Abstract
Introduction: Multidisciplinary team (MDT) meetings use precise prognostic factors to select treatment options for patients with prostate cancer. Comorbidity is judged subjectively. Recent publications favour the Charlson comorbidity score (CS) for the use in the management of prostate cancer. We assess the feasibility of using the CS by our MDT in planning the treatment of patients with prostate cancer.
Patients and methods: Patients from the histopathology database aged less than 75 years and with a diagnosis of localized prostate cancer between 1993 and 1995 were included in a notes audit. A second group consisted of patients recommended for curative treatment for localized prostate cancer by the local MDT in 2004. Data on comorbidity, prostatic malignancy and survival up to 10 years was collected. The prognostic accuracy of the CS was assessed for those patients offered radical treatment between 1993 and 1995.
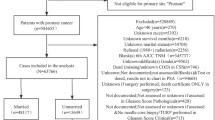
Results: Of 1043 patients initially assessed, 37 patients with localized prostate cancer were identified. Using Cox regression, we found the CS to be a statistically significant predictor of survival, following radical treatment for localized prostate cancer (P=0.005). Current practice in 2004 (56 patients) shows a mean (range) Charlson probability of 10-year survival for radical prostatectomy of 0.823 (0.592–0.923) and for radical radiotherapy of 0.653 (0.07–0.936).
Conclusions: Our results support the findings of recent research. We also found the CS easy to calculate and therefore feasible to use in our MDT setting. We propose the introduction of the Charlson score by prostate cancer MDTs to assess age and comorbidity.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 4 print issues and online access
$259.00 per year
only $64.75 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
The NHS Cancer Plan. DoH: London, 2000.
Wilson J, Clarke M, Ewings P, Graham J, MacDonagh R . The assessment of patient life-expectancy: how accurate are oncologists and urologists? BJU Int 2005; 95: 794–798.
Report from the working party on co-morbidity assessment in cancer – its role in the national core cancer dataset. www.nhsia.nhs.uk,04 Jul 2001.
Singh R, O'Brien TS . Comorbidity assessment in localized prostate cancer: a review of currently available techniques. Eur Urol 2004; 46: 28–41.
Froehner M, Koch R, Litz R, Oehlschlaeger S, Wirth MP . Which conditions contributing to the Charlson score predict survival after radical prostatectomy? J Urol 2004; 171 (Part 1): 697–699.
Froehner M, Koch R, Litz R, Heller A, Oehlschlaeger S, Wirth MP . Comparison of the American society of anesthesiologists physical status classification with the Charlson score as predictors of survival after radical prostatectomy. Urology 2003; 62: 698–701.
Charlson ME, Pompei P, Ales KL, MacKenzie CR . A new method of classifying prognostic comorbidity in longitudinal studies: development and validation. J Chron Dis 1987; 40: 373–383.
Charlson ME, Szatrowski TP, Peterson J, Gold J . Validation of a combined co-morbidity index. J Clin Epidemiol 1994; 47: 1245–1251.
Tewari A, Johnson CC, Divine G, Crawford ED, Gamito EJ, Demers R et al. Long-term survival probability in men with clinically localized prostate cancer: a case–control, propensity modeling study stratified by race, age, treatment and comorbidities. J Urol 2004; 171: 1513–1519.
Froehner M, Koch R, Litz R, Oehlschlaeger S, Wirth MP . Which conditions contributing to the Charlson score predict survival after radical prostatectomy? J Urol 2004; 171: 697–699.
Froehner M, Koch R, Litz R, Oehlschlaeger S, Hakenberg OW, Wirth MP . Feasibility and limitations of comorbidity measurement in patients undergoing radical prostatectomy. Eur J Urol 2005; 47: 190–195.
Post PN, Hansen BE, Kil PJ, Janssen-Heijnen ML, Coebergh JW . The independent prognostic value of comorbidity among men aged <75 years with localized prostate cancer: a population based study. BJU Int 2001; 87: 821–826.
Barry MJ, Albertsen PC, Bagshaw MA, Blute ML, Cox R, Middleton RG et al. Outcomes for men with clinically nonmetastatic prostate carcinoma managed with radical prostatectomy, external beam radiotherapy or expectant management: a retrospective analysis. Cancer 2001; 911: 2302–2314.
Albertsen PC, Fryback DG, Storer BE, Kolon TF, Fine J . The impact of co-morbidity on life expectancy among men with localized prostate cancer. J Urol 1996; 156: 127–132.
Holmberg L, Bill-Axelson A, Helgesen F, Salo JO, Folmerz P, Haggman M et al. Randomized trial comparing radical prostatectomy with watchful waiting in early prostate cancer. N Engl J Med 2002; 347: 781–789.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Kastner, C., Armitage, J., Kimble, A. et al. The Charlson comorbidity score: a superior comorbidity assessment tool for the prostate cancer multidisciplinary meeting. Prostate Cancer Prostatic Dis 9, 270–274 (2006). https://doi.org/10.1038/sj.pcan.4500889
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.pcan.4500889
Keywords
This article is cited by
-
Baseline serum folate, vitamin B12 and the risk of prostate and breast cancer using data from the Swedish AMORIS cohort
Cancer Causes & Control (2019)
-
Serum glucose, triglycerides, and cholesterol in relation to prostate cancer death in the Swedish AMORIS study
Cancer Causes & Control (2019)
-
Glucose, lipids and gamma-glutamyl transferase measured before prostate cancer diagnosis and secondly diagnosed primary tumours: a prospective study in the Swedish AMORIS cohort
BMC Cancer (2018)
-
Can pre-diagnostic serum levels of sodium and potassium predict prostate cancer survival?
BMC Cancer (2018)
-
Availability and feasibility of structured, routine collection of comorbidity data in a colorectal cancer multi-disciplinary team (MDT) setting
International Journal of Colorectal Disease (2018)