Abstract
Objective:
To evaluate the effectiveness of an interactive computerized order set with decision support (ICOS-DS) in preventing medication errors in neonatal late-onset sepsis (LOS).
Study Design:
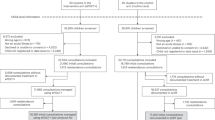
Prospective, controlled comparison of error rates in antibiotic orders for neonates admitted to the Medical University of South Carolina neonatal intensive care unit with suspected LOS (after postnatal day of life 3) prior to (n=153) and after (n=146) implementation of the ICOS-DS. Antibiotic orders were independently evaluated by two pharmacists for prescribing errors, potential errors and omissions. Prescribing errors included>10% overdoses or underdoses, inappropriate route, schedule or antibiotic, drug–drug or drug–disease interactions, and incorrect patient demographics. Potential errors included misspelled drugs, leading decimals, trailing zeroes, impractical doses and error-prone abbreviations. Multiple errors and omissions in an order were counted individually.
Results:
Overall error rate per order decreased from 1.7 to 0.8 (P<0.001) and potential error rate from 1.0 to 0.06 (P<0.001). The reduction in omission error rate per order from 0.2 to 0.1 was not significant (P=0.17). The prescribing error rate per order increased from 0.4 to 0.7 (P=0.03) because of the use of incorrect patient weights (P<0.001). Renal dysfunction was significantly associated with an increased risk of prescribing errors (odds ratio=3.7, P=0.01) which was not significantly different for handwritten versus ICOS-DS orders (P=0.15).
Conclusions:
The ICOS-DS significantly improved the quality of neonatal LOS antibiotic orders although the use of incorrect patient weights was increased. In both groups, orders for patients with renal dysfunction were at risk for prescribing errors. Further evaluation of interventions to promote medication safety for this population is needed.
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$259.00 per year
only $21.58 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout



Similar content being viewed by others
References
The National Coordinating Council for Medication Error Reporting and Prevention. Definition of medication errors http://www.nccmerp.org/ Accessed August 14 2013.
Kaushal R, Bates DW, Landrigan C, McKenna KJ, Clapp MD, Federico F et al. Medication errors and adverse drug events in pediatric patients. JAMA 2001; 285 (16): 2114–2120.
Gonzales K . Medication administration errors and the pediatric population: a systematic search of the literature. J Pediatr Nursing 2010; 25: 555–565.
Ghaleb MA, Barber N, Franklin BD, Yeung VW, Khaki ZF, Wong IC et al. Systematic review of medication errors in pediatric patients. Ann Pharmacother 2006; 40: 1766–1776.
Chedoe I, Molendijk HA, Dittrich ST, Jansman FG, Harting JW, Brouwers JR et al. Incidence and nature of medication errors in neonatal intensive care with strategies to improve safety: A review of the current literature. Drug Safety 2007; 30 (6): 503–513.
Snijders C, van Lingen RA, Fetter WPF . Incidents and errors in neonatal intensive care: review of the literature. Arch Dis Child Fetal Neonatal Ed 2007; 92: 391–398.
Ross LM, Wallace J, Paton JY . Medication errors in a paediatric teaching hospital in the UK: five years operational experience. Arch Dis Child 2000; 83: 492–497.
Holdsworth MT, Fichtl RE, Behta M, Raisch DW, Mendez-Rico E, Adams A et al. Incidence and impact of adverse drug events in pediatric inpatients. Arch Pediatr Adolesc Med 2003; 157 (1): 60–65.
Di Pentima MC, Chan S, Eppes SC, Klein JD . Antimicrobial prescription errors in hospitalized children: Role of antimicrobial stewardship program in detection and intervention. Clin Pediatr 2009; 48 (5): 505–512.
Bissinger RL, Mueller M, Cox TH, Cahill J, Garner SS, Irving MG et al. Antibiotic timing in neonates with suspected hospital-acquired infections. Advances in Neonatal Care 2013; 13 (1): 22–28.
Taketomo CK . Pediatric Dosage Handbook 14th ed.Lexi-Comp, Inc.: Hudson, Ohio, 2007.
Lexi-Comp Online™ Pediatric Lexi-Drugs Online™ 2007. Lexi-Comp, Inc.: Hudson, Ohio.
Liang KY, Zeger SL . Longitudinal data analysis using generalized linear models. Biometrika 1986; 73: 13–22.
Zeger SL, Liang KY, Albert PS . Models for longitudinal data: a generalized estimating equation approach. Biometrics 1988; 44: 1049–1060.
Cochran WG . Sampling Techniques 3rd EditionJohn Wiley & Sons: New York, 1977.
Rao JNK, Scott AJ . The analysis of categorical data from complex sample surveys: chi-squared tests for goodness of fit and independence in two-way tables. J Am Stat Assoc 1981; 76: 221–229.
Cordero L, Kuehn L, Kumar RR, Mekhjian HS . Impact of computerized physician order entry on clinical practice in a newborn intensive care unit. J Perinatol 2004; 24 (2): 88–93.
Kazemi A, Ellenius J, Pourasghar F, Tofighi S, Salehi A, Amanati A et al. The effect of computerized physician order entry and decision support system on medication errors in the neonatal ward: Experiences from an Iranian teaching hospital. J Med Syst 2011; 35: 25–37.
Nightingale PG, Adu D, Richards NT, Peters M . Implementation of rules based computerized bedside prescribing and administration: intervention study. BMJ 2000; 320: 750–753.
Raju TNK, Suresh G, Higgins RD . Patient safety in the context of neonatal intensive care: Research and educational opportunities. Pediatr Res 2011; 70: 109–115.
Han YY, Carcillo JA, Venkataraman ST, Clark RS, Watson RS, Nguyen TC et al. Unexpected increased mortality after implementation of a commercially sold computerized physician order entry system. Pediatrics 2005; 116: 1506–1512.
Teufel RJ, Kazley AS, Basco WT . Early adopters of computerized physician order entry in hospitals that care for children: A picture of U.S. health care shortly after the Institute of Medicine reports on quality. Clin Pediatr 2009; 48: 389–396.
DesRoches CM, Charles D, Furukawa MF, Joshi MS, Kralovec P, Mostashari F et al. Adoption of electronic health records grows rapidly, but fewer than half of U.S. hospitals had at least a basic system in 2012. Health Affairs 2013; 32: 1478–1485.
Acknowledgements
We would like to acknowledge Lizbeth Hansen, Pharm.D., for her tireless efforts with data collection and entry.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no conflict of interest.
Rights and permissions
About this article
Cite this article
Garner, S., Cox, T., Hill, E. et al. Prospective, controlled study of an intervention to reduce errors in neonatal antibiotic orders. J Perinatol 35, 631–635 (2015). https://doi.org/10.1038/jp.2015.20
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/jp.2015.20
This article is cited by
-
Interventions to Reduce Pediatric Prescribing Errors in Professional Healthcare Settings: A Systematic Review of the Last Decade
Pediatric Drugs (2021)
-
Effect of Electronic Prescribing Strategies on Medication Error and Harm in Hospital: a Systematic Review and Meta-analysis
Journal of General Internal Medicine (2019)