Abstract
Background
The association between body fat composition and risk of cancer in normal weight individuals (body mass index (BMI) 18.5–24.9 kg/m2) is unclear.
Methods
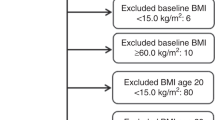
We examined the association of measures of adiposity with risk of incident cancers of the breast (postmenopausal), endometrium, ovary and colon/rectum among 149,928 normal weight individuals (40–70 years) who were enrolled in the UK Biobank cohort between 2006 and 2010.
Results
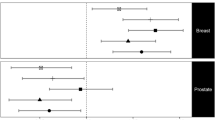
All of the body fat measures were positively associated with invasive postmenopausal breast cancer risk (hazard ratios (HR) for the uppermost quintile (Q5) versus the lowest quintile (Q1) ranged from 1.32 (95% CI: 1.09–1.60) for waist circumference (WC) to 1.56 (1.28–1.90) for BMI). Trunk fat mass index (HRQ5 vs Q1: 1.72, 95% CI: 1.02–2.89) and WC (HRQ5 vs Q1: 1.65, 95% CI: 1.01–2.70)) were positively associated with risk of endometrial cancer. Among males, trunk fat:trunk fat free mass ratio, trunk fat:leg fat mass ratio and (HRQ5 vs Q1: 1.63, 95% CI: 1.02–2.60; 1.92, 1.20–3.07 and 1.68, 1.05–2.66, respectively) were positively associated with colon cancer risk. None of the body fat measures was associated with risk of ovarian cancer or colorectal cancer in women.
Conclusion
The findings of this study suggest that the current normal weight category based on BMI includes individuals who are at increased risk of some obesity-related cancers.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 24 print issues and online access
$259.00 per year
only $10.79 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Lauby-Secretan, B., Scoccianti, C., Loomis, D., Grosse, Y., Bianchini, F. & Straif, K. Body fatness and cancer—viewpoint of the IARC Working Group. N. Engl. J. Med. 375, 794–798 (2016).
Borga, M., West, J., Bell, J. D., Harvey, N. C., Romu, T., Heymsfield, S. B. et al. Advanced body composition assessment: from body mass index to body composition profiling. J. Invest. Med. 66, 1 (2018).
Goodpaster, B. H., Krishnaswami, S., Harris, T. B., Katsiaras, A., Kritchevsky, S. B., Simonsick, E. M. et al. Obesity, regional body fat distribution, and the metabolic syndrome in older men and women. INTEMED 165, 777–783 (2005).
Avgerinos, K. I., Spyrou, N., Mantzoros, C. S. & Dalamaga, M. Obesity and cancer risk: Emerging biological mechanisms and perspectives. Metabolism 92, 121–135 (2019).
Iyengar, N. M., Arthur, R., Manson, J. E., Chlebowski, R. T., Kroenke, C. H., Peterson, L. et al. Association of body fat and risk of breast cancer in postmenopausal women with normal body mass index: A secondary analysis of a randomized clinical trial and observational study. JAMA Oncology 5, 155–163 (2019).
Friedenreich, C. M., Biel, R. K., Lau, D. C. W., Csizmadi, I., Courneya, K. S., Magliocco, A. M. et al. Case-control study of the metabolic syndrome and metabolic risk factors for endometrial cancer. Cancer Epidemiol Biomarkers Prev 20, 2384 (2011).
Gunter, M. J., Xie, X., Xue, X., Kabat, G. C., Rohan, T. E., Wassertheil-Smoller, S. et al. Breast cancer risk in metabolically healthy but overweight postmenopausal women. Cancer Res 75, 270 (2015).
Park, Y. M., White, A. J., Nichols, H. B., O’Brien, K. M., Weinberg, C. R. & Sandler, D. P. The association between metabolic health, obesity phenotype and the risk of breast cancer. Int J Cancer 140, 2657–2666 (2017).
Murphy, N., Cross, A. J., Abubakar, M., Jenab, M., Aleksandrova, K., Boutron-Ruault, M. et al. A nested case-control study of metabolically defined body size phenotypes and risk of colorectal cancer in the European Prospective Investigation into Cancer and Nutrition (EPIC). PLOS Med 13, e1001988 (2016).
Marra, M., Sammarco, R., De Lorenzo, A., Iellamo, F., Siervo, M., Pietrobelli, A. et al. Assessment of body composition in health and disease using bioelectrical impedance analysis (BIA) and dual energy X-Ray absorptiometry (DXA): A critical overview. Contrast Media Mol Imaging 2019, 3548284 (2019).
Böhm, A. & Heitmann, B. L. The use of bioelectrical impedance analysis for body composition in epidemiological studies. Eur J Clin Nutr 67, S79–S85 (2013).
Allen, N., Sudlow, C., Downey, P., Peakman, T., Danesh, J., Elliott, P. et al. UK Biobank: Current status and what it means for epidemiology. Health Policy and Technology 1, 123–126 (2012).
Sudlow, C., Gallacher, J., Allen, N., Beral, V., Burton, P., Danesh, J. et al. UK Biobank: An open access resource for identifying the causes of a wide range of complex diseases of middle and old age. PLOS Medicine 12, e1001779 (2015).
Fry, A., Littlejohns, T. J., Sudlow, C., Doherty, N., Adamska, L., Sprosen, T. et al. Comparison of sociodemographic and health-related characteristics of uk biobank participants with those of the general population. Am J Epidemiol 186, 1026–1034 (2017).
VanItallie, T. B., Yang, M. U., Heymsfield, S. B., Funk, R. C. & Boileau, R. A. Height-normalized indices of the body’s fat-free mass and fat mass: potentially useful indicators of nutritional status. Am J Clin Nutr 52, 953–959 (1990).
Gavi, S., Feiner, J. J., Melendez, M. M., Mynarcik, D. C., Gelato, M. C. & McNurlan, M. A. Limb fat to trunk fat ratio in elderly persons is a strong determinant of insulin resistance and adiponectin levels. J Gerontol A Biol Sci Med Sci 62, 997–1001 (2007).
Lahmann, P. H., Hoffmann, K., Allen, N., van Gils, C. H., Khaw, K., Tehard, B. et al. Body size and breast cancer risk: Findings from the European prospective investigation into cancer and nutrition (EPIC). Int J Cancer 2004 111, 762–771 (2019).
Collaborative Group on Hormonal Factors in Breast Cancer. Breast cancer and hormone replacement therapy: collaborative reanalysis of data from 51 epidemiological studies of 52 705 women with breast cancer and 108 411 women without breast cancer. Lancet 350, 1047–1059 (1997).
Pazoki, R., Dehghan, A., Evangelou, E., Warren, H., Gao, H., Caulfield, M. et al. Genetic predisposition to high blood pressure and lifestyle factors: Associations with midlife blood pressure levels and cardiovascular events. Circulation 137, 653–661 (2018).
Omiyale W., Allen N. E., Sweetland S. Body size, body composition and endometrial cancer risk among postmenopausal women in UK Biobank. Int J Cancer 2020; https://doi.org/10.1002/ijc.33023.
Basraon, S. K., Mele, L., Myatt, L., Roberts, J. M., Hauth, J. C., Leveno, K. J. et al. relationship of early pregnancy waist-to-hip ratio versus body mass index with gestational diabetes mellitus and insulin resistance. Am J Perinatol 33, 114–121 (2016).
Sorosky, J. I. Endometrial Cancer. Obstet Gynecol 120, 383–397 (2012).
Duska L. R., Tew W. P., Moore K. N. Epithelial ovarian cancer in older women: Defining the best management approach. Am Soc Clin Oncol Educ Book. 2015;e311–e321. https://doi.org/10.14694/EdBook_AM.2015.35.e311.
Ortega, L. S., Bradbury, K. E., Cross, A. J., Morris, J. S., Gunter, M. J. & Murphy, N. A prospective investigation of body size, body fat composition and colorectal cancer risk in the UK Biobank. Sci Rep 7, 17807 (2017).
Ogundiran, T. O., Huo, D., Adenipekun, A., Campbell, O., Oyesegun, R., Akang, E. et al. Body fat distribution and breast cancer risk: findings from the Nigerian breast cancer study. Cancer Causes Control 23, 565–574 (2012).
World Cancer Research Fund / American Institute for Cancer Research. Continuous Update Project Expert Report. Diet, Nutrition, Physical Activity, and Endometrial Cancer. Continuous Update Project Expert Report. Diet, Nutrition, Physical Activity, and Ovarian Cancer. 2018; Available at: http://www.dietandcancerreport.org. Accessed 13 June 2018.
Kim, H. & Giovannucci, E. L. Sex differences in the association of obesity and colorectal cancer risk. Cancer Causes Control 28, 1–4 (2017).
Karastergiou, K., Smith, S. R., Greenberg, A. S. & Fried, S. K. Sex differences in human adipose tissues - the biology of pear shape. Biol Sex Differ 3, 13–13 (2012).
Candido, J. & Hagemann, T. Cancer-Related Inflammation. J Clin Immunol 33, 79–84 (2013).
Manolopoulos, K. N., Karpe, F. & Frayn, K. N. Gluteofemoral body fat as a determinant of metabolic health. Int J Obes 34, 949–959 (2010).
Kirschner, M. A. & Samojlik, E. Sex hormone metabolism in upper and lower body obesity. Int J Obes 15(Suppl 2), 101–108 (1991).
Staiger, H., Tschritter, O., Machann, J., Thamer, C., Fritsche, A., Maerker, E. et al. Relationship of serum adiponectin and leptin concentrations with body fat distribution in humans. Obes Res 11, 368–376 (2003).
Kettaneh, A., Heude, B., Romon, M., Oppert, J. M., Borys, J. M., Balkau, B. et al. High plasma leptin predicts an increase in subcutaneous adiposity in children and adults. Eur J Clin Nutr 61, 719–726 (2007).
Garofalo, C. & Surmacz, E. Leptin and cancer. J Cell Physiol 207, 12–22 (2006).
Faria, S. L., Faria, O. P., Cardeal, M. D. A. & Ito, M. K. Validation study of multi-frequency bioelectrical impedance with dual-energy x-ray absorptiometry among obese patients. Obesity Surg 24, 1476–1480 (2014).
Sun, G., French, C. R., Martin, G. R., Younghusband, B., Green, R. C., Xie, Y. et al. Comparison of multifrequency bioelectrical impedance analysis with dual-energy X-ray absorptiometry for assessment of percentage body fat in a large, healthy population. Am J Clin Nutr 81, 74–78 (2005).
Tikkanen, E., Gustafsson, S., Knowles, J. W., Perez, M., Burgess, S. & Ingelsson, E. Body composition and atrial fibrillation: A Mendelian randomization study. Eur Heart J 40, 1277–1282 (2019).
Acknowledgements
This study was presented as an e-poster at the 2020 AACR Virtual Annual Meeting 11 on June 22, 2020 during the Obesity, Physical Activity and Related Biomarkers session. This research was conducted using the UK Biobank Resource (Project ID: 40525).
Author information
Authors and Affiliations
Contributions
R.S.A. contributed to the conception and design, analyses and interpretation of the data, writing the manuscript and final approval of the version to be published. A.J.D. contributed to the conception and design, reviewing the manuscript and final approval of the manuscript. M.K. contributed to the analyses and interpretation of the data, reviewing the manuscript and final approval of the manuscript. T.R. contributed to the conception and design, interpretation of the data, reviewing the manuscript and final approval of the manuscript.
Corresponding author
Ethics declarations
Ethical approval and consent to participate
The study was approved by the North West Multi-centre Research Ethics Committee, the National Information Governance Board for Health and Social Care in England and Wales and the Community Health Index Advisory Group in Scotland. All participants provided written informed consent. The study was performed in accordance with the Declaration of Helsinki.
Data availability
This study was conducted using data from the UK Biobank study. Information on data availability can be obtained via the UK Biobank website (http://www.ukbiobank.ac.uk).
Competing interests
The authors declare no competing interests.
Funding information
This work was supported by the Breast Cancer Research Foundation (BCRF-16–140 to T.E.R.; BCRF-19–034, NCI U54 CA210184 to A.J.D.).
Additional information
Note This work is published under the standard license to publish agreement. After 12 months the work will become freely available and the license terms will switch to a Creative Commons Attribution 4.0 International (CC BY 4.0).
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Arthur, R.S., Dannenberg, A.J., Kim, M. et al. The association of body fat composition with risk of breast, endometrial, ovarian and colorectal cancers among normal weight participants in the UK Biobank. Br J Cancer 124, 1592–1605 (2021). https://doi.org/10.1038/s41416-020-01210-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41416-020-01210-y