Abstract
Background:
Epidemiologic and laboratory evidence supports a role for cholesterol in prostate cancer (PC). Dietary saturated fat content impacts serum cholesterol levels. However, epidemiologic associations between saturated fat and PC aggressiveness are inconsistent. We hypothesized that high saturated fat intake would be associated with increased PC aggressiveness, and that statin use would modify this association.
Methods:
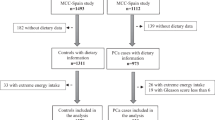
Of 1854 PC cases in the North Carolina-Louisiana PC Project, 321 (17%) were classified as high aggressive (Gleason sum ⩾8, PSA>20 ng ml−1, or Gleason sum ⩾7 and clinical stage T3-4) or low/intermediate aggressive (all other cases). Using low/intermediate aggressive cases as the referent group, we examined the association between tertiles of total fat-adjusted saturated fat intake and high aggressive PC using logistic regression, overall and stratified by race and statin use. We examined total fat-adjusted polyunsaturated and monounsaturated fatty acids (PUFA and MUFA, respectively), trans fat and cholesterol intake in secondary analysis.
Results:
High total fat-adjusted saturated fat intake was associated with an elevated odds ratio (OR) for aggressive PC (ORT3vsT1 1.51; 95% CI 1.10–2.06; P-trend=0.009), with an attenuated association in statin users (ORT3vsT1 1.16; 95% CI 0.67–2.01; P-trend=0.661) compared with non-users (ORT3vsT1 1.71; 95% CI 1.16–2.51; P-trend=0.053). High total fat-adjusted cholesterol intake was associated with aggressive PC in European Americans (ORT3vsT1 1.62; 95% CI 1.02–2.58; P-trend=0.056), but not African Americans (ORT3vsT1 0.92; 95% CI 0.60–1.42; P-trend=0.750). High total fat-adjusted PUFA was inversely associated with PC aggressiveness (ORT3vsT1 0.75; 95% CI 0.55–1.03), although this was not significant. No associations were found between total fat-adjusted MUFA or trans fat and PC aggressiveness.
Conclusions:
High total fat-adjusted saturated fat intake was associated with increased PC aggressiveness, with a suggestion of a stronger effect in men not using statins. The association between total fat-adjusted cholesterol intake and PC aggressiveness was most pronounced in European Americans.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Center MM, Jemal A, Lortet-Tieulent J, Ward E, Ferlay J, Brawley O et al. International variation in prostate cancer incidence and mortality rates. Eur Urol 2012; 61: 1079–1092.
Micha R, Khatibzadeh S, Shi P, Fahimi S, Lim S, Andrews KG et al. Global, regional, and national consumption levels of dietary fats and oils in 1990 and 2010: a systematic analysis including 266 country-specific nutrition surveys. BMJ 2014; 348: g2272.
Kobayashi N, Barnard RJ, Said J, Hong-Gonzalez J, Corman DM, Ku M et al. Effect of low-fat diet on development of prostate cancer and Akt phosphorylation in the Hi-Myc transgenic mouse model. Cancer Res 2008; 68: 3066–3073.
Allott EH, Hursting SD . Obesity and cancer: mechanistic insights from transdisciplinary studies. Endocr Relat Cancer 2015; 22: R365–R386.
Park SY, Murphy SP, Wilkens LR, Henderson BE, Kolonel LN . Fat and meat intake and prostate cancer risk: the multiethnic cohort study. Int J Cancer 2007; 121: 1339–1345.
Kristal AR, Arnold KB, Neuhouser ML, Goodman P, Platz EA, Albanes D et al. Diet, supplement use, and prostate cancer risk: results from the prostate cancer prevention trial. Am J Epidemiol 2010; 172: 566–577.
Xu C, Han FF, Zeng XT, Liu TZ, Li S, Gao ZY . Fat intake is not linked to prostate cancer: a systematic review and dose-response meta-analysis. PLoS One 2015; 10: e0131747.
Pelser C, Mondul AM, Hollenbeck AR, Park Y . Dietary fat, fatty acids, and risk of prostate cancer in the NIH-AARP diet and health study. Cancer Epidemiol Biomarkers Prev 2013; 22: 697–707.
Giovannucci E, Rimm EB, Colditz GA, Stampfer MJ, Ascherio A, Chute CG et al. A prospective study of dietary fat and risk of prostate cancer. J Natl Cancer Inst 1993; 85: 1571–1579.
Epstein MM, Kasperzyk JL, Mucci LA, Giovannucci E, Price A, Wolk A et al. Dietary fatty acid intake and prostate cancer survival in Orebro County, Sweden. Am J Epidemiol 2012; 176: 240–252.
Van Blarigan EL, Kenfield SA, Yang M, Sesso HD, Ma J, Stampfer MJ et al. Fat intake after prostate cancer diagnosis and mortality in the Physicians' Health Study. Cancer Causes Control 2015; 26: 1117–1126.
Grundy SM, Vega GL . Causes of high blood cholesterol. Circulation 1990; 81: 412–427.
Allott EH, Howard LE, Cooperberg MR, Kane CJ, Aronson WJ, Terris MK et al. Postoperative statin use and risk of biochemical recurrence following radical prostatectomy: results from the Shared Equal Access Regional Cancer Hospital (SEARCH) database. BJU Int 2014; 114: 661–666.
Allott EH, Howard LE, Cooperberg MR, Kane CJ, Aronson WJ, Terris MK et al. Serum lipid profile and risk of prostate cancer recurrence: results from the SEARCH Database. Cancer Epidemiol Biomarkers Prev 2014; 23: 2349–2356.
Allott EH, Farnan L, Steck SE, Arab L, Su, Mishel M et al. Statin use and prostate cancer aggressiveness: results from the population-based North Carolina-Louisiana Prostate Cancer Project. Cancer Epidemiol Biomarkers Prev 2016.
Schroeder JC, Bensen JT, Su LJ, Mishel M, Ivanova A, Smith GJ et al. The North Carolina-Louisiana Prostate Cancer Project (PCaP): methods and design of a multidisciplinary population-based cohort study of racial differences in prostate cancer outcomes. Prostate 2006; 66: 1162–1176.
Subar AF, Thompson FE, Kipnis V, Midthune D, Hurwitz P, McNutt S et al. Comparative validation of the Block, Willett, and National Cancer Institute food frequency questionnaires: the Eating at America's Table Study. Am J Epidemiol 2001; 154: 1089–1099.
Thompson FE, Subar AF, Brown CC, Smith AF, Sharbaugh CO, Jobe JB et al. Cognitive research enhances accuracy of food frequency questionnaire reports: results of an experimental validation study. J Am Diet Assoc 2002; 102: 212–225.
Willett W, Stampfer MJ . Total energy intake: implications for epidemiologic analyses. Am J Epidemiol 1986; 124: 17–27.
Whittemore AS, Kolonel LN, Wu AH, John EM, Gallagher RP, Howe GR et al. Prostate cancer in relation to diet, physical activity, and body size in blacks, whites, and Asians in the United States and Canada. J Natl Cancer Inst 1995; 87: 652–661.
Hayes RB, Ziegler RG, Gridley G, Swanson C, Greenberg RS, Swanson GM et al. Dietary factors and risks for prostate cancer among blacks and whites in the United States. Cancer Epidemiol Biomarkers Prev 1999; 8: 25–34.
Rodriguez C, McCullough ML, Mondul AM, Jacobs EJ, Chao A, Patel AV et al. Meat consumption among Black and White men and risk of prostate cancer in the Cancer Prevention Study II Nutrition Cohort. Cancer Epidemiol Biomarkers Prev 2006; 15: 211–216.
Gromadzka-Ostrowska J . Effects of dietary fat on androgen secretion and metabolism. Reprod Biol 2006; 6 (Suppl 2): 13–20.
Shankar E, Bhaskaran N, MacLennan GT, Liu G, Daneshgari F, Gupta S . Inflammatory signaling involved in high-fat diet induced prostate diseases. J Urol Res 2015; 2; pii: 1018.
Di Sebastiano KM, Mourtzakis M . The role of dietary fat throughout the prostate cancer trajectory. Nutrients 2014; 6: 6095–6109.
Mensink RP, Zock PL, Kester AD, Katan MB . Effects of dietary fatty acids and carbohydrates on the ratio of serum total to HDL cholesterol and on serum lipids and apolipoproteins: a meta-analysis of 60 controlled trials. Am J Clin Nutr 2003; 77: 1146–1155.
Platz EA, Till C, Goodman PJ, Parnes HL, Figg WD, Albanes D et al. Men with low serum cholesterol have a lower risk of high-grade prostate cancer in the placebo arm of the prostate cancer prevention trial. Cancer Epidemiol Biomarkers Prev 2009; 18: 2807–2813.
Platz EA, Leitzmann MF, Visvanathan K, Rimm EB, Stampfer MJ, Willett WC et al. Statin drugs and risk of advanced prostate cancer. J Natl Cancer Inst 2006; 98: 1819–1825.
Agalliu I, Kirsh VA, Kreiger N, Soskolne CL, Rohan TE . Oxidative balance score and risk of prostate cancer: results from a case-cohort study. Cancer Epidemiol 2011; 35: 353–361.
Lovegrove C, Ahmed K, Challacombe B, Khan MS, Popert R, Dasgupta P . Systematic review of prostate cancer risk and association with consumption of fish and fish-oils: analysis of 495,321 participants. Int J Clin Pract 2015; 69: 87–105.
Ahn J, Lim U, Weinstein SJ, Schatzkin A, Hayes RB, Virtamo J et al. Prediagnostic total and high-density lipoprotein cholesterol and risk of cancer. Cancer Epidemiol Biomarkers Prev 2009; 18: 2814–2821.
Acknowledgements
We thank the staff, advisory committees and research subjects participating in the PCaP study for their important contributions. This work was supported by the American Institute for Cancer Research (to EHA). The North Carolina-Louisiana Prostate Cancer Project (PCaP) was funded by the Department of Defense contract DAMD 17-03-2-0052.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
Supplementary Information accompanies the paper on the Prostate Cancer and Prostatic Diseases website
Supplementary information
Rights and permissions
About this article
Cite this article
Allott, E., Arab, L., Su, L. et al. Saturated fat intake and prostate cancer aggressiveness: results from the population-based North Carolina-Louisiana Prostate Cancer Project. Prostate Cancer Prostatic Dis 20, 48–54 (2017). https://doi.org/10.1038/pcan.2016.39
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/pcan.2016.39
This article is cited by
-
Obesity and prostate cancer — microenvironmental roles of adipose tissue
Nature Reviews Urology (2023)
-
The lipidomic profile of the tumoral periprostatic adipose tissue reveals alterations in tumor cell’s metabolic crosstalk
BMC Medicine (2022)
-
The Problem of Underrepresentation: Black Participants in Lifestyle Trials Among Patients with Prostate Cancer
Journal of Racial and Ethnic Health Disparities (2020)
-
Stylosin and some of its synthetic derivatives induce apoptosis in prostate cancer cells as 15-lipoxygenase enzyme inhibitors
Naunyn-Schmiedeberg's Archives of Pharmacology (2019)
-
Optimisation of cooking properties of healthier beef patties and quality evaluation during frozen storage
Journal of Food Measurement and Characterization (2019)