Abstract
Ultra-processed foods (UPFs) and food additives have become ubiquitous components of the modern human diet. There is increasing evidence of an association between diets rich in UPFs and gut disease, including inflammatory bowel disease, colorectal cancer and irritable bowel syndrome. Food additives are added to many UPFs and have themselves been shown to affect gut health. For example, evidence shows that some emulsifiers, sweeteners, colours, and microparticles and nanoparticles have effects on a range of outcomes, including the gut microbiome, intestinal permeability and intestinal inflammation. Broadly speaking, evidence for the effect of UPFs on gut disease comes from observational epidemiological studies, whereas, by contrast, evidence for the effect of food additives comes largely from preclinical studies conducted in vitro or in animal models. Fewer studies have investigated the effect of UPFs or food additives on gut health and disease in human intervention studies. Hence, the aim of this article is to critically review the evidence for the effects of UPF and food additives on gut health and disease and to discuss the clinical application of these findings.
Key points
-
Ultra-processed foods (UPFs) are widely consumed in the food chain, and epidemiological studies indicate an increased risk of gut diseases, including inflammatory bowel disease, colorectal cancer and possibly irritable bowel syndrome.
-
A causal role of food processing on disease risk is challenging to identify as the body of evidence, although large, is almost entirely from observational cohorts or case–control studies, many of which measured UPF exposure using dietary methodologies not validated for this purpose and few were adjusted for the known dietary risk factors for those diseases.
-
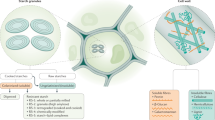
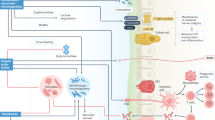
Food additives commonly added to UPFs, including emulsifiers, sweeteners, colours, and microparticles and nanoparticles, have been shown in preclinical studies to affect the gut, including the microbiome, intestinal permeability and intestinal inflammation.
-
Although a randomized controlled trial demonstrated that consumption of UPF resulted in increased energy intake and body weight, no studies have yet investigated the effect of UPFs, or their restriction, on gut health or disease.
-
Few studies have investigated the effect of dietary restriction of food additives on the risk or management of gut disease, although multicomponent diets have shown some initial promise.
This is a preview of subscription content, access via your institution
Access options
Access Nature and 54 other Nature Portfolio journals
Get Nature+, our best-value online-access subscription
$29.99 / 30 days
cancel any time
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout

Similar content being viewed by others
References
Baker, P. et al. Ultra-processed foods and the nutrition transition: global, regional and national trends, food systems transformations and political economy drivers. Obes. Rev. 21, e13126 (2020).
Sadler, C. R. et al. Processed food classification: conceptualisation and challenges. Trends Food Sci. Technol. 112, 149–162 (2021).
Monteiro, C. A., Cannon, G., Lawrence, M., Costa Louzada, M.L. & Pereira Machado, P. Ultra-Processed Foods, Diet Quality, and Health Using the NOVA Classification System (FAO, 2019).
Marino, M. et al. A systematic review of worldwide consumption of ultra-processed foods: findings and criticisms. Nutrients 13, 2778 (2021).
Bonaccio, M. et al. Ultra-processed food consumption is associated with increased risk of all-cause and cardiovascular mortality in the Moli-Sani study. Am. J. Clin. Nutr. 113, 446–455 (2021).
Gupta, S. et al. Characterising percentage energy from ultra-processed foods by participant demographics, diet quality and diet cost: findings from the Seattle Obesity Study (SOS) III. Br. J. Nutr. 126, 773–781 (2021).
Moubarac, J. C. et al. Processed and ultra-processed food products: consumption trends in Canada from 1938 to 2011. Can. J. Diet. Pract. Res. 75, 15–21 (2014).
Juul, F. & Hemmingsson, E. Trends in consumption of ultra-processed foods and obesity in Sweden between 1960 and 2010. Public Health Nutr. 18, 3096–3107 (2015).
Wang, L. et al. Trends in consumption of ultraprocessed foods among US Youths aged 2-19 years, 1999-2018. JAMA 326, 519–530 (2021).
Schnabel, L. et al. Association between ultraprocessed food consumption and risk of mortality among middle-aged adults in France. JAMA Intern. Med. 179, 490–498 (2019).
Ruggiero, E. et al. Ultra-processed food consumption and its correlates among Italian children, adolescents and adults from the Italian Nutrition & Health Survey (INHES) cohort study. Public Health Nutr. 24, 6258–6271 (2021).
Marron-Ponce, J. A., Flores, M., Cediel, G., Monteiro, C. A. & Batis, C. Associations between consumption of ultra-processed foods and intake of nutrients related to chronic non-communicable diseases in Mexico. J. Acad. Nutr. Diet. 119, 1852–1865 (2019).
Martini, D., Godos, J., Bonaccio, M., Vitaglione, P. & Grosso, G. Ultra-processed foods and nutritional dietary profile: a meta-analysis of nationally representative samples. Nutrients 13, 3390 (2021).
Griffin, J., Albaloul, A., Kopytek, A., Elliott, P. & Frost, G. Effect of ultraprocessed food intake on cardiometabolic risk is mediated by diet quality: a cross-sectional study. BMJ Nutr. Prev. Health 4, 174–180 (2021).
Gehring, J. et al. Consumption of ultra-processed foods by pesco-vegetarians, vegetarians, and vegans: associations with duration and age at diet initiation. J. Nutr. 151, 120–131 (2021).
Julia, C. et al. Respective contribution of ultra-processing and nutritional quality of foods to the overall diet quality: results from the NutriNet-Santé study. Eur. J. Nutr. 62, 157–164 (2023).
Dicken, S. J. & Batterham, R. L. The role of diet quality in mediating the association between ultra-processed food intake, obesity and health-related outcomes: a review of prospective cohort studies. Nutrients 14, 23 (2021).
Hess, J. M. et al. Dietary guidelines meet NOVA: developing a menu for a healthy dietary pattern using ultra-processed foods. J. Nutr. 153, 2472–2481 (2023).
Suksatan, W. et al. Ultra-processed food consumption and adult mortality risk: a systematic review and dose-response meta-analysis of 207,291 participants. Nutrients 14, 174 (2021).
Rico-Campa, A. et al. Association between consumption of ultra-processed foods and all cause mortality: SUN prospective cohort study. BMJ 365, l1949 (2019).
Du, S., Kim, H. & Rebholz, C. M. Higher ultra-processed food consumption is associated with increased risk of incident coronary artery disease in the atherosclerosis risk in communities study. J. Nutr. 151, 3746–3754 (2021).
Srour, B. et al. Ultra-processed food intake and risk of cardiovascular disease: prospective cohort study (NutriNet-Santé). BMJ 365, l1451 (2019).
Juul, F., Vaidean, G., Lin, Y., Deierlein, A. L. & Parekh, N. Ultra-processed foods and incident cardiovascular disease in the Framingham offspring study. J. Am. Coll. Cardiol. 77, 1520–1531 (2021).
Duan, M. J., Vinke, P. C., Navis, G., Corpeleijn, E. & Dekker, L. H. Ultra-processed food and incident type 2 diabetes: studying the underlying consumption patterns to unravel the health effects of this heterogeneous food category in the prospective Lifelines cohort. BMC Med. 20, 7 (2022).
Fiolet, T. et al. Consumption of ultra-processed foods and cancer risk: results from NutriNet-Santé prospective cohort. BMJ 360, k322 (2018).
Lane, M. M. et al. Ultraprocessed food and chronic noncommunicable diseases: a systematic review and meta-analysis of 43 observational studies. Obes. Rev. 22, e13146 (2021).
Hall, K. D. et al. Ultra-processed diets cause excess calorie intake and weight gain: an inpatient randomized controlled trial of ad libitum food intake. Cell Metab. 30, 226 (2019).
Scientific Advisory Committee on Nutrition. SACN Statement on Processed Foods and Health. gov.uk https://www.gov.uk/government/publications/sacn-statement-on-processed-foods-and-health (2023).
Chen, J. et al. Intake of ultra-processed foods is associated with an increased risk of Crohn’s disease: a cross-sectional and prospective analysis of 187,154 participants in the UK Biobank. J. Crohns Colitis 17, 535–552 (2022).
Vasseur, P. et al. Dietary patterns, ultra-processed food, and the risk of inflammatory bowel diseases in the NutriNet-Santé cohort. Inflamm. Bowel Dis. 27, 65–73 (2021).
Narula, N. et al. Association of ultra-processed food intake with risk of inflammatory bowel disease: prospective cohort study. BMJ 374, n1554 (2021).
Meyer, A. et al. Food processing and risk of Crohn’s disease and ulcerative colitis: a European prospective cohort study. Clin. Gastroenterol. Hepatol. 21, 1607–1616.e6 (2022).
Lo, C. H. et al. Ultra-processed foods and risk of Crohn’s disease and ulcerative colitis: a prospective cohort study. Clin. Gastroenterol. Hepatol. 20, e1323–e1337 (2022).
Narula, N. et al. Food processing and risk of inflammatory bowel disease: a systematic review and meta-analysis. Clin. Gastroenterol. Hepatol. 21, 2483–2495.e1 (2023).
Piovani, D. et al. Environmental risk factors for inflammatory bowel diseases: an umbrella review of meta-analyses. Gastroenterology 157, 647–659.e4 (2019).
Narula, N. et al. Enteral nutritional therapy for induction of remission in Crohn’s disease. Cochrane Database Syst. Rev. 4, CD000542 (2018).
Rutgeerts, P. et al. Effect of faecal stream diversion on recurrence of Crohn’s disease in the neoterminal ileum. Lancet 338, 771–774 (1991).
Schnabel, L. et al. Association between ultra-processed food consumption and functional gastrointestinal disorders: results from the French NutriNet-Santé cohort. Am. J. Gastroenterol. 113, 1217–1228 (2018).
Wang, L. et al. Association of ultra-processed food consumption with colorectal cancer risk among men and women: results from three prospective US cohort studies. BMJ 378, e068921 (2022).
Zhong, G. C. et al. Ultra-processed food consumption and the risk of pancreatic cancer in the prostate, lung, colorectal and ovarian cancer screening trial. Int. J. Cancer 152, 835–844 (2023).
El Kinany, K. et al. Food processing groups and colorectal cancer risk in Morocco: evidence from a nationally representative case-control study. Eur. J. Nutr. 61, 2507–2515 (2022).
Fliss-Isakov, N., Zelber-Sagi, S., Ivancovsky-Wajcman, D., Shibolet, O. & Kariv, R. Ultra-processed food intake and smoking interact in relation with colorectal adenomas. Nutrients 12, 3507 (2020).
Romaguera, D. et al. Consumption of ultra-processed foods and drinks and colorectal, breast, and prostate cancer. Clin. Nutr. 40, 1537–1545 (2021).
Shu, L. et al. Association between ultra-processed food intake and risk of colorectal cancer: a systematic review and meta-analysis. Front. Nutr. 10, 1170992 (2023).
Arayici, M. E., Mert-Ozupek, N., Yalcin, F., Basbinar, Y. & Ellidokuz, H. Soluble and insoluble dietary fiber consumption and colorectal cancer risk: a systematic review and meta-analysis. Nutr. Cancer 74, 2412–2425 (2022).
Di, Y., Ding, L., Gao, L. & Huang, H. Association of meat consumption with the risk of gastrointestinal cancers: a systematic review and meta-analysis. BMC Cancer 23, 782 (2023).
Khandpur, N. et al. Categorising ultra-processed foods in large-scale cohort studies: evidence from the Nurses’ Health Studies, the Health Professionals Follow-up Study, and the Growing Up Today Study. J. Nutr. Sci. 10, e77 (2021).
Lo, C. H. et al. Ultra-processed foods and risk of Crohn’s disease and ulcerative colitis: a prospective cohort study. Clin. Gastroenterol. Hepatol. 20, e1323–e1337 (2021).
Sokol, H. et al. Faecalibacterium prausnitzii is an anti-inflammatory commensal bacterium identified by gut microbiota analysis of Crohn disease patients. Proc. Natl Acad. Sci. USA 105, 16731–16736 (2008).
Chervy, M., Barnich, N. & Denizot, J. Adherent-invasive E. coli: update on the lifestyle of a troublemaker in Crohn’s disease. Int. J. Mol. Sci. 21, 3734 (2020).
Nagao-Kitamoto, H. et al. Functional characterization of inflammatory bowel disease-associated gut dysbiosis in gnotobiotic mice. Cell Mol. Gastroenterol. Hepatol. 2, 468–481 (2016).
Travinsky-Shmul, T. et al. Ultra-processed food impairs bone quality, increases marrow adiposity and alters gut microbiome in mice. Foods 10, 3107 (2021).
Cuevas-Sierra, A., Milagro, F. I., Aranaz, P., Martinez, J. A. & Riezu-Boj, J. I. Gut microbiota differences according to ultra-processed food consumption in a Spanish population. Nutrients 13, 2710 (2021).
Hidalgo-Cantabrana, C. et al. Bifidobacteria and their health-promoting effects. Microbiol. Spectr. https://doi.org/10.1128/microbiolspec.BAD-0010-2016 (2017).
Garcia-Vega, A. S., Corrales-Agudelo, V., Reyes, A. & Escobar, J. S. Diet quality, food groups and nutrients associated with the gut microbiota in a nonwestern population. Nutrients 12, 2938 (2020).
Regulation (EC) No 1333/2008 of the European Parliament and the Council of 16 December 2008 on Food Additives. gov.uk https://www.legislation.gov.uk/eur/2008/1333/contents#:~:Text=Regulation%20(EC)%20No%201333%2F,additives%20(Text%20with%20EEA%20relevance (2008).
Fennema, O. R. Food additives — an unending controversy. Am. J. Clin. Nutr. 46, 201–203 (1987).
Food Standards Agency. Approved additives and E numbers. Food Standards Agency https://www.food.gov.uk/business-guidance/approved-additives-and-e-numbers (2018).
CODEX Alimentarius: International Food Standards. Class Names and the International Numbering System for Food Additives. Report no. CAC/GL 36-1989 (FAO & WHO, 2015).
Trakman, G. L. et al. Processed food as a risk factor for the development and perpetuation of Crohn’s disease — the ENIGMA study. Nutrients 14, 3627 (2022).
Srour, B. & Touvier, M. Ultra-processed foods and human health: what do we already know and what will further research tell us? EClinicalMedicine 32, 100747 (2021).
Cox, S., Sandall, A., Smith, L., Rossi, M. & Whelan, K. Food additive emulsifiers: a review of their role in foods, legislation and classifications, presence in food supply, dietary exposure, and safety assessment. Nutr. Rev. 79, 726–741 (2020).
Chazelas, E. et al. Exposure to food additive mixtures in 106,000 French adults from the NutriNet-Santé cohort. Sci. Rep. 11, 19680 (2021).
Vin, K. et al. Estimation of the dietary intake of 13 priority additives in France, Italy, the UK and Ireland as part of the FACET project. Food Addit. Contam. Part A Chem. Anal. Control. Expo. Risk Assess. 30, 2050–2080 (2013).
Swidsinski, A. et al. Bacterial overgrowth and inflammation of small intestine after carboxymethylcellulose ingestion in genetically susceptible mice. Inflamm. Bowel Dis. 15, 359–364 (2009).
Roberts, C. L. et al. Translocation of Crohn’s disease Escherichia coli across M-cells: contrasting effects of soluble plant fibres and emulsifiers. Gut 59, 1331–1339 (2010).
Maronpot, R. R., Davis, J., Moser, G., Giri, D. K. & Hayashi, S. M. Evaluation of 90-day oral rat toxicity studies on the food additive, gum ghatti. Food Chem. Toxicol. 51, 215–224 (2013).
Chassaing, B. et al. Dietary emulsifiers impact the mouse gut microbiota promoting colitis and metabolic syndrome. Nature 519, 92–96 (2015).
Lecomte, M. et al. Dietary emulsifiers from milk and soybean differently impact adiposity and inflammation in association with modulation of colonic goblet cells in high-fat fed mice. Mol. Nutr. Food Res. 60, 609–620 (2016).
Viennois, E., Merlin, D., Gewirtz, A. T. & Chassaing, B. Dietary emulsifier-induced low-grade inflammation promotes colon carcinogenesis. Cancer Res. 77, 27–40 (2017).
Chassaing, B., Van de Wiele, T., De Bodt, J., Marzorati, M. & Gewirtz, A. T. Dietary emulsifiers directly alter human microbiota composition and gene expression ex vivo potentiating intestinal inflammation. Gut 66, 1414–1427 (2017).
Jiang, Z. et al. Antimicrobial emulsifier-glycerol monolaurate induces metabolic syndrome, gut microbiota dysbiosis, and systemic low-grade inflammation in low-fat diet fed mice. Mol. Nutr. Food Res. 62, 1700547 (2018).
Lock, J. Y., Carlson, T. L., Wang, C. M., Chen, A. & Carrier, R. L. Acute exposure to commonly ingested emulsifiers alters intestinal mucus structure and transport properties. Sci. Rep. 8, 10008 (2018).
Laudisi, F. et al. The food additive maltodextrin promotes endoplasmic reticulum stress-driven mucus depletion and exacerbates intestinal inflammation. Cell Mol. Gastroenterol. Hepatol. 7, 457–473 (2019).
Holder, M. K. et al. Dietary emulsifiers consumption alters anxiety-like and social-related behaviors in mice in a sex-dependent manner. Sci. Rep. 9, 172 (2019).
Temkin, A. M. et al. Increased adiposity, inflammation, metabolic disruption and dyslipidemia in adult male offspring of DOSS treated C57BL/6 dams. Sci. Rep. 9, 1530 (2019).
Furuhashi, H. et al. Dietary emulsifier polysorbate-80-induced small-intestinal vulnerability to indomethacin-induced lesions via dysbiosis. J. Gastroenterol. Hepatol. 35, 110–117 (2020).
Zhao, M. et al. Modulation of the gut microbiota during high-dose glycerol monolaurate-mediated amelioration of obesity in mice fed a high-fat diet. mBio 11, e00190-20 (2020).
Sandall, A. M. et al. Emulsifiers impact colonic length in mice and emulsifier restriction is feasible in people with Crohn’s disease. Nutrients 12, 2827 (2020).
Miclotte, L. et al. Dietary emulsifiers alter composition and activity of the human gut microbiota in vitro, irrespective of chemical or natural emulsifier origin. Front. Microbiol. 11, 577474 (2020).
Nishimura, S. et al. Polysorbate 80-induced leaky gut impairs skeletal muscle metabolism in mice. Physiol. Rep. 8, e14629 (2020).
Viennois, E. et al. Dietary emulsifiers directly impact adherent-invasive E. coli gene expression to drive chronic intestinal inflammation. Cell Rep. 33, 108229 (2020).
Viennois, E. & Chassaing, B. Consumption of select dietary emulsifiers exacerbates the development of spontaneous intestinal adenoma. Int. J. Mol. Sci. 22, 2602 (2021).
Naimi, S., Viennois, E., Gewirtz, A. T. & Chassaing, B. Direct impact of commonly used dietary emulsifiers on human gut microbiota. Microbiome 9, 66 (2021).
Um, C. Y. et al. Association of emulsifier and highly processed food intake with circulating markers of intestinal permeability and inflammation in the cancer prevention study-3 diet assessment sub-study. Nutr. Cancer 74, 1701–1711 (2021).
Rousta, E. et al. The emulsifier carboxymethylcellulose induces more aggressive colitis in humanized mice with inflammatory bowel disease microbiota than polysorbate-80. Nutrients 13, 3565 (2021).
Chassaing, B. et al. Randomized controlled-feeding study of dietary emulsifier carboxymethylcellulose reveals detrimental impacts on the gut microbiota and metabolome. Gastroenterology 162, 743–756 (2022).
Viennois, E. & Chassaing, B. First victim, later aggressor: how the intestinal microbiota drives the pro-inflammatory effects of dietary emulsifiers? Gut Microbes 9, 1–4 (2018).
Daniel, N., Lecuyer, E. & Chassaing, B. Host/microbiota interactions in health and diseases — time for mucosal microbiology! Mucosal Immunol. 14, 1006–1016 (2021).
Jin, G. et al. Maternal emulsifier p80 intake induces gut dysbiosis in offspring and increases their susceptibility to colitis in adulthood. mSystems 6, e01337-20 (2021).
Tang, Q. et al. Early life dietary emulsifier exposure predisposes the offspring to obesity through gut microbiota-FXR axis. Food Res. Int. 162, 111921 (2022).
Bhattacharyya, S. et al. A randomized trial of the effects of the no-carrageenan diet on ulcerative colitis disease activity. Nutr. Healthy Aging 4, 181–192 (2017).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT04046913 (2024).
Gardner, C. et al. Nonnutritive sweeteners: current use and health perspectives: a scientific statement from the American Heart Association and the American Diabetes Association. Diabetes Care 35, 1798–1808 (2012).
Roberts, A., Renwick, A. G., Sims, J. & Snodin, D. J. Sucralose metabolism and pharmacokinetics in man. Food Chem. Toxicol. 38, S31–41 (2000).
Byard, J. L. & Goldberg, L. The metabolism of saccharin in laboratory animals. Food Cosmet. Toxicol. 11, 391–402 (1973).
Asif, M. The prevention and control the type-2 diabetes by changing lifestyle and dietary pattern. J. Educ. Health Promot. 3, 1 (2014).
Sylvetsky, A. C., Welsh, J. A., Brown, R. J. & Vos, M. B. Low-calorie sweetener consumption is increasing in the United States. Am. J. Clin. Nutr. 96, 640–646 (2012).
Fitch, S. E. et al. Use of acceptable daily intake (ADI) as a health-based benchmark in nutrition research studies that consider the safety of low-calorie sweeteners (LCS): a systematic map. BMC Public Health 21, 956 (2021).
Qin, X. Etiology of inflammatory bowel disease: a unified hypothesis. World J. Gastroenterol. 18, 1708–1722 (2012).
Suez, J. et al. Artificial sweeteners induce glucose intolerance by altering the gut microbiota. Nature 514, 181–186 (2014).
Rodriguez-Palacios, A. et al. The artificial sweetener splenda promotes gut proteobacteria, dysbiosis, and myeloperoxidase reactivity in Crohn’s disease-like ileitis. Inflamm. Bowel Dis. 24, 1005–1020 (2018).
Magnuson, B. A. et al. Aspartame: a safety evaluation based on current use levels, regulations, and toxicological and epidemiological studies. Crit. Rev. Toxicol. 37, 629–727 (2007).
Palmnas, M. S. et al. Low-dose aspartame consumption differentially affects gut microbiota-host metabolic interactions in the diet-induced obese rat. PLoS ONE 9, e109841 (2014).
Zani, F. et al. The dietary sweetener sucralose is a negative modulator of T cell-mediated responses. Nature 615, 705–711 (2023).
Bian, X. et al. Gut microbiome response to sucralose and its potential role in inducing liver inflammation in mice. Front. Physiol. 8, 487 (2017).
Bian, X. et al. Saccharin induced liver inflammation in mice by altering the gut microbiota and its metabolic functions. Food Chem. Toxicol. 107, 530–539 (2017).
Markus, V. et al. Inhibitory effects of artificial sweeteners on bacterial quorum sensing. Int. J. Mol. Sci. 22, 9863 (2021).
Landman, C. et al. Inter-kingdom effect on epithelial cells of the N-Acyl homoserine lactone 3-oxo-C12:2, a major quorum-sensing molecule from gut microbiota. PLoS ONE 13, e0202587 (2018).
Li, X. et al. Sucralose promotes colitis-associated colorectal cancer risk in a murine model along with changes in microbiota. Front. Oncol. 10, 710 (2020).
Shil, A. et al. Artificial sweeteners disrupt tight junctions and barrier function in the intestinal epithelium through activation of the sweet taste receptor, T1R3. Nutrients 12, 1862 (2020).
Guo, M. et al. Sucralose enhances the susceptibility to dextran sulfate sodium (DSS) induced colitis in mice with changes in gut microbiota. Food Funct. 12, 9380–9390 (2021).
Hanawa, Y. et al. Acesulfame potassium induces dysbiosis and intestinal injury with enhanced lymphocyte migration to intestinal mucosa. J. Gastroenterol. Hepatol. 36, 3140–3148 (2021).
Basson, A. R., Rodriguez-Palacios, A. & Cominelli, F. Artificial sweeteners: history and new concepts on inflammation. Front. Nutr. 8, 746247 (2021).
Lobach, A. R., Roberts, A. & Rowland, I. R. Assessing the in vivo data on low/no-calorie sweeteners and the gut microbiota. Food Chem. Toxicol. 124, 385–399 (2019).
Hugenholtz, F. & de Vos, W. M. Mouse models for human intestinal microbiota research: a critical evaluation. Cell Mol. Life Sci. 75, 149–160 (2018).
Seok, J. et al. Genomic responses in mouse models poorly mimic human inflammatory diseases. Proc. Natl Acad. Sci. USA 110, 3507–3512 (2013).
Frankenfeld, C. L., Sikaroodi, M., Lamb, E., Shoemaker, S. & Gillevet, P. M. High-intensity sweetener consumption and gut microbiome content and predicted gene function in a cross-sectional study of adults in the United States. Ann. Epidemiol. 25, 736–742.e4 (2015).
Thomson, P., Santibanez, R., Aguirre, C., Galgani, J. E. & Garrido, D. Short-term impact of sucralose consumption on the metabolic response and gut microbiome of healthy adults. Br. J. Nutr. 122, 856–862 (2019).
Serrano, J. et al. High-dose saccharin supplementation does not induce gut microbiota changes or glucose intolerance in healthy humans and mice. Microbiome 9, 11 (2021).
Ahmad, S. Y., Friel, J. & Mackay, D. The effects of non-nutritive artificial sweeteners, aspartame and sucralose, on the gut microbiome in healthy adults: secondary outcomes of a randomized double-blinded crossover clinical trial. Nutrients 12, 3408 (2020).
Mendoza-Martinez, V. M. et al. Is a non-caloric sweetener-free diet good to treat functional gastrointestinal disorder symptoms? A randomized controlled trial. Nutrients 14, 1095 (2022).
Riboli, E. et al. Carcinogenicity of aspartame, methyleugenol, and isoeugenol. Lancet Oncol. 24, 848–850 (2023).
Stepien, M. et al. Consumption of soft drinks and juices and risk of liver and biliary tract cancers in a European cohort. Eur. J. Nutr. 55, 7–20 (2016).
Jones, G. S. et al. Sweetened beverage consumption and risk of liver cancer by diabetes status: a pooled analysis. Cancer Epidemiol. 79, 102201 (2022).
McCullough, M. L., Hodge, R. A., Campbell, P. T., Guinter, M. A. & Patel, A. V. Sugar- and artificially-sweetened beverages and cancer mortality in a large U.S. prospective cohort. Cancer Epidemiol. Biomark. Prev. 31, 1907–1918 (2022).
Zhao, L. et al. Sugar-sweetened and artificially sweetened beverages and risk of liver cancer and chronic liver disease mortality. JAMA 330, 537–546 (2023).
European Food Safety Authority. Food colours. European Food Safety Authority https://www.efsa.europa.eu/en/topics/topic/food-colours (2023).
Sharma, V., McKone, H. T. & Markow, P. G. A global perspective on the history, use, and identification of synthetic food dyes. J. Chem. Educ. 88, 24–28 (2011).
Bastaki, M., Farrell, T., Bhusari, S., Bi, X. & Scrafford, C. Estimated daily intake and safety of FD&C food-colour additives in the US population. Food Addit. Contam. Part A Chem. Anal. Control. Expo. Risk Assess. 34, 891–904 (2017).
He, Z. et al. Food colorants metabolized by commensal bacteria promote colitis in mice with dysregulated expression of interleukin-23. Cell Metab. 33, 1358–1371.e5 (2021).
Chen, L. et al. Diet modifies colonic microbiota and CD4+ T-cell repertoire to induce flares of colitis in mice with myeloid-cell expression of interleukin 23. Gastroenterology 155, 1177–1191.e16 (2018).
Feng, J., Cerniglia, C. E. & Chen, H. Toxicological significance of azo dye metabolism by human intestinal microbiota. Front. Biosci. 4, 568–586 (2012).
Zou, L. et al. Bacterial metabolism rescues the inhibition of intestinal drug absorption by food and drug additives. Proc. Natl Acad. Sci. USA 117, 16009–16018 (2020).
Kwon, Y. H. et al. Chronic exposure to synthetic food colorant Allura Red AC promotes susceptibility to experimental colitis via intestinal serotonin in mice. Nat. Commun. 13, 7617 (2022).
Lomer, M. C., Thompson, R. P. & Powell, J. J. Fine and ultrafine particles of the diet: influence on the mucosal immune response and association with Crohn’s disease. Proc. Nutr. Soc. 61, 123–130 (2002).
Becker, H. M., Bertschinger, M. M. & Rogler, G. Microparticles and their impact on intestinal immunity. Dig. Dis. 30, 47–54 (2012).
European Food Safety Authority. Safety assessment of titanium dioxide (e171) as a food additive. EFSA J. 19, e06585 (2021).
Lomer, M. C. et al. Dietary sources of inorganic microparticles and their intake in healthy subjects and patients with Crohn’s disease. Br. J. Nutr. 92, 947–955 (2004).
Huybrechts, I. et al. Long-term dietary exposure to different food colours in young children living in different European countries. EFSA Supporting Publ. 7, 53E (2010).
Ruiz, P. A. et al. Titanium dioxide nanoparticles exacerbate DSS-induced colitis: role of the NLRP3 inflammasome. Gut 66, 1216–1224 (2017).
Bettini, S. et al. Food-grade TiO2 impairs intestinal and systemic immune homeostasis, initiates preneoplastic lesions and promotes aberrant crypt development in the rat colon. Sci. Rep. 7, 40373 (2017).
Proquin, H. et al. Transcriptomics analysis reveals new insights in E171-induced molecular alterations in a mouse model of colon cancer. Sci. Rep. 8, 9738 (2018).
Urrutia-Ortega, I. M. et al. Food-grade titanium dioxide exposure exacerbates tumor formation in colitis associated cancer model. Food Chem. Toxicol. 93, 20–31 (2016).
Pineton de Chambrun, G. et al. Aluminum enhances inflammation and decreases mucosal healing in experimental colitis in mice. Mucosal Immunol. 7, 589–601 (2014).
Talbot, P. et al. Food-grade TiO2 is trapped by intestinal mucus in vitro but does not impair mucin O-glycosylation and short-chain fatty acid synthesis in vivo: implications for gut barrier protection. J. Nanobiotechnol. 16, 53 (2018).
Powell, J. J. et al. Characterisation of inorganic microparticles in pigment cells of human gut associated lymphoid tissue. Gut 38, 390–395 (1996).
Lomer, M. C. et al. Lack of efficacy of a reduced microparticle diet in a multi-centred trial of patients with active Crohn’s disease. Eur. J. Gastroenterol. Hepatol. 17, 377–384 (2005).
Lomer, M. C., Harvey, R. S., Evans, S. M., Thompson, R. P. & Powell, J. J. Efficacy and tolerability of a low microparticle diet in a double blind, randomized, pilot study in Crohn’s disease. Eur. J. Gastroenterol. Hepatol. 13, 101–106 (2001).
Vasant, D. H. & Ford, A. C. Functional gastrointestinal disorders in inflammatory bowel disease: time for a paradigm shift? World J. Gastroenterol. 26, 3712–3719 (2020).
Cox, S. R. et al. Effects of low FODMAP diet on symptoms, fecal microbiome, and markers of inflammation in patients with quiescent inflammatory bowel disease in a randomized trial. Gastroenterology 158, 176–188.e7 (2020).
Levine, A. et al. Crohn’s disease exclusion diet plus partial enteral nutrition induces sustained remission in a randomized controlled trial. Gastroenterology 157, 440–450.e8 (2019).
Logan, M. et al. Analysis of 61 exclusive enteral nutrition formulas used in the management of active Crohn’s disease — new insights into dietary disease triggers. Aliment. Pharmacol. Ther. 51, 935–947 (2020).
Yanai, H. et al. The Crohn’s disease exclusion diet for induction and maintenance of remission in adults with mild-to-moderate Crohn’s disease (CDED-AD): an open-label, pilot, randomised trial. Lancet Gastroenterol. Hepatol. 7, 49–59 (2022).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT03171246 (2024).
US National Library of Medicine. ClinicalTrials.gov https://clinicaltrials.gov/ct2/show/NCT04225689 (2020).
Koios, D., Machado, P. & Lacy-Nichols, J. Representations of ultra-processed foods: a global analysis of how dietary guidelines refer to levels of food processing. Int. J. Health Policy Manag. 11, 2588–2599 (2022).
Global Food Research Program. Fiscal policies. Global Food Research Program https://www.globalfoodresearchprogram.org/policy-research/fiscal-policies/ (2023).
Srour, B. et al. Effect of a new graphically modified Nutri-Score on the objective understanding of foods’ nutrient profile and ultraprocessing: a randomised controlled trial. BMJ Nutr. Prev. Health 6, 108–118 (2023).
Tobias, D. K. & Hall, K. D. Eliminate or reformulate ultra-processed foods? Biological mechanisms matter. Cell Metab. 33, 2314–2315 (2021).
Braesco, V. et al. Ultra-processed foods: how functional is the NOVA system? Eur. J. Clin. Nutr. 76, 1245–1253 (2022).
Institute of Grocery Distribution. Ultraprocessed foods: a consumer perspective. IGD https://www.igd.com/articles/article-viewer/t/ultra-processed-foods-a-consumer-perspective/i/30969 (2023).
Staudacher, H. M., Yao, C. K., Chey, W. D. & Whelan, K. Optimal design of clinical trials of dietary interventions in disorders of gut-brain interaction. Am. J. Gastroenterol. 117, 973–984 (2022).
Sandall, A., Smith, L., Svensen, E. & Whelan, K. Emulsifiers in ultra-processed foods in the United Kingdom food supply. Public Health Nutr. 26, 2256–2270 (2023).
Chazelas, E. et al. Food additives: distribution and co-occurrence in 126,000 food products of the French market. Sci. Rep. 10, 3980 (2020).
Staudacher, H. M., Irving, P. M., Lomer, M. C. E. & Whelan, K. The challenges of control groups, placebos and blinding in clinical trials of dietary interventions. Proc. Nutr. Soc. 76, 203–212 (2017).
Ramirez Carnero, A. et al. Presence of perfluoroalkyl and polyfluoroalkyl substances (PFAS) in food contact materials (FCM) and its migration to food. Foods 10, 1443 (2021).
Li, J. et al. Per- and polyfluoroalkyl substances exposure and its influence on the intestinal barrier: an overview on the advances. Sci. Total. Env. 852, 158362 (2022).
Daniel, N., Gewirtz, A. T. & Chassaing, B. Akkermansia muciniphila counteracts the deleterious effects of dietary emulsifiers on microbiota and host metabolism. Gut 72, 906–917 (2023).
Kordahi, M. C., Delaroque, C., Bredeche, M. F., Gewirtz, A. T. & Chassaing, B. Vaccination against microbiota motility protects mice from the detrimental impact of dietary emulsifier consumption. PLoS Biol. 21, e3002289 (2023).
Bian, X. et al. The artificial sweetener acesulfame potassium affects the gut microbiome and body weight gain in CD-1 mice. PLoS ONE 12, e0178426 (2017).
Wang, Q. P., Browman, D., Herzog, H. & Neely, G. G. Non-nutritive sweeteners possess a bacteriostatic effect and alter gut microbiota in mice. PLoS ONE 13, e0199080 (2018).
Van den Abbeele, P. et al. Low-no-calorie sweeteners exert marked compound-specific impact on the human gut microbiota ex vivo. Int. J. Food Sci. Nutr. 74, 630–644 (2023).
Chi, L. et al. Effects of the artificial sweetener neotame on the gut microbiome and fecal metabolites in mice. Molecules 23, 367 (2018).
Anderson, R. L. & Kirkland, J. J. The effect of sodium saccharin in the diet on caecal microflora. Food Cosmet. Toxicol. 18, 353–355 (1980).
Becker, S. L. et al. Effect of stevia on the gut microbiota and glucose tolerance in a murine model of diet-induced obesity. FEMS Microbiol. Ecol. 96, fiaa079 (2020).
Shil, A. & Chichger, H. Artificial sweeteners negatively regulate pathogenic characteristics of two model gut bacteria, E. coli and E. faecalis. Int. J. Mol. Sci. 22, 5228 (2021).
Abou-Donia, M. B., El-Masry, E. M., Abdel-Rahman, A. A., McLendon, R. E. & Schiffman, S. S. Splenda alters gut microflora and increases intestinal p-glycoprotein and cytochrome p-450 in male rats. J. Toxicol. Env. Health A 71, 1415–1429 (2008).
Zheng, Z. et al. Low dose of sucralose alter gut microbiome in mice. Front. Nutr. 9, 848392 (2022).
Uebanso, T. et al. Effects of low-dose non-caloric sweetener consumption on gut microbiota in mice. Nutrients 9, 560 (2017).
Escoto, J. A. et al. Chronic consumption of sweeteners in mice and its effect on the immune system and the small intestine microbiota. Biomedica 41, 504–530 (2021).
Rosales-Gomez, C. A. et al. Chronic consumption of sweeteners and its effect on glycaemia, cytokines, hormones, and lymphocytes of GALT in CD1 mice. Biomed. Res. Int. 2018, 1345282 (2018).
Gerasimidis, K. et al. The impact of food additives, artificial sweeteners and domestic hygiene products on the human gut microbiome and its fibre fermentation capacity. Eur. J. Nutr. 59, 3213–3230 (2020).
Suez, J. et al. Personalized microbiome-driven effects of non-nutritive sweeteners on human glucose tolerance. Cell 185, 3307–3328.e19 (2022).
Svolos, V. et al. Treatment of active Crohn’s disease with an ordinary food-based diet that replicates exclusive enteral nutrition. Gastroenterology 156, 1354–1367.e6 (2019).
Lewis, J. D. et al. A randomized trial comparing the specific carbohydrate diet to a Mediterranean diet in adults with Crohn’s disease. Gastroenterology 161, 837–852.e9 (2021).
Konijeti, G. G. et al. Efficacy of the autoimmune protocol diet for inflammatory bowel disease. Inflamm. Bowel Dis. 23, 2054–2060 (2017).
Albenberg, L. et al. A diet low in red and processed meat does not reduce rate of Crohn’s disease flares. Gastroenterology 157, 128–136.e5 (2019).
Slimani, N. et al. Contribution of highly industrially processed foods to the nutrient intakes and patterns of middle-aged populations in the European Prospective Investigation into Cancer and Nutrition study. Eur. J. Clin. Nutr. 63, S206–225, (2009).
Eicher-Miller, H. A., Fulgoni, V. L. III & Keast, D. R. Energy and nutrient intakes from processed foods differ by sex, income status, and race/ethnicity of US adults. J. Acad. Nutr. Diet. 115, 907–918.e6 (2015).
Acknowledgements
The authors acknowledge research funding from The Leona M. and Harry B. Helmsley Charitable Trust. The funder had no role in the design, performance or approval of this Review.
Author information
Authors and Affiliations
Contributions
The authors contributed equally to all aspects of the manuscript.
Corresponding author
Ethics declarations
Competing interests
K.W. has received research grants related to diet and gut health and disease from government agencies, including the Medical Research Council and National Institute of Health Research, charities, including Crohn’s & Colitis UK, The Helmsley Charitable Trust, Kenneth Rainin Foundation, and commercial funders, including Almond Board of California, Danone, and International Nut and Dried Fruit Council. K.W. has received speaker fees from Danone. K.W. is the holder of a joint patent to use volatile organic compounds as biomarkers in irritable bowel syndrome (PCT/GB2020/051604). A.S.B. is funded through a fellowship from The Helmsley Charitable Trust. J.O.L. has received research grants related to diet and gut health and disease from The Helmsley Charitable Trust. B.C. is supported by a starting grant from the European Research Council (ERC) under the European Union’s Horizon 2020 research and innovation programme (ERC-2018-StG-804135), a Chaire d’Excellence from IdEx Université de Paris (ANR-18-IDEX-0001), an Innovator Award from the Kenneth Rainin Foundation, an award from the Fondation de l’Avenir (AP-RM-21-032), ANR grants EMULBIONT (ANR-21-CE15-0042-01) and DREAM (ANR-20-PAMR-0002) and the national programme “Microbiote” from INSERM. B.C. reports honorarium and consulting fees from Nestlé, Procter and Gamble, and Qiagen.
Peer review
Peer review information
Nature Reviews Gastroenterology & Hepatology thanks Andrew Chan, Gerhard Rogler and the other, anonymous, reviewer(s) for their contribution to the peer review of this work.
Additional information
Publisher’s note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Review criteria An online literature search was performed using the Medline database for studies investigating mechanisms (for example, in vitro, animal studies), associations from observational studies (for example, case–control, cohort), and causal or effectiveness outcomes from intervention studies (for example, randomized controlled trials) in relation to ultra-processed food and food additives in gut health and disease. All studies that addressed the aim of this Review were potentially eligible, and strengths and limitations of study design that influence interpretation of the outcome are discussed.
Supplementary information
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Whelan, K., Bancil, A.S., Lindsay, J.O. et al. Ultra-processed foods and food additives in gut health and disease. Nat Rev Gastroenterol Hepatol (2024). https://doi.org/10.1038/s41575-024-00893-5
Accepted:
Published:
DOI: https://doi.org/10.1038/s41575-024-00893-5