of PND14 mice. N = 4–7. Two-way ANOVA. Olig2: diet effect, F(1,20) = 3.48, p = 0.08; MIA effect, F(1,20) = 4.78, p = 0.041. PLP: MIA effect, F(1,22) = 5.01, p = 0.036. APC: diet effect, F(1,17) = 4.96, p = 0.0397.
We further studied the consequences of altered microglia-neuron interactions on neuronal morphology at PND28, when most of the synaptic refinement is complete in the hippocampus. N-3 PUFA deficiency significantly decreased spine density (Fig. 3c). We also observed that MIA-exposed n-3 deficient mice had greater number of spines on pyramidal neuron and expressed higher amount of PSD95 protein vs n-3 deficient-Saline animals (Fig. 3c, d). MAP2 protein expression was similar across all experimental groups (Supplementary Fig. 2d).
Overall, our data suggest that n-3 PUFA deficiency affected the amplitude of response to MIA in terms of dendritic spine density and microglia-neuron communication during the post-natal period.
No interaction between MIA and n-3 PUFA deficiency on myelin and oligodendrocyte protein expression
According to the transcriptomic analysis, “gliogenesis” and “myelination” processes are likely to be altered by MIA and n-3 PUFA deficiency (Fig. 2j). MIA significantly reduced the expression of Olig2 (marker of all oligodendrocytes) and PLP (mature oligodendrocytes marker) at PND14, the peak of oligodendrocyte maturation and myelination in the developing brain (Fig. 3e, f). APC protein (for Adenomatous Polyposis Coli, a marker for mature oligodendrocytes) levels were significantly increased by n-3 PUFA deficiency while the expression of the myelin proteins MAG and MBP were not altered (Fig. 3g–i). Overall, we did not observe any interaction between MIA exposure and low n-3 PUFA dietary intake on oligodendrocyte and myelin protein expression.
MIA differentially alters microbiota composition in both dietary groups and reveals gut alterations under n-3 PUFA deficiency
A growing body of evidence suggests microbial modulation of brain functions, especially when occurring during the post-natal developmental phase [12, 59, 61, 69, 70, 74, 88,89,90,91,92,93,94,95,96,97,98,99,100,101,102,103,104,105,106,107]. We therefore assessed the gut microbiota at PND14 and PND21, i.e., during a critical time window for gut physiology and gut-brain communication. Alpha diversity was significantly higher in n-3 sufficient-Saline group than in any other group, at both time points, (Fig. 4a–e; Tables 4, 5). While n-3 PUFA deficiency decreased diversity at both time points, at PND21 MIA restored microbial diversity up to control levels in n-3 deficient mice (Fig. 4e; Table 5). A strong effect of diet and MIA was observed at phyla, family and genus levels (Fig. 4b, c–f, g; Tables 4, 5). At both ages, n-3 PUFA deficiency increased the amount of Proteobacteria and decreased the proportion of Lachnospiraceae. It also decreased the amount of Prevotellaceae and increased Akkermansiacaceae and Entoreobacteriaceae at PND14, and decreased the Lactobacillaceae and increased the Tannerellaceae and Rikenellaceae at PND21 (Fig. 4c–g). All groups clustered together by PCA analysis at PND14, while they clustered distinctly from controls (n-3 sufficient-Saline) at PND21 (Fig. 4d–h). Our data revealed a robust effect of MIA and low n-3 PUFA intake, alone and combined, on gut microbiota composition, in an age-dependent manner.
All graphs show Means ± SEM. a 16S rRNA-sequencing-based alpha diversity analysis of the microbiota, measured by Shannon index in PND14 mice. N = 8–12. Two-way ANOVA: diet effect, F(1,39) = 12.76, p < 0.001; MIA effect, F(1,39) = 5.39, p = 0.026. Bacteria phyla (b) and family (c) observed in all experimental groups at PND14. d PCA of all subjects at PND14. Confidence ellipses appear around each group. e 16S rRNA-sequencing-based alpha diversity analysis, measured by Shannon index in PND21 mice. N = 8–13. Two-way ANOVA: n-3 sufficient-Saline vs n-3 sufficient-LPS, ***p = 0.0005; n-3 sufficient-LPS vs n-3 deficient-LPS, *p = 0.019; n-3 sufficient-Saline vs n-3 deficient-Saline, **p = 0.0078. Bacteria phyla (f) and family (g) observed in all experimental groups at PND21. h PCA of all subjects at PND14. Confidence ellipses appear around each group. Quantification of MLN lymphocytes cytokine release measured by ELISA at PND14 (i) and PND21 (j). N = 6–15; Kruskal–Wallis test followed by Mann–Whitney comparisons; *p < 0.05, **p < 0.01, ***p < 0.001 (all comparisons in Table S2). Z-score of T cells inflammatory reactivity in PND14 (k) and PND21 (l) mice. N = 7–15. Kruskal–Wallis test followed by Mann–Whitney comparisons; PND14: n-3 deficient-Saline vs n-3 deficient-LPS, ***p < 0.001. PND21: n-3 sufficient-Saline vs n-3 sufficient-LPS, **p = 0.0011, n-3 sufficient-LPS vs n-3 deficient-LPS, ***p = <0.0004.
At PND14, n-3 PUFA deficiency significantly shortened colon length and increased its permeability. MIA displayed no effect on these parameters (Supplementary Fig. 3a, b). At PND21, n-3 deficient-Saline mice still exhibited shorter colon but lower permeability compared with n-3 sufficient group. MIA increased both parameters in n-3 deficient mice while it had no effect in mice fed n-3 PUFA sufficient diet (Supplementary Fig. 3c, d).
We then assessed mesenteric lymph node T-cells cytokine secretion as a marker of gut immune reactivity [59, 108]. T cells sorted from PND14 n-3 deficient-LPS mice released greater levels of TNFα, IFN-γ, and IL-17 upon anti-CD3/anti-CD28 stimulation compared with n-3 sufficient-LPS group, while production of the anti-inflammatory cytokine IL-10 was hampered (Fig. 4i). We calculated a z-score that summarizes the cytokine profile of mice and confirmed that the effect of MIA on cytokine release was more pronounced in n-3 deficient mice (Fig. 4k). At PND21, MIA increased cytokine production more drastically in stimulated T cells sorted from n-3 sufficient mice (Fig. 4j, l). At histological levels, inflammation (Ameho score) was not different between groups (Supplementary Fig. 3e, f).
Hence, n-3 PUFA deficiency enhanced gut immune reactivity during the post-natal period, shifting the MIA-mediated proinflammatory response towards the earlier time point.
Microbial modifications correlate with gut inflammatory reactivity and neurobiological alterations
Spearman’s correlation matrix between gut immune cells reactivity and bacterial genera show that the microbial composition was tightly correlated with gut inflammatory reactivity both at PND14 and PND21 (Fig. 5a–c). Our data also revealed correlations between microbial composition and markers of myelin (olig2, MAP2, PLP) and microglial cells (Iba-1) (Fig. 5b–d).
a Spearman’s correlation matrix between gut immune cells reactivity (e.g cytokine release after T-cells stimulation) and bacterial genera in PND14 mice (*p = 0.05). b Spearman’s correlation matrix between neurobiological measurements (PLP, Olig2, Iba-1 and MAP2) and bacterial genera in PND14 mice (*p = 0.05). c Spearman’s correlation matrix between gut immune cells reactivity (e.g cytokine release after T-cells stimulation) and bacterial genera in PND21 mice (*p = 0.05). d Spearman’s correlation matrix between neurobiological measurements (PLP, Olig2, Iba-1, and MAP2) and bacterial genera in PND21 mice (*p = 0.05). e Spearman’s correlation between gut immune cells reactivity (e.g released cytokines after stimulation) and neurobiological parameters in PND21 mice (*p = 0.05). N = 20–22. Escherichia-Shig: Escherichia-Shigella; Eubacterium copro: Eubacterium coprostanoligenes group; Lachno NK4A136: Lachnospiraceae NK4A136 group; Lachno UCG-008: Lachnospiraceae UCG-008; Prevo UCG-001: Prevotellaceae UCG-001; Rikenellaceae RC9: Rikenellaceae RC9 gut group; Ruminococcus gg: Ruminococcus gnavus group. f Schematic summarizing the main findings. Exposure of n-3 PUFA deficient dams to MIA alters the gut microbiota composition and increases the inflammatory reactivity of the gut T-lymphocytes in the offspring during the post-natal period. This is correlated with an impairment in microglia-neuron crosstalk during this phase, with consequences on hippocampus function and memory abilities later in life.
We further assessed potential correlations between gut inflammatory reactivity and neurobiological features at PND21. Spearman correlation analysis revealed a strong correlation between Iba-1 and T cells-induced cytokines (Fig. 5e). We also observed significant correlation between Olig2 expression and the production of TNF-α and IL-17 (Fig. 5e). This suggests that alterations of gut physiology are linked to neurobiological defects in the developing brain.
Discussion
We and others previously showed that maternal dietary n-3 PUFA intake influences neurobiological and behavioral outcome in mice exposed to prenatal inflammation [6, 9, 28, 109, 110]. Our study is the first to extensively explore the mechanisms underlying the cumulative effects of MIA and n-3 PUFA deficiency, along the gut-brain axis and at various ages (Fig. 5f). We show that (1) n-3 PUFA dietary deficiency reveals MIA-induced behavioral alterations in adult offspring but not in pups, (2) MIA-exposed n-3 deficient adult mice display alterations in the metabolism of n-6 PUFAs in the hippocampus. (3) This was correlated to profound transcriptomic alterations, especially for genes involved in CNS development processes, such as synaptic plasticity, myelination and inflammation. (4) N-3 PUFA deficiency worsened the impact of MIA on microglia-neuron interaction in pups. (5) N-3 PUFA deficiency worsened MIA-induced microbiota and gut alterations in the post-natal period. (6) Microbial composition and gut inflammatory molecules correlated with neurobiological outcome in pups. This study must now be extended to female mice, since most, if not all, the parameters studied are sensitive to sex, and to increase its clinical relevance [74, 111,112,113].
We show that MIA reveals spatial memory deficits and hyper-locomotion behavior only when combined with low n-3 PUFA intake. This is contradictory to previous studies that showed a significant effect of MIA alone on behavior of adult mice, including learning and memory abilities [8, 114,115,116,117,118,119,120,121,122,123,124]. We however confirmed a previous report from our group in which n-3 PUFA deficiency induces memory deficits in MIA-exposed mice [28]. As a plausible explanation for this discrepancy, our control animals are fed with an n-3 sufficient diet, whose composition is distinct from standard chow (less MUFA, more PUFA and higher n-6/n-3 ratio in the standard chow vs n-3 sufficient diet) [125]. Moreover, the type and the dose of MIA-inducing agent, as well as the embryonic age of exposure, are also key for long-term behavioral deficits [8].
One cannot rule out that MIA-induced maternal care defects is a plausible cause for the long term deficits observed in the offspring. Indeed, it was previously shown that the adoption of control neonates by surrogate rearing mothers, previously exposed to MIA during pregnancy, is sufficient to trigger cognitive deficits in the fostered offspring [13, 109, 126,127,128,129]. Nonetheless, unlike other studies using a similar approach to ours, i.e., one single i.p. administration of LPS at E17 in mice, we could not find any major effects of MIA in n-3 sufficient mice, especially on memory and anxiety [11, 80, 82, 118, 130, 131]. This suggests intrinsic differences between standard chow-fed (as used in previous studies) and n-3 PUFA sufficient-fed mice and questions the underlying mechanisms. We previously showed that the brain fatty acid composition of mice fed either a standard or n-3 sufficient diet is quite similar [125]. However, the two diets vary in total saturated fat, monounsaturated, PUFAs, LA/ALA ratio, proteins, carbohydrates, and total lipids. Hence, aspects other than brain fatty acid composition are likely to explain differences between both groups, such as cell energy metabolism, lipid composition at the cellular resolution or production of lipid derivatives. This remains to be addressed.
We evaluated the effect of dietary n-3 PUFA deficiency combined with MIA on gut inflammation and microbiota composition, as a plausible mechanism underlying behavioral alterations. α-divesity was decreased by both interventions at PND14 and PND21. Similar observations were made in patients with neurodevelopmental diseases such as ADHD [132]. Of note, bacteria from the Prevotellaceae family were less abundant in n-3 deficient mice while Akkermansia was increased. While we must be cautious in making comparisons between human and mice findings regarding gut microbiota composition [133], similar differences have been observed between autistic children and controls of similar age [134, 135]. Moreover, increased levels of Prevotella following a fecal material transfer in autistic patients have been associated with improvements of autistic symptoms [136], while some studies report that Akkermansia levels are elevated in multiple sclerosis (MS) or Parkinson’s Disease patients’ [137,138,139]. We also observe an elevation of Enterobacteriaceae in n-3 deficient mice, which was similarly found to be increased in autistic children [140] and decreased after n-3 PUFA supplementation [141]. Our work is also in line with two studies demonstrating that maternal n-3 PUFA deficiency induces compositional and functional disturbances to the gut microbiome, closely associated with long term behavioral consequences in the offspring [142, 144].
We show for the first time that low maternal n-3 PUFA intake alone or combined to MIA alters gut structure and physiology during post-natal development in a time-dependent manner. Previous study reported altered intestinal permeability in the offspring in a poly(I:C) model of MIA [59]. Several studies reveal the impact of n-3 PUFAs on gut health (intestinal permeability and gut innervation) [143, 145,146,147,148,149,150]. The gut immune response, tightly related to gut permeability, was exacerbated in n-3 deficient mice at PND14, while at PND21, it was enhanced in n-3 sufficient mice. More studies are needed to understand whether and how the delay of response in n-3 sufficient mice explains their protection in terms of long-term cognitive abilities. A recent study highlighted the prominent role of T helper 17 (TH17)-derived IL-17A in neurodevelopmental abnormalities in the offspring of pregnant mothers undergoing MIA [61]. In our study, we observed a general overactivation of the gut inflammatory response in MIA-exposed offspring during CNS development. Interestingly, clinical studies report defects in gut permeability and inflammatory response in ASD and schizophrenic patients [60, 107, 133], suggesting that the double environmental insult recapitulates some aspects of these diseases.
At PND14, we found that levels of several members of the Lachnospiraceae family correlate with and myelin markers and markers of gut immune reactivity. Recent study highlighted, Ruminococcus Gnavus as a central player in Crohn’s disease. These bacteria have been shown to stimulate gut inflammation through the release of specific metabolites [150]. Lachnospiraceae is decreased in MS patients [151], who are known to exhibit an altered T-cell response together with alterations of the intestinal barrier permeability [152]. Contrary to our own data, Hsiao et al. showed that MIA increases Lachnospiraceae [59]. The discrepancy could result from different timelines of analysis: we analyzed microbiota composition in PND14-21 mice, while Hsiao et al. studied its composition after weaning. It could also be explained by the different MIA protocols used: bacterial at E17 vs viral mimetic at E12.5. At the genus level, we observed opposite variation of members of this family. Linking global Lachnospiraceae levels with biological outcomes appears to be inappropriate, as the family comprises of a large number of distinct bacteria. It could explain why a human study of associations between the levels of Lachnospiraceae and neurological diseases, such as depression, also found conflicting results [153].
N-3 PUFA deficiency exacerbated MIA-induced defects in microglia-neuron interactions, while microglial density, phenotype and inflammatory activity were unaffected in pups. This confirms most previous reports in which no effect of MIA on microglial density were ever observed [34, 116, 154,155,156,157,158]. We previously demonstrated that the proinflammatory cytokine expression is exacerbated in both maternal and embryonic brains of the n-3 deficient group [28], which is no longer the case at PND14. However, increased number of Iba1/PSD95 positive cells were measured in the hippocampus of n-3 deficient offspring at PND14, suggestive of synaptic pruning [29]. In line with these data, the hippocampal synaptic density was decreased at PND28. These findings reinforce our previous observations that early-life n-3 PUFA dietary deficiency alters post-natal microglia phenotype and phagocytic activity in the hippocampus [44, 77, 159]. However, while n-3 PUFA deficiency combined with MIA further increased Iba-1/PSD95 colocalization at PND14, at PND28 the spine density in this group was higher compared with that of saline-injected n-3 deficient mice. These data suggest that the regulation of spine density relies on microglia-independent mechanisms in the n-3 deficient/LPS mice. Microglial phagocytic capacity might be overridden in that context, or compensatory mechanisms are put in place between PND14 and PND28, leading to a significant increase in spine density. More experiments are required to test the functional state of the excess spines of n-3 deficient/LPS mice at PND28 and how it relates to behavioral deficits observed in these mice in adulthood. Our study also revealed an impact of n-3 PUFA deficiency and MIA on microglia-neuron crosstalk, confirming a previous report describing a correlation between spine density and CX3CR1 expression in the hippocampus of MIA-exposed mice [160]. The crucial pathways for this interaction are likely to be dysregulated in our experimental context (complement cascade, fractalkine pathway, CD47) [29, 30, 161]. This concurs with previous studies showing that n-3 PUFAs modulate spine density and microglial activity [20, 44, 77, 162,163,164].
In conclusion, our study is the first to examine potential mechanisms underlying the link between low n-3 PUFA intake and MIA, including interactions between enteric microbiota and the CNS. We uncover a correlative relationship between diet- and MIA-induced gut alterations and deleterious neurobiological outcomes. We also highlight the post-natal period as a vulnerable time window for perinatal dietary and immune stress. We finally demonstrate the long-lasting effect of these stressors, both at the transcriptional and behavioral levels. This work furthers our understanding of the link between MIA, poor nutritional habits and NDD, emphasising a potential role of the gut-brain axis.
Funding and disclosure
PG reports having received consulting fees from Chiesi Pharma AB. All other authors reported no biomedical financial interests or potential conflicts of interest. Funding for this research was provided by the Institut National pour la Recherche Agronomique, l’Alimentation et l’Environnement (INRAE), the Bordeaux Univ, the New Aquitania Region, NeurATRIS (Paris, France), the International Laboratory OptiNutriBrain, the Foundation for Medical Research (FRM) (DEQ20170336724), the French Foundation (FDF, #00070700). QL was supported by the Region Ile de France (PICRI, the Ceberal Palsy Foundation #13020605) and by the FRM, FD is supported by an Idex PhD grant, GB is supported by the French Ministry for Research and Higher Education, CL was supported by Idex grant, AQ and IV were supported by an Erasmus Mundus scholarship, ABB was supported by the Ecole Normale Supérieure (Lyon). TB, BM and PG were supported by Inserm, Université de Paris, Région Île-de-France (DIM Cerveau et Pensée, NeoPhen), Investissement d'Avenir (ANR-11-INBS-0011, NeurATRIS), ERA-NET Neuron (Micromet). The Western blot analyses were done in the Biochemistry and Biophysics Platform of the Bordeaux Neurocampus at the Bordeaux University funded by the LABEX BRAIN (ANR-10-LABX-43). This work benefited from the facilities and expertise of the imaging platform Imag'In (www.incia.u-bordeaux1.fr), which is supported by CNRS and Region Aquitaine and from the Bordeaux Imaging Center. The microscopy was done in the Bordeaux Imaging Center a service unit of the CNRS-INSERM and Bordeaux University, member of the national infrastructure France BioImaging supported by the French National Research Agency (ANR-10-INBS-04).
References
Thapar A, Cooper M, Rutter M. Neurodevelopmental disorders. Lancet Psychiatry. 2017;4:339–46.
Wallace R. Environmental induction of neurodevelopmental disorders. Bull Math Biol. 2016;78:2408–26.
Al-Haddad BJS, Jacobsson B, Chabra S, Modzelewska D, Olson EM, Bernier R, et al. Long-term risk of neuropsychiatric disease after exposure to infection in utero. JAMA Psychiatry. 2019;76:594–602.
Cormack BE, Harding JE, Miller SP, Bloomfield FH. The influence of early nutrition on brain growth and neurodevelopment in extremely preterm babies: a narrative review. Nutrients. 2019;11. https://doi.org/10.3390/nu11092029.
Georgieff MK, Ramel SE, Cusick SE. Nutritional influences on brain development. Acta Paediatr. 2018;107:1310–21.
Guma E, Plitman E, Chakravarty MM. The role of maternal immune activation in altering the neurodevelopmental trajectories of offspring: a translational review of neuroimaging studies with implications for autism spectrum disorder and schizophrenia. Neurosci Biobehav Rev. 2019;104:141–57.
Knuesel I, Chicha L, Britschgi M, Schobel SA, Bodmer M, Hellings JA, et al. Maternal immune activation and abnormal brain development across CNS disorders. Nat Rev Neurol. 2014;10:643–60.
Madore LeyrolleQ, Lacabanne C, Benmamar-Badel A, Joffre C, Nadjar A, Layé S. Neuroinflammation in autism: plausible role of maternal inflammation, dietary omega 3, and microbiota. Neural Plast. 2016;2016:3597209.
Bilbo SD, Block CL, Bolton JL, Hanamsagar R, Tran PK. Beyond infection – Maternal immune activation by environmental factors, microglial development, and relevance for autism spectrum disorders. Exp Neurol. 2018;299:241–51.
Bilbo SD, Schwarz JM. The immune system and developmental programming of brain and behavior. Front Neuroendocrinol. 2012;33:267–86.
Boksa P. Effects of prenatal infection on brain development and behavior: a review of findings from animal models. Brain Behav Immun. 2010;24:881–97.
Estes ML, McAllister AK. Immune mediators in the brain and peripheral tissues in autism spectrum disorder. Nat Rev Neurosci. 2015;16:469–86.
Meyer U, Nyffeler M, Yee BK, Knuesel I, Feldon J. Adult brain and behavioral pathological markers of prenatal immune challenge during early/middle and late fetal development in mice. Brain Behav Immun. 2008;22:469–86.
Missault S, Van den Eynde K, Vanden Berghe W, Fransen E, Weeren A, Timmermans JP, et al. The risk for behavioural deficits is determined by the maternal immune response to prenatal immune challenge in a neurodevelopmental model. Brain Behav Immun. 2014;42:138–46.
Reisinger S, Khan D, Kong E, Berger A, Pollak A, Pollak DD. The poly(I:C)-induced maternal immune activation model in preclinical neuropsychiatric drug discovery. Pharm Ther. 2015;149:213–26.
Bazinet RP, Layé S. Polyunsaturated fatty acids and their metabolites in brain function and disease. Nat Rev Neurosci. 2014;15:771–85.
Bolton JL, Bilbo SD. Developmental programming of brain and behavior by perinatal diet: focus on inflammatory mechanisms. Dialogues Clin Neurosci. 2014;16:307–20.
Bourre JM. Roles of unsaturated fatty acids (especially omega-3 fatty acids) in the brain at various ages and during ageing. J Nutr Health Aging. 2004;8:163–74.
Calderon F, Kim H-Y. Docosahexaenoic acid promotes neurite growth in hippocampal neurons. J Neurochem. 2004;90:979–88.
Cao D, Kevala K, Kim J, Moon H-S, Jun SB, Lovinger D, Kim H-Y. Docosahexaenoic acid promotes hippocampal neuronal development and synaptic function. J Neurochem. 2009;111:510–21.
Martins BP, Bandarra NM, Figueiredo-Braga M. The role of marine omega-3 in human neurodevelopment, including Autism Spectrum Disorders and Attention-Deficit/Hyperactivity Disorder - a review. Crit Rev Food Sci Nutr. 2020;60:1431–46.
Poduslo SE, Jang Y. Myelin development in infant brain. Neurochem Res. 1984;9:1615–26.
Salvati S, Attorri L, Avellino C, Di Biase A, Sanchez M. Diet, lipids and brain development. Dev Neurosci. 2000;22:481–7.
van Elst K, Bruining H, Birtoli B, Terreaux C, Buitelaar JK, Kas MJ. Food for thought: dietary changes in essential fatty acid ratios and the increase in autism spectrum disorders. Neurosci Biobehav Rev. 2014;45:369–78.
Yehuda S, Rabinovitz S, Mostofsky DI. Essential fatty acids and the brain: from infancy to aging. Neurobiol Aging. 2005;26 Suppl 1:98–102.
Innis SM. Fatty acids and early human development. Early Hum Dev. 2007;83:761–6.
Brown CM, Austin DW. Autistic disorder and phospholipids: a review. Prostaglandins Leukot Ess Fat Acids. 2011;84:25–30.
Labrousse VF, Leyrolle Q, Amadieu C, Aubert A, Sere A, Coutureau E, et al. Dietary omega-3 deficiency exacerbates inflammation and reveals spatial memory deficits in mice exposed to lipopolysaccharide during gestation. Brain Behav Immun. 2018;73:427–40.
Paolicelli RC, Bolasco G, Pagani F, Maggi L, Scianni M, Panzanelli P, et al. Synaptic pruning by microglia is necessary for normal brain development. Science. 2011;333:1456–8.
Schafer DP, Lehrman EK, Kautzman AG, Koyama R, Mardinly AR, Yamasaki R, et al. Microglia sculpt postnatal neural circuits in an activity and complement-dependent manner. Neuron. 2012;74:691–705.
Zhan Y, Paolicelli RC, Sforazzini F, Weinhard L, Bolasco G, Pagani F, et al. Deficient neuron-microglia signaling results in impaired functional brain connectivity and social behavior. Nat Neurosci. 2014;17:400–6.
Arnò B, Grassivaro F, Rossi C, Bergamaschi A, Castiglioni V, Furlan R, et al. Neural progenitor cells orchestrate microglia migration and positioning into the developing cortex. Nat Commun. 2014;5:5611.
Bialas AR, Stevens B. TGF-β signaling regulates neuronal C1q expression and developmental synaptic refinement. Nat Neurosci. 2013;16:1773–82.
Cunningham CL, Martínez-Cerdeño V, Noctor SC. Microglia regulate the number of neural precursor cells in the developing cerebral cortex. J Neurosci. 2013;33:4216–33.
Marín-Teva JL, Dusart I, Colin C, Gervais A, van Rooijen N, Mallat M. Microglia promote the death of developing Purkinje cells. Neuron. 2004;41:535–47.
Peri F, Nüsslein-Volhard C. Live imaging of neuronal degradation by microglia reveals a role for v0-ATPase a1 in phagosomal fusion in vivo. Cell. 2008;133:916–27.
Shigemoto-Mogami Y, Hoshikawa K, Goldman JE, Sekino Y, Sato K. Microglia enhance neurogenesis and oligodendrogenesis in the early postnatal subventricular zone. J Neurosci. 2014;34:2231–43.
Sierra A, Abiega O, Shahraz A, Neumann H. Janus-faced microglia: beneficial and detrimental consequences of microglial phagocytosis. Front Cell Neurosci. 2013;7:6.
Sierra A, Encinas JM, Deudero JJP, Chancey JH, Enikolopov G, Overstreet-Wadiche LS, et al. Microglia shape adult hippocampal neurogenesis through apoptosis-coupled phagocytosis. Cell Stem Cell. 2010;7:483–95.
Squarzoni P, Oller G, Hoeffel G, Pont-Lezica L, Rostaing P, Low D, et al. Microglia modulate wiring of the embryonic forebrain. Cell Rep. 2014;8:1271–9.
Swinnen N, Smolders S, Avila A, Notelaers K, Paesen R, Ameloot M, et al. Complex invasion pattern of the cerebral cortex bymicroglial cells during development of the mouse embryo. Glia. 2013;61:150–63.
Tremblay M-È, Lowery RL, Majewska AK. Microglial interactions with synapses are modulated by visual experience. PLoS Biol. 2010;8:e1000527.
Ueno M, Fujita Y, Tanaka T, Nakamura Y, Kikuta J, Ishii M, Yamashita T. Layer V cortical neurons require microglial support for survival during postnatal development. Nat Neurosci. 2013;16:543–51.
Madore, Leyrolle Q, Morel L, DelpechJC, Greenhalgh AD, Lacabanne C, et al. Essential omega-3 fatty acids tune microglial phagocytosis of synaptic elements in the developing brain. bioRxiv. 2019:744136.
Aoki Y, Yoncheva YN, Chen B, Nath T, Sharp D, Lazar M, et al. Association of white matter structure with autism spectrum disorder and attention-deficit/hyperactivity disorder. JAMA Psychiatry. 2017;74:1120–8.
Kochunov P, Coyle TR, Rowland LM, Jahanshad N, Thompson PM, Kelly S, et al. Association of white matter with core cognitive deficits in patients with schizophrenia. JAMA Psychiatry. 2017;74:958–66.
Kreitz S, Zambon A, Ronovsky M, Budinsky L, Helbich TH, Sideromenos S, et al. Maternal immune activation during pregnancy impacts on brain structure and function in the adult offspring. Brain Behav Immun. 2020;83:56–67.
Bernardo A, Giammarco ML, De Nuccio C, Ajmone-Cat MA, Visentin S, De Simone R, Minghetti L. Docosahexaenoic acid promotes oligodendrocyte differentiation via PPAR-γ signalling and prevents tumor necrosis factor-α-dependent maturational arrest. Biochim Biophys Acta Mol Cell Biol Lipids. 2017;1862:1013–23.
McNamara RK, Schurdak JD, Asch RH, Peters BD, Lindquist DM. Deficits in docosahexaenoic acid accrual during adolescence reduce rat forebrain white matter microstructural integrity: an in vivo diffusion tensor imaging study. Dev Neurosci. 2018;40:84–92.
Salvati S, Natali F, Attorri L, Di Benedetto R, Leonardi F, Di Biase A, et al. Eicosapentaenoic acid stimulates the expression of myelin proteins in rat brain. J Neurosci Res. 2008;86:776–84.
Tian C, Fan C, Liu X, Xu F, Qi K. Brain histological changes in young mice submitted to diets with different ratios of n-6/n-3 polyunsaturated fatty acids during maternal pregnancy and lactation. Clin Nutr. 2011;30:659–67.
Gu Y, Vorburger RS, Gazes Y, Habeck CG, Stern Y, Luchsinger JA, et al. White matter integrity as a mediator in the relationship between dietary nutrients and cognition in the elderly. Ann Neurol. 2016;79:1014–25.
McNamara RK, Szeszko PR, Smesny S, Ikuta T, DeRosse P, Vaz FM, et al. Polyunsaturated fatty acid biostatus, phospholipase A2 activity and brain white matter microstructure across adolescence. Neuroscience. 2017;343:423–33.
Peters BD, Voineskos AN, Szeszko PR, Lett TA, DeRosse P, Guha S, et al. Brain white matter development is associated with a human-specific haplotype increasing the synthesis of long chain fatty acids. J Neurosci. 2014;34:6367–76.
Peters BD, Ikuta T, DeRosse P, John M, Burdick KE, Gruner P, et al. Age-related differences in white matter tract microstructure are associated with cognitive performance from childhood to adulthood. Biol Psychiatry. 2014;75:248–56.
Peters BD, Machielsen MWJ, Hoen WP, Caan MWA, Malhotra AK, Szeszko PR, et al. Polyunsaturated fatty acid concentration predicts myelin integrity in early-phase psychosis. Schizophr Bull. 2013;39:830–8.
Peters BD, Duran M, Vlieger EJ, Majoie CB, den Heeten GJ, Linszen DH, de Haan L. Polyunsaturated fatty acids and brain white matter anisotropy in recent-onset schizophrenia: a preliminary study. Prostaglandins Leukot Ess Fat Acids. 2009;81:61–63.
Cryan JF, Dinan TG. Gut microbiota: microbiota and neuroimmune signalling-Metchnikoff to microglia. Nat Rev Gastroenterol Hepatol. 2015;12:494–6.
Hsiao EY, McBride SW, Hsien S, Sharon G, Hyde ER, McCue T, et al. Microbiota modulate behavioral and physiological abnormalities associated with neurodevelopmental disorders. Cell. 2013;155:1451–63.
Kelly JR, Minuto C, Cryan JF, Clarke G, Dinan TG. Cross talk: the microbiota and neurodevelopmental disorders. Front Neurosci. 2017;11:490.
Kim S, Kim H, Yim YS, Ha S, Atarashi K, Tan TG, et al. Maternal gut bacteria promote neurodevelopmental abnormalities in mouse offspring. Nature. 2017;549:528–32.
Finegold SM, Downes J, Summanen PH. Microbiology of regressive autism. Anaerobe. 2012;18:260–2.
Finegold SM, Dowd SE, Gontcharova V, Liu C, Henley KE, Wolcott RD, et al. Pyrosequencing study of fecal microflora of autistic and control children. Anaerobe. 2010;16:444–53.
Kang D-W, Ilhan ZE, Isern NG, Hoyt DW, Howsmon DP, Shaffer M, et al. Differences in fecal microbial metabolites and microbiota of children with autism spectrum disorders. Anaerobe. 2018;49:121–31.
Parracho HM, Bingham MO, Gibson GR, McCartney AL. Differences between the gut microflora of children with autistic spectrum disorders and that of healthy children. J Med Microbiol. 2005;54:987–91.
Wang L, Conlon MA, Christophersen CT, Sorich MJ, Angley MT. Gastrointestinal microbiota and metabolite biomarkers in children with autism spectrum disorders. Biomark Med. 2014;8:331–44.
Castro-Nallar E, Bendall ML, Pérez-Losada M, Sabuncyan S, Severance EG, Dickerson FB, et al. Composition, taxonomy and functional diversity of the oropharynx microbiome in individuals with schizophrenia and controls. PeerJ. 2015;3:e1140.
Cryan JF, O’Riordan KJ, Cowan CSM, Sandhu KV, Bastiaanssen TFS, Boehme M, et al. The microbiota-gut-brain axis. Physiol Rev. 2019;99:1877–2013.
Erny D, Hrabě de Angelis AL, Jaitin D, Wieghofer P, Staszewski O, David E, et al. Host microbiota constantly control maturation and function of microglia in the CNS. Nat Neurosci. 2015;18:965–77.
Gacias M, Gaspari S, Santos P-MG, Tamburini S, Andrade M, Zhang F, et al. (2016): Microbiota-driven transcriptional changes in prefrontal cortex override genetic differences in social behavior. Elife 5. 10.7554/eLife.13442
Hoban AE, Stilling RM, Ryan FJ, Shanahan F, Dinan TG, Claesson MJ, et al. Regulation of prefrontal cortex myelination by the microbiota. Transl Psychiatry. 2016;6:e774.
Lu J, Lu L, Yu Y, Cluette-Brown J, Martin CR, Claud EC. Effects of intestinal microbiota on brain development in humanized gnotobiotic mice. Sci Rep. 2018;8:5443.
Ntranos A, Casaccia P. The microbiome-gut-behavior axis: crosstalk between the gut microbiome and oligodendrocytes modulates behavioral responses. Neurotherapeutics. 2018;15:31–35.
Thion MS, Low D, Silvin A, Chen J, Grisel P, Schulte-Schrepping J, et al. Microbiome influences prenatal and adult microglia in a sex-specific manner. Cell. 2018;172:500. e16
Delpech J-C, Thomazeau A, Madore C, Bosch-Bouju C, Larrieu T, Lacabanne C, et al. Dietary n-3 PUFAs deficiency increases vulnerability to inflammation-induced spatial memory impairment. Neuropsychopharmacology. 2015;40:2774–87.
Lafourcade M, Larrieu T, Mato S, Duffaud A, Sepers M, Matias I, et al. Nutritional omega-3 deficiency abolishes endocannabinoid-mediated neuronal functions. Nat Neurosci. 2011;14:345–50.
Madore NadjarA, Delpech J-C, Sere A, Aubert A, Portal C, et al. Nutritional n-3 PUFAs deficiency during perinatal periods alters brain innate immune system and neuronal plasticity-associated genes. Brain Behav Immun. 2014;41:22–31.
Mingam R, Moranis A, Bluthé R-M, De Smedt-Peyrusse V, Kelley KW, Guesnet P, et al. Uncoupling of interleukin-6 from its signalling pathway by dietary n-3-polyunsaturated fatty acid deprivation alters sickness behaviour in mice. Eur J Neurosci. 2008;28:1877–86.
Moranis A, Delpech J-C, De Smedt-Peyrusse V, Aubert A, Guesnet P, Lavialle M, et al. Long term adequate n-3 polyunsaturated fatty acid diet protects from depressive-like behavior but not from working memory disruption and brain cytokine expression in aged mice. Brain Behav Immun. 2012;26:721–31.
Golan HM, Lev V, Hallak M, Sorokin Y, Huleihel M. Specific neurodevelopmental damage in mice offspring following maternal inflammation during pregnancy. Neuropharmacology. 2005;48:903–17.
Roumier A, Pascual O, Béchade C, Wakselman S, Poncer J-C, Réal E, et al. Prenatal activation of microglia induces delayed impairment of glutamatergic synaptic function. PLoS ONE. 2008;3:e2595.
Kentner AC, Bilbo SD, Brown AS, Hsiao EY, McAllister AK, Meyer U, et al. Maternal immune activation: reporting guidelines to improve the rigor, reproducibility, and transparency of the model. Neuropsychopharmacology. 2019;44:245–58.
Yavas E, Gonzalez S, Fanselow MS. Interactions between the hippocampus, prefrontal cortex, and amygdala support complex learning and memory. 2019;F1000Res 8. https://doi.org/10.12688/f1000research.19317.1.
Bult C. Mouse genome database (MGD) 2019. Nucleic Acids Res. 2019;D801–D806. https://doi.org/10.1093/nar/gky1056.
Neniskyte U, Gross CT. Errant gardeners: glial-cell-dependent synaptic pruning and neurodevelopmental disorders. Nat Rev Neurosci. 2017;18:658–70.
Semple BD, Blomgren K, Gimlin K, Ferriero DM, Noble-Haeusslein LJ. Brain development in rodents and humans: Identifying benchmarks of maturation and vulnerability to injury across species. Prog Neurobiol. 2013;106–107:1–16.
Chhor V, Le Charpentier T, Lebon S, Oré M-V, Celador IL, Josserand J, et al. Characterization of phenotype markers and neuronotoxic potential of polarised primary microglia in vitro. Brain Behav Immun. 2013;32:70–85.
Aatsinki A-K, Lahti L, Uusitupa H-M, Munukka E, Keskitalo A, Nolvi S, et al. Gut microbiota composition is associated with temperament traits in infants. Brain Behav Immun. 2019;80:849–58.
Arentsen T, Raith H, Qian Y, Forssberg H, Diaz Heijtz R. Host microbiota modulates development of social preference in mice. Micro Ecol Health Dis. 2015;26:29719.
Buffington SA, Di Prisco GV, Auchtung TA, Ajami NJ, Petrosino JF, Costa-Mattioli M. Microbial reconstitution reverses maternal diet-induced social and synaptic deficits in offspring. Cell. 2016;165:1762–75.
Carlson AL, Xia K, Azcarate-Peril MA, Goldman BD, Ahn M, Styner MA, et al. Infant gut microbiome associated with cognitive development. Biol Psychiatry. 2018;83:148–59.
Christian LM, Galley JD, Hade EM, Schoppe-Sullivan S, Kamp Dush C, Bailey MT. Gut microbiome composition is associated with temperament during early childhood. Brain Behav Immun. 2015;45:118–27.
Chu C, Murdock MH, Jing D, Won TH, Chung H, Kressel AM, et al. The microbiota regulate neuronal function and fear extinction learning. Nature. 2019;574:543–8.
Cowan CSM, Dinan TG, Cryan JF. Annual Research Review: Critical windows - the microbiota-gut-brain axis in neurocognitive development. J Child Psychol Psychiatry. 2019. https://doi.org/10.1111/jcpp.13156.
Desbonnet L, Clarke G, Shanahan F, Dinan TG, Cryan JF. Microbiota is essential for social development in the mouse. Mol Psychiatry. 2014;19:146–8.
Gao W, Salzwedel AP, Carlson AL, Xia K, Azcarate-Peril MA, Styner MA, et al. Gut microbiome and brain functional connectivity in infants-a preliminary study focusing on the amygdala. Psychopharmacol. 2019;236:1641–51.
Gareau MG, Wine E, Rodrigues DM, Cho JH, Whary MT, Philpott DJ, et al. Bacterial infection causes stress-induced memory dysfunction in mice. Gut. 2011;60:307–17.
Hoban AE, Stilling RM, Moloney G, Shanahan F, Dinan TG, Clarke G, Cryan JF. The microbiome regulates amygdala-dependent fear recall. Mol Psychiatry. 2018;23:1134–44.
Luczynski P, Whelan SO, O’Sullivan C, Clarke G, Shanahan F, Dinan TG, Cryan JF. Adult microbiota-deficient mice have distinct dendritic morphological changes: differential effects in the amygdala and hippocampus. Eur J Neurosci. 2016;44:2654–66.
Luk B, Veeraragavan S, Engevik M, Balderas M, Major A, Runge J, et al. Postnatal colonization with human “infant-type” Bifidobacterium species alters behavior of adult gnotobiotic mice. PLoS ONE. 2018;13:e0196510.
Ong IM, Gonzalez JG, McIlwain SJ, Sawin EA, Schoen AJ, Adluru N, et al. Gut microbiome populations are associated with structure-specific changes in white matter architecture. Transl Psychiatry. 2018;8:6.
Provensi G, Schmidt SD, Boehme M, Bastiaanssen TFS, Rani B, Costa A, et al. Preventing adolescent stress-induced cognitive and microbiome changes by diet. Proc Natl Acad Sci USA. 2019;116:9644–51.
Sgritta M, Dooling SW, Buffington SA, Momin EN, Francis MB, Britton RA, Costa-Mattioli M. Mechanisms underlying microbial-mediated changes in social behavior in mouse models of autism spectrum disorder. Neuron. 2019;101:246. e6
Sherwin E, Bordenstein SR, Quinn JL, Dinan TG, Cryan JF. Microbiota and the social brain. Science 2019;366. https://doi.org/10.1126/science.aar2016.
Stilling RM, Moloney GM, Ryan FJ, Hoban AE, Bastiaanssen TF, Shanahan F, et al. Social interaction-induced activation of RNA splicing in the amygdala of microbiome-deficient mice. Elife 2018;7. https://doi.org/10.7554/eLife.33070.
Tillisch K, Mayer EA, Gupta A, Gill Z, Brazeilles R, Le Nevé B, et al. Brain structure and response to emotional stimuli as related to gut microbial profiles in healthy women. Psychosom Med. 2017;79:905–13.
Vuong HE, Hsiao EY. Emerging roles for the gut microbiome in autism spectrum disorder. Biol Psychiatry. 2017;81:411–23.
Turner JR. Intestinal mucosal barrier function in health and disease. Nat Rev Immunol. 2009;9:799–809.
Careaga M, Murai T, Bauman MD. Maternal immune activation and autism spectrum disorder: from rodents to nonhuman and human primates. Biol Psychiatry. 2017;81:391–401.
Meyer U, Feldon J, Fatemi SH. In-vivo rodent models for the experimental investigation of prenatal immune activation effects in neurodevelopmental brain disorders. Neurosci Biobehav Rev. 2009;33:1061–79.
Villa A, Gelosa P, Castiglioni L, Cimino M, Rizzi N, Pepe G, et al. Sex-specific features of microglia from adult mice. Cell Rep. 2018;23:3501–11.
Morris A. Microbiota drives sex-specific differences. Nat Rev Endocrinol. 2018;15:4.
Darling JS, Daniel JM. Pubertal hormones mediate sex differences in levels of myelin basic protein in the orbitofrontal cortex of adult rats. Neuroscience. 2019;406:487–95.
Batinić B, Santrač A, Divović B, Timić T, Stanković T, Obradović AL, et al. Lipopolysaccharide exposure during late embryogenesis results in diminished locomotor activity and amphetamine response in females and spatial cognition impairment in males in adult, but not adolescent rat offspring. Behav Brain Res. 2016;299:72–80.
Bauman MD, Iosif A-M, Smith SEP, Bregere C, Amaral DG, Patterson PH. Activation of the maternal immune system during pregnancy alters behavioral development of rhesus monkey offspring. Biol Psychiatry. 2014;75:332–41.
Ben-Yehuda H, Matcovitch-Natan O, Kertser A, Spinrad A, Prinz M, Amit I, Schwartz M. Maternal Type-I interferon signaling adversely affects the microglia and the behavior of the offspring accompanied by increased sensitivity to stress. Mol Psychiatry. 2019. https://doi.org/10.1038/s41380-019-0604-0.
Fortier M-E, Luheshi GN, Boksa P. Effects of prenatal infection on prepulse inhibition in the rat depend on the nature of the infectious agent and the stage of pregnancy. Behav Brain Res. 2007;181:270–7.
Hava G, Vered L, Yael M, Mordechai H, Mahoud H. Alterations in behavior in adult offspring mice following maternal inflammation during pregnancy. Dev Psychobiol. 2006;48:162–8.
Kirsten TB, Taricano M, Maiorka PC, Palermo-Neto J, Bernardi MM. Prenatal lipopolysaccharide reduces social behavior in male offspring. Neuroimmunomodulation. 2010;17:240–51.
Li X-Y, Wang F, Chen G-H, Li X-W, Yang Q-G, Cao L, Yan W-W. Inflammatory insult during pregnancy accelerates age-related behavioral and neurobiochemical changes in CD-1 mice. Age (Dordr). 2016;38:59.
Machado CJ, Whitaker AM, Smith SEP, Patterson PH, Bauman MD. Maternal immune activation in nonhuman primates alters social attention in juvenile offspring. Biol Psychiatry. 2015;77:823–32.
Malkova NV, Yu CZ, Hsiao EY, Moore MJ, Patterson PH. Maternal immune activation yields offspring displaying mouse versions of the three core symptoms of autism. Brain Behav Immun. 2012;26:607–16.
Solek CM, Farooqi N, Verly M, Lim TK, Ruthazer ES. Maternal immune activation in neurodevelopmental disorders. Dev Dyn. 2018;247:588–619.
Wu Z-X, Cao L, Li X-W, Jiang W, Li X-Y, Xu J, et al. Accelerated deficits of spatial learning and memory resulting from prenatal inflammatory insult are correlated with abnormal phosphorylation and methylation of histone 3 in CD-1 mice. Front Aging Neurosci. 2019;11:114.
Joffre C, Grégoire S, De Smedt V, Acar N, Bretillon L, Nadjar A, Layé S. Modulation of brain PUFA content in different experimental models of mice. Prostaglandins Leukot Ess Fat Acids. 2016;114:1–10.
Meyer U, Nyffeler M, Schwendener S, Knuesel I, Yee BK, Feldon J. Relative prenatal and postnatal maternal contributions to schizophrenia-related neurochemical dysfunction after in utero immune challenge. Neuropsychopharmacology. 2008;33:441–56.
Meyer U, Schwendener S, Feldon J, Yee BK. Prenatal and postnatal maternal contributions in the infection model of schizophrenia. Exp Brain Res. 2006;173:243–57.
Schwendener S, Meyer U, Feldon J. Deficient maternal care resulting from immunological stress during pregnancy is associated with a sex-dependent enhancement of conditioned fear in the offspring. J Neurodev Disord. 2009;1:15–32.
Richetto J, Calabrese F, Meyer U, Riva MA. Prenatal versus postnatal maternal factors in the development of infection-induced working memory impairments in mice. Brain Behav Immun. 2013;33:190–200.
Golan H, Stilman M, Lev V, Huleihel M. Normal aging of offspring mice of mothers with induced inflammation during pregnancy. Neuroscience. 2006;141:1909–18.
Ning H, Wang H, Zhao L, Zhang C, Li X-Y, Chen Y-H, Xu D-X. Maternally-administered lipopolysaccharide (LPS) increases tumor necrosis factor alpha in fetal liver and fetal brain: Its suppression by low-dose LPS pretreatment. Toxicol Lett. 2008;176:13–19.
Prehn-Kristensen A, Zimmermann A, Tittmann L, Lieb W, Schreiber S, Baving L, Fischer A. Reduced microbiome alpha diversity in young patients with ADHD. PLoS ONE. 2018;13:e0200728.
Nguyen TT, Kosciolek T, Maldonado Y, Daly RE, Martin AS, McDonald D, et al. Differences in gut microbiome composition between persons with chronic schizophrenia and healthy comparison subjects. Schizophr Res. 2019;204:23–29.
Kang D-W, Park JG, Ilhan ZE, Wallstrom G, Labaer J, Adams JB, Krajmalnik-Brown R. Reduced incidence of prevotella and other fermenters in intestinal microflora of autistic children. PLoS ONE. 2013;8:e68322.
Pulikkan J, Maji A, Dhakan DB, Saxena R, Mohan B, Anto MM, et al. Gut microbial dysbiosis in indian children with autism spectrum disorders. Micro Ecol. 2018;76:1102–14.
Kang D-W, Adams JB, Coleman DM, Pollard EL, Maldonado J, McDonough-Means S, et al. Long-term benefit of Microbiota Transfer Therapy on autism symptoms and gut microbiota. Sci Rep. 2019;9:5821.
Gerhardt S, Mohajeri MH. Changes of Colonic Bacterial Composition in Parkinson’s Disease and Other Neurodegenerative Diseases. Nutrients. 2018;10. https://doi.org/10.3390/nu10060708.
Jangi S, Gandhi R, Cox LM, Li N, von Glehn F, Yan R, et al. Alterations of the human gut microbiome in multiple sclerosis. Nat Commun. 2016;7:12015.
Pröbstel A-K, Baranzini SE. The role of the gut microbiome in multiple sclerosis risk and progression: towards characterization of the “MS Microbiome.”. Neurotherapeutics. 2018;15:126–34.
Coretti L, Paparo L, Riccio MP, Amato F, Cuomo M, Natale A, et al. Gut microbiota features in young children with autism spectrum disorders. Front Microbiol. 2018;9:3146.
Ghosh S, Molcan E, DeCoffe D, Dai C, Gibson DL. Diets rich in n-6 PUFA induce intestinal microbial dysbiosis in aged mice. Br J Nutr. 2013;110:515–23.
Robertson RC, Seira Oriach C, Murphy K, Moloney GM, Cryan JF, Dinan TG, et al. Omega-3 polyunsaturated fatty acids critically regulate behaviour and gut microbiota development in adolescence and adulthood. Brain Behav Immun. 2017;59:21–37.
De Quelen F, Chevalier J, Rolli-Derkinderen M, Mourot J, Neunlist M, Boudry G. n-3 polyunsaturated fatty acids in the maternal diet modify the postnatal development of nervous regulation of intestinal permeability in piglets. J Physiol. 2011;589:4341–52.
Robertson RC, Oriach CS, Murphy K, Moloney GM, Cryan JF, Dinan TG, et al. Deficiency of essential dietary n-3 PUFA disrupts the caecal microbiome and metabolome in mice. Br J Nutr. 2017;118:959–70.
Desaldeleer C, Ferret-Bernard S, de Quelen F, Le Normand L, Perrier C, Savary G, et al. Maternal 18:3n-3 favors piglet intestinal passage of LPS and promotes intestinal anti-inflammatory response to this bacterial ligand. J Nutr Biochem. 2014;25:1090–8.
Innis SM, Dai C, Wu X, Buchan AMJ, Jacobson K. Perinatal lipid nutrition alters early intestinal development and programs the response to experimental colitis in young adult rats. Am J Physiol Gastrointest Liver Physiol. 2010;299:G1376–1385.
Kaliannan K, Wang B, Li X-Y, Kim K-J, Kang JX. A host-microbiome interaction mediates the opposing effects of omega-6 and omega-3 fatty acids on metabolic endotoxemia. Sci Rep. 2015;5:11276.
Coquenlorge S, Van Landeghem L, Jaulin J, Cenac N, Vergnolle N, Duchalais E, et al. The arachidonic acid metabolite 11β-ProstaglandinF2α controls intestinal epithelial healing: deficiency in patients with Crohn’s disease. Sci Rep. 2016;6:25203.
Pochard C, Coquenlorge S, Jaulin J, Cenac N, Vergnolle N, Meurette G, et al. Defects in 15-HETE production and control of epithelial permeability by human enteric glial cells from patients with crohn’s disease. Gastroenterology. 2016;150:168–80.
Henke MT, Kenny DJ, Cassilly CD, Vlamakis H, Xavier RJ, Clardy J. Ruminococcus gnavus, a member of the human gut microbiome associated with Crohn’s disease, produces an inflammatory polysaccharide. Proc Natl Acad Sci USA. 2019;116:12672–7.
Tremlett H, Fadrosh DW, Faruqi AA, Hart J, Roalstad S, Graves J, et al. Gut microbiota composition and relapse risk in pediatric MS: a pilot study. J Neurol Sci. 2016;363:153–7.
Buscarinu MC, Fornasiero A, Romano S, Ferraldeschi M, Mechelli R, Reniè R, et al. The contribution of gut barrier changes to multiple sclerosis pathophysiology. Front Immunol. 2019;10:1916.
Cheung SG, Goldenthal AR, Uhlemann A-C, Mann JJ, Miller JM, Sublette ME. Systematic review of gut microbiota and major depression. Front Psychiatry. 2019;10:34.
Giovanoli S, Weber-Stadlbauer U, Schedlowski M, Meyer U, Engler H. Prenatal immune activation causes hippocampal synaptic deficits in the absence of overt microglia anomalies. Brain Behav Immun. 2016;55:25–38.
Giovanoli S, Notter T, Richetto J, Labouesse MA, Vuillermot S, Riva MA, Meyer U. Late prenatal immune activation causes hippocampal deficits in the absence of persistent inflammation across aging. J Neuroinflammation. 2015;12:221.
Mattei D, Djodari-Irani A, Hadar R, Pelz A, de Cossío LF, Goetz T, et al. Minocycline rescues decrease in neurogenesis, increase in microglia cytokines and deficits in sensorimotor gating in an animal model of schizophrenia. Brain Behav Immun. 2014;38:175–84.
Paylor JW, Lins BR, Greba Q, Moen N, de Moraes RS, Howland JG, Winship IR. Developmental disruption of perineuronal nets in the medial prefrontal cortex after maternal immune activation. Sci Rep. 2016;6:37580.
Smolders S, Smolders SMT, Swinnen N, Gärtner A, Rigo J-M, Legendre P, Brône B. Maternal immune activation evoked by polyinosinic:polycytidylic acid does not evoke microglial cell activation in the embryo. Front Cell Neurosci. 2015;9:301.
Rey C, Nadjar A, Joffre F, Amadieu C, Aubert A, Vaysse C, et al. Maternal n-3 polyunsaturated fatty acid dietary supply modulates microglia lipid content in the offspring. Prostaglandins Leukot Ess Fat Acids. 2018;133:1–7.
Fernández de Cossío L, Guzmán A, van der Veldt S, Luheshi GN. Prenatal infection leads to ASD-like behavior and altered synaptic pruning in the mouse offspring. Brain Behav Immun. 2017;63:88–98.
Lehrman EK, Wilton DK, Litvina EY, Welsh CA, Chang ST, Frouin A, et al. CD47 protects synapses from excess microglia-mediated pruning during development. Neuron. 2018;100:120–34. e6
Chang PK-Y, Khatchadourian A, McKinney RA, Maysinger D. Docosahexaenoic acid (DHA): a modulator of microglia activity and dendritic spine morphology. J Neuroinflammation. 2015;12:34.
Chen X, Wu S, Chen C, Xie B, Fang Z, Hu W, et al. Omega-3 polyunsaturated fatty acid supplementation attenuates microglial-induced inflammation by inhibiting the HMGB1/TLR4/NF-κB pathway following experimental traumatic brain injury. J Neuroinflammation. 2017;14. https://doi.org/10.1186/s12974-017-0917-3.
McNamara RK, Vannest JJ, Valentine CJ. Role of perinatal long-chain omega-3 fatty acids in cortical circuit maturation: Mechanisms and implications for psychopathology. World J Psychiatry. 2015;5:15–34.
Acknowledgements
We thank Atika Zouine and Vincent Pitard for technical assistance at the Flow cytometry facility, CNRS UMS 3427, INSERM US 005, Univ. Bordeaux, F-33000 Bordeaux, France. We also thank Christel Poujol, Sébastien Marais, Fabrice Cordelières, Jérémie Teillon, Magali Mondin, Monica Fernandez-Monreal who help for all the experiment of microscopy as well as Franck Letourneur and Sébastien Jacques, from the Genom’ic platform (Institut Cochin, Paris, France) who performed microarray experiments. We finally thank the animal facility for taking care of and providing the animals that were necessary to perform the experiments.
Author information
Authors and Affiliations
Contributions
QL, FD, ARAAQ, IV, CL, ANB, JB, AA, AS, FC, LS, BM, TB, SG, JMC performed all animal experimentations. SG, CJ, and LB performed and analyzed lipid experiments on whole hippocampus. BM and TB performed physiological and behavioral measurements on neonates. GB performed and UR and PT oversaw bioinformatic analyses of transcriptomic data. CA performed correlation analyses. FG performed microbiota analyses. JMC and FC performed gut measurements. SL and AN equally supervised the entire project and wrote the manuscript. All authors proof-read the manuscript.
Corresponding authors
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Leyrolle, Q., Decoeur, F., Briere, G. et al. Maternal dietary omega-3 deficiency worsens the deleterious effects of prenatal inflammation on the gut-brain axis in the offspring across lifetime. Neuropsychopharmacol. 46, 579–602 (2021). https://doi.org/10.1038/s41386-020-00793-7
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41386-020-00793-7