Abstract
Objective:
The incidence of acute neurologic events prior to discharge in neonates with congenital heart disease (CHD) was determined and peri-operative characteristics predictive of a neurologic event were identified.
Study design:
A retrospective chart review over 1 year was conducted of infants <1 month of age with a diagnosis of CHD. Outcomes were measured by the occurrence of an acute neurologic event defined as electroencephalogram (EEG)-proven seizure activity, significant hypertonia or hypotonia, or choreoathetosis prior to hospital discharge. Stepwise logistic regression identified variables most likely to be associated with an acute neurologic event.
Results:
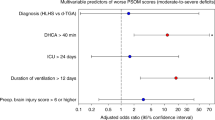
Surgical intervention occurred in 95 infants who were admitted with a diagnosis of CHD. The survival rate was 92%. Of the survivors, 16 (17%) had an acute neurologic event, with 19% of events occurring preoperatively. Factors associated with neurologic events included an elevated nucleated red blood cell (NRBC) count, an abnormal preoperative brain imaging study, and a 5-min Apgar score <7 (P<0.05).
Conclusions:
Neonates with CHD have a significant risk of neurologic events. Preoperative brain imaging, the 5-min Apgar score, and initial serum NRBC counts may identify infants at highest risk for central nervous system injury.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Ferry PC . Neurologic sequelae of cardiac surgery in children. AJDC 1987; 41: 309–312.
Ferry PC . Neurologic sequelae of open-heart surgery in children. AJDC 1990; 144: 369–373.
Bellinger DC, Wypij D, duPlessis A, Rappaport LA, Jonas RA, Wernovsky G et al. Neurodevelopmental status at eight years in children with dextro-transposition of the great arteries: The Boston Circulatory Arrest Trial. J Thorac Cardiovasc Surg 2003; 126: 1385–1396.
Limperopoulos C, Majnemer A, Shevell MI, Rohlicek C, Rosenblatt B, Tchervenkov C et al. Predictors of developmental disabilities after open heart surgery in young children with congenital heart defects. J Pediatr 2002; 141: 51–58.
Miller G, Eggli KD, Contant C, Baylen BG, Myers JL . Postoperative neurologic complications after open heart surgery in young infants. Arch Pediatr Adolesc Med 1995; 149: 764–768.
Clancy RR, McGaurn SA, Wernovsky G, Gaynor JW, Spray TL, Norwood WI et al. Risk of seizures in survivors of newborn heart surgery using deep hypothermic circulatory arrest. Pediatrics 2003; 111: 592–601.
Mahle WT, Tavani F, Zimmerman R, Nicolson S, Galli KK, Gaynor JW et al. An MRI study of neurological injury before and after congenital heart surgery. Circulation 2002; 106: I109–I114.
Limperopoulos C, Majnemer A, Shevell MI, Rosenblatt B, Rohlicek C, Tchervenkov C et al. Neurologic status of newborns with congenital heart defects before open heart surgery. Pediatrics 1999; 103: 402–408.
Limperopoulos C, Majnemer A, Shwevell MI, Rosenblatt B, Rohlicek C, Tchervenkov C et al. Neurodevelopmental status of newborns and infants with congenital heart defects before and after open heart surgery. J Pediatr 2000; 137: 638–645.
Glauser TA, Rorke LB, Weinberg PM, Clancy RR . Congenital brain anomalies associated with the hypoplastic left heart syndrome. Pediatrics 1990; 85: 984–990.
Van Houten JP, Rothman A, Bejar R . High incidence of cranial ultrasound abnormalities in full-term infants with congenital heart disease. Am J Perinatol 1996; 13: 47–53.
Dexter F, Hindman B . Theoretical analysis of cerebral venous blood hemoglobin oxygen saturation as an index of cerebral oxygenation during hypothermic cardiopulmonary bypass. Anesthesiology 1995; 83: 405–412.
Wypij D, Newburger JW, Rappaport LA, duPlessis AJ, Jonas RA, Wernovsky G et al. The effect of duration of deep hypothermic circulatory arrest in infant heart surgery on late neurodevelopment: The Boston Circulatory Arrest Trial. J Thorac Cardiovasc Surg 2003; 126: 1397–1403.
Bellinger DC, Wypij D, Kuban KC, Rappaport LA, Hickey PR, Wernovsky G et al. Developmental and neurological status of children at 4 years of age after heart surgery with hypothermic circulatory arrest or low-flow cardiopulmonary bypass. Circulation 1999; 100: 526–532.
Steinberg JB, Kapelanski DP, Olson JD, Weiler JM . Cytokine and complement levels in patients undergoing cardiopulmonary bypass. J Thorac Cardiovasc Surg 1993; 106: 1008–1016.
Newburger JW, Jonas RA, Wernovsky G, Wypij D, Hickey PR, Kuban KC et al. A comparison of the perioperative neurologic effects of hypothermic circulatory arrest versus low-flow cardiopulmonary bypass in infant heart surgery. N Engl J Med 1993; 329: 1057–1064.
Mahle WT, Clancy RR, McGaurn SP, Goin JE, Clark BJ . Impact of prenatal diagnosis on survival and early neurologic morbidity in neonates with the hypoplastic left heart syndrome. Pediatrics 2001; 107: 1277–1282.
Trittenwein G, Nardi A, Pansi H, Golej J, Burda G, Hermon M et al. Early postoperative prediction of cerebral damage after pediatric cardiac surgery. Annal Thorac Surg 2003; 76: 576–580.
Hamrick SE, Gremmels DB, Keet CA, Leonard CH, Connell JK, Hawgood S et al. Neurodevelopmental outcome of infants supported with extracorporeal membrane oxygenation after cardiac surgery. Pediatrics 2003; 111: e671–e675.
Richardson DK, Gray JE, McCormick MC, Workman K, Goldmann DA . Score for Neonatal Acute Physiology: a physiologic severity index for neonatal intensive care. Pediatrics 1993; 91: 617–623.
Bellinger DC, Jonas R, Rappaport L, Wypij D, Wernovsky G, Kuban KC et al. Developmental and neurologic status of children after heart surgery with hypothermic circulatory arrest or low-flow cardiopulmonary bypass. N Engl J Med 1995; 332: 549–555.
Korst LM, Phelan JP, Ahn MO, Martin GI . Nucleated red blood cells: an update on the marker for fetal asphyxia. Am J Obstet Gynecol 1996; 175: 843–846.
Buonocore G, Perrone S, Gioia D, Gatti MG, Massafra C, Agosta R et al. Nucleated red blood cell count at birth as an index of perinatal damage. Am J Obstet Gynecol 1999; 181: 1500–1505.
Hamrick SE, Miller SP, Newton NR, Parer JT, Ferriero DM, Barkovich AJ et al. Nucleated red blood cell counts: not associated with brain injury or outcome. Pediatr Neurol 2003; 29: 278–283.
Miller SP, McQuillen PS, Vigneron DB, Glidden DV, Barkovich AJ, Ferriero DM et al. Preoperative brain injury in newborns with transposition of the great arteries. Ann Thorac Surg 2004; 77: 1698–1706.
Acknowledgements
We thank William E Benitz, MD for his assistance with the statistical analysis and Stephen J Roth, MD for his critical review of the manuscript. Dr Chock received support from the Neonatal and Developmental Biology Training Grant at Stanford University.
Author information
Authors and Affiliations
Corresponding author
Additional information
Supplementary Information accompanies the paper on the Journal of Perinatology website (http://www.nature.com/jp)
Supplementary information
Rights and permissions
About this article
Cite this article
Chock, V., Reddy, V., Bernstein, D. et al. Neurologic events in neonates treated surgically for congenital heart disease. J Perinatol 26, 237–242 (2006). https://doi.org/10.1038/sj.jp.7211459
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/sj.jp.7211459
Keywords
This article is cited by
-
Evaluation of Seizure Risk in Infants After Cardiopulmonary Bypass in the Absence of Deep Hypothermic Cardiac Arrest
Neurocritical Care (2022)
-
Electroencephalographic Monitoring in the Pediatric Intensive Care Unit
Current Neurology and Neuroscience Reports (2013)
-
Post pump chorea in a 77-year-old male
Neurological Sciences (2011)