Abstract
Generalization of conditioned fear is adaptive in some situations but maladaptive when fear excessively generalizes to innocuous stimuli with incidental resemblance to a genuine threat cue. Recently, empirical interest in fear generalization as a transdiagnostic explanatory mechanism underlying anxiety-related disorders has accelerated. As there are now several studies of fear generalization across multiple types of anxiety-related disorders, the authors conducted a meta-analysis of studies reporting behavioral measures (subjective ratings and psychophysiological indices) of fear generalization in anxiety-related disorder vs. comparison groups. We conducted systematic searches of electronic databases (conducted from January–October 2020) for fear generalization studies involving anxiety-related disorder groups or subclinical analog groups. A total of 300 records were full-text screened and two unpublished datasets were obtained, yielding 16 studies reporting behavioral fear generalization measures. Random-effects meta-analytic models and meta-regressions were applied to the identified data. Fear generalization was significantly heightened in anxiety-related disorder participants (N = 439) relative to comparison participants (N = 428). We did not identify any significant clinical, sample, or methodological moderators. Heightened fear generalization is quantitatively supported as distinguishing anxiety-related disorder groups from comparison groups. Evidence suggests this effect is transdiagnostic, relatively robust to experimental or sample parameters, and that generalization paradigms are a well-supported framework for neurobehavioral investigations of learning and emotion in anxiety-related disorders. We discuss these findings in the context of prior fear conditioning meta-analyses, past neuroimaging investigations of fear generalization in anxiety-related disorders, and future directions and challenges for the field.
Similar content being viewed by others
Introduction
Animals, including humans, rarely reencounter the exact same threat, and therefore generalizing from prior threatening encounters is crucial for survival. For example, a soldier who encountered an explosion while in a military convoy might display increased readiness and high sensitivity for threat detection when in similar convoys in the future. However, overly broad threat generalization can hinder adaptive functioning when it promotes fear to stimuli or situations that are largely safe. For example, a veteran who witnessed a roadside bomb in a warzone might feel vigilant and severely anxious while stuck in traffic back home, symptoms characteristic of posttraumatic stress disorder (PTSD). Maladaptive generalization of learned fear is a core clinical feature in anxiety-related disorders, which are among the most common and debilitating of psychopathologies [1, 2]. Although empirical demonstration of this clinically-relevant process dates back to the beginning of the previous century [3, 4], later research efforts on stimulus generalization shifted almost entirely toward appetitive instrumental conditioning paradigms. A recent reemergence of empirical fear generalization research in laboratory animals and humans is due in large part to the continued relevance of conditioning-based models for the understanding and treatment of anxiety-related disorders [5,6,7], and recent research in clinical populations provides preliminary evidence that overly broad behavioral (e.g., self-report ratings, psychophysiology) and neural generalization to an array of harmless stimuli is related to these psychopathologies [8, 9]. Yet, to date, the amount of empirical focus on fear generalization pales in comparison to research using other fear conditioning paradigms, such as extinction [6, 10, 11].
Neuroscience investigations into fear generalization in healthy populations serve as a foundation for understanding the emergence of increased generalization in clinical populations and provide avenues for potential treatment targets [5, 8, 12]. One mechanistic account of fear generalization, for example, centers on the role of the hippocampus in pattern separation of similar but discrete experiences. Specifically, intense stress can compromise the hippocampus’ ability to pattern separate, which in turn hinders discrimination of threat from safety and thus contributes to excessive generalization [13]. This indicates a possible target for intervention: addressing hippocampal dysfunction to limit fear generalization. A recent comprehensive model, inspired in part by LeDoux’s “low road” hypothesis of threat processing [14], centers on the role of subcortical (e.g., thalamic, amygdala, locus coeruleus) responses to stimuli that resemble a learned threat triggering pattern completion processes in the hippocampus [15]. When coupled with impaired prefrontal inhibitory regulation, rapid threat detection along with pattern completion are proposed to lead to heightened generalization in anxiety-related disorders.
Importantly, neural models of pathological generalization are built almost entirely on pre-clinical animal models and knowledge of the symptomatology of various anxiety-related disorders—not on direct tests in anxiety-related disorder samples [9]. Put another way, current mechanistic models of fear generalization in anxiety-related disorders put the theoretical cart in front of the empirical horse. Fundamental assumptions that heightened fear generalization is a marker of anxiety-related disorders will benefit from systematic meta-analyses and reviews of empirical work linking fear generalization to neuropathophysiology. Such evidence could further propel the use of the fear generalization paradigm, as well as behavioral generalization as a viable treatment target, in a manner similar to the widespread use of fear extinction as both an experimental paradigm and explanatory construct for poor retention of corrective information in exposure-based therapy [10, 11].
Central to efforts to map the etiology and pathophysiology of anxiety-related disorders are laboratory tasks that probe pathogenic mechanisms of fear and anxiety behavior and biology [16]. Differential fear conditioning remains the most common laboratory protocol to measure fear-based processes in humans. In the acquisition phase, one neutral stimulus (CS+), such as a simple shape or sound, is paired with an aversive unconditioned stimulus (US), such as an uncomfortable electric shock, while another neutral stimulus is never paired with the US (CS−). Whereas extinction training presents the CS+ in the absence of the US, fear generalization tests introduce generalization stimuli (GS), which typically include several stimuli that vary in perceptual or conceptual similarity to the CS+ and are never paired with the US (see Fig. 1 for example illustrations). A practical benefit to generalization tests includes the ability to rapidly assess the effects of acquisition on subsequent learning and behavior. In contrast, deficits in extinction training between clinical and healthy populations are frequently identified only after a delay (between-session) during an extinction-recall test [17], although this can depend on the specific disorder [18,19,20]. Generalization tests are also likely better approximations of the clinical reality of anxiety pathology than simple differential paradigms [21, 22]. Those with anxiety-related disorders rarely, if ever, encounter the exact same threatening stimulus that previously frightened or traumatized them, nor one that always guarantees safety—the experience of living with pathological anxiety is much more uncertain and complex [23]. Fear generalization offers a compelling framework for going beyond basic differential conditioning to understand pathological maladaptation in anxiety-related disorders. Given there are a growing number of studies of fear generalization in anxiety populations and conditioning work remains relevant to advances in exposure therapies for clinical anxiety [10, 24, 25], a meta-analysis of this work is warranted.
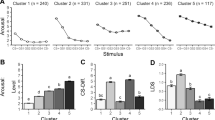
A Successful discrimination between CS+ and CS− vs. poorer discrimination, meta-analytically observed in anxiety-related disorders (Duits et al. [26]). B Successful extinction, in which conditioned responses diminish, vs. poorer extinction, in which CS+ remains elevated, meta-analytically observed in anxiety-related disorders. C Generalization test, in which generalization stimuli (GSs, white points) that parametrically differ in similarity from the CS+ (red points) are presented with hypothetical response slopes. Conditioned responses typically diminish as a function of similarity to the CS+ in a curvilinear (i.e., quadratic) fashion—proposed to be characteristic of psychiatrically normative/non-anxiety groups (bottommost slope). Heightened generalization (also referred to as overgeneralization, middle slope) involves relatively increased responding to GSs—proposed to be linked to anxiety-related disorders. Monotonic responding (topmost slope) represents a failure to discriminate between stimuli—not considered a form of stimulus generalization. Abbreviations: CS+ conditioned threat cue, CS− conditioned safety cue, GS generalization stimuli, US unconditioned stimulus.
The current meta-analysis
For fear generalization to transition from a specialty technique within the conditioning field to a widely recognized experimental paradigm for clinical research requires quantitative confirmation that heightened fear generalization is a consistent marker of anxiety psychopathology. Here, we present a meta-analysis of fear generalization in anxiety-related disorders. Prior meta-analytic reports of differential fear conditioning in anxiety-related disorders identified increased CS- responding during acquisition [26, 27], consistent, but not synonymous, with generalization to an unpaired cue. Prior reviews of fear generalization have not been quantitative [8, 28] or are of continuous anxiety-related traits and excluded clinical samples [29]. Overall, the relation between heightened fear generalization and pathological anxiety remains unclear.
Our primary aim is to test group differences between anxiety-related disorder and comparison groups on behavioral measures of fear generalization. We test standard group differences as a broad assessment of the overall effect size, which includes all identified studies. In a separate analysis, we test group differences in quadratic effects (i.e., quadratic contrast interactions testing curvilinear gradients of generalization that decrease from the CS+ to the CS−, with less curved gradients implicated as related to anxiety-related disorders), which are proposed as a more sensitive measure of heightened generalization [9] but are not analyzed in all studies. We predict that anxiety-related disorder groups will demonstrate heightened fear generalization relative to comparison groups and that this effect will not be contingent on a particular disorder or experimental design parameter [30]. We also evaluate differences in design and study quality and test their influence on generalization differences.
Methods and materials
The current effort’s methodology aligns with prior meta-analyses of fear conditioning and anxiety [26, 27, 29]. We preregistered (PROPSERO: CRD42021234718) and materials and data are accessible at osf.io/89gjr.
Search and selection strategy
English-language records were selected through a systematic search of PubMed, PsycINFO, Embase, and OpenGrey (conducted January–October 2020) with a combination of terms related to conditioning (e.g., conditioning), fear (e.g., fear/Pavlovian/classical), and anxiety-related disorders (e.g., panic/phobi*). Table ST1 provides the complete search strategies. In addition, SEC contacted several fear generalization experts to request data from potentially unpublished studies. Studies were included when they tested conditioned generalization among individuals with clinical or subclinical/sub-threshold anxiety-related disorders (i.e., PTSD, generalized anxiety disorder (GAD), panic disorder (PD), social anxiety disorder (SAD), specific phobia (SP), or obsessive-compulsive disorder (OCD)) relative to comparison groups without (subclinical/sub-threshold levels of) anxiety-related disorders. Of note is that both PTSD and OCD have been removed from the Anxiety Disorder category for DSM-5 [31]. Because conditioned fear generalization is clearly a clinical component of PTSD and OCD [18, 20], they were included in our analysis and collectively referred to as anxiety-related disorders [32]. We did not include studies that only reported analyses of continuous anxiety traits in relation to fear generalization. We only extracted data for behavioral measures (e.g., psychophysiology, self-report ratings); this included behavioral data reported in experiments that also collected functional magnetic resonance imaging (fMRI) data. See for full selection and screening details.
Data extraction and quality assessment (QA)
Test statistics and p values were extracted for each Group x Stimulus analysis for each dependent variable and for quadratic contrast interactions when available (56% of identified studies). Clinical, demographic, and experimental details were extracted for all studies (see Supplementary Materials for a list of extracted variables and coding information). Statistical data extraction was done by SEC and independently verified by AMK. Study quality was measured using a custom standardized rubric (see Table ST2 for details) adapted from prior work [29] and Cochrane Collaboration’s risk of bias tool [33, 34].
Statistical analyses
All analyses were conducted in R [35]. Hedge’s g was chosen as the group difference effect size due to its robust properties across sample sizes and interpretability within meta-analytic frameworks [36]. Cluster-robust p values and 95% CIs are reported [37]. Primary outcome measures were subjective (e.g., threat expectancy ratings, self-reported fear) and physiological measures of conditioned fear (e.g., fear-potentiated startle and skin conductance response). Effect sizes were coded as positive in the case of increased generalization (determined through GS means relative to CS+ and CS− or, when not available, visual inspection using a standardized rubric that assesses the linearity of a gradient from CS+ to CS−, see Supplementary Materials for full description) in the anxiety-related disorder group relative to comparisons. Other outcomes were coded as negative, yielding a conservative metric of anxiety vs. comparison group differences that proportionally penalized any generalization result not clearly indicative of heightened generalization in anxiety groups relative to comparison participants.
See Supplementary Materials for full meta-analytic modeling details. Briefly, primary hypotheses were tested using three-level random-effects models (participant-level observations nested within effect size for each dependent variable, nested within study). One model included Group × Stimulus interaction effect sizes from all identified studies (For the n = 3 studies that did not report standard Group × Stimulus interactions for all dependent variables but did report quadratic analyses, we included these quadratic effects in the full-data model and later test if their effects significantly influenced results) to provide; another included quadratic interaction effect sizes from the subset of studies that reported this test. Multiple effect sizes from the same study, corresponding to each dependent variable used to measure generalization, were nested within each study as a random effect. We tested standard heterogeneity statistics in both models. We then conducted moderation analyses using these models to statistically explain potential heterogeneity due to cross-study differences in clinical and experimental parameters (see Table ST3). We tested for both omnibus moderation and for the significance of each level of the moderator (i.e., coefficient tested against zero). We also conducted meta-regressions that included a priori-defined continuous measures of clinical, methodological (including QA), and demographic fixed effects. False discovery rate correction was applied to all moderation and meta-regression tests per recommendations [38]. We tested for risk of publication bias using standard methods (see Supplementary Materials).
Results
Study identification and characteristics
Figure 2A depicts the flow of the selection and inclusion of studies. A total of 5549 titles and abstracts were screened; 300 records were selected for full-text screening. An additional two unpublished studies were also obtained from fear generalization researchers [39, 40]. In total, 16 studies [41,42,43,44,45,46,47,48,49,50,51,52,53,54] reporting unique data met our inclusion criteria (total N = 867, anxiety n = 439, comparison n = 428, Mage = 30.1, % women = 54%, see Supplementary Table 1 for full details). The following disorders were represented in these studies: GAD (n = 82), OCD (n = 28), PD (n = 58), PTSD (n = 152), SAD (n = 73), and SP (n = 46).
PRISMA flow diagram (A) shows the process of identification, screening, eligibility determination, and inclusion that lead to the final N = 16 studies that were meta-analyzed. B shows results from QA of included studies, which were evaluated by independent reviewers and assigned a rating of “low risk of bias”, “some concerns”, “high risk of bias”, or “no information” for each criterion. Bars represent proportion of studies that obtained each rating on each criterion, with a greater proportion of “low risk of bias” (pale yellow) indicative of higher overall study quality. Unpublished studies were not included in QA. Abbreviations: PRISMA Preferred Reporting Items for Systematic Reviews and Meta-Analyses, QA quality assessment.
QA results
Figure 2B provides a summary graph of the overall risk of bias across published studies; Figure SF1 displays risk of bias for each study. Unpublished studies were not evaluated, see Supplementary Materials for further description.
Meta-analyses of full-data and quadratic interaction effects
Primary models
Meta-analysis of the full-data (n = 16 studies, k = 35 effect sizes) yielded a small effect size in favor of anxiety-related disorder groups demonstrating heightened fear generalization compared with comparison participants, g = 0.24, 95% CIc-r [0.1, 0.37], t(15) = 3.84, pc-r = 0.001 (see Fig. 3). Heterogeneity was non-significant, I2 = 25.45%, Q(34) = 47.39, p = 0.063. The quadratic model (n = 9, k = 15) yielded a larger effect size in the same direction as the full-data model, g = 0.3, 95% CIc-r [0.02, 0.58], t(14) = 2.31, pc-r = 0.036 (see Fig. 3). Heterogeneity for this model was significant, I2 = 58.45%, Q(14) = 28.15, p = 0.013. Exclusion of the n = 2 unpublished studies resulted in larger meta-analytic effect sizes in both models but did not change direction or significance.
Plotted points represent effect sizes and 95% confidence intervals derived from random-effects meta-analytic models. Pooled effects are the average effect size for each disorder; summary pooled effect represents average effect size across all disorders. GAD generalized anxiety disorder, OCD obsessive-compulsive disorder, PD panic disorder, PTSD posttraumatic stress disorder, SAD social anxiety disorder, SP specific phobia.
Moderation and meta-regressions
All tested categorical moderators were non-significant (see Table 1 for all moderation results, Figs. SF2 and SF3 for visualization of differences in effect sizes by dependent variable). This included a lack of moderation by anxiety diagnosis or by PTSD compared with all other disorders, although some diagnoses had significant effect sizes when tested against zero (with the largest found for PTSD, then GAD, and then SAD; all pfdr ≤ 0.048) in the full-data model. Similarly, clinical status (threshold vs. sub-threshold) was not a significant moderator, but only studies with threshold samples were significant when the effect size was tested against zero (threshold: pfdr < 0.001; sub-threshold: pfdr = 0.765). In terms of differences due to dependent variable, both physiological (pfdr = 0.035) and self-report rating measures (pfdr = 0.004) yielded significant effect sizes when tested against zero, but again the overall moderation was not significant. All meta-regressions were also non-significant (all pfdr > 0.24; see Table ST4).
Publication bias and QA
For both models, most analyses indicated no risk of publication bias (see Figs. SF4–SF9). However, funnel plots indicated significant asymmetry in both models driven by positive outliers (see Figs. SF6 and SF7). Removal of outliers in each analysis yielded smaller but still significant effect sizes (full-model: g = 0.21; quadratic model: g = 0.26).
Discussion
Improved understanding of the relationship between heightened fear generalization and anxiety-related disorders is an important step in the process of translating laboratory findings to clinical practice. Our primary hypothesis was supported: when meta-analyzing data from all 16 available studies, a small positive effect size was found in favor of heightened generalization in the anxiety-related disorder groups relative to comparison participants. This effect size increased in the meta-analysis that only tested quadratic effects, indicating that less curvilinear generalization gradients (i.e., shallower declines from CS+ to CS−, consistent with increased responding to GSs) differentiate anxiety-related disorder groups from comparison participants. Heterogeneity ranged from negligible to moderate. Cross-study variations in conditioning parameters did not significantly moderate meta-analytic effect sizes. Similarly, within-study variation in dependent variables (physiological vs. self-report ratings) was not a significant moderator. Both results align with prior fear conditioning meta-analyses that did not find study design parameters significantly affected results [26, 27, 29]. Significant heterogeneity was, however, found in the quadratic model, which is possibly due to the smaller number of effect sizes analyzed relative to the full-data analysis. Publication bias was largely acceptable across multiple indices. An exception was in our funnel plots, as extreme positive effect sizes were identified. That said, outlier removal did not significantly change results.
A key strength of this effort is the breadth of designs and disorders we analyzed. In line with hypotheses and theory regarding the transdiagnostic import of fear generalization, anxiety-related disorder diagnosis did not moderate the observed meta-analytic effects. However, this does not mean that all diagnoses exhibited the same effect size, as can be seen in Table 1. When comparing each diagnosis effect size to zero (i.e., a null effect) in isolation from other disorders, GAD and PTSD emerged as the two statistically strongest effect sizes (although caution in interpretation is needed due to the non-significant overall moderation test). This is not unexpected, as etiological accounts of both disorders highlight fear generalization to a wide range of stimuli and contexts as central pathological factors [7]. We also note that PTSD studies yielded the overall largest effect size, and although not significantly different when compared to other disorders, this is an encouraging datapoint for further testing of generalization-focused models of the disorder [7, 19, 55]. Smaller effect sizes in other disorders are undoubtedly a function of smaller sample sizes (particularly for OCD and SP), but also potentially reflects that fear generalization functions more peripherally or is limited to fewer stimuli in these disorders, therefore limiting the capacity for laboratory tests to detect stronger effects.
The clinical status of the anxiety-related disorder group was also not a significant moderator. However, effect sizes tested in isolation against zero revealed stronger overall effect sizes for studies of threshold clinical groups compared to those that tested subclinical groups (which, again, must be interpreted with caution). A recent meta-analysis of dimensional anxiety traits and fear generalization that explicitly excluded threshold or sub-threshold anxiety-related disorder data found a significant small and positive correlational effect size (r = 0.19) [29]. Taken together, meta-analytic evidence suggests that fear generalization varies as a function of anxiety symptom or trait severity and is not circumscribed to specific disorders. Although requiring further empirical work to verify, including more data from each disorder and more studies analyzing continuous anxiety symptom and trait assessments, this pattern implies that heightened fear generalization is a dimensional phenotype that more closely relates to degree, as opposed to type, of anxiety pathology [30]. Future studies might consider using assessments that measure multiple internalizing symptom dimensions [56] located within empirical psychopathology structures (e.g., the Hierarchical Taxonomy of Psychopathology) [57] to more precisely investigate the relation between fear generalization and dimensional anxiety.
The current effort highlights the value of behavioral fear generalization paradigms for identifying abnormalities in threat reactivity associated with anxiety-related disorders. Our findings suggest these paradigms reliably provide a clinically-relevant behavioral marker that distinguishes between anxiety-related disorder patients and comparison participants. Further, researchers can expect a group difference effect size that is similar to or larger than those generated by differential conditioning paradigms (see Fig. SF10 for visualized comparison of meta-analytic effect sizes). For example, the small effect size of g = 0.24 found for the full-data analysis is larger than prior meta-analytic effect sizes of differential fear conditioning (CS+ vs. CS−, |d| = 0.15) and slightly smaller than the CS− acquisition effect size (|d| = 0.29) [26]. Promisingly, the quadratic effect model yielded one of the largest anxiety-related disorder meta-analytic effect sizes for a conditioning index in the literature to date, and the largest for an index that accounts for multiple stimuli. The overall largest is the effect size for CS+ extinction (|d| = 0.35), but this is a single cue index that does not consider other stimuli (e.g., CS−). Taken together, current results and the clinical relevance of fear generalization paradigms lend themselves well to psychiatric investigations, such as those measuring neuropathophysiological markers to use as predictors of symptoms development and of treatment effects.
Fear generalization in the clinically anxious brain
Improved understanding of the neural circuits that underlie fear generalization in clinical populations is crucial to inform precise models of neuropathophysiology that can then guide innovative therapies. The current meta-analysis was limited to behavioral and psychophysiological data; however, fMRI data were collected in five of the identified studies testing a limited number of anxiety-related disorders [42, 43, 45, 50, 51] (see Table ST5). Due to limited fMRI data, an expected small-to-moderate effect, and imaging meta-analysis power concerns [58], we did not perform a quantitative analysis of fMRI data. Instead, we provide a brief qualitative discussion of the available data.
Several cingulo-opercular and frontoparietal regions are implicated in studies of fear generalization in psychiatrically healthy people [15]. Only some of these regions were significantly related to an anxiety-related disorder in the identified studies (see Fig. SF11 for summary illustration). The most consistent cross-study findings were hypoactive ventromedial prefrontal cortex, hyperactive striatal regions (e.g., caudate, putamen), and primarily hyperactivation in the insula to be related to anxiety-related disorders. Due to their prominence in animal work and theoretical accounts of generalization, the lack of consistent amygdala and hippocampus findings in the reviewed studies is notable. Higher-resolution fMRI studies that can reliably detect activity in functional subregions with more specific relations to generalization processes (e.g., lateral central amygdala, hippocampal subfields) [59] are needed. However, broad conclusions regarding all fMRI findings are preliminary, especially considering the small number of identified studies that cover only some disorders.
In terms of the current behavioral meta-analysis, the fMRI findings are generally in line with the finding of heightened fear generalization in anxiety-related disorders, as neural regions that were related to fear generalization, such as the insula and striatum, are associated with behavioral measures of conditioned responding [60]. The fMRI findings also highlight a notable weakness of the analyzed behavioral data: psychophysiological and rating measures cannot disentangle excitatory and inhibitory contributions to fear generalization, whereas fMRI is well-suited to this goal. A recent meta-analysis (15) identified regions associated with increased (excitatory) and decreased (inhibitory) generalization gradients. An fMRI meta-analysis might reveal changes in effect size magnitude or significant moderators if these two types of generalization gradients were examined separately. Once sufficient studies are available, this is a key next step for the field.
Current and future challenges
Fear generalization research in clinical populations is a growing field, and the limitations of the present effort reflect this. First, the available number of studies complicates fine-grained examination of subtle mechanisms and variations of fear generalization in anxiety-related disorders. Our primary analysis of standard interaction effects can only speak to the overall magnitude of generalization differences between anxiety and comparison groups, not to differences in the shape of generalization gradients. Crucially, this is a coarse metric that does not statistically differentiate between GSs and CS+/CS−, and therefore, non-generalization processes (e.g., sensitization) might be present to an extent. More linear or less curvilinear (i.e., GSs more similar to CS+ elicit responses closer in magnitude to the CS+) generalization gradients are proposed as a pathogenic marker of those with anxiety-related disorders [9]. Our analysis of quadratic effects in the subset of studies with relevant data supports this assertion, but was not optimized to detect subtle individual differences in gradient shape related to one or more GSs. Further, the meaning and quantification of generalization gradients is an ongoing topic of empirical discussion [61, 62]. Thus, we cannot state that anxiety-related disorders are clearly defined by a particular gradient shape.
Second, for some disorders (e.g., OCD, SP), there were not enough studies to make sound conclusions regarding their relation to fear generalization at this time; thus, caution is needed in interpreting effect sizes from specific disorders. We also note that caution is generally needed when interpreting moderation effects in the meta-analytic framework, particularly with the relatively small number of studies in the current effort [63]. There is also the issue of potentially impactful moderators that were not assessed in the original studies and therefore were not tested (e.g., childhood maltreatment) [64, 65]. Finally, we were not able to fully test the impact of specific comorbid disorders (e.g., depressive disorders) and psychoactive medications in our meta-regressions due to small sample size or imbalances in study protocols.
Open science practices and study quality
Our QA found some trends that merit discussion, particularly in the context of increasing open science practices [66]. On the one hand, most articles reported having matched their comparison groups, having counterbalanced their stimuli, and having used validated assessment instruments—all of which contribute to study quality and reliability. On the other hand, some risks of bias should be noted. First, no studies preregistered their hypotheses regarding fear generalization. Although a recent development, this open science practice is crucial for improving the trustworthiness of published findings [67]. Second, no studies reported an a priori power analysis, and, given their relatively small sample sizes, they might be statistically underpowered. Compounding this issue is that the reliability of meta-analyses might be reduced when including many studies with small sample sizes, as they often have stronger heterogeneity or chance findings (i.e., small-study effect) [68]. Third, reasons for exclusions and for missing data differed across each study or were not reported. More transparency on treating excluded or missing data might increase the integrity of findings and across-study comparability.
Future directions
In addition to the challenges outlined above, it is important to emphasize key opportunities for future work. The current meta-analysis does not explain the how of heightened fear generalization across anxiety-related disorders, and this remains a critical next step. All analyzed studies were cross-sectional, and behavioral measures do not allow us to disentangle specific mechanisms of the fear generalization process (as done in the reviewed fMRI studies). This also means we cannot yet determine if heightened fear generalization is one of, or a combination of, the following: a predisposing risk factor for anxiety-related pathology, a pathogenic mechanism, or a manifest symptom of the pathology. Further, we do not know if generalization deficits are isolated to threat processes or if there are non-affective dysfunctions that serve to predispose people toward heightened generalization (e.g., perceptual discrimination difficulties) [69]. Additional studies using prospective longitudinal designs, testing other forms of generalization and related processes, and linking fear generalization task data to clinical data are needed to comprehensively address this important issue. In line with previously addressed limitations, we also recommend that these future studies, when feasible, use dimensional assessments and neuroimaging to facilitate precise measurement of the underlying components of fear generalization and their relations to fine-grained markers of anxiety psychopathology.
Conclusion
Overall, it is clear there are many future avenues generalization research can take to enhance the study of pathological anxiety. The current meta-analytic results suggest that conditioning researchers might strongly consider using a generalization design instead of simple differential conditioning when investigating anxiety-related differences in fear learning, although some paradigms that only use differential stimuli (e.g., extinction designs) are still valuable for understanding other learning processes. We contend that fear generalization has notable empirical and conceptual advantages over differential acquisition and extinction paradigms and holds promise for innovative clinical translational research on emotional memory and learning in anxiety-related disorders.
References
Bandelow B, Michaelis S. Epidemiology of anxiety disorders in the 21st century. Dialogues Clin Neurosci. 2015;17:327–35.
Baxter AJ, Scott KM, Vos T, Whiteford HA. Global prevalence of anxiety disorders: a systematic review and meta-regression. Psychological Med. 2013;43:897–910.
Pavlov IP. Conditioned reflexes: an investigation of the physiological activity of the cerebral cortex. Oxford University Press; Oxford, UK, 1927.
Watson JB, Rayner R. Conditioned emotional reactions. J Exp Psychol. 1920;3:1–14.
Pittig A, Treanor M, LeBeau RT, Craske MG. The role of associative fear and avoidance learning in anxiety disorders: gaps and directions for future research. Neurosci Biobehav Rev. 2018;88:117–40.
Vervliet B, Boddez Y. Memories of 100 years of human fear conditioning research and expectations for its future. Behav Res Ther. 2020;135:103732.
Zinbarg RE, Williams AL, Mineka S. A current learning theory approach to the etiology and course of anxiety and related disorders. Annu Rev Clin Psychol. 2022. https://doi.org/10.1146/annurev-clinpsy-072220-021010.
Dymond S, Dunsmoor JE, Vervliet B, Roche B, Hermans D. Fear generalization in humans: systematic review and implications for anxiety disorder research. Behav Ther. 2015;46:561–82.
Lissek S. Toward an account of clinical anxiety predicated on basic, neurally mapped mechanisms of pavlovian fear-learning: the case for conditioned overgeneralization. Depress Anxiety. 2012;29:257–63.
Craske MG, Hermans D, Vervliet B. State-of-the-art and future directions for extinction as a translational model for fear and anxiety. Philos Trans R Soc B. 2018;373:20170025.
Dunsmoor JE, Niv Y, Daw N, Phelps EA. Rethinking extinction. Neuron 2015;88:47–63.
Lopresto D, Schipper P, Homberg JR. Neural circuits and mechanisms involved in fear generalization: Implications for the pathophysiology and treatment of posttraumatic stress disorder. Neurosci Biobehav Rev. 2016;60:31–42.
Besnard A, Sahay A. Adult hippocampal neurogenesis, fear generalization, and stress. Neuropsychopharmacology. 2016;41:24–44.
LeDoux JE. Emotion, memory and the brain. Sci Am. 1994;270:50–7.
Webler RD, Berg H, Fhong K, Tuominen L, Holt DJ, Morey RA, et al. The neurobiology of human fear generalization: meta-analysis and working neural model. Neurosci Biobehav Rev. 2021;128:421–36.
Holmes EA, Ghaderi A, Harmer CJ, Ramchandani PG, Cuijpers P, Morrison AP, et al. The Lancet Psychiatry Commission on psychological treatments research in tomorrow’s science. Lancet Psychiatry. 2018;5:237–86.
Milad MR, Quirk GJ. Fear extinction as a model for translational neuroscience: ten years of progress. Annu Rev Psychol. 2012;63:129–51.
Cooper SE, Dunsmoor JE. Fear conditioning and extinction in obsessive-compulsive disorder: a systematic review. Neurosci Biobehav Rev. 2021;129:75–94.
Lissek S, van Meurs B. Learning models of PTSD: theoretical accounts and psychobiological evidence. Int J Psychophysiol. 2014. https://doi.org/10.1016/j.ijpsycho.2014.11.006.
Zuj DV, Palmer MA, Lommen MJJ, Felmingham KL. The centrality of fear extinction in linking risk factors to PTSD: a narrative review. Neurosci Biobehav Rev. 2016;69:15–35.
Beckers T, Krypotos A-M, Boddez Y, Effting M, Kindt M. What’s wrong with fear conditioning? Biol Psychol. 2013;92:90–6.
Lissek S, Pine DS, Grillon C. The strong situation: a potential impediment to studying the psychobiology and pharmacology of anxiety disorders. Biol Psychol. 2006;72:265–70.
Grupe DW, Nitschke JB. Uncertainty and anticipation in anxiety: an integrated neurobiological and psychological perspective. Nat Rev Neurosci. 2013;14:488–501.
Arch JJ, Abramowitz JS. Exposure therapy for obsessive–compulsive disorder: an optimizing inhibitory learning approach. J Obsessive-Compuls Relat Disord. 2015;6:174–82.
Foa EB, McLean CP. The efficacy of exposure therapy for anxiety-related disorders and its underlying mechanisms: the case of OCD and PTSD. Annu Rev Clin Psychol. 2016;12:1–28.
Duits P, Cath DC, Lissek S, Hox JJ, Hamm AO, Engelhard IM, et al. Updated meta-analysis of classical fear conditioning in the anxiety disorders. Depress Anxiety. 2015;32:239–53.
Lissek S, Powers AS, McClure EB, Phelps EA, Woldehawariat G, Grillon C, et al. Classical fear conditioning in the anxiety disorders: a meta-analysis. Behav Res Ther. 2005;43:1391–424.
Dunsmoor JE, Paz R. Fear generalization and anxiety: behavioral and neural mechanisms. Biol Psychiatry. 2015;78:336–43.
Sep MSC, Steenmeijer A, Kennis M. The relation between anxious personality traits and fear generalization in healthy subjects: a systematic review and meta-analysis. Neurosci Biobehav Rev. 2019;107:320–8.
Marin M-F, Hammoud MZ, Klumpp H, Simon NM, Milad MR. Multimodal categorical and dimensional approaches to understanding threat conditioning and its extinction in individuals with anxiety disorders. JAMA Psychiatry. 2020. https://doi.org/10.1001/jamapsychiatry.2019.4833.
American Psychiatric Association. Diagnostic and statistical manual of mental disorders. 5th ed. Arlington, VA: American Psychiatric Association; 2013.
Asmundson GJG. A rose by any other name…How should we refer to the collective of conditions characterized by clinically significant anxiety? J Anxiety Disord. 2019;68:102143.
Higgins JPT, Altman DG, Gøtzsche PC, Jüni P, Moher D, Oxman AD, et al. The Cochrane Collaboration’s tool for assessing risk of bias in randomised trials. BMJ. 2011;343:d5928.
RoB 2: A revised Cochrane risk-of-bias tool for randomized trials | Cochrane Bias. 2022. https://methods.cochrane.org/bias/resources/rob-2-revised-cochrane-risk-bias-tool-randomized-trials.
R Core Team. R: A language and environment for statistical computing. Vienna, Austria: R Foundation for Statistical Computing; 2018.
Lakens D. Calculating and reporting effect sizes to facilitate cumulative science: a practical primer for t-tests and ANOVAs. Front Psychol. 2013;4:863.
Cameron AC, Miller DL. A practitioner’s guide to cluster-robust inference. J Hum Resour. 2015;50:317–72.
Cafri G, Kromrey JD, Brannick MT. A meta-meta-analysis: empirical review of statistical power, type I error rates, effect sizes, and model selection of meta-analyses published in psychology. Multivar Behav Res. 2010;45:239–70.
Cooper SE, Berg HE, Grillon C, Lissek S. Behavioral fear generalization task data in social anxiety disorder. [Unpublished raw data]. University of Minnesota, 2016.
Fullana MA, Torrents-Rodas D, Torrubia R. Behavioral fear generalization task data in panic disorder. [Unpublished raw data]. Hospital Clinic, Barcelona & Universitat Autònoma, 2016.
Ahrens LM, Pauli P, Reif A, Mühlberger A, Langs G, Aalderink T, et al. Fear conditioning and stimulus generalization in patients with social anxiety disorder. J Anxiety Disord. 2016;44:36–46.
Greenberg T, Carlson JM, Cha J, Hajcak G, Mujica-Parodi LR. Ventromedial prefrontal cortex reactivity is altered in generalized anxiety disorder during fear generalization. Depress Anxiety. 2013;30:242–50.
Kaczkurkin AN, Burton PC, Chazin SM, Manbeck AB, Espensen-Sturges T, Cooper SE, et al. Neural substrates of overgeneralized conditioned fear in PTSD. AJP. 2017;174:125–34.
Kaczkurkin AN, Lissek S. Generalization of conditioned fear and obsessive-compulsive traits. J Psychol Psychother. 2013;7:3.
Lange I, Goossens L, Bakker J, Michielse S, Marcelis M, Wichers M, et al. Functional neuroimaging of associative learning and generalization in specific phobia. Prog Neuro-Psychopharmacol Biol Psychiatry. 2019;89:275–85.
Lis S, Thome J, Kleindienst N, Mueller-Engelmann M, Steil R, Priebe K, et al. Generalization of fear in post-traumatic stress disorder. Psychophysiology. 2019;57:e13422.
Lissek S, Rabin S, Heller RE, Lukenbaugh D, Geraci M, Pine DS, et al. Overgeneralization of conditioned fear as a pathogenic marker of panic disorder. Am J Psychiatry. 2010;167:47–55.
Lissek S, Kaczkurkin AN, Rabin S, Geraci M, Pine DS, Grillon C. Generalized anxiety disorder is associated with overgeneralization of classically conditioned fear. Biol Psychiatry. 2014;75:909–15.
Lissek S, Grillon C. Learning models of PTSD. The Oxford handbook of traumatic stress disorders. Beck JG, Sloan DM. (eds). Oxford University Press, 2012. https://doi.org/10.1093/oxfordhb/9780195399066.013.0013.
Morey RA, Dunsmoor JE, Haswell CC, Brown VM, Vora A, Weiner J, et al. Fear learning circuitry is biased toward generalization of fear associations in posttraumatic stress disorder. Transl Psychiatry. 2015;5:e700.
Morey RA, Haswell CC, Stjepanović D, Dunsmoor JE, LaBar KS. Mid-Atlantic MIRECC Workgroup,. Neural correlates of conceptual-level fear generalization in posttraumatic stress disorder. Neuropsychopharmacology. 2020;45:1380–9.
Neueder D, Andreatta M, Pauli P. Contextual fear conditioning and fear generalization in individuals with panic attacks. Front Behav Neurosci. 2019;13:152.
Reichenberger J, Pfaller M, Forster D, Gerczuk J, Shiban Y, Mühlberger A. Men scare me more: gender differences in social fear conditioning in virtual reality. Front Psychol. 2019;10:1617.
Tinoco-González D, Fullana MA, Torrents-Rodas D, Bonillo A, Vervliet B, Blasco MJ, et al. Conditioned fear acquisition and generalization in generalized anxiety disorder. Behav Ther. 2015;46:627–39.
Dunsmoor JE, Cisler JM, Fonzo GA, Creech SK, Nemeroff CB. Laboratory models of post-traumatic stress disorder: the elusive bridge to translation. Neuron. 2022;S0896-6273(22)00202-1:24.
Watson D, O’Hara MW, Naragon-Gainey K, Koffel E, Chmielewski M, Kotov R, et al. Development and validation of new anxiety and bipolar symptom scales for an expanded version of the IDAS (the IDAS-II). Assessment. 2012;19:399–420.
Watson D, Levin-Aspenson HF, Waszczuk MA, Conway CC, Dalgleish T, Dretsch MN, et al. Validity and utility of hierarchical taxonomy of psychopathology (HiTOP): III. Emotional dysfunction superspectrum. World Psychiatry. 2022;21:26–54.
Müller VI, Cieslik EC, Laird AR, Fox PT, Radua J, Mataix-Cols D, et al. Ten simple rules for neuroimaging meta-analysis. Neurosci Biobehav Rev. 2018;84:151–61.
Huggins AA, Weis CN, Parisi EA, Bennett KP, Miskovic V, Larson CL. Neural substrates of human fear generalization: a 7T-fMRI investigation. NeuroImage. 2021;239:118308.
Schiller D, Delgado MR. Overlapping neural systems mediating extinction, reversal and regulation of fear. Trends Cogn Sci. 2010;14:268–76.
Lee JC, Mills L, Hayes BK, Livesey EJ. Modelling generalisation gradients as augmented Gaussian functions. Q J Exp Psychol. 2020;74:1747021820949470.
Vanbrabant K, Boddez Y, Verduyn P, Mestdagh M, Hermans D, Raes F. A new approach for modeling generalization gradients: a case for hierarchical models. Front Psychol. 2015;6:652.
Borenstein M, Higgins JPT. Meta-analysis and subgroups. Prev Sci. 2013;14:134–43.
Lange I, Goossens L, Bakker J, Michielse S, van Winkel R, Lissek S, et al. Neurobehavioural mechanisms of threat generalization moderate the link between childhood maltreatment and psychopathology in emerging adulthood. J Psychiatry Neurosci. 2019;44:185–94.
Teicher MH, Gordon JB, Nemeroff CB. Recognizing the importance of childhood maltreatment as a critical factor in psychiatric diagnoses, treatment, research, prevention, and education. Mol Psychiatry. 2021:1–8.
Nosek BA, Alter G, Banks GC, Borsboom D, Bowman SD, Breckler SJ, et al. Promoting an open research culture. Science. 2015;348:1422–5.
Bell V. Open science in mental health research. Lancet Psychiatry. 2017;4:525–6.
Nuijten MB, van Assen MALM, Augusteijn HEM, Crompvoets EAV, Wicherts JM. Effect sizes, power, and biases in intelligence research: a meta-meta-analysis. J Intell. 2020;8:36.
Struyf D, Zaman J, Hermans D, Vervliet B. Gradients of fear: How perception influences fear generalization. Behav Res Ther. 2017;93:116–22.
Acknowledgements
We thank Sophie Bergmeijer, Mona Laskar, Annemijn Hoekman, Michelle Gersmann, and Layla Vergeer for their assistance in the article screening and selection process. We also thank Ryan Webler, Nicole Keller, and Gus Hennings for helpful discussions regarding fMRI results and figures.
Funding
This work was supported by the National Institutes of Health (F32 MH129136, awarded to SEC; R01 MH122387, awarded to JED) and National Science Foundation (CAREER Award 1844792, awarded to JED). IME and EAMvD were supported by a Vici grant (453-15-005, awarded to IME) from the Netherlands Organization for Scientific Research.
Author information
Authors and Affiliations
Contributions
SEC: conceptualization, methodology, formal analysis, data curation, project administration, visualization, writing—original draft. EAMvD: conceptualization, methodology, project administration, data Curation, writing—original draft. MAH and CBN: writing—reviewing and editing. A-MK: methodology, writing—reviewing and editing. SL: conceptualization, writing—reviewing and editing. IME: conceptualization, writing—reviewing and editing, supervision. JED: conceptualization, writing—reviewing and editing, supervision, funding acquisition.
Corresponding authors
Ethics declarations
Competing interests
CBN has received research support from NIH; he has served as a consultant for ANeuroTech (division of Anima BV), Signant Health, Magstim, Inc., Navitor Pharmaceuticals, Inc., Intra-Cellular Therapies, Inc., EMA Wellness, Acadia Pharmaceuticals, Sage, BioXcel Therapeutics, Silo Pharma, XW Pharma, Neuritek, Engrail Therapeutics, Corcept Therapeutics Pharmaceuticals Company, SK Life Science, Alfasigma, Pasithea Therapeutic Corp., EcoR1; he has served on scientific advisory boards for the ANeuroTech (division of Anima BV), Brain and Behavior Research Foundation (BBRF), Anxiety and Depression Association of America (ADAA), Skyland Trail, Signant Health, Laureate Institute for Brain Research (LIBR), Inc., Magnolia CNS, Heading Health, TRUUST Neuroimaging, Pasithea Therapeutic Corp.; he is a stockholder in Xhale, Seattle Genetics, Antares, BI Gen Holdings, Inc., Corcept Therapeutics Pharmaceuticals Company, EMA Wellness, TRUUST Neuroimaging; he serves on the board of directors for Gratitude America, ADAA, Xhale Smart, Inc., Lucy Scientific Discovery, Inc; and he holds patents on a method and devices for transdermal delivery of lithium (patent 6,375,990B1) and a method of assessing antidepressant drug therapy via transport inhibition of monoamine neurotransmitters by ex vivo assay (patent 7,148,027B2). The other authors report no financial relationships with commercial interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Cooper, S.E., van Dis, E.A.M., Hagenaars, M.A. et al. A meta-analysis of conditioned fear generalization in anxiety-related disorders. Neuropsychopharmacol. 47, 1652–1661 (2022). https://doi.org/10.1038/s41386-022-01332-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41386-022-01332-2
This article is cited by
-
The ventromedial prefrontal cortex in response to threat omission is associated with subsequent explicit safety memory
Scientific Reports (2024)
-
Understanding clinical fear and anxiety through the lens of human fear conditioning
Nature Reviews Psychology (2023)
-
Sequential fear generalization and network connectivity in trauma exposed humans with and without psychopathology
Communications Biology (2022)