Abstract
The NpmA bacterial 16S rRNA methyltransferase, which is identified from Escherichia coli strains, confers high resistance to many types of aminoglycoside upon its host cells. But despite its resistance-conferring ability, only two cases of its isolation from E. coli (14 years apart) have been reported to date. Here, we investigated the effect of the npmA gene on aminoglycoside resistance in Pseudomonas aeruginosa and Klebsiella pneumoniae and its stability in E. coli cells by comparing it with armA, another 16S rRNA methyltransferase gene currently spreading globally. As a result, we found that npmA conferred resistance to all types of aminoglycoside antibiotics we tested (except streptomycin) in both P. aeruginosa and K. pneumoniae, as well in E. coli. In addition, co-expression of armA and npmA resulted in an additive effect for the resistance. However, in return for the resistance, we also observed that the growth rates and the cell survivability of the strains transformed with the npmA-harboring plasmids were inferior than those of the control strains and that these plasmids were easily disrupted by IS10, IS1, and IS5 insertion sequences. We discuss these data in the context of the threat posed by pathogenic strains possessing npmA.
Similar content being viewed by others
Introduction
The history of antibiotics is also the history of the fight against drug-resistant pathogens. As the World Health Organization has reported, the global spread of drug-resistant pathogenic bacterial strains is becoming an increasingly urgent issue to be addressed [1]. In particular, infectious diseases caused by drug-resistant Gram-negative bacteria are particularly concerning. Gram-negative bacteria originally have natural resistance to various classes of antibiotics, but worse still, new drug-resistant genes, such as the colistin resistance mcr-1 gene [2], the carbapenem resistance blaNDM-1 gene, blaKPC gene, and other β-lactamase-encoding genes [3], have been isolated from various pathogenic species worldwide. In this study, we focused on another two genes of concern, armA and npmA, which each encode 16S rRNA methyltransferases that confer high-level resistance to aminoglycoside drugs.
armA, which was originally identified on a plasmid from a Citrobacter freundii strain [4], was found to be widely spread in Asia, Europe, and the United States [5]. It should also be noted that armA is often found with other antibiotic-resistant genes on highly transmissible plasmids [6,7,8]. The armA gene product, ArmA, catalyzes the methylation of guanine at position 1405 in the 16S rRNA located in the decoding site of 30S ribosomes [9]. The strains expressing enzymes related to ArmA, such as RmtB and RmtC, are also found in various parts of the world [5].
In contrast, npmA encodes a 16S rRNA methyltransferase that catalyzes the methylation of adenine at position 1408 located in the decoding site of 30S ribosomes [9]. npmA, which was originally found in an Escherichia coli strain isolated in 2003 in Japan, confers high resistance to many aminoglycoside types upon the host E. coli cells [10]. But surprisingly, despite it contributing to strong resistance against a broad range of aminoglycoside antibiotics, the second report of the isolation of the bacteria possessing npmA did not appear in the scientific literature until August 2017 from China [11].
Hence, we performed a comparative study on armA and npmA, in which we evaluated their activities against aminoglycosides, their stabilities, and their effects on E. coli, P. aeruginosa, and K. pneumoniae as host bacterial cells.
Results
Drug resistance in an E. coli DH5α derivative expressing rRNA methylase genes
For the purpose of understanding the properties of armA and npmA, E. coli DH5α strains possessing armA and/or npmA were constructed (Table 1) and they were used to evaluate their drug resistance patterns against various aminoglycoside types. As shown in Table 2, the NCGM58 strain was highly resistant to dibekacin, arbekacin, gentamicin, sisomicin, and fortimicin A, as compared with the NCGM57 vector control strain, indicating that armA confers resistance to these compounds. In contrast, the NCGM59 strain showed intermediate or high resistance against all the aminoglycosides we tested except streptomycin, indicating that npmA confers resistance to various kinds of aminoglycoside compounds. Moreover, the NCGM60 strain transformed by a plasmid containing both armA and npmA displayed the resistance properties of both NCGM58 and NCGM59. In particular, the differences we observed in the MIC values for paromomycin and lividomycin A among the test strains were clearly related to the co-expression of armA and npmA.
Effect of armA and npmA on E. coli proliferation
Although both armA and npmA were determined to be responsible for aminoglycoside resistance, these gene products might adversely affect E. coli cells because the enzymes they encode alter the partial structure of a decoding site in the ribosome by methylating the 16S rRNA. Therefore, we examined the effect of armA and npmA on proliferation of the DH5α derivative strains in LB medium supplemented with 30 µg/ml of chloramphenicol. As a result, the growth rate of the NCGM58 strain possessing armA was similar to the vector control NCGM57 strain, as shown in Fig. 1. In contrast, the NCGM59 strain, which possesses npmA, grew slower, while the NCGM60 strain, which possesses both armA and npmA, grew much slower than the other strains.
Turbidity time course of the E. coli DH5α derivatives possessing armA and/or npmA methyltransferase genes. Overnight cultures of each strain were inoculated into LB medium containing chloramphenicol and then incubated at 37 °C at 140 spm. Symbols: diamonds, NCGM57 vector control strain; squares, NGCM58 possessing armA; triangles, NCGM59 possessing npmA; circles, NCGM60 possessing armA and npmA
The effect of the npmA gene on aminoglycoside resistance and its proliferation patterns in K. pneumoniae and P. aeruginosa
As there have been no reports of a strain possessing npmA except for two cases in E. coli, it was unclear whether npmA could function in other Gram-negative species as well as in E. coli. Therefore, we introduced either or both armA and npmA into K. pneumoniae PCI 602 and P. aeruginosa PAO1 using a broad-host-range plasmid (Table 1). We then evaluated the resistance of these bacterial species to aminoglycoside drugs and their proliferation rates.
The results (Table 3) of these experiments showed that armA possessing K. pneumoniae BKKZ1437 and P. aeruginosa BKKZ1463 displayed resistance to arbekacin and gentamicin, whereas the npmA-possessing BKKZ1438 and BKKZ1465 strains displayed resistance to apramycin and butirosin A. It was interesting that npmA conferred higher resistance to arbekacin and gentamicin in P. aeruginosa compared with E. coli and K. pneumoniae. All the aminoglycoside drugs we tested, except streptomycin, were ineffective against BKKZ1443 and BKKZ1467, which both possess armA and npmA, as does E. coli NCGM60.
Slower growth was also observed in K. pneumoniae BKKZ1438 and BKKZ1443 and in P. aeruginosa BKKZ1465 and BKKZ1467, both of which harbored the npmA-containing plasmid (Fig. 2 and Table 4). K. pneumoniae BKKZ1437 and P. aeruginosa BKKZ1463, which both possess amrA, also had slightly slower growth rates than their respective BKKZ1436 and BKKZ1461 vector control strains.
Turbidity time course for K. pneumoniae PCI 602 (A) and P. aeruginosa PAO1 (B) derivatives harboring armA and/or npmA methyltransferase genes. Overnight cultures of each strain were inoculated into LB medium containing kanamycin and then incubated at 37 °C at 140 spm. Symbols: diamonds, BKKZ1436 (A) and BKKZ1461 (B) vector control strains; squares, BKKZ1437 (A) and BKKZ1463 (B) possessing armA; triangles, BKKZ1438 (A) and BKKZ1465 (B) possessing npmA; circles, BKKZ1443 (A) and BKKZ1467 (B) possessing armA and npmA
Evaluation of methylase gene stability in the plasmids
Incidentally, we observed that the NCGM59 strain had lost its resistance to apramycin after several subculturing procedures. We hypothesized that this may have occurred via the disruption of npmA. Therefore, we performed continuous subculturing experiments with the strains and analyzed the plasmids obtained from each successive culture. Another host strain, E. coli AG1, was also used for this experiment. Strains BKKZ1594, BKKZ1595, BKKZ1596, and BKKZ1597, which are AG1 derivatives transformed via the uptake of GS1, GS73, GS79, and GS81 plasmids, respectively, showed similar growth properties to those of the NCGM strains (data not shown). As expected, the size of the plasmid had altered over the 16 rounds of subculturing that had been performed in LB medium for all of the quintuple cultures in all the cultures of strains possessing npmA (Fig. 3A). On the one hand, eight subcultures (nearly equivalent of an eightieth generation) were needed to detect the plasmid alteration in NCGM59 and BKKZ1596 (Fig. S2A) and the cells harboring the original plasmid were not completely replaced by the new derivatives harboring the altered plasmid within the 16 subcultures. On the other hand, it is notable that only two subcultures were needed to detect the plasmid alteration and five subcultures were enough for the derivative strains to replace the original NCGM60 and BKKZ1597 strains completely (Fig. S2B).
A Agarose gel electrophoresis of the EcoRI digestion patterns of the plasmids extracted from the double or quintuple cultures of E. coli strains subjected to 16 rounds of subculturing. The strains were transformed with the original plasmids shown in the figure. The EcoT14I digest of λ DNA was used as the size marker. The size marker contains the following 11 discrete fragments (in base pairs): 19,329, 7743, 6223, 4254, 3472, 2690, 1882, 1489, 925, 421, and 74 (invisible). B Outline of the transposon insertion positions detected preferentially in npmA or armA from the plasmids shown in Fig. 3 (A). IS10, IS1, and IS5 are shown by white, pale gray, and dark gray circles, respectively. Alphabetical letters represent the culture IDs for each strain and bold font mean that the disruptant was found to be the most preferential
The sequencing analysis revealed that the GS79 and GS81 plasmids had their npmA or armA genes (including the untranslated regions) disrupted via addition of the insertion sequence (IS) in the all the cultures (Fig. 3B). In the DH5α derivative NCGM59 and NCGM60 strains, IS10 played a major role in plasmid disruption. In contrast, in the AG1 derivative strains BKKZ1596 and BKKZ1597, IS10 was not present in their genomic DNAs and, therefore, no IS10-inserted plasmids were identified in them. Alternatively, it is possible that these plasmids were disrupted by insertion of IS1 or IS5.
It is not unreasonable that the IS fragments were preferentially inserted into the npmA gene of the GS79 plasmid. But interestingly, all the IS fragments were preferentially inserted into the armA gene in the case of GS81, with the exception of one culture. Additionally, it should be noted that base substitutions, deletions, or insertions (other than transposons) were not observed in both armA and npmA throughout this experiment.
Effect of npmA on transposon movement
It was surprising to us that the npmA and armA genes in the npmA-containing plasmids were easily disrupted by the transposons. Therefore, we examined whether npmA could activate movement of the transposon. In this experiment, NCGM59, NCGM60, and BKKZ1054, which is the control strain possessing the aac(3)-IV apramycin acetyltransferase encoding gene, were cultivated continuously and the collected cells were analyzed by Southern blotting to detect the movement of IS10. Apramycin was used to prevent disruption of the npmA gene.
Agarose gel electrophoresis of the plasmids (Fig. 4A) and genomic Southern blotting analysis (Fig. 4B) revealed that movement of two IS10 elements, which DH5α possesses, was not observed in any of the triplicate cultures of BKKZ1054. By contrast, one extra band was detected in the Southern blot of the NCGM59 strain. This band probably comes from the plasmid disrupted by IS10, although the plasmid amount was too small to be detected by electrophoresis. In the case of the NCGM60 strain, electrophoresis and sequencing analyses revealed that the armA gene in the plasmid from all the triplicate cultures was disrupted by ISs and the original plasmids were completely excluded. Therefore, the additional band we detected probably comes from a plasmid disrupted by IS10, as detected by Southern blotting. However, no other extra bands were observed.
A Agarose gel electrophoresis showing the EcoRI digestion patterns of the plasmids extracted from triplet cultures of E. coli strains subjected to 0, 4, 8, and 12 rounds of subculturing. B Southern blot analysis of the genomic DNA from triplet cultures of E. coli strains subjected to 12 rounds of subculturing. Samples of the genomic DNA were digested with ClaI and the IS10 sequences were detected by Southern blotting. The size marker on the membrane (EcoT14I digest of λ DNA digest) was stained with azure C
Plasmid stability in the IS-less E. coli strain
To estimate the effect of the IS elements on the mutation frequency in the npmA-expressing E. coli cells, continuous subculture was performed using the transformants of the IS-less strain, MDS42 ∆recA. After 12 rounds of subculturing, the plasmids were extracted and analyzed. Although no drastic change in the plasmid size was observed (Fig. S3), deletions or base substitutions were observed in the GS79 plasmid in three of the quintuple cultures of BKKZ1753 and in the GS81 plasmid in four of the quintuple cultures of the BKKZ1754 strain (Table 5). Unlike the cases of NCGM60 and BKKZ1597, all the mutations in the bacteria from the BKKZ1754 cultures were observed in the npmA gene.
E. coli cell viability in the competition cultures
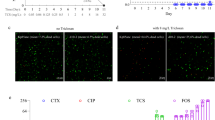
Lastly, we observed the time courses of cell viability of NCGM59 strain cocultured with NCGM57 or NCGM58. As shown in Fig. 5, CFU of NCGM59 strain was decreased to 1/100 of the end of growth phase even in the monoculture. In the competition cultures, CFU of NCGM59 strain was drastically decreased after stationary phase and was superseded by competition strain, regardless of the initial cell numbers.
Time courses of CFU in the competitive culture of NCGM59 with NCGM57 (A) or NCGM58 (B). Overnight cultures of NCGM59 strain and competitive strains were mixed at the ratio of 1:10 (diamond), 1:1 (triangle), or 10:1 (circle) and these mixtures were used for inoculation source. NCGM59 monoculture (square) was also performed in parallel. LB agar plates supplemented with chloramphenicol or apramycin were used to evaluate the total cell number (opened symbol, dashed line) or viable cell number of NCGM59 (closed symbol, solid line), respectively
Discussion
In this study, we investigated the properties of E. coli, P. aeruginosa, and K. pneumoniae strains that possess two RNA methyltransferase genes, armA and npmA. The different aminoglycoside-resistant spectrums among the strains possessing either or both of the methyltransferase genes seems to result from the difference of the mode of binding to the ribosome among aminoglycoside drugs. Broader drug-resistant spectrum in the strain possessing both armA and npmA is a reasonable outcome considering that more methylation of the decoding site makes it more difficult for aminoglycoside drugs to approach the site. Unlike the other aminoglycoside compounds we tested, streptomycin does not interact directly with positions 1405 and 1408 of 16S rRNA [12], and this may be the reason why streptomycin is active against the control strains. Additionally, acquisition of resistance against aminoglycosides by npmA was observed in three species of Gram-negative bacteria, implying that npmA-expressing strains of various Gram-negative genera could potentially be spread and isolated at any moment in time.
However, this does not actually happen, implying that methylation by NpmA is probably a double-edged sword; it would also disturb ribosome assembly and/or smooth and accurate translation, which would lead to decreased cell proliferation and poor survivability after the growth phase. This means that in the absence of aminoglycoside antibiotics, bacterial strains expressing NpmA will be easily excluded from the environment. In fact, npmA is inactivated by IS elements with great ease. Although the npmA gene was also inactivated by deletion or base substitution in the IS-less MDS42 strain, the frequency of mutation induction was much less than in the case of the DH5α derivatives and AG1, indicating that IS insertion is the principal cause of inactivation of npmA and armA co-expressed with npmA. Recently, a causal relationship has been established between IS elements and adaptation to some unfavorable environmental condition [13] such as high osmolarity [14], metal limitation [15], or nutrient-limitation [16]. Although we did not obtain any evidence that npmA stimulates the movement of IS elements, it seems likely that expression of this gene is unfavorable to cells and cells can easily adapt to this condition via IS elements.
If so, are we free from the threat of the rapid spread of npmA-possessing pathogens? This is possibly true, but we need to consider why the second report of an npmA-possessing strain took such a long time (14 years), because although this strain did not expand to become dominant, it did survive long enough to spread between Japan and China, at least. The two following possibilities may explain these observations.
The first possibility is that the stable maintenance of npmA in bacterial cells requires additional genetic variation in the bacterial chromosomal genes, such as those of the 16S rRNA or those encoding ribosomal proteins. In this scenario, the npmA transmission frequency would be lower than that of strains carrying other drug-resistant genes, even when npmA is located on highly transmittable plasmids. If additional genetic variation is needed in all of the multicopy 16S rRNA genes for npmA maintenance, then transmission would rarely occur. Genome analysis and biochemical analyses of the two isolates possessing npmA should provide us with clues to support or refute this possibility.
The second possibility is that the npmA gene spreads as a disruptant by ISs (or by other transposable elements). Given that npmA is easily inactivated by the insertion of IS elements, it is conceivable that these elements could also be easily eliminated from npmA and gain aminoglycoside antibiotic resistance again. If so, this could represent a novel, unique mechanism that could be classified as “ready to use IS-dependent resistance”, because npmA is usually inactivated by a transposon and only when the host cell is exposed to aminoglycoside does npmA become active by eliminating the IS elements. Although a bacterium harboring an IS-inactivated npmA gene has not yet been identified, the accumulating genome sequence data from clinical and community-acquired isolates, including data for aminoglycoside-sensitive strains, will disclose whether this IS-dependent mechanism actually exists.
It appears likely that the presence of the npmA gene is unfavorable for the growth and survival of general pathogenic bacteria, making it possible that the explosive spreading of npmA may not occur. However, further investigation to understand the mechanism of npmA maintenance in bacterial cells will also be needed to make a final judgment on the potential threat to public health posed by npmA-possessing pathogens.
Materials and methods
Bacterial strains
The bacterial strains used in this study are listed in Table 1. E. coli DH5α (TaKaRa Bio Inc., Shiga, Japan), AG1 (Agilent Technologies Japan, Ltd., Tokyo, Japan), the IS-less MDS42 strain [17] (Scarab Genomics, LCC, Madison, WI), P. aeruginosa PAO1, and K. pneumoniae PCI 602 were used to host the plasmids containing armA and/or npmA.
Plasmid construction and transformation
The plasmids used in this study are listed in Table 1. Plasmids GS73, GS79, and GS81 are derivatives of pSTV28 (TaKaRa Bio Inc., designated as GS1 in this study), which contains armA or npmA or both genes, respectively, in the multi-cloning site in lacZα. Plasmid pSTV-aac is a pSTV28 derivative containing the aac(3)-IV gene, which encodes an aminoglycoside 3-N-acetyltransferase. These plasmids were used to transform the E. coli strains. Plasmids pBHR-GS1/73/79/81 were made from GS1/73/79/81 by inserting the kanamycin-resistant aph(3′)-Ia gene and the genes for replication from the broad-host-range plasmid, pBHR1 [18] (MoBiTec GmbH, Göttingen, Germany). These plasmids were used to transform K. pneumoniae and P. aeruginosa by chemical transformation [19] and electroporation [20], respectively.
Evaluation of the antibacterial activities of the aminoglycoside compounds
Antibacterial activities of the aminoglycosides were evaluated by the agar dilution method. Overnight cultures of the test strains were diluted and spotted onto BD™ Difco™ Muller-Hinton agar (Thermo Fisher Scientific Kabushiki Kaisha, Kanagawa, Japan) containing the test compounds at concentrations of 0.031–128 µg/ml in a twofold dilution series. After incubation for 16 h at 37 °C, the antibacterial activities of the bacterial species were evaluated using the ten aminoglycoside compounds shown in Fig. S1. All of these compounds were of analytical grade or were ethical pharmaceuticals.
Proliferation properties
Overnight cultures of the different bacterial species were inoculated at 1% into fresh LB medium (3 ml) supplemented with chloramphenicol at 30 µg/ml (for E. coli) or 50 and 100 µg/ml of kanamycin for K. pneumoniae and P. aeruginosa, respectively. The cultures were incubated with shaking at 140 spm (strokes per minute) at 37 °C, and their turbidity time courses were monitored.
Continuous subculture
Single colonies of the test strains obtained by transformation were inoculated into 3 ml of LB medium supplemented with 30 µg/ml of chloramphenicol and the cultures were incubated overnight at 37 °C. Three microliters of each culture were added to 3 ml of LB medium supplemented with chloramphenicol, after which one was incubated for 24 h at 37 °C. Aliquots (3 µl) of the cultures were then used for the next subculture. This process was repeated 16 times at most. Where indicated, 30 µg/ml of apramycin was used instead of chloramphenicol.
To detect alterations in the plasmids, they were extracted from each culture using the QuickLyse Miniprep Kit (Qiagen K. K., Toyko, Japan), and then analyzed by EcoRI digestion and subsequent agarose gel electrophoresis. To determine the plasmid sequences, they were digested and tagged using the Nextera XT DNA Library Prep Kit (Illumina Kabushiki Kaisha, Tokyo, Japan), and then analyzed by MiSeq sequencing with the paired-end read 300-cycle option.
To detect movement of the IS10 insertion sequence, genomic DNA from the strains was extracted using the RBC Genomic DNA Extraction Kit Mini (RBC Bioscience, New Taipei City, Taiwan). Next, the genomic DNA samples were digested with ClaI and subjected to Southern blotting. A DIG DNA Labeling Kit (Roche Diagnostics K.K., Tokyo, Japan) was used to label the DNA probe, which contained the partial fragment (bases 438–765) of the IS10 transposase gene obtained by PCR amplification.
All reagents and chemicals used in this study were analytical grade and the restriction enzymes were purchased from New England Biolabs Japan (Tokyo, Japan).
Competition cultures
The overnight culture of NCGM59 strain in LB medium with 30 µg/ml of chloramphenicol at 37 °C was combined with the overnight culture of NCGM57 or NCGM58 at the ratio of 1:10, 1:1, and 10:1. Ten microliters of each mixture were inoculated in 10 ml of fresh LB medium supplemented with 30 µg/ml of chloramphenicol and the cultures were incubated at 37 °C. The colony forming units (CFU) of there cultures were periodically counted using LB agar plate supplemented with 30 µg/ml of chloramphenicol or apramycin to evaluate the total cell number or viable cell number of NCGM59, respectively.
References
WHO. Antimicrobial resistance: global report on surveillance. http://apps.who.int/iris/bitstream/10665/112642/1/9789241564748_eng.pdf. 2014.
Al-Tawfiq JA, Laxminarayan R, Mendelson M. How should we respond to the emergence of plasmid-mediated colistin resistance in humans and animals? Int J Infect Dis. 2017;54:77–84.
Sheng WH, Badal RE, Hsueh PR, on behalf of the SMART Program. Distribution of extended-spectrum β-lactamases, AmpC β-lactamases, and carbapenemases among enterobacteriaceae isolates causing intra-abdominal infections in the Asia-Pacific region: Results of the Study for Monitoring Antimicrobial Resistance Trends (SMART). Antimicrob Agents Chemother. 2013;57:2981–8.
Galimand M, Courvalin P, Lambert T. Plasmid-mediated high-level resistance to aminoglycosides in Enterobacteriaceae due to 16S rRNA methylation. Antimicrob Agents Chemother. 2003;47:2565–71.
Wachino J, Arakawa Y. Exogenously acquired 16S rRNA methyltransferases found in aminoglycoside-resistant pathogenic Gram-negative bacteria: an update. Drug Resist Updat. 2012;15:133–48.
Sekizuka T, et al. Complete sequencing of the blaNDM-1-positive IncA/C plasmid from Escherichia coli ST38 isolate suggests a possible origin from plant pathogens. PLoS ONE. 2011;6:e25334 https://doi.org/10.1371/journal.pone.0025334.
Ho PL, et al. Complete sequencing of pNDM-HK encoding NDM-1 carbapenemase from a multidrug-resistant Escherichia coli strain isolated in Hong Kong. PLoS ONE. 2011;6:e17989 https://doi.org/10.1371/journal.pone.0017989.
Waterman PE, et al. Bacterial peritonitis due to Acinetobacter baumannii sequence type 25 with plasmid-borne New Delhi metallo-β-lactamase in Honduras. Antimicrob Agents Chemother. 2013;57:4584–6.
Beauclerk AAD, Cundliffe E. Sites of action of two ribosomal RNA methylases responsible for resistance to aminoglycosides. J Mol Biol. 1987;193:661–71.
Wachino J, et al. Novel plasmid-mediated 16S rRNA m1A1408 methyltransferase, NpmA, found in a clinically isolated Escherichia coli strain resistant to structurally diverse aminoglycosides. Antimicrob Agents Chemother. 2007;51:4401–9.
Zhao Z, et al. Evaluation of automated systems for aminoglycosides and fluoroquinolones susceptibility testing for Carbapenem-resistant. Enterobact Antimicrob Resist Infect Control. 2017;6:77 https://doi.org/10.1186/s13756-017-0235-7.
Demirci H, et al. A structural basis for streptomycin-induced misreading of the genetic code. Nat Commun. 2013;4:1355 https://doi.org/10.1038/ncomms2346
Casacuberta E, González J. The impact of transposable elements in environmental adaptation. Mol Ecol. 2013;22:1503–17.
Stoebel DM, Dorman CJ. The effect of mobile element IS10 on experimental regulatory evolution in Escherichia coli. Mol Biol Evol. 2010;27:2105–12.
Chou HH, Berthet J, Marx CJ. Fast growth increases the selective advantage of a mutation arising recurrently during evolution under metal limitation. PLoS Genet. 2009;5:e1000652 https://doi.org/10.1371/journal.pgen.1000652.
Gaffé J, et al. Insertion sequence-driven evolution of Escherichia coli in chemostats. J Mol Evol. 2011;72:398–412.
Pósfai G, et al. Emergent properties of reduced-genome Escherichia coli. Science. 2006;312:1044–6.
Szpirer CY, Faelen M, Couturier M. Mobilization function of the pBHR1 plasmid, a derivative of the broad-host-range plasmid pBBR1. J Bacteriol. 2001;183:2101–10.
Merrick MJ, Gibbins JR, Postgate JR. A rapid and efficient method for plasmid transformation of Klebsiella pneumoniae and Escherichia coli. J Gen Microbiol. 1987;133:2053–7.
Dennis JJ, Sokol PA. Electrotransformaiton of Pseudomonas. Methods Mol Biol. 1995;47:125–33.
den Dunnen JT, et al. HGVS recommendations for the description of sequence variants: 2016 update. Hum Mutat. 2016;37:564–9.
Acknowledgements
We thank Ms. Sayaka Takahashi for technical assistance. This work is partially supported by Research Program on Emerging and Re-emerging Infectious Diseases from Japan Agency for Medical Research and Development, AMED (16fk0108120j0001).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Electronic supplementary material
Rights and permissions
About this article
Cite this article
Ishizaki, Y., Shibuya, Y., Hayashi, C. et al. Instability of the 16S rRNA methyltransferase-encoding npmA gene: why have bacterial cells possessing npmA not spread despite their high and broad resistance to aminoglycosides?. J Antibiot 71, 798–807 (2018). https://doi.org/10.1038/s41429-018-0070-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41429-018-0070-y
This article is cited by
-
Cycloimidamicins, Novel natural lead compounds for translation inhibition in Pseudomonas aeruginosa
The Journal of Antibiotics (2023)