Abstract
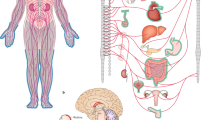
A nonhereditary form of systemic amyloidosis associated with wild-type transthyretin causes heart involvement predominantly in elderly men (systemic senile amyloidosis, or SSA). However, hereditary transthyretin-related amyloidosis (ATTR) is the most frequent form of familial systemic amyloidosis, a group of severe diseases with variable neurological and organ involvement. ATTR remains a challenging and widely underdiagnosed condition, owing to its extreme phenotypic variability: the clinical spectrum of the disease ranges from an almost exclusive neurologic involvement to a strictly cardiac presentation. Such heterogeneity principally results from differential effects of the various reported transthyretin mutations, the geographic region the patient is from and, in the case of the most common mutation, Val30Met, whether or not large foci of cases occur (endemic versus nonendemic aggregation). Genetic or environmental factors (such as age, sex, and amyloid fibril composition) also contribute to the heterogeneity of ATTR, albeit to a lesser extent. The existence of exclusively or predominantly cardiac phenotypes should lead clinicians to consider the possibility of ATTR in all patients who present with an unexplained increase in left ventricular wall thickness at echocardiography. Assessment of such patients should include an active search for possible red flags that can point to the correct final diagnosis.
Key Points
-
Amyloidotic cardiomyopathy is a challenging condition that can mimic many other diseases, such as hypertrophic cardiomyopathy or coronary artery disease
-
Hereditary transthyretin-related amyloidosis (ATTR) is the most frequent form of familial systemic amyloidosis
-
The clinical spectrum of ATTR ranges from almost exclusive neurologic involvement within a clearly familial context, to apparently sporadic cases with a strictly cardiac presentation
-
Phenotypic heterogeneity is linked to at least three different factors: the type of transthyretin mutation, geographic region, and the type of Val30Met aggregation (endemic or nonendemic)
-
Diagnosis of ATTR-related amyloidotic cardiomyopathy generally involves electrocardiography and echocardiography; the specific clinical signs can be very mild and may be missed by the patient
-
Orthotopic liver transplantation or combined heart–liver transplantation can provide surgical 'gene therapy' for amyloidotic cardiomyopathy; the combined procedure can be offered to patients with severe heart failure
This is a preview of subscription content, access via your institution
Access options
Subscribe to this journal
Receive 12 print issues and online access
$209.00 per year
only $17.42 per issue
Buy this article
- Purchase on Springer Link
- Instant access to full article PDF
Prices may be subject to local taxes which are calculated during checkout


Similar content being viewed by others
References
Falk, R. H. & Dubrey, S. W. Amyloid heart disease. Prog. Cardiovasc. Dis. 52, 347–361 (2010).
Shah, K. B., Inoue, Y. & Mehra, M. R. Amyloidosis and the heart: a comprehensive review. Arch. Intern. Med. 166, 1805–1813 (2006).
Maron, B. J. et al. Contemporary definitions and classification of the cardiomyopathies: an American Heart Association scientific statement from the Council on Clinical Cardiology, Heart Failure and Transplantation Committee; Quality of Care and Outcomes Research and Functional Genomics and Translational Biology Interdisciplinary Working Groups; and Council on Epidemiology and Prevention. Circulation 113, 1807–1816 (2006).
Elliott, P. et al. Classification of the cardiomyopathies: a position statement from the European Society of Cardiology Working Group on myocardial and pericardial diseases. Eur. Heart J. 29, 270–276 (2008).
Westermark, P. et al. A primer of amyloid nomenclature. Amyloid 14, 179–183 (2007).
Planté-Bordeneuve, V. et al. Diagnostic pitfalls in sporadic transthyretin familial amyloid polyneuropathy (TTR-FAP). Neurology 69, 693–698 (2007).
Rapezzi, C. et al. Phenotypic and genotypic heterogeneity in transthyretin-related cardiac amyloidosis: towards tailoring of therapeutic strategies? Amyloid 13, 143–153 (2006).
Lachmann, H. J. et al. Misdiagnosis of hereditary amyloidosis as AL (primary) amyloidosis. N. Engl. J. Med. 346, 1786–1791 (2002).
The BEST Steering Committee. Design of the Beta-Blocker Evaluation Survival Trial (BEST). Am. J. Cardiol. 75, 1220–1223 (1995).
Herlenius, G., Wilczek, H. E., Larsson, M., Ericzon, B. G. & Familial Amyloidotic Polyneuropathy World Transplant Registry. Ten years of international experience with liver transplantation for familial amyloidotic polyneuropathy: results from the Familial Amyloidotic Polyneuropathy World Transplant Registry. Transplantation 77, 64–71 (2004).
Sekijima, Y., Kelly, J. W. & Ikeda, S. Pathogenesis of and therapeutic strategies to ameliorate the transthyretin amyloidoses. Curr. Pharm. Des. 14, 3219–3230 (2008).
Dickson, P. W. et al. High prealbumin and transferrin mRNA levels in the choroid plexus of rat brain. Biochem. Biophys. Res. Commun. 127, 890–895 (1985).
Robbins, J. Thyroxine binding proteins. Prog. Clin. Biol. Res. 5, 331–355 (1976).
Benson, M. D. & Kincaid, J. C. The molecular biology and clinical features of amyloid neuropathy. Muscle Nerve 36, 411–423 (2007).
Westermark, P., Sletten, K., Johansson, B. & Cornwell, G. G. Fibril in senile systemic amyloidosis is derived from normal transthyretin. Proc. Natl Acad. Sci. USA 87, 2843–2845 (1990).
Hou, X., Aguilar, M. I. & Small, D. H. Transthyretin and familial amyloidotic polyneuropathy. Recent progress in understanding the molecular mechanism of neurodegeneration. FEBS J. 274, 1637–1650 (2007).
Ando, Y., Nakamura, M. & Araki, S. Transthyretin-related familial amyloidotic polyneuropathy. Arch. Neurol. 62, 1057–1062 (2005).
Rapezzi, C. et al. Systemic cardiac amyloidoses. Disease profiles and clinical courses of the three main types. Circulation 120, 1203–1212 (2009).
Dubrey, S. W., Burke, M. M., Hawkins, P. N. & Banner, N. R. Cardiac transplantation for amyloid heart disease—the United Kingdom experience. J. Heart Lung Transplant. 23, 1142–1153 (2004).
Lessell, S., Wolf, P. A., Benson, M. D. & Cohen, A. S. Scalloped pupils in familial amyloidosis. N. Engl. J. Med. 293, 914–915 (1975).
Ikeda, S. Cardiac amyloidosis: heterogenous pathogenic backgrounds. Intern. Med. 43, 1107–1114 (2004).
Koyama, J. et al. Usefulness of pulsed tissue Doppler imaging for evaluating systolic and diastolic left ventricular function in patients with AL (primary) amyloidosis. Am. J. Cardiol. 89, 1067–1071 (2002).
Klein, A. L. et al. Doppler characterization of left ventricular diastolic function in cardiac amyloidosis. J. Am. Coll. Cardiol. 13, 1017–1026 (1989).
Andrade, C. A peculiar form of peripheral neuropathy. Familial atypical generalized amyloidosis with special involvement of the peripheral nerves. Brain 75, 408–427 (1952).
Conceição, I. & De Carvalho, M. Clinical variability in type I familial amyloid polyneuropathy (Val30Met): comparison between late- and early-onset cases in Portugal. Muscle Nerve 35, 116–118 (2007).
Bittencourt, P. L. et al. Phenotypic expression of familial amyloid polyneuropathy in Brazil. Eur. J. Neurol. 12, 289–293 (2005).
Ikeda, S., Nakazato, M., Ando, Y. & Sobue, G. Familial transthyretin-type amyloid polyneuropathy in Japan: clinical and genetic heterogeneity. Neurology 58, 1001–1007 (2002).
Suhr, O. B. et al. Hereditary transthyretin amyloidosis from a Scandinavian perspective. J. Intern. Med. 254, 225–235 (2003).
Ohmori, H. et al. Common origin of the Val30Met mutation responsible for the amyloidogenic transthyretin type of familial amyloidotic polyneuropathy. J. Med. Genet. 41, 51–55 (2004).
Soares, M. L. et al. Haplotypes and DNA sequence variation within and surrounding the transthyretin gene: genotype–phenotype correlations in familial amyloid polyneuropathy (V30M) in Portugal and Sweden. Eur. J. Hum. Genet. 12, 225–237 (2004).
Hellman, U. et al. Heterogeneity of penetrance in familial amyloid polyneuropathy, ATTR Val30Met, in the Swedish population. Amyloid 15, 181–186 (2008).
Jacobson, D. R. et al. Variant-sequence transthyretin (isoleucine 122) in late-onset cardiac amyloidosis in black Americans. N. Engl. J. Med. 336, 466–473 (1997).
Koeppen, A. H., Wallace, M. R., Benson, M. D. & Altland, K. Familial amyloid polyneuropathy: alanine-for-threonine substitution in the transthyretin (prealbumin) molecule. Muscle Nerve 13, 1065–1075 (1990).
Yamamoto, K. et al. Familial amyloid polyneuropathy in Taiwan: identification of transthyretin variant (Leu55>Pro). Muscle Nerve 17, 637–641 (1994).
Mak, C. M. et al. Identification of a novel TTR Gly67Glu mutant and the first case series of familial transthyretin amyloidosis in Hong Kong Chinese. Amyloid 14, 293–297 (2007).
Jacobson, D. R. et al. Revised transthyretin Ile122 allele frequency in African-Americans. Hum. Genet. 98, 236–238 (1996).
Svendsen, I. H., Steensgaard-Hansen, F. & Nordvåg, B. Y. Hereditary amyloid cardiomyopathy related to a mutation at transthyretin protein number 111. A clinical, genetic and echocardiographic study of an affected Danish family. Ugeskr. Laeger. 161, 4995–4999 (1999).
Plante-Bordeneuve, V. et al. Genotypic–phenotypic variations in a series of 65 patients with familial amyloid polyneuropathy. Neurology 51, 708–714 (1998).
Gillmore, J. D., Booth, D. R., Pepys, M. B., Hawkins, P. N. Hereditary cardiac amyloidosis associated with the transthyretin Ile122 mutation in a white man. Heart 82, e2 (1999).
Rapezzi, C. et al. Gender-related risk of myocardial involvement in systemic amyloidosis. Amyloid 15, 40–48 (2008).
Ihse, E. et al. Amyloid fibril composition is related to the phenotype of hereditary transthyretin V30M amyloidosis. J. Pathol. 216, 253–261 (2008).
Rahman, J. E. et al. Noninvasive diagnosis of biopsy-proven cardiac amyloidosis. J. Am. Coll. Cardiol. 43, 410–415 (2004).
Murtagh, B. et al. Electrocardiographic findings in primary systemic amyloidosis and biopsy-proven cardiac involvement. Am. J. Cardiol. 95, 535–537 (2005).
Sun, J. P. et al. Differentiation of hypertrophic cardiomyopathy and cardiac amyloidosis from other causes of ventricular wall thickening by two-dimensional strain imaging echocardiography. Am. J. Cardiol. 103, 411–415 (2009).
Selvanayagam, J. B., Hawkins, P. N., Paul, B., Myerson, S. G. & Neubauer, S. Evaluation and management of the cardiac amyloidoses. J. Am. Coll. Cardiol. 50, 2101–2110 (2007).
Koyama, J., Davidoff, R. & Falk, R. H. Longitudinal myocardial velocity gradient derived from pulsed Doppler tissue imaging in AL amyloidosis: a sensitive indicator of systolic and diastolic dysfunction. J. Am. Soc. Echocardiogr. 17, 36–44 (2004).
Maceira, A. M. et al. Cardiovascular magnetic resonance in cardiac amyloidosis. Circulation 111, 186–193 (2005).
Perugini, E. et al. Non-invasive evaluation of the myocardial substrate of cardiac amyloidosis by gadolinium cardiac magnetic resonance. Heart 92, 343–349 (2006).
Glaudemans, A. W. et al. Nuclear imaging in cardiac amyloidosis. Eur. J. Nucl. Med. Mol. Imaging 36, 702–714 (2009).
Hazenberg, B. P. et al. Diagnostic performance and prognostic value of extravascular retention of 123I-labeled serum amyloid P component in systemic amyloidosis. J. Nucl. Med. 48, 865–872 (2007).
Gertz, M. A. et al. Definition of organ involvement and treatment response in immunoglobulin light chain amyloidosis (AL): a consensus opinion from the 10th international symposium on amyloid and amyloidosis. Am. J. Hematol. 79, 319–328 (2005).
Kyle, R. A. & Gertz, M. A. Primary systemic amyloidosis: clinical and laboratory features in 474 cases. Semin. Hematol. 32, 45–59 (1995).
Merlini, G. & Palladini, G. Amyloidosis: is a cure possible? Ann. Oncol. 19, iv63–iv66 (2008).
Ng, B. et al. Senile systemic amyloidosis presenting with heart failure: a comparison with light chain-associated amyloidosis. Arch. Intern. Med. 165, 1425–1429 (2005).
Dubrey, S. W., Cha, K., Skinner, M., LaValley, M. & Falk, R. H. Familial and primary (AL) cardiac amyloidosis: echocardiographically similar diseases with distinctly different clinical outcomes. Heart 78, 74–82 (1997).
Berk, J. L. et al. Persistent pleural effusions in primary systemic amyloidosis: etiology and prognosis. Chest 124, 969–977 (2003).
Santarone, M. et al. Atrial thrombosis in cardiac amyloidosis: diagnostic contribution of transesophageal echocardiography. J. Am. Soc. Echocardiogr. 12, 533–536 (1999).
Gertz, M. A., Falk, R. H., Skinner, M., Cohen, A. S. & Kyle, R. A. Worsening of congestive heart failure in amyloid heart disease treated by calcium channel-blocking agents. Am. J. Cardiol. 55, 1645 (1985).
Pollak, A. & Falk, R. H. Left ventricular systolic dysfunction precipitated by verapamil in cardiac amyloidosis. Chest 104, 618–620 (1993).
Wright, B. L., Grace, A. A. & Goodman, H. J. Implantation of a cardioverter-defibrillator in a patient with cardiac amyloidosis. Nat. Clin. Pract. Cardiovasc. Med. 3, 110–114 (2006).
Becker, R., Katus, H. A. & Bauer, A. Prophylactic implantation of cardioverter-defibrillator in patients with severe cardiac amyloidosis and high risk for sudden cardiac death. Heart Rhythm 5, 235–240 (2008).
Falk, R. H., Rubinow, A. & Cohen, A. S. Cardiac arrhythmias in systemic amyloidosis: correlation with echocardiographic abnormalities. J. Am. Coll. Cardiol. 3, 107–113 (1984).
Freeman, R. Neurogenic orthostatic hypotension. N. Engl. J. Med. 358, 615–624 (2008).
Obayashi, K. et al. Effect of sildenafil citrate (Viagra) on erectile dysfunction in a patient with familial amyloidotic polyneuropathy ATTR Val30Met. Auton. Nerv. Syst. 12, 89–92 (2000).
Dubrey, S. W. et al. Progression of ventricular wall thickening after liver transplantation for familial amyloidosis. Transplant 64, 74–80 (1997).
Yazaki, M. et al. Cardiac amyloid in patients with familial amyloid polyneuropathy consists of abundant wild-type transthyretin. Biochem. Biophys. Res. Commun. 274, 702–706 (2000).
Stangou, A. J., Heaton, N. D. & Hawkins, P. N. Transmission of systemic transthyretin amyloidosis by means of domino liver transplantation. N. Engl. J. Med. 352, 2356 (2005).
Arpesella, G. et al. Combined heart and liver transplantation for familial amyloidotic polyneuropathy. J. Thorac. Cardiovasc. Surg. 125, 1165–1166 (2003).
Ferreira, N. et al. Binding of epigallocatechin-3-gallate to transthyretin modulates its amyloidogenicity. FEBS Lett. 583, 3569–3576 (2009).
Palladini, G. et al. Serum N-terminal pro-brain natriuretic peptide is a sensitive marker of myocardial dysfunction in AL amyloidosis. Circulation 107, 2440–2445 (2003).
Perugini, E. et al. Noninvasive etiologic diagnosis of cardiac amyloidosis using 99mTc-3, 3-diphosphono-1, 2-propanodicarboxylic acid scintigraphy. J. Am. Coll. Cardiol. 46, 1076–1084 (2005).
Dispenzieri, A. et al. Survival in patients with primary systemic amyloidosis and raised serum cardiac troponins. Lancet 361, 1787–1789 (2003).
Dispenzieri, A. et al. Prognostication of survival using cardiac troponins and N-terminal pro-brain natriuretic peptide in patients with primary systemic amyloidosis undergoing peripheral blood stem cell transplantation. Blood 104, 1881–1887 (2004).
Suhr, O. B. et al. Do troponin and B-natriuretic peptide detect cardiomyopathy in transthyretin amyloidosis? J. Intern. Med. 263, 294–301 (2008).
Acknowledgements
We thank Robin M. T. Cooke for editorial advice and writing assistance, which was indirectly funded by a 1-year contract with the Fondazione Maugeri, a not-for-profit organization providing evidence-based medical services within the framework of the Italian National Health Service.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Competing interests
The authors declare no competing financial interests.
Rights and permissions
About this article
Cite this article
Rapezzi, C., Quarta, C., Riva, L. et al. Transthyretin-related amyloidoses and the heart: a clinical overview. Nat Rev Cardiol 7, 398–408 (2010). https://doi.org/10.1038/nrcardio.2010.67
Published:
Issue Date:
DOI: https://doi.org/10.1038/nrcardio.2010.67
This article is cited by
-
Molecular dynamics simulation-based understanding of the structure and property of amyloid proteins at multiple length scales
JMST Advances (2023)
-
Does [99mTc]-3,3-diphosphono-1,2-propanodicarboxylic acid (DPD) soft tissue uptake allow the identification of patients with the diagnosis of cardiac transthyretin-related (ATTR) amyloidosis with higher risk for polyneuropathy?
Journal of Nuclear Cardiology (2023)
-
Multi-parametric speckle tracking analyses to characterize cardiac amyloidosis: a comparative study of systolic left ventricular longitudinal myocardial mechanics
Heart and Vessels (2022)
-
Assessment of cardiac amyloidosis with 99mTc-pyrophosphate (PYP) quantitative SPECT
EJNMMI Physics (2021)
-
Patient-reported burden of hereditary transthyretin amyloidosis on functioning and well-being
Journal of Patient-Reported Outcomes (2021)