Abstract
Background
Literature examining the relationship of circulating omega-3 and omega-6 polyunsaturated fatty acids [n-3(ω-3) and n-6 (ω-6) PUFAs] and arterial elasticity in large cohort-based populations are lacking. We investigated the association of circulating ω-3and ω-6 PUFAs with large artery elasticity (LAE) and small artery elasticity (SAE) in participants from the Multi-Ethnic Study of Atherosclerosis (MESA).
Methods
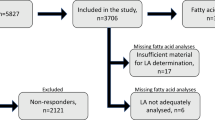
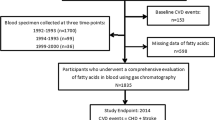
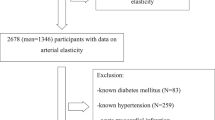
A total of 6124 participants (mean age 61.9; 52% female; 38% White, 27% Black, 22% Hispanic, and 13% Chinese-American) with plasma phospholipid PUFAs and arterial elasticity measured at baseline were included. LAE and SAE were derived from pulse contour analysis of the radial artery in all subjects in a supine position using tonometry. Linear regression models were used to determine associations for levels of (1) each circulating fatty acid, (2) total ω-3PUFAs, and (3) total ω-6 PUFAs with log-transformed LAE and SAE.
Results
Each standard deviation (SD) increment in circulating levels of total ω-3 PUFAs, eicosapentaenoic acid, and docosahexaenoic acid were associated with a 0.017 ml/mmHg, 0.017 ml/mmHg, and 0.015 ml/mmHg higher LAE respectively (p values all <0.01). No significant trends were observed for ω-3 PUFAs levels with SAE.22 Similarly, no significant trends were observed for ω-6 PUFA levels with either LAE or SAE.
Conclusions
In a multi-ethnic cohort of individuals free of baseline cardiovascular disease, higher plasma levels of total and individual ω-3 PUFAs were associated with an increased LAE. Further understanding into differential associations of ω-6 PUFAs with LAE and SAE is needed.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
Data availability
The data that support the findings of this study are available from MESA but restrictions apply to the availability of these data, which were used under license for the current study, and so are not publicly available. Data are however available from the authors upon reasonable request and with permission of MESA.
References
Albert CM, Hennekens CH, O’Donnell CJ, Ajani UA, Carey VJ, Willett WC, et al. Fish consumption and risk of sudden cardiac death. JAMA. 1998;279:23–28.
Harris WS, Kris-Etherton PM, Harris KA. Intakes of long-chain omega-3 fatty acid associated with reduced risk for death from coronary heart disease in healthy adults. Curr Atheroscler Rep. 2008;10:503–9.
Yokoyam M, Origasa H, Matsuzaki M, Matsuzawa Y, Saito Y, Ishikawa Y, et al. Effects of eicosapentaenoic acid on major coronary events in hypercholesterolaemic patients (JELIS): a randomised open-label, blinded endpoint analysis. Lancet. 2007;369:1090–8.
Bhatt DL, Steg G, Miller M, Brinton EA, Jacobson TA, Ketchum SB, et al. Cardiovascular risk reduction with icosapent ethyl for hypertriglyceridemia. N Engl J Med. 2019;380:11–22.
Sonnweber T, Pizzini A, Nairz M, Weiss G, Tancevski I. Arachidonic acid metabolites in cardiovascular and metabolic diseases. Int J Mol Sci. 2018;19:3285.
Simopoulos AP, Leaf A, Salem N Jr. Essentiality of and recommended dietary intakes for omega-6 and omega-3 fatty acids. Ann Nutr Metab. 1999;43:127–30.
Calder PC. Polyunsaturated fatty acids and inflammatory processes: New twists in an old tale. Biochimie 2009;91:791–5.
Shearer GC, Walker RE. An overview of the biologic effects of omega-6 oxylipins in humans. Prostaglandins Leukot Ess Fat Acids. 2018;137:26–38.
Marklund M, Wu JH, Imamura F, Del Gobbo LC, Fretts A, de Goede J, et al. Biomarkers of dietary Omega-6 fatty acids and incident cardiovascular disease and mortality: an individual-level pooled analysis of 30 cohort studies. Circulation 2019;139:2422–36.
Harris WS, Tintle NL, Imamura F, Qian F, Korat AV, Marklund M, et al. Blood n-3 fatty acid levels and total and cause-specific mortality from 17 prospective studies. Nat Commun. 2021;12:2329.
Vlachopoulos C, Aznaouridis K, Stefanadis C. Prediction of cardiovascular events and all-cause mortality with arterial stiffness: a systematic review and meta-analysis. J Am Coll Cardiol. 2010;55:1318–27.
Ben-Shlomo Y, Spears M, Boustred C, May M, Anderson SG, Benjamin EJ, et al. Aortic pulse wave velocity improves cardiovascular event prediction: an individual participant meta-analysis of prospective observational data from 17,635 subjects. J Am Coll Cardiol. 2014;63:636–46.
Redheuil A, Wu CO, Kachenoura N, Ohyama Y, Yan RT, Bertoni AG, et al. Proximal aortic distensibility is an independent predictor of all-cause mortality and incident CV events: the MESA study. J Am Coll Cardio. 2014;64:2619–29.
Bild DE, Bluemke DA, Burke GL, Detrano R, Diez Roux AV, Folsom AR, et al. Multi-ethnic study of atherosclerosis: objectives and design. Am J Epidemiol. 2002;156:871–81.
Cao J, Schwichtenberg KA, Hanson NQ, Tsai MY. Incorporation and clearance of omega-3 fatty acids in erythrocyte membranes and plasma phospholipids. Clin Chem. 2006;52:2265–72.
Duprez DA, Jacobs DR, Lutsey PL, Bluemke DA, Brumback LC, Polak JF, et al. Association of small artery elasticity with incident cardiovascular disease in older adults: the multi-ethnic study of atherosclerosis. Am J Epidemiol. 2011;174:528–36.
Brumback LC, Jacobs DR Jr, Dermond N, Chen H, Duprez DA. Reproducibility of arterial elasticity parameters derived from radial artery diastolic pulse contour analysis: the multi-ethnic study of atherosclerosis. Blood Press Monit. 2010;15:312–5.
Zimlichman R, Shargorodsky M, Boaz M, Duprez D, Rahn K, Rizzoni D, et al. Determination of arterial compliance using blood pressure waveform analysis with the CR-2000 system: Reliability, repeatability, and establishment of normal values for healthy European population–the seven European sites study (SESS). Am J Hypertens. 2005;18:65–71.
Alavi H, Prisant LM, Jupin D, Oracion A. Comparison of arterial elasticity measured in left and right arms using the HDI/Pulsewave CR-2000 Research System. Blood Press Monit. 2002;7:277–80.
Alidadi M, Montecucco F, Jamialahmadi T, Al-Rasadi K, Johnston TP, Sahebkar A. Beneficial effect of statin therapy on arterial stiffness. Biomed Res Int. 2021:5548310.
Chung H, Nettleton JA, Lemaitre RN, Barr RG, Tsai MY, Tracy RP, et al. Frequency and type of seafood consumed influence plasma (n-3) fatty acid concentrations. J Nutr. 2008;138:2422–7.
Mason RP. New insights into mechanisms of action for Omega-3 fatty acids in atherothrombotic cardiovascular disease. Curr Atheroscler Rep. 2019;21:2.
Endo J, Arita M. Cardioprotective mechanism of omega-3 polyunsaturated fatty acids. J Cardiol. 2016;67:22–27.
Duprez DA, Somasundaram PE, Sigurdsoon G, Hoke L, Florea N, Cohn JN. Relationship between C-reactive protein and arterial stiffness in an asymptomatic population. J Hum Hypertension. 2005;19:515–9.
Mori TA, Woodman RJ. The independent effects of eicosapentaenoic acid and docosahexaenoic acid on cardiovascular risk factors in humans. Curr Opin Clin Nutr Metab Care. 2006;9:95–104.
Codde JP, Croft KD, Barden A, Mathews E, Vandongen R, Beilin LJ. An inhibitory effect of dietary polyunsaturated fatty acids on renin secretion in the isolated perfused rat kidney. J Hypertens. 1984;2:265–70.
Tousoulis D, Plastiras A, Siasos G, Oikonomou E, Verveniotis A, Kokkou E, et al. Omega-3 PUFAs improved endothelial function and arterial stiffness with a parallel antiinflammatory effect in adults with metabolic syndrome. Atherosclerosis. 2014;232:10–16.
Siasos G, Tousoulis D, Oikonomou E, Zaromitidou M, Verveniotis A, Plastiras A, et al. Effects of omega-3 fatty acids on endothelial function, arterial wall properties, inflammatory and fibrinolytic status in smokers: a cross over study. Int J Cardiol. 2013;166:340–6.
Monahan KD, Feehan RP, Blaha C, McLaughlin DJ. Effect of omega-3 polyunsaturated fatty acid supplementation on central arterial stiffness and arterial wave reflections in young and older healthy adults. Physiol Rep. 2015;3:e12438.
Pase MP, Grima NA, Sarris J. Do long-chain n-3 fatty acids reduce arterial stiffness? A meta-analysis of randomised controlled trials. Br J Nutr. 2011;106:974–80.
Reinders I, Murphy RA, Song X, Mitchell GF, Visser M, Cotch MF. Higher plasma phospholipid n–3 PUFAs, but lower n–6 PUFAs, are associated with lower pulse wave velocity among older adults. J Nutr. 2015;145:2317–24.
Panaich S, Zalawadiya S, Veeranna V, Afonso L. Association between arterial elasticity indices and coronary artery calcium in a healthy multi-ethnic cohort. Cardiology. 2012;123:24–30.
Cohn JN, Duprez DA, Grandits GA. Arterial elasticity as part of a comprehensive assessment of cardiovascular risk and drug treatment. Hypertension. 2005;46:217–20.
Kohn JC, Lampi MC, Reinhart-King CA. Age-related vascular stiffening: causes and consequences. Front Genet. 2015;6:112.
Das UN. Long-chain polyunsaturated fatty acids interact with nitric oxide, superoxide anion, and transforming growth factor-beta to prevent human essential hypertension. Eur J Clin Nutr. 2004;58:195–203.
Saravanan P, Davidson NC, Schmidt EB, Calder PC. Cardiovascular effects of marine omega-3 fatty acids. Lancet. 2010;376:540–50.
Torrejon C, Jung UJ, Deckelbaum RJ. N-3 fatty acids and cardiovascular disease: Actions and molecular mechanisms. Prostaglandins Leukot Ess Fat Acids. 2007;77:319–26.
Tomiyama H, Matsumoto C, Odaira M, Yamada J, Yoshida M, Shiina K, et al. Relationships among the serum omega fatty acid levels, serum C-reactive protein levels and arterial stiffness/ wave reflection in Japanese men. Atherosclerosis. 2011;217:433–6.
Yamada T, Strong JP, Ishii T, Ueno T, Koyama M, Wagayama H, et al. Atherosclerosis and omega-3 fatty acids in the populations of a fishing village and a farming village in Japan. Atherosclerosis. 2000;153:469–81.
Fukuoka Y, Nuruki N, Amiya S, Tofuku K, Aosaki S, Tsubouchi H. Effects of a fish-based diet and administration of pure eicosapentaenoic acid on brachial-ankle pulse wave velocity in patients with cardiovascular risk factors. J Cardiol. 2014;63:211–7.
Nelson JR, Raskin S. The eicosapentaenoic acid:arachidonic acid ratio and its clinical utility in cardiovascular disease. Postgrad Med. 2019;131:268–77.
Manning TS, Shykoff BE, Izzo JL Jr. Validity and reliability of diastolic pulse contour analysis (Windkessel model) in humans. Hypertension. 2002;39:963–8.
Acknowledgements
We thank the staff and participants of the MESA study for their important contributions.
Funding
This research was supported by contracts HHSN268201500003I, N01-HC-95159, N01-HC-95160, N01-HC-95161, N01-HC-95162, N01-HC-95163, N01-HC-95164, N01-HC-95165, N01-HC-95166, N01-HC-95167, N01-HC-95168 and N01-HC-95169 and by grant R01-HL-127659 from the National Heart, Lung, and Blood Institute, and by grants UL1-TR-000040, UL1-TR-001079, and UL1-TR-001420 from NCATS.
Author information
Authors and Affiliations
Contributions
PG, WG, and MT contributed to the conception or design of the work. All contributed to the acquisition, analysis, or interpretation of data for the work. PG and WG drafted the manuscript. All critically revised the manuscript, gave final approval, and agree to be accountable for all aspects of work ensuring integrity and accuracy.
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing interests.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Rights and permissions
About this article
Cite this article
Garg, P.K., Guan, W., Nomura, S. et al. Associations of plasma omega-3 and omega-6 pufa levels with arterial elasticity: the multi-ethnic study of atherosclerosis. Eur J Clin Nutr 76, 1770–1775 (2022). https://doi.org/10.1038/s41430-022-01172-9
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/s41430-022-01172-9