Abstract
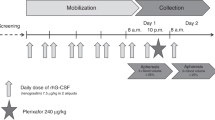
Increasing demand on the apheresis service makes efficient harvesting of peripheral blood stem cells (PBSCs) essential. A total of 168 adult patients with haematological malignancy were primed using low–moderate dose cyclophosphamide (1.5–3 g/m2) with G-CSF 5–10 μg/kg per day. Harvesting was booked and peripheral blood (PB) counts first checked between 6 and 10 days post-priming. One hundred and thirty (77%) patients harvested successfully (total harvest yield ⩾2 × 106 CD34+/kg) and the median PBSC collection per procedure was 2.18 × 106/kg (range 0.1–14.5). Only more lines of prior chemotherapy predicted failure to harvest in multivariate analysis (P=0.003). The PB CD34+ cell count correlated significantly with harvest yield (r=0.8448, P<0.0001). A PB CD34+ count ⩾10/μl predicted a collection of ⩾2 × 106/kg (positive-predictive value of 61%, negative-predictive-value 100%). Patients first attending day 9 required significantly fewer visits to achieve a successful harvest than those first attending days 6–8 without increasing the risk of failure. No significant difference in failure rates, number of days attending and total harvest yield was found between days 9 and 10 attendees. Collection from day 9 may however enable higher target yields to be achieved. PB CD34+ count monitoring should commence and harvesting booked from day 9 to optimize both the harvest and the efficiency of the PBSC harvesting service.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout




Similar content being viewed by others
References
Hill GR, Inder A, Patton WN, Hart DN . High dose therapy and autologous bone marrow versus blood cell rescue. South Island bone marrow transplant unit. N Z Med J 1996; 109: 45–48.
To LB, Roberts MM, Haylock DN, Dyson PG, Branford AL, Thorp D et al. Comparison of haematological recovery times and supportive care requirements of autologous recovery phase peripheral blood stem cell transplants, autologous bone marrow transplants and allogeneic bone marrow transplants. Bone Marrow Transplant 1992; 9: 277–284.
Tyndall A, Daikeler T . Autologous hematopoietic stem cell transplantation for autoimmune diseases. Acta Haematol 2005; 114: 239–247.
Jantunen E, Putkonen M, Nousiainen T, Pelliniemi TT, Mahlamaki E, Remes K . Low-dose or intermediate-dose cyclophosphamide plus granulocyte colony-stimulating factor for progenitor cell mobilisation in patients with multiple myeloma. Bone Marrow Transplant 2003; 31: 347–351.
Scott MA, Ager S, Apperley JF, Jestice HK, Bloxham DM, Boraks P et al. Peripheral blood progenitor cell harvesting in multiple myeloma and malignant lymphoma. Leuk Lymphoma 1995; 19: 479–484.
Deliliers GL, Annaloro C, Marconi M, Soligo D, Morandi P, Luchesini C et al. Harvesting of autologous blood stem cells after a mobilising regimen with low-dose cyclophosphamide. Leuk Lymphoma 2002; 43: 1957–1960.
Jones HM, Jones SA, Watts MJ, Khwaja A, Mills W, Fielding A et al. Development of a simplified single-apheresis approach for peripheral-blood progenitor-cell transplantation in previously treated patients with lymphoma. J Clin Oncol 1994; 12: 1693–1702.
Lerro KA, Medoff E, Wu Y, Seropian SE, Snyder E, Krause D et al. A simplified approach to stem cell mobilization in multiple myeloma patients not previously treated with alkylating agents. Bone Marrow Transplant 2003; 32: 1113–1117.
Petrucci MT, Avvisati G, La Verde G, De Fabritiis P, Ribersani M, Palumbo G et al. Intermediate-dose cyclophosphamide and granulocyte colony-stimulating factor is a valid alternative to high-dose cyclophosphamide for mobilizing peripheral blood CD34+ cells in patients with multiple myeloma. Acta Haematol 2003; 109: 184–188.
Sutherland DR, Anderson L, Keeney M, Nayar R, Chin-Yee I . The ISHAGE guidelines for CD34+ cell determination by flow cytometry. International Society of Hematotherapy and Graft Engineering. J Hematother 1996; 5: 213–226.
Alcorn MJ, Farrell E, Barr J, Pearson C, Green R, Holyoake T . The number of CD34+ cells mobilized into the peripheral blood can predict the quality of subsequent collections. J Hematother Stem Cell Res 2000; 9: 89–93.
Armitage S, Hargreaves R, Samson D, Brennan M, Kanfer E, Navarrete C . CD34 counts to predict the adequate collection of peripheral blood progenitor cells. Bone Marrow Transplant 1997; 20: 587–591.
Elliott C, Samson DM, Armitage S, Lyttelton MP, McGuigan D, Hargreaves R et al. When to harvest peripheral-blood stem cells after mobilization therapy: prediction of CD34-positive cell yield by preceding day CD34-positive concentration in peripheral blood. J Clin Oncol 1996; 14: 970–973.
Gibbs G, Bolam S . Peripheral blood CD34+ cell counts allow improved management of peripheral blood stem cell collections. Br J Biomed Sci 2004; 61: 35–37.
Gidron A, Verma A, Doyle M, Boggio L, Evens A, Gordon L et al. Can the stem cell mobilization technique influence CD34+ cell collection efficiency of leukapheresis procedures in patients with hematologic malignancies? Bone Marrow Transplant 2005; 35: 243–246.
Yu J, Leisenring W, Bensinger WI, Holmberg LA, Rowley SD . The predictive value of white cell or CD34+ cell count in the peripheral blood for timing apheresis and maximizing yield. Transfusion 1999; 39: 442–450.
Fontao-Wendel R, Lazar A, Melges S, Altobeli C, Wendel S . The absolute number of circulating CD34+ cells as the best predictor of peripheral hematopoietic stem cell yield. J Hematother 1999; 8: 255–262.
Kudo Y, Minegishi M, Saito N, Itoh T, Fushimi J, Takahashi H et al. The absolute number of peripheral blood CD34+ cells predicts a timing for apheresis and progenitor cell yield in patients with hematologic malignancies and solid tumors. Tohoku J Exp Med 2003; 199: 111–118.
Moncada V, Bolan C, Yau YY, Leitman SF . Analysis of PBPC cell yields during large-volume leukapheresis of subjects with a poor mobilization response to filgrastim. Transfusion 2003; 43: 495–501.
Drake M, Ranaghan L, Morris TC, Nolan L, Desai ZR, Irvine AE et al. Analysis of the effect of prior therapy on progenitor cell yield: use of a chemotherapy scoring system. Br J Haematol 1997; 98: 745–749.
Ford CD, Green W, Warenski S, Petersen FB . Effect of prior chemotherapy on hematopoietic stem cell mobilization. Bone Marrow Transplant 2004; 33: 901–905.
Haas R, Mohle R, Fruhauf S, Goldschmidt H, Witt B, Flentje M et al. Patient characteristics associated with successful mobilizing and autografting of peripheral blood progenitor cells in malignant lymphoma. Blood 1994; 83: 3787–3794.
Baars JW, Holtkamp MJ, Nooyen WJ, Walll EV, Te VA, Dalesio O et al. Mobilisation of blood progenitor cells with ifosfamide and etoposide (VP-16) in combination with recombinant human G-CSF (Filgrastim) in patients with malignant lymphomas or solid tumours. Anticancer Res 1996; 16: 3089–3095.
Hertzberg MS, Crombie C, Benson W, Taper J, Gottlieb D, Bradstock KF . Outpatient-based ifosfamide, carboplatin and etoposide (ICE) chemotherapy in transplant-eligible patients with non-Hodgkin's lymphoma and Hodgkin's disease. Ann Oncol 2003; 14 (Suppl 1): i11–i16.
Kroger N, Zeller W, Fehse N, Hassan HT, Kruger W, Gutensohn K et al. Mobilizing peripheral blood stem cells with high-dose G-CSF alone is as effective as with Dexa-BEAM plus G-CSF in lymphoma patients. Br J Haematol 1998; 102: 1101–1106.
Nowrousian MR, Waschke S, Bojko P, Welt A, Schuett P, Ebeling P et al. Impact of chemotherapy regimen and hematopoietic growth factor on mobilization and collection of peripheral blood stem cells in cancer patients. Ann Oncol 2003; 14 (Suppl 1): i29–i36.
Watts MJ, Ings SJ, Leverett D, MacMillan A, Devereux S, Goldstone AH et al. ESHAP and G-CSF is a superior blood stem cell mobilizing regimen compared to cyclophosphamide 1.5 g m−2 and G-CSF for pre-treated lymphoma patients: a matched pairs analysis of 78 patients. Br J Cancer 2000; 82: 278–282.
Lee JL, Kim S, Kim SW, Kim EK, Kim SB, Kang YK et al. ESHAP plus G-CSF as an effective peripheral blood progenitor cell mobilization regimen in pretreated non-Hodgkin's lymphoma: comparison with high-dose cyclophosphamide plus G-CSF. Bone Marrow Transplant 2005; 35: 449–454.
Martinez C, Urbano-Ispizua A, Marin P, Merino A, Rovira M, Carreras E et al. Efficacy and toxicity of a high-dose G-CSF schedule for peripheral blood progenitor cell mobilization in healthy donors. Bone Marrow Transplant 1999; 24: 1273–1278.
Kroger N, Renges H, Sonnenberg S, Kruger W, Gutensohn K, Dielschneider T et al. Stem cell mobilisation with 16 vs 10 microg/kg of G-CSF for allogeneic transplantation in healthy donors. Bone Marrow Transplant 2002; 29: 727–730.
Cottler-Fox M, Lapidot T . Mobilizing the older patient with myeloma. Blood Rev 2006; 20: 43–50.
Acknowledgements
Thanks to Phil Jenkin for assistance with data collection.
Author information
Authors and Affiliations
Corresponding author
Additional information
Data have been presented in abstract form at the following meetings.
QA Hill, GM Smith, JA Child and G Cook. Optimal timing of autologous peripheral blood stem cell harvest following priming with cyclophosphamide and G-CSF: significant improvement in outcome harvesting day 9 compared with days 6, 7, 8 or 10. Haematologica, 90(Suppl 2), June 2005, Abstract No. 0487. (Poster presentation: EHA, Stockholm, Sweden, 2005.)
QA Hill, GM Smith, JA Child and G Cook. Optimal timing of autologous peripheral blood stem cell harvest following priming with cyclophosphamide and G-CSF: significant improvement in progenitor cell yield harvesting on day 9–10 compared with day 7–8. British Journal of Haematology, 129(Suppl 1), April 2005, Abstract No. 114. (Poster presentation: BSH, Manchester, 2005.)
Rights and permissions
About this article
Cite this article
Hill, Q., Buxton, D., Pearce, R. et al. An analysis of the optimal timing of peripheral blood stem cell harvesting following priming with cyclophosphamide and G-CSF. Bone Marrow Transplant 40, 925–930 (2007). https://doi.org/10.1038/sj.bmt.1705847
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.bmt.1705847