Key Points
-
This is a joint statement from UK specialist dental societies highlighting the risks and benefits of elective cosmetic dentistry.
-
Identifies key areas of concern including endodontic and periodontal complications that may ensue.
-
Highlights the 'duty of candour' in relation to elective cosmetic dental interventions.
Abstract
Cosmetic dentistry has become increasingly popular, largely as a result of social trends and increased media coverage. This understandable desire for the alleged 'perfect smile' needs to be tempered with an appropriate awareness of the significant risks associated with invasive cosmetic procedures such as veneers and crowns. Patients need to be properly informed that elective removal of healthy enamel and dentine can result in pulpal injury and poorer periodontal health in the longer term, particularly if they are young. The duty of candour means that they ought to be informed that aggressive reduction of sound tooth tissue is not biologically neutral and results in structural weakening of their teeth. Less invasive procedures such as bleaching on its own or for example, combined with direct resin composite bonding, can satisfy many patient's demands, while still being kinder to teeth and having much better fall-back positions for their future requirements. It is the opinion of the British Endodontic Society, British Society for Restorative Dentistry, Restorative Dentistry UK, Dental Trauma UK, British Society of Prosthodontics and the British Society of Paediatric Dentistry that elective invasive cosmetic dental treatments can result in great benefit to patients, but that some aggressive treatments used to achieve them can produce significant morbidities in teeth which were previously healthy. This is a worrying and growing problem with many ethical, legal and biologic aspects, but many adverse outcomes for patients who request cosmetic dental improvements are preventable by using biologically safer initial approaches to treatment planning and its provision.
Similar content being viewed by others
Introduction
The exact role and importance of dental appearance remains controversial within the dental profession and society at large. The pursuit of facial beauty has intrigued artists, philosophers and dentists for generations. Just as artists argue about their views on art and some architects have strong views on buildings, so it is that many patients and dentists have strongly held opinions on what constitutes dental beauty. Some patients and their dentists prefer the natural dental appearance, while others prefer the 'very white, very even' appearance which has become more popular recently. Ultimately the individual patient should have the final say on what they prefer as their dental appearance, but achieving this is often fraught with various difficulties including interpretive, psychological, ethical, artistic, technical and legal problems. Various articles in the popular and dental press, as well as images in films or on websites have heightened patient expectations by drawing attention to what is possible to achieve with cosmetic dentistry interventions. There is little doubt that cosmetic dentistry, if performed skilfully on the right patients, at the right time, for the right reasons, can be life enhancing for many people.
Cosmetic dentistry has become the popular term both within professional and patient domains and is defined as procedures that are provided primarily to improve the appearance of the teeth, mouth and face. While standard dental treatment often helps to improve the appearance of diseased teeth, what is of serious concern now are unnecessarily destructive procedures which appear to be increasingly provided on largely sound, or mainly intact, teeth in order to conform to a supposedly 'cosmetically desirable' ideal, but which are biologically risky and offer no obvious long term functional benefits (Fig. 1).
Despite poor oral hygiene, having numerous cavities and teeth with unrestorable decay a dentist was only keen on providing her with 'cosmetic' dentistry. Unfortunately, numerous teeth were extracted subsequently and she was provided with a denture. Note the marked gingival inflammation associated with the veneers
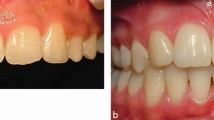
The procedures that are promoted and used vary in the levels of their invasiveness. They range from the minimalistic approach such as straight forward changes in colour, which can be achieved by bleaching techniques, through bleaching and bonding with direct resin composite, to the provision of multiple porcelain veneers or crown restorations (Fig. 2a and 2b).1,2,3,4,5,6,7
The patient was concerned at the discolouration of the teeth and reduced height of the crowns. b) Endodontic treatment was provided for the central and upper right lateral incisors. This was followed by internal-external bleaching and composite restorations at an increased occlusal vertical dimension. Posterior contacts were relinquished within a year of provision. Photographs courtesy of Alex Falanga, Specialist in Endodontics Kings College Hospital
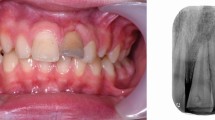
At the extreme end of such approaches are those advocating the elective removal of compromised teeth in order to place implants because it has been suggested that implants are 'more predictable'. This is a view that has become increasingly questioned (Fig. 3).8,9,10,11
The subsequent post and core restorations failed resulting in extraction. Implants were placed with the aid of a block graft from the chin. The graft failed. In a vain effort to harmonise her teeth the upper right and left lateral, canine and first premolars were also crowned or veneered. b) Unfortunately all the teeth with extra-coronal restorations presented with pain soon after cementation. Six previously intact teeth were accessed (arrowed) and root canal treatment provided. The patient sought psychological counselling as a result of her experiences. c) OPT illustrating the numerous previously intact teeth either root canal treated or accessed for future endodontic treatment
Orthodontics is one recognised way of dealing with problems of misplaced and unattractive teeth. The extraction of teeth, or significant tooth stripping for the purposes of space creation for orthodontic alignment is an accepted, different type of destruction, but if the result is unstable, or relapses significantly, then the presumed long term cosmetic benefit may not prove to have justified the elective removal of tooth tissue.12 However, such approaches, if adequately discussed to obtain valid consent and stabilised, may well be preferable to massive destruction of multiple teeth for dealing with crowded or malaligned teeth.13
Terminology
The word cosmetic is derived from the Greek word 'cosmetikos' and strictly speaking means an adornment. In general, cosmetics used around the face are temporary, transient and superficial, such as lipstick or eye shadow. They have to be applied every time one wants that effect. Cosmetic products do not damage the surfaces on which they are placed and are readily reversible. The increase in popularity of supposedly cosmetic dental procedures, many of which are not benign, not reversible and often unnecessarily destructive of sound tooth tissue may, in part, be linked to fashion changes, where ultra-white, very even, big teeth are deemed to be a desirable fashion accessory, or adornment, in some countries and cultures.
Greater media coverage of dental and other oral cosmetic procedures has increased patient pressures on dentists to provide allegedly beautiful smiles.14 Many dentists with appropriate training and experience are able, willing and in some cases anxious, to provide whatever they perceive as being 'what the patient wants' in return for an adequate fee.14 A recent survey of members of the American Academy of Esthetic Dentistry produced notable results. Dentists surveyed perceived overtreatment as being the biggest threat to aesthetic dentistry provision (33%) followed by patients having unrealistic expectations (23%).15 The results from this study demonstrate an awareness within the profession of 'cosmetic dentistry' decisions which are heavily influenced by the media and patient expectations, but without addressing the required balance of conservation of sound tooth tissue for the patients' longer term function. This decision to provide such cosmetic treatment may be criticised further when it is known that dentists prefer much more conservative treatment for their own teeth when compared to that which they provide for their patients.16,17,18,19,20 Indeed when patients were asked on their preferences between direct composite and more destructive indirect veneers for 'cosmetic' improvement there was no difference in perceived improvement between the two modalities.21 Interestingly patients were shown to favour composite due to conservation of tooth structure, cost and the need for one visit for treatment delivery.21
The fact that there are often larger fees involved for the more destructive treatments and/or that the constructive aspects of the treatment are subsequently undertaken by a highly skilled ceramist in a laboratory may be conscious, or unconscious, influencing factors in some dentist's prescribing patterns for their patients. The right combination of trained and talented clinician and technician can indeed produce beautiful end results on appropriate patients. However beneficial the individual patients or their dentist might perceive these changes to be when first done these are likely to deteriorate, or have some problems, in the fullness of time. It is understandable that the publicly funded dental healthcare systems might well seek to minimise their exposure to these potentially great costs for remedial treatment later on for what can be perceived by them to have been unnecessary interventions in the first place (Fig. 4).
The veneer had debonded on a number of occasions and cemented. The patient presented having lost the veneer. b) As provision of a further veneer would have resulted in greater tooth tissue removal as well as reducing the presence of enamel to bond to a direct composite veneer was provided. The result was acceptable to a patient with high aesthetic demands
However, it should be stressed that patients with congenital or acquired defects of the face and oral cavity (such as those problems caused by dental trauma, cancer or cleft lip and palate, hypodontia and developmental anomalies of tooth formation) clearly do require appropriate aesthetic and functional rehabilitation with the aim of improving speech, function, quality of life and aid integration into society and these should obviously continue to be treated in the publicly funded health services (Fig. 2).22,23,24,25,26,27,28
Risks of cosmetic dentistry complications
The longer term risks and comorbidities of the more invasive treatments such as preparations for porcelain veneers and full coverage or all ceramic crowns are biologically significant and can result in later serious problems that patients may not have been be adequately warned of, or have been made fully aware of the viable alternatives, before giving their permission for such treatment. Sadly, the need for root filings through ceramic restorations has become a common problem (Fig. 3b).29,30,31,32,33,34,35,36,37,38,39
In other words, there may well be serious issues of lack of adequately informed and therefore valid consent before unnecessarily destructive procedures are undertaken while the alternative, less damaging, options may not have been properly or fairly presented to the patient, discussed or adequately considered. Later disappointments due to pain, swelling, and infection or dissatisfaction with the appearance, ceramic chipping, loss of restorations or other complications may be sources of complaint or claims especially when the teeth were previously healthy and mainly intact.40 The 2013 figures from the Dental Protection show that consent and communication issues were major problems in both complaints and claims.40 Patients complaining about what they perceived to be unsatisfactory appearance outcomes and the collateral damage inflicted on the teeth to achieve this were also major sources of litigation.40 Other issues involving claims included dentists supplying misleading, or incomplete, information to secure treatment acceptance or of some dentists making exaggerated claims of having extra expertise in the field that could not be substantiated in a court of law.40 For instance, there is no GDC recognised specialist list in 'cosmetic dentistry' or 'aesthetic dentistry' and so seeking to persuade someone that there is such a list, or that one is on it could be construed as 'wilful mis-representation'.
Biological and financial costs
Allegedly 'just cosmetic' dental treatments (such as those required for ceramic veneers and crowns) can result in the removal of significant portions of healthy sound tooth tissue, with up to 30% of tooth tissue being lost extended for extended veneers and 62-73% for full coverage crowns (Fig. 5).41
This is a real concern, especially when the treated teeth are unrestored, or minimally restored, with no history of significant dental disease. Where such teeth are prepared extensively, the previously healthy dentition can enter a restorative cycle where the need for restoration replacement will result in further hard tissue removal. Given that sound enamel and natural tooth tissue is finite, this often unnecessary structural and biological destruction can lead to pulpal or periodontal problems and sometimes premature tooth loss.
Pulpal problems
Tooth preparation for ceramic restorations can result in irreversible pulpal damage due to the heat and physical damage produced during deep preparation of teeth previously unaffected by caries.42 Caries is a slow process which normally gives teeth time to lay down reparative protective dentine but intact teeth which are quickly and aggressively prepared get no such chance to protect themselves, especially in the pulpal horns or cervical regions. The damage involved in newly prepared teeth may well be further compromised during the temporisation stage of treatment and where this is inadequate it can allow microleakage with bacterial ingress progressing down the freshly opened dentinal tubules leading straight to the pulp. The toxicity of the temporisation material used can also provide pulpal insult (Fig. 6).43
The patient wanted lighter coloured teeth. The upper and lower teeth were all prepared for veneers. When these were deemed unacceptable by the patient increasingly more aggressive crown preparations were undertaken. The patient sued the original dentist as he had caused her significant pain and after three attempts had failed to satisfy her 'cosmetic' demands. These temporary linked crowns were over contoured and engaging interproximal undercuts for retention. Gingival bleeding and inflammation were detected as the restorations were uncleansable. The patient refused to return to the original dentist as he had 'overpromised and under-delivered'
If loss of vitality results from the preparations, or from subsequent problems of microleakage the patient may experience a variety of co-morbidities. Acute pulpitis is likely to be painful requiring pulp extirpation and subsequent root canal treatment. Root canal treatment weakens the residual tooth tissue resulting in greater chance of future tooth fracture (Fig. 7).44,45 In some cases the pulpal 'blushing' or loss of vitality can result in tooth discolouration due to blood breakdown products being incorporated into the dentine.46 Where pulp vitality is maintained, symptoms such as chronic sensitivity can develop post restoration.47,48 This is often due to poor adhesive technique and the poor sealing of the restorative luting system. The loss of vitality and other collateral damage have been significant sources of complaints by patients after the provision of veneers, especially when the endodontic treatment subsequently undertaken is deemed to be suboptimal in a dento-legal expert's opinion.40 In this regard the standard of endodontic therapy in general dental practice gives further grounds for concern.49,50,51,52 Adverse outcomes are often difficult to defend mainly because the teeth would not have needed the endodontic therapy had they not had the destructive cosmetic dentistry procedures undertaken in the first place.
Composite versus amalgam in posterior teeth for cosmetic reasons
Elective restoration replacement of dental amalgam with 'white fillings' of various direct or indirect types can also result in significant pulpal symptoms (Fig. 8). Pulpal problems have been shown to be more likely the use of composite as opposed to amalgam particularly in deep cavities.53 Pulpal inflammation has been shown to be more pronounced with the use of resin composite than with alternative restorative material choices.54 This is probably associated with gingival or salivary contamination of the adhesive or luting systems, or due to c-factor shrinkage in larger molar restorations, thereby increasing the likelihood of bacterial ingress deep down cervically close to the pulp.55 The imminent 'phase down' of dental amalgam, a material which has been proven to be more tolerant of suboptimal placement conditions than composite under similar circumstances has potentially serious pulpal and tooth retention implications for patients which ought not to be ignored.56,57,58,59
Cosmetic dentistry and periodontal problems
The interface between veneers and crowns and the gingival margin can result in the development of inflammation which can result in periodontal defects (Figs 9 and 10).60,61,62,63 Over contoured restorations, residual cement and positive margins can result in plaque accumulation and thereby result in gingivitis, gingival recession or periodontitis, all of which can result in significant morbidity.60,61,62,63 Encroachment by the restoration into the biological width can result in chronic inflammation of the gingival margin.60,61,62,63
Longer term biological and financial repercussions
Any dental restoration, including veneers and crowns, will require replacement in the future. Where teeth have been prepared extensively, especially when they have to be subsequently root canal treated, this may result in the restoration replacement becoming progressively more difficult to achieve satisfactorily due to a lack of remaining sound tooth tissue (Fig. 11).
These possible biological risks and complications need to be considered against a backdrop of significant financial outlay and time by the patient for the initial, usually private, treatment provision. Remedial work to correct any problems resulting from cosmetic dental treatment is also likely to result in further financial burdens in the longer term. This burden may fall upon the patient, the treating dentist, future dentists in that practice, other general dental practices, or on to secondary care specialist services to provide remedial treatment, or advice on its planning if this is not within their remit. One thing seems certain, however, that is that there will be further costs incurred by someone, sometime, and both patients and dentists need to be well aware of those likely issues and their future implications as part of the properly informed processes.
In the future, attitudes may well have hardened against some currently fashionable cosmetic treatments, which are often voluntary and unnecessarily destructive. Subsequently some dentists faced with the potential costs of consequent treatment could well encourage patients to pursue litigation to obtain funds for their remedial treatment. This is partly because the state system is unlikely to be particularly sympathetic about these issues, or be willing to prioritise funding for renewal or repair for what it might contend were elective aggressive cosmetic procedures.
The Francis report: consent and communication
These issues may have serious implications for dentistry when considering the Francis report relating to the duty of candour.64 This report states that all relevant information needs to be volunteered to persons who have, or may have been harmed, by the provision of services, whether or not the information has been requested and whether or not a complaint or a report about that provision has been made.64
Conclusions
It is the opinion of the British Endodontic Society, British Society for Restorative Dentistry, Restorative Dentistry UK, Dental Trauma UK, British Society of Prosthodontics and the British Society of Paediatric Dentistry that elective invasive cosmetic dental treatments can result in great benefit to patients but that these can also produce significant morbidities in teeth which were previously considered healthy. This is a worrying and growing problem that is preventable by using a biologically safer initial approach to treatment planning and it's provision wherever possible. Minimally invasive approaches, which are associated with lower risks and good fall-back positions, should be advocated and practised wherever possible as the first choice of treatment for patient seeking improvements in their dental appearance. In contrast, where teeth have large restorations the provision of an extra-coronal restoration is an accepted treatment option in order to protect the remaining tooth tissue. However the full range of dental materials – including sandblasted gold or other metals – as well as ceramic of various types should be considered carefully, especially in low visibility situations.
Patients seeking cosmetic dental improvement should be made fully aware of the associated risks, possible complications, the lack of permanence of restorations and their longer-term biological and financial costs. As is the case with other dental treatments neutral, sensible, considered language and information needs to be given to patients in advance and preferably in writing in order to obtain their properly informed consent for elective cosmetic invasive procedures. This should be the agreed basis for the acceptance of cosmetic dental treatment by these potentially demanding, but vulnerable, patients.
References
Rosenstiel S F, Gegauff A G, Johnston W M . Randomised clinical trial of the efficacy and safety of a home bleaching procedure. Quintessence Int 1996; 27: 413–424.
Matis B A, Cochran M A, Eckert G . Review of the effectiveness of various tooth whitening systems. Oper Dent 2009; 34: 230–235.
Curtis J W, Dickinson G L, Downey M C et al. Assessing the effects of 10 percent carbamide peroxide on oral soft tissues. J Am Dent Assoc 1996; 127: 1218–1223.
Kelleher M G, Djemal S, Al-Khayatt A S, Ray-Chaudhuri J, Briggs P F, Porter R W . Bleaching and bonding for the older patient. Dent Update 2011; 38: 294–296, 298–300, 302–303.
Burke F J, Lucarotti P S . Ten-year outcome of porcelain laminate veneers placed within the general dental services in England and Wales. J Dent 2009; 37: 31–38.
Burke F J, Lucarotti P S . Ten-year outcome of crowns placed within the General Dental Services in England and Wales. J Dent 2009; 37: 12–24.
Walton T R . The up to 25-year survival and clinical performance of 2,340 high gold-based metal-ceramic single crowns. Int J Prosthodont 2013; 26: 151–160.
Lindhe J . 'There is an overuse of implants in the world and an underuse of teeth as targets for treatment. Br Dent J 2014 217: 396–397.
Gillot L, Cannas B, Buti J, Noharet R . A retrospective cohort study of 113 patients rehabilitated with immediately loaded maxillary cross-arch fixed dental prostheses in combination with immediate implant placement. Eur J Oral Implantol 2012; 5: 71–79.
Covani U, Chiappe G, Bosco M, Orlando B, Quaranta A, Barone A . A 10-year evaluation of implants placed in fresh extraction sockets: a prospective cohort study. J Periodontol 2012; 83: 1226–1234.
Barbier L, Abeloos J, De Clercq C, Jacobs R . Peri-implant bone changes following tooth extraction, immediate placement and loading of implants in the edentulous maxilla. Clin Oral Investig 2012; 16: 1061–1070.
Chate R A . Truth or consequences: the potential implications of short-term cosmetic orthodontics for general dental practitioners. Br Dent J 2013; 215: 551–553.
Alani A, Kelleher M G . Technique tips - the use of extra-coronal restorations in the correction of mal-aligned teeth. Dent Update 2014; 41: 88–89.
Theobald A H, Wong B K, Quick A N, Thomson W M . The impact of the popular media on cosmetic dentistry. N Z Dent J 2006; 102: 58–63.
Goldstein R E . Attitudes and problems faced by both patients and dentists in esthetic dentistry today: an AAED membership survey. J Esthet Restor Dent 2007; 19: 164–170.
Rosenstiel S F, Land M F, Rashid R G . Dentists' molar restoration choices and longevity: a web-based survey. J Prosthet Dent 2004; 91: 363–367.
Espelid I, Cairns J, Askildsen J E, Qvist V, Gaarden T, Tveit A B . Preferences over dental restorative materials among young patients and dental professionals. Eur J Oral Sci 2006; 114: 15–21.
Christensen G J . The use of porcelain fused to-metal restorations in current dental practice: a survey. J Prosthet Dent 1986; 56: 1–3.
Jørnung J, Fardal Ø . Perceptions of patients' smiles: a comparison of patients' and dentists' opinions. J Am Dent Assoc 2007; 138: 1544–53; quiz 1613–1614.
Alani A, Bishop K, Djemal S . Decision-making in the provision of extra-coronal restorations. Dent Update 2013; 40: 378–380, 383–384.
Nalbandian S, Millar B J . The effect of veneers on cosmetic improvement. Br Dent J 2009; 207: E3.
Antunes L S, Maués C P, Nadaes M R, Costa M C, Küchler E C, Antunes L A . The impact of nonsyndromic oral clefts on family quality of life. Spec Care Dentist 2014; 34: 138–143.
Gkantidis N, Papamanou D A, Christou P, Topouzelis N . Aesthetic outcome of cleft lip and palate treatment. Perceptions of patients, families, and health professionals compared to the general public. J Craniomaxillofac Surg 2013; 41: e105–110.
Pace-Balzan A, Shaw R J, Butterworth C . Oral rehabilitation following treatment for oral cancer. Periodontol 2000 2011; 57: 102–117.
Pace-Balzan A, Butterworth C J, Dawson L J, Lowe D, Rogers S N . The further development and validation of the Liverpool Oral Rehabilitation Questionnaire (LORQ) version 3: a cross-sectional survey of patients referred to a dental hospital for removable prostheses replacement. J Prosthet Dent 2008; 99: 233–242.
Bendo C B, Paiva S M, Varni J W, Vale M P . Oral health-related quality of life and traumatic dental injuries in Brazilian adolescents. Community Dent Oral Epidemiol 2014; 42: 216–223.
Ramos-Jorge J, Paiva S M, Tataounoff J, Pordeus I A, Marques L S, Ramos-Jorge M L . Impact of treated/untreated traumatic dental injuries on quality of life among Brazilian schoolchildren. Dent Traumatol 2014; 30: 27–31.
Antunes L S, Debossan P F, Bohrer L S, Abreu F V, Quintanilha L E, Antunes L A . Impact of traumatic dental injury on the qualityoflife of children and adolescents: a case-control study. Acta Odontol Scand 2013; 71: 1123–1128.
Felton D, Madison S, Kanoy E et al. Long-term effects of crown preparations on pulp vitality. J Dent Res 1989; 68: 1009.
Saunders W P, Saunders E M . Prevalence of periradicular periodontitis associated with crowned teeth in an adult Scottish subpopulation. Br Dent J 1998; 185: 137–140.
Cheung G S, Lai S C, Ng R P . Fate of vital pulps beneath a metal-ceramic crown or a bridge retainer. Int Endod J 2005; 38: 521–530.
Abou-Rass M . The stressed pulp condition: an endodontic-restorative diagnostic concept. J Prosthet Dent 1982; 48: 264–267.
Encke B S, Heydecke G, Wolkewitz M, Strub J R . Results of a prospective randomized controlled trial of posterior ZrSiO(4)-ceramic crowns. J Oral Rehabil 2009; 36: 226–235.
Murray P E, Smith A J, Windsor L J, Mjör I A . Remaining dentine thickness and human pulp responses. Int Endod J 2003; 36: 33–43.
Wisithphrom K, Murray P E, About I, Windsor L J . Interactions between cavity preparation and restoration events and their effects on pulp vitality. Int J Periodontics Restorative Dent 2006; 26: 596–605.
Felton D A, Kanoy B E, Bayne S C, Wirthman G P . Effect of in vivo crown margin discrepancies on periodontal health. J Prosthet Dent 1991; 65: 357–364.
Larato D C . The effect of crown margin extension on gingival inflammation. J South Calif Dent Assoc 1969; 37: 476–478.
Richter W A, Ueno H . Relationship of crown margin placement to gingival inflammation. J Prosthet Dent 1973; 30: 156–161.
Koth D L . Full crown restorations and gingival inflammation in a controlled population. J Prosthet Dent 1982; 48: 681–685.
Kevin Lewis, Dental Protection. Personal communication.
Edelhoff D, Sorensen J A . Tooth structure removal associated with various preparation designs for anterior teeth. J Prosthet Dent 2002; 87: 503–509.
Baldissara P, Catapano S, Scotti R . Clinical and histological evaluation of thermal injury thresholds in human teeth: a preliminary study. J Oral Rehabil 1997; 24: 791–801.
Fleisch L, Cleaton-Jones P, Forbes M, van Wyk J, Fat C . Pulpal response to a bisacrylplastic (Protemp) temporary crown and bridge material. J Oral Pathol 1984; 13: 622–631.
Sobhani O E, Gulabivala K, Knowles J C, Ng Y L . The effect of irrigation time, root morphology and dentine thickness on tooth surface strain when using 5% sodium hypochlorite and 17% EDTA. Int Endod J 2010; 43: 190–199.
Rajasingham R, Ng Y L, Knowles J C, Gulabivala K . The effect of sodium hypochlorite and ethylenediaminetetraacetic acid irrigation, individually and in alternation, on tooth surface strain. Int Endod J 2010; 43: 31–40.
Ahmed H M, Abbott P V . Discolouration potential of endodontic procedures and materials: a review. Int Endod J 2012; 45: 883–897.
Chen J H, Shi C X, Wang M, Zhao S J, Wang H . Clinical evaluation of 546 tetracycline-stained teeth treated with porcelain laminate veneers. J Dent 2005; 33: 3–8.
Aykor A, Ozel E . Five-year clinical evaluation of 300 teeth restored with porcelain laminate veneers using total-etch and a modified self-etch adhesive system. Oper Dent 2009; 34: 516–523.
Palmer N O, Ahmed M, Grieveson B . An investigation of current endodontic practice and training needs in primary care in the north west of England. Br Dent J 2009 13; 206: E22; discussion 584–585.
Stewardson DA . Endodontic standards in general dental practice; a survey in Birmingham, part I. Eur J Prosthodont Restor Dent 2001; 9: 107–112.
Whitworth J M, Seccombe G V, Shoker K, Steele J G . Use of rubber dam and irrigant selection in UK general dental practice. Int Endod J 2000; 33: 435–441.
Jenkins S M, Hayes S J, Dummer P M . A study of endodontic treatment carried out in dental practice within the UK. Int Endod J 2001; 34: 16–22.
Whitworth J M, Myers P M, Smith J, Walls A W, McCabe J F . Endodontic complications after plastic restorations in general practice. Int Endod J 2005; 38: 409–416.
Chandwani N D, Pawar M G, Tupkari J V, Yuwanati M . Histological evaluation to study the effects of dental amalgam and composite restoration on human dental pulp: an in vivo study. Med Princ Pract 2014; 23: 40–44.
Shimazu K, Karibe H, Ogata K . Effect of artificial saliva contamination on adhesion of dental restorative materials. Dent Mater J 2014; 33: 545–550.
Bergenholtz G . Evidence for bacterial causation of adverse pulpal responses in resin-based dental restorations. Crit Rev Oral Biol Med 2000; 11: 467–480.
Kouros P, Koliniotou-Koumpia E, Koulaouzidou E, Helvatjoglu-Antoniades M, Tziafas D . Pulp response to dentine adhesives: a study on mature human pulps. Eur J Dent 2013; 7: S26–32.
FDI World Dental Federation. FDI policy statement on dental amalgam and the Minamata Convention on Mercury: adopted by the FDI General Assembly: 13 September 2014, New Delhi, India. Int Dent J 2014; 64: 295–296.
Alexander G, Hopcraft M S, Tyas M J, Wong R H . Dentists' restorative decision-making and implications for an 'amalgamless' profession. Part 1: a review. Aust Dent J 2014; 59: 408–419.
Felton D A, Kanoy B E, Bayne S C, Wirthman G P . Effect of in vivo crown margin discrepancies on periodontal health. J Prosthet Dent 1991; 65: 357–364.
Larato D C . The effect of crown margin extension on gingival inflammation. J South Calif Dent Assoc 1969; 37: 476–478.
Richter W A, Ueno H . Relationship of crown margin placement to gingival inflammation. J Prosthet Dent 1973; 30: 156–161.
Koth D L . Full crown restorations and gingival inflammation in a controlled population. J Prosthet Dent 1982; 48: 681–685.
Walsh P . The future for Medico-Legal disputes a patient perspective. Med Leg J 2014; 82: 18–28.
Author information
Authors and Affiliations
Corresponding author
Additional information
Refereed Paper
Rights and permissions
About this article
Cite this article
Alani, A., Kelleher, M., Hemmings, K. et al. Balancing the risks and benefits associated with cosmetic dentistry – a joint statement by UK specialist dental societies. Br Dent J 218, 543–548 (2015). https://doi.org/10.1038/sj.bdj.2015.345
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bdj.2015.345