Abstract
Defective S-phase checkpoint activation results in an inability to downregulate DNA replication following genotoxic insult such as exposure to ionizing radiation. This 'radioresistant DNA synthesis' (RDS) is a phenotypic hallmark of ataxia–telangiectasia1, a cancer-prone disorder caused by mutations in ATM2. The mismatch repair system principally corrects nucleotide mismatches that arise during replication3. Here we show that the mismatch repair system is required for activation of the S-phase checkpoint in response to ionizing radiation. Cells deficient in mismatch repair proteins showed RDS, and restoration of mismatch repair function restored normal S-phase checkpoint function. Catalytic activation of ATM and ATM-mediated phosphorylation of the protein NBS1 (also called nibrin) occurred independently of mismatch repair. However, ATM-dependent phosphorylation and activation of the checkpoint kinase CHK2 and subsequent degradation of its downstream target, CDC25A, was abrogated in cells lacking mismatch repair. In vitro and in vivo approaches both show that MSH2 binds to CHK2 and that MLH1 associates with ATM. These findings indicate that the mismatch repair complex formed at the sites of DNA damage facilitates the phosphorylation of CHK2 by ATM, and that defects in this mechanism form the molecular basis for the RDS observed in cells deficient in mismatch repair.
Similar content being viewed by others
Main
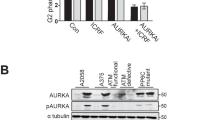
Several lines of evidence indicate that, in addition to repairing replicative errors within the genome, the mismatch repair system is a component in signaling events that activate cell-cycle checkpoints or apoptosis4,5,6. Cells deficient in mismatch repair have altered G2–M arrest in response to ionizing radiation7. We examined human tumor lines impaired in expression of MSH2 (HEC59) or MLH1 (HCT-116) for inhibition of DNA synthesis after γ-irradiation to evaluate a potential role for the mismatch repair system in establishing the S-phase checkpoint. In normal human fibroblasts, exposure to ionizing radiation caused a marked, dose-dependent decrease in DNA synthesis (Fig. 1). As expected, ataxia–telangiectasia fibroblasts showed only a minimal (<15%) inhibition of DNA synthesis after irradiation, and HCT-116 and HEC59 cells had a negligible decrease in DNA synthesis after irradiation (Fig. 1a). The small decreases in DNA synthesis in ataxia–telangiectasia fibroblasts, HCT-116 cells and HEC59 cells were similar regardless of the dose of ionizing radiation (Fig. 1b).
a, The normal human fibroblast line GM06037H (NHF), ataxia–telangiectasia fibroblast line GM05849C (A–T), and the mismatch repair–deficient tumor lines HCT-116 and HEC59 were exposed to 5 Gy of ionizing radiation and DNA synthesis measured at indicated time points after irradiation. b, Cells were exposed to indicated doses of ionizing radiation (IR), and DNA synthesis was measured 15 min after irradiation. c, Normal human fibroblasts (NHF), ataxia–telangiectasia fibroblasts (A–T) and the indicated mismatch repair–deficient cell lines were irradiated (4 Gy), and DNA synthesis was measured 30 min after irradiation. d, Mismatch repair–deficient (HCT116+ch2, HEC59, RKO) and isogenic mismatch repair–proficient (HCT-116+ch3, HEC59+ch2, RKO/aza50) cell lines were irradiated (4 Gy), and DNA synthesis was measured 15 min after irradiation. e, MC5 (Mlh1+/+), MC2 (Mlh1−/−) and B4-5 (Mlh1−/− ectopically expressing MLH1) MEFs were irradiated (5 Gy) and then assayed for DNA synthesis. In all cases, data represent the mean ± s.d. of 3–5 experiments.
We measured the amount of radiolabeled thymidine incorporated in a panel of other human tumor lines defective in either MLH1 (RKO, SW48) or MSH2 (LoVo) after exposure to ionizing radiation (4 Gy; Fig. 1c). Normal fibroblasts incorporated 57.4 ± 7.2% (s.d.; n = 4) as much radiolabeled thymidine as did unirradiated controls, indicating activation of the S-phase checkpoint. In contrast, we observed significantly greater (P ≤ 0.05) DNA synthesis after irradiation in ataxia–telangiectasia fibroblasts (86.9 ± 7.9%, n = 3), LoVo cells (91.2 ± 16.9%, n = 4), SW-48 cells (95.4 ± 17.8%, n = 4) and RKO cells (77.9 ± 6.0%, n = 3) compared with normal fibroblasts.
Next, we examined DNA synthesis in HCT-116 and HEC59 cells expressing MLH1 and MSH2, respectively. DNA synthesis after exposure to ionizing radiation was significantly lower (P < 0.01) in these cells than in isogenic parental lines deficient in mismatch repair (Fig. 1d). It has been previously shown that treatment with 5-aza-2′-deoxycytidine restores MLH1 expression in RKO cells8, and we found that re-expression of MLH1 in these cells also markedly reduced the rate of DNA synthesis after exposure to ionizing radiation.
We also measured DNA synthesis in Mlh1−/− and Mlh1+/+ mouse embryonic fibroblasts (MEFs) and in Mlh1−/− MEFs that express recombinant MLH1 (Fig. 1e). Thymidine incorporation after exposure to ionizing radiation in Mlh1+/+ MEFs (n = 3) was 58.3 ± 1.7% that of unirradiated cells, similar to the proportion observed in irradiated normal human fibroblasts, but in Mlh1−/− MEFs (n = 3), thymidine incorporation was 102.4 ± 4.9% that of unirradiated cells, indicative of RDS. Expression of recombinant MLH1 partially complemented the RDS defect in Mlh1−/− MEFs (76.8 ± 4.5%, n = 3). Taken together, these findings indicate that RDS in cells deficient in mismatch repair is directly attributable to loss of mismatch repair.
The S-phase checkpoint is activated through two distinct ATM-dependent pathways in response to ionizing radiation. One involves phosphorylation of the DNA repair protein NBS1 (ref. 9–11); the second involves phosphorylation and activation of the checkpoint kinase CHK2 leading to destruction of the phosphatase CDC25A12,13. Although the mechanism(s) by which events downstream of NBS1 phosphorylation activate the S-phase checkpoint remain unresolved, it is known that loss of CDC25A activity blocks entry into S phase14,15.
We observed increased ATM catalytic activity in response to ionizing radiation in mismatch repair–proficient HCT-116+ch3 cells and mismatch repair–deficient HCT-116+ch2 cells, as judged by in vitro kinase assays (Fig. 2a). We confirmed kinase reaction specificity by examining ATM activity in both normal and ataxia–telangiectasia fibroblasts (Fig 2a). Consistent with ATM activation, we also observed increased c-ABL kinase activity16 in HCT-116+ch3 and HCT-116+ch2 cells after irradiation (Fig. 2b). We confirmed the ATM dependency of c-ABL activation by testing c-ABL activity in irradiated normal and ataxia–telangiectasia fibroblasts (Fig. 2b). Irradiation also resulted in a shift in electrophoretic mobility of NBS1 in HCT-116+ch3 and HCT-116+ch2 cells (Fig. 2c), consistent with phosphorylation induced by ionizing radiation9. We confirmed this interpretation using an antibody specific for the ATM-phosphorylated form of NBS1 (Fig. 2c). We also observed that NBS1 localized to nuclear foci17 in both HCT-116+ch3 and HCT-116+ch2 cells (Fig. 2d). In all cases, we obtained similar results with mismatch repair–proficient HEC59+2 cells and mismatch repair–deficient HEC59 cells (data not shown). Taken together, these findings are consistent with irradiation-induced activation of ATM and ATM-dependent phosphorylation of NBS1, and suggest that RDS in cells deficient in mismatch repair probably does not stem from abrogation of the ATM→NBS1 pathway.
a, Mismatch repair–deficient cells (HCT116+ch2; lanes 1,2), isogenic mismatch repair–proficient cells (HCT-116+ch3; lanes 3,4), normal human fibroblasts (NHF; GM06037H; lanes 5,6) and ataxia–telangiectasia fibroblasts (A–T; GM05849C; lanes 7,8) were mock-treated (−IR) or exposed to ionizing radiation (5 Gy; +IR), and ATM kinase activity was then measured by an in vitro kinase reaction using recombinant c-ABL (GST–HP–ABL) as substrate. Reaction mixtures were subjected to SDS–PAGE and autoradiography (top). Immunocomplexes were also subjected to immunoblot analysis with antibody against ATM (bottom). Relative intensity of radiolabeled substrate is indicated. b, Cell lines described in a were mock-treated (−IR) or irradiated (5 Gy; +IR), and c-ABL activity was determined by in vitro kinase assay using GST–CTD as the substrate (top). Immunocomplexes were also subjected to immunoblot analysis with antibody against ABL (bottom). c, HCT-116+ch2 (lanes 1,2) and HCT-116+ch3 (lanes 3,4) cells were mock-treated (−IR) or irradiated (5 Gy; +IR), and 1 hr later extracts were formed and subjected to immunoblot with antibody against (total) NBS1 (top) or immunoblotted with antibody against phospho-specific (Ser343) NBS1 (bottom). d, HCT-116+ch2 and HCT-116+ch3 were either mock-treated (−IR) or irradiated with 5 Gy (+IR), and 2 hr after irradiation, cells were fixed and stained with antibody against NBS1 followed by secondary antibody labeled with fluorescein isothiocyanate. Counterstaining with DAPI indicated that these foci were intranuclear (data not shown).
The kinase CHK2 has a key role in triggering establishment of the S-phase checkpoint by phosphorylating CDC25A and targeting this phosphatase for degradation12. We probed lysates from control and irradiated mismatch repair–deficient (HCT-116+ch2 and HEC59) cells and mismatch repair–proficient (HCT-116+ch3 and HEC59+ch2) cells with a phospho-specific antibody (Thr68) that recognizes ATM-phosphorylated CHK2 (ref. 18). HCT-116+ch3 and HEC59+ch2 cells showed Thr68 phosphorylation in response to ionizing radiation, but HCT-116+ch2 and HEC59 cells did not (Fig. 3a). Analysis of CHK2 kinase activity in irradiated HCT-116+ch2 and HCT-116+ch3 confirmed that activation of CHK2 after irradiation was dependent on mismatch repair (Fig. 3b). We noted a reduction of approximately 71% in CHK2 activity when this kinase was immunoprecipitated in the presence of competing peptide (Fig. 3b), confirming the specificity of the observed catalytic activity.
a, Mismatch repair–deficient (lanes 1,2,5,6) and isogenic mismatch repair–proficient (lanes 3,4,7,8) cells were either mock-treated (−IR) or irradiated (5 Gy; +IR), and 1 h later, lysates were formed and subjected to immunoblot analysis with antibodies against phospho-specific (Thr68) CHK2 (top) or total CHK2 (bottom). b, Irradiation-induced (5 Gy) activation of CHK2 catalytic activity in HCT-116+ch2 (lanes 1,2) and HCT-116+ch3 (lanes 3–5) was assessed by in vitro kinase assay using GST–CDC25A fusion protein as substrate. Where indicated (lane 5), CHK2 immunoprecipitation was done in the presence of competing peptide to confirm specificity. Reaction products were resolved by SDS–PAGE followed by autoradiography (top). Immunocomplexes were also subjected to immunoblot analysis with antibody against CHK2 (bottom). c, Irradiation-induced (5 Gy) activation of CHK2 catalytic activity in mismatch repair–deficient HEC59 (lanes 1,2) and mismatch repair–proficient HEC59+ch2 (lanes 3,4) was assessed by in vitro kinase assay. d, Mismatch repair–deficient (lanes 1,2,5,6) and isogenic mismatch repair–proficient (lanes 3,4,7,8) cells were either mock-treated (−IR) or irradiated (5 Gy; +IR), and lysates were subjected to immunoblot analysis with antibodies against CDC25A (top) or tubulin (bottom) to confirm equivalent loading.
We also observed mismatch repair–dependent defects in irradiation-induced activation of CHK2 in HEC59 cells (Fig. 3c). Immunoblot analysis of CDC25A levels indicated that exposure to ionizing radiation did not induce degradation of CDC25A in HEC59 cells, but we did observe irradiation-induced degradation of CDC25A in HEC59+ch2 cells (Fig 3d). We also observed defective phosphorylation of CHK2 and degradation of CDC25A in irradiated Mlh1−/− MEFs (data not shown). These results clearly indicate that activation of CHK2 and subsequent degradation of CDC25A in response to ionizing radiation are dependent on mismatch repair.
Collectively, these data suggest that RDS in cells deficient in mismatch repair is not linked to defects in the ATM→NBS1 pathway but rather to abrogation of the ATM→CHK2→CDC25A pathway. Deficiency in either ATM or NBS1 renders mammalian cells radiosensitive19, but deficiency in mismatch repair does not7,20. Thus, if the aforementioned radiosensitivity stems from defective activation of the S-phase checkpoint, then NBS1-dependent mechanisms would be more important in protecting cells from the cytotoxic effects of ionizing radiation than activation of the ATM→CHK2→CDC25A pathway.
We examined interactions between MLH1 or MSH2 and CHK2 to gain a mechanistic understanding of the role of the mismatch repair system in activating the CHK2 kinase. We incubated purified glutathione S-transferase (GST)–CHK2 fusion protein immobilized on glutathione-agarose beads with lysates prepared from unirradiated and irradiated HEC59 and HEC59+ch2 cells. Immunoblotting of bound material showed that MSH2 was associated with GST–CHK2, which was enhanced in extracts from irradiated cells (Fig. 4a). Under these conditions, GST alone did not bind MSH2, and GST–CHK2 did not bind MLH1 (data not shown). When CHK2 was immunoprecipitated from HEC59+ch2 cell extracts, we detected co-precipitation of MSH2 with CHK2, and this association was greater in irradiated cell extracts (Fig. 4b). Co-incubation with competing peptide greatly reduced precipitation of both CHK2 and MSH2 (Fig 4b), indicating the specificity of the observed interaction.
a, Lysates prepared from irradiated (5 Gy; +IR) and mock-treated (−IR) HEC59 (lanes 1,2) and HEC59+ch2 (lanes 3,4) cells were incubated with GST–CHK2 bound to glutathione-agarose beads. After extensive washing, bound material was probed by immunoblotting with antibodies against MSH2 (top) or CHK2 (bottom). b, CHK2 was immunoprecipitated from extracts prepared from irradiated (5 Gy; +IR) and mock-treated (−IR) HEC59 (lanes 1,2) or HEC59+ch2 (lanes 3–5) cells and analyzed by immunoblotting for co-precipitation of MSH2 (top) or CHK2 (bottom). CHK2 immunoprecipitation was done in the presence of competing peptide (lane 5) to confirm specificity of immunoprecipitation. c, ATM was immunoprecipitated from mock-treated (−IR) and irradiated (5 Gy; +IR) HCT-116+ch2 (lanes 1,2) and HCT-116+ch3 (lanes 3,4) cells and analyzed for co-precipitation of MLH1 (top) or ATM (bottom). d, ATM immunoprecipitates from extracts of mock-treated (−IR) and irradiated (5 Gy; +IR) ataxia–telangiectasia fibroblasts (A–T; lanes 1,2) and normal human fibroblasts (NHF; lanes 3,4) were analyzed for the co-precipitation of MLH1 (top) or ATM (bottom).
ATM immunoprecipitates from HCT-116+ch3 extracts showed detectable levels of co-precipitating MLH1, but we observed greater association between these proteins after ionizing radiation (Fig. 4c). This finding suggests that ATM–MLH1 association is regulated by DNA damage. Enhanced co-precipitation of ATM and MLH1 in extracts from irradiated normal fibroblasts but not from irradiated ataxia–telangiectasia fibroblasts (Fig. 4d) confirmed the specificity of these experiments. Although this approach does not allow us to determine whether these interactions are direct or indirect, the results indicate that MSH2 interacts with CHK2 and MLH1 interacts with ATM, and that these interactions are enhanced in response to DNA damage.
Exposure to ionizing radiation results in a variety of DNA lesions, including single- and double-strand breaks. Although we are unsure of the exact nature of the damage that triggers ATM-dependent activation of CHK2, irradiation-induced oxidation of guanine residues results in production of mutagenic 8-oxoguanine adducts21 that are recognized by the mismatch repair system22. Therefore, assembly of a mismatch repair complex (for example, MutSα/MutLα3) at such damage sites could establish a molecular scaffold that allows ATM to phosphorylate and consequently activate CHK2 (Fig. 5). A number of DNA-repair proteins, including MLH1, MSH2, BRCA1, NBS1 and ATM co-exist in a macromolecular complex termed BRCA1-associated surveillance complex (BASC)23. Thus, it is also plausible that activation of CHK2 enabled by mismatch repair could be facilitated through the function of this larger complex at sites of DNA damage.
A recent study identified mutations in MRE11A (meiotic recombination 11 homolog A) in families diagnosed with mismatch repair mutations24. Although we found no evidence for reduced expression of MRE11A in the cell lines used in this study (data not shown), our findings indicate that loss of CHK2 activation accounts for abrogation of the S-phase checkpoint in response to ionizing radiation in cells deficient in mismatch repair. Mutations in MRE11A could potentially accentuate this defect.
Our results indicate that mismatch repair complexes act as adaptors that link ATM and a key downstream effector, CHK2, in response to DNA damage. Such interactions between the mismatch repair system and ATM→CHK2 signaling elucidate a relationship between checkpoint signaling activated by DNA damage and mechanisms of DNA repair. In addition to the mutator phenotype associated with deficiency in mismatch repair3, abrogated S-phase checkpoint activation may further explain the genomic instability and cancer predisposition arising from inactivation of the mismatch repair system.
Methods
Cell lines and culture.
We cultured the MLH1-deficient HCT-116 colorectal tumor line and its derivatives (HCT-116+ch2, HCT-116+ch3; ref. 25) and the MSH2-deficient endometrial adenocarcinoma tumor line HEC59 and its derivative (HEC59+ch2; ref. 26) with or without 400 μg ml−1 G418 (geneticin) as previously outlined27. We obtained the mismatch repair–deficient tumor lines LoVo (MSH2-deficient) and SW48 (MLH1-deficient) from American Type Culture Collection and RKO (MLH1-deficient) cells from T. Pandita. We isolated the RKO derivative that re-expresses MLH1 (RKO/aza50) after two consecutive 4-d treatments with 0.2 μg ml−1 5-aza-2′-deoxycytidine. We obtained SV-40-transformed normal (GM06037H) and ataxia–telangiectasia (GM05849C) fibroblasts from Corriel Cell Repository and cultured them as instructed. We obtained Mlh1+/+ (MC5), Mlh1−/− (MC2) and recombinant MLH1-expressing Mlh1−/− MEFs from R. Liskay and cultured them as outlined28. We confirmed the status of mismatch repair protein expression in all lines by immunoblotting (data not shown).
RDS assay.
We used a modification of a previously outlined procedure1 to analyze the integrity of the S-phase checkpoint. We plated cells in 60-mm tissue-culture dishes at approximately 50% confluency. We removed the medium the next day, replaced it with fresh medium containing 0.01 μCi ml−1 of 14C-labeled thymidine (Amersham) and returned the cells to the incubator. After 24 h, we removed the medium, washed the cells and added fresh medium. We exposed cells to indicated doses of ionizing radiation from a 137Cs source (Gammacell 1000, Atomic Energy of Canada; dose rate = 318 rad min−1) and, unless noted otherwise, returned them to the incubator for 30 min. We then added 20 μCi ml−1 of 3H-labeled thymidine (Amersham) to the medium and incubated cells at 37 ° C for 10 min. After labeling, we washed cells with phosphate-buffered saline, collected them by trypsinization, pelleted them and lysed them in 500 μl of 0.1 N NaOH, 1.0% SDS, 1 mM EDTA. We incubated the lysates at 60 °C in a water bath for 30 min and then added an equal volume of 20% trichloroacetic acid. After vigorous vortexing, we applied the lysates to Whatman GF/A filters and washed them extensively with 10% trichloroacetic acid. Finally, we rinsed the filters with 100% ethanol, air dried them, placed them in glass vials containing 3 ml of scintillation fluid and analyzed them on a Beckman scintillation counter with windows set to record both 14C and 3H d.p.m. We calculated the percent DNA synthesis after exposure to ionizing radiation as ((3H/14C ratio in irradiated cells)/(the 3H/14C ratio in unirradiated cells)) ×100.
Antibodies and immunoblotting.
We purchased the antibody against MLH1 from BD Biosciences and antibody against MSH2 from Calbiochem. We purchased the antibody against CHK2 (total) used for immunoblotting from Oncogene Research, the antibody against phospho-specific (Thr68) CHK2 from Cell Signaling and the antibody against phosphospecific (Ser343) NBS1 from Santa Cruz Biotechnology. We obtained the antibodies against CDC25A and ABL from Lab Vision Corporation and the antibody against NBS1 from Novus Biologicals. We obtained secondary antibodies conjugated with horseradish peroxidase from Bio-Rad and secondary antibody conjugated with fluorescein isothiocyanate from Kirkegaard and Perry Labs. We carried out SDS–PAGE, electrotransfer and immunoblotting as previously outlined29.
Immunoprecipitation.
We treated approximately 1 × 107 cells as outlined above, washed them with ice-cold phosphate-buffered saline and lysed them in 1× lysis buffer (20 mM Tris-HCl (pH 7.5), 150mM NaCl, 5mM EDTA, 0.5% Nonidet-P40, 1 mM NaF, 1mM dithiothreitel, 1mM sodium vanadate and 1 mM leupeptin and aprotinin). After preclearing, we adjusted the lysates for equal protein content and added 5 μl of antiserum against ATM (pAb 132; ref. 29) or 3 μl antibody against CHK2 (ab8108, Abcam). Where indicated, we added 400 ng of the peptide NH2-SRESDVEAQQSHGSSAC-COOH (used as the immunogen for the production of antibody against CHK2) to the lysate before adding antibody against CHK2. After incubating for 2 hr on ice, we added 10 μl of a 50/50 slurry of Protein-A/G beads (Pharmacia) in phosphate-buffered saline and continued the incubation for 1 hr with end-over-end rocking. We washed immunocomplexes three times with 1× lysis buffer containing 500 mM NaCl and twice with 1× lysis buffer containing 100 mM NaCl. We either resuspended immunocomplexes in 1× SDS–PAGE loading buffer and subjected them to immunoblotting (for co-immunoprecipitation experiments) or used them in in vitro kinase assays.
ATM, CHK2 and c-ABL kinase assays.
After immunoprecipitation, we suspended immunocomplexes in 25 μl kinase buffer (25 mM HEPES (pH 7.5), 500 mM NaCl, 5 mM MnCl2, 0.5 mM EDTA, 5 mM dithiothreitol, 2.5 nM phenylmethylsulfonyl fluroride) and added 1 μg of purified recombinant GST–HP–ABL (for ATM kinase assays) or GST–CDC25A (for CHK2 kinase assays), 50 μCi of γ-32P-ATP and 1 mM unlabelled ATP. We carried out c-ABL kinase assays as previously described16 using a GST fusion protein encoding the C-terminal domain of human RNA Pol II (GST–CTD) as the substrate. We incubated reactions for 30 min at room temperature and terminated them by adding an equal volume of 3× SDS–sample buffer. We resolved reaction products on 5–15% acrylamide gels, transferred them onto Immobilon-P membranes and subjected them to autoradiography. We quantified signal intensities by densitometry of exposed films. We also subjected the immunocomplexes to immunoblotting with antibodies against ATM, CHK2 or ABL to assure equivalent kinase abundance in the assays.
Immunofluorescence microscopy.
We seeded cells into dishes containing pre-sterilized glass coverslips. We allowed cells to attach overnight and then exposed them to 10 Gy of ionizing radiation or mock irradiation. We returned dishes to the incubator for 1 h, removed coverslips, rinsed them in phosphate-buffered saline and immersed them in cold (−20 ° C) methanol for 20 min. We then immersed cells in cold acetone for 10 s and washed them three times with phosphate-buffered saline. We labeled cells with a 1:500 dilution of antibody against NBS1 and then stained them with goat antibody against rabbit conjugated with fluorescein isothiocyanate. We photographed cells using a Leitz microscope equipped with epi-fluorescence optics and a SPOT CCD camera.
In vitro association assays (GST pull-down).
We expressed and purified bacterially produced, recombinant GST–CHK2 fusion protein from E. coli as previously described30. We bound approximately 100 ng of this protein to 25 μl glutathione-agarose beads (Pharmacia) and washed it three times with 500 μl binding buffer as outlined by the manufacturer. We prepared lysates from cells exposed to ionizing radiation and from mock-treated cells, adjusted the lysates for equal protein content, added lysates to the suspension of protein-bound glutathione beads in 500 μl binding buffer and incubated the mixture at 4 °C for 1 h with gentle agitation. We then washed the beads three times with binding buffer and suspended them in 1× SDS–PAGE loading buffer. We resolved proteins by SDS–PAGE, transferred them to nitrocellulose sheets and probed them with antibodies against MLH1, MSH2 or CHK2.
References
Painter, R.B. Radioresistant DNA synthesis: an intrinsic feature of ataxia–telangiectasia. Mutat. Res. 84, 183–190 (1981).
Savitsky, K. et al. A single ataxia–telangiectasia gene with a product similar to PI-3 kinase. Science 268, 1749–1753 (1995).
Modrich, P. & Lahue, R. Mismatch repair in replication fidelity, genetic recombination, and cancer biology. Annu. Rev. Biochem. 65, 101–133 (1996).
Goldmacher, V.S., Cuzick, R.A. Jr. & Thilly, W.G. Isolation and partial characterization of human cell mutants differing in sensitivity to killing and mutation by methylnitrosourea and N-methyl-N′-nitro-N-nitrosoguanidine. J. Biol. Chem. 261, 12462–12471 (1986).
Kat, A. et al. An alkylation-tolerant, mutator human cell line is deficient in strand-specific mismatch repair. Proc. Natl. Acad. Sci. USA 90, 6424–6428 (1993).
Zhang, H. et al. Apoptosis induced by overexpression of hMSH2 or hMLH1. Cancer Res. 59, 3021–3027 (1999).
Yan, T. et al. Loss of DNA mismatch repair imparts defective cdc2 signaling and G2 arrest responses without altering survival after ionizing radiation. Cancer Res. 61, 8290–8297 (2001).
Veigl, M.L. et al. Biallelic inactivation of hMLH1 by epigenetic gene silencing, a novel mechanism causing human MSI cancers. Proc. Natl. Acad. Sci. USA 95, 8698–8702 (1998).
Lim, D.S. et al. ATM phosphorylates p95/nbs1 in an S-phase checkpoint pathway. Nature 404, 613–617 (2000).
Gatei, M. et al. ATM-dependent phosphorylation of nibrin in response to radiation exposure. Nat. Genet. 25, 115–119 (2000).
Zhao, S. et al. Functional link between ataxia–telangiectasia and Nijmegen breakage syndrome gene products. Nature 405, 473–477 (2000).
Falck, J., Mailand, N., Syljuasen, R.G., Bartek, J. & Lukas, J. The ATM–Chk2–CDC25A checkpoint pathway guards against radioresistant DNA synthesis. Nature 410, 842–847 (2001).
Falck, J., Petrini, J.H., Williams, B.R., Lukas, J. & Bartek, J. The DNA damage-dependent intra-S phase checkpoint is regulated by parallel pathways. Nat. Genet. 30, 290–294 (2002).
Jinno, S. et al. CDC25A is a novel phosphatase functioning early in the cell cycle. EMBO J. 13, 1549–1556 (1994).
Mailand, N. et al. Rapid destruction of human CDC25A in response to DNA damage. Science 288, 1425–1429 (2000).
Baskaran, R. et al. Ataxia–telangiectasia mutant protein activates c-Abl tyrosine kinase in response to ionizing radiation. Nature 387, 516–519 (1997).
Maser, R.S., Monsen, K.J., Nelms, B.E. & Petrini, J.H. hMre11 and hRad50 nuclear foci are induced during the normal cellular response to DNA double-strand breaks. Mol. Cell. Biol. 17, 6087–6096 (1997).
Matsuoka, S. et al. Ataxia–telangiectasia-mutated phosphorylates Chk2 in vivo and in vitro. Proc. Natl. Acad. Sci. USA 97, 10389–10394 (2000).
Shiloh, Y. Ataxia–telangiectasia and the Nijmegen breakage syndrome: related disorders but genes apart. Annu. Rev. Genet. 31, 635–662 (1997).
Fritzell, J.A. et al. Role of DNA mismatch repair in the cytotoxicity of ionizing radiation. Cancer Res. 57, 5143–5147 (1997).
Chen, S.K., Tsai, M.H., Hwang, J.J., Chang, W.P. & Chan, W.P. Determination of 8-oxoguanine in individual cell nucleus of γ-irradiated mammalian cells. Radiat. Res. 155, 832–836 (2001).
Ni, T.T., Marsischky, G.T. & Kolodner, R.D. MSH2 and MSH6 are required for removal of adenine misincorporated opposite 8-oxo-guanine in S. cerevisiae. Mol. Cell 4, 439–444 (1999).
Wang, Y. et al. BASC, a super complex of BRCA1-associated proteins involved in the recognition and repair of aberrant DNA structures. Genes Dev. 14, 927–939 (2000).
Giannini, G. et al. Human MRE11 is inactivated in mismatch repair–deficient cancers. EMBO Rep. 3, 248–254 (2002).
Koi, M. et al. Human chromosome 3 corrects mismatch repair deficiency and microsatellite instability and reduces N-methyl-N′-nitro-N-nitrosoguanidine tolerance in colon tumor cells with homozygous hMLH1 mutation. Cancer Res. 54, 4308–4312 (1994).
Umar, A. et al. Correction of hypermutability, N-methyl-N′-nitro-N-nitrosoguanidine resistance, and defective DNA mismatch repair by introducing chromosome 2 into human tumor cells with mutations in MSH2 and MSH6. Cancer Res. 57, 3949–3955 (1997).
Nehme, A. et al. Differential induction of c-Jun NH2-terminal kinase and c-Abl kinase in DNA mismatch repair-proficient and -deficient cells exposed to cisplatin. Cancer Res. 57, 3253–3257 (1997).
Buermeyer, A.B., Wilson-Van Patten, C., Baker, S.M. & Liskay, R.M. The human MLH1 cDNA complements DNA mismatch repair defects in Mlh1-deficient mouse embryonic fibroblasts. Cancer Res. 59, 538–541 (1999).
Brown, K.D. et al. The ataxia–telangiectasia gene product, a constitutively expressed nuclear protein that is not upregulated following genome damage. Proc. Natl. Acad. Sci. USA 94, 1840–1845 (1997).
Lee, C.H. & Chung, J.H. The hCds1 (Chk2)-FHA domain is essential for a chain of phosphorylation events on hCds1 that is induced by ionizing radiation. J. Biol. Chem. 276, 30537–30541 (2001).
Acknowledgements
The authors thank S. Elledge for supplying the GST–CHK2 plasmid, J. Lazo for the GST–CDC25A plasmid and B. Gebhardt for access to the 137Cs irradiator. This work was supported by grants from the American Cancer Society to K.D.B. and R.B. and the US National Institutes of Health to R.B.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Brown, K., Rathi, A., Kamath, R. et al. The mismatch repair system is required for S-phase checkpoint activation. Nat Genet 33, 80–84 (2003). https://doi.org/10.1038/ng1052
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1038/ng1052
This article is cited by
-
Pharmacological inhibition of ataxia-telangiectasia mutated exacerbates acute kidney injury by activating p53 signaling in mice
Scientific Reports (2020)
-
The capacity of oocytes for DNA repair
Cellular and Molecular Life Sciences (2018)
-
Deoxyinosine triphosphate induces MLH1/PMS2- and p53-dependent cell growth arrest and DNA instability in mammalian cells
Scientific Reports (2016)
-
Synchronous glioblastoma and medulloblastoma in a child with mismatch repair mutation
Child's Nervous System (2016)
-
TRIM29 regulates the assembly of DNA repair proteins into damaged chromatin
Nature Communications (2015)