Abstract
Objective:
Delayed cord clamping has been shown to decrease the need for transfusion in preterm neonates, but may delay resuscitation. The aim of this study was to determine whether umbilical cord milking compared with immediate cord clamping in extremely preterm deliveries reduces the need for neonatal red blood cell transfusion.
Study design:
Women admitted to a tertiary care center and expected to deliver between 24 to 28 completed weeks of gestation were randomized to cord milking before clamping or immediate cord clamping. The primary outcome was the risk of neonatal transfusion, reported as risk ratio (RR) and 95% confidence interval (CI).
Result:
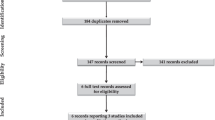
Of 113 women who were enrolled and randomized, 56 were assigned to cord milking with 36 remaining eligible and completing the study and 57 were assigned to the control group with 39 remaining eligible and completing the study. Albeit not statistically significant, neonates in the cord milking group were less likely to require transfusion compared with those in the control group (RR: 0.86; 95% CI: 0.73 to 1.0). Neonates whose cords were milked had higher hematocrits at birth (P=0.004) and were less likely to develop an intraventricular hemorrhage (P=0.0195).
Conclusion:
Milking the umbilical cord of a preterm neonate is an easy intervention with the potential to improve perinatal outcomes. Our results suggest that milking of the cord increases the neonate’s initial hematocrit and may lessen the need for transfusion in the neonatal period. The observed reduction in the incidence of intraventricular hemorrhage may have important long-term implications that warrant further study.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout
Similar content being viewed by others
References
Hosono S, Ohno T, Kimoto H, Shimizu M, Harada K . Morbidity and mortality of infants born at the threshold of viability: ten year’s experience in a single neonatal intensive care unit, 1991-2000. Pediatr Int 2006; 48: 33–39.
Stockman JA, Graeber JE, Clark DA, McClellan K, Garcia JF, Kavey RE . Anemia of prematurity: determinants of the erythropoietin response. J Pediatr. 1984; 105: 786–792.
Ohls RK . The use of erythropoietin in neonates. Clin Perinatol. 2000; 27: 681–696.
Haiden N, Schwindt J, Cardona F, Berger A, Klebermass K, Wald M et al. Effects of a combined therapy of erythropoietin, iron, folate, and vitamin B12 on the transfusion requirements of extremely low birth weight infants. Pediatrics 2006; 118: 2004–2013.
Ross MP, Christensen RD, Rothstein G, Koenig JM, Simmons MA, Noble NA et al. A randomized trial to develop criteria for administering erythrocyte transfusions to anemic preterm infants 1 to 3 months of age. J Perinatol 1989; 9: 246–253.
Padbury JF . Placental Transfusion In Rudolph’s Pediatrics. McGraw Hill Medical: New York, NY, USA (2003) pp 163–164.
Rabe H, Reynolds G, Diaz-Rossello J . A systematic review and meta-analysis of a brief delay in clamping the umbilical cord of preterm infants. Neonatology 2008; 93: 138–144.
Rabe H, Diaz-Rossello JL, Duley L, Dowswell T . Effect of timing of umbilical cord clamping and other strategies to influence placental transfusion at preterm birth on maternal and infant outcomes. Cochrane Database Syst Rev 2012; ((8)).
Aladagandy N, McHugh S, Aitchison TC, Wardrop CA, Holland B . Infant’s blood volume in a controlled trial of placental transfusion at preterm delivery. Pediatrics 2006; 117: 93–98.
Strauss RG, Mock DM, Johnson KJ, Cress GA, Burmeister LF, Zimmerman MB et al. A randomized clinical trial comparing immediate versus delayed clamping of the umbilical cord in preterm infants: short-term clinical and laboratory endpoints. Transfusion 2008; 48: 658–665.
Oh W, Fanaroff AA, Carlo WA, Donovan EF, McDonald SA, Poole WK et al. Effects of delayed cord clamping in very-low-birth-weight infants. J Perinatol 2011; 31 (Suppl 1): S68–S71.
Kinmond S, Aitchison TC, Holland BM, Jones JG, Turner TL, Wardrop CA . Umbilical cord clamping and preterm infants: a randomized trial. BMJ 1993; 306: 172–175.
Kugelman A, Borenstein-Levin L, Riskin A, Chistyakov I, Ohel G, Gonen R et al. Immediate versus delayed umbilical cord clamping in premature neonates born <35 weeks: a prospective, randomized, controlled study. Am J Perinatol 2007; 24 (5): 307–315.
Mercer JS, Vohr BR, McGrath MM, Padbury JF, Wallach M, Oh W . Delayed cord clamping in very preterm infants reduces the incidence of intraventricular hemorrhage and late-onset sepsis: a randomized, controlled trial. Pediatrics 2006; 117: 1235–1242.
Rabe H, Wacker A, Hulskamp G, Hornig-Franz I, Schulze-Everding A, Harms E et al. A randomized controlled trial of delayed cord clamping in very low birth weight preterm infants. Eur J Pediatr 2000; 159: 775–777.
Utlee CA, Van der Deure J, Swart J, Lasham C, van Baar AL . Delayed cord clamping in preterm infants delivered at 34-36 weeks’ gestation: a randomized controlled trial. Arch Dis Child Fetal Neonatal Ed 2008; 93: F20–F23.
Rabe H, Jewison A, Alvarez RF, Crook D, Stilton D, Bradley R et al. Milking compared with delayed cord clamping to increase placental transfusion in preterm neonates. Obstet Gynecol 2011; 117: 205–211.
Erickson-Owens DA, Mercer JS, Oh W . Umbilical cord milking in term infants delivered by cesarean section: a randomized controlled trial. J Perinatol 2012; 32: 580–584.
American College of Obstetricians and Gynecologists. Committee Opinion No. 543:Timing of umbilical cord clamping after birth. Obstet Gynecol 2012; 120: 1522–1526.
Hosono S, Mugishima H, Fujita H, Hosono A, Minato M, Okada T et al. Umbilical cord milking reduces the need for red cell transfusions and improves neonatal adaptation in infants born less than 29 weeks’ gestation: a randomized control trial. Arch Dis Child Fetal Neonatal Ed 2007; 10: 1136.
Hosono S, Mugishima H, Fujita H, Hosono A, Okada T, Takahashi S et al. Blood pressure and urine output during the first 120 h of life in infants born at less than 29 weeks’ gestation related to umbilical cord milking. Arch Dis Child Fetal Neonatal Ed 2009; 94: F328–F331.
Takami T, Suganami Y, Sunohara D, Kondo A, Mizukaki N, Fujioka T et al. Umbilical cord milking stabilizes cerebral oxygenation and perfusion in infants born before 29 weeks gestation. J Pediatr. 2012; 161 (4): 742–747.
Pocock S . Group sequential methods in the design and analysis of clinical trials. Biometrika 1977; 62: 191–199.
Acknowledgements
This work was conducted with support from Harvard Catalyst. The Harvard Clinical and Translational Science Center (National Center for Research Resources and the National Center for Advancing Translational Sciences, National Institutes of Health Award 8UL1TR000170-05 and financial contributions from the Harvard University and its affiliated academic health-care centers.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Additional information
This study was previously presented at the Society for Maternal Fetal Medicine’s 31st Annual Meeting, held in San Francisco, CA (‘The Efficacy of Umbilical Cord Milking on the Reduction of Red Blood Cell Transfusion Rates in Infants Born Between 24 and 28 6/7 Weeks Gestation - A Randomized Controlled Trial,’ Abstract ID: 221362) on 7–12 February 2011.
Supplementary Information accompanies the paper on the Journal of Perinatology website
Supplementary information
Rights and permissions
About this article
Cite this article
March, M., Hacker, M., Parson, A. et al. The effects of umbilical cord milking in extremely preterm infants: a randomized controlled trial. J Perinatol 33, 763–767 (2013). https://doi.org/10.1038/jp.2013.70
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2013.70
Keywords
This article is cited by
-
The hematological impact of umbilical cord milking versus delayed cord clamping in premature neonates: a randomized controlled trial
BMC Pregnancy and Childbirth (2022)
-
Placental transfusion during neonatal resuscitation in an asphyxiated preterm model
Pediatric Research (2022)
-
Neurodevelopmental outcomes of very preterm infants who received cord milking at birth: a randomized controlled trial
European Journal of Pediatrics (2022)
-
Short-term efficacy of umbilical cord milking in preterm infants: systematic review and meta-analysis
Pediatric Research (2021)
-
Antenatal and perinatal factors influencing neonatal blood pressure: a systematic review
Journal of Perinatology (2021)