Abstract
Activation of focal adhesion kinase (FAK), overexpressed in several human cancers, induces survival, proliferation and motility of cells in culture, but its functional importance in human tumor growth in vivo has not been elucidated. I explored the role of FAK in regulating tumorigenicity of human carcinoma cells, HEp3. These cells overexpress urokinase receptor (uPAR) which, by activating α5β1 integrin, initiates an intracellular signal through FAK and Src leading to ERK activation and tumorigenicity in vivo. Down regulation of uPAR in these cells led to a ∼3–5-fold reduction in FAK phosphorylation and association with Src and dormancy in vivo. Both FAK phosphorylation and ability to grow in vivo were restored by re-expression of uPAR. The FAK signaling pathway in T-HEp3 cells, measured by FAK phosphorylation, GTP-loaded Ras and ERK activation, was inhibited by transient or stable transfection of FAK related non-kinase (FRNK), known to have a dominant negative function, but not by a FRNK mutant version (S1034-FRNK). Most importantly, while vector- and mutant-S1034-FRNK transfected cells inoculated onto chicken embryo CAMs formed progressively growing tumors, the HA-FRNK-expressing T-HEp3 cells did not proliferate in vivo and remained dormant for at least 6 weeks. Both cell types had similar rate of apoptosis in vivo and the p38SAPK or PI3K-Akt signaling pathways were unaffected by FRNK. FRNK induced dormancy could be reverted by expression of an active-R4F-Mek1 mutant. These results show that active FAK is an important mediator of uPAR-regulated tumorigenicity of HEp3 cells and that interruption of FAK mitogenic signaling either through down-regulation of uPAR or by expression of FRNK can force human carcinoma cells into dormancy.
Similar content being viewed by others
Introduction
It has been widely proposed that tumor cells expressing activated oncogenes or enhanced growth factor signaling, can bypass the need for anchorage-derived signals in order to survive and proliferate (Ruoslahti, 1999). However, growing evidence indicates that loss of cell–cell interactions (E-cadherin-based) (Genda et al., 2000) and gain of cell–matrix interactions (integrin-based) (Trusolino et al., 2000) by epithelial tumor cells may be a source of survival and mitogenic signals important for successful growth and dissemination.
In normal fibroblast and endothelial cells integrins initiate mitogenic signaling through α- and/or β-integrin subunit-associated signaling molecules (Giancotti and Ruoslahti, 1999). Important among them is the focal adhesion kinase (FAK), a 125-kD non-receptor tyrosine kinase, a transducer of integrin-derived signals for motility, survival and proliferation (Cary and Guan, 1999). FAK association with the integrin β-subunits can, in the presence of fibronectin (FN), generate a sufficiently high level of active ERKMAPK activation to initiate proliferation in culture (Zhao et al., 1998). In addition, FAK signaling can activate the PI3K-Akt/PKB or Cas/Crk pathways, which are important for growth factor and matrix-dependent induction of cell survival and migration in vitro (Cary and Guan, 1999; Gu et al., 1998). Much of the available information on the participation of ECM-integrin-FAK signaling in induction of proliferation is derived from tissue culture studies. Only very recently the role of these signaling pathways in tumor growth in vivo has come under scrutiny (Aguirre Ghiso et al., 1999; Schiller and Bittner, 1995; Weaver et al., 1997; Wang et al., 1998). But, in spite the fact that FAK was shown to be overexpressed in several types of human primary and metastatic tumor samples of epithelial and non-epithelial origin (Kornberg, 1998), and to promote survival of cancer cells in culture (Xu et al., 1996, 1998) its functional role in tumors in vivo has not been elucidated.
We have shown recently that tumorigenicity of HEp3 human carcinoma cells is dependent on uPAR-α5β1-integrin association, which regulates FN-matrix assembly and constitutively activates Mek-ERKMAPK (mitogenic) pathway and suppresses p38SAPK (growth suppressive) pathways (Aguirre Ghiso et al., 1999, 2001). Downregulation of uPAR forces HEp3 cells into dormancy by reversing the state of activation of these two pathways. Because both uPAR and α5β1 integrin are strong activators of FAK signaling (Giancotti and Ruoslahti, 1999; Nguyen et al., 2000), I reasoned that this model of cancer growth and dormancy may be amenable to testing of the role of FAK activation in tumorigenicity. Regulation of FAK activity by a genetic approach provided evidence that activation of FAK signaling is essential for uPAR-α5β1-induced tumorigenicity while its inhibition induces cancer dormancy in vivo.
Results
FAK phosphorylation and FAK-Src association induced by uPAR is β1-integrin dependent
As we have recently shown (Aguirre Ghiso et al., 1999, 2001), association of uPAR with α5β1 integrin in tumorigenic HEp3 cells, leads to activation of the integrin and generation of a signaling cascade resulting in activation of ERK and proliferation in vivo. Confirming previous results (Aguirre Ghiso et al., 1999, 2001), T-HEp3 cells with high uPAR levels were able to develop progressively growing tumors upon inoculation in vivo, while D-HEp3 cells with fourfold less uPAR protein and ERK activation (Aguirre Ghiso et al., 1999) formed only small nodules that did not increase in size over passage (Figure 1a). That more full-length uPAR associated with α5β1 integrins in uPAR-overexpressing T-HEp3 than in low uPAR D-HEp3 cells was confirmed by co-IP experiments (Figure 1b). I next tested whether FAK was expressed in HEp3 cells and whether it was activated by the uPAR-α5β1 complex that activates ERK (Aguirre Ghiso et al., 1999). The basal level of FAK protein, as detected by Western blotting of whole cell lysates, was similar in T-HEp3 and D-HEp3 cells (Figure 1c). This level remained unchanged even if the cells were plated on fibronectin (FN) (Figure 1d). In contrast, the level of phosphorylated FAK was ∼3–4-fold greater in T-HEp3 than in D-HEp3 cells growing in monolayers (Figure 1d) and it was further increased upon adhesion to FN. Similarly, the level of phosphorylated FAK was much greater in LK25 clone of T-HEp3 cells transfected with an ‘empty’ vector than in AS24 clone transfected with an uPAR antisense expressing vector with low uPAR level (Figure 1e,f). This difference was maintained in cells grown on plastic or cells adherent to FN, supporting the notion that FN-integrin mediated FAK phosphorylation was dependent on uPAR (Figure 1e,f).
FAK is activated by uPAR in HEp3 cells. (a) Growth of HEp3 cells on CAMs. T-Hep3 (high uPAR, empty squares) or D-Hep3 (low-uPAR, empty diamonds) cells were inoculated on 9 day old CAMs (5×105 cells/CAM) and at the indicated times live tumor cells were counted (see Materials and methods). Mean and SD (n=4) of the number of cells per tumor are shown. (b) Co-IP of uPAR and α5β1 integrins. Cell lysates (400 μg) from T-HEp3 or D-HEp3 cells were subjected to IP with anti-α5β1 integrin. The IP was tested for β1 and uPAR content (uPAR levels as determined by densitometry are T-HEp3: 0.5 and D-HEp3 0.1 expressed in O.D. arbitrary units). The numbers under the blots show the ratio of uPAR/β1 relative OD levels. (c) The same cell lysates (50 μg/lane) used in (b) were used to detect FAK expression with an anti-FAK mAb by Western blot. (d) FAK phosphorylation as detected by IP (IP : FAK) and Western blot (WB : PY, WB : FAK). Cell lysates (600 μg) from T-HEp3 and D-HEp3 cells grown in monolayers or plated on 4 μg/ml poly-L-lysine (PL) or fibronectin for 20 min were subjected to IP with anti-FAK 2A7 mAb. The IPs were blotted first with anti-phospho-Y using RC20-HRP conjugated Ab (upper panel), stripped and blotted with anti-FAK (lower panel). IP: IgG, negative control IP where T-HEp3 cell lysates were subjected to a parallel IP using an irrelevant isotype matched IgG. The graph shows the OD ratio for PY-FAK/FAK bands as quantitated by laser scanning densitometry. Note the strong difference in FAK-phosphorylation between T-HEp3 and D-HEp3 cells. (e) FAK and phospho-tyrosine levels in vector and uPAR-antisense expressing HEp3 cells plated on FN. Cell lysates from LK25 vector transfected cells or AS24 cells transfected with an antisense to uPAR, starved for 24 h and plated on FN were used to detect phospho-Y proteins at ∼97–220 kDa MW (upper panel) and FAK expression (lower panel) by Western blot. The arrows indicate ∼120–125 kDa phospho-P protein and FAK protein which co-migrates with the P-Y band. (f) FAK phosphorylation and co-precipitation with β1 integrin. LK25 or AS24 cells grown as monolayers were starved for 24 h and lysed. The cell lysates were subjected to IP with anti FAK antibodies and the IPs were used to detect phospho-FAK (upper panel), FAK (middle panel) and β1-integrin (lower panel)
I next examined whether FAK phosphorylation was dependent on its association with the β1-integrin and whether this association was dependent on the state of integrin activation. FAK immunoprecipitated from LK25 (with active α5β1) or AS24 (with inactive α5β1) cell lysates was associated with a similar amount of β1-integrin (Figure 1e), suggesting that the state of integrin activation does not regulate FAK binding. However, the level of FAK phosphorylation was reduced by threefold in AS24 and in D-HEp3 cells with low uPAR (Figure 1d,e). Thus, while FAK association with the integrin appears to be constitutive, its phosphorylation correlates with the level of uPAR and the state of activation of the β1-integrin. Confocal laser scanning microscopy revealed that Tyr-397 phosphorylated FAK was enriched in focal and point contact-like structures at the cell margins of T-HEp3 cells (Figure 2a). In contrast, D-HEp3 cells with low uPAR had no detectable focal contacts, the point contact-like structures were diminished and a weaker staining of PY-397-FAK was found at the cell margins (Figure 2b), suggesting that uPAR reduction prevents the organization of these structures and efficient FAK phosphorylation. I confirmed the dependence of FAK activation on uPAR by overexpressing uPAR in D-HEp3 cells that have low uPAR and low FAK activity. High level of uPAR protein (threefold increase) (Figure 2c) did not affect significantly FAK level, but caused an increase in FAK phosphorylation as detected with anti-phosphotyrosine Ab (total phosphorylation ∼120 kDa band) and with an anti phospho-FAK-Tyr397 Ab (Figure 2c). Immunoprecipitation of FAK followed by Western blotting for phospho-FAK-Tyr397 and for FAK after stripping of the membrane (Figure 2d), showed a strong uPAR-dependent increase in FAK phosphorylation of the Y397 residue. These results linked FAK activation to high level of uPAR.
Comparison of phospho-FAK localization and Src association with FAK in T-HEp3 and D-HEp3 cells. Effect of uPAR re-expression on FAK activation in D-HEp3 cells. T-HEp3 (a) or D-HEp3 (b) cells were plated (4×105 cells/well) on serum coated glass coverslips and grown overnight in 10% FBS and for an additional 24 h in the absence of serum. Cells were washed fixed and stained for phosphorylated FAK at Tyr-397 as indicated in Materials and methods. Note the large point and focal contact-like structures evident at the cell margins of T-HEp3 but not D-HEp3 cells. (c) Lysates of D-HEp3-vector (Vector) or -uPAR (uPAR) transfected cells were used to detect uPAR (uPAR) levels, phosphorylation of FAK Tyr-397 (PY-397-FAK), total phosphorylation of FAK (∼120 kDa band, PY) and total FAK (FAK) level by Western blot. The O.D. for uPAR levels in arbitrary units are 0.29 and 0.99 for D-HEp3-Vector and D-HEp3-uPAR, respectively. The ratio of PY/FAK in Vector and uPAR cells was 0.15 and 0.32 (arbitrary units) respectively and the ratio of PY397-FAK/FAK signals in Vector- and uPAR-transfected cells was 0.33 and 1.18 (arbitrary units) respectively. (d) Lysates of D-HEp3-Vector or D-HEp3-uPAR cells were subjected to IP with anti FAK antibodies and blotted with anti PY397FAK (upper panel) and FAK (lower panel), as indicated above. The numbers beneath the blots show the ratios of PY397-FAK/FAK signals. (e) Association of FAK and Src. T-HEp3 and D-HEp3 cells were grown as monolayers, starved for 24 h and lysed. The cell lysates were subjected to IP with anti-Src mAb 327 and the IPs were analysed by SDS–PAGE and Western blotting for either phospho-Y-proteins (P-FAK and P-Src), FAK (FAK) or Src (Src). The arrows indicate phospho FAK, FAK, Src and phospho-Src bands. (f) Detection of phosphorylated Src at Tyr-416 by Western blot of T-HEp3 or D-HEp3 lysates prepared with RIPA lysis buffer and using phospho-specific anti Tyr416-Src polyclonal antibodies
In addition, since FAK association with Src is indicative of an active signaling complex (Zhao et al., 1998), Src association with FAK was compared in lysates of T-HEp3 and D-HEp3 cells. In spite of similar amounts of Src being present in immunoprecipitates of T-HEp3 and D-HEp3 cell lysates (Figure 2e), Src was found to form a complex with FAK only in T-HEp3 cells (Figure 2e). The Src that associated with FAK in T-HEp3 cells showed higher phosphorylation than in D-HEp3 cells as detected with anti phospho-Tyr Western blot of the Src IP. In addition, blotting of T-HEp3 and D-HEp3 RIPA extracted lysates with specific anti-PY-416 antibodies showed that phosphorylation of this residue (activating phosphorylation) was higher in T-HEp3 and D-HEp3 cells, strongly suggesting that Src is active when in complex with FAK (Figure 2f). These data strongly suggest that there is a constitutive association between phosphorylated forms of FAK and Src at activation residues only in tumorigenic cells with high uPAR levels and active α5β1 integrins.
Interference with FAK signaling by FRNK inhibits Ras and ERK activation
Since there is a major difference between T-HEp3 and D-HEp3 cells in the state of ERK activation, and because Ras is the best characterized activator of the Raf-Mek-ERK signaling cascade, Ras activation in these cells was analysed. Using a GST pull-down assay, in which only the active GTP-bound Ras is precipitated with a Ras-binding domain of Raf-1 and GST (RBD-GST) fusion protein bound to Sepharose beads, a ∼2.5-fold increase in GTP-bound Ras was found in T-HEp3 cells, compared to D-HEp3 cells. This difference was not due to a difference in total Ras expression levels (Figure 3a). In addition, the low level of GTP-Ras found in AS24 or vector-transfected D-HEp3 cells, was restored to that found in T-HEp3 cells (Figure 3b) by over-expression of uPAR in D-HEp3 cells (Figure 2c). No differences in total Ras levels were observed among these cell lines (Figure 3b). Thus, the association between uPAR-α5β1, which activates FAK, generates a constitutive and robust activation of Ras, which is absent in dormant uPAR-poor cells. This result correlates with the divergent ERK activation observed in T-HEp3 and D-HEp3 cells or in D-HEp3 cells stably expressing an ‘empty’ vector or uPAR (Figures 3b, 4f), suggesting that activation of FAK and Src by uPAR-α5β1 integrin promotes mitogenic signaling through Ras and ERK. To test the activation of potential FAK downstream targets, HEp3 cells were stably transfected with a dominant negative FAK related non-kinase protein (HA-FRNK) or a mutant FRNK (HA-S1034-FRNK) (Figure 3c,d and 4e). Expression of HA-FRNK reduced the level of FAK phosphorylation detected with anti-phospho-Tyr Ab or anti-phospho-Tyr397-FAK antibodies without affecting total FAK protein levels (Figure 3c). The inhibitory effect of FRNK is believed to be due to its ability to compete with and displace FAK from focal contacts (Zhao et al., 1998). This mechanism is supported by the findings in HEp3 cells showing that immunofluorescence staining of phospho-Y397-FAK (not present in FRNK) in Vector and S1034-FRNK expressing cells produced a pattern of clear punctate fluorescence localized at cell margins and resembling point and focal contact-like structures at adhesion sites (Figure 3d left and right panels). In contrast, cells expressing FRNK in addition to showing a marked decrease in the number (∼70–80%) and size of these structures, and in the intensity of the fluorescence also showed a more random distribution of the remaining phosphorylated-FAK (Figure 3d middle panel). FRNK, when expressed negates FAK function by displacing FAK from focal adhesions (Zhao et al., 1998), while S1034-FRNK, is not targeted to focal adhesions, does not inhibit cell migration and does not prevent FAK phosphorylation (Cooley et al., 2000; Sieg et al., 1998). In contrast to the vector or S1034-FRNK transfected T-HEp3 cells, where active Ras was readily detected, in cells stably expressing HA-FRNK the amount of active Ras was dramatically reduced (Figure 4a). To test whether FRNK inhibition of FAK signaling specifically affected ERK activation, T-HEp3 cells were transiently co-transfected with wt HA-FRNK or the mutant HA-S1034-FRNK and an HA-ERK2 expression vector. Expression of HA-FRNK reduced the activation of HA-ERK2 by threefold compared to vector transfected cells (Figure 4b). In contrast, expression of S-1034-HA-FRNK did not reduce the phosphorylation of the co-transfected HA-ERK2 (Figure 4c) confirming that FAK is an upstream activator of ERK.
Ras activation in uPAR-rich and uPAR-poor HEp3 cells and effect of FRNK expression on FAK phosphorylation and localization. (a) Ras activation in T-HEp3 and D-HEp3 cells. Whole cell lysates (600 μg) were incubated with sepharose beads conjugated with GST-RBD-Raf1 (RBD-Raf1, Ras binding domain of Raf1) and the precipitates (GTP-loaded Ras, upper panel) or whole cell lysates (total Ras) were analysed for Ras levels by Western blot using anti-Ras mAb. (b) (Upper two panels) Re-expression of uPAR in D-HEp3 cells activates Ras. The same GST-pull down assay used in (a) was used for whole cell lysates (400 μg) of AS24 cells or D-HEp3 cells transfected with an empty vector or with uPAR-containing vector. The levels of active and total Ras were determined as in (a); (Lower two panels) Active (P-ERK1/2) and total (ERK1/2) levels of ERK1/2 in D-HEp3 cells transfected with an empty vector or with uPAR-containing vector. (c) Stable expression of HA-FRNK in T-HEp3 cells inhibits FAK phosphorylation. T-HEp3 cells were transfected with a pcDNA3.1 vector, ‘empty’ or encoding HA-FRNK and hygromycin (125 μg/ml in 10% FBS-containing RPMI) resistant clones were selected. The empty vector (Vector) or the HA-FRNK expressing (FRNK) clones were pooled, expanded and whole cell lysates were tested by Western blot for FAK phosphorylation (P-FAK and PY397-FAK) and for FAK and HA-FRNK expression levels (FAK and HA-FRNK). (d) Localization of phospho-FAK in FRNK and S1034-FRNK expressing HEp3 cells. T-HEp3-Vector, -FRNK or -S1034-FRNK (left, center and right panels, respectively) cells were plated (4×105 cells/well) on serum coated glass coverslips and grown overnight in 10% FBS and for an additional 24 h in the absence of serum. Cells were washed fixed and stained for phosphorylated FAK at Tyr-397 as indicated in Materials and methods. In Vector and S1034-FRNK expressing cells, P-Y397-FAK had a clear punctate and focal distribution at the cell margins where active adhesion and de-adhesion events take place. In contrast the intensity of phosphorylated FAK was reduced in FRNK-expressing cells and the remaining phosphorylated FAK appeared randomly distributed, suggesting reduced phosphorylation and targeting to adhesion sites due to competition by FRNK. Bar 40 μm
FRNK specifically inhibits uPAR-induced activation of Ras and ERK. (a) The GST-pull down assay was used to detect active (GTP-Ras) or total (Ras) Ras in whole cell lysates (250 μg) of T-HEp3 cells stably transfected with an empty vector (Vector), with a vector encoding HA-FRNK (HA-FRNK) or a vector encoding the mutant S1034-FRNK (S1034-FRNK). (b) wt HA-FRNK inhibits constitutive ERK activation. Control LK25 cells or cells co-transfected with HA-ERK expression vector and empty pcDNA3.1 or HA-FRNK expression vectors (10 μg of each) were grown for 24 h in 10% FBS-containing medium and for an additional 24 h in the absence of serum. The cells were lysed and the lysates were IPed with anti-HA-Ab and the IPs were analysed for activated ERK and HA-tagged proteins using phospho-ERK specific Abs and anti-HA Abs, respectively. The arrows indicate phosphorylated HA-ERK2 (upper panel) and HA-FRNK (lower panel, 46 kDa band) and HA-ERK2 (lower panel, 42 kDa band). NT, not transfected controls. (c) A mutant S-1034-HA-FRNK that does not localize to focal contacts does not inhibit ERK activation. Cell transfections, cell culture conditions, IP and Western blot were performed as in b, except that the co-transfections were performed using an S-1034-HA-FRNK mutant. The arrows also indicate the position of phospho-ERK (upper panel) and HA-tagged proteins (lower panel). HA-FRNK and S-1034-HA-FRNK have the same MW. In b and c PE/E indicates the ratios of phospho-ERK/ERK signals in arbitrary units. (d) Stable expression of HA-FRNK in T-HEp3 cells inhibits ERK activation. T-HEp3 cells stably expressing an ‘empty’ or HA-FRNK encoding vector were tested for ERK phosphorylation (P-ERK, upper panel) and expression (ERK, middle panel). FRNK does not inhibit uPAR expression (lower panel). Whole cell lysates from Vector or FRNK T-HEp3 cells were tested for uPAR levels using R2 mAb as indicated in Materials and methods. (e) Stable expression of HA-S1034-FRNK mutant did not affect ERK protein levels (middle panel) or its phosphorylation state (upper panel); HA-S1034-FRNK expression was confirmed by Western blot anti HA-epitope (lower panel). (f) Total (ERK2) and active (P-ERK1/2) ERK levels in T-HEp3 cells vector- or HA-FRNK-transfected and in D-HEp3 cells grown as monolayers and serum-starved for 24 h
FAK activation of ERK is essential for HEp3 cells tumor growth in vivo
To study the role of FAK-activated Ras-ERK pathway in T-HEp3 tumor cells growth in vivo, I further characterized the stable transfectants of T-HEp3 cells expressing HA-FRNK, HA-S1034-FRNK or vector controls. The level of active, but not total ERK, was reduced only in FRNK-expressing cells (Figure 4d). In contrast, stable transfection of HA-S1034-FRNK caused no inhibition of ERK phosphorylation, supporting the specificity of the dominant negative function of FRNK (Figure 4e). Although ERK was reduced in FRNK expressing cells their in vitro growth in 10, 5, 1 or 0.5% serum was similar to vector-expressing cells as measured using an MTT assay (data not shown) indicating that, as previously reported (Aguirre Ghiso et al., 1999, 2001), the lower ERK activation does not affect in vitro growth of HEp3 cells. We have previously shown that uPAR-mRNA (and protein) level was correlated with the level of ERK activation in T-HEp3 cells; active ERK positively regulated uPAR expression (Aguirre Ghiso et al., 1999). Expression of FRNK, however, did not reduce uPAR expression (Figure 4d), possibly because active ERK levels in FRNK-expressing cells were still higher than those in D-HEp3 cells (Figure 4f). Together, these results indicate that FAK is an essential mediator of ERK activation signal initiated by uPAR-integrin association and that interfering with FAK activation inhibits the signal to ERK. Based on our previous results (Aguirre Ghiso et al., 1999, 2001), this reduction in active ERK levels may induce tumor dormancy in vivo.
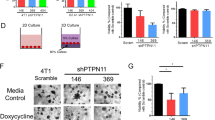
To test whether inhibition of FAK activity by FRNK expression was sufficient to bring the mitogenic signal below a threshold required for in vivo growth, T-HEp3 cells (2×105) expressing an empty vector, HA-FRNK or HA-S1043-FRNK containing vector were inoculated onto CAMs of 9–10 day old chick embryos and their growth was followed for up to 6 weeks by weekly re-inoculation of tumor fragments onto new CAMs as previously reported (Yu et al., 1997). As shown in Figure 5a, T-HEp3 cells expressing an empty vector formed progressively growing, large tumors. In contrast, T-HEp3 cells expressing HA-FRNK (Figure 3c) developed small nodules (∼25 mm3), that did not increase in size over the period of 6 weeks (Figure 5a). S1034-FRNK-expressing cells produced large tumors indistinguishable from those produced by Vector-expressing cells as early as 2 weeks after inoculation, indicating that the reduction in FAK-ERK signaling and growth in vivo was FRNK-dependent (Figure 5a). I further examined if reduced proliferation in vivo due to FRNK expression was in fact due to low ERK signaling, by expressing a constitutively active mutant of Mek (R4F-Mek) in T-HEp3-FRNK cells (Figure 5c); expression of active R4F-Mek was confirmed by Western blot with anti-Mek Abs (Figure 5c, inset) and expression of the Mek mutant did not affect FRNK expression as detected by Western blot with anti-HA antibodies (Figure 5c, inset). Vector or R4F-Mek expressing cells were inoculated on the CAMs and after 5 days the number of cells per tumor nodule were determined as indicated previously (Aguirre Ghiso et al., 1999, 2001). Expression of R4F-Mek in FRNK expressing HEp3 cells was accompanied by a loss of dormancy and after 5 days on the CAM, their number was similar to that produced by inoculation of T-HEp3-vector cells transfected with an ‘empty’ vector. Transfection of FRNK expressing cells with an ‘empty’ vector did not interfere with FRNK ability to lower the number of tumor cells in the tumor nodules (Figure 5c).
FRNK expression inhibits tumor growth of T-HEp3 cells. (a) Vector transfected or HA-FRNK transfected T-HEp3 cells were inoculated onto 9–10 days old chicken embryos CAMs (2×105 cells/CAM). Tumor growth was monitored by weekly measurements of the tumor diameters after which the tumors were excised, minced and reinoculated onto new 9–10 days old CAMs. The Y-axis of the graph shows the tumor volume in mm3 as calculated using the formula (Dxd2)/2 where D is the longest diameter and d is the shorter diameter. Starting with the first week of growth the tumor volumes between T-HEp3-Vector and T-HEp3-FRNK cells were statistically different (Mann–Whitney test P<0.001). In two independent experiments no statistically significant difference was found between T-HEp3-Vector and T-HEp3-S1034-FRNK tumors after two weeks (Mann–Whitney test P<0.3). The upper panel shows a photograph of three representative T-HEp3-Vector and T-HEp3-HA-FRNK tumors after 6 weeks of growth (Bar: 8 mm). This experiment was repeated three times with similar results. (b) Phosphorylation of Akt kinase after serum starvation in vector or FRNK expressing HEp3 cells detected with specific anti-phospho Akt (P-Akt) or anti-Akt (Akt) antibodies in a Western blot. (c) An active mutant of Mek rescues FRNK-expressing cells from dormancy. T-Vector or T-FRNK cells transfected with an empty vector or T-FRNK cells transfected with a vector encoding an active mutant of Mek (R4F-Mek) were inoculated onto 10 day old CAMs and 5 days later the number of tumor cells per CAM was determined as indicated in Materials and methods; levels of Mek (upper inset) or HA-FRNK (lower inset) in T-Vector (lane 1), T-FRNK (lane 2) and T-FRNK-R4F-Mek (lane 3) expressing cells. A ∼2.8-fold increase in Mek levels were detected upon transfection of the R4F-Mek mutant as compared with empty vector transfected cells. *P<0.001 T-Vector vs T-FRNK and **P<0.01 T-FRNK vs T-FRNK-R4F-Mek1 as determined by ANOVA test. (d) Apoptosis in T-HEp3-Vector and T-HEp3-HA-FRNK tumors as determined using a TUNEL assay. Tumors grown for a week were excised, fixed and paraffin sections were stained for DNA breaks as indicated in Materials and methods. As a positive control, sections from FRNK tumors were treated for 10 min with DNAse to induce DNA cleavage. Note the high staining in DNAse treated section (DNAse) and equally low apoptosis in both Vector and FRNK tumors (Bar: ∼40 μm). This experiment was repeated twice
To test whether an increased rate of apoptosis was responsible for the lack of progressive growth (dormancy) of the FRNK-expressing cells, sections of T-HEp3-Vector and FRNK-expressing cells, grown for a week in vivo, were analysed by TUNEL staining. As shown in Figure 5d, the per cent of apoptotic cells was similar in growing and dormant tumors (Figure 5d), suggesting that reduced proliferation was responsible for dormancy. This conclusion was strengthened by the finding (Figure 5b) that there was no difference between T-HEp3-Vector and T-HEp3-FRNK cells in the expression and phosphorylation of Akt/PKB, known to be an important survival pathway and by the fact that R4F-Mek expression (that activates the ERK mitogenic pathway downstream of FAK), can revert the FRNK-induced inhibition (Figure 5c). These results indicate that FAK signaling through Ras and Mek is essential for generation of high ERK signaling crucial for sustaining of the cell cycle progression and tumor growth in vivo. Inhibition of FAK signaling is sufficient to force HEp3 carcinoma cells into dormancy in vivo.
Discussion
Results of the experiments described in this manuscript, which directly test the role of FAK in tumor growth in vivo, suggest a functional basis (Jones et al., 2000) for the correlation described in the literature (Kornberg, 1998; Owens et al., 1995) that links the overexpression of FAK in human tumors with their increased malignant potential.
In the HEp3 cancer cell model described here FAK signaling, induced by FN and the activating association of uPAR with α5β1 integrin, was shown to be essential for maintaining a high level of Ras-ERK signaling, a crucial pathway for in vivo growth of this epithelial tumor. The role of FAK function in the signaling cascade leading to ERK activation was tested by transfecting the tumorigenic cells with FRNK, a naturally occurring dominant negative form of FAK. Expression of FRNK, which reduced ERK activation in these cells by threefold, severely impaired their ability to proliferate in vivo. Compared to vector-transfected HEp3 cells, that formed large tumors on the CAMs of chick embryos, the FRNK expressing cells produced small nodules that survived but did not increase in size even after 6 weeks in vivo. Induction of tumor dormancy by FRNK was not due to increased apoptosis (Figure 5d), and its expression did not change the level of active Akt (Figure 5b), a known mediator of cell survival pathway. The lack of increased apoptosis was not entirely surprising since FRNK, which like FAK, contains the proline rich SH3-binding site (PR1), can bind and activate a Cas-Rac-PAK-JNK matrix-dependent survival pathway (Almeida et al., 2000). It is only when FAK expression per se is eliminated by antisense inhibition, or when a truncated form of FAK which does not contain the PR1 domain is overexpressed, causing a loss of CAS or PI3K binding to FAK, that apoptosis is induced (Xu et al., 1996, 1998). Recently, Wang et al. (2000) showed that astrocytoma cells overexpressing wtFAK had increased proliferation rates when inoculated into the brains of SCID mice and this behavior correlated with increased mitosis and not reduced apoptosis. It is therefore possible to conclude that FRNK-induced blockade of tumor growth is due to a reduced level of active ERK that blocks proliferation without affecting apoptosis. A different scenario was recently described (Lu et al., 2001) where inhibition of FAK activation by EGF treatment, or by FRNK expression, stimulated in vitro motility and invasion in A431 cells highly overexpressing EGFR. FRNK induced rounding of A431 cells, (not observed in HEp3 cells), did not affect EGF-induced ERK mitogenic signals but increased the incidence of metastasis. The source of the difference with our results remains unclear, but while the authors attributed the increased metastatic ability of FRNK-expressing cells to the increased motility and invasion in vitro (Lu et al., 2001), alternatively FRNK-induced survival (Almeida et al., 2000), might contribute to the increased incidence in metastases as detected by Alu-sequence specific PCR. In support of a role for FAK in cell invasion, recent experiments showed that active FAK has a functional role during invasion of trophoblast cells (Ilic et al., 2001).
We have previously shown that in T-HEp3 cells, the interaction of over-expressed uPAR with the α5β1 integrin in the presence of endogenously produced uPA, which occupies ∼90% of uPA receptors, promotes ERK activation and the formation of FN-fibril that suppress p38SAPK signaling, stimulating proliferation in vivo (Aguirre-Ghiso et al., 1999, 2001). Published evidence indicates that FRNK affects FAK-mediated signaling by displacing it from focal adhesion sites where it normally co-localizes at the tips of stress fibers with integrins (Cooley et al., 2000). This seems to be the case in the experiments shown here because FRNK, but not its inactive mutant S1034-FRNK, caused a reduction in the staining of phosphorylated-FAK at adhesion sites and the remaining phospho-FAK appeared randomly distributed in the cell body. However, the reduction of FAK and ERK phosphorylation mediated by expression of FRNK affected neither the activation of p38SAPK (data not shown) nor the ability to form FN-fibrils; both vector and FRNK-transfected cells formed a rich matrix of fibrillar FN (data not shown). That FRNK expression did not prevent FN-fibrillogenesis may be explained by the fact that fibrillogenesis may be initiated predominantly at tensin-containing ECM-contacts, where FAK is not present (Zamir et al., 2000). These results suggest that in these cells induction of dormancy by FRNK is due to specific targeting of the Ras-ERK, but not the p38SAPK pathways.
Published work indicates that caveolin, which is downregulated in tumor cells and in transformed fibroblasts (Bender et al., 2000, Racine et al., 1999; Koleske et al., 1995) is required for FAK and Src activation in uPAR-transfected 293 kidney cells (Wei et al., 1999). However, in other reports (Sanders and Basson, 2000), integrin signaling can proceed in the absence of caveolin. Western blot using anti-caveolin antibodies showed no expression of this protein in HEp3 cells (data not shown). This suggests that another scaffolding protein may be involved in organizing the signaling complexes, or that highly expressed uPAR may be fulfilling this role. The latter possibility is suggested by the finding that in HEp3 cells FAK is associated with β1 integrins regardless of their state of activation but, only in the presence of high level of uPAR, the β1-associated FAK is phosphorylated. It is possible that the high number of uPA receptors on the cell surface cluster integrins and that ligand-induced conformational change increases the proximity between FAK molecules leading to their trans-phosphorylation (Zhao et al., 1998). The constitutive phosphorylation of Tyr397 of FAK in uPAR-overexpressing cells may explain the enhanced interaction with phosphorylated Src, since this is the major Src binding site on FAK (Zhao et al., 1998). It cannot be excluded that other mechanisms, such as ‘activating’ phosphatases (Arregui et al., 1998) may activate Src and therefore FAK. The expected downstream sequel of FAK and Src activation is activation of Ras. Although the precise mechanism of this event is not entirely clear, the fact that Ras activation is significantly inhibited by expression of FRNK puts this mediator down-stream in the path of FAK activation. Preliminary analysis showed that neither Shc nor Grb2 bind to FAK in T-HEp3 cells (data not shown), suggesting that direct interaction of these molecules is not required for Ras activation. However, this does not exclude that through other mechanisms independent of interaction with FAK, Shc and Grb may lead to Ras activation (Brown and Cooper, 1996).
Together, these results represent one of the first attempts of testing the role of FAK in signal transduction induced by activating association of uPAR with integrin and its effect on epithelial tumor growth in vivo. These results lend functional significance to the finding of frequent overexpression of FAK in tumors from different origin by indicating that active FAK may enable tumor cells to activate more efficiently survival and mitogenic signals derived from the ECM, providing a growth advantage at the primary or metastatic growth site. These results also show that, similarly to blocking uPAR expression (Aguirre Ghiso et al., 1999; Yu et al., 1997), blocking FAK signaling can reduce ERK signaling and induce dormancy in vivo making FAK a potential target for induction of cancer dormancy in vivo.
Materials and methods
Reagents and antibodies
DMSO, Triton X-100, Na-orthovanadate, NaFl, protease inhibitors, BSA, normal goat serum, collagenase type 1A, rhodamine-phalloidin conjugate, human fibronectin were from Sigma Chemical Co (St. Louis, MO, USA). Aprotinin and trypsin were from ICN Biomedicals Inc (Aurora, OH, USA). Dulbecco's modified minimal essential medium (DMEM), OPTI–MEM medium, glutamine and antibiotics were from GIBCO Laboratories (Grand Island, NY, USA). Fetal bovine serum was from JRH Biosciences (Lenexa, KS, USA), COFAL-negative embryonated eggs were from Specific Pathogen-Free Avian Supply (SPAFAS) (North Franklin, CT, USA); protein G-Agarose beads were from Boehringer Mannheim (Indianapolis, IN, USA). PVDF membranes and Enhanced Chemiluminescence (ECL) detection reagents were from Amersham (Amersham Life Sciences, Little Chalfont, UK). DAPI, 49,6-diamidino-2-phenylindole was from Hoechst (Germany). Antibodies: anti-phospho ERKoslash; (anti-phospho-Tyr 204; clone E4) and anti-p38 antibodies were from Santa Cruz Biotechnology Inc. (Santa Cruz, CA, USA). Anti-phospho-p38 rabbit polyclonal antibodies were from New England Biolabs (Beverly, MA, USA). Antibodies to ERKoslash; (Clone MK12), FAK, Caveloin-1 and phosphotyrosine (RC20) were from Transduction Laboratories (Lexington, KY, USA). Antibodies to FAK (2A7), to phosphorylated-Src (PY-416) and active-Ras detection kit were from Upstate-Biotechnology (Lake Placid, NY, USA). Anti-FAK phosphorylation state specific antibody which recognizes phospho-Tyr397 was from BioSource International (Camarillo, CA, USA). Normal mouse IgG was from Sigma. Anti-human uPAR monoclonal Ab R2 was kindly provided by Dr Michael Ploug (Finsen Laboratory, Copenhagen, DK). Anti-Src antibody (mAb 327) was kindly provided by Dr Irwin Gellman (Mount Sinai School of Medicine). Anti-uPAR polyclonal rabbit antibody (399R) was from American Diagnostica, polyclonal rabbit anti-β1 antibody (Mab1952) and anti-α5β1 antibody (Clone HA5) were from Chemicon International, Inc. (Temecula, CA, USA). Anti-mouse IgG monoclonal Ab conjugated with HRP and mounting media (Vectashield) were from Vector Laboratories (Burlingame, CA, USA). Anti-rabbit IgG-HRP and anti-HA Abs (clone 12CA5) were from Boehringer Mannheim (Germany).
Cell lines, cDNA transfections and cell culture conditions
Human epidermoid carcinoma HEp3 (T-HEp3) (Toolan, 1954), serially passaged on chicken embryo CAMs, was used as a source of tumorigenic cells (Aguirre Ghiso et al., 1999; Yu et al., 1997). The source of ‘spontaneous’ dormant tumor cells (D-HEp3) were HEp3 cells passaged in vitro 120 to 170 times (Ossowski and Reich, 1983) with uPAR level of only ∼20% of that in tumorigenic cells (Aguirre Ghiso et al., 1999). HEp3 cells transfected with the expression vector LK444 (control, LK25, high uPAR and tumorigenic) or with LK444 vector expressing antisense uPAR-mRNA (clone AS24, uPAR message and protein reduced by 70–80%, dormant) were described previously (Aguirre Ghiso et al., 1999; Yu et al., 1997). After FugeneTM transfection (Roche) stable transfectants of D-HEp3 cells expressing pCDNA3.1 vector alone (encoding hygromycin resistance) or pCDNA3.1 encoding full-length uPAR cDNA, were selected with hygromycin (125 μg/ml). Also, T-HEp3 cells were transfected using FugeneTM transfection method with pCDNA3.1 vector alone or pCDNA3.1 vector encoding triple-HA-tagged-FRNK or HA-tagged-S1034-FRNK mutant, kindly provided by Dr David Schlaepfer (Scripps Institute, CA, USA) and selected with 125 μg/ml hygromycin (Sigma). For all hygromycin resistant cell lines, clones were pooled and these pools were used in all experiments to avoid clonal variation. Expressions of uPAR or HA-epitope were monitored by Western blot (see below). Cell lines were always kept in D-MEM+10%FBS and 125–150 μg/ml hygromycin. These cell lines did not differ dramatically in their growth rates or morphology in culture after transfection and hygromycin selection even in different serum concentrations (0.5–10% FBS) as detected using an MTT assay (data not shown). Vector or FRNK expressing cells were also transiently transfected using FugeneTM, with 4 μg of an empty vector or with 4 μg of a vector encoding R4F-Mek mutant, kindly provided by Dr Natalie Ahn (University of Colorado, CO, USA).
To test the effect of FRNK expression on ERK activation using transient transfections T-HEp3 or LK25 cells were co-transfected with 1 μg of pCDNA3.1 vector alone and 1 μg of HA-ERK2 construct as previously reported (Aguirre Ghiso et al., 1999) or with 1 μg of pCDNA3.1-HA-FRNK with the same HA-ERK2 construct. As a control of FRNK specificity T-HEp3 cells were cotransfected with pCDNA3.1 alone and the HA-ERK2 construct or pCDNA3.1-S1034-HA-FRNK (a mutant of FRNK that does not localize to focal contacts and therefore does not compete with endogenous FAK) (Cooley et al., 2000; Sieg et al., 1998) and the HA-ERK2 construct. After transfection and 48 h in culture to ensure maximal expression, HA-FRNK expression and HA-ERK2 expression and phosphorylation were detected by immunoprecipitation and Western blot as previously reported (Aguirre Ghiso et al., 1999).
Immunoprecipitation (IP) and Western blot
For optimal α5β1-integrin and uPAR co-IP cells, were lysed and extracted for 30 min with a lysis buffer containing 1% Triton X-100, 50 mM HEPES pH 7.5, 150 mM NaCl, 1 mM CaCl2, 1 mM MgCl2, 1 mM orthovanadate, 1 mM NaFl, and protease inhibitors. Triton X-100 insoluble fractions (400 μg protein) were extracted for 30 min with RIPA lysis buffer and incubated with 4 μg of anti-α5β1 (HA5) or matched isotype IgG overnight at 4°C. For FAK IP cells were lysed using a 0.5% NP-40, 150 mM NaCl, 50 mM Tris HCl pH 8.0 5 mM EDTA lysis buffer and 400–600 μg of soluble extract were incubated 1.5 h at 4°C with 4 μg of anti-FAK 2A7 monoclonal Ab. For Src IP 1–1.5 mg of lysates obtained with the same NP-40 lysis buffer were incubated 1.5 h at 4°C with 10 μg of anti-Src mAb 327. The NP-40 buffer was found to be optimal for FAK and Src IP and co-IP studies. For IP of HA-tagged proteins cells were lysed using a lysis buffer, which optimizes HA-FRNK and HA-ERK extraction, containing 300 mM NaCl, 10% glycerol, 20 mM HEPES (pH 7.6), 5 mM MgCl2, 1 mM EGTA, 1 mM DTT, 1 mM Na-orthovanadate and 10 mM NaFl and a cocktail of protease inhibitors and 400 μg of protein were incubated 1.5 h in with 2.5 μg of 12CA5 anti-HA mAb. In all cases antibody antigen complexes were precipitated with protein G-agarose beads and washed three times. The beads were resuspended in 2× Laemmli sample buffer, heated to 95°C for 5 min and analysed by Western blotting. Cell lysates samples or the IPs were separated in SDS–PAGE gels in reducing or non-reducing conditions (depending on the antigen) and after electro-transfer to PVDF membranes, these were blocked with 5% skim milk in TBS except for phospho-Y blots for which the membranes were blocked with 3% BSA in TBS. Integrin β1 was detected using a pAb (anti-β1 MAB1952) and uPAR using anti-uPAR 399R pAb. FAK protein was detected using anti-FAK mAb in IPs and cell lysates. Immunoprecipitated phospho-Y-FAK or phospho-Y proteins present in whole cell lysates were detected using anti-phospho-Y-HRP conjugated Ab (RC20) or anti-phospho-Tyr397 FAK. Urokinase receptor in whole cell lysates was detected using R2 mAb. Except for RC20 Ab, all signals were developed with either goat anti-mouse IgG-HRP or goat anti-rabbit-HRP conjugated antibodies. The signal was developed using ECL (Amersham Life Sciences) and X-OMAT films (Eastman Kodak). When indicated the bands were quantitated by laser densitometry using GelScan XL (Pharmacia, Upsala, Sweden).
Detection of activated Ras by GST pull-down
GTP-loaded and therefore active Ras was detected using a Ras activation kit from Upstate Biotechnology following the vendor's instructions. Briefly, cell monolayers were lysed directly after removing the media with a 2% glycerol, 25 mM HEPES, pH 7.5, 150 mM NaCl, 1% Igepal CA-630, 10 mM MgCl2 and 1 mM EDTA containing lysis buffer with all protease and phosphatase inhibitors. After 20-min extraction, the lysates were cleared by centrifugation. The supernatants (200–600 μg of protein) were incubated for 30 min with sepharose beads conjugated with a GST-Ras binding domain of Raf-1 (3–10 μl of beads/3–10 μg of RBD-Raf1) fusion protein, which binds only to GTP but not GDP loaded Ras. After incubation, the beads were spun down and washed 3× with lysis buffer. The beads were resuspended in 2× Laemmli sample buffer with 100 mM β-mercaptoethanol and Ras protein in the precipitate or cell lysates was detected by Western blot using anti-Ras mAb from Upstate Biotechnology (Lake Placid, NY, USA) as indicated above.
In vivo growth of tumor cells on CAMs
T-HEp3, D-HEp3, Vector- or HA-FRNK- or HA-S1034-FRNK-transfected T-HEp3 cells were detached with 2 mM EDTA in PBS, washed and inoculated (0.2–1×106 cells/CAM in 50 μl of PBS plus Ca2+ and Mg2+) on the CAMs of 9–10 day old chick embryos. In addition, Vector- or HA-FRNK-transfected cells re-transfected with vector alone or a vector encoding R4F-Mek mutant were inoculated onto CAMs as indicated above. At different times post-inoculation on the CAMs, the tumor nodules diameters were measured, the tumors were excised, enzymatically dissociated with a 30 min collagenase treatment (Aguirre Ghiso et al., 1999), and single cell suspensions inspected for the presence of tumor cells and quantitated by hemocytometer counting. Alternatively after measuring the tumor size the tumor nodules were minced and passages onto new 9–10 days old CAMs in order to continue and monitor tumor growth (Yu et al., 1997).
Detection of apoptosis in vivo by TUNEL assay
Tumors grown on the CAM for 1 week were paraffin embedded and sections were analysed for DNA breaks at single cell level using a terminal deoxydinucleotidyl transferase (TdT) assay kit from Boehringer Mannheim (Germany). Briefly, tumor sections were deparaffinized as described previously (Aguirre-Ghiso et al., 2001) and after permeabilization sections were labeled using fluorescein-tagged nucleotides and TdT from calf thymus. After washing, the sections were first incubated with anti-fluorescein antibodies conjugated with alkaline phosphatase, then for 10 min with NBT/BCIP substrate and the reaction was stopped by washing. A positive control was included in all experiments by incubating the sections with DNAseI (1 μg/ml) in 50 mM Tris HCl, pH 7.5, 1 mg/ml BSA. Sections incubated with all reagents except TdT were used as negative controls. The sections were then mounted and inspected using a Zeiss Axioskop photomicroscope (Oberkochen, Germany) using Plan-Neofluar 20× and 40× lenses (Zeiss) through a Diagnostic Instruments Inc. SPOT digital camera and Adobe Photoshop 5.0 software.
Confocal laser scanning and standard immunofluorescence (IF) microscopy
The protocol for immunostaining was as described previously (Aguirre-Ghiso et al., 2001). Briefly, cells grown on cover slips were fixed with 3% paraformaldehyde in PBS for 15 min. The cover slips were washed and either permeabilized with 0.1% Triton X-100, washed, blocked with 3% normal goat serum in PBS, and incubated for 1 h at room temperature with anti-PY397-FAK polyclonal Ab (1 : 75) in 0.1% BSA/PBS or with vehicle alone. After washing and blocking, the secondary antibody in 0.1% BSA/PBS was added. Cover slips were mounted in Vectashield and kept at −20°C. Standard epifluorescence was captured with a Nikon E-700 epifluorescence photomicroscope (Tokyo, Japan) using Plan-Apochromat 40×, 63× and 100× (N.A. 1.5 Oil) lenses (Nikon) through a Diagnostic Instruments Inc. SPOT digital camera and Adobe Photoshop 5.0 software. Confocal microscopy was performed using a Leica TCS SP Spectral Confocal Laser Scanning Microscope (Leica Microsystems, Heidelberg, Germany) equipped with fiber coupled UV, VIS and IR lasers, using Plan-Apo 40×, 63× and 100× lenses (N.A. 1.4 oil). Data were captured and analysed using the TCS/SP software and Adobe Photoshop 5.0 software.
Abbreviations
- Ab:
-
antibody
- CAM:
-
chorioallantoic membrane
- co-IP:
-
coimmunoprecipitate
- DMSO:
-
dimethylsulfoxide
- ECL:
-
enhanced chemiluminescence ERK, extracellular regulated kinase
- FAK:
-
focal adhesion kinase
- FBS:
-
fetal bovine serum
- FN:
-
fibronectin
- GPI:
-
glycosyl-phosphatidylinositol
- GST:
-
glutathione-S-transferase, HA-ERK hemaglutinin-tagged ERK
- HA-FRNK:
-
hemaglutinin tagged FAK related non kinase
- IF:
-
immunofluorescence
- IP:
-
immunoprecipitation
- MAPK:
-
mitogen-activated protein kinase
- p38:
-
p38-MAPK/stress activated protein kinase 2
- PBS:
-
phosphate buffered saline
- PKB:
-
protein kinase B
- PI3K:
-
phosphatidylinositol-3′-kinase, uPA, urokinase-type plasminogen activator
- uPAR:
-
uPA receptor
References
Aguirre Ghiso JA, Kovalski K, Ossowski L . 1999 J. Cell. Biol. 147: 89–104
Aguirre Ghiso JA, Liu D, Mignatti A, Kovalski K, Ossowski L . 2001 Mol. Biol. Cell. 12: 863–879
Almeida EA, Ilic D, Han Q, Hauck CR, Jin F, Kawakatsu H, Schlaepfer DD, Damsky CH . 2000 J. Cell. Biol. 149: 741–754
Arregui CO, Balsamo J, Lilien J . 1998 J. Cell. Biol. 143: 861–873
Bender FC, Reymond MA, Bron C, Quest AF . 2000 Cancer Res. 60: 5870–5878
Brown MT, Cooper JA . 1996 Biochim. Biophys. Acta 7: 121–149
Cary LA, Guan JL . 1999 Front Biosci. 4: D102–D113
Cooley MA, Broome JM, Ohngemach C, Romer LH, Schaller MD . 2000 Mol. Biol. Cell. 11: 3247–3263
Genda T, Sakamoto M, Ichida T, Asakura H, Hirohashi S . 2000 Lab. Invest. 80: 387–394
Giancotti FG, Ruoslahti E . 1999 Science 285: 1028–1032
Gu J, Tamura M, Yamada KM . 1998 J. Cell. Biol. 143: 1375–1383
Ilic D, Genbacev O, Jin F, Caceres E, Almeida EA, Bellingard-Dubouchaud V, Schaefer EM, Damsky CH, Fisher SJ . 2001 Am. J. Pathol. 159: 93–108
Jones RJ, Brunton VG, Frame MC . 2000 Eur. J. Cancer 36: 1595–1606
Koleske AJ, Baltimore F, Lisanti MP . 1995 Proc. Natl. Acad. Sci. USA 92: 1381–1385
Kornberg LJ . 1998 Head Neck 20: 745–752
Lu Z, Jiang G, Blume-Jensen P, Hunter T . 2001 Mol. Cell. Biol. 21: 4016–4031
Nguyen DH, Webb DJ, Catling AD, Song Q, Dhakephalkar A, Weber MJ, Ravichandran KS, Gonias SL . 2000 J. Biol. Chem. 275: 19382–19388
Ossowski L, Reich E . 1983 Cell 33: 323–333
Owens LV, Xu L, Craven RJ, Dent GA, Weiner TM, Kornberg L, Liu ET, Cance WG . 1995 Cancer Res. 55: 2752–2755
Racine C, Belanger M, Hirabayashi H, Boucher M, Chakir J, Couet J . 1999 Biochem. Biophys. Res. Commun. 255: 580–586
Ruoslahti E . 1999 Adv. Cancer Res. 76: 1–20
Sanders MA, Basson MD . 2000 J. Biol. Chem. 275: 38040–38047
Schiller JH, Bittner G . 1995 Cancer Res. 55: 6215–6221
Sieg DJ, Ilic D, Jones KC, Damsky CH, Hunter T, Schlaepfer DD . 1998 EMBO J. 17: 5933–5947
Toolan HW . 1954 Cancer Res. 14: 660–666
Trusolino L, Cavassa S, Angelini P, Ando M, Bertotti A, Comoglio PM, Boccaccio C . 2000 FASEB J. 14: 1629–1640
Wang F, Weaver VM, Petersen OW, Larabell CA, Dedhar S, Briand P, Lupu R, Bissell MJ . 1998 Proc. Natl. Acad. Sci. USA 95: 14821–14826
Wang D, Grammer JR, Cobbs CS, Stewart Jr JE, Liu Z, Rhoden R, Hecker TP, Ding Q, Gladson CL . 2000 J. Cell. Sci. 113: 4221–4230
Weaver VM, Petersen OW, Wang F, Larabell CA, Briand P, Damsky C, Bissell MJ . 1997 J. Cell. Biol. 137: 231–245
Wei Y, Yang X, Liu Q, Wilkins JA, Chapman HA . 1999 J. Cell. Biol. 144: 1285–1294
Xu LH, Owens LV, Sturge GC, Yang X, Liu ET, Craven RJ, Cance WG . 1996 Cell Growth Differ. 7: 413–418
Xu LH, Yang X, Craven RJ, Cance WG . 1998 Cell Growth Differ. 9: 999–1005
Yu W, Kim J, Ossowski L . 1997 J. Cell. Biol. 137: 767–777
Zamir E, Katz M, Posen Y, Erez N, Yamada KM, Katz BZ, Lin S, Lin DC, Bershadsky A, Kam Z, Geiger B . 2000 Nat. Cell. Biol. 2: 191–196
Zhao JH, Reiske H, Guan JL . 1998 J. Cell. Biol. 143: 1997–2008
Acknowledgements
I am deeply grateful to Dr Liliana Ossowski (Mount Sinai School of Medicine) for continuous encouragement, support and critical reading of the manuscript. I would also like to thank Dr Rafael Mira y Lopez (Mount Sinai School of Medicine) for helpful discussion and critical reading of the manuscript and Dr Dusko Ilic (UCSF) for his helpful and expert advice. The help of Mr Yeriel Estrada and rotating PhD student Lic. Luciana Giono with some of the experiments, is greatly acknowledged. I also thank Dr David Schlaepfer (Scripps Institute, CA, USA) for providing the HA-FRNK and HA-FRNK-S1034 constructs, Dr Fillipo Giancotti (Memorial Sloan Kettering Cancer Center, NY, USA) for the HA-ERK2 construct, Dr Michael Ploug (Finsen Laboratory, Copenhagen, Denmark) for the gift of R2 antibodies, Dr Irwin Gellman (Mount Sinai School of Medicine) for the anti-Src mAb and helpful discussion and Dr Natalie Ahn for the R4F-Mek construct. Confocal laser scanning microscopy was supported with funding from an NSF Major Research Instrumentation grant (DBI-9724504) of the Mount Sinai School of Medicine Microscopy Center. This work was supported by US Public Health Research grant CA-40758 to Dr Liliana Ossowski and by a Charles H Revson Foundation Postdoctoral Fellowship to Dr Julio Aguirre-Ghiso.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Aguirre Ghiso, J. Inhibition of FAK signaling activated by urokinase receptor induces dormancy in human carcinoma cells in vivo. Oncogene 21, 2513–2524 (2002). https://doi.org/10.1038/sj.onc.1205342
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.onc.1205342
Keywords
This article is cited by
-
YY1 regulates the proliferation and invasion of triple-negative breast cancer via activating PLAUR
Functional & Integrative Genomics (2023)
-
Urokinase-type plasminogen activator receptor (uPAR) as a therapeutic target in cancer
Journal of Translational Medicine (2022)
-
Role of integrin α2 in methotrexate-induced epithelial-mesenchymal transition in alveolar epithelial A549 cells
Toxicological Research (2022)
-
KISS1 in metastatic cancer research and treatment: potential and paradoxes
Cancer and Metastasis Reviews (2020)
-
Unearthing Regulatory Axes of Breast Cancer circRNAs Networks to Find Novel Targets and Fathom Pivotal Mechanisms
Interdisciplinary Sciences: Computational Life Sciences (2019)